Introduction
The past two decades have seen numerous changes in the delivery of maternity care in Australia including: the introduction of birth centres and midwifery models of care (although not yet available to all women), various shared care arrangements and early discharge. In the state of Victoria, the Victorian Surveys of Recent Mothers, a series of large population surveys conducted in 1989, 1994 and 20001 highlighted these changes and how they were experienced by women. The results have provided a rich source of data that have been presented in numerous studies and used to design interventions to evaluate care and lobby for change. For example the surveys revealed areas of dissatisfaction with care shared between hospitals and GPs, resulting in changes which significantly improved satisfaction in subsequent reviews2,3. A further population study is underway and for the first time this includes South Australian as well as Victorian women4. However, when the present study was undertaken such detailed data about women's views and experiences of their maternity care had not been collected in rural populations in South Australia. The South Australian perinatal statistics collections provide comprehensive demographic and outcome data; however, responses by women about aspects of their care have not been collected5.
In planning the evaluation of a new partnership model of care provided by Aboriginal Maternal Infant Care workers and midwives6-8, the researchers followed Campbell and Brown6, who modified the Victorian survey questions for Aboriginal women and compared responses with all Victorian rural residents. The aim of the present study was to use selected data from rural women for comparison with that of a sample of Aboriginal women who received care in that program, reported elsewhere6-8. As the research plan progressed it became clear that a survey of rural women was timely and could progress as research in its own right. The decision was made to aim for a sample of up to 100 women. A subsample of 54 was used for comparison with the Aboriginal women who participated in the partnership model7.
The overall study aim was to assess the views and experiences of a sample of women who gave birth in three regional hospitals, hospitals A, B, and C. These hospitals delivered 888 of 5257 births (16.9 %) to South Australian women of rural residence in 2006, and 4.8% of 18 519 South Australian births overall5.
At the time of the study non-Aboriginal women who gave birth at hospitals A and C received one of four models of antenatal care: (i) GP and obstetrician shared care; (ii) GP and midwife shared care; (iii) midwife-only care; and/or (iv) a combination of these. Generally an obstetrician was involved only if the pregnancy became high risk. Women who had midwife-only care were initially screened as free from risk factors and transferred to other care if risks emerged. All hospitals utilised GP/obstetricians and midwives during labour and birth for women of low risk. Hospitals A and C had access to an obstetrician if required in labour, and also provided visits from community midwives after discharge home. At the time, hospital B differed in the provision of midwifery care: it provided neither midwife-only antenatal care nor home visits from a community midwife in the postnatal period. There are no private hospitals in the regions studied and privately insured women normally received their birthing and postnatal care in the regional hospital. Birthing centre care was not an available option at any of the study hospitals.
Survey questions sought the following information:
- demographic detail, such as age, parity and birth outcomes
- practices that may affect birth outcome (eg smoking)
- model of pregnancy and birth care
- women's ratings of their care during pregnancy, labour and after birth
- breastfeeding rates in the first week at home and at 6 weeks postpartum
- rates of likely depression after birth at 6 weeks postpartum
As in the Victorian surveys the 10 item Edinburgh Postnatal Depression Scale (EPDS) was used; it was designed for self-administration to screen for likely postnatal depression9. The EPDS has been validated for use in Australian populations with excellent sensitivity and specificity9,10, and has been in used extensively in Australian or international research11,12.
Where, appropriate, demographic and outcome data from the study were compared with routinely collected data from the South Australian Pregnancy Outcome Unit5.
Methods
University human research and ethics approval was obtained and three hospitals gave consent to enrol women into the study from their postnatal wards. Consenting women were mailed questionnaires 6-8 weeks after the birth.
Developed and validated specifically for the Victorian population surveys1 and slightly modified for use with rural South Australian women, the survey was segmented into sections that included questions about demographic data, and the three domains of antenatal; labour and birth; and postnatal care. At the end of each section open-ended questions invited women to comment further on aspects of the domains with which they were either happy or unhappy; or found helpful or unhelpful, as well as a generic response for overall care (n = 4). Three further questions invited women to comment on the need for further information in labour and birth; help and/or advice women would have liked postnatally; and an overall 'anything else to add' question.
Between December 2005 and November 2006, three researchers approached women in hospital after the birth of their baby and invited them to participate in the study. Interested women received a detailed oral explanation of the study and were given an information sheet. Those women who agreed to participate completed a consent form. We obtained consent to contact the women for the purpose of clarification and in cases where there were any issues; this included a referral to their GP.
At 6 to 8 weeks after the birth a questionnaire was mailed to consenting women. Where there was no response within 6 weeks of sending the questionnaire, the women were contacted to ensure they received the questionnaire and that they still wished to participate; in some cases a second questionnaire was then sent. If no response was gained from this it was assumed the woman was no longer interested and no further contact was made.
Although three hospitals approved the research, the researcher at hospital C was unable to continue due to a change of employment after enrolling only two participants; it was not possible to gain a replacement. Data from the two women from hospital C were included in the results.
Non-identifiable data were entered into a database developed using Statistical Package for Social Sciences (SPSS) v15 (SPSS Inc; Chicago, IL, USA). Data were analysed using descriptive statistics and t-tests, as well as 2 x 2 contingency tables and relative risks, where appropriate, using the StatCalc facility of Epi Info v3.4.2 (CDC; Atlanta, GA, USA), a public domain statistical package for use in population research. For the open-ended questions, themes were developed and agreed by consensus13.
Results
Although data were not formally collected, the number of women at all sites who declined participation was negligible. Of the 136 women who consented to participation, 85 (63%) returned a completed questionnaire. One woman had been transferred from a metropolitan hospital for her postnatal care.
The number of births conducted at the 3 hospitals in 2006 are given, as are the numbers and percentages of participants enrolled at each hospital (Table 1). The births at the 3 hospitals are also presented as percentages of the total births in South Australia (Table 1).
Table 2 presents the age ranges, health insurance and parity of the women in the study. For 33 women (40%) this was their first baby. The age mode was shared by women aged between 25 and 29 years (15%) and 30-34 years (15%). Thirty women (36%) had private health insurance, usually with a GP/obstetrician.
Among the 18 519 births to women in South Australia in 2006, 5257 (28.4%) lived in a rural area2. Rates of spontaneous vaginal birth for the study sample were lower than that of the combined rural residents, 38% versus 58% (RR 0.77 [0.61-0.97], p = 0.01; Table 3). Although there was a definite trend, no significant difference was found in the total caesarean section rate between the study group (40%) and rural residents (31%; RR 1.27 [0.98-1.66], p = 0.10; Table 3). Neither was there any difference in comparison with South Australian births overall (33%; RR 1.36 [0.88-2.09], p = 0.2)2. 'Elective' is the term used to describe a planned caesarean section delivery, while 'emergency' describes a planned vaginal birth that results in a caesarean. Study participants had a significantly higher rate of elective caesarean section (25%) when compared with rural residents (16%; [RR 1.53, 1.05-2.23], p = 0.05; Table 3). Fewer study women smoked throughout pregnancy (8 of 85 [9%] vs 1238 of 5237 [24%] of rural residents [RR 0.40, 0.21-0.77], p = 0.002; Table 3).
Table 1: Births in participating hospitals in 2006, and study return proportions

Table 2: Participants' status according to age, parity and hospital insurance
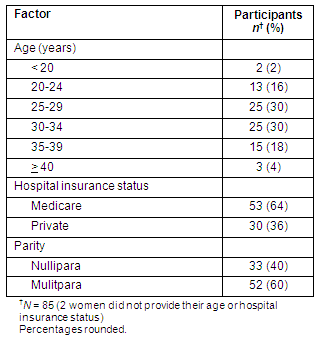
Table 3: Method of birth and smoking status: study group versus rural residents in South Australia, 2006
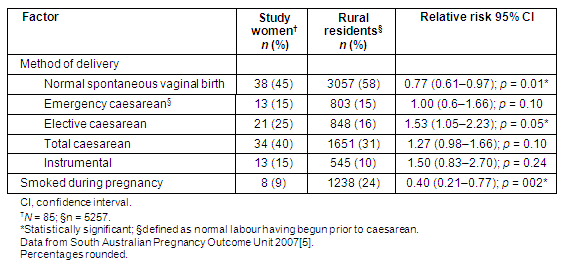
The birth weights of babies in the study ranged from 2270 to 4082 g (mean 3154 g). The models of care used varied among sites and within individual locations. The majority of women (58 of 81, 72%) for whom data were provided received care shared between their GP and midwives, compared with 23 of 81 (28%) who had midwife-only care. While more of those who had midwife-only care rated their antenatal care as 'very good', the difference was not statistically significant (16 of 23 [70%] vs 30 of 58 [52%]; RR 1.74, 0.88-3.76, p = 0.2).
Women were invited to rate their overall antenatal; labour and birth; and postnatal care as 'very good', 'good', 'mixed', 'poor' or 'very poor'. A rating of 'very good' indicates a high level of satisfaction3. Fifty-nine percent of women rated their care as 'very good' during the antenatal period; 73% during labour and birth; and (52%) postnatally, followed by 'good' at 35%, 23% and 29%, respectively (Table 4). The response 'mixed' which indicates low satisfaction3 was more prevalent for postnatal care (18%) than for labour and birth (4%), or antenatal care (5%). Of the women whose response to their postnatal care question was 'mixed', 12 of 15 (80%) provided further comments with specific concerns. These are summarised as: being left to 'fend for themselves' (n = 7), having negative experiences with a staff member (n = 4), and being given conflicting advice (n = 2). When asked how they viewed their maternity care overall, most women (60 of 85; 71%) responded positively. A further 55 of 85 (65%) indicated that there were no aspects of their care with which they were unhappy. For example one woman stated 'midwives were always available, always encouraging and were also kind', while another felt that a positive aspect was being 'monitored the whole time'. Some women provided comments about specific issues with which they were unhappy. One women was unhappy with 'not being given a clear picture as to why my labour was not progressing to possibly avoid a "caesar"', and another who had a caesarean delivery commented about the 'number of people in the theatre that I didn't know or think really needed to be there'. Responses from the 30 women who were privately insured when compared with the 55 women with Medicare-only (the Australian government-funded national healthcare system) cover revealed no differences in any of the ratings of care.
Significantly more women in this study stayed in hospital for 5 or more days, compared with South Australian women overall in 2006 (45 of 85 [53%] vs 5295 of 18 519 [40%], RR 1.85 [95% CI 1.51-2.27], p = 0.0000014). When asked their opinion about length of stay, 73 of 85 women (86%) indicated that this was 'about right'. When additional open-ended questions were analysed, 60 women (71%) provided personal choice reasons for going home. Many of the women used the word 'ready' or the phrase 'other children at home' when explaining their reason for going home, with one woman stating 'other children at home [and], husband not coping well!!' Another woman's reason for going home was 'the ward got very busy and I was left to my own devices anyway'.
Breastfeeding was commenced by 81 of the 85 women (95%; Table 5). Women were asked whether they were breastfeeding in their first week at home and again at 6 weeks after the birth. Seventy of the total sample (82%) were breastfeeding during their first week at home, and 59 of the sample (69%) were still breastfeeding at 6 weeks (Table 5). When rates of breastfeeding for hospital and privately insured women were compared there were no differences identified at any assessment points.
Table 4: Women's ratings of antenatal, intra-partum and postnatal care
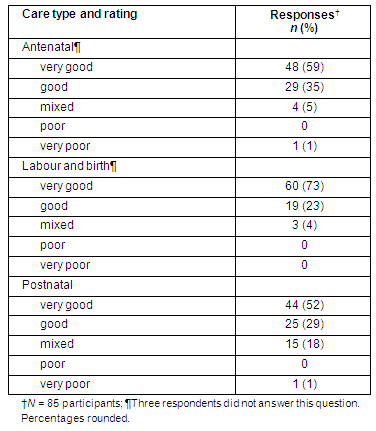
Table 5: Status according to having commenced breastfeeding and breastfeeding during the first week at home and at 6 weeks postpartum; and Edinburgh Postnatal Depression Scale score of >12 at 6 weeks postpartum
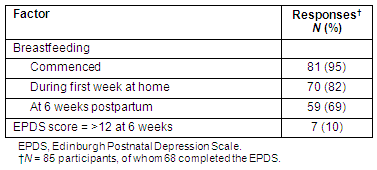
Not every woman chose to complete the EPDS. Among the 68 respondents (80%) who did, 10% scored >12 (indicative of probable major depression; Table 5). If a woman's EPDS score was of concern a phone call was made to her to offer referral for further care.
Discussion
Our investigation makes a contribution to the literature on rural women's views of their birthing care in South Australia; at the time of the study this type of research had not been undertaken in such a population. The participants comprised 17% of 301 and 14% of 285 women who gave birth at hospitals A and B, respectively, during 2006. As such, the participants are likely to be reasonably representative of the total population. The study design is robust, using a well-validated structured questionnaire developed by a team of experienced Australian perinatal researchers, used previously with thousands of women and allowing the examination of complex data and associations.
One possible study limitation is that the sample size may be under-powered to make comparisons among smaller sub-groups (such as those with private health insurance and midwife-only care models) as was possible in the larger Victorian surveys. In addition, the regional hospital settings may not be representative of other rural or remote South Australian locations. The state-wide population survey currently in progress contacts women at 6 months after the birth and uses the Victorian questionnaire and, as such, will have sufficient power to make a wider range of comparisons4.
Consideration must be given to the possibility that the timing of the assessment (at 6-8 weeks after birth) may have influenced women's views. Some may have been experiencing a 'halo effect', in which positive effects are emphasised due to invoked heightened emotions which may lessen a few months later14. The 6-8 week time frame was chosen for this study because it was felt that women approached in hospital after the birth were more likely to remember consenting to the study, and less likely to have moved house and so lost to follow up.
The study's breastfeeding rates are comparable with other rural Victorian and rural South Australian data. For example, compared with the women in the 2000 Victorian survey of recent mothers, the numbers of women breastfeeding in their first week at home were 70 of 85 (82%) versus 396 of 447 (88.6%; RR 0.97, 95% CI 0.87-1.08)13. When compared with a small study undertaken in an adjoining rural area15, the study's breastfeeding rate at 6 weeks was 69% versus 73% (RR 1.13, 95% CI 0.94-1.36). Higher rates of breastfeeding have been found in women of higher socioeconomic status16, for which private health insurance may be a surrogate measure. There were no such differences found in this study; however, the sample size may not have been large enough to show this (type 2 error).
A hospital stay of longer than 5 days was significantly higher in the study group. Responses demonstrated that the length of stay was what women desired: 86% highlighted that their length of stay was 'about right' with 70% providing 'further reasons' that indicated the women had elected to stay this length of time.
Women who had midwife-only care rated their antenatal care as 'very good' (RR 1.74, 0.88-3.76; p = 0.2) which is indicative of a moderate effect size; given the lack of study power, this is likely to be a clinically, if not statistically, significant difference. This question may be answered more definitively by the state-wide survey.
The study also supports the striking finding in the Victorian survey that fewer rural women rated their postnatal care as 'very good' (study 52% vs Victorian rural 55%) when compared with antenatal (59% vs 63%) and intrapartum care (73% vs 75%)13. Furthermore, in a trial of team midwifery in Melbourne, Victoria, although team midwife care was associated with increased satisfaction, this was least noticeable for postnatal care14. Lower ratings for postnatal care are not confined to Australian childbearing women. Another study undertaken in the UK found that midwife intervention improved satisfaction in all areas except postnatal care17. Qualitative data from open-ended questions confirmed that postnatal care left room for improvement. Unlike the Victorian study, the present study did not uncover differences between privately insured and Medicare-only care, although the present study may have lacked the power to reveal this. It is also possible that the lack of a private hospital and/or access to a private obstetrician may have diluted potential differences in care between privately and Medicare-insured women.
An earlier South Australian study of 222 urban women found that 9% scored >12 using the EPDS at 6 weeks postpartum18. Our study finding of 10% of the rural sample is similar. Why 20% of the women chose not to complete the EPDS is unclear.
Although the combined caesarean section rates were not significantly different for women in the present study and the rural South Australian residents2, there was a trend towards a higher rate in the study, and a significantly lower rate of spontaneous normal vaginal birth (Table 3). The higher rate of elective caesarean section in the study sample may indicate less willingness on the part of clinicians or women to undergo a trial of labour in a regional setting, particularly as one of the hospitals did not have a resident obstetrician; however, this finding warrants further investigation.
Results from the state-wide survey of South Australian women using the same survey instrument are awaited as an opportunity to provide broader insights into, and comparisons with, our findings.
Acknowledgements
The authors acknowledge Professor Judith Lumley and Associate Professor Stephanie Brown for permission to use and modify the Victorian Recent Mothers' Questionnaire. Stephanie Brown provided helpful comments on drafts of this manuscript. Also thanked are Pauline Zanet who was originally a researcher on this study, and the midwives and staff on the postnatal wards for their support of the study. Thanks also to the directors of nursing at the three regional hospitals for permission to approach women to enrol them in the study. The authors also acknowledge Associate Professor Annabelle Chan and the Pregnancy Outcome Unit, SA Health, Government of South Australia for provision of additional data on rural residents. Finally, the authors thank the women who participated in the study during their busy time as the mothers of young babies.
References
1. Brown S, Darcy M-A, Bruinsma F. Having a baby in Victoria 1989-2000: continuity and change in the decade following the Victorian Ministerial Review of Birthing Services. Australian and New Zealand Journal of Public Health 2002; 26: 242-250.
2. Brown S, Lumley J, Small R, Astbury J. Missing voices: the experience of motherhood. Melbourne, VIC: Oxford University Press, 1994.
3. Brown S, Lumley J. Changing childbirth: lessons from an Australian survey of 1336 women. British Journal of Obstetrics and Gynaecology 1998; 105: 143-155.
4. Mothers and Childrens Research Institute. Healthy Mothers Health Families Newsletter: A population-based survey of recent mothers in South Australia. (Online) 2008. Available: http://www.mcri.edu.au/Downloads/HMHF/SA_HMHF_January.pdf (Accessed 25 June 2009).
5. Chan A, Scott J, Anh-Minh Nguyen, Kean R. Pregnancy outcome in South Australia in 2006. Adelaide, SA: Pregnancy Outcome Unit, SA Health, Government of South Australia, 2007.
6. Campbell S, Brown S. Maternity care with the Women's Business Service at the Mildura Aboriginal Health Service. Australian and New Zealand Journal of Public Health 2004; 28: 376-382.
7. Stamp G, Champion S, Zanet P, Anderson G, Coulthard K, Paige K et al. Regional Family Birthing and Anangu Bibi Birthing Program: the first 50 births. Whyalla, SA: Spencer Gulf Rural Health School, 2007.
8. Stamp GE, Champion S, Anderson G, Warren B, Stuart-Butler D, Doolan J et al. Aboriginal maternal infant care workers, partners in caring for Aboriginal mothers and babies. Rural and Remote Health 8: 883. (Online) 2008. Available: www.rrh.org.au (Accessed 22 June 2009).
9. Cox JL, Holden JM, Sagovsky R. Detection of postnatal depression: development of the 10 item Edinburgh Postnatal Depression Scale. British Journal of Psychiatry 1987; 150: 782-786.
10. Boyce P, Stubbs J, Todd A. The Edinburgh Postnatal Depression Scale: validation for an Australian sample. Australian and New Zealand Journal of Psychiatry 1993; 27: 472-476.
11. Brown S, Lumley J. Physical health problems after childbirth and maternal depression at six to seven months postpartum. British Journal of Obstetrics and Gynaecology 2000; 107: 1194-1201.
12. Brown S, Lumley J. The 1993 Survey of Recent Mothers: issues in survey design, analysis and influencing policy. International Journal for Quality in Health Care 1997; 9: 265-275.
13. D'Arcy M-A, Brown S, Bruinsma F, Lumley J. Victorian Survey of Recent Mothers 2000. 5. Having a baby in metropolitan and rural Victoria. Melbourne, Vic: Centre for the Study of Mothers' and Children's Health, La Trobe University, 2001.
14. Waldenstrom U, Brown S, McLachlan H, Forster D, Brennecke S. Does team midwife care increase satisfaction with antenatal, intrapartum, and postpartum care? A randomized controlled trial. Birth 2000; 27(3): 156-167.
15. Stamp GE, Casanova HT. A breastfeeding study in a rural population in South Australia. Rural and Remote Health 6: 495. (Online) 2006. Available: www.rrh.org.au (Accessed 22 June 2009).
16. Donath S, Amir LH. Rates of breastfeeding in Australia by state and socio-economic status: evidence from the 1995 National Health Survey. Journal of Paediatric and Child Health 2000; 36(2): 164-168.
17. MacArthur C, Winter HR, Bick DE, Lilford RJ, Lancashire RJ, Knowles H et al. Redesigning postnatal care: a randomised controlled trial of protocol-based-midwifery-led care focused on individual women's physical and psychological health needs. Health Technology Assessment 2003; 7(37): 1-98.
18. Stamp GE, Crowther CA. Postnatal Depression: a South Australian prospective survey. Australian and New Zealand Journal of Obstetrics and Gynaecology 1994; 34(2): 164-167.
Published 15 July 2009; modified 8 October 2009.
A correction was made to the second author's institutional affiliation.

