Context
Healthcare systems are dynamic. Accordingly, healthcare stakeholders and professional practitioners must be prepared to update policies, procedures, protocols and processes. Professional practitioners are duty bound to implement practices, procedures and guidelines based on recent evidence, and to undertake professional development and continuing professional education programs. Self and system review must be based on reflection on practice, observed and assessed needs, and directions from statutory bodies and government departments. In addition, action research can identify outdated information. This article provides an example of such processes in the review of a remote operators' (RO) radiation-licence training manual in Darwin, Northern Territory (NT), Australia, which ensured effective practice to safeguard the service sector, professional practitioners and their clients.
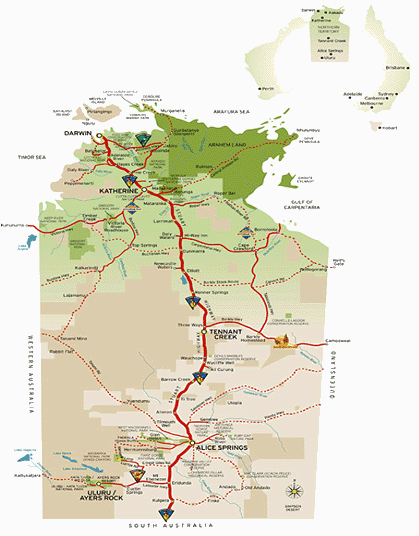
Figure 1: Map of Northern Territory and Australia (reproduced with permission of Tourism NT, http://www.travelnt.com).
Darwin, the territory capital, is a geographically and culturally isolated city. Among the NT population of 206 6881, 96 573 reside in the metropolitan areas of Darwin and Palmerston. Of the remaining population, 56 084 live in the towns of Alice Springs, Tennant Creek, Katherine and the Litchfield area. The remaining 54 031 people live in remote communities. English may not the language of choice, and is nominated by only 66% as the only language spoken at home. Languages other than English spoken at home are Djambarrpuyngu (1.4%), Arrernte (1.4%), Greek (1.3%), Kriol (1.3%) and Warlpiri (1.2%)1.
The Royal Darwin Hospital (RDH) is in a unique situation as a centre for NT healthcare services, facing difficulties and challenges not encountered in other major Australian health centres. It is geographically isolated, being 318 km from the nearest district hospital at Katherine, 1502 km from the Alice Springs Base Hospital, and over 3000 km distant from other major metropolitan hospitals in adjoining state capitals2. Because of this isolation, the RDH is the major trauma centre for the majority of northern Australia, including NT and parts of northern Western Australia and north Queensland. As need arises, the RDH also provides emergency services to the South-East Asian region, with recent examples including the current civil war in East Timor, both Bali terrorist bombings and the Asian tsunami. The RDH is a recognised National Trauma Response Centre, with attendant responsibilities which include maintaining adequate response resources.
One unique strategy designed to assist in meeting these challenges and responsibilities was the implementation of the Radiographers Act permit system, also known as a Remote Operators (RO) License. The RO are GPs or district medical officers (DMOs) who attend RDH for a 2-4 week training program. At the end of this program the RO is permitted to take a restricted range of X-rays in their remote Aboriginal communities.
Remote Operators training program
The RO training program reduces social, emotional and system costs by diagnosing and treating patients, where possible, in their home communities, a high priority for many remotely settled Aboriginal people in the NT. Apart from reducing the emotional stress to patients and their families, the program also addresses the government expense involved in unnecessary patient transfers. Efficiency is also achieved by reducing the workload of the RDH Radiology Department staff.
During training, the doctors work with radiographers at the RDH Radiology Department and learn to perform a restricted range of radiographic examinations. After successfully completing an examination, the doctors are granted a limited NT Radiation Permit. Holders of the permit are permitted to undertake radiographic examinations in the community of patients' legs (from toe to knee), arms (from finger to elbow) and chests (CXR). Projections of the extremities may include AP and lateral, and oblique where relevant. Although CXR is taught in PA, AP and lateral projections, few RO have the equipment available to perform anything other than AP views. As a supplement to their training, and for reference when the training is complete, the doctors are given a copy of the 1981 Radiographic Procedures Manual3, prepared by the NT Radiographers Registration Board.
Issue
Rationale for review
While the RO must also be familiar with all relevant legislation, the two major components of the training are the practical education provided by RDH staff and the supply of the manual. The 89 page manual was written in 1981 and revised in 1984. It contains five sections relating to different aspects of radiography: (i) a general introduction; (ii) general radiation physics; (iii) radiographic equipment; (iv) working procedures and instructions; and (v) specific radiographic procedures.
Due to advances in health care, specifically in the arena of trauma and emergency management, senior radiology staff at RDH and previously trained RO recognised a need for this important document to be revised and updated. This article analyses the key factors and processes and activities involved.
Preparation for review
Interpretive perspectives are among the many points to consider when assessing a clinical education program, and the statements made about a specific educational activity are subject to evaluation and re-evaluation4,5. The essential questions used in reviewing this program and its manual, and the answers arrived at, included the following.
Is it necessary? Yes, this program is designed to reduce the health, financial, social, emotional and ill-health impact of patient travel in the NT. By implementing such programs, many patients are able to stay in their home community for diagnosis and treatment, and unnecessary travel is avoided.
Is it happening? Yes, since 1981 when the Radiographic Procedures Manual was first produced.
What is its purpose? To enable doctors to perform chest and extremity radiographic examinations in the remote Aboriginal communities where they are employed.
Are there any trends and quality issues? Yes there are. The number of doctors attending RDH for RO training is ad hoc and irregular, for reasons that include the high turnover of remote doctors. Many doctors in such communities are on a short-term contracts (usually for a 12 month period), so new doctors regularly attend for training on the radiographic equipment, procedures and protocols in the specific community. An associated trend identified is that the training program is reactive. This is time consuming and presents a risk for ineffective practice due to the issues inherent in the nature of this training and environment.
What are the political influences and associated governing bodies? The Radiographers Registration Board of the NT and its associated protocols directly influences the program. The RO are also bound by many different Acts and pieces of legislation, including the Radiographers Act 1976, Radiation Protection Act 2004 and the undated Radiation (Safety Control) Act. The Australian Radiation Protection and Nuclear Safety Agency (ARPANSA) Code of Practice (Radiation Protection in the Medical Applications of Ionizing Radiation) also bind the RO.
Are there any financial restraints for support? The initial training program is well supported with respect to finance and available training personnel. However, on completion of training, RO hands-on training opportunities cease due to staffing and budgetary constraints. The RO can, however, contact key professional practitioners at RDH for telephone or email support on an ad hoc basis.
Are there any accreditation issues? The program is recognised within the NT by the peak licensing body, the Radiographer Registration Board. Therefore, it is essential that directives and guidelines from the Board are closely followed.
What are the levels of support for those involved? As established, the level of support at initial training is strong. The program, however, would benefit from provision for further and ongoing training of the RO. There is an identified need for additional work-based and work-place professional development activities using resources and facilities available at the remote sites. This would also provide invaluable opportunities for mentoring and coaching.
Addressing the points identified by the analysis assured that the RO radiographic training program would improve and evolve to meet the current community healthcare and professional RO needs. The Radiographic Procedures Manual is a vital learning resource for use during the training period, and also a source of information beyond formal training. While the foremost objective was to improve the entire RO training program, the need to revise and update the Radiographic Procedures Manual was established early in the process.
The review process
Throughout the 3 years prior to reviewing the Radiographic Procedures Manual, both doctors undergoing RO training and their supervising radiographers had consistently complained that poor print quality of text and diagrams, and outdated content made this resource ineffective. A review by senior radiology staff, including the RDH Superintendent Radiographer, identified that this was a genuine problem and the decision was made to revise the manual. However the revision and editing of the Radiographic Procedures Manual was a much larger and lengthier process than was initially anticipated.
The first step was to obtain a current copy of the Radiographic Procedures Manual, which is archived as a PDF file of scanned images of the original typewritten document on the NT Government computer system. Once the document was obtained it was analysed by the first author of this article and several other senior radiographers. Their technical comments and suggestions for correction were considered and added to by a Charles Sturt University senior academic and co-author of this article [AJ]. The analysis revealed a number of issues:
- sections of the manual that had been left blank with the intention of adding information at a later date remained blank
- some of the information was outdated
- some of the information was incorrect
- diagrams and pictures were illegible
- diagrams and pictures taken from secondary sources were not referenced
- there was little in the way of further reading for continued education
- the manual's design was not aesthetically pleasing.
After the initial analysis, the process of editing and updating the document began. This involved extensive research of current literature, texts and the professional experience of professionals within the RDH Radiology Department. A copy of the Western Australian equivalent assisted in the development.
The revision is in progress and at the time of writing only the 'patient positioning' (specific radiographic procedures) section was finalised. This section was identified as least useful and most in need of attention by RO and RDH staff. Because it encompasses the practical aspects of the training, it is most likely to be used by the RO in their remote locations. Alterations and corrections to the other sections of the manual will be professional incorporated and the manual design improved to publication standard.
Challenges faced during the review process: The first of many challenges encountered during the revision of the Radiographic Procedures Manual was the enormity of the task. This professional document had not been updated for 13 years, requiring a careful revision of the entire text, with attention to detail and the accuracy of information presented in it.
Another difficulty was in contacting previously trained RO. As established earlier in this article, this was a highly mobile group and many had moved from addresses current at the time of training. Eventually the questionnaire was distributed to six previously trained RO's (eight doctors had attended training during the allotted time, however two were unable to be contacted) with an 83% return rate of those that were contacted.
The third challenge was the time requirement and coordination for those contributing to the review, all of whom were full time shift workers.
Finally, one of the most significant challenges during the process of the review was that, in this period, no doctor scheduled for RO training attended. Therefore, there were no ROs who could be involved directly in the review. Had an RO attended for training during the review process it would have enabled immediate feedback and also allowed the reviewers to implement any suggestions made by the ROs.
Results of review questionnaire
Once the need for revision had been established, evaluation of the Radiographic Procedures Manual and the current method of training was conducted through the use of a questionnaire titled 'Evaluation of Radiographic Procedures Manual' (which also covered course content) which was sent to the doctors who had undergone training since January 2005. This date was chosen as the cut-off point because tracking doctors who had previously undergone training would have been extremely difficult due to the mobility of these professionals.
Their degree of satisfaction with the manual and practical training was sought using eight relatively simple and self-explanatory questions with subsections relating to each component of the manual, and a general comments section. The questions concerned the:
- relevance of information
- correlation between theoretical and practical learning
- accuracy of information
- design and layout of the manual
- flow of information and order of topics
- clarity of diagrams, tables and images
- frequency of referral to the manual after completion of training
- practical aspects of the training.
Respondents were asked to answer each question from one to 10, with 10 being the highest and one the lowest level of satisfaction. Their responses are summarised (Tables 1, 2).
Table 1: Analysis of the remote operators' satisfaction questionnaire
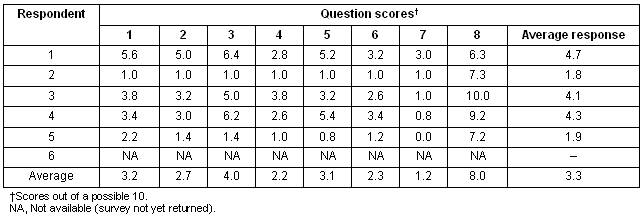
Table 2: Comments provided on the remote operators' satisfaction questionnaire

Lessons learned
The practical educational method employed at RDH combines many different supervisory techniques. This approach facilitates many radiographers contributing to the training of doctors.
The unique method of practical supervision combines both managerial and consultative supervision techniques, and also blends team and individual supervision techniques, as outlined by van Ooijen6. The combination of managerial and consultative supervision4 was in response to the different locations/communities in which the doctors' worked. The differences in radiographic equipment, processing capabilities and locations must then be considered. Also the fact that the RO's are located in their remote communities and their respective health organisations and the supervising radiographers are located at RDH meant that such supervision was required. However, as well as teaching, the supervising radiographers also have a reporting role. They must notify their manager (the superintendent radiographer) and professional authority (the radiographers' registration board) as to whether doctor trainees have satisfactorily met the training program's practical requirements. This double-barrel approach is believed, by the authors, to be the most effective way to teach all that is required in order to provide the RO with the most complete and rounded training and ongoing support in the short timeframe available. The amalgamation of team and individual supervisory techniques is complementary to this approach6; the doctors usually attend training individually but a team of radiographers is present to conduct the training and undertake the supervisory role. This comprehensive approach to training evolved due to the number of available radiographers and the many radiography procedures to be learned.
By working with a variety of radiographers, the doctors are exposed to many different approaches to the same issues, leading to the acquisition of a greater depth of knowledge and practical skills. This learning equips them to deal with the variety of patient issues they will face on return to their communities, many requiring lateral thinking and critical decision-making.
This approach to training also accommodates the shift rotations of supervising radiographers. If one is not available during the business hours training program, others will be. And exposure to a team of radiographers also ensures the development of a wide collegial network available to the RO for advice once they return to their remote communities. This essential aspect of the training program is part of a formative and developmental 'hidden curriculum'.
Reflection on the results (Tables 1, 2) reveals a strong positive response to the practical training (question 8) that was absent from the other questions (primarily related to the Radiographic Procedures Manual), indicating that the manual was a weak accompaniment to effective training. Strategies have been planned to ensure this situation does not reoccur after the manual is revised.
The RO who participated in the original review will be asked to rate the revised and redesigned manual using the same questionnaire. It is envisaged that RO comments will assist in further development of the manual. Extending this process of continuous improvement, all future RO trainees in the RDH program will be required to complete this or a revised questionnaire relating to their opinion of the new manual.
In this way it will be possible to provide future RO with a comprehensive learning experience supported by an up-to-date reference. This reference will subsequently become a valuable resource for their use in fulfilling their role and responsibilities relating to radiographic procedures performed in the rural and remote healthcare sector.
Recommendations
A final reflection on this process leads to a reminder to all in the remote healthcare sector about our professional obligation to ensure that policies, operational procedures, manuals and other procedural documents are up-dated on a regular basis.
Extending our experience to the larger sphere, a national system of RO training should be considered. Such a proposal highlights the current Australian situation where state radiographic bodies function independently of the Australian Institute of Radiography and of each other. Differing levels of competency and training required to perform radiographs impacts on a national training system for remote X-ray operators. International resources and directions from WHO may, in such a case, be instructive.
Conclusion
The revision and editing of the Radiographic Procedures Manual, as part of a larger training program review, has been a long, arduous and ongoing task. As a dynamic resource, its revision will and should be continuous. Future feedback from RO as they are trained, and from their supervising radiographers, will prompt continuous improvement.
By using the simple evaluation technique of the questionnaire, the RO feedback and evaluation has contributed to the development of the revised Radiographic Procedures Manual. The revision, as part of the training program evaluation, has been of benefit educationally and will result in a valuable resource for remote RO to underpin a vital training program, and to support them when they return to their communities.
Acknowledgements
The authors acknowledge the support given and contributions from the following people: the doctors who acknowledged the need for up-dating the manual and participated in the survey; Roger Weckert, the Superintendent Radiographer, RDH; Margaret Buba, James Bainbridge, Kim Hayward and Mark Palmer, Senior Radiographers at Royal Darwin Hospital, for their collegiality and contribution to the review process; the Radiographers Board of the Northern Territory.
References
1. Australian Bureau of Statistics. Regional Population Growth, Australia, 2005-06. (Online) 2007. Available: http://www.abs.gov.au/AUSSTATS/abs@.nsf/Lookup/3218.0Main%20Features122005-06?opendocument&tabname=Summary&prodno=3218.0&issue=2005-06&num=&view= (Accessed 29 June 2007).
2. Whereis.com. Directions. (Online) 2007. Available: http://www.whereis.com/whereis/directions.do (Accessed 29 June 2007).
3. Radiographer Registration Board. Radiographic Procedures Manual. Darwin, NT: Northern Territory Government, 1994.
4. Gardner R, Cairns J, Lawton D. Education for values: morals, ethics and citizenship in contemporary teaching. London: Kogan Page, 2000.
5. Jeeawody B. A transformative CPE model: critical perspectives and challenges. In: P Rushbrook (Ed.). Innovations in professional practice: influences and perspectives. Proceedings of the 2003 Continuing Professional Education Conference. 7-8 March, 2003; Bathurst, NSW, Australia. Centre for Research into professional Practice, Learning and Education, Charles Sturt University, 2003; 122-131.
6. van Ooijen E. Clinical supervision: a practical approach. Edinburgh: Churchill Livingstone, 2000; 56-60.
