Introduction
Gestational diabetes mellitus (GDM), defined as glucose intolerance with onset or first recognition during pregnancy1, occurs in 3.6% of pregnant women in Victoria Australia2, increasing to 15% among some ethnic groups3. Women with a history of GDM are at high risk of developing type 2 diabetes mellitus (T2DM), with up to 70% developing T2DM, depending on ethnicity4. Given the rapidly increasing prevalence of diabetes globally, there is an urgent need to develop preventative strategies and to identify high risk populations who would most benefit from diabetes prevention5,6. Individuals with impaired glucose tolerance are one such high risk population, and the results of several large randomised controlled trials indicate that T2DM is a potentially preventable condition7-9. Women with a history of GDM are another high risk population who would benefit from lifestyle interventions such as healthy weight, regular exercise and healthy eating. While approximately 15% of the population of women enrolled in the Diabetes Prevention Program had a history of GDM, there are limited studies targeting interventions to reduce diabetes risk in women with a history of GDM, and none involving rural women10.
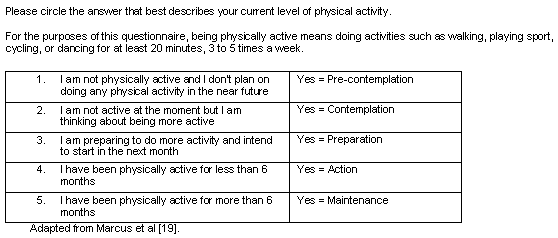
Mothers with young children have difficulties engaging in healthy lifestyle programs because of lack of time, multiple commitments, lack of energy and resuming work11-15. Successful healthy lifestyle programs must address these barriers and consider participants' readiness to make lifestyle changes. The stages of change or transtheoretical model16 describes five stages in a person's readiness to change health behaviour. The first two stages represent individuals who are not ready to change (pre-contemplation) or who are ambivalent about change (contemplation). The third stage (preparation) represents individuals who have decided to make a change and intend to do so within the next month. The last two stages represent active behaviour change, with recent (action) or sustained, defined as more than 6 months, behaviour change (maintenance). Individuals can move in either direction between stages, usually in spiral rather than linear fashion, where relapse of behaviour is the rule rather than the exception17.
This pilot study aimed to examine the readiness of a cohort of rural women with a history of GDM to engage in diabetes risk reduction behaviour with respect to physical activity and achieving a healthy weight.
Background
The diabetes centre of a large regional hospital in northern Victoria, Australia is the major referral site for specialist care of women with GDM. Based on the 1998 Australasian Diabetes in Pregnancy Society (ADIPS) guidelines, all pregnant women are screened for GDM at 28 weeks gestation with a 50 g glucose challenge test. A 75 g oral glucose tolerance test (OGTT) is used to confirm the diagnosis18. After the birth of their baby, women who have had GDM are routinely supplied with a pathology request for a repeat OGTT at 6 weeks postpartum, and are given lifestyle advice regarding the risk of developing T2DM. No routine follow up is offered to these women. The current system offers limited opportunities for effective diabetes prevention.
Methods
This pilot study examined a population of women who had attended the diabetes centre over a 14 month period (July 2004 to July 2005) for management of GDM. All women in this population were eligible, and women who were unable to complete the questionnaire but who wished to participate were given assistance to do so, for example by engaging an interpreter when a language barrier existed. Women were recruited by mail using contact details obtained from medical records. A survey package containing the questionnaire, plain language statement, consent and withdrawal of consent, was mailed to all women. A reminder letter was mailed 2 weeks after the initial survey, and a further survey package was mailed to those women who had not responded after 3 weeks. All participating women gave written informed consent to participate in the study. Approval was obtained from the Goulburn Valley Health Ethics Review Committee and the University of Melbourne Human Research Ethics Committee.
Stage of change was measured using a validated instrument (Appendix I) adapted from Marcus et al19, in which participants reported stage of change for physical activity and current weight loss behaviour. Perception of diabetes risk was assessed using a six-point Likert scale, with responses ranging from strongly agree to strongly disagree (Table 1). Descriptive information was collected about participants' ages, number of children, age of youngest child, postcode, working status, family income category and language spoken at home. Self-reported weight and height was used to calculate body mass index (BMI) in kg/m2. Physical activity was defined as walking, playing sport, cycling or dancing, for 20-30 min, three to five times weekly, which is recommended as minimum physical activity required for health benefits20.
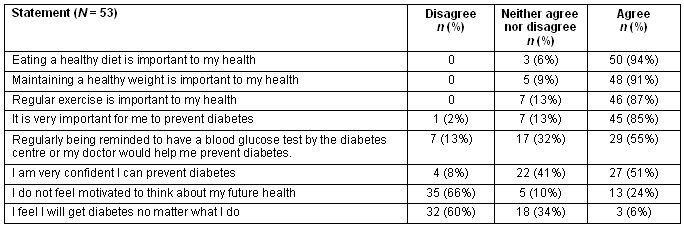
Table 1: Perception of risk of developing diabetes
Statistical analysis
Due to small numbers in the study respondents were divided into pre-action (includes the women in pre-contemplation, contemplation and preparation stages) and action (includes the women in action and maintenance stages) groups for comparative analyses. To assess the relationship between stage of change for weight loss and other variables, women who reported their weight as being at a healthy level were excluded from analysis. Responses for perception of diabetes risk questions were categorised as disagree (1 & 2), neither agree nor disagree (3 & 4), and agree (5 & 6). Each completed questionnaire was coded, entered into a database and analysed using the Statistical Package for Social Sciences (SPSS Inc; Chicago, IL, USA). Statistical tests (χ squared, Fisher exact probability test, frequencies and cross tabulations) were conducted to test for differences in responses between the action and pre-action groups.
Results
There were 53 women who completed the survey (mean age 32.5 (±5.08), mean ± SD years); response rate 75%. Two-thirds of the women (68%) had two or more children, and half (49%) had a child less than 6 months old. A quarter (26%) had resumed paid work (part or full time). Fifteen percent reported Arabic as the primary language. Three women did not report their weight and three women did not report working status. Based on self-reported height and weight, 24% of women were overweight (BMI 25-29 kg/2 and 42% were obese (BMI ≥ 30 kg/m2.
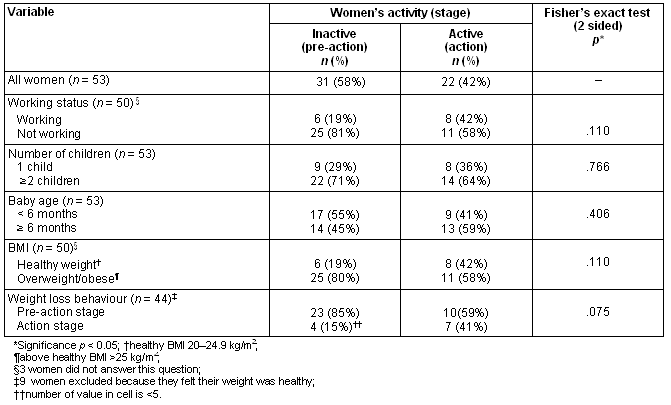
Table 2 shows that 58% of respondents were classified as pre-action for physical activity. Of these, 3% were at pre-contemplation stage, 45% at contemplation and 52% at the preparatory stage. In those respondents meeting activity guidelines, half were at action stage and half at maintenance stage. Women in pre-action for activity were slightly younger (mean age 31.5 ± 3.9) than women in action (mean age 34.1 ± 6.0). Prevalence of pre-action for activity was highest in women with a BMI above 25kg/m2, women in pre-action for weight loss and women not engaged in paid work. For the women in pre-action for activity, 85% were also in pre-action for weight loss. Physical activity did not appear to be influenced by baby age. Of the women with more than two children, two-thirds (61%) were in pre-action for activity and the majority (80%) were in pre-action for weight loss.
Table 2: Prevalence of readiness for physical activity
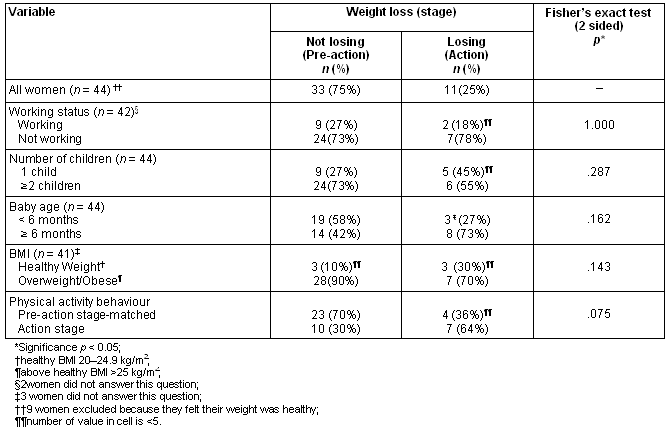
Seventeen percent of women felt their weight was at a healthy level. Of those women who felt they needed to lose weight 41% were at contemplation, 34% were at preparation for weight loss, 15% were at action and 10% were at maintenance for weight loss. The age of women in pre-action for weight loss (mean age 31.9 ± 4.5) was similar to women in action (mean age 31.7 ± 2.8). Table 3 summarises women who felt they needed to lose weight and shows that 75% of this group were in pre-action for weight loss. Prevalence of pre-action for weight loss was highest among women with more than two children, not engaged in paid work; in pre-action for activity and women with a BMI above 25kg/m2. Prevalence of pre-action for weight loss was not influenced by baby age. Despite these trends, there were no statistically significant differences between women in pre-action and action for physical activity or weight loss.
Table 3: Prevalence of readiness for weight loss behaviour
Women engaging in optimal diabetes risk reduction would either be a healthy weight, or be actively losing weight while also being physically active. Of the total sample, 15 women (30%) were active and managing their weight; either having a healthy BMI or currently losing weight. These women were using all available opportunities for diabetes risk reduction. Nearly half (43%) were at pre-action for both activity and weight loss and so not engaging in any diabetes risk reduction behaviour.
Responses relating to risk of developing diabetes are summarised (Table 1). The majority of women agreed healthy lifestyle choices, eating a healthy diet, maintaining a healthy weight and doing regular exercise, were important for good health. Similarly, importance for preventing diabetes was rated highly. Two-thirds of respondents disagreed with the statements 'I do not feel motivated to think about my future health' and 'I feel I will get diabetes no matter what I do'.
Discussion
This study is the first to investigate readiness to change among Australian rural women with a history of GDM, which increases their risk of developing T2DM. The findings indicate a clear need to promote physical activity and weight loss in the postnatal period to this high risk group. The majority of women were in pre-action for physical activity and, of those who felt they needed to lose weight, for weight loss. This finding is consistent with pre-action in other populations. In a review of five cross-sectional studies of health behaviours in adults, including activity and weight loss, weight loss pre-action ranged between 34.1% and 68.2% and physical activity pre-action between 43.4% to 59%21.
The majority of women in pre-action for activity were also in pre-action for weight loss. This group of women were the least engaged in diabetes risk behaviours. There is limited literature exploring lifestyle choices in women with a history of GDM. One Australian study involving 225 women with a history of GDM identified two-thirds of the sample (66.4%) were not achieving sufficient activity for health benefits and more than half (51.3%) were above their healthy weight range. Main barriers to physical activity were identified as lack of assistance with child care and insufficient time. Confidence to be active was lowest when these women were time pressured and tired22. Strategies to engage women who are in pre-action for diabetes risk reduction behaviours will need to explore individual barriers to change and target ambivalence12,23. Further research is needed to test the efficacy of time-friendly interventions such as mail, telephone and electronic communications in this population, given that women in the postnatal period may be difficult to engage in intervention projects due to multiple commitments.
In this study prevalence of pre-action for physical activity and weight loss behaviour was highest among mothers with larger families. Time commitments of having multiple children may prevent mothers from engaging in physical activity. In addition, exercising with one child is likely to be easier than with multiple children, especially when older children reach an age of not wanting to or not being able to sit in a pusher. The combination of low physical activity and being overweight creates a cycle of behaviour that is difficult for many women to break. These findings are of concern in light of research indicating that failure to lose weight in the first year postpartum is a predictor of longer term obesity in the mother24,25. If weight gained during pregnancy is not lost by the time a woman falls pregnant again, it is likely that a cumulative weight gain effect will occur.
Our study found that women who were engaged in paid work (full or part time) were more active than those not working. This is surprising because working mothers would be expected to have less time to be physically active and 'no time' has previously been reported as a significant barrier to physical activity26. However, employed women may value physical activity more than women not engaged in paid work. Employed women may also be better placed to negotiate partner support for and engagement in domestic chores and childrearing. Partner support has been found to be pivotal in mothers being able to prioritise activity as part of an already busy schedule27. These issues warrant further study in the rural setting.
The fact that less women with a healthy weight reported that they thought their weight was healthy may reflect a lack of knowledge of what constitutes a healthy weight by women wanting to return to their pre-pregnancy weight, or a cultural view that lower weight represents healthy weight. While the vast majority of postnatal women may require advice regarding weight loss, a smaller number may need to be advised about the benefits of weight maintenance. Similar numbers of women with a healthy BMI were in action and pre-action for activity. Regular physical activity should be encouraged on its own merit and not be confused with it being a weight management tool.
Women expressed a high level of motivation, optimism and confidence to prevent diabetes along with a high awareness of the importance of regular physical activity, healthy weight and healthy diet. This occurred despite the high level of pre-action for physical activity and weight loss. Despite this finding, a large proportion of the study sample in pre-action were in preparation stage for activity and weight loss (planning to do more physical activity in the next month and planning on losing weight in the next month). If this were the case, subsequent analysis may show a higher degree of engagement in diabetes risk reduction behaviours. However, previous research has indicated that women with a history of GDM, although concerned about their health and aware of their risk of developing diabetes, do not necessarily engage in risk reduction behaviour28. It is generally felt that women maintain the healthy eating patterns established as part of management of GDM because the immediate priority is the health of their baby. Once an episode of GDM is over, maintenance of these behaviours may be more difficult.
Lifestyle change requires both motivation and readiness. The women in this study, while motivated, were not ready to adopt healthy lifestyle behaviours. Women may not see the risk of diabetes as of immediate concern, particularly when there are no symptoms associated with the early development of diabetes. In addition, the postnatal period is a time during which many changes occur in a woman's life. Competing responsibilities can alter sleeping habits, work schedules, eating patterns, exercise regularity and time allocation14,26. This can challenge even the most committed mother of young children. Clearly, strategies to assist this population to overcome barriers associated with behaviour change in the postnatal period are needed.
Despite a high level of motivation to prevent type 2 diabetes, one-third of the study sample felt they were either unsure or agreed that they would get diabetes even if they followed recommended lifestyle changes. This indicates a number of women may feel there is little incentive for them to increase activity and reduce weight if they are going to get diabetes anyway. An opportunity exists for health professionals to empower these women to believe they have a role in diabetes prevention, despite high risk.
The limitations of this study include a small sample size and reliance on self-reported physical activity, weight loss behaviour and weight/height. While self-report is a less reliable technique than objective measurement, it allows for easier data collection, at low cost, and does not alter the behaviour under study29. However, previous research indicates that individuals over-report level of physical activity and height and under-report weight30,31. Results presented are likely to be an underestimation of weight status and an overestimate of actual physical activity, suggesting that proportions of women in the overweight/obese category may be greater than reported, with lower proportions engaging in physical activity. While the sample is representative of this population, it may be underpowered to detect significant correlations (type II error).
As with other research projects conducted in communities where researchers and subjects are known to each other, a social desirability bias may have influenced the self-reported information. All subjects in this pilot study had previously attended the diabetes centre and knew the researchers. This could explain the high level of preparation for both weight loss and activity, because respondents may believe it preferable to answer that they are about to commence a behaviour rather than not seriously considering change. Readiness to change behaviour, as reported within stage of change, may not equate to actual readiness to modify behaviour.
The current study measured readiness to change activity but no measurement of amount of activity was performed. Hence, it is unclear from this study how much or what type of activity women were performing. In addition, no information about patterns of lactation, educational status or income level was obtained. These data may have helped to explain patterns of readiness to engage in healthy lifestyle behaviour. Studies with larger samples in rural populations may be able to further investigate these issues.
Overall these results represent the views of this group of rural women with a history of GDM. The study adds to the limited information available on this population group and provides insight into the health behaviours and beliefs about diabetes prevention following an episode of GDM. Encouraging individuals at high risk of chronic disease to change lifestyle behaviours if often difficult and, therefore, understanding what factors these women believe to be important in diabetes prevention may help in the development of more effective and efficient interventions. However, larger cohort studies are needed to obtain a better estimate of the impacts of GDM and to fully understand the issues, readiness to change, levels of engagement and interventions that may be effective in this vulnerable population in rural Victoria.
Conclusion
The results reported here demonstrate that the majority of rural women with a history of GDM in northern Victoria were not ready to actively prevent diabetes. More than half were not active and three-quarters were overweight. Although most respondents were aware of how to prevent diabetes, only half were involved in some diabetes risk reduction behaviour. The reasons are likely to be multifactorial. In addition to child-care and partner support programs, there is need for programs designed to increase readiness to change in this vulnerable group. Successful health interventions will need to target ambivalence to behaviour change, while keeping in mind this population have multiple commitments and may have difficulty being able to prioritise health promotion and disease prevention activities. The challenge remains to design interventions that do not add to the already busy life of a mother with young children.
Acknowledgements
This research project was funded by a University of Melbourne School of Rural Health Primary HealthCare Research Evaluation and Development (PHCRED) Fellowship. The project was made possible with the help of the GV Health Diabetes Centre team and the willing participants.
References
1. American Diabetes Association. Gestational diabetes mellitus. Diabetes Care 2003; 26 (Suppl1): S103-S105.
2. Stone CA, McLachlan KA, Halliday JL, Wein P, Tapsell C. Gestational diabetes in Victoria in 1996: incidence, risk factors and outcomes. Medical Journal of Australia 2002; 177: 486-491.
3. Beischer NA, Oats JN, Henry OA, Sheedy MT, Walstab JE. Incidence and severity of gestational diabetes mellitus according to country of birth in women living in Australia. Diabetes 1991; 40(Suppl2): 35-38.
4. Kim C, Newton KM, Knopp RH. Gestational diabetes and the incidence of type 2 diabetes. Diabetes Care 2002; 25: 1862-1868.
5. Cheung NW, Byth K. Population health significance of gestational diabetes. Diabetes Care 2003; 26: 2005-2009.
6. King H, Aubert RE, Herman WH. Global Burden of Diabetes, 1995-2025. Diabetes Care 1998; 21: 1414-1431.
7. American Diabetes Association. The prevention or delay of type 2 diabetes. Diabetes Care 2002; 25: 742-749.
8. Eriksson KF, Lindgarde F. Prevention of type 2 (non-insulin-dependent) diabetes mellitus by diet and physical exercise. The 6-year Malmö feasibility study. Diabetologia 1991; 34: 891-898.
9. Lindström J, Eriksson J, Louheranta A, Uusitupa M, Mannelin M, Tuomilehto J et al. The Finnish Diabetes Prevention Study. Lifestyle intervention and 3-year results on diet and physical activity. Diabetes Care 2003; 26: 3232-3236.
10. The Diabetes Prevention Program. The Diabetes Prevention Program (DPP). Description of lifestyle intervention. Diabetes Care 2002; 25: 2165-2171.
11. Gennaro S, Fehder W. Health behaviours in postpartum women. Family Community Health 2000; 22(4): 16-26.
12. O'Toole ML, Sawicki MA, Artal R. Structured diet and physical activity prevent postpartum weight retention. Journal of Women's Health 2003; 12: 991-998.
13. Sampselle CM, Seng J, Yeo S, Killion C, Oakley D. Physical activity and postpartum well being. Journal of Obstetric, Gynecologic and Neonatal Nursing 1999; 28: 41-49.
14. Walker LO. Factors related to new mothers' readiness to manage weight. American Journal of Health Behaviour1999; 23(4268-279): 268-279.
15. Symons Downs D, Ulbrecht JS. Understanding exercise beliefs and behaviors in women with gestational diabetes mellitus. Diabetes Care 2006; 29: 236-240.
16. Prochaska JO, DiClemente CC. Stages and processes of self-change of smoking: toward an integrative model of change. Journal of Consulting and Clinical Psychology 1983; 51: 390-395.
17. Prochaska JO, Velicer WF. The transtheoretical model of health behaviour change. American Journal of Health Promotion 1997; 12: 38-48.
18. Hoffman L, Nolan C, Wilson JD, Oats JJN, Simmons D. Gestational diabetes mellitus-management guidelines. The Australasian diabetes in pregnancy society. Medical Journal of Australia 1998; 169: 93-97.
19. Marcus BH, Banspach SW, Lefebvre RC, Rossi JS, Carleton RA, Abrams DB. Using the stages of change model to increase the adoption of physical activity among community participants. American Journal of Health Promotion1992; 6: 424-429.
20. Department Of Health And Ageing. National physical activity guidelines for Australians, Canberra. (Online) 2005. Available: http://www.health.gov.au/internet/wcms/publishing.nsf/content/phd-physical-activity-adults-pdf-cnt.htm (Accessed 20 October 2006).
21. Laforge R, Velicer WF, Richmond R, Owen N. Stage distributions for five health behaviours in the United States and Australia. Preventive Medicine 1999; 28: 61-74.
22. Smith BJ, Zehle K, Cheung NW, McLean M, Bauman AE. Postpartum physical activity and related psychosocial factors among women with recent gestational diabetes mellitus. Diabetes Care 2005; 28: 2650-2654.
23. Leermakers EA, Anglin K, Wing RR. Reducing postpartum weight retention through a correspondence intervention. International Journal of Obesity 1998; 22:1103-1109.
24. Linné Y, Dye L, Barkeling B, Rössner S. Long-term weight development in women: A 15-year follow-up of the effects of pregnancy. Obesity Research 2004; 12:1166-1178.
25. Rooney BL, Schauberger CW. Excess pregnancy weight gain and long-term obesity: one decade later. American Journal of Obstetrics and Gynecology 2002; 100: 245-252.
26. Lo Cascio M, Thomas M, Connelly A. Busy mums wanted: A qualitative study of mothers and physical activity. Sydney, NSW: Social Health Research Unit, Central Sydney Area Health Service, 1999.
27. Bauman A, Bellow B, Booth ML, Hahn A, Stoker L, Thomas M. Towards best practice for the promotion of physical activity in the areas of NSW. Sydney, NSW: NSW Health, 1996.
28. Feig DS, Chen E, Naylor CD. Self-perceived health status of women three to five years after the diagnosis of gestational diabetes: a survey of cases and matched controls. American Journal of Obstetrics and Gynecology 1998; 178: 386-393.
29. Sallis JF, Saelens BE. Assessment of physical activity by self-report: status, limitations, and future directions. Research Quarterly for Exercise and Sport 2000; 71: 1-14.
30. Flood V, Webb K, Lazarus R, Pang G. Use of self-report to monitor overweight and obesity in populations: some issues for consideration. Australian and New Zealand Journal of Public Health 2000; 24: 96-99.
31. Booth ML, Owen N, Bauman AE, Gore CJ. Retest reliability of recall measures of leisure-time physical activity in Australian adults. International Journal of Epidemiology 1996; 25: 153-159.
_________________________
Appendix I
Stage of Change Questionnaire for exercise (for weight loss substitute losing weight for physical activity)