Introduction
The geographic maldistribution of physicians (ie the concentration of physicians in urban areas and their consequent shortage in rural areas), has long been an important welfare and political issue in Japan, as well as in other countries1. Japan's government has introduced many strategies to establish physicians in rural areas, including the 1956 'Strategy to Promote Rural Health and Medical Services', in which Japan's national and local governments vigorously supported the distribution of medical resources to rural areas2.
This problem is not unique to Japan as markedly high concentrations of physicians in urban areas and shortages in rural areas have been reported worldwide3-6. It has long been assumed that the root of the problem, and therefore its possible solution, lies with market forces influencing the distribution of doctors7. If this was so, increasing the total number of physicians would lead to an improvement in some rural areas. However, at least in Japan, it has been reported that this has not resulted in improvement; in fact, it has led to an exacerbation of the maldistribution3. A new way to redress the problem is needed, and the most appropriate strategy can only be found by a thorough evaluation of all the factors that influence the geographic distribution of physicians.
Therefore, this study analyzed physicians' geographic distribution and movement, using available census data on Japanese physicians in 1980 and 2002, and identified the factors which are associated with the long-term settlement of physicians in rural areas.
Methods
Upon obtaining a license to practice, all physicians in Japan are enrolled in the National Register of Physicians and are assigned a unique physician identification (ID) number by the Ministry of Health, Labour and Welfare. The Ministry conducts a Physician Census every 2 years, and all licensed physicians are legally required to update their information. The information collected includes the physician's name, sex, ID number, date of enrollment, employment address, employing institution, and medical specialty. With the permission of the Ministry of Health, Labour and Welfare, an electronic file of the 1980 and 2002 versions of the Physician Census were accessed. All physicians who were registered in both 1980 and 2002 were extracted by merging both years' Physician Census data. Duplicate reports for the same physician were checked and modified for the 2002 Physician Census, but not for the 1980 Physician Census. Thus, physicians who duplicated reports in the 1980 Physician Census were excluded from this study, reducing the number of physicians by less than 0.5% (from 156 235 to 155 530). The career length of physicians in 1980 was estimated by subtracting the year of issue of their physician's license from 1980.
To assess the relationship between types of specialty and practice location, physicians who registered their specialties as internal medicine, surgery, pediatrics, or general medicine were classified as primary care physicians. Because the Japanese medical system does not have a formally recognized specialty of integrated primary care comparable to family medicine in the US, internists, pediatrician and general surgeons play a substantial role in primary care8. Physicians were also classified into three categories according to their employing institutions: clinic, hospital and other. In Japan, a clinic is a medical institution having less than 20 inpatients. A hospital is a medical institution with 20 or more inpatient beds. Accordingly, clinic practice tends to be an indication of primary care rather than hospital practice. In Japan, clinic practitioners are mostly in sole practice and hospital physicians are mostly in group practice. The 'other' category indicates non-clinical institutions, such as a public health division, a non-medical profession and a non-working physician.
Japan has 47 prefectures which consist of municipalities; the basic administrative units are categorized as cities, towns and villages. In 1980, there were 669 cities (including the 23 special districts of Japan's capital, Tokyo), 1991 towns and 618 villages in Japan. Population size is the main difference among the three categories; according to national law, a city must have a population of 50 000 or more. Towns and villages have smaller populations and tend to be rural and remote from prefectural capital cities. Towns and villages belong to an upper administrative district, which is termed 'county' in Japan. Thus, we classified all the municipalities of Japan into two administrative areas: city and county, which for the purpose of this study have been termed urban and rural, respectively. The working addresses of physicians reported in the Physician Census 1980 and 2002 were categorized as either urban or rural. Combining the data from the 1980 version of Physician Census and the 1980 National Population Census, the 1980 physician-to-population ratio of each geographical area was calculated as the number of physicians per 100 000 residents. The physician-to-population ratio in 2002 was calculated from the 2002 Physician Census and from the 2000 National Population Census. The difference between the whole national population in the 2000 version of the National Population Census (126 925 843) and the estimated national population in 2002 (127 377 000) was 0.4%. For the purposes of this study, the physician information was anonymous.
The software SPSS for Windows v15.0J (SPSS inc; Chicago, IL, USA) was used for statistical analysis. The relationship between a physician's attributes and practicing in a rural area after 22 years was examined by univariate and multivariate logistic regression analysis.
Results
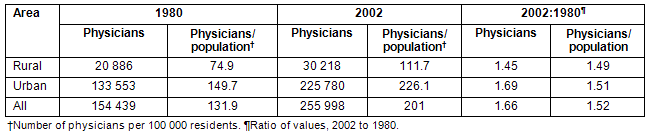
Data were available on 155 530 and 262 680 physicians in the 1980 and 2002 Physician Censuses, respectively. Table 1 shows the physician distribution in Japan in 1980 and 2002. The increases in the physician-to-population ratios between 1980 and 2002 in urban and rural areas were virtually identical (51% vs 49%). Both in 1980 and 2002, the physician-to-population ratios of rural areas were approximately half the physician-to-population ratios of urban areas, indicating that the physician-underserved status of rural areas relative to urban areas had not improved.
Table 1: Distribution of physicians in 1980 and 2002 in Japan
The 1980 and 2002 Physician Census data were merged to extract the 93 077 physicians who were recorded in both censuses. This physician cohort amounted to 59.8% of the total physicians in 1980 and 35.4% of the total physicians in 2002. Table 2 shows the characteristics of the 93 007 physicians according to their working areas (urban or rural) in 1980 and 2002. In 1980, 10 663 physicians (11.5%) worked in rural areas and 82 414 physicians (88.5%) worked in urban areas. In 2002, 11 937 physicians worked in rural areas, an increase of 11.9%. In 2002, more than 90% of the 1980 urban physicians had remained in city areas. In contrast, half of the 1980 rural physicians had stayed in rural areas, and the remainder had moved to city areas.
Table 2: Characteristics of the 93 007 physicians in 1980 and 2002
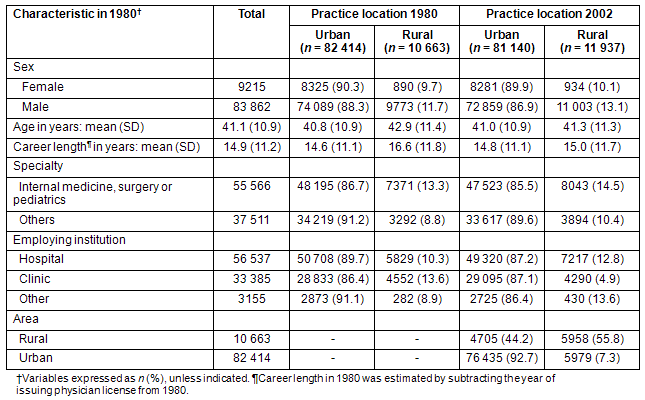
Figure 1 shows the details of the flow of physicians between urban and rural areas. It shows the number of physicians who remained in the same geographic categories between 1980 and 2002, according to their career lengths. The graph shows the difference between 1980 urban and rural physicians. In 2002, most of the 1980 urban physicians had remained in city areas, with a slightly higher staying rate as their career lengthened (from 88.1% at 0-1 years to 96.7% at 18 years or longer). However, the 1980 rural physicians had a markedly lower staying rate than urban physicians, and this substantially increased with career length (from 25.2% at 0-1 years to 75.3% at 18 years or longer). The staying rates of county physicians among the three youngest groups (0-1, 2-3 and 4-5 years) were almost constant.
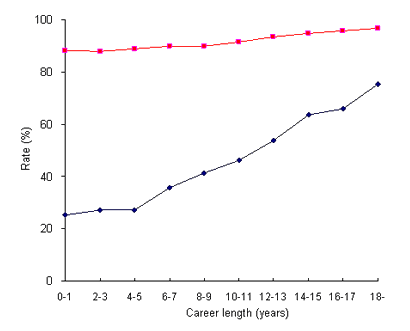
Figure 1: Stay rate of urban physicians (red line) and rural physicians (blue line) in their respective area in 2002 (according to their career length in years from the 1980 baseline).
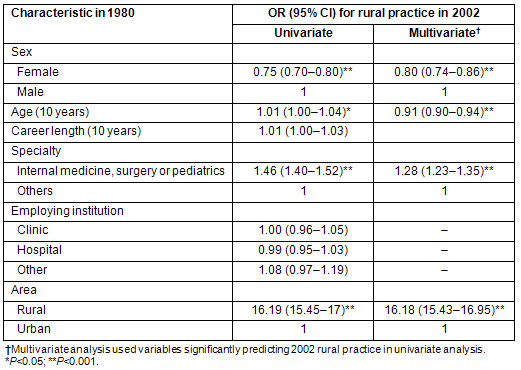
Table 3 shows the results of simple and multiple logistic regression analysis to identify variables in 1980 that predicted rural practice in 2002. In multiple logistic regression analysis, primary care discipline (internal medicine, surgery or pediatrics) and rural practice in 1980 positively predicted rural practice in 2002. However, sex (female) and age (10 years' increase) in 1980 were negative predictors of rural practice in 2002. Among these, rural practice was the strongest predictor with an odds ratio of 16.18 (15.43-16.95) over the other variables.
Table 3: Analysis of physicians' characteristics in 1980 predicting rural practice in 2002
Discussion
This study revealed that the extent of the physician maldistribution remains unchanged despite an overall increase in the number of physicians. The study also showed that physicians who spent their career in urban areas were unlikely to move to rural areas. Rural physicians were much less likely than urban physicians to have stayed in the same geographical area by follow up. However, rural practice at the 1980 baseline was a strong predictor of rural practice 22 years later, dominating the other predictors.
There are some limitations to this study. First, this study did not take into account physicians who received their physician license after the 1980 baseline year. These 'newcomer' physicians may influence the distribution of physicians examined in this study. Because the newcomer group contains more females and younger physicians than the study group it may exhibit a different distribution trend over time, which should be examined in future research. Second, due to the use of existing data, some potentially influential variables such as geographical background, marital status, family information, type of medical school, salary and workload were not analyzed. Some of these factors have been reported to be associated with rural practice8-10. Third, this study could not take into account multiple physicians' movements between urban and rural areas during the follow-up period. It would be useful to study rural physicians who had moved to an urban area but returned to a rural area by follow up. The complex answer to the question of why physicians move to other areas may only be gained through a study incorporating a detailed questionnaire or interview.
In 1970, the national government of Japan announced a plan to increase the number of physicians to the level of other developed countries (150 physicians/100 000 residents) by 1985, and predicted that the shortage of physicians in rural areas would be resolved when this goal was achieved11. For this purpose, the government established 34 new medical schools (18 national and 16 private) in the 1970s, in the hope of establishing at least one medical school in each prefecture. By placing medical schools of similar size in each part of the country, the government expected to accelerate the equitable distribution of physicians, as well as to increase the overall number of physicians11. A similar approach has been taken in the USA, according to policy-makers' 'trickle-down theory' that assumed the overall increase of physicians would intensify economic competition in urban areas and accelerate the migration of surplus physicians to medically-underserved rural areas, leading to a more even national distribution12.
The results of this study indicate this national policy did little to improve the geographic disparity of physicians. Kobayashi et al. tracked the longitudinal change in the distribution of Japanese physicians between 1980 and 1990, and found a persistent gap in the physician-to-population ratio between urban and rural areas in spite of the overall increase in the number of physicians3. Our study found the same trend has continued over the last two decades.
Also notable is that only 7.3% of urban physicians moved to rural areas, while approximately half the rural physicians were still there 22 years later. This is a phenomenon previously unreported, at least in Japan. If Newhouse's trickle-down theory holds, an increase in the number of physicians forces them to move from saturated urban markets into rural areas where jobs and profits are more easily obtained12. In fact there is evidence that the recent distribution of physicians in USA has been influenced by economic forces and there is a flow of physicians from urban to rural areas13. The movement of physicians described in this study suggests that the flow of physicians in Japan has not been influenced by market factors. Because of the much higher number of physicians in urban areas, movement of a small proportion from urban to rural resulted in a significant increase in the rural workforce and offset the loss of a large proportion of rural physicians. In the end this maintained the net gain-loss balance of the rural workforce.
There is a serious nationwide shortage of physicians in Japan. The number of physicians per unit population in Japan ranks among the fourth lowest of all 30 OECD countries14. It is thus possible that the net shortage of physicians in Japan makes even urban areas economically non-competitive, and therefore market forces do not play a part in physician distribution. Another reason for the continuing maldistribution appears to be physicians' preference for urban jobs. The proportion of rural-origin medical students in Japan is only one-third of that expected from the geographical distribution of the nation's young population15. Thus, physicians are disproportionately city residents. Urban-background medical students are more likely to aspire to an urban job, regardless of the job's conditions. There has been no quantitative study that evaluated the workload and salary of rural physicians in Japan, but it has been reported that there was little difference in satisfaction regarding salary and workload between rural and urban physicians16. The heavily urban-biased background may thus be a key determinant of the urban concentration of physicians.
The literature from other countries has also reported that the rural background of physicians is a strong predictor they will pursue a rural career17,18. Another possible contributor to the urban concentration of physicians is the increased demand for medical services in urban areas. It is presumed that technological innovation causes specialization and the diversification of medical care, leading to a concentration of patients in large or highly specialized urban hospitals and clinics. The development of transportation between urban and rural areas would facilitate this trend.
In the present study, practicing in rural areas was the most powerful predictor of future rural practice among all attributes of the physicians, and this will be a key factor in redressing the maldistribution of physicians. Physicians who were in a rural area in 1980 were 16 times more likely to be in rural area in 2002. The odds were much higher than the other physician attributes and the value was stable in both univariate and multivariate analysis. It is notable that among early-career physicians who were highly mobile, 25% of those who had been in rural areas stayed there (Fig1). Several reasons for this phenomenon can be proposed. Prior experience of rural practice may ease the psychological and technical difficulties of practicing in rural areas. In addition, settling in one place may promote financial stability, compared with relocating.
Other than rural experience, the results showed that physician factors such as a primary-care specialty, male sex, and a long professional career were most likely to influence practice in a rural area. Matsumoto et al. reported that being male, older and having a primary care specialty were positively related to the physicians' intention to continue in rural practice10. Studies from other countries also reported that primary-care physicians were most likely to practice in rural areas19-21. There are two possible reasons for this. First, primary-care physicians are more capable than other specialists of dealing with the broad range of health problems found in rural communities. Second, those who hope to practice in rural areas tend to choose primary care as a specialty15. Longer career or age is related to the 'geographical fixation' of the physicians regardless of where they practice.
In contrast, early-career physicians were more mobile than later-career physicians. However, when focusing on novice physicians whose careers were of less than 6 years duration (1979-1980, 1977-1978 and 1975-1976 in their registration year), the moving rate does not increase significantly, perhaps because these physicians are still in clinical training. Doctors-in-training usually have a temporary status, holding positions such as 'resident', which means they must move to another institution to obtain a long-term post22. Thus, the probability of moving to another geographic category would be similar for all residents until the end of their training, usually in the fifth or sixth year after graduation.
The results of this study have implications for improving the geographic maldistribution of physicians. Most teaching hospitals for postgraduate physicians are located in urban areas. The failure of teaching hospitals to recognize primary care as an established specialty in Japan disadvantages attempts to rectify the uneven distribution of physicians. The results of this study indicate that physicians who chose to practice in urban areas in the early stages of their career will have little chance of working in rural areas. A possible solution is the establishment of programs that encourage physicians, particularly early-career physicians, to experience rural practice and become primary-care specialists. Several such programs have been reported as successful in increasing the number of rural physicians20,21,23,24.
Because physician distribution is influenced by social, economic and political factors, the inclusion of factors such as where the physician grew up and their income level as explanatory variables would make a more comprehensive analysis possible. It will be interesting to continue observing the geographic trends of postgraduate physicians in rural practice.
Acknowledgement
The authors are grateful to Dr Jane Farmer for her comments on this study. This study was supported by a grant-in-aid (H16-Policy-010) from the Ministry of Health, Labour and Welfare.
References
1. Jichi Medical School. Chiiki-iryo hakusyo [White paper on community healthcare]. Tochigi: Jichi Medical School; 2002. (In Japanese)
2. Matsumoto M, Okayama M, Inoue K, Kajii E. High-tech rural clinics and hospitals in Japan: a comparison to the Japanese average. Australian Journal of Rural Health 2004; 12: 215-219.
3. Kobayashi Y, Takaki H. Geographic distribution of physicians in Japan. Lancet 1992; 340: 1391-1393.
4. Australian Medical Workforce Advisory Committee. The General Practice Workforce in Australia. Sydney, NSW: Australian Medical Workforce Advisory Committee, 2000.
5. Bureau of Health Professions. Rural health professions facts: supply and distribution of health professions in rural America. Rockville, MD: Health Resources and Services Administration, 1992.
6. Rivo ML, Kindig DA. A report card on the physician work force in the United States. New England Journal of Medicine 1996; 334: 892-896.
7. Newhouse JP, Williams AP, Bennett BW, Schwartz WB. Where have all the doctors gone? Journal of American Medical Association 1982; 247: 2392-2396.
8. Matsumoto M, Inoue K, Kajii E. Contract-based training system for rural physicians: follow-up of Jichi Medical University graduates (1978-2006). Journal of Rural Health 2008; 24: 360-368.
9. Matsumoto M, Inoue K, Kajii E. Characteristics of medical students with rural origin: Implications for selective admission policies. Health Policy 2008; 87: 194-202.
10. Matsumoto M, Okayama M, Inoue K, Kajii E. Factors associated with rural doctors' intention to continue a rural career: a survey of 3072 doctors in Japan. Australian Journal of Rural Health 2005; 13: 219-225.
11. Ministry of Health, Labour and Welfare. Ishi no jukyu ni kansuru kentoukai houkokusyo [Working party report on the national supply of physicians]. (Online) 2006. Available: http://www.mhlw.go.jp/shingi/2006/07/dl/s0728-9c.pdf (Accessed 25 March 2007). (In Japanese)
12. Newhouse JP. Geographic access to physician services. Annual Review of Public Health 1990; 11: 207-230.
13. Ricketts TC, Randolph R. Urban-rural flows of physicians. Journal of Rural Health 2007; 23: 277-285.
14. Organization for Economic Co-operation and Development. OECD health data 2006. Electronic ed. Paris: OECD, 2006.
15. Takayashiki A, Inoue K, Okayama M, Nakamura Y, Matsumoto M, Otaki J. Primary care education for undergraduates in Japan: is it enough to increase student interest in and career preference for primary care? Education for Primary Care 2007; 18: 156-164.
16. Jichi Medical School. Chiiki-iryo hakusyo [White paper on community healthcare]. Tochigi: Jichi Medical School; 2007. (In Japanese)
17. Brooks RG, Walsh M, Mardon RE, Lewis M, Clawson A. The roles of nature and nurture in the recruitment and retention of primary care physicians in rural areas: a review of the literature. Academic Medicine 2002; 77: 790-798.
18. Laven G, Wilkinson D. Rural doctors and rural backgrounds: how strong is the evidence? A systematic review. Australian Journal of Rural Health 2003; 11: 277-284.
19. Cullison S, Reid C, Colwill JM. Medical school admissions, specialty selection, and distribution of physicians. Journal of American Medical Association 1976; 235: 502-505.
20. Rabinowitz HK. Evaluation of a selective medical school admissions policy to increase the number of family physicians in rural and underserved areas. New England Journal of Medicine 1988; 319: 480-486.
21. Rabinowitz HK. Recruitment, retention, and follow-up of graduates of a program to increase the number of family physicians in rural and underserved areas. New England Journal of Medicine 1993; 328: 934-939.
22. Inoue K, Matsumoto M. Japan's new postgraduate medical training system. Clinical Teacher 2004; 1: 39-41.
23. Rosenblatt RA, Whitcomb ME, Cullen TJ, Lishner DM, Hart LG. Which medical schools produce rural physicians? Journal of American Medical Association 1992; 268: 1559-1565.
24. Inoue K, Matsumoto M, Sawada T. Evaluation of a medical school for rural doctors. Journal of Rural Health 2007; 23: 183-187.
Abstract
Introduction: The geographic maldistribution of physicians (their concentration in urban areas and shortage in rural areas) has long been an important political issue in post-war Japan. The aim of this study was to evaluate long-term transition in the geographic distribution of physicians, and to reveal which rural physician characteristics predict their retention in rural areas after 22 years.
Methods: A record-linkage study was conducted to extract a physician cohort by merging the 1980 and 2002 Physician Census in which all licensed physicians are legally required to register. Physician characteristics in 1980 that predicted rural practice in 2002 were identified.
Results: Data were used from the 93 077 physicians who were recorded in both 1980 and 2002 Physician Censuses. The number of physicians increased by 52% between 1980 and 2002. In both 1980 and 2002, the physician-to-population ratios in rural areas were approximately half that in urban areas, indicating that the physician maldistribution had not improved. In 1980, 82 414 (88.5%) physicians worked in urban areas and 10 663 (11.5%) worked in rural areas. In 2002, 76 435 (92.7%) of the 1980 urban physicians were still practicing in cities, but only 5958 (55.9%) of the 1980 rural physicians had stayed in their rural area. Logistic regression analysis showed that primary-care discipline and rural practice in 1980 positively predicted rural practice in 2002 (OR [95% CI]: 1.28 [1.23-1.35] and 16.18 [15.43-16.95], respectively). However, female sex and age in 1980 were negative predictors for rural practice in 2002 (OR [95% CI]: 0.80 [0.74-0.86] and 0.91 [0.90-0.94], respectively).
Conclusions: The rapid increase of physicians between 1980 and 2002 has not substantially affected their geographic distribution. Baseline rural practice, primary care discipline and male sex of physicians were found to be predictors of rural practice after 22 years.
Key words: Japan, medically underserved area, medical workforce, physician/distribution.
You might also be interested in:
2011 - Oral health of pre-school children in rural and remote Western Australia


