Introduction
The shortage of healthcare professionals in rural communities remains an intractable problem that poses a serious challenge to equitable healthcare delivery1. Both developed and developing countries report geographically skewed distributions of healthcare professionals, favouring urban and wealthier areas2-6. Rural communities are on average sicker, poorer and less well educated; they also have worse access to health care than people in urban areas. This discrepancy between health needs and service provision is captured by Hart's 'inverse care law', which states that those with the greatest health needs usually have the worst access to healthcare services7. Rapid urbanization is a global phenomenon but it poses particular problems in developing countries with poor infrastructure development; improved access to healthcare is often cited as one of the driving forces8.
A systematic review performed by the Cochrane Effective Practice and Organization of Care (EPOC) group aimed to evaluate critically the impact of various strategies aimed at reducing the rural-urban mismatch. Formal Cochrane reviews usually only include randomized control trials (RCTs) but, because no RCTs could be identified, review criteria were adjusted to include quasi-randomized studies, controlled before and after studies and interrupted time-series studies9-10. Despite using less stringent inclusion criteria, very few scientifically rigorous intervention studies were identified, which highlights the need for high quality research in this area.
At the same time, there is an urgent need to communicate the strength of the existing evidence to policy-makers and health educators in an effective and user-friendly manner. The aim of this review was to provide a comprehensive overview of the existing evidence, including studies that failed to meet requirements for inclusion in the Cochrane review, regarding the efficacy of various strategies to recruit healthcare professionals to, and retain them in rural communities. We attempted to critically assess the available evidence and summarize it in an easily accessible, user-friendly format.
Methods
A comprehensive search of the English literature was conducted using the National Library of Medicine's (PubMed) database and the keywords '(rural OR remote) AND (recruitment OR retention)' on 3 July 2008, yielding 1261 references. All titles and/or abstracts were screened to identify original studies that reported the outcome of an actual intervention. The search was extended by scrutinizing the references of selected articles. Relevant review articles were also screened to identify articles that may have been missed using the original search criteria. Due to the paucity of prospective primary intervention studies, retrospective observational studies and questionnaire-driven surveys were also included. In total, 110 articles were included.
In order to provide a comprehensive overview in a clear and user friendly fashion, we classified the available evidence into five intervention categories: Selection, Education, Coercion, Incentives and Support. For purposes of this review, these terms were defined as follows:
- Selection: focus on criteria used to select students into health profession training programs based on various factors that may increase the likelihood of retaining their services in rural and remote areas once qualified. Selection criteria evaluated include geographic origin, ethnicity, gender, career intent and service orientation.
- Education: focus on strategies that optimize medical training programs (pre-vocational and post-vocational) in such a way as to stimulate interest and participation in community-based medicine (including rural practice).
- Coercion: focus on the use of authoritarian methods (by medical councils, professional bodies and/or governments) to force health professionals into rural practice.
- Incentives: focus on the provision of financial incentives or bursary schemes that are linked to rural service agreements.
- Support: focus on different ways to support the health professional while practising in rural locations.
Table 1 provides a detailed description of the categories and sub-categories used. Studies that reported on multiple variables were considered in all the relevant categories.
Table 1: Classification of interventions aimed at reducing the inequitable distribution of medical doctors to rural areas
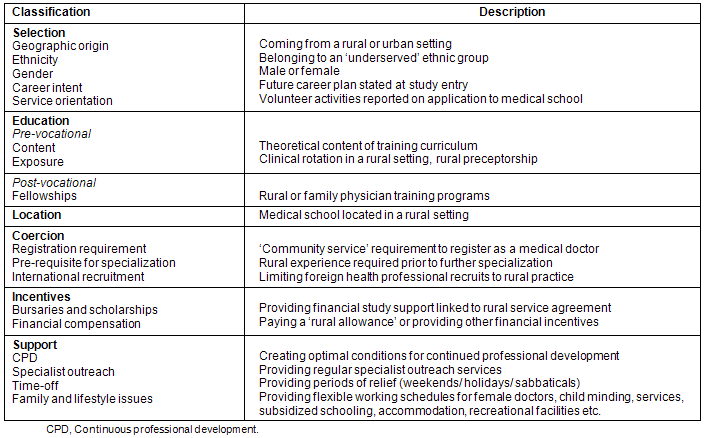
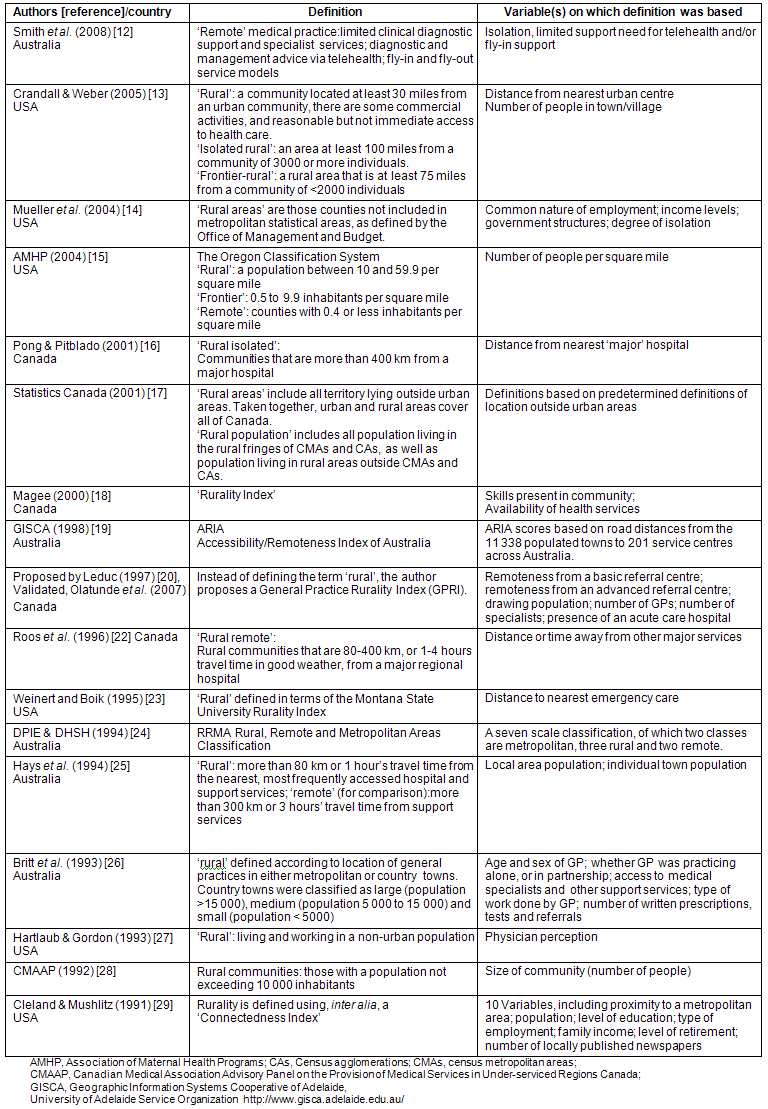
Specific definitions of 'rural' and/or 'remote' were not formulated and we accepted the range of definitions found in the literature reviewed. Table 2 summarizes the diversity of definitions utilized, which reflects the need to develop universal definitions that will facilitate study comparison and research collaboration. Definitions were selected from various manuscripts, including a review by Muula that emphasized the absence of universal definitions11. Recruitment was defined as the attraction of healthcare professionals to, and their installation in, rural settings. Retention was defined as a stay (or intended stay when questioned) of more than 5 years in total or more than 2 years beyond the termination of service agreement requirements.
In order to convey the strength of the existing evidence in a user-friendly fashion, a simple grading system was developed that utilized five categories: convincing, strong, moderate, weak and absent. Prospective RCTs were regarded as convincing evidence but, as mentioned, the recent Cochrane Review9 failed to identify any RCTs. Therefore, in the absence of prospective studies with sufficiently rigorous methodology, none of the evidence discussed in this review was rated as convincing. A strong rating was defined as 'consistent findings from multiple studies (retrospective and/or prospective) performed in various settings, where the independent effect of the particular variable was confirmed through multivariate analysis'. Moderate was defined as 'consistent qualitative and/or quantitative findings from multiple studies and in various settings, but without multivariate analysis'. Weak was defined as 'qualitative and/or quantitative findings that were inconsistent across studies or only reported in a single study'. Absent was defined as 'no evidence meeting any of the set criteria'.
Table 2: Summary of definitions used to define 'rural' and/or 'remote'12-29
Results
A short summary of the evidence that supports each of the intervention categories specified is provided. Table 3 provides an overview and also rates the strength of the evidence according to the definitions provided.
Table 3: Overview and rating of interventions aimed at reducing the rural-urban mismatch
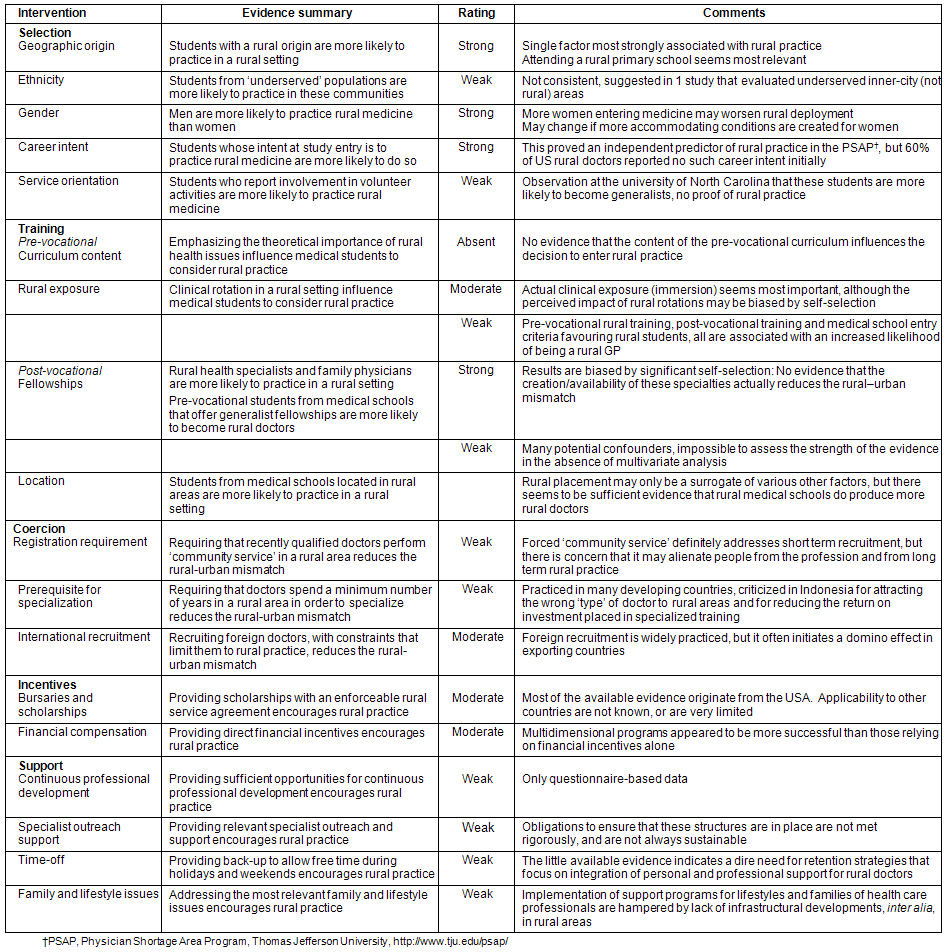
Selection
There is strong evidence from various countries that 'rural origin' (or rural background) is associated with rural practice30-34. Most studies defined rural origin as completing primary and/or secondary school education in a rural setting. In this respect, rural origin is especially linked to the decision to choose a rural community as one's first practice location35-37. The potential impact of selecting medical students of rural origin was quantified by Rabinowitz38 in a longitudinal study that evaluated the impact of the Physician Shortage Area Program (PSAP) in the USA. The PSAP combined selective admission criteria with a rurally orientated educational program. On multivariate analysis, rural origin was the single variable most strongly associated with rural practice (OR 4.2, 95% confidence interval [CI] 2.8-6.3)38. Another strong influence that was rarely considered is the origin of the spouse. Rabinowitz38 found that 64% of rural physicians had spouses of rural origin; in Australia, doctors whose spouses had a rural background were significantly more likely to practice in a rural setting (OR 3.14; 95% CI 1.96-5.1)39. A home prefecture recruiting scheme in Japan was successful in recruiting medical professionals from rural areas and retaining them as qualified professionals in medically underserved prefectures40. Table 4 reflects the evidence that selection according to geographic origin increases the number of graduates who practise in rural settings.
Table 4: Evidence that selection according to geographic origin may reduce the rural-urban mismatch31,33,38,41-44
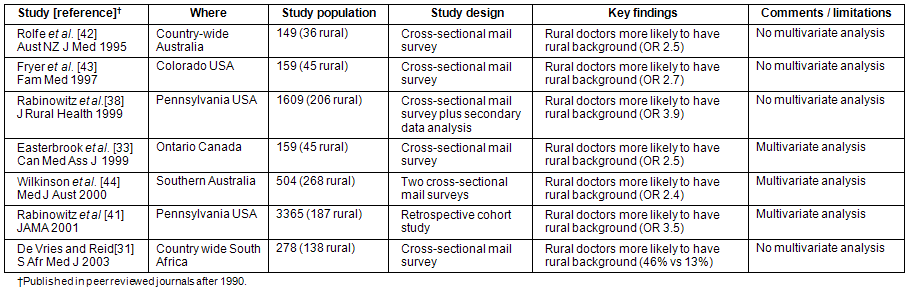
There is limited evidence that being from a minority ethnic group or an underserved population increases the likelihood of practising in a rural or underserved area. A single study that investigated underserved, inner-city populations in the USA45 reported that Hispanic generalists established practices in areas in which the percentages of the population that were (i) below poverty level; (ii) Hispanic; (iii) Hispanic and below poverty level; and (iv) white, non-Hispanic, and below poverty level, were greater than in areas in which white, non-Hispanic primary care physicians practiced. However, ethnicity has not been associated with rural practice in any of the other studies evaluated. Men were previously reported to be more likely than women to enter rural practice46,47, although the strength of the association was highly variable3. In contrast, Laven and Wilkinson32 concluded that gender was not found to be significant in 3 of the 9 studies. Five studies found that rural GPs were more likely to be male32. There is thus a great need to understand gender-related differences and how this influences geographic and specialty distribution; as more women enter medicine it may have the effect of further reducing the supply of medical doctors to rural areas.
The PSAP experience demonstrated an association between initial career intent (freshmen's interest in family practice, which was one of the selection criteria) and ultimate rural practice (OR 1.8; 95% CI 1.2-2.6)38; however, 60% of practising rural doctors in the US reported no intent to become a generalist at the onset of their medical studies41. Service orientation, as demonstrated by involvement in volunteer activities reported at the time of medical school application, has been associated with a generalist career in a single report48. The significance of this observation and its association with eventual practice in rural and/or underserved areas has not been evaluated.
The Rural Physician Associate Program (RPAP), also in the USA, has demonstrated success in providing rural primary care physicians to the State of Minnesota49,50. While selection is important as a success factor in the success of RPAP, many of these students had already expressed an interest in primary care. Students were also encouraged to spend 9 months in a primary-care setting to increase their interest and relevant experience. Flinders University established the Northern Territory Clinical School in Australia and employed a local quota program51. This quota program has been an effective method of enlisting local students who express an interest in living and studying in the sparsely populated Northern Territory52. Quota students (Northern Territory resident, Aboriginal and Torres Strait Islander) undertook longer rural placements than their non-quota peers and were 10 times more likely to spend their intern year in the Northern Territory. Both these programs thus support the concept of combining selection with local training.
Education
It is generally accepted that the tertiary hospital-based model of medical education exposes students mainly (even exclusively) to curative and specialized care, reducing the likelihood of a future generalist career and rural practice. Curricular content and clinical exposure may influence the career choice of graduate and post-graduate students, but few prospective studies have evaluated the influence exercised by medical education. Retrospective questionnaire-driven surveys indicate that theoretical course content had very little influence on the decision of rural doctors to enter rural practice31. Rural field residencies (immersion) together with adequate local guidance and supervision (preceptorship) seem to exercise the greatest influence53-56. It is extremely difficult to evaluate the independent contribution of rural field residencies, because these rotations are usually optional, which introduces considerable selection bias. Data from one medical school in Thailand indicated the majority of graduates continued in rural practice after completing a compulsory rural residency, using the immersion model57. Retrospective surveys conducted among rural doctors in other countries also support the value of pre-graduate rural exposure and the need to be equipped with the necessary skills to practise in a rural location32,58.
At the post-vocational level, doctors who completed generalist fellowships, such as family medicine or a rural health specialty, were predictably more likely to enter rural practice59-61. However, self-selection again introduces significant bias and there is no evidence that the availability of these generalist specialties actually recruits more doctors into rural practice. Countries such as Canada62 and Brazil63 have successfully adopted policies to reverse the trend towards specialization with positive results in terms of geographical deployment, but in general the restriction of specialist training has faced strong resistance from medical schools and professional associations. A survey of medical schools in the USA, titled 'Which medical schools produce rural physicians?'64 identified the following characteristics in medical schools that were most successful in producing rural practitioners: location in a rural state, public ownership, offering generalist specialties and receiving little research funding from the National Institutes of Health (NIH). More recently, Worley et al51 investigated the vocational career paths of graduate entry medical students of Flinders University in Australia. A comparison of rural, remote and tertiary tracks found that students who chose the 'parallel rural community curriculum' program or trained at the Northern Territory Clinical School were more likely to choose a rural career after graduation than their urban-trained counterparts.
Coercion
Forced redress, where penalties are applied if doctors do not comply with certain requirements, remain limited and controversial65,66. Coercive measures are often regarded as unfair, because other career professionals are rarely required to perform compulsory 'community service'. By singling out the healthcare profession, potential students may be discouraged from considering a medical career. Coercive measures can be particularly problematic for physicians and may result in a significant proportion being unable or unwilling to complete these service requirements, preventing them from entering professional practice. Problems associated with coercive measures are exacerbated by cultural and/or religious beliefs that prohibit physicians (especially women) and other medical staff from rendering much-needed health services, as discussed in articles that report the issue of gender-related problems in Pakistan67,68. Barley et al69, using a 37 item survey to obtain demographic information about the background, community and practice of rural female physicians, concluded that assumptions regarding rural physicians, especially women, must be updated to assist communities in recruiting rural physicians and to assist medical schools and residencies in adequately preparing graduates for rural practice69.
No published evidence was found that demonstrated the impact of coercive measures, such as compulsory 'community service'. Concern has been expressed that although coercive measures address short-term recruitment problems, it may worsen human resource constraints in the long term. This contradiction arises as coercive measures are usually applied to recently graduated and inexperienced doctors. Observational studies from South Africa suggests that requiring inexperienced doctors to perform 'community service' in rural areas without adequate guidance and support, may force them to practise outside their scope of competence, which undermines their confidence and leaves them open to litigation; these negative experiences often alienated junior doctors from considering rural practice as a career option70,71.
Incentives
Table 5 reflects the evidence that scholarships or bursaries with rural return of service agreements successfully recruit and retain more rural doctors. Few studies documented the efficacy of these interventions and the reported outcomes are highly variable. For example, many service-linked scholarships, loans and loan repayment programs have been described, but the effect of these on the rural or remote workforce are not clear72. In addition, contracts with a public service agreement in return for state sponsored training have been implemented in many developing countries in Latin America, Africa and South East Asia73, but a report by the WHO concluded that, overall, these policies have had very little influence on the geographic distribution of health professionals74. Ensuring that return of service agreements are honoured remained a challenge in all settings, and imposing excessive penalties has been strongly opposed by medical schools and professional associations57,75.
Table 5: Evidence that scholarships/bursaries with rural return of service agreements may result in more rural health professionals41,72,76-81
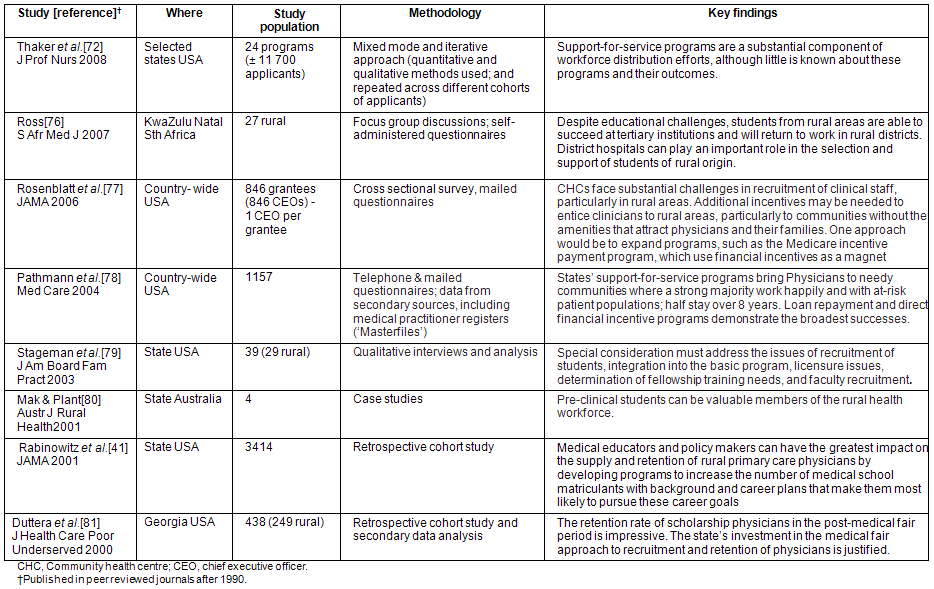
The experience with paying direct financial incentives, such as special rural allowances, has been variable. In Canada, the distribution of general practitioners was positively influenced by specifying raised fees in rural and underserved areas, and reduced fees in 'overserved' areas62. In the Philippines, rural incentives (linked to decentralization of the health service) had an unintended negative impact resulting from the fact that rural local governments were unable to hire healthcare professionals at the high salary levels specified82. Although remuneration issues feature prominently in questionnaire-based surveys and market theory predicts that financial incentives should help to remedy the situation, little quantitative evidence could be found to support the value of financial incentives.
More recently, incorporating both recruitment data and qualitative assessment using focus group discussions and questionnaires, Ross76 reported on the success of a novel scholarship scheme (Friends of Mosvold Scholarship Scheme; FOMSS). Despite educational challenges, students from rural areas in South Africa were able to succeed at tertiary institutions if provided with dedicated mentoring and support. In the program rural hospital managers played an important role in the selection and support of students and assumed responsibility in partnership with the bursary scheme. Providing ongoing support to students while at university (by maintaining regular contact, encouraging peer support and facilitating constructive volunteer work) and ensuring that on graduating they are integrated into the hospital workforce, proved to be an effective recruitment strategy. Of the 24 FOMSS students who have graduated, 18 were working in the district that supported them.
Support
Questionnaire-based surveys indicate that adequate support is valued by rural health professionals83,84. However, optimal strategies have not been identified and there is little empiric evidence to quantify its impact. Supportive measures receive more emphasis in countries where rural doctors are state-employed, compared with countries where rural health care is provided by private practitioners. Rural doctors listed the following complaints: academic isolation, lack of consultant support, insufficient locum relief and poor physical infrastructure at hospitals85,86. Family and lifestyle issues included access to good schools for children, poor recreational infrastructure, inadequate accommodation facilities and limited employment opportunities for the spouse87-89. An example of potentially contradictory qualitative evidence was the request for improved access to consultant services, while also indicating that the 'independence' of rural work and the need to deal with varied and challenging situations is an important attraction90.
Continuing Professional Development (CPD), formerly known as Continuing Medical Education (CME), includes all in-service training programs that supplement basic medical education and post-vocational training throughout a doctor's professional working life. Continuing professional development is a professional imperative for every doctor. Not only does it improve patient care but, if done efficiently, it also improves professional job satisfaction and may support rural recruitment and retention of doctors and other health professionals70,91,92. A study from Canada93 demonstrated that practice-based learning plays an increasingly important role as regulators require physicians to participate in CPD; it is stated that research in this area should explore ways of enhancing critical self-reflection. Investment in infrastructure, equipment and buying time-out may be required to support CPD activities94, but with the necessary commitment it is possible to identify simple and pragmatic ways to establish and maintain meaningful CPD activities in academically isolated rural hospitals70,95.
Discussion
Empiric evidence that supports the value of interventions to redress this inequitable distribution of healthcare professionals to rural and remote areas is limited, and huge healthcare disparities continue to present a global challenge74. In fact, the maldistribution of health professionals seems to be worsening in many developing countries2,96. The available evidence indicates that well-defined selection and education strategies hold value, which echoes the views of Strasser who stated:
...evidence shows that the three factors most strongly associated with entering rural practice after completing education and training are a rural upbringing, positive clinical experiences at the pre-vocational level, and specific post-vocational training for rural practice97.
Strategies that fall into the Incentives and Coercion categories address short-term recruitment needs, but little evidence supports their long-term impact, which may even be negative.
Qualitative research has identified numerous factors that may influence health professionals' decisions to stay in rural areas98; however, there is a need to conduct more rigorous quantitative studies to evaluate both the short- and long-term impact of interventions within each of the categories identified. The most important policies to consider in addressing the inequitable distribution of healthcare professionals, rated according to the strength of the available evidence, are reflected in Table 6. Government commitment to improve healthcare delivery to rural and underserved communities is essential, but policy should be guided by the best available evidence and every attempt should be made to generate rigorous evidence if novel or untested policies are adopted. The available evidence suggests that student selection, favouring rural applicants with a stated interest (or 'career intention') in general practice and a service orientation, is the strategy with the greatest likelihood of reducing the rural-urban gap. Continual research efforts that aim to determine career intent by medical graduates will add significant insight to understanding factors that may increase the likelihood of retaining their services in rural areas. Gender differences may be more pronounced in settings where female doctors have little chance of structuring their service hours to be more accommodating. In addition, the work ethos of medical professionals is changing in that many professionals would prefer to work fewer hours99-101. The impact of gender on future service commitments and deployment to rural and underserved communities requires further investigation, because there has been a major increase in the number of female students entering medical schools in recent years.
Table 6: Reducing the rural-urban mismatch - policy issues, implementation strategies and topics for further research
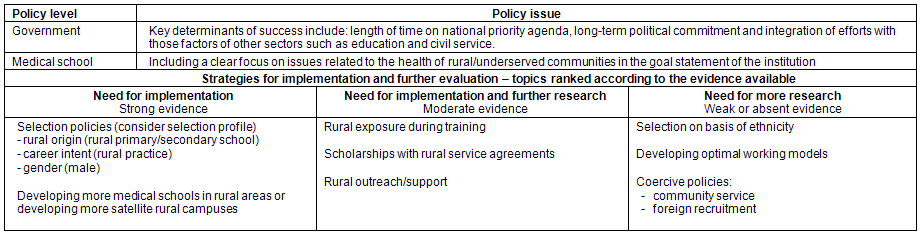
Another area of importance is measuring the short- and long-term impact of coercive measures. The success of scholarships or bursaries with rural return of service agreements (Table 5) is highly variable and the impact of novel bursary schemes and/or financial incentives requires further investigation76,102,103. Recruiting foreign doctors from countries that experience a dire shortage of doctors themselves may offer a short-term reprieve, but the ethical issues relating to foreign recruitment and forced rural deployment require further scrutiny. Similarly, the effect of intergovernmental arrangements requires careful impact evaluation to consider issues such as language, cultural barriers, experience of doctors and patients, and ethical issues. It remains important to try and identify optimal models for supplemented remuneration, but in general it appears that economic incentives alone are not enough to influence redeployment. The financial incentives issue illustrates an important point, namely that identifying reasons for dissatisfaction among rural doctors using questionnaire-based approaches may be useful to highlight problems that should be addressed, but it does not establish whether an intervention will actually improve the situation.
The value of supportive interventions may be difficult to measure and it may be argued that there is an ethical obligation to provide sufficient support to rural practitioners. Nevertheless, it would be worthwhile to quantify the impact of various support strategies; in other words, to move beyond simply asking physicians why they left or what they found unsatisfactory about rural practice, to using more sophisticated qualitative and quantitative methods to measure the response to specific interventions. Greater developmental investment with improvement in basic services such as water and sanitation, electricity, roads and schools is required, especially in developing countries, because poor infrastructure is frequently quoted as a reason why people, including health professionals, leave rural areas104.
In relation to educational support, it is difficult to determine the independent effect of locating medical schools in more rural settings, because findings would be confounded by multiple factors, such as the recruitment of more rural students or an increased likelihood that students will find a life partner of rural origin. However, identifying the exact variables that exercise the greatest independent influence seems irrelevant if the strength of the association between rural location of medical schools and ultimate rural practice is shown to be significant.
Interestingly, current evidence offers contradictory conclusions regarding the value of expert consultant support. On one hand rural doctors place great value on their independence and the challenge of coping with a variety of conditions on their own. On the other hand they express a need for improved access to and support from specialist services. Independence is a strong feature of rural practice, but it should not be promoted to the detriment of optimal patient care. More research on the interaction between consultant outreach services and rural physicians is needed to provide better guidance on how to optimize expert support services. Well structured CPD activities have demonstrated value to enhance knowledge and skill levels; significant event audits, regular peer review, group-based learning, and computer generated CPD reminders have all been shown to be effective educational strategies for general practice105. The impact of CPD programs in developing countries is less well described. For example, the Health Professions Council of South Africa only recently amended its CPD guidelines to encourage practical and participatory educational activities; therefore an evaluation of the impact of this policy change is not yet possible106.
Adding to the complexity is the distortion that may be created by research initiatives and decision-makers' lack of insight. Bowman107 contends that medical educators, deans and editors often spend most of their lives 'inside' privileged areas with high physician concentrations and lack knowledge about what is happening on the 'outside'. Thus the fact that 70-80% of rural or underserved origin candidates do not go 'outside' current concentrations of physicians and health resources allows them to ignore the fact that they go outside at rates that are between 2 and 10 times higher than the average medical student. He argues that it is difficult for those on the inside to give time and attention to, or even understand, the principles underlying distribution of physicians to underserved areas, which he summarises to be about physician origins outside, training outside, and policy supporting physician location outside current concentrations of physicians. Ultimately, closer collaboration between those inside and outside is required to perform research and inform pragmatic policy change geared to improving physician distribution.
A factor that has not been evaluated in the recruitment and retention debate is the need to define best practice models in various settings70. In the developed world where most of the studies were conducted, free market or state sponsored private practice is the norm, but in developing countries a major part of rural service delivery is provided by state employed doctors. In South Africa there is tension between these two models, although some 'public-private partnerships' (PPPs) have been successful in reducing this tension108. In addition, an 'ideal nation' model has been put forward that suggests a role for PPPs in academic medicine109. The development of best practice models may depend on pragmatic integration of the 'PPP-philosophy' into current healthcare platforms but, to date, no empiric evidence has been generated to guide this process.
The summary of definitions used for 'rural' and 'remote' illustrates the complexity of establishing universal definitions. There is a lack of research output and involvement in the formulation of workable definitions from developing countries, where the disparities are most pronounced and a developmental rather than a service approach to health is the norm. In other words, in developing countries health is inextricably linked to broader intersectoral issues of community development in terms of the primary healthcare approach, and the term 'rural' denotes more than just a geographic issue. Standard international definitions will assist researchers, policymakers and educators to collaborate, compare and share information more effectively12. This is important because the available pool of healthcare professionals represents a global asset110.
Strikingly, the emphasis on rural and underserved communities often represents 'narrow-minded' nationalistic views regarding inequitable distributions of healthcare professionals within a single country. While it is understandable that countries struggle to find solutions for their own problems, it is disconcerting to see how little emphasis is placed on the true health inequities from a global perspective. The main inequities are not within countries but between countries. If national boundaries are disregarded in order to look at the problem of inequitable access to healthcare from a global perspective, it becomes clear that the problem of health equity is far greater than mere rural-urban (or remote-urban) discrepancies. Innovative solutions need to be found.
One innovative alternative involves the development of new cadres of healthcare workers, for example through formalization of the role of the community health worker, or training mid-level medical workers (physician assistants)111-118. This cadre represents an important component of health service delivery recommended by the WHO and has been incorporated into primary healthcare initiatives in both developed and developing countries119. Their role in promoting public health is well-established in countries with successful primary and preventive care services such as Cuba, and in the face of the growing strain that HIV/AIDS are placing on public health facilities in sub-Saharan Africa120.
In conclusion, this review recognizes a dire need to evaluate in a scientifically rigorous fashion the impact of interventions and policies that aim to redress the inequitable distribution of healthcare professionals to rural and remote areas. It is only with the availability of more rigorous evidence and sufficient political commitment that we will be able to address the pressing issue of equitable healthcare delivery and identify winning strategies to guide future practice and policy.
Acknowledgements
The authors acknowledge the main authors of the Cochrane review, L Grobler and J Volmink, for conducting the formal Cochrane review process and making us aware of the limitations associated with the current evidence.
References
1. WHO. WHR 2003 (The World Health Report 2003) - shaping the future. (Online) 2003. Available: http://www.who.int/whr/previous/en/index.html (Accessed 5 May 2008).
2. Lehmann U, Dieleman M, Martineau T. Staffing remote rural areas in middle- and low-income countries: a literature review of attraction and retention. BMC Health Services Research 2008; 8: 19.
3. Vanasse A, Ricketts TC, Courteau J, Orzanco MG, Randolph R, Asghari S. Long term regional migration patterns of physicians over the course of their active practice careers. Rural Remote Health 7: 812. (Online) 2007. Available: www.rrh.org.au (Accessed 15 April 2008).
4. Dussault G, Franceschini MC. Not enough there, too many here: understanding geographical imbalances in the distribution of the health workforce. Human Resources and Health 2006; 4: 1.
5. Priester R, Elliott TE. Forecasting physician workforce requirements in Minnesota. Minnesota Medicine 1995; 78(10): 21-28.
6. Wright JS, Jablonowski AR. The rural-urban distribution of health professionals in Georgia. Journal of Rural Health 1987; 3(1): 53-70.
7. Hart JT. The inverse care law. Lancet 1971; 1(7696): 405-412.
8. Phillips DR. Urbanization and human health. Parasitology 1993; 106(Suppl): S93-S107.
9. Grobler LA, Marais BJ, Mabunda SA, Marindi PN, Reuter H, Volmink J. Interventions for increasing the proportion of health professionals practising in rural and other underserved areas. Cochrane Database of Systemic Reviews 2009 Jan 21;(1): CD005314.
10. Grobler LA, Marindi PN, Mabunda SA, Reuter H, Volmink J. Interventions for increasing the proportion of health professionals practising in under-served communities. Cochrane Database of Systematic Reviews 2005; issue 1. Art. no: CD005314. DOI: 10.1002/14651858.CD005314.
11. Muula A. How do we define 'rurality' in the teaching on medical demography? Rural Remote Health 7: 653. (Online) 2007. Available: www.rrh.org.au (Accessed 15 April 2008).
12. Smith JD, Margolis SA, Ayton J, Ross V, Chalmers E, Giddings P et al. Defining remote medical practice. A consensus viewpoint of medical practitioners working and teaching in remote practice. Medical Journal of Australia 2008; 188(3): 159-161.
13. Crandall M, Weber B. Defining rural Oregon: an exploration. Oregon: Rural Studies Program, Oregon State University, 2005; 13.
14. Mueller KJ, Slifkin R, Shambaugh-Miller MD, Randolph RK. Definition of rural in the context of MMA Access Standards for Prescription Drug Plans. Chapel Hill, NC: RUPRI Center for Rural Health Policy, Omaha, Nebraska and North Carolina Rural Health Research and Policy Center, 2004.
15. The Association of Maternal Health Programs. The Association of Maternal Health Programs. From rural to remote America. Family health care in Alaska, Idaho, Oregon and Washington. Washington, DC: AMHP, 2004.
16. Pong RW, Pitblado JR. Don't take 'geography' for granted! Some methodological issues in measuring geographic distribution of physicians. Canadian Journal of Rural Medicine 2001; 6: 103-112.
17. Statistics Canada. Geographic units: Rural Area (RA). (Online) 2009. Available: http://www12.statcan.ca/english/census01/Products/Reference/dict/geo042.htm (accessed 21 July 2008).
18. Magee GC. Procedural skills rurality index for the medical community. Canadian Journal of Rural Medicine 2000; 5: 18.
19. The National Key Centre for the Social Applications of GIS. ARIA vs RRMA. (Online) 2000. Available: http://www.gisca.adelaide.edu.au/web_aria/Rural_Health/aria_rrma/aria_1.html (Accessed 4 June 2009).
20. Leduc E. Defining rurality: a General Practice Rurality Index for Canada. Canadian Journal of Rural Medicine 1997; 2(2): 125.
21. Olatunde S, Leduc ER, Berkowitz J. Different practice patterns of rural and urban general practitioners are predicted by the General Practice Rurality Index. Canadian Journal of Rural Medicine 2007; 12(2): 73-80.
22. Roos N, Fransoo R, Bogdanovic B, Friesen D, Frohlich N, Carriere KC. Needs-based planning for Manitoba's generalist physicians. Winnipeg, Manitoba: Manitoba Centre for Health Policy and Evaluation, University of Manitoba, 1996.
23. Weinert C, Boik RJ. MSU rurality index: development and evaluation. Research, Nursing and Health 1995; 18: 453-464.
24. DPIE and DHSH. RRMA Methodology: Introduction. (Online) 2000. Available: http://www.gisca.adelaide.edu.au/web_aria/Rural_Health/aria_rrma/aria_1.html (Accessed 4 June 2009).
25. Hays RB, Craig ML, Wise AL, Nichols A, Mahoney MD, Adkins PB et al. A sampling framework for rural and remote doctors. Australian Journal of Public Health 1994; 18(3): 273-276.
26. Britt H, Miles DA, Bridges-Webb CB, Neary S, Charles J, Traynor V. A comparison of country and metropolitan general practice. Medical Journal of Australia 1993; 159(Suppl): S9-S64.
27. Hartlaub PP, Gordon RL. Rural practice. Preference, perception, and reality. Archives of Family Medicine 1993; 2(11): 1198-1201.
28. Canadian Medical Association Advisory Panel. Advisory Panel on the Provision of Medical Services in Underserviced Regions. Report of the Advisory Panel on the Provision of Medical Services in Underserviced Regions. Ottawa: Canadian Medical Association, 1992.
29. Cleland CL, Mushlitz B. Measuring rurality: connections. Columbus, OH: Ohio Rural Sociological Society, 1991.
30. Playford D, Larson A, Wheatland B. Going country: rural student placement factors associated with future rural employment in nursing and allied health. Australian Journal of Rural Health 2006; 14(1): 14-19
31. De Vries E, Reid S. Do South African medical students of rural origin return to rural practice? South African Medical Journal 2003; 93: 789-793.
32. Laven G, Wilkinson D. Rural doctors and rural backgrounds: how strong is the evidence? A systematic review. Australian Journal of Rural Health 2003; 11: 277-284.
33. Easterbrook M, Godwin M, Wilson R, Hodgetts G, Brown G, Pong R et al. Rural background and clinical rural rotations during medical training: effect on practice location. Canadian Medical Association Journal 1999; 160(8): 1159-1156.
34. Rabinowitz HK. Recruitment, retention, and follow-up of graduates of a program to increase the number of family physicians in rural and underserved areas. New England Journal of Medicine 1993; 328(13): 934-939.
35. Bowman RC. Continuing family medicine's unique contribution to rural health care. American Family Physician 1996; 54(2): 471-4,479,483.
36. Rourke JT. Politics of rural health care: recruitment and retention of physicians. Canadian Medical Association Journal 1993; 148(8): 1281-1284.
37. Barer ML, Stoddart GL. Toward integrated medical resource policies for Canada: 8. Geographic distribution of physicians. Canadian Medical Association Journal 1992; 147(5): 617-623.
38. Rabinowitz HK, Diamond JJ, Hojat M, Hazelwood CE. Demographic, educational and economic factors and retention of physicians in rural Pennsylvania. Journal of Rural Health 1999; 15: 212-218.
39. Laven GA, Beilby JJ, Wilkinson D, McElroy HJ. Factors associated with rural practice among Australian-trained general practitioners. Medical Journal of Australia 2003; 179(2): 75-79.
40. Matsumoto M, Inoue K, Kajii E. Long-term effect of the home prefecture recruiting scheme of Jichi Medical University, Japan. Rural Remote Health 8: 930. (Online) 2008. Available: www.rrh.org.au (Accessed 23 July 2008).
41. Rabinowitz HK, Diamond JJ, Markham FW, Paynter NP. Critical factors for designing programs to increase the supply and retention of rural primary care physicians. JAMA 2001; 286: 1041-1048.
42. Rolfe IE, Pearson SA, O'Connell DL, Dickinson JA. Finding solutions to the rural doctor shortage: the roles of selection versus undergraduate medical education at Newcastle. Australian and New Zealand Journal of Medicine 1995; 25(5): 512-517.
43. Fryer GE Jr, Stine C, Vojir C, Miller M. Predictors and profiles of rural versus urban family practice. Family Medicine 1997; 29(2): 115-118.
44. Wilkinson D, Beilby J, Thompson DJ, Laven GA, Chamberlain NL, Laurence CO. Associations between rural background and where South Australian general practitioners work. Medical Journal of Australia 2000; 173: 137-140.
45. Fryer GE Jr, Green LA, Vojir CP, Krugman RD, Miyoshi TJ, Stine C et al. Hispanic versus white, non-Hispanic physician medical practices in Colorado. Journal of Health Care of the Poor and Underserved 2001; 12(3): 342-351.
46. Lindsay S. Gender differences in rural and urban practice location among mid-level health care providers. Journal of Rural Health 2007; 23(1): 72-76.
47. Shannon CK. A gender-based study of attitudes and practice characteristics of rural physicians in West Virginia. WV Medical Journal 2006; 102(6): 22-25.
48. Madison DL. Medical school admission and generalist physicians: a study of the class of 1985. Academic Medicine 1994; 69(10): 825-831.
49. Halaas GW. The Rural Physician Associate Program: successful outcomes in primary care and rural practice. Rural Remote Health 5: 453. (Online) 2005. Available: www.rrh.org.au (Accessed 15 April 2008).
50. Whitcomb ME, Cohen JJ. The future of primary care medicine. New England Journal of Medicine 2004; 351: 710-712.
51. Worley P, Martin A, Prideaux D, Woodman R, Worley E, Lowe M. Vocational career paths of graduate entry medical students at Flinders University: a comparison of rural, remote and tertiary tracks. Medical Journal of Australia 2008; 188(3): 177.
52. McDonnel Smedts A, Lowe MP. Clinical training in the top end: impact of the NTCS, Australia, on the Territory's health workforce. Rural Remote Health 7: 723. (Online) 2007. Available: www.rrh.org.au (Accessed 15 April 2008).
53. Smedley AM. Becoming and being a preceptor: a phenomenological study. Journal of Continence Education Nursing 2008; 39(4): 185-191.
54. Diefenbeck CA, Plowfield LA, Herrman JW. Clinical immersion: a residency model for nursing education. Nurse Education Perspective 2006; 27(2): 72-79.
55. Erkel EA, Nivens AS, Kennedy DE. Intensive immersion of nursing students in rural interdisciplinary care. Journal of Nursing Education 1995; 34(8): 359-65.
56. Hale FA, McConnochie KM, Chapman RJ, Whiting RD. The impact of a required preceptorship on senior medical students. Journal of Medical Education 1979; 54(5): 396-401.
57. Wibulpolprasert S, Pengpaibon P. Integrated strategies to tackle the inequitable distribution of doctors in Thailand: four decades of experience. Human Resources and Health 2003; 1(1): 12.
58. Kirby BA. The rural rotation in a medical technology program: a ten-year retrospective study. Clinical Laboratory Sciences 2007; 20(4): 202-209.
59. Acosta DA. Impact of rural training on physician workforce: the role of postresidency education. Journal of Rural Health 2000; 16(3): 254.
60. Acosta D. Current status of residency fellowships in rural health. Chicago: Society of Teachers of Family Medicine Working Group on Rural Health, 1998.
61. Bowman RC, Penrod JD. Family practice residency programs and the graduation of rural family physicians. Family Medicine 1998; 30: 288.
62. Fournier M. Les politiques de main-d'oeuvre médicale au Québec: bilan 1970-2000. Ruptures (revue transdisciplinaire en santé) 2001; 7(2): 79-98. (In French)
63. Ministeria de Salude. Programa Saude da Familia. (Online) 2004. Available: http://dtr2004.saude.gov.br/dab/ (Accessed 12 May 2008). (In Spanish)
64. Rosenblatt RA, Whitcomb ME, Cullen TJ, Lishner DM, Hart LG. Which medical schools produce rural physicians? JAMA 1992; 268(12): 1559-1565.
65. Kotzee T, Couper ID. What interventions do South African qualified doctors think will retain them in rural hospitals of the Limpopo province of South Africa? Rural Remote Health 6: 581. (Online) 2006. Available: www.rrh.org.au (Accessed 15 April 2008).
66. Ricketts TC. Workforce issues in rural areas: a focus on policy equity. American Journal of Public Health 2005; 95: 42.
67. Shaikh BT, Reza S, Afzal M, Rabbani F. Gender sensitization among health providers and communities through transformative learning tools: experiences from Karachi, Pakistan. Education in Health (Abingdon) 2007; 20(3): 118.
68. Mumtaz Z, Salway S, Waseem M, Umer N. Gender-based barriers to primary health care provision in Pakistan: the experience of female providers. Health Policy Planning 2003; 18(3): 261-269.
69. Barley GE, Reeves CB, O'Brien-Gonzales A, Westfall JM. Characteristics of and issues faced by rural female family physicians. Journal of Rural Health 2001; 17(3): 251.
70. Marais BJ, De Villiers M, Kruger J, Conradie H, Jenkins L, Reuter H. The role of educational strategies to reverse the inverse performance spiral in academically isolated rural hospitals. South African Family Practice 2007; 49(7): 15a-15e.
71. Nemutandani MS, Maluleke FRS, Rudolph MJ. Community service doctors in Limpopo province. South African Medical Journal 2006; 96(3): 180.
72. Thaker SI, Pathman DE, Mark BA, Ricketts TC 3rd. Service-linked scholarships, loans, and loan repayment programs for nurses in the southeast. Journal of Professional Nursing 2008; 24(2): 122-130.
73. Hammer J, Jack W. The design of incentives for health care providers in developing countries: contracts, competition and cost-control. Policy Research Paper no 2547. Washington, DC: World Bank, 2001.
74. WHO. World Health Report. Geneva: WHO, 2000.
75. Wibulpolprasert S: Inequitable distribution of doctors: can it be solved? Human Resources Development Journal 1999; 3(1): 2-22.
76. Ross AJ. Success of a scholarship scheme for rural students. South African Medical Journal 2007; 97: 1087-1090.
77. Rosenblatt RA, Andrilla CH, Curtin T, Hart LG. Shortages of medical personnel at community health centers: implications for planned expansion. JAMA 2006; 295(9): 1042-1049.
78. Pathman DE, Konrad TR, King TS, Taylor DH Jr, Koch GG. Outcomes of states' scholarship, loan repayment, and related programs for physicians. Medical Care 2004; 42(6): 560-568.
79. Stageman JH, Bowman RC, Harrison JD. An accelerated rural training program. Journal of the American Board of Family Practice 2003; 16(2): 124-130
8. Mak D, Plant AJ. John Flynn Scholarship Students: case studies of useful contributions to remote health care. Australian Journal of Rural Health 2001; 9: 246-250.
81. Duttera MJ Jr, Blumenthal DS, Alan Dever GE, Lawley JB. Improving recruitment and retention of medical scholarship recipients in rural Georgia. Journal of Health Care of the Poor and Underserved 2000; 11(2): 135.
82. Perez, JA. Discussion, in Wibulpolprasert S. Inequitable distribution of doctors: can it be solved? Human Resources Development Journal 1999; 3(1): 2-22.
83. Gardiner M, Sexton R, Durbridge M, Garrard K. The role of psychological wellbeing in retaining rural GPs. Australian Journal of Rural Health 2005; 13: 149-155.
84. Gardiner M, Sexton R, Kearns H, Marshall K. Impact of support initiatives on retaining rural general practitioners Australian Journal of Rural Health 2006; 14: 196-201.
85. McLean R. Continuing professional development for rural physicians: an oxymoron or just non-existent? Internal Medicine Journal 2006; 36(10): 661-664.
86. Kamien M. Staying in or leaving rural practice: 1996 outcomes of rural doctors' 1986 intentions. Medical Journal of Australia 1998; 169: 318-321.
87. Richards HM, Farmer J, Selvaraj S. Sustaining the rural primary healthcare workforce: survey of healthcare professionals in the Scottish Highlands. Rural Remote Health 5: 365. (Online) 2005. Available: www.rrh.org.au (Accessed 15 April 2008).
88. Jones JA, Humphreys JS, Adena M. Rural GP's ratings of initiatives designed to improve rural medical workforce recruitment and retention. Rural Remote Health 4: 314. (Online) 2004. Available: www.rrh.org.au (Accessed 15 April 2008).
89. Humphreys JS, Jones MP, Jones JA, Mara PR. Workforce retention in rural and remote Australia: determining the factors that influence length of practice. Medical Journal of Australia 2002; 176: :472-476.
90. Pathman DE, Konrad KR, Agnew CR. Studying the retention of rural physicians. Journal of Rural Health 1994; 10: 183-192.
91. Fahey CM, Monaghan JS. Australian rural midwives: perspectives on continuing professional development. Rural Remote Health 5: 468. (Online) 2005. Available: www.rrh.org.au (Accessed 15 April 2008).
92. Humphreys J, Wakerman J, Wells R, Kuipers P, Jones J, Entwistle P et al. Improving primary health care workforce retention in small rural and remote communities: how important is ongoing education and training? Canberra, ACT: Australian Primary Health Care Research Institute, Australian National University, 2007. Available: http://www.anu.edu.au/aphcri/Domain/Workforce/Humphreys_25_final.pdf (Accessed 2 June 2008).
93. Silver I, Campbell C, Marlow B, Sargeant J. Self-assessment and continuing professional development: the Canadian perspective. Journal of Continence Education Health Professionals 2008; 28(1): 25-31.
94. Gagliardi AR, Wright FC, Anderson MA, Davis D. The role of collegial interaction in continuing professional development. Journal of Continence Education Health Professionals 2007; 27(4): 214-219.
95. Edginton ME, Holst HL. Doctors in rural hospitals in Kwazulu and Natal. South African Medical Journal 1991; 80: 511.
96. Health Systems Trust. HST publishes its 1Oth SAHR: The Importance of the Health Worker. (Online) 2005. Available: http://www.hst.org.za/news/20040927 (Accessed 22 May 2008).
97. Strasser R. Training for rural practice: lessons from Australia. Canadian Family Physician 2001; 47: 2196.
98. Couper ID, Hugo JFM, Conradie H, Mfenyana K. Influences on the choice of health professionals to practice in rural areas. South African Medical Journal 2007; 97(11): 1082.
99. Bond JT, Galinsky E, Swanberg JE. The 1997 National Study of the Changing Workforce. New York, NY: Family and Work Institute, 1998.
100. Jacobs JA, Gerson K. The endless day or flexible Office? Working hours, work-family conflict, and gender equity in the modern workplace. New York, NY: Alfred P Sloan Foundation, 1997.
101. Carr PL, Gareis KC, Barnett RC. Characteristics and outcomes for women physicians who work reduced hours. Journal of Womens Health 2003; 12: 399.
102. Sempowski IP. Effectiveness of financial incentives in exchange for rural and underserviced area return-of-service commitments: systematic review of the literature. Canadian Journal of Rural Medicine 2004; 9(2): 82.
103. Ross AJ, Couper ID. Rural Scholarship Schemes: A solution to the human resource crisis in rural district hospitals. South African Family Practice 2004; 46(1): 5-6.
104. Katrak H. Measuring the shortage of medical practitioners in rural and urban areas in developing countries: a simple framework and simulation exercises with data from India. International Journal of Health Planning and Management 2007; 23: 93-105.
105. Cantillon P, Jones R. Does continuing medical education in general practice make a difference? BMJ 1999; 318(7193): 1276-1279.
106. Health Professions Council of South Africa. Continuing professional development. (Online) 2007. Available: http://www.hpcsa.co.za/hpcsa/default.aspx?id=183 (accessed 5 May 2008).
107. Bowman RC. They really do go. Rural Remote Health 8: 1035. (Online) 2008. Available: www.rrh.org.au (Accessed 29 May 2009).
108. Du Toit J. PPP insights in South Africa. World Hospitla Health Service 2003; 39(1): 2-10,30,32.
109. Mokoena T. Public-private partnerships in academic medicine - an 'ideal nation' model. South African Medical Journal 1999; 89(2): 134-135.
110. Shuchman M. Searching for docs on foreign shores. Canadian Medical Association Journal 2008; 178(4): 379-380.
111. Couper ID. Mid-level workers: high-level bungling? South African Medical Journal 2007; 97(3): 146. (Comment)
112. Hugo J, Mfenyana K. Mid-level workers: high-level bungling? South African Medical Journal 2007; 97(3): 146,148. (Comment)
113. Van Niekerk JP. Mid-level workers: high-level bungling? South African Medical Journal 2006; 96: 1209-1211. , , , ,
114. Hugo J. Mid-level health workers in South Africa: not an easy option. In: P Ijumba, P Barron (Eds). South African Health Review . (Online) 2005. Available: http://www.hst.org.za/generic/29 (Accessed 5 July 2008).
115. Pfaff C. Mid-level primary health care workers in Nepal. South African Family Practice 2004; 46(2): 32-33.
116. Thetard R. Clinical officers in Malawi. South African Family Practice 2004; 46(2): 32.
117. Mittman DE, Cawley JF, Fenn H, Physician assistants in the United States. BMJ 2002; 325: 485.
118. Pick WM, Khanyisa N, Cornwall JT, Masuku M. Human resources for health: a national strategy. Pretoria: Department of Health, 2001.
119. Kuhn L, Zwarenstein MF, Thomas GC, Yach D, Conradie HH, Hoogendoorn L et al. Village health-workers and GOBI-FFF. An evaluation of a rural programme. South African Medical Journal 1990; 77(9): 471-475.
120. Doherty TM, Coetzee M. Community health workers and professional nurses: defining the roles and understanding the relationships. Public Health Nursing 2005, 22(4): 360-365.






