Context
Pandemic A/H1N1/2009 virus
The pandemic A/H1N1/2009 virus has been described by Tang et al1, who also outlined the worldwide response. In the United Kingdom, in May 2009 the national strategy was to seek to contain outbreaks2. The UK had stockpiled the anti-viral drugs oseltamivir and zanamivir, as well as supplies of masks and other relevant equipment. All areas in National Health Service (NHS) Scotland had produced plans for management of an influenza outbreak. Stark et al2 have described initial lessons from an outbreak in the rural area of Cowal and Bute, Scotland. In this article a detailed case study of the Cowal and Bute outbreak is provided, and lessons are identified for other rural areas.
The area
Cowal and Bute is a predominantly rural area in the west of Scotland. The population of the Cowal peninsula is 15 000, and approximately 9000 of these live in the town of Dunoon. Access to the peninsula is by road or ferry. The island of Bute has a population of 7200, and 5000 of these live in Rothesay, which has the main ferry port for the island.
Health services in Cowal and Bute
Most health care in the United Kingdom is provided through the publicly funded NHS. The NHS in Scotland is provided in 14 geographic areas. The NHS Highland covers 41% of Scotland's land area but contains only 5% of the Scottish population. The area is sub-divided in to 4 geographic NHS operational units termed Community Health Partnerships (CHPs). The Argyll and Bute CHP is, in turn, divided in to localities, each of which has a locality manager.
The Cowal and Bute locality provides community services, including primary care. Primary care services are delivered through general practices, each of which is an independent business with its own staff, including GPs, practice nurses and reception staff. Other community services, such as community nursing, are provided by staff who are directly employed by the CHP. Out of working hours, the main service access is through NHS 24, a national telephone line which triages calls and can then offer advice, arrange a home visit by a doctor, direct the individual to a primary care emergency centre (PCEC) or, in an emergency, can arrange an ambulance to take the person to hospital.
The Cowal and Bute locality operates two community hospitals, Cowal Community Hospital in Dunoon, and the Victoria Hospital in Rothesay. District General Hospital services are provided by the neighbouring NHS Glasgow and Clyde, and patients from Cowal and Bute travel to access these in-patient services, although some out-patient services are delivered locally by visiting specialists. Cowal Community Hospital and the Victoria Hospital both have PCECs.
Public health services are provided from Inverness, which is approximately 4.5 hours by road from Dunoon. This includes services for health protection (Communicable Disease & Environmental Health), environmental health and communicable diseases. A national organisation, Health Protection Scotland (HPS), provides a national advice and guidance service, advises the Scottish Government, and works closely with the health protection teams in each NHS area. Infection control services are based in each CHP, and the Argyll and Bute CHP also has a public health specialist whose role is split between the Argyll and Bute CHP and a Highland-wide role within the Public Health Department in Inverness.
Issue
The outbreak
The duty Public Health Consultant for NHS Highland was informed by the West of Scotland Virus Reference Laboratory of two confirmed cases of pandemic A/H1N1/2009. A telephone interview with the two confirmed cases identified a number of people who met the definition of a close contact. The confirmed cases were offered a treatment dose of oseltamivir, and asymptomatic contacts were offered a prophylactic dose, in line with national policy at the time. The medicines were provided by the Out of Hours Service in Dunoon.
One set of contacts had travelled with the affected individuals on a football (soccer) supporters bus on the previous weekend. When telephone contact tracing was undertaken it became clear that a substantial proportion of individuals who had been on the supporters' bus, and some of who had subsequently spent time together in bars, were symptomatic. Further swabbing of symptomatic individuals and contact tracing identified a large number of cases. There was no evidence of links to overseas travel, so it appeared that the index cases had arisen from contact within the UK.
As identification of cases continued. There was a second wave of confirmed cases, mainly among household contacts of confirmed cases, although also in people with whom they had prolonged social or work contact. Figure 1 shows the dates of onset of confirmed cases.
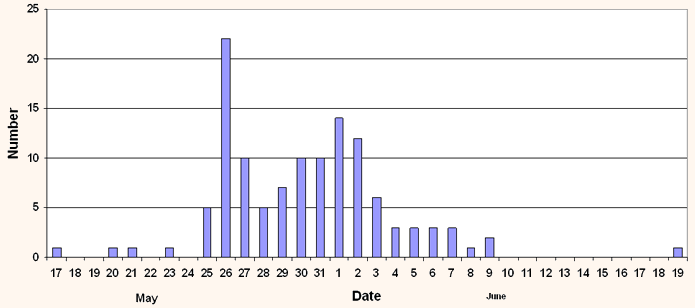
Figure 1: Dates of symptom onset in Cowal and Bute confirmed cases.
Where the cases identified were school children who had attended school while symptomatic, prophylaxis was offered to classmates. When a second case occurred in the same year in a secondary school, all the children in the year were excluded for one week from last contact with the symptomatic confirmed case in order to disrupt social transmission. When cases occurred in several years of a secondary school, the whole school was closed by the Education Department for the same 7 day period. In some cases, small primary schools consisted of only one room, and so the whole school was closed following one confirmed case.
Health Protection Scotland, the national health protection organisation, concluded that there was evidence of sustained community transmission, and that anyone in the area with compatible clinical symptoms should be treated as a possible case. After the second, smaller, peak of contacts of the initial cases, the number of new cases fell rapidly, despite widespread virological testing of individuals with viral symptoms in the area (Figure 2) shows the number of viral swab results, and the proportion that were positive for pandemic A/H1N1/2009, by day. When testing symptomatic contacts of confirmed cases, a high proportion were positive but this fell rapidly as local services started to test anyone in the area with compatible symptoms. This suggests that pandemic A/H1N1/2009 was only one of a number of viral strains circulating in the community.
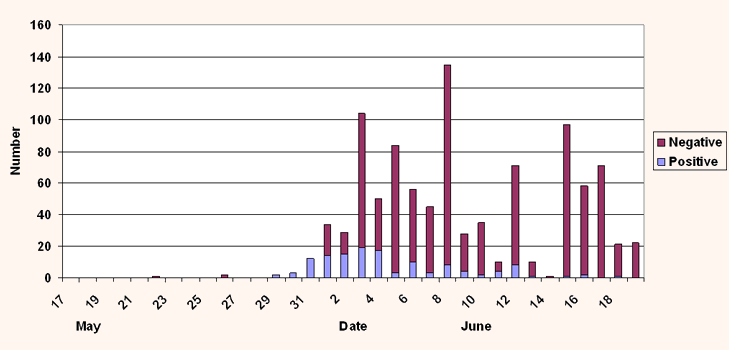
Figure 2: Swab results received according to day.
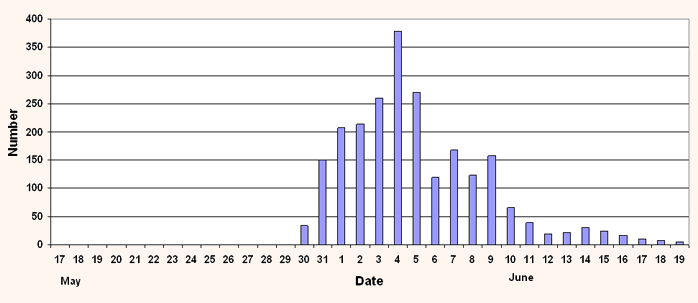
Figure 3: Attendances at treatment centres in Dunoon and Rothesay.
Service response
Over the first weekend of the outbreak, GPs employed as part of the Out of Hours Service in the locality visited symptomatic contacts to undertake swabbing and provide anti-viral medication where indicated. Telephone contact tracing was conducted from Public Health in Inverness. The local service hoped that the larger number of staff rostered for routine duties during the week would allow services to cope with increased demand. It became clear, however, that the volume of contacts, particularly school contacts, was such that this could not be sustained. With the national advice that anyone in the area with compatible symptoms should be treated as a case, the volume of symptomatic individuals needing to be seen also increased substantially (Figure 3).
As a result the locality manager decided to open an anti-viral distribution and swabbing centre at the Cowal Community Hospital. It proved possible to separate symptomatic and asymptomatic individuals, although this added to the complexity of the service rotas. A patient group directive (PGD) was applied, which allowed designated staff, such as nurses, to dispense medication to individuals who met the terms of the directive. This reduced the need for medical staff, although as the PGD excluded children under 1 year of age, medical availability was still required on each shift, both for children and to help with any other medication queries that arose. In addition, the availability of a clinical pharmacist was indispensible, particularly in the early days of the outbreak when clinical staff were less familiar with the situation.
A second cluster of cases linked to the first cases developed on the adjacent Isle of Bute and it proved necessary to open an antiviral distribution centre on the island. Symptomatic cases were seen at the local health centre where they could be segregated from other patients, and asymptomatic cases on Bute were seen at the community hospital. Opening hours were initially 0900-2100 h but these were reduced as the volume of people presenting reduced.
The telephone helpline NHS 24 used to access out of hours services was provided with an appropriate algorithm, and was then able to direct people to the service when it opened the following day, thus reducing the need for out of hours work.
The Argyll and Bute CHP treated the outbreak as a major incident, and invoked its Major Incident Plan. The Cowal and Bute locality created an incident room at each anti-viral centre. These incident rooms were managed by the equivalent of a clinical service manager. This person, with administrative support, took responsibility for liaison with area and regional services where required, for collation of information, and for resolving any immediate problems that arose in the course of a shift. A CHP incident management team was created, in line with the Major Incident Plan. This was made up of the locality manager, the CHP head nurse, the CHP infection control nurse, and the CHP public health specialist. Daily teleconferences were held with Public Health in Inverness to ensure consistency of response, and to address any issues that were identified that day.
Public health response
There were several layers of public health response. The main public health resource was with the extended Public Health team in Inverness. There was a major demand for information, advice and decision-making. The volume of contact tracing was far greater than for normal communicable disease and environmental decision-making, and a shift system was created with staff brought in from other parts of the organisation to undertake tasks that could be delegated. Information handling capacity was essential.
The volume of clinical queries increased rapidly, and capacity had to be provided to answer clinical queries. It was more efficient to do this by noting requests at a central switchboard, and responding to queries in batches.
A system was created at the NHS offices in Inverness, with a shift manager; shift clinical lead; database operator, clinical query responders and contact tracers. The shift clinical lead briefed the contact tracers and liaised with the clinical query responders (usually doctors) to reply to questions from clinicians or from the public. The shift manager ensured that the whole system functioned efficiently, and resolved any issues that arose during their shift. The database operator worked with the shift manager to keep records up to date, and to produce lists that allowed actions to be checked. The shift manager proved to be a key role for keeping the system operating effectively. Shift managers ensured a clear hand-over at each shift, and contributed to twice-daily staff briefings. Daily briefings were also held for senior NHS managers.
Daily teleconferences were held with Health Protection Scotland, and figures were provided to contribute to national figures. The daily conferences allowed sharing of experience across the country, and allowed the experience in Cowal to contribute the revision of national guidelines and, through the Health Protection Scotland links with the Health Protection Agency in England and Wales, to UK policy and practice.
Lessons learned
Use of existing plans
There has been a recent focus on planning for bioterrorism, and some suggestion that rural areas may be less prepared3,4. Some rural areas report a focus on major incidents on staff training, reflecting the common responses needed across different types of incident5. Advance planning for major communicable disease incidents is essential but hospital plans in some countries vary widely in quality6-8. Community staff also play a key role in the recognition and management of incidents9. All CHPs in the NHS Highland area have pre-existing Major Incident Plans, and Pandemic Influenza Plans.
The Major Incident Plans follow a set format and include consideration of when to identify a major incident. These are generic plans intended to allow adaptation to events varying from a communicable disease outbreak to a major accident. The rapid identification of this influenza outbreak as a major incident defined it as an organisational priority, and allowed resources to be drawn from other areas of work. All areas have undertaken tabletop exercises in the last year, and this helps to identify local changes required4.
For sporadic cases, the response was intended to be by home visits by GPs in order to keep symptomatic people separate from asymptomatic people in waiting rooms and public transport. At a later stage, a national 'Flu Telephone Helpline' would be activated. The national plan envisaged individuals dialling in to this line, being triaged and then directed to appropriate services. If anti-viral drugs were required, the individual would be allocated a unique identifying number and directed to an anti-viral distribution centre to collect their anti-viral drugs.
National policy was for containment in order to slow spread. There was no expectation that the spread of the virus could be stopped in Scotland; however, slowing the spread in order to allow preparation time, and to spread demand, was seen as valuable. The main problem for NHS Highland was that this relatively isolated rural area was the first part of Scotland to have a significant number of cases. The Scottish Government, understandably, did not choose to initiate a national anti-viral distribution system and associated centres for one rural area. This meant that NHS Highland had to create a local system in response to local circumstance that would function in the absence of a nationally available system. Using established major incident procedures, within the framework of the Pandemic Influenza Plans, allowed rapid decision-making and service response.
Changes to emergency planning arrangements
The incident had an enormous impact on the ability of the organisation to carry out its routine work. Manley and colleagues10 suggest that consideration of surge capacity and preparedness across rural healthcare organisations is essential. Our experience supports this, but in practice it was extremely difficult to move staff from one area to another because of distance, and because of the expectation that the outbreak could spread to neighbouring areas, resulting in a reluctance to shed staff who may be needed urgently. Including 'surge capacity' and support from other areas in plans and exercises will be useful for future planning.
Staff in Dunoon and Rothesay were able to apply lessons learned in generic training and emergency planning exercises to this incident, emphasising the importance of investing in local staff11. Hoard12 has argued that disaster preparedness in rural areas, including hospital surge capacity, could be usefully modelled using simulation software, and this is something that could be integrated in to future exercises.
Integrated working
By UK standards, NHS Highland covers a large, sparsely populated area, and local resilience is therefore particularly important13. The main public health staff resource in Inverness is distant from the site of this outbreak. The CHP headquarters are in Lochgilphead, which is itself some distance from Cowal and Bute. Bute is separate from Cowal, and requires a ferry journey for access. The laboratory services are in Glasgow, operated by a different NHS area. Argyll and Bute Council Education Department, based in Lochgilphead, is in charge of schools. The effect of this was to produce considerable potential for confusion.
The NHS Highland overcame this by identifying clearly the role of each part of the system, and by ensuring regular liaison and co-ordination. Operational issues, including supplies, were dealt with by the CHP Incident Management Team. The local Incident Management Team had a daily telephone conference with the Public Health team in Inverness. Decision-making at the anti-viral distribution centres was delegated to the shift manager, who was authorised to make any relevant operational decisions. Liaison with the Education Department in Argyll and Bute Council was, for policy decisions, via Public Health and again done at least once per day.
Health Protection Scotland (HPS) had daily telephone conferences with the NHS Highland Public Health team, who then liaised with the operational services in Dunoon and Rothesay. In turn, HPS had a daily teleconference with all Scottish NHS areas which allowed them to share lessons across Scotland. This provided a direct, daily route to share lessons from the site of the outbreak to Scotland as a whole, and also allowed direct contact for Highland with the officials responsible for decision-making on Scottish policy. This integrated working - at national, regional and local level - was essential to minimise the opportunity for confusion, and to allow real time national learning.
Conclusions
The NHS Highland is a relatively small NHS organisation with a widely distributed staff. Despite this, it was able to respond rapidly to the first significant outbreak of pandemic A/H1N1/2009 in Scotland, and to contain the local outbreak. The main lessons from the outbreak were that the appropriate place to make an operational decision was as close to the patient as possible, and that clear differentiation of staff roles in different parts of the organisation was essential.
Local staff were empowered, through existing major incident procedures, to take the steps necessary to move staff and other resource to the places required to respond to the incident. Local knowledge was essential14, and the experience that Dunoon-based staff brought to the incident was invaluable. Contact tracing, tracking of patients and results, and liaison with national organisations, were conducted by staff geographically removed from the incident.
The NHS Highland staff are used to working by telephone and videconference, and these arrangements proved to be robust even in the face of substantial pressure caused by an evolving incident. Daily liaison between staff in NHS Highland, and with national services, produced a coherent response that would not have been possible if different organisational priorities had emerged. The authors conclude that rural health services are best able to respond to major incidents by drawing on their existing plans, and by using the pre-existing expertise of their local operational staff combined with appropriate specialist support.
Acknowledgements
The authors are grateful to Eric Baijal, Susan Birse, Martin Donaghy, Pip Farman, Roger Gibbins, Sara Huc, Elaine Mead, Christine McIntosh, Lorraine McKee, Derek MacRae, Sheila Ogilvie, Robbie Paterson, Virginia Paul-Ebohimhen, Ken Proctor, Colin Ramsay, Viv Smith, Helen Tissington, Dennis Tracey, Pat Tyrell and to all the staff who so willingly undertook contact tracing, anti-viral provision and other work in relation to this outbreak.
References
1. Tang JW, Shetty N, Lam TT. Features of the new pandemic influenza A/H1N1/2009 virus: virology, epidemiology, clinical and public health aspects. Current Opinions in Pulmonary Medicine 2010, 16(3): 235 - 241.
2. Stark C, Tissington H, Ogilvie S, Tyrrell P, Smith V, Oates K. Swine flu in rural Scotland - containment phase. Rural and Remote Health 9: 1249. (Online) 2009. Available: www.rrh.org.au (Accessed 5 July 2010).
3. Dobalian A, Tsao JC, Putzer GJ, Menendez SM. Improving rural community preparedness for the chronic health consequences of bioterrorism and other public health emergencies. Journal of Public Health Management and Practice 2007; 13(5): 476-480.
4. Edwards JC, Kang J, Silenas R. Promoting regional disaster preparedness among rural hospitals. Journal of Rural Health 2008; 24(3): 321-325.
5. Furbee PM, Coben JH, Smyth SK, Manley WG, Summers DE, Sanddal ND et al. Realities of rural emergency medical services disaster preparedness. Prehospital Disaster Medicine 2006; 21(2): 64-70.
6. Adini B, Goldberg A, Laor D, Cohen R, Bar-Dayan Y. Factors that may influence the preparation of standards of procedures for dealing with mass-casualty incidents. Prehospital Disaster Medicine 2007; 22(3): 175-180.
7. Graham J, Shirm S, Liggin R, Aitken ME, Dick R. Mass-casualty events at schools: a national preparedness survey. Pediatrics 2006; 117(1): e8-15.
8. Hsu CE, Mas FS, Jacobson H, Papenfuss R, Nkhoma ET, Zoretic J. Assessing the readiness and training needs of non-urban physicians in public health emergency and response. Disaster Management and Response 2005; 3(4): 106-111.
9. Williams JC. State of emergency preparedness of Kentucky's rural public health workforce: assessing its ability to identify community health problems. Public Health Report 2008; 123(2): 178-188.
10. Manley WG, Furbee PM, Coben JH, Smyth SK, Summers DE, Althouse RC et al. Realities of disaster preparedness in rural hospitals. Disaster Management and Response 2006; 4(3): 80-87.
11. Heideman M, Hawley SR. Preparedness for allied health professionals: risk communication training in a rural state. Journal of Allied Health 2007; 36(2): 72-76.
12. Hoard M, Homer J, Manley W, Furbee P, Haque A, Helmkamp J. Systems modeling in support of evidence-based disaster planning for rural areas. International Journal of Hygiene and Environmental Health 2005; 208(1-2): 117-125.
13. Gilbert M. Bridging the gap: building local resilience and competencies in remote communities. Prehospital Disaster Medicine 2008; 23(4): 297-300.
14. Akins RB, Williams JR, Silenas R, Edwards JC. The role of public health nurses in bioterrorism preparedness. Disaster Management and Response 2005; 3(4): 98-105.
Abstract
Context: Pandemic Influenza (A/H1N1/2009) caused worldwide concern because of its potential to spread rapidly in human populations. In Scotland, Government policy had been to seek to contain the spread of the virus for as long as possible in order to allow time for service preparations, and for vaccine development and supply.
Issue: The first major Scottish outbreak of pandemic A/H1N1/2009 was in the rural area of Cowal and Bute. After two initial cases were identified, contact tracing found a cluster of cases associated with a football supporters' bus. Within 3 weeks, 130 cases had been identified in the area. Rapid provision of treatment doses of anti-viral medication to cases and prophylactic treatment of asymptomatic close contacts, advice on self-isolation and, where required, interruption of transmission by temporary school closure, were successful in containing the outbreak.
Lessons learned: Pre-existing Major Incident and Pandemic Flu plans were used and adapted to the particular circumstances of the outbreak and the area. Supporting operational decision-making as close to the cases as possible allowed for speed and flexibility of response. Contact tracing and tracking of cases and results was performed by specialist public health staff who were geographically removed from the cases. This was possible because of effective use of existing telephone conferencing facilities, clarity of roles, and frequent communication among staff working on all areas of the response. Basing the work on established plans, staff experience of rural areas and rural service provision was successful.
Key words: disaster planning, disease outbreaks, emergency preparedness, influenza A virus A/H1N1/2009, mass casualty incidents, public health, rural health services, rural hospitals.




