Introduction
The nurse shortage in the USA is expected to intensify from 12% in 2010 to a projected 29% in 20201. The expectation is especially troubling for small rural hospitals which were among the first to feel the impact of the nursing shortage2,3. Rural nurse recruitment is more difficult during 'an unprecedented shortage of qualified nurses' because rural sites have always had trouble recruiting staff for lower pay and generalized practice in small communities with few resources4. Critical access hospitals identify filling nurse vacancies as their number one concern5.
Approximately 20% of the US population resides in 'health professions shortage areas'. Specifically, 35 of 39 counties in Washington are designated as health professional shortage areas6. Four-fifths of Montana and two-thirds of Oregon have the classification of medically underserved, while 90% of Idaho is designated as a health professions shortage area7. The shortage areas struggle not only to recruit but also to retain their health professionals.
Rural literature describes physician characteristics in order to develop recruiting programs but fails to describe rural nurse characteristics8-11. The literature also describes successful work environments and the need for innovative programs12-14. Authors Tierney15 and Aiken, Clarke and Sloane16 suggest learning more about rural nurse characteristics and their work environment preferences in order to retain and recruit the needed workforce.
Examining rural nurses characteristics may help universities/nursing programs identify and recruit students who are more likely to join the rural nursing workforce. For example, Bushy and Leipert17 found that nursing students in both the US and Canada were more likely to opt for rural practice post-graduation if they had life experiences and connections in small communities. Similarly, an evaluation study of the Clinical Placement Support Scheme at Queensland University of Technology in Australia indicated that final year Bachelor of Nursing students were more likely to choose a rural clinical placement if they possessed rural background, worked previously in a rural community, and/or had financial or family commitments18.
Most nursing workforce studies occur in urban settings due to the availability of larger sample sizes. The lack of rural studies is problematic because rural nursing is recognized as a different type of practice19. Rural theorists suggest urban study results may not be appropriate for rural practice. The aim of this study is to describe the job satisfaction, lifestyles and community preferences of rural hospital nurses in the Northwest region of the USA.
Literature review
The sparseness of rural studies found in the literature is partly due to small sample sizes in hospitals where the total nursing staff may range from 5 to 30. The few rural nursing studies with larger samples report an older and less educated employee than those in urban studies20. Studies also report lower ratios of registered nurses to licensed practical nurses, and fewer bachelor's degrees20. Rural hospitals also report possessing fewer professional and technological resources for patient care21.
Rural nursing differs from urban nursing in another way. The rural patient's health issues differ from those in urban populations. Rural residents suffer from more chronic disease and more occupational health issues22. The population is more elderly and obese, has less healthcare insurance, and purchases more expensive medications. Rural theory states residents define health functionally and seek care later than urban residents, meaning nurses must practice more crisis management. These trends alter the type of healthcare strategies provided in rural hospitals.
Administrators try to attract new graduates to small hospitals. Rural practice offers outdoor lifestyles, a chance to meet neighbors and friends, early middle-management career opportunities, and assignment variety17,23. The challenges occur when the few available graduates learn of lower salaries and a lack of sign-on bonuses than offered in urban centers24 In addition, the shortage of spousal employment opportunities and lack of cultural opportunities hampers recruitment away from urban centers22,17. Smaller hospitals also suffer from the high cost of turnover because small facilities generally have fewer financial resources than larger ones.
Powers24 reports that recruiting nurses for turnover positions may cost as much as 3 million dollars in a medium-sized hospital. Patient outcomes are also impacted when the turnover rate exceeds 22%. In addition, the patient length of stay increases by 1.2 days24. Nurse retention is known to increase staff education levels, improve quality of care, improve patient safety rates and reduce organizational costs9. Nurse recruitment and retention impact the health of rural hospitals and populations.
Retaining rural nurses may be a challenge due to stressors not identified in the nursing literature19. For example, the generalist practice role is misunderstood. The rural nurse generalist role requires advanced skills most new graduates do not possess25. Rural generalists perform crisis assessment and management skills for populations across the lifespan and for all health conditions. A rural nurse may manage traumas, calm the mentally ill, stabilize the critically ill, deliver emergency births, care for children and comfort the dying within the same shift. Retention may be difficult because employers sometimes hold unrealistic expectations of new nurses due to rural practice needs. Because basic education programs often lack generalist principles, graduates are unprepared for their responsibilities26.
New graduates in rural hospitals are expected to possess advanced critical thinking as well as cross-discipline assessment and intervention skills20,27. Longer orientation and specialty training are required to develop the generalist skills, and yet small hospitals lack the finances, personnel, technology and time to provide new employees with the additional training required28. The high job stress levels nurses report are thought to impact on the high job turnover rates29,30. Discerning what factors mediate stress is important to prevent a worsening of the nurse shortage.
Even if hospitals were to hire enough new graduates, the shortage would continue because most nursing school students are older and entering nursing as a second career. The exodus of new graduates in addition to the retirement of experienced nurses is expected to deepen the nurse shortage problem31,32. Within the next 5-10 years the profession will lose its most experienced, educated, satisfied and committed nurses31,33.
During times of nurse shortage, the importance of job satisfaction becomes critical. Because job satisfaction is related to turnover rates, a large body of literature explores the concept. Ingersoll and associates report that satisfaction is related to the nurse's educational level33. Associate degree graduates (this US term is equivalent to Canadian graduates holding a diploma) were more dissatisfied with employment than higher educated peers. In the Western region of the USA, most rural nurses are associate degree graduates. Another study compared graduates from technical and university programs34 and reported that technically trained nurses were significantly more satisfied with their workload and professional support. Technical graduates also reported dissatisfaction with their on the job training and opportunities for further education. There are no comparative US rural studies.
Job satisfaction: Job satisfaction was first studied in 1940 by Nahm with an increasing number of studies occurring during shortage periods35. Nurse job satisfaction is defined as the difference between the amount of rewards received and the amount nurses believe they should receive. Job satisfaction is studied as both an independent and dependent variable.
As an independent variable, job satisfaction is recognized as the cause of burnout, absenteeism, turnover, and retention. The results of studies using job satisfaction as an independent variable indicate that poor job satisfaction may increase the nurse shortage36. Some argue that in rural areas with few nurses, job dissatisfaction can actually threaten a hospital's existence37.
As a dependent variable, job satisfaction is associated with factors such as individual and organizational characteristics or job mechanics35. Moreover, Fletcher38 contends that psychological burnout appears to cause lower job satisfaction and not vice versa. On the other hand, other authors argue that job satisfaction has both direct and indirect influences on burnout and leaving employment. For example, Golembiewski and Munzenrider39 and Kalliath and Morris40 found job satisfaction has a direct negative effect on emotional exhaustion, whereas emotional exhaustion has a direct effect on depersonalization. An indirect effect of job satisfaction on depersonalization via exhaustion was found, confirming its role as a predictor of burnout40. Overall, prior research demonstrates that nurse burnout experiences are common41.
The literature also considers job stressors and relationships with job satisfaction. Hays and associates42 found the most frequent stressors in an intensive care unit were staff shortages, apathetic/ incompetent nursing, responsibility/decision making, critical/ unstable patients, and unnecessary prolongation of life. The study indicates organizational characteristics were more stressful than professional challenges. Another study in Canada demonstrated that nurses' job satisfaction was affected by a combination of individual, workplace, and community characteristics43. The four most important of these interrelated predictors were availability of up-to-date equipment and supplies, satisfaction with scheduling and shifts, low level of psychological job demands, and home community satisfaction.
Research by Mills and Blaesing44 report urban nurses were more satisfied with nursing as a career than their rural counterparts. Furthermore, Ma, Samuels, and Alexander35 found that two-thirds of the RNs surveyed reported their job satisfaction remained the same or had lessened in the past 2 years. Their findings also indicate job satisfaction is dependent on organizational factors such as job position, hospital retirement plan, and geographic area. Increased nurse-to-patient ratios lead to job dissatisfaction and burnout that intensify the turnover and vacancy rates.
Readers need to carefully analyze how researchers are using 'job satisfaction' so as not to compare apples with oranges. Table 1 describes how researchers use job satisfaction as both an independent and dependent variable. In this study the concept is used to examine the intention to remain employed by measuring individual and organizational characteristics (job satisfaction as a dependent variable).
Table 1: Job satisfaction as a research variable

Work commitment: Tourangeau and Cranley45 found the strongest predictors of job commitment of nurses in urban hospitals were nurse age, overall nurse job satisfaction and years of employment in the current hospital. Other statistically significant determinants of nurse intention to remain in a job include: job satisfaction, personal characteristics, work group cohesion and collaboration, and organizational commitment. In a mixed urban-rural study nurses were highly dissatisfied with the work culture45. Other studies report organizational environment and educational factors affect job satisfaction, organizational commitment, and plans for continuing as a nurse3. Moreover, nurses who report higher levels of job satisfaction also report a greater likelihood of remaining at their current institution45.
Research about retention of new graduate nurses in rural Australia revealed similar findings46. Specifically, workplace cultural issues, workload and level of responsibilities influenced new graduates decisions to stay within the rural nursing workforce. Also, nurses providing maternity services in rural areas of Canada identified affordable and accessible continuing professional education as the most important factor for recruiting and retaining rural nurses47.
The North-western region of the USA has only recently begun collecting information about rural nurse characteristics. The literature lacks information about rural nurse job satisfaction, work commitment, lifestyles and community preferences. A study of rural nurses in several hospitals was undertaken as part of a Health Resource Services Administration funded program to increase nurse recruitment and retention.
Methods
The conceptual framework for this study is based on the Penn Nursing Outcome Model16. The Penn model identifies both individual and work characteristics as important to job retention. This study used a cross-sectional design to identify the individual, work, and geographic factors impacting on nursing job satisfaction. The study was approved for human subjects by the university institutional review board.
Instruments
Three instruments, including two open-ended questions, were placed in two online survey formats. The authors created a demographic survey which was reviewed by experts, piloted, and then placed online. The survey included questions on personal preferences about work, community, lifestyles and practice confidence. The second survey contained the McCloskey/Mueller Satisfaction Scale (MMSS) and the Gerber Control Over Practice Scale (GCOPS). The online format permitted anonymous participation from many rural hospitals.
After human subject approval, 103 nurses with at least one year of experience in a rural hospital completed the two online surveys. The MMSS is used extensively in research and practice to measure job satisfaction but was originally developed to rank the rewards that encourage nurses to stay employed43,48. The MMSS49,50 has 8 subscales of nurse satisfaction. Cronbach alphas for each subscale were obtained and are as follows: satisfaction with extrinsic rewards (.65), scheduling (.76), family/work balance (.58), co-workers (.65), interaction opportunities (.78), professional opportunities (.80), praise and recognition (.82), and control and responsibility (.80). The instrument measures nurse job satisfaction, with an overall alpha of .89. Participants were asked to indicate their level of satisfaction with 32 aspects of their job using a 7 point scale, where 1 = least and 7 = most satisfaction with salary, vacation, benefit package, work schedule, supervisors, peers, physicians, responsibility etc.
The GCOPS has 21 items with responses ranging from strongly agree to strongly disagree on a 7 point scale. Each statement begins with 'As a nurse I am free to...'. This scale is traditionally scored as a single factor scale with an overall alpha of .96. The alphas for the subscales were: skillful/team member (.91), clinical leadership (.86), and evaluation (.81).
At the end of the survey, respondents were asked to describe their most satisfying and least satisfying aspects of work. Responses reflected on some of the same aspects mentioned in the MMSS.
Results
In the demographics survey, participants were asked to indicate how important 16 community and lifestyle factors were to them in choosing a practice. Response categories ranged from 1 = not important to 5 = important. Nurses reporting high satisfaction levels also reported a rural life background. Tables 2 and 3 provide ratings of personal and organizational characteristics.
Table 2: Ratings of community/lifestyle factors
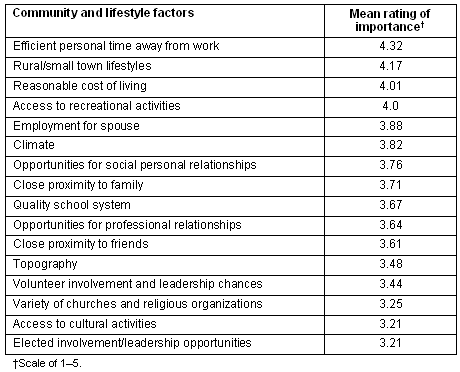
Table 3: Ratings of organizational characteristics
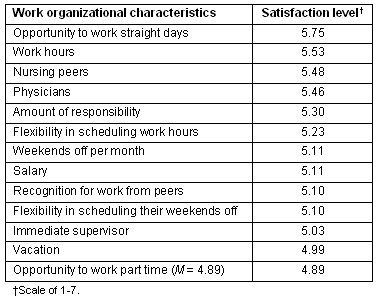
Answers to the satisfaction scale questions were compared with participant responses to the two open-ended questions, because ratings alone do not describe reasoning. Nurses' responses to the MMSS and GCOPS questions indicate nurses were somewhat satisfied with organizational aspects of their job.
Responses to the open-ended responses indicate most satisfied with interactions with staff and patients, work schedule/hours, autonomy, skills, small facility, work variety, the amount of responsibility with the job, and positive feelings about their jobs. At the same time, MMSS and GCOP responses indicate nurses were less satisfied with compensation for working weekends (M = 4.68), control over work conditions (M = 4.63), recognition for their work from superiors (M = 4.56), for career advancement opportunities (M = 4.48), participation in organizational decision making (M = 4.37). amount of encouragement and positive feedback (M = 3.81), and benefit packages (M = 3.53).
Analysis of the open-ended responses reinforced the survey findings. Nurses were least satisfied with staff interactions, work schedules, amount of responsibility, salary, and benefits. Although the majority of nurses intended to remain employed, those who planned to leave employment were unmarried, without children, and reported no preference for rural life. Narrative responses indicated some organizational factors (eg staff interactions, work schedule, and the amount of responsibility given) were mentioned as both the most and least satisfying aspects of the job.
A further examination of the responses provides some clarity to the seeming contradictions. The majority of nurses mentioned that interactions with the hospital staff made a difference in job satisfaction. Supportive, encouraging, helpful, cheerful, and positive co-workers were variables listed among the most satisfying aspects of work. One nurse wrote: 'The staff that I work with is wonderful and they are doing everything to help me learn new things and answer any questions that I may have'. Several respondents used words such as 'great' and 'excellent teamwork' to describe co-worker relationships. One described the work environment as a 'family atmosphere'. Others mentioned the importance of positive communication with, encouragement from, and 'the helping spirit' of co-workers.
Interactions with nursing peers and supervisors were also mentioned as the least satisfying aspect of the job. Low staffing numbers were also mentioned, as were co-worker characteristics. Unsatisfying relationships occurred when co-workers did not help, support, appreciate or provide positive recognition. Perceptions of a lack of communication or demonstration of a lack of respect can deteriorate nurses' relationships. Nurses in this sample expressed a desire for 'adequately trained' supervisors with good leadership skills.
Several rural nurses indicated appreciation for work flexibility and scheduling independence. For instance, one nurse explained, 'As long as I complete my work and meet the requirements of my job, I may put my 40 hours in whenever most convenient for me'. Nurses mentioned that flexible work hours are helpful for personal life management and for spending time with children.
Some nurses wrote that the least satisfying aspects of the rural nurse were work scheduling problems and the amount of responsibility the job demanded. Nurses reported not having much flexibility or control over their work hours (eg working weekends and holidays). Several mentioned not being able to take scheduled breaks, to call in sick, or to take off more than a few days for vacation. One response described the 'Amount of responsibility, not enough time to finish work and working 9-10 hours a day without taking scheduled times off for breaks and lunch' as a problem. The staffing shortage was blamed for these issues.
Rural nurses report valuing autonomy and opportunities to make decisions regarding patient care. Nurses enjoyed job variety like working in different departments, with different types of patients, and learning and then practicing new skills. Moreover, nurses appreciated working in small facilities where it is possible to know staff members on a personal level. As one nurse wrote:
The small setting means that I know everyone, from the environmental services to the CEO. I know all the nurses, all the aides, almost all the dietary. I get on well with all the MDs, all half-dozen of them. I interact with a few of PT people, and all of the Respiratory people. I mix my own antibiotics, start my own IVs, run my own breathing treatments. I am jack of all trades, master of none. I like - I REALLY like - not having to specialize. I love the variety in the ages, in the conditions. I love seeing a patient's name and knowing from past experience his history and what to expect. I like being able to do everything for my patients, even if I don't do them all. I also work in the Emergency Room, and I love the added variety there...
Salary and benefits for themselves as well as for family members were named as the least satisfying aspect of the job. Nurses expressed feelings of being paid very little for the amount of responsibility given. One nurse noted, 'The abysmal compensation that nurses and other non-MD healthcare providers receive for their work (weekends, holidays, 24 hours a day) as least satisfying. No pension plan'. 'Miserable' healthcare insurance benefits were also mentioned.
In general, nurses enjoyed care giving and interacting with patients and families. Respondents listed patients as a most satisfying job aspect. Participants reported liking the responsibility of many types of patients. Nurses valued patient feedback and teaching. For example, one nurse responded, 'Helping patients and their families/significant others navigate through an increasingly complicated, confusing hostile/frightening healthcare juggernaut' was the most satisfying element of practice. Another wrote that 'providing good healthcare and treatment with a friendly face...' provided the most satisfaction.
Rural nurses' responses conveyed positive feelings about their job. Several nurses acknowledged the most satisfying aspect of their work environment was pride in the profession. They enjoyed taking care of patients and their families and felt that they made a difference. One nurse responded to the question with:
Saving a life or watching the process of trauma, surgery, recovery, and discharge is most satisfying. Helping a baby being born, comforting someone in pain or injured either physically or emotionally...
Discussion and Conclusion
The study of rural nurse practice perceptions indicates satisfaction concepts may differ from those of urban nurses. Results give us clues as to what is important to rural nurses, how the concepts relate to rural health and nursing theory concepts, the fact that satisfaction levels change over time, and the importance of rural nurse leaders. A short discussion of each topic is provided here.
Rural nurses reported lifestyle and personal life issues were important to the job choice. This was not identified in the literature. Concepts such as time away from work, rural lifestyle, recreation opportunities, climate and social activities were necessary for retention. Rural nurses with the most satisfaction preferred to live in rural areas and possessed rural backgrounds. Satisfied nurses lived close to family, friends, and spousal employment. Therefore, in order to increase retention, hospitals may consider marketing rural lifestyle opportunities and interviewing applicants about their rural backgrounds and connections.
Participants provide emphatic thoughts about the most and least satisfying aspects of their jobs. It should be noted the questions were placed after the scales, giving nurses time to reflect before writing responses. Although several findings may be applicable to urban nurses, the combination of findings seems an important extension to rural nursing literature. Findings can be related to rural theories22. Nurses reported a desire for organizational elements that supported personal lifestyles and values. For instance, flexible work hours that support family lifestyles and supportive-encouraging staff communication is in line with personal values.
Rural health and nursing theories were reinforced by the data from this sample. No literature was found linking rural nursing theory to job satisfaction. Findings suggest there is a link that needs further study of the links between lifestyle and job satisfaction. This sample stated preferences for work lifestyles mirrored rural lifestyle preferences. Examples include: work interactions were a priority, just as theory tells us rural residents are neighbor/community focused and build strong social networks. The sample nurses enjoyed practice autonomy and variety which is similar to the rural theory concept of independence22.
A job satisfaction study of the links between rural health theories and organizational elements is needed. If we understood the strength of the linkages between practice and rural lifestyle perhaps we could understand why nurse's overall job satisfaction varied based on length years worked. Why are nurses with 1-3 years' experience more dissatisfied than those with less than one year experience29 and or more than 10 years experience? Findings could impact organizational practices. Would a larger sample, a look at resource allocation or nurse background change the findings?
The satisfied nurses in this sample preferred the generalist role. Since most rural nurses practice as generalists and are trained across many specialties, the preference is fortuitous. Both the demand and preference for generalist practice impacts basic and professional education content. Educators may want to consider expanding opportunities for crisis assessment and management across specialties and rural clinical experiences to better prepare rural generalists.
Another issue for educators is the definition of the word 'generalist'. Basic education programs are required to produce generalists, and yet the term as defined in urban centers is a medical/surgical nurse. This is too narrow a definition for the rural setting where generalists must practice crisis assessment and management in all age groups and sub-specialties. Basic program educators need to understand differences in the 'generalist' term before they can educate rural generalists.
Findings in this study suggest examining both the hiring of rural leaders and the impact of leadership skills on job satisfaction. The sample stressed the importance of praise, recognition, communication and teamwork for their satisfaction. Administrators need more information about the challenges facing new nurse leaders and how to address the issues. The authors postulate that hiring rural nurse leaders may be a difficult task. There are two sources for hiring leaders: urban leaders and rural staff members. When urban leaders are hired for small rural hospitals, they are often considered 'outsiders' and have difficulty finding acceptance in stable communities22,25. However, if experienced rural staff members are promoted, leadership training is required because previous roles did not require the same management skills. In both cases transition to the new role takes time.
Findings suggest several organizational factors influencing rural nurse job satisfaction are within an executive's control. Rural administrators can address nurse personal characteristics during hiring and retention activities. Educators need more rural data in order to change their practice. Future studies with larger samples may reveal more evidence to take the guess work out of successful rural organizations.
References
1. Health Resources and Services Administration. Supply, demand, and shortages of registered nurses: 2000-2020. (Online) 2002. Available: http://www.ahca.org/research/rnsupply_demand.pdf (Accessed 1 September 2007).
2. McGuire M, Houser J, Jarrar T, Moy W, Wall M. Retention it's all about respect. Health Care Manager 2003; 22(1): 38-44.
3. Rambur B, Palumbo M, McIntosh B, Mongeon J. Statewide analysis of RNs' intention to leave their position. Nursing Outlook 2003; 51(4): 182-187.
4. Erickson JI, Holm LJ, Chelminiak L. Keeping the nursing shortage from becoming a nursing crisis. Journal of Nursing Administration 2004; 34(2): 83-87.
5. University of Washington. Health Workforce Recruitment and Retention in Critical Access Hospitals. CAH/FLEX National Tracking Project 2003; 3(5): Available: http://www.unmc.edu/ruprihealth/programs/results/vol3num5.pdf (Accessed 1 June 2008).
6. Washington State Department of Health, Office of Community and Rural Health. Health professions shortage areas. (Online) 2008. Available: http://www.doh.wa.gov/hsqa/ocrh/HPSA/hpsa1.htm (Accessed 1 June 2008).
7. Idaho Rural Health Association. Health professions shortage areas 2008. (Online) 2008. Available: http://www.isu.edu/irh/IRHA (Accessed 1 June 2008)
8. Schofield D, Fuller J, Fletcher S, Birden H, Page S, Kostal K, Wagner S et al. Decision criteria in health professionals choosing a rural practice setting: development of the Careers in Rural Health Tracking Survey (CIRHTS). Rural and Remote Health 7: 666. (Online) 2007. Available: http://www.rrh.org.au/ (Accessed 26 November 2008).
9. Gunderson A, Menachemi N, Brummel-Smith K, Brooks R. Physicians who treat the elderly in rural Florida: trends indicating concerns regarding access to care. Journal of Rural Health 2006; 22(3): 224-228.
10. Emmons SL, Nichols M, Schulkin J, James KE, Cain JM. The influence of physician gender on practice satisfaction among obstetrician gynecologists. American Journal of Obstetrics and Genecology 2006; 194(6): 1728-1733.
11. Backer EL, McIlvain HE, Paulman PM, Ramaekers RC. The characteristics of successful family physicians in rural Nebraska: A qualitative study of physician interviews. Journal of Rural Health 2006; 22(2): 189-191.
12. Lewis D. Multiple factors affect job satisfaction of hospital RNs. Robert Wood Johnson Foundation. Research Highlights 2007; 22: 1-2.
13. Wandel JC. Charting the course: The power of expert nurses to define the future. Journal for Nurses in Staff Development 2003; 21(6): no page range.
14. Kovner C, Brewer C, Wu Y, Cheng Y, Suzuki M. Factors associated with work satisfaction of registered nurses. Journal of Nursing Scholarship 2006; 38(1): 71-79.
15. Tierney AJ. What's the scoop on the nursing shortage? Journal of Advanced Nursing 2003; 43(4): 325-326.
16. Aiken L, Clarke S, Sloane D, Sochalski J, Silber J. Hospital nurse staffing and patient mortality, nurse burnout, and job dissatisfaction. Journal of American Medical Association 2000; 288(16): 1987-1993.
17. Bushy A, Leipert BD. Factors that influence students in choosing rural nursing practice: A pilot study. Rural and Remote Health 5: 387. (Online) 2005. Available: http://www.rrh.org.au/ (Accessed 10 June 2005).
18. Smith S, Edwards H, Courtney M, Finlayson K. Factors influencing student nurses in their choice of a rural clinical placement site. Rural and Remote Health 1: 89. (Online) 2001. Available: http://www.rrh.org.au/ (Accessed 3 November 2008).
19. Moszcynski AB, Haney CJ. Stress and coping of Canadian rural nurses caring for trauma patients who are transferred out. Journal of Emergency Nursing 2002; 28(6): 496-504.
20. Eldridge CR, Judkins S. Rural nurse administrators: essentials for practice. Online Journal of Rural Nursing and Health Care 2002; 3(2). Available: http://www.rno.org/journal/index.php/online-journal/article/viewFile/116/114 (Accessed 1 June 2008).
21. Glasser M, Peters K, McDowell M. Rural Illinois hospital chief executive officers' perceptions of provider shortages and issues in rural recruitment and retention. Journal of Rural Health 2006; 22(1): 59-62.
22. Bushy A. American Nurses Association Continuing Education Program Rural nursing: Practice and issues. (Online) 2004. Available: http://www.Nursingworld.org/mods/mod700/rurlfull.htm (Accessed 18 September 2005).
23. Bushy A. Orientation to nursing in the rural community. Thousand Oaks, CA: Sage, 2000.
24. O'Malley J, Fearnley J. Can generalist nurses be specialists? How can a rural secondary nursing service be sustained into the future? Kai Tiaki: Nursing New Zealand. (Online) 2007. Available: http://findarticles.com/p/articles/mi_hb4839/is_/ai_n29349218?tag=artBody;col1 (Accessed 28 November 2008).
25. Lee HJ, Winters C. Rural nursing: concepts, theory and practice. New York: Springer, 2006.
26. Lavoie-Tremblay M, Viens C, Forcier M, Labrosse N, Lafrance M, Laliberte D et al. How to facilitate the orientation of new nurses into the workplace. Journal for Nurses in Staff Development 2002; 18(2): 80-85.
27. Commonwealth Department of Education, Science and Training. Rural nurses: knowledge and skills required to meet challenges of a changing work environment in the 21st century: a review of literature. (Online) 2002. Available: http://www.dest.gov.au/archive/highered/nursing/pubs/rural_nurses/12.htm (Accessed 1 September 2007).
28. Floyd BO, Kretschmann S, Young H. Facilitating role transition for new graduate RNs in a semi-rural healthcare setting. Journal for Nurses in Staff Development 2005; 21(6): 284-290.
29. Molinari DL, Monserud M, Hudzinski D. The rural nurse internship: A new type of nurse residency. Journal of Continuing Education in Nursing 2008; 39(1): 42-46.
30. Ashton C, Block S, Buettner C, Burns M, Darrington D, Evans et al. Report of the Governor's Nursing Task Force. (Online) 2006. Available: http://gov.idaho.gov/Nursing%20Task%20Force%20Report%20Final.pdf (Accessed 28 November 2008).
31. Minnick AF. Retirement, the nursing work force, and the year 2005. Nursing Outlook 2000; 48: 211-217.
32. Watson R. The global shortage of registered nurses. Journal of Clinical Nursing 2005; 14(4): 409-409.
33. Ingersoll GL, Olsan T, Drew-Cates J, DeVinney BC, Davies J. Nurses' job satisfaction, organizational commitment, and career intent. Journal of Advanced Nursing 2002; 32(5): 250-63.
34. Yaktin US, Azoury NB, Doumit M. Personal characteristics and job satisfaction among nurses in Lebanon. Journal of Nursing Administration 2003; 33(7-8): 384-390.
35. Ma CC, Samuels ME, Alexander JW. Factors that influence nurses' job satisfaction, Journal of Nurse Administration 2003; 33(5): 293-299.
36. Gardner JK, Thomas-Hawkins C, Fogg L, Latham CE. The relationships between nurses' perceptions of the hemodialysis unit work environment and nurse turnover, patient satisfaction, and hospitalizations. Nephrology Nursing Journal 2007; 34(3): 271-281.
37. Pinikahana P, Happell B. Stress, burnout and job satisfaction in rural psychiatric nurses. Australian Journal of Rural Health 2004; 12(3): 120-125.
38. Fletcher CE. Hospital RNs' job satisfactions and dissatisfactions. Journal of Nursing Administration 2001; 31(6): 324-331.
39. Golembiewski RT, Hilles R, Rick D. Some effects of multiple OD interventions on burnout and work site features. Journal of Applied Behavioural Science 1987; 23: 295-313.
40. Kalliath T, Morris R. Job satisfaction among nurses: a predictor of burnout levels. Journal of Nursing Administration 2002; 32 (12): 648-654.
41. Laschinger HKS, Finnegan J. Situational and dispositional predictors of nurse manager burnout: a time-lagged analysis. Journal of Nursing Management 2008; 16(5):601-607.
42. Hays MA, All AC, Mannahan C, Cuaderes E, Wallace D. Reported stressors and ways of coping utilized by intensive care unit nurses. Dimensions of Critical Care Nursing 2006; 25(4): 185-193.
43. Penz K, Stewart NJ, D'Arcy C, Morgan D. Predictors of job satisfaction for rural acute care registered nurses in Canada. Western Journal of Nursing Research 2008; 30(7): 785-800.
44. Mills A, Blaesing S. A lesson from the last nursing shortage. Journal of Nursing Administration 2000; 30(6): 309-315.
45. Tourangeau AE, McGillis Hall L, Doran DM, Petch T. Measurement of nurse job satisfaction using the McCloskey/Mueller Satisfaction Scale. Nurse Research 2006; 55(2): 128-36.
46. Lea J, Cruickshank MT. The experience of new graduate nurses in rural practice in New South Wales. Rural and Remote Health 7: 814. (Online) 2007. Available: http://www.rrh.org.au/ (Accessed 3 November 2008).
47. MacKinnon KA. Labouring to nurse: The work of rural nurses who provide maternity care. Rural and Remote Health 8: 1047. (Online) 2008. Available: http://www.rrh.org.au/(Accessed 3 November 2008).
48. Irvine DM, Evans MG. Job satisfaction and turnover among nurses: integrating research findings across studies. Nurse Research 1995; 44: 246-252.
49. Aiken LH, Clarke SP, Sloane DM. Hospital staffing, organization, and quality of care: cross-national findings. Nursing Outlook 2002; 50(5): 187-194.
50. Mueller CW, McCloskey JC. Nurses' job satisfaction: a proposed measure. Nursing Research 1990; 39(2): 113-117.
