Introduction
As patients move between components of an increasingly complex Australian healthcare system, the quality of health care received by patients may be compromised by many factors, including medication misadventure1 and interrupted continuity of care2. This study addresses the combination of these factors by investigating the transfer and early application of information about older persons' current medication (or 'medication information') as patients move into aged care facilities from other healthcare settings.
Many older persons are prescribed multiple medications for chronic conditions and many experience adverse drug events3. When patients on long-term medications are admitted to hospital, their medications may be changed before discharge and the reasons for those changes are frequently not communicated to the patient's GP4. In addition, recent research suggests medication errors are common when elderly patients are discharged from hospital5 and that health literacy about medications is often limited in older patients6.
The communication of both medication and broader clinical information about aged care residents as they are transferred to the acute care sector has received attention in the literature7. However, despite the availability of guidelines for the management of medication in aged care facilities8 and recognition of the need for effective information transfer when patients move in the reverse direction9, less attention has been directed to the communication of patient medication information from acute care to the long-term aged care sector10.
The role of interprofessional team work in rural health has been emphasised11. With health professionals from a number of disciplines potentially involved in the transfer and application of medication information, activating the interprofessional team may be specifically useful in rural settings.
In addressing difficulties associated with medication information transfer to aged care facilities, a number of responses have been identified. It has been suggested that patients act as their own advocate, overseeing their individual medication reconciliation process (eg maintaining an accurate list of their own medications)10. While this approach may generally limit medication errors associated with patient transfers, its application is limited for residents of aged care facilities, a significant proportion of whom experience dementia. Electronic prescribing and information transfer have also been suggested12. However, while this may be a future solution, the focus of this article is on current practices in rural Australia, where electronic approaches are yet to be fully developed, standardised and introduced.
Aim
This rural Australian pilot study had two aims: (i) to investigate how medication information about patients admitted to an aged care facility was communicated; and (ii) to investigate the administration of prescribed medications to patients following their admission, including delays to the first scheduled dose in that facility.
Method
An observational study was undertaken over a 3 month period during 2007 in a rural Australian setting with a catchment population of 130 000. Outcomes for patients being admitted to residential aged care facilities, and the experiences of nurses involved in their admission were investigated. Patients came from an acute hospital, a rehabilitation facility, another aged care facility or the community. One senior nurse was recruited from each of the region's 22 aged care facilities, and these nurses recruited patients into the study.
Patients' permission was obtained for the nurse to complete a questionnaire about the details of their admission to the facility. If the nurse considered a patient to be cognitively impaired, consent was sought from the patient's nominated responsible person. Research ethics approval for the project was provided by the regional health service.
The data, gathered within 7 days of the patient's admission, was predominantly derived from the patient's medical/nursing record. This was supplemented, if required, by information supplied by the admitting nurse/s. A customised questionnaire was developed for the study in consultation with the local division of general practice aged care interest group. In addition to limited demographic information, it included questions about the circumstances of the patient's transfer, questions about the patient's medication information transfer and initial administration, and questions about staff actions to ensure timely medication administration to that patient.
Results
Questionnaires relating to 59 individual patient transfers were received from 14 aged care facilities. All questionnaires were completed by a senior nurse. More than two-thirds of the questionnaires were completed within 2 days of the patient's admission to the facility.
Almost 60% of patients were admitted to high-level care facilities (nursing homes), and the remainder to low-level care facilities (hostels). Most patients were female (39/59), aged over 80 years (40/59) and assessed by the nurse as cognitively impaired (38/59). Thirteen of the patients were admitted to the aged care facility directly from the community, nine from another aged care facility and the remainder from an acute hospital or rehabilitation unit.
Medication information transfer
A number of pathways used to communicate medication information were identified. Two out of three patients (38/59) arrived at the aged care facility with written medication information. Medication information was also sent to aged care facilities separately as part of a hospital discharge summary, by fax from a community pharmacy or the patient's GP, or by direct (phone) contact from either hospital staff or the patient's GP. Medication information about a number of patients was transferred using more than one pathway. For a small number of patients (4/59), no specific information about prescribed medication was received in any format by the aged care facility by the time of questionnaire completion (Table 1).
Table 1: Reported medication information transfer pathways
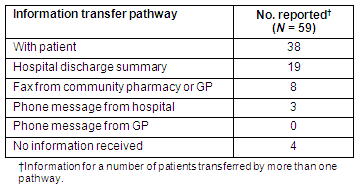
Preparation for patient arrival
Most patient transfers were associated with at least 12 hours notice to the aged care facility and occurred during routine week-day working hours. However some patients (7/59) arrived with no more than one hour of warning, and three of these patients arrived with no warning. Twice as many patients were transferred on Tuesday and on Friday than on any other week day. However, only two patients were transferred after 5 pm on Friday.
Administration of medication after admission
Following admission most patients (41/59) received their medication/s without delay. However, a number of patients (12/59) experienced a delay of up to 4 hours and two patients experienced a delay of more than 7 hours (Table 2). Reported reasons for delays included a medication chart not being signed by a doctor, and required medications not being available at the aged care facility. However, the single most commonly reported reason for delay, affecting seven patients, was that medications had not been written on the medication chart used in that aged care facility.
Table 2: Reported delay in administration of first scheduled medication dose following transfer to aged care facility
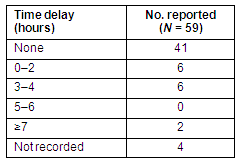
Variation from usual practice
Following admission to an aged care facility, patients' medication charts were most often completed by the patient's GP during a visit to the facility. However, five instances were reported of an aged care facility's staff member taking a medication chart to the clinic of the patient's GP for a signature, and a similar three instances were reported when this was done by members of the patient's family. A number of registered nursing staff reported that they had to act beyond their normal employee duties to ensure timely medication administration to their aged care residents, or that such an action had been required of a colleague.
Discussion
This research focused on outcomes for patients being admitted to residential aged care facilities and the experiences of the nurses involved in theses admission. Hospital medical staff, GPs, nurses and pharmacists were involved in the transfer and application of medication information, highlighting the need for cooperation among the health professionals involved in the process. Appropriate patient discharge and transfer policies may facilitate this.
Previous research has focused specifically on the transfer of medication information, with less consideration of the immediate application of this information. This study highlights the need for effective information transfer and effective processes for the immediate application of that information. Growth in electronic prescribing has the potential to facilitate more effective prescribed medication information transfer, but not necessarily the timely response to that information. While both the impact and time frame of widespread future electronic medication information transfer remains unclear, the present research supports attention being directed to both current mechanisms for medication information transmission and medication administration.
This study was undertaken in a defined rural setting, served by one public and one private hospital. In this context, an established single pathway agreed to by local participants, rather than the range of pathways and multiple pathways for individual patients that were identified, might have been expected. It has been argued that medication should be transferred by as many routes as possible9. However, an effective single default pathway for medication information transfer should be regarded as the ideal, minimising adverse outcomes associated with the potential confusion resulting from a range of possible pathways. Such a default single pathway could be backed up by additional supplementary pathways, if appropriate, specific to local circumstances. Defined rural areas, with the likelihood of established personal communication links among key health professionals, may be an ideal setting for the implementation of a locally acceptable and effective single pathway. In this study medication information was most often transferred with the patient in written form. This would seem an appropriate single pathway for immediate use while waiting for the implementation of electronic mechanisms. This could be supplemented by concurrent forwarding of information to the relevant community pharmacist, if appropriate.
In this study medication information was received in a timely manner. However, for this to result in seamless administration of medication the facility must have the capacity to apply the information it receives. Few rural Australian aged care facilities have a resident pharmacist, pharmacy or medical staff, with most relying on visiting pharmacists and GPs13. Adequate warning of the arrival of a new patient, efficient pharmacy links and a timely response from responsible medical staff are required for seamless medication administration to occur. In this study, aged care facilities received adequate warning of most patient arrivals, although more than one in ten patients arrived with no more than one hour of warning, a time frame that has the potential to result in delayed medication administration. Little evidence was found in this study to suggest that patients were being returned to aged care facilities from acute hospitals immediately before the weekend.
Elderly patients are more likely than younger patients to experience difficulties with medications14. It is therefore of concern that while most patients received medication without delay, a number experienced a delay of a number of hours before receiving initial medications. The most commonly reported reason for delay in administration of medication was that the medications were not written on the correct drug chart. This may relate to meticulous but inflexible protocols linked to staff concerns about aged care facility accreditation. This and other reported reasons for delay, including medications not being available and the drug chart not being signed by the doctor, may have greater potential to be addressed in rural than urban settings if links between key health care stakeholders are utilised. Creative local responses to identified barriers that limit ideal medication information transfer and administration should be encouraged by health service providers.
A number of aged care staff reported that they and/or their colleagues had acted outside their designated role to ensure timely medication administration to their patients. While taking medication forms to GPs' clinics for signature may be regarded as laudable commitment by nurses trying to 'keep the system going', it is also an inefficient use of professional nursing staff time. Such actions are likely to be unofficial responses by individual staff. As with other identified barriers to ideal care, alternative arrangements developed at a local level may avoid this and similar practices that do not optimise limited staff capacity.
Addressing some of the noted barriers may require all healthcare participants (nursing staff, hospital resident medical officers, GPs and pharmacists) to be more aware of the legal responsibilities and limitations of both their own and other healthcare professionals. For example, GPs may be unaware that pharmacists may not dispense from a faxed prescription. Given the diversity of settings in the rural aged care sector (ranging from the patient, nurse, GP and pharmacist being co-located in the one building to each of these being separated by significant time and distance), a customised approach may be needed for each setting. However, this study supports at least one common approach, that medication information should move (in hard copy or electronic format) with the patient as they move into an aged care facility. The ideal response to that information may best be achieved by locally developed and implemented protocols. It is a disservice to current patients to assume that all medication information transfer difficulties for aged care residents will be solved by future technology.
This research project was limited by its restriction to one rural location, data being available from only two-thirds of the aged care facilities in that region, and data from health professionals other than nurses not being available. In addition, the collection of data was constrained by dependence on nursing staff to complete questionnaires; it was not possible to determine if nursing staff were selective in the patients they included. Data collection that ensures access to information on all admissions and that is independent of the nurses who provide clinical care should be considered in future, similar work. Notwithstanding these limitations, the findings should encourage further research and stimulate review of local practices.
Conclusions
This study encourages a review of current mechanisms used to transfer medication information about patients being admitted to aged care facilities and the immediate application of that information. Health professionals in rural Australia may be in a good position to utilise links between key health care stakeholders to develop and implement effective local responses to identified barriers. In addressing the problems identified in this study, health professionals may both facilitate better health care now and more effective future implementation of electronic prescribing approaches.
Acknowledgements
This research was assisted by the Primary Health Care Research, Evaluation and Development program funded by the Australian Government.
References
1. Roughead E, Gilbert A, Primrose J, Sansom L. Drug-related hospital admissions: a review of Australian studies published 1988-1996. Medical Journal of Australia 1998; 168: 405-408.
2. Mant A, Kehoe L, Cockayne N, Kaye K, Rotem W. A quality use of medicines program for continuity of care in therapeutics from hospital to community. Medical Journal of Australia 2002; 177(1): 32-34.
3. Gurwitz J, Field T, Harrold L, Rothschild J, Debellis K, Seger A et al. Incidence and preventability of adverse drug events among older persons in the ambulatory setting. JAMA 2003; 289(9): 1107-1116.
4. Himmel W, Tabache M, Kochen M M. What happens to long-term medication when general practice patients are referred to hospital? European Journal of Pharmacology 1996; 50: 253-257.
5. Midlov P, Holmdahl L, Eriksson T, Bergkvist A, Ljungberg B, Widner H et al. Medication report reduces number of medication errors when elderly patients are discharged from hospital. Pharmacy World and Science 2008; 30: 92-98.
6. Simon S, Gurwitz G. Drug therapy in the elderly: improving quality and access. Clinical Pharmacology and Therapeutics 2003; 73: 387-393.
7. Finn J C, Flicker L, Mackenzie E, Jacobs I G, Fatovich D M, Drummond S et al. Interface between residential aged care facilities and a teaching hospital emergency department in Western Australia. Medical Journal of Australia 2006; 184(9): 432-435.
8. Australian Pharmaceutical Advisory Council. Guidelines for medication management in residential aged care facilities, 3rd edn. Canberra: Australian Government, 2002.
9. Hilmer S, Ogle S. Discharge medication. Australian Prescriber 2006; 29(3): 58-59.
10. Barnsteiner J H. Medication reconciliation: transfer of medication information across settings - keeping it free from error. American Journal of Nursing 2005; 105(3Suppl): 31-36.
11. Bourke L, Sheridan C, Russell U, Jones G, DeWitt D, Liaw S T. Developing a conceptual understanding of health practice. Australian Journal of Rural Health 2004; 12(5): 181-186.
12. Bollen C, Warren J, Whenan G. Introduction of electronic prescribing in an aged care facility. Australian Family Physician 2005; 34(4): 283-286.
13. Gadzhanova S, Reed R. Medical services provided by general practitioners in residential aged-care facilities in Australia. Medical Journal of Australia 2007; 187(2): 92-94.
14. Herman R. Drug therapy consideration in the elderly. South Africa Medical Journal 1982; 61: 544-546.
Abstract
Introduction:
As patients move within Australia's increasingly complex healthcare system, it is desirable that they receive uninterrupted, timely and accurate administration of medication. For this to occur, effective communication of medication information is required, and mechanisms must be in place to ensure timely administration. This study focused on these issues as they apply to patients being admitted to aged care facilities in an Australian rural setting, including investigation of the transfer and early application of information about their current medications (or 'medication information'). Electronic prescribing and associated information transfer may improve the transfer of medication information in the future; however, this study focused on the current situation in rural Australia.Method: In this observational study, patient outcomes and participating nurses' experience of medication issues related to admissions to rural residential aged care facilities from an acute hospital, a rehabilitation facility, another aged care facility or the community were investigated. Data were collected using a customised questionnaire completed by nursing staff at participating aged care facilities.
Results: Data relating to 59 individual patient transfers were obtained from 14 aged care facilities. A number of pathways for the communication of medication information were identified, with timely and effective information transfer occurring for most patients. However, one in five patients experienced a delay of up to 4 hours, and a limited number of incidents of inadequate information transfer were identified. While most patient transfers occurred with 12 or more hours notice, one in ten transfers occurred with no more than one hour of notice. Transfers were not evenly distributed among week days; however, very few transfers occurred after 5 pm on Friday. A number of staff reported that they had felt it necessary to act beyond their normal employee duties to ensure timely medication delivery to their aged care residents.
Conclusions: This study identified pathways used to transfer medication information about patients being admitted to aged care facilities, and also immediate responses to that information. The study indicates that these processes, while generally satisfactory, are at times less than ideal. Health professionals in rural Australia may be in an ideal position to develop and implement effective local responses to identified problems, by activating interprofessional links. The study also highlights the issue of aged care staff acting outside their designated role in an attempt to ensure timely medication administration to their patients, a potentially inefficient use of limited staff time.
Key words: aged care, Australia, interprofessional links, medication information.
