Cervical screening programs have been introduced in many countries and are generally regarded as the most appropriate and effective method currently available for preventing cervical cancer1,2. Cervical screening leads to significant improvements in health outcomes that can be expressed in life years gained, and generally are more cost-effective than other screening strategies3-8. The effectiveness of community-oriented primary-care programs in countries with well-developed general practice/family medicine and primary care is well documented. Effective health education programs are known to be the most helpful intervention to augment the participation rate in and compliance with screening programs among women2,9,10.
There is an absence of a national screening program in Greece and some effective community-based interventions have been reported11-13. The guidelines by the European consensus on cancer screening recommended that Pap smears should be used for cervical screening among a core age group of women aged 30-60, and that the screening interval should be 3 to 5 years14,15. Although some rural practitioners, in most cases district midwives, have undertaken activities with the aim of increasing uptake, there are still few published data on the effectiveness of community oriented cervical screening programs in Greece13,16. While there are several promising approaches regarding recruiting strategies in cervical screening programs, in rural areas of Crete there is still room for improvement13. This study reports on the effectiveness of a health education meeting in recruiting women for a cervical screening program in a primary-care setting in rural Crete.
Methods
Setting
The discussion meeting took place in an open state centre for elderly citizens' members (Kentro Anoiktis Prostasias Ilikiomenon [KAPI]). The KAPI is located in the small town of Rethymno in Crete, a Greek Mediterranean island. Rethymnon has a population of 20 000 permanent residents. The screening program was implemented at the Spili Health Centre (SHC). The SHC and its five regional surgeries are responsible for the health care of a rural population of approximately 9000 residents who live in 26 small villages in the mountains of Rethymnon, a distance of 30 km from the town.
Participants
Sixteen women currently registered as members of KAPI participated in the educational discussion meeting. The KAPI members are retired citizens, who take part in different group entertainment activities (eg daily tea and coffee meetings in the KAPI venue, art activities, choirs, playing musical instruments, theatre, hand-made art, sporting activities, organised trips for pleasure).
Theoretical model
The theoretical model underpinning the development of this intervention is based on 'social learning theory'17,18 . The learning process, according to social learning theory, takes place in a social context through observation of the actions of others (eg a lay woman who participates in a cancer screening program). As a result of the strong relationships within a community, this observation may lead to modelling and imitation of a particular behaviour (eg participation in a cervical screening program)2. The dynamics of a social group in remote areas may have a more positive effect on human behaviour. As in epidemiology, 'binding' relations between the women and 'cluster' phenomenon within the community, after the educational intervention has taken place, may be observed.
Description of the health education intervention
At this centre for the elderly, an educational discussion meeting was organised with women in order to promote cervical screening. The small group discussion meeting took place at the seminar room of the KAPI building where the women usually met for KAPI team activities. At the beginning of the meeting a brochure was given to the participants. Two community midwives (VV and TR), staff of the SHC, gave a 30 min lecture which was based on specific questions (Fig 1) and followed the problem based learning model19,20. The attending staff participated in the process by answering questions posed and formulating more specific questions. The participants in the discussion meeting who had been screened before for cervical cancer (62.5%: n = 10) were encouraged to answer and comment on the questions that were put by the participants who had not been screened previously (37.5%: n = 6). The key messages of this health education discussion were that cervical screening reduces the risk of developing cervical cancer and, moreover, due to cervical screening cervical cancer is now an uncommon disease in many countries. The key messages are shown (Fig 2).

Figure 1: Questions posed at the educational discussion meeting.
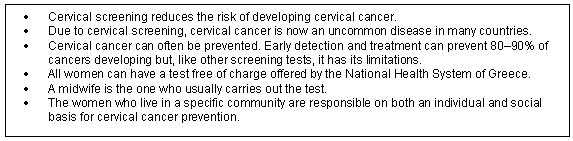
Figure 2: Key messages conveyed during the educational discussion meeting.
An active discussion between the participants of the educational meeting and the two midwives followed. The emphasis was on individual and social responsibility regarding cervical cancer. The women who participated in the educational discussion meeting were invited to organise a group visit to the SHC within the next 15 days, in order to be screened together as a team.
Ethical considerations
Although cervical screening services were well established in the SHC, the participants were asked to provide oral consent when the cervical smear results were given.
Results
Participants in the educational discussion meeting (Group A)
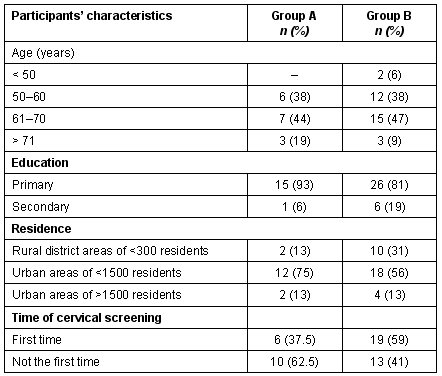
There were 79 women members of KAPI. A total number of 16 women participated in the educational discussion meeting (Group A). The descriptive characteristics of the women who attended the interactive meeting are illustrated (Table 1). The majority (43.8%) of these women were between 61 and 70 years of age, and approximately 37.5% were between 50 and 60 years old. Fifteen of 16 women (93.8%) who participated in the education discussion meeting had only primary education. Six women (37.5%) had not been screened previously for cervical cancer.
Table 1: Descriptive characteristics of the participants in the educational discussion meeting (Group A) and the 32 women who did not participate in the educational discussion meeting but participated in the cervical screening 15 days later (Group B)
Participants in the cervical screening program
A total number of 48 women (mean age = 62 years), including all the participants of the discussion meeting, visited the SHC 15 days after the educational discussion meeting had taken place (Fig 3).
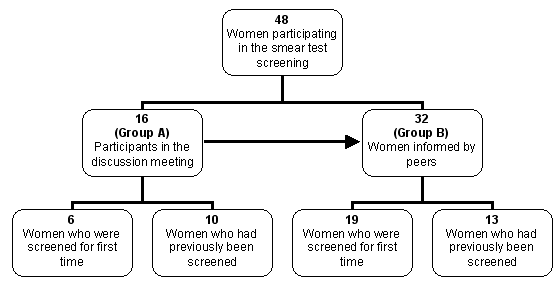
Figure 3: The breakdown of participants in the Cretan cervical screening study.
The descriptive characteristics of women who did not attend the educational discussion meeting and who later participated in the cervical screening (Group B) are shown (Table 1). Of Group B members, 46.9% (n = 15) were between 61 and 70 years of age. Moreover (31.3%, n = 10) were living in a rural district area that had a population of less than 300 inhabitants. Of Group B members, 26 out of 32 (81.3%) had only primary education. While the age of Group B women of was over 50 years of age, the majority of this group (59.4%: n = 19) underwent cervical screening for the first time.
Discussion
While information (given in educational sessions, by flyers, posters or in other ways) is obviously a useful first step, factors such as the influence of peers21-24, attitudes, motivation, wider social influences, as well as practical skills development, are considered important factors in changing behaviour2,25-27. Moreover, it has been suggested that educational intervention workshops (which are based on problem solving), as well as small group discussion sessions that use innovative methods and are led by peer educators, can also be effective in changing behaviour2,28-30. It is important that educational interventions are guided by sound theoretical constructs2,31.
The main finding of this study was the high compliance rate of the women who participated in the educational discussion meeting (Group A) and the augmented action of the health education program, which was effective in recruiting all the initial participants in the educational discussion meeting. Group A women who made an important contribution to the success of the initiative, were not selected for particular attributes and it is not known whether they were the most articulate or persuasive in their peer group. No formal leaders were included in Group A and it is not known whether there were any informal leaders. However, these laywomen were part of a group (KAPI)with specific common characteristics and potentially had personal relationships with their peers. In their capacity as key messengers, the women of Group A were able to convince the women of Group B (members of the same team, KAPI) to participate as KAPI team members for the first time in a screening program for cervical cancer, rather than as individuals.
The recruits (Group B) were all members of KAPI. The researchers did not supervise nor interfere during the process of recruitment. As a result, it is not possible to measure the actual number of women who were approached but did not come for a Pap smear, or the number of women who did not participate in the screening program because they had already undergone cervical screening. However, it appears that the health education message was transmitted effectively among peers, since Group B is larger than Group A.
The study approached women with a mean age of 62 years. This cohort falls outside the peak ages for cervical cancer, therefore representing a low risk population. However, 26 of these women (52%) had never been screened for cervical cancer previously. Many factors have been associated with difficulties in recruiting older women. These include low awareness, low or even lack of education and lower cognitive status scores32. Although all the recruits were members of an open centre for the elderly, there is no evidence that younger women would behave differently; however, this recruitment strategy needs further research.
Factors that may augment the power of the message transmission should be further discussed, as should the potential mechanisms and the concept of contact. The type of contact in our study resembles that experienced by people who live in the same house during a period of infection. As Halloran explains, in epidemiological terms the transmission probability depends on characteristics of the infective source ('problem based learning lecture'), the parasite ('the health education message'), the susceptible host ('the participants') and the type and definition of the contact ('the educational discussion meeting')33. The understanding and definition of risk differs among epidemiologists, clinicians, and lay people34. In epidemiology, risk expresses a statistical association between a characteristic and a disease in a defined population. The lay perspective corresponds with the 'subjectivist' interpretation of probability, reflecting the context and our expectations and observations of events24,35.
Group behaviour and the dynamics of rural Greece may mean that the sample of women in our study were likely to have a more positive attitude to this community activity than other sections of the population. This may explain the high recruitment rate. The concept of social responsibility regarding cervical cancer, and encouraging women to recommend cervical screening to their peers needs further research to determine whether it is possible to use a similar approach in other traditional communities.
We are aware of the methodological limitations of the study. The small number of participants and the highly selective nature of the sample may affect external validity of the study and preclude generalization of our results. There is, moreover, some evidence that the population of rural Crete is still homogenous and has its own particular expression on values, culture and beliefs36-37. Despite these limitations, this study has explored the suitability and appropriateness of a health education meeting in recruiting women for a cervical screening program in a primary-care setting in rural Crete.
Conclusions
Despite the exploratory nature of this study and its methodological limitations it is suggested that the approach taken in this study may be an inexpensive and effective technique for increasing uptake of cervical screening in traditional societies where the rate of cervical screening is still low. Such an approach may have an effect on the early detection of cervical cancer, contributing to a reduction of morbidity. Although our study describes an innovative approach to recruiting rural women in Crete, further research is needed before these findings can be translated into guidance for policy makers and practitioners.
Acknowledgement
The authors would like to express their gratitude to Professor Sarah Davies for linguistic assistance and her important comments.
References
1. Munoz N, Bosch FX. The causal link between HPV and cervical cancer and its implications for prevention of cervical cancer. Bulletin of the Pan American Health Organization 1996; 30: 362-377.
2. Shepherd J, Weston R, Peersman G, Napuli IZ. Interventions for encouraging sexual lifestyles and behaviours intended to prevent cervical cancer. The Cochrane Database of Systematic Reviews, 1999.
3. Goldie SJ, Kuhn L, Denny L, Pollack A, Wright TC. Policy analysis of cervical cancer screening strategies in low-resource settings: clinical benefits and cost-effectiveness. JAMA 2001; 285: 3107-3115.
4. Brown AD, Garber AM. Cost-effectiveness of 3 methods to enhance the sensitivity of Papanicolau testing. JAMA 1999; 281: 347-353.
5. Sato S, Matsunaga G, Tsuji I, Yajima A, Sasaki H. Determining the cost-effectiveness of mass screening for cervical cancer using common analytic models. Acta Cytologica 1999; 43: 1006-1014.
6. Matsunaga G, Tsuji I, Sato S, Fukao A, Hisamichi S, Yajima A. Cost-effective analysis of mass screening for cervical cancer in Japan. Journal of Epidemiology 1997; 7: 135-141.
7. Waugh N, Robertson A. Costs and benefits of cervical screening. Is it worthwhile reducing the screening interval from 5 to 3 years? Cytopathology 1996; 7: 241-248.
8. Gyrd-Hansen D, Holund B, Andersen P. A cost-effectiveness analysis of cervical cancer screening: health policy implications. Health Policy 1995; 34: 35-51.
9. Cancer Research Campaign. Cancer of the Cervix Uteri. London: Cancer Research Campaign, 1994.
10. Cancer Research Campaign. Cervical Cancer Screening. London: Cancer Research Campaign, 1994.
11. WHO Regional Office of Europe. Highlights on Health in Greece. Copenhagen: WHO, 1997.
12. Riza E, Kyriakogianni-Psaropoulou P, Koumantakis E, Symiakaki H, Garas I, Linos A. Cervical cancer screening in Greece. European Journal of Cancer 2000; 36: 2227-2232.
13. Romanidou T, Konsolaki M, Giotaki J, Karpeta N, Frantzeskakis G, Sasarolis S, Lionis C. Analysis of the abnormal cervical smears in a community-based screening programme and the compliance behaviour in women with abnormal test. Primary Health Care 1996; 8: 97-105.
14. Advisory Committee on Cancer Prevention. Recommendations on cancer screening in the European Union. European Journal of Cancer 2000; 36: 1473-1478.
15. Patncik J. European consensus on cancer screening should be applied urgently by health ministers. BMJ 2001; 323: 396.
16. Anttila A, Ronco G, Arbyn M et al. Cervical cancer screening programmes and policies in 18 European countries. British Journal of Cancer 2004; 91: 935-941.
17. Bandura A, Ross D, Ross S. Vicarious reinforcement and imitative learning. Journal of Abnormal and Social Psychology 1963; 67: 601-607.
18. Bandura A. Perceived self-efficacy in the exercise of control over AIDS infection. Evaluation and program planning 1990; 13: 9-17.
19. Bouhuijs P, Schmidt H, Van Berkel H. Problem-based learning as an Educational Strategy. Maastricht: Network of Community-Oriented Educational Institutions for Health Sciences, 1993.
20. Schmidt HG. Problem-based learning: rationale and description. Medical Education 1983; 17: 11-16.
21. Eng E, Parker E, Halrlan C. Lay health advisor intervention strategies: A continuum from natural paraprofessional helping. Health Education and Behaviour 1997; 249: 414-417.
22. Eng E. Natural helping functions of lay health advisors in breast cancer education. British Cancer Treatment 1995; 35: 23-29.
23. Eng E. The Save our Sisters Project. A social network strategy for reaching rural black women Cancer 1993; 72: 1071-1077.
24. Salber E. The lay advisor as a community health resource. Journal of Health Politics Policy Law 1979; 249: 413-417.
25. Bhave G, Lindan CP, Hudes ES et al. Impact of an intervention on HIV, sexually transmitted diseases, and condom use among sex workers in Bombay, India. AIDS 1995; 9: 21-30.
26. Corby NH, Wolitski RJ. Condom use with main and other sex partners among high-risk women: Intervention outcomes and correlates of reduced risk. Drugs and Society 1996; 9: 75-96.
27. DiClemente RJ, Wingood GM. A randomized controlled trial of an HIV sexual risk-reduction intervention for young African-American women. JAMA 1995; 274: 1271-1276.
28. Hobfoll S, Jackson AP, Lavin J, Britton PJ, Shepherd JB. Reducing inner-city women's AIDS risk activities: a study of single, pregnant women. Health Psychology 1994; 13: 397-403.
29. Kelly JA, Murphy DA, Washington CD et al. The effects of HIV/AIDS intervention groups for high-risk women in urban clinics. American journal of public health 1994; 84: 1918-1922.
30. St Lawrence J, Eldridge GD, Shelby MC, Little CE, Brasfield TL, O'Bannon RE III. HIV risk reduction for incarcerated women: a comparison of brief interventions based on two theoretical models. Journal of Consulting and Clinical Psychology 1997; 65: 504-509.
31. Barratt A, Trevena L, Davey H, Mc Caffery K. Use of decision aids to support informed choices about screening. BMJ 2004; 329: 507-510.
32. Wu ZH, Black SA, Markides KS. Prevalence and associated factors of cancer screening: why are so many older Mexican American women never screened? Preventive Medicine 2001; 33: 268-73.
33. Halloran E. Concepts of Infectious Disease Epidemiology. In: KJ Rothman, S Greenland (Eds). Modern epidemiology. Lippincott Williams and Wilkins, 1996; 529-554.
34. Edwards A, Pill R, Stott N. Communicating risk. BMJ 1996; 313: 1483.
35. Prior L, Bunton R, Nettleton S, Burrows R. Chance and modernity: accidents as a public health problem. In: L Prior, R Bunton, S Nettleton, R Burrows (Eds). The sociology of health promotion. London: Routledge, 1995: 133-144.
36. Smak Gregoor J. The District Ag. Vasiliou: A description of the health care and a sociographic profile of the population. Doctoral Research Report, School of Social and Cultural Studies, Leiden University. June 1990.
37. van de Kerk R. Blood is thicker than water. The role of the illness-management group towards the patient in the village Sellia, Crete. Doctoral Research Report, School of Social and Cultural Studies, Leiden University. June 1993.
Abstract
Introduction: Cervical screening programs have been introduced in many countries and are generally regarded as the most appropriate and effective method currently available for preventing cervical cancer. Although action has been undertaken by some rural practitioners, especially by district midwives, there are still few published data on the effectiveness of community-oriented cervical screening programs in Greece. Objective: To explore an innovative approach in a primary-care setting in rural Crete. This study reports on the effectiveness of a health education meeting in recruiting women for a cervical screening program.
Methods: At a centre for the elderly, 16 women participated in an educational discussion meeting organised to promote cervical screening. The women who participated in the discussion meeting were invited to organise a group visit to a rural primary healthcare centre, in order to be screened as a team during the following 15 days. The theoretical model underpinning the development of this intervention was based on the 'social learning theory'. Emphasis was placed up individual and social responsibility regarding cervical cancer.
Results: A total number of 48 women (average age 62 years) including all those who participated in the educational discussion meeting, visited the Spili Health Center, Crete, 15 days after the discussion meeting. The main finding was the high compliance rate of the women who participated in the educational discussion meeting, resulting in recruiting all the initial participants. Moreover, the lay women who participated in the small group discussion meeting, in the capacity of key messengers convinced an additional 32 women to participate in a screening program for cervical cancer as members of a team, rather than individually. The majority (52.1%, n = 25 out of 48) of the women had not been previously screened for cervical cancer.
Conclusions: Health education is an important factor in the process of health promotion, and health professionals should consider the dynamics of a specific group in order to carry out their work effectively. Awareness of the special characteristics of an individual as a member of a defined group can contribute to increasing the motivation for participation in health programs as a member of that group. It is suggested that more educational programs take place in rural Crete in order to augment the compliance rate of women in cervical screening programs.
Key words: cervical cancer screening, community, discussion meeting, health education, women's health.
You might also be interested in:
2007 - Disease mongers in a nation in transition?
2006 - Home medication reviews: what do people in the Australian Riverland think of them?



