Context
Mongolia
Since the 1990s, Mongolia (population 2.6 million) has undergone rapid social and economic transitions. Prior to this period, the government obtained significant external funding from the former Soviet Union. In the 1980s and 1990s, the nation had developed an impressive network of health facilities and professionals, extending from centralized tertiary institutions to primary care facilities. However, since transition to the free market economic system and the withdrawal of Soviet state subsides there have been increased financial pressures on the Mongolian economic and social sectors, particularly in rural areas. In the peak transition period between 1990 and 1994 real incomes collapsed, unemployment rose sharply and quality of life deteriorated. Widening income inequalities and little progress in poverty reduction were associated with the transition1.
Mongolia is divided into 22 administrative units, including 21 provinces or aimags and Ulaanbaatar. The aimags consist of 331 soums or rural towns (population 5000-10 000), which are further divided into 15550 baghs (migratory family groups). The capital city is divided into 9 districts and 121 sub-districts or khoroos.
Urban areas: There has been rapid migration to the urban areas of the national capital Ulaanbaatar. The main reasons for this are social sector decline in rural areas, and the potential for employment opportunities in urban areas. Currently, 60% of the total population lives in urban areas2. Associated with social sector decline and the opening of free economic markets, there have also been changes in patterns of migration, and labor policy and practices.
In a national study completed in 2003, an estimated 10.2% (n = 68 580) of children aged 5-17 years were classified as part of an 'economically active child population'. Of this economically active group, 65% (n = 38 857) meet the ILO Convention definition of child laborer3. It has been estimated that 6148 children are employed as domestics workers in 6 Ulaanbaatar districts, and one-third of these have not completed schooling4.
During planning exercises conducted as part of this study, city officials reported that up to 67% of the capital's population now lives in a 'ger district' (characterized by 'ger' or traditional Mongolian housing on free land). Many of these residents are recent migrants, and up to 20% are not registered for social welfare benefits, and so are excluded from access to social health insurance benefits. Additionally, primary healthcare facilities (family group practices in the city and soum hospitals in rural areas) are not financed to track and care for unregistered populations.
Rural and remote areas: Recent developments in the economic sector have led to new patterns of internal migration in rural areas, partially responsible for the development of informal mining sites and child labor, school drop outs and homelessness. It has been estimated that nationwide 45 902 people over the age of 5 years are engaged in informal gold and fluorspar mining, and that 17.4 % of these are children aged 5-17 years5.
Maintaining Mongolian healthcare services for traditional rural herding families has always been a challenge for system planners and managers. However, until recently an extensive network of soum hospitals in small service towns, and the placement of a primary care worker in the traditional Mongolian herdsmen family group have ensured very high coverage rates for preventive services such as immunization and MCH care. The recent social and economic transitions have compromised this.
The Ministry of Health (MOH) has undertaken significant reforms in recent years in response to the challenges of the social transition. A decentralized health planning system has been developed, incorporating annual program review, objective setting, and activity planning linked to costing, monitoring and evaluation systems6. In 1999, although operating the majority of public health facilities, the government privatized previously salaried family doctors. These family doctors established family group practices (FGPs). Each 'registered' population member means there is payment of a risk adjusted capitation fee from government capitation. The capitation method (applied also in rural areas) involves a formula that allocates funding on the basis of risk-adjusted capitation, 20% on assets costs, 10% on distance-related costs and 5% on a performance-related cost7.
However, despite these system innovations, concern is still expressed by the MOH and its development partners that the significant mobile and socially vulnerable sub-population is not reached by the health system. For instance, measles incidence, although low in absolute numbers on a regional basis, is higher than in many other western-Pacific countries, according to WHO (41.8 per 1 000 000 population)8. An information system data quality audit self-assessment conducted in 2006 found a higher measles disease burden than was anticipated, based on reported immunization coverage9. There is also heightened awareness of the risk of current or emerging communicable diseases. An outbreak of enterovirus 71 (hand, foot and mouth disease) in June 2008 resulted in the diagnosis of 2163 people, 83% of whom were children below the age of 10 years10.
Given the pace of social change, concerns about the quality of coverage data, and the persistence of communicable diseases, the MOH and its international partners sought to strengthen micro-planning systems in order to detect and reach more difficult to access populations in Mongolia. This article describes and analyses the 'Reaching Every District strategy' (RED) planning processes, and highlights lessons learned for use in planning development in Mongolia and elsewhere. The planning design, activity and guidelines (including authorship of this article) were prepared by national and district planners and advisers directly involved in the development and trial of the micro-planning process.
Intervention
The reaching every district strategy
Internationally, RED is intended to address common obstacles to increasing immunization coverage; the obstacles include inadequate district planning, inadequate and unreliable services and monitoring and supervision of health workers. The five international RED operational components include the following:
- linking services with communities
- re-establishing outreach vaccination services
- supportive supervision
- monitoring and use of data for action
- planning and management of resources.
Since 2003, 53 developing countries (mostly in Africa and Asia) have commenced implementation of RED11. One evaluation and one other published study have demonstrated that the strategy can improve access to services and particularly to immunization12.
Sources of data and steps in micro-planning
Four main activities were undertaken in order to develop a national strategy and micro-planning process to detect and difficult to reach populations:
- A literature review of the RED internationally
- Conducting a strategic planning workshop at central level, with the participation of national and district planners
- Testing and development of micro-planning methodology in Byanzurkh District, Ulaanbaatar
- Presentation of the district micro-plan to national-level planners for analysis and feed back.
Data from each step of the planning process (Fig1) were entered into a single planning sheet and integrated (from step 2 target population to step 6 costing of district management and supervision). Data were then aggregated by district (in a district-wide map and planning tool). This planning tool is supplementary to written RED guidelines developed as part of the initial RED13. The primary sources of data used in the lessons learned section of this article were: (i) planning data entered into the planning templates; (ii) authors' participant observation in micro-planning workshops (as planners, facilitators and advisers); (iii) the RED guidelines developed as a result of the planning process; and (iv) the District Micro-plan presented at the national forum.

Figure 1: Steps in reaching every district strategy planning in Mongolia.
Study area and target population
The study area of Byanzurkh District consists of a population of 272 000, of whom 52 000 are not registered for health or social security benefits. This unregistered status is related to a range of factors including community attitude, health provider capacity to reach the populations, and lack of adequate health finance coverage. The district is divided into 21 urban khoroo and rural soum. The khoroo is further subdivided into neighborhood areas or sections in the urban area. The equivalent of this in the rural area is the bagh (cluster of family groups or ger). The planning process demonstrated that the district has a very rapid rate of internal migration. District officials reported during the planning process that 100 000 people had moved into the district in the past 3 years. Byanzurkh is considered a 'ger district' with over 90% of the population residing in ger accommodation (transient mobile traditional housing).
In terms of health system infrastructure, each khoroo in the urban area has an FGP, and in Byanzurkh District these FGPs are staffed by doctors, nurses and interns. A package of primary care services is provided by each FGP, supported by a national capitation based funding system. A typical FGP (eg Andsaikhan FGP) has a population of 17 850 people, consisting of those from 11 sections in a service radius of 5-8 km.
Nationally, the target population for RED planning was classified by national and district planners into the following categories:
- Category 1, or 'mobile populations', referring to migrants and temporary residents, herders, travelling business families and informal miners
- Category 2, or 'remote area populations', referring to traditional ethnic groups, migrating herder populations, remote households in soums in the furthest areas and people living in the mountains
- Category 3 or 'vulnerable populations', referring to homeless people, populations resident on waste sites, orphaned and disabled people, the very poor, working children, and populations with limited education
- Category 4 or 'unregistered populations' referring to those living on the peripheries of Ulaanbaatar city and in rural and remote locations and who do not have official registration with civil registration and social welfare offices.
These target populations were re-analyzed at district and FGP level during the study (and are further described, particularly in Figure 3, which defines target population at FGP level). Because Byanzurkh is on the edge of Ulaanbaatar City, target populations relate to all four categories.
Reaching every district strategic components and main activities
The National level RED planning meeting commenced with an analysis of the 'strategic components' of RED, as adapted to the conditions in Mongolia. Following a review of the international RED concepts, national planners (with district representatives) articulated the strategic components adapted to Mongolia in greater detail.
The emphasis on community involvement encouraged local area planners to identify strategies to access difficult to reach populations by forming of service delivery partnerships with local authorities and social welfare agencies, including:
- collaboration with governors at all levels, including social workers in governors' offices
- liaison with state and non-government organizations (NGOs)
- conducting outreach services to migrants and other vulnerable groups with the aid of international organizations, the state and NGOs
- collaboration and exchange of information on location and registration of unreached population governors (through governors' offices, health facilities, civil registration, social welfare institutions, and police).
At national and district level, concepts and styles of supportive supervision were discussed, with FGP practitioners requested by district leaders to identify successful components of district supportive supervision.
In terms of re-establishment of outreach services, district planners were also able to identify at-risk target groups and map and strategize ways to reach them. Specific activities to support re-establishment of outreach services included mapping problem areas, conducting surveys, implementing mobile health services for remote areas, conducting health education and mobilizing volunteers.
Finally, in terms of data analysis and planning and management, the district and FGPs were able to map areas of low coverage, undertake barrier analysis, and cost in detail the activities required to reach these populations. Proposals were also put forward for establishing more integrated information networks and the analysis of monthly reports. Amendments to existing FGP service contracts were also recommended, in order to provide additional incentives for health staff to access the most difficult to reach populations.
Three modes of service delivery were identified in the micro-planning sessions: (i) fixed strategy (increased use of health facilities); (ii) health outreach; and (iii) mobile services (access to the most remote populations). Additional activities planned for the FGPs and the district consistent with overall RED components included: in-depth health and demographic surveys; registration of difficult to reach populations (in collaboration with social welfare departments and local authorities); public health education; additional transport to access the hard to reach; and increased funding for human resources.
Barrier analysis
During the national strategic planning meeting, participants were invited by the district facilitator to analyse determinants of low health service access according to specific population, health system and immunization program factors. These were recorded on planning templates.
Although the barriers aligned well at FGP and national level, the FGPs were able to describe in more detail the system barriers to health service performance. System barriers at the local level specifically related to:
- lack of human resource motivation due to insufficient staff
- under-financing of health care by up to 20% through the capitation based health funding system due to high levels of unregistered populations
- infrastructure barriers to population health, including poor road access for remote areas and poor water and sanitation.
Mapping the difficult to reach
Participants at three levels of the health system were requested to bring to the RED planning meetings maps of catchment areas, and relevant immunization, MCH and demographic data. During the planning, participants were asked to chart geographic and topographic features, and the target difficult to access populations and, where possible, to record these on the map in numbers (Fig2).
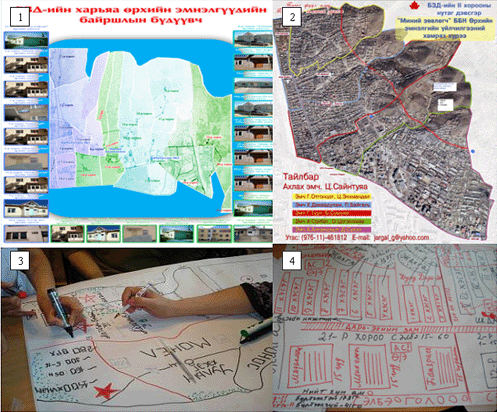
Figure 2: Pictorial and hand drawn maps of catchment areas indentifying difficult to reach populations, used in the Byanzurkh District, Ulaanbataar Reaching Every District strategy, Mongolia 2008. Image 3: family group practice (FGP) practitioners chart missed populations in high risk areas of their catchment. Image 4: another FGP maps sections, watercourses and dumpsites (top left of picture with arrows) where difficult-to-reach populations are concentrated. Image 2: one FGP used aerial mapping. The two dots represent the distance between two water sources. Mountainous areas in the centre right of the picture indicate remote population areas on the edges of Ulaanbaatar. Image 1: FGP maps were integrated into a district-wide view of the difficult to reach, with 'red areas' indicating locations of high risk populations.
At the primary care level, significant detail was recorded on maps, reflecting participants' in depth knowledge of local area topography and demographic and service accessibility patterns.
Participants were then asked to present their findings to the wider audience. During these presentations FGP practitioners and managers demonstrated their local knowledge and expertise. The clarity and confidence of the presentations indicated how visualization of data can be an effective means of realistically reflecting local health situations. Based on the presentation of FGP maps, the district integrated the local area maps into a district-wide picture of difficult to access populations (Fig2).
Identifying the target population and the package of services
In Khoroo 21, the total estimated difficult to reach population was estimated to be 4932 or 27.6% of the population. The categories of difficult to reach as defined at one FGP are provided (Fig3). The total unregistered population is 4150 or 23.2% of the total population. The living areas of these populations were reported by FGP practitioners to be dumpsites, beside waterways and over the hills around the periphery of Ulaanbaatar. In these areas there are limited road access points, water and sanitation facilities. It can take FGP practitioners up to 2 hours on foot to reach some of these communities.
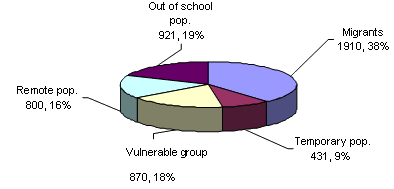
Figure 3: Target population as defined by family group practice practitioners Khoroo 21, Byanzurkh district.
District wide, 52 000 (19.1%) of the total population of 272 000 is unregistered, reflecting the high rate of internal migration into Ulaanbaatar from rural areas, the high level of unmet need and, consequently, the strain this places on existing FGP practices. These populations mostly live in newly established ger areas, the three biggest markets of the city, in areas where student dormitories or child care centers are located and in locations with extremely under-developed infrastructure. The issue of poor infrastructure, particularly for water and sanitation, was a recurring theme in the FGP plan presentations.
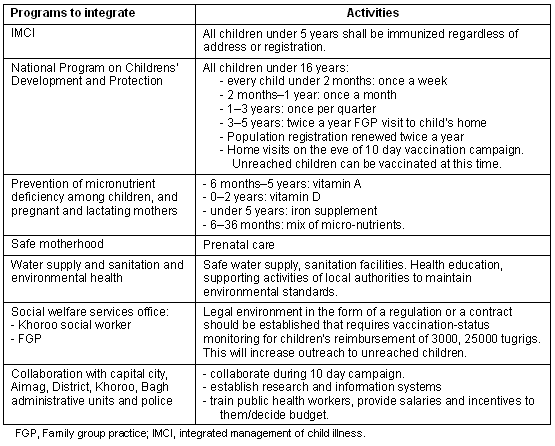
On the basis of these findings, FGP practitioners recommended additions to the package of services to be provided through the RED, which is inclusive of MCH services, environmental health and water and sanitation. In recognition of the local area social determinants of health, the package defines community and cross-sector collaborations (ie social welfare and local authorities) as also being an essential component of the essential service package (Table 1).
Table 1: Package of services of the Reaching Every District strategy, Mongolia
Monitoring, evaluating and sustaining the planning process
As part of RED development, concepts of supportive supervision were introduced nationally and at the district level. Supportive supervision was defined during planning consultations as a process that promotes quality at all levels of the health system by:
- focusing on solving problems
- helping to improve allocation of resources
- promoting high standards
- improving team work and two-way communication.
On the basis of these definitions and values and their applicability to the Mongolian setting, a supervision strategy was devised (including a checklist) that incorporated many of the elements of local problem solving, on-site training, local community partnerships and a system for data quality auditing.
Planners reached consensus that RED micro-planning activities and budgets should be requested through normal annual operational planning and budgeting cycles in order to sustain the program. The RED is therefore not a separate project, but is an operational approach to implementation of the priority Health Sector Master Plan Strategy through the annual operational planning system. The operational strategy could be financed from both national and international sources.
Lessons learned
Mapping and barrier analysis
The barrier analysis and mapping process of the RED trial in Mongolia demonstrates clearly how problem-solving approaches can be catalytic in creating opportunities for health planning and health service improvement. The classifications of barrier analysis into population, system and immunization factors were quickly grasped by participants and used effectively to analyse problems in a comprehensive social and health system analysis. This comprehensive rather than program-specific analysis clearly opened wider planning opportunities. It was also a contributing factor to planners deciding on a MCH package of services for RED planning, as well as making the strategic decision to link the health and social sectors in order to outreach unregistered populations.
Data mapping was also critical in generating problem-solving analysis. The keen participation in mapping, the ease with which local area experts were able to identify risk factors, target groups and locations were all generated by visual mapping of data, either using computer graphics or manually drawing catchments areas. These maps are also effective for the presentation of data to planning forums. As has been demonstrated in other settings14, mapping can be a highly effective tool for giving confidence to local planners through recognition of local area knowledge and expertise in potentially addressing the national issue of lack of accessibility to healthcare services.
When local-area and district maps were presented to the forum of national decision-makers, one manager remarked that it was like 'looking in the mirror'. Another remarked that the local mapping and data presentation was an awakening for national decision-makers who often see the world 'only from office windows'. Bringing health data alive using analytic and problem-solving tools such as barrier analysis and data mapping gives local area planners the confidence to express local needs to high-level planners; and high-level policy-makers are given the capacity to base national planning strategies on the reality of local epidemiological and environmental conditions.
Micro-planning process and management style
Changing the style and approach to planning requires a change in the style of and approach to management. In Mongolia, traditional centralized planning has placed the focus on the related management style of 'inspection' as the principal method of supervision. The management style of inspection can conflict with decentralized or local-area management style, where the main principle at work is an assumption of the expertise in local-area knowledge. This local-area knowledge was expressed in the Mongolia planning trial in answers to the following questions:
- Where are at risk populations?
- What are their risks?
- At what time of year are they most exposed to risk?
- Who are the key local actors who can make a difference in reaching these populations?
As only local-area planners have the knowledge and skill to answer these questions, the role of the 'inspector' from afar correcting local problems through direct on-site instruction loses its management effect. In a decentralized environment the 'supportive' supervisor assists local-area managers and planners to problem solve issues that have local-area answers (rather than those centrally directed), backed by technical advice from the upper-level manager.
The RED planners from Mongolia were quick to recognise themes of 'supportive supervision'15. District planners created lively discussion among FGP practitioners by asking what they expected from their managers in terms of a supervision visit. The discussion demonstrated the level of openness and flexibility in current Mongolian government and society. Although up to 20% of the population are living in conditions of poverty and limited access to social services, the system is sufficiently flexible to permit open advocacy at both local and senior decision-making level for the change in management and planning practice and style necessary to meet these unmet needs. This demonstrated the close links between a micro-planning process and the reorientation of management style.
Wider applications of the reaching every district strategy for health system strengthening
Internationally, RED is identified in WHO member states as a strategy to achieving the goal of at least 80% immunization coverage in all districts, and 90% nationally. However, in the Mongolian trial, planners included a wider MCH services package (rather than a sole immunization focus) in order to be consistent with the national health-sector plan and the defined health system's essential services package. An additional rationale for adopting the wider health system focus for RED is that the determinants of low immunization coverage (distance, level of education and poverty) are the same as those for low access to maternal and other child care services. Planners determined that the principal barriers to immunization and MCH performance were health system and population barriers, rather than always immunization program specific.
In conclusion, the main success factors in the development of the planning methodology were the use of barrier analysis and mapping approaches for data analysis and problem solving at the local level, and a reorientation of management approaches from 'inspection' to supportive supervision. Additionally, although the RED is intended internationally as an immunization-specific intervention, evidence from the development and trial of the process in Mongolia indicates its potential for wider health system applications. This is particularly so in relation to the use of the strategy to detect and respond to the MCH service needs of more difficult to reach sub-population groups.
Acknowledgements
The development of this program was facilitated through the Regional Office of UNICEF, Bangkok Thailand (Ms Diana Chang Blanc) and the National Centre for Communicable Diseases, Ministry of Health, Mongolia, with technical support from the country offices of UNICEF and the World Health Organization. Funding was through the Global Alliance for Vaccines and Immunization.
References
1. Government of Mongolia. UNDP Human Development Report. Ulaanbaatar: Government of Mongolia, 2003.
2. UNICEF. Situation analysis of children and women in Mongolia. Ulaanbaatar: UNICEF, 2007.
3. National Statistics Office Mongolia. Report on National Child Labour Survey. Ulaanbaatar: National Statistics Office Mongolia, 2004.
4. Population Teaching and Research Centre. National State University Baseliner Survey on Child Domestic Workers in Mongolia. Ulaanbaatar: Population Teaching and Research Centre, 2005.
5. Population Teaching and Research Centre. National State University Baseliner Survey on Child Domestic Workers and Adult Workers in Informal Gold and Fluorspar Mining. Ulaanbaatar: Population Teaching and Research Centre, 2005.
6. Ministry of Health. Mongolia Health Sector Master Plan 2006-2015. Ulaanbaatar: Mongolia Ministry of Health, 2006.
7. Hindle D, Khulan B. New payment model for rural health services in Mongolia. Rural and Remote Health 6: 434. (Online) 2006. Available: www.rrh.org.au (Accessed 2 April 2009).
8. WHO WPRO. Measles bulletin; issue 14, November 2007. (Online) 2008. Available: www.wpro.who.int/NR/rdonlyres/AED0A592-219C-4C48-996D-B81D6CE5C66D/0/MeasBulletinIssue14.pdf (Accessed 11 July 2008).
9. NCCD/WHO. Data quality audit self-assessment. Ulaanbataar: WHO, 2006.
10. International Federation of the RED Cross Mongolia. Hand, foot and mouth disease. (Online) 2008. Available: http://www.ifrc.org/docs/appeals/08/MDRMN001.pdf (Accessed 11 July 2008).
11. WHO. Reaching Every District (RED) approach: a way to improve immunization performance. Bulletin of the World Health Organisation 2008; 86: 3.
12. WHO, USAID, CDC, UNICEF. Reaching Every District strategy Implementation in the Africa Region Evaluation Report. Geneva: WHO, 2005.
13. Mongolian Ministry of Health/UNICEF. Reaching Every District Guidelines. Ulaanbaatar: Mongolia MOH/UNICEF, 2008.
14. Soeung S, Grundy J, Ly CK, Samnang C, Boreland M, Brooks A et al. Improving immunization coverage through budgeted micro-plans and sub-national performance agreements: early experience from Cambodia'. Asia Pacific Journal of Public Health 2006; 18(1): 29-38.
15. WHO/PATH. Guidelines for supportive supervision. Geneva: WHO, 2004.

