Introduction
Medical practice in Japan has recently changed due to factors such as an increasing numbers of lawsuits1-3, the establishment of a new medical residency system4-6, and an uneven distribution of doctors7,8. The consequent collapse of the medical system in regional medical centers has become a social issue, especially in rural and remote areas9-11. Hematologic treatments, including intensive chemotherapy and stem-cell transplantation, are usually performed in regional centers because the treatments are high risk and the patients require the cooperative treatment of other specialist physicians12,13. Hematologists in Japan's rural and remote areas have had difficulty in maintaining their practices during the last decade14 while the number of patients with malignant diseases has been increasing15, creating the possibility that patients with hematological malignancies in rural and remote areas may not receive standard medical treatment.
In Japan, prefectures are the large local governing units that control municipalities such as cities, towns and villages. A secondary medical area consists of several municipalities and is expected to provide general medical care for inpatients in its own area (Fig1C). Tokushima Prefecture in western Japan (Fig1A) has some interesting features in relation to medical supply and demand. In 2006 the number of doctors per 100 000 people was the second largest (270.1) in Japan16. However, the Tokushima Prefectural Government commenced a doctors' registration system called 'Doctor Bank' and developed a Department of Rural Medicine in the University of Tokushima Faculty of Medicine to address the lack of doctors17,18. Tokushima Prefecture also faced issues common in the Japanese social system, such as over- and under-population, and an aging population19. Its total population (805 028 persons), proportion of migrants from other prefectures per year (3.2%), and total area (4146.55 km2) were all small in comparison with the medians of all other Japanese prefectures (1 738 000 persons, 3.7% and 5761.15 km2, respectively)20,21.
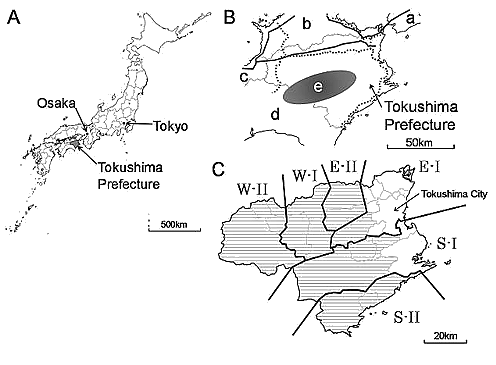
Figure 1: Tokushima Prefecture in western Japan (1A) and secondary medical areas. Tokushima Prefecture is surrounded by Hyogo (1B; a), Kagawa (b), Ehime (c) and Kochi (d) Prefectures. A mountainous region occurs mid-Tokushima (e). There are 6 secondary medical areas (1C): E-I, east-I; E-II, east-II; W-I, west-I; W-II: west-II; S-I, south-I; and S-II, south-II medical areas. Bold lines (1B) = expressways; dotted lines = railways. Shading (1C) shows legally determined rural areas.
This pilot study reports on the regional medical supply and demand for patients with hematological malignancies in Tokushima Prefecture.
Methods
Patients
The number of patients in Tokushima Prefecture with newly diagnosed leukemia, malignant lymphoma and multiple myeloma, and their zip codes, was determined in 2006 by survey. Patients who transferred from centers in other prefectures were excluded from the study.
The number of patients with newly developed hematologic malignancies was then estimated for each municipality and secondary medical area, based on population and incidence of disease by age group15.
For the purposes of this study, the 7 Tokushima regional hospitals with hematology departments with inpatient beds were defined as core hematologic centers. The home zip codes of identified patients hospitalized for the first time in one of these 7 centers for treatment of hematological malignancy were determined.
Survey of hematologist numbers
The physicians of departments of hematology in hospitals or clinics were defined 'hematologists' in this study. The number of these hematologists was determined by survey of core hematologic centers' websites, or by telephone. The hospital addresses of part-time hematologists were also collected in order to take into account the unique Japanese 'Ikyoku' system where medical care in rural areas is supported by part-time physicians mainly affiliated with medical schools22,23.
Definition of rural and urban areas
According to the legal Japanese determination24, an area is defined as rural according to population and financial factors. Population factors include the rate of: (i) decrease being greater than 30% for the period 1965-2000; (ii) decrease being greater than 25% and the proportion of elderly people (aged over 65 years) being greater than 24% for the period 1965-2000; (iii) decrease being greater than 25% and the proportion of young people (>15 and <30 years) and less than 15% for the period 1965-2000; and (iv) decrease being greater than 19% for the period 1970-2005. Financial factors included the mean value of the financial power index (the ratio of total financial income to total financial demand25) in the period 1998-2000 being less than 0.42.
In this study, urban areas were defined as municipalities other than rural areas.
Analysis and ethical considerations
This study was conducted according to the 2007 ethical guidelines for epidemiologic research of Japan's Ministry of Health, Labour and Welfare26. Approval for this multicenter study was granted by the central Institutional Review Board of the Institute of Medical Science, University of Tokyo, which determines on behalf of hospitals without an independent ethics committee26. Zip codes were collected anonymously and converted into addresses for categorization by municipality and secondary medical area.
Statistics
An unpaired t-test was used for comparison of differences in means between the two groups. A p-value less than 0.05 was considered statistically significant.
Results
Population density and the proportion of elderly people
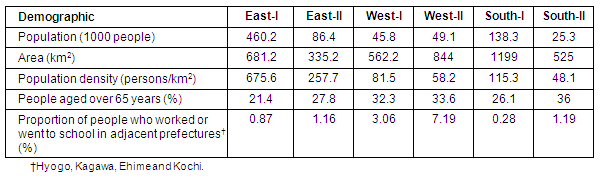
There was a wide range of population density (median [range], 170.3 persons/km2 [15.0-2362.3]) and proportion of people aged over 65 years (28.3% [13.8-49.6]) according to municipality (Fig2A,B). Table 1 provides basic demographic data according to the 6 secondary medical areas. The south-II medical area had the lowest population and population density, and highest proportion of people over 65 years. The proportion of people who worked in adjacent prefectures was highest in west-II27.
Table 1: Basic demographics of the 6 secondary medical areas
Estimated numbers of patients
Estimated numbers of newly developed patients per 100 000 people/year are shown by municipality (Fig2C). The estimated numbers of patients were also calculated according to secondary medical area (Fig3B). The total estimated number of patients in Tokushima Prefecture was 230 (28.6 per 100 000 people).
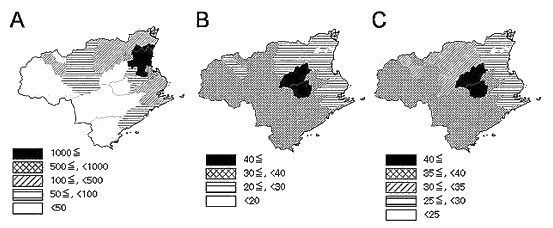
Figure 2: Population density (A), proportion (%) of people aged over 65 years (B) and estimated numbers of newly developed patients with hematological malignancies per 100 000 people/year (C) in Tokushima Prefecture, according to municipality.
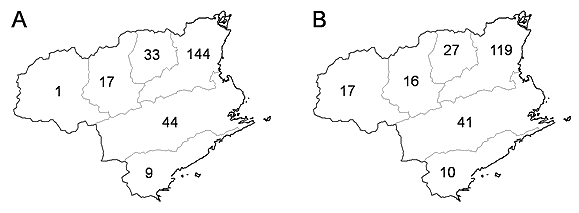
Figure 3: Comparison of surveyed (A) and estimated (B) numbers of patients of the 7 surveyed centers according to secondary medical areas.
Comparison between rural and urban areas
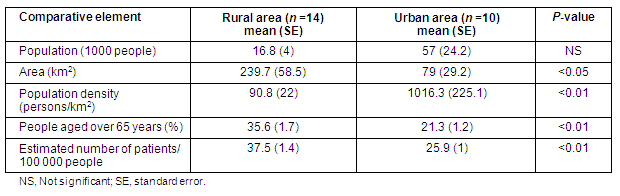
Basic rural and urban demographics were compared according to municipality (Table 2). There were significant differences between the two groups in area, population density, the proportion of persons over 65 years, and the estimated numbers of patients per 100 000 population.
Table 2: Comparison of rural and urban areas' basic demographics
Surveyed numbers of patients
The surveyed number of patients (n 248) by municipality at each center are shown (Figure 4). More than 70% (80% [72-100%]) received their treatment within a radius of approximately 25 km from each center: center A (79%), center B (87%), center C (76%), center D (80%), center E (72%), center F (96%), and center G (100%).
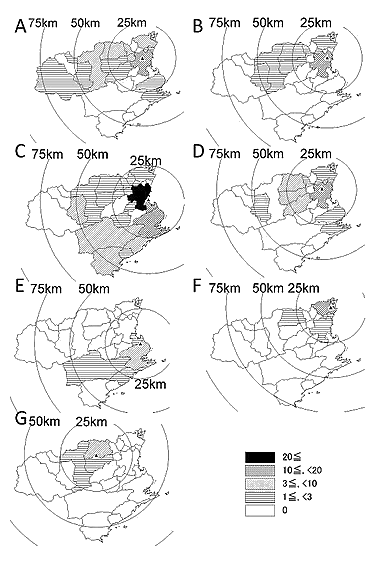
Figure 4: Surveyed numbers of newly diagnosed patients for each center (A-G). Annual numbers of patients hospitalized for newly developed hematological malignancies are shown for each surveyed center, according to municipality. Triangle = location of the center; concentric rings show areas within 25, 50 and 75 km.
Distribution of patients
The surveyed and estimated numbers of patients in each secondary medical region were compared (Fig3). The numbers were similar in all secondary medical areas except for west-II, and most of the patients with hematological malignancies were treated within the prefecture by in-prefecture hematologists.
Distribution of hematologists
In November 2006 there were 24 hematologists in Tokushima Prefecture (Fig5). Of these, 21 were affiliated with the Department of Medicine at Tokushima University Hospital, 21 worked for core hematologic centers, and 15 worked for core hematologic centers in Tokushima City. Of the 15 part-time hematologists, 14 worked in or close to Tokushima City.
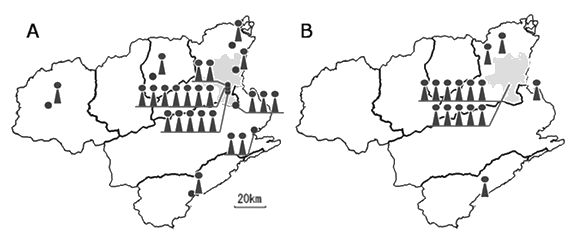
Figure 5: Distribution of hematologists and their part-time workplaces. Those working in core hematologic centers (A); and in part-time workplaces (B). Shading = Tokushima City.
Discussion
The estimated number of newly developed patients per unit population in Tokushima Prefecture was higher than the national mean (22.2 per 100 000 people)15, attributable to an aging population (>65 years in 2006: 24.9% Tokushima vs 20.8% Japan)28. Intra-prefectural comparisons among municipalities provided similar results. In rural areas that had high numbers of elderly people the estimated number of patients per unit population were significantly higher than in urban areas (Table 2; Figs2B,C). As the population ages, establishing a social system of medical care for aged patients in rural and remote areas will become more important.
Estimated and surveyed numbers of patients were similar in all secondary medical areas except for west-II (Fig3). This suggests that patients in rural and remote areas received standard treatments by hematologists, largely within the prefecture. For the west-II medical area, it was presumed that patients migrated to neighboring prefectures, due to road and rail connections (Fig1B); this area had the highest proportion of people who worked in adjacent prefectures (Table 1).
The present study demonstrated that more than 70% of patients lived within an approximate radius of 25 km from their treating medical center (Fig4); it was calculated that these patients could reach a medical center within approximately 1 hour (based on an average travel speed of 20-30 km per hour29). Consideration of regional features is important when establishing an equitable system of medical provision. For instance, patient distribution for the core center shown in Figure 4C was not limited to the urban area but extended to southern rural areas, unlike the distribution patterns of other centers; south-II patients had a long distance to travel to hospital because there was no core center in their area.
Ota recently discussed the maldistribution of physicians and hospitals for hematologic treatments in Hokkaido (north Japan)14 and the present study suggests this is also the case in Tokushima Prefecture. While 63% of the hematologists worked in Tokushima City (which has the largest population), only 31% of newly developed patients lived there. According to Japan's Ikyoku system, physicians' training and the staffing of rural medical services are supported by the clinical departments of medical universities22,23. As well as performing academic activities, some university-affiliated physicians work in main hospitals while also treating patients in rural clinics on a part-time basis. We had hypothesized that medical care in rural and remote areas was supported by part-time physicians; however, part-time medical practice was found to be localized in and around urban Tokushima City. This suggests that the rural medical system for managing patients with hematological malignancies is at risk of collapse.
The present study also provided basic information on the centralization of intensive therapies. Centers shown in Figure 4(E,F,G) had only one or two hematologists and this did not provide sufficient capacity for the treatment of severe conditions, such as new-onset patients or those requiring stem cell transplantation. This presents an issue that could be addressed by dividing the functions of hospitals, according to the capacity of each medical center. Under such a system, acute-phase patients could be intensively managed at urban core medical centers with subsequent management provided at rural clinics supported by urban hematologists. However, innovations in patient transportation and the application of information/communication technologies30,31 would be essential. Collaboration between rural clinic physicians and hematologists from core centers at such venues as conferences or reunions might pave the way for a redesign of roles. In our fieldwork research in Tokushima Prefecture many local practitioners were eager to discover the medical specialties of physicians who worked in regional hospitals.
There are some limitations to the present study. The subjects were limited to hospitalized patients with hematological malignancies in Tokushima Prefecture and qualitative data was not collected about their medical care, nor was information collected about patients' socioeconomic status. The study assumed that most patients with hematological malignancies are treated by 'hematologists', without defining a level of qualification. This was because the provision of intensive chemotherapy is a highly specialized skill; not all well-trained hematologists in Japan have the certification of a scientific association; and collaborative, team-based care is important to improving quality of care, not just the ability of an individual physician32,33. However, it is possible that some patients were treated by physicians who rarely treated hematological malignancies. A further limitation is that there is little information on the precise distribution of patients with hematological malignancies in Japan, and it is possible that regional differences exist, as has been suggested for adult T-cell leukemia/lymphoma34. In the present study, patient data were collected in 2006, but the 2002 incidence of hematological malignancies was used15 as the latest available at the time of data analysis. Careful interpretation is needed when comparing surveyed and estimated data. Finally, it was difficult to assess the adequacy of the number of hematologists due to limited data relating to absolute indexes, and a number of qualifying factors, such as degrees of risk for treatments, hematologists' working hours, and patient and physician satisfaction. Further studies are recommended that include these factors.
Following on from the present pilot study, further rural studies are planned for prefectures other than Tokushima, including qualitative studies to investigate patient migration and other diseases.
Conclusions
Most patients with newly developed hematological malignancies in Tokushima Prefecture were treated by hematologists within the prefecture. Most of the patients visited hospitals within 25 km of their homes; however, the distribution of patients' homes was different according to regional medical center. The clustering of hematologists in urban centers has led to a shortage in rural areas. It is therefore recommended that the functions of core medical centres and rural clinics are redesigned according the availability of specialized hematologic treatments. The cooperation of physicians at rural clinics and hematologists at urban hospitals will be essential and must be encouraged for the benefit of rural patients' care.
Acknowledgements
This study was supported by Health Labour Sciences Research Grant for Clinical Cancer Research (H18-Ganrinsho-Ippan-006) from the Japanese Ministry of Health Labour and Welfare. The authors express their appreciation of the assistance of the following people: T Matsumoto, M Abe (University of Tokushima Graduate School of Health Biosciences, Department of Medicine and Bioregulatory Sciences), T Muraichi (Health Insurance Naruto Hospital), S Watanabe (Tokushima City Hospital), M Shinohara (Anan Kyoei Hospital), S Fujiwara (Tokushima Prefectural Miyoshi Hospital), T Inoshita (Tokushima Prefectural Kaifu Hospital), Y Maeda (Awa Hospital), Y Sengoku (House of Representatives), Y Sano, K.Toyoda (Tokushima Prefecture Government), H Ishimoto (Tokushima Public Health Center), S Ueda (International Research Institute of Health and Welfare) and Y Kikuchi (Osaka Prefectural Government).
References
1. Hiyama T, Tanaka S, Yoshihara M, Fukuhara T, Mukai S, Chayama K. Medical malpractice litigation related to gastrointestinal endoscopy in Japan: a two-decade review of civil court cases. World Journal of Gastroenterology 2006; 12(42): 6857-6860.
2. Kato S. Medical malpractice, past, today and future. Nippon Geka Gakkai Zasshi 2003; 104(4): 373-376. (In Japanese)
3. Hagihara A, Nishi M, Abe E, Nobutomo K. The structure of medical malpractice decision-making in Japan. Journal of Law and Medicine 2003; 11(2): 162-184.
4. Teo A. The current state of medical education in Japan: a system under reform. Medical Education 2007; 41(3): 302-308.
5. Kozu T. Medical education in Japan. Academic Medicine 2006; 81(12): 1069-1075.
6. Onishi H, Yoshida I. Rapid change in Japanese medical education. Medical Teacher2004; 26(5): 403-408.
7. Hoya Y, Okamoto T, Yanaga K. Stop the 'surgeon shortage' what could be done and what should be done right now. Series 3: correction of uneven distribution of doctors. Nippon Geka Gakkai Zasshi 2008; 109(2): 115-116. (In Japanese)
8. Matsuda H. The new national postgraduate residency program and its relation to the general surgery board in Japan. Nippon Geka Gakkai Zasshi 2003; 104(4): 341-344. (In Japanese)
9. Inoue K, Matsumoto M, Sawada T. Evaluation of a medical school for rural doctors. Journal of Rural Health 2007; 23(2): 183-187.
10. Matsumoto M, Okayama M, Kajii E. Rural doctors' satisfaction in Japan: a nationwide survey. Australian Journal of Rural Health 2004; 12(2): 40-48.
11. Inoue K, Matoba S, Sugiya Y, Okuno M. A comparative study of rural clinics in remote islands and inland areas. Asia-Pacific Journal of Public Health 2000; 12(1): 22-26.
12. Capria S, Vitolo D, Cartoni C, Dessanti L, Micozzi A, Mandelli F et al. Neutropenic enterocolitis in acute leukemia: diagnostic and therapeutic dilemma. Annals of Hematology 2004; 83(3): 195-197.
13. Rohaly-Davis J, Johnston K. A new collaborative practice: critical care and hematology/oncology - altering the misconceptions. Critical Care Nursing Quality 1996; 18(4): 61-65.
14. Ota S. Current status of investigator-initiated clinical trials on hematological diseases - Northern Hematology Study Group. The Japanese Journal of Clinical Hematology 2008; 49(7): 455-463. (In Japanese)
15. Matsuda T, Marugame T, Kamo K, Katanoda K, Ajiki W, Sobue T. Cancer incidence and incidence rates in Japan in 2002: based on data from 11 population-based cancer registries. Japan Journal of Clinical Oncology 2008; 38(9): 641-648.
16. Ministry of Health, Labor and Welfare of Japan. Ishi Shikaishi Yakuzaishi Chosa [National survey of physicians, dentists, and pharmacists in 2006]. (Online) 2006. Available: http://www.mhlw.go.jp/toukei/saikin/hw/ishi/06/index.html (Accessed 3 March 2009). (In Japanese)
17. Tokushima Prefectural Government. Tokushima Ishi Banku [Doctor Bank Tokushima]. (Online) no date. Available: http://our.pref.tokushima.jp/dr-bank/ (Accessed 3 March 2009). (In Japanese)
18. Department of Community and Primary Care Medicine, The University of Tokushima Faculty of Medicine. The Homepage of Department of Community and Primary Care Medicine. (Online) no date. Available: http://www.tiiki.umin.jp/ (Accessed 3 March 2009). (In Japanese)
19. Tokushima Prefectural Government. Tokushima-ken Hoken-Iryo Keikaku. [Medical care plan in Tokushima] (Online) 2005. Available: http://www1.pref.tokushima.jp/hoken/iryouseisaku/plan_index.html (Accessed 3 March 2009). (In Japanese)
20. Ministry of Internal Affairs and Communication of Japan. Jumin Kihon Daicho Jinko Ido Hokoku [Report on migration derived from basic resident registers] (Online) no date. Available: http://www.stat.go.jp/data/idou/index.htm (Accessed 3 March 2009). (In Japanese)
21. Geographical Survey Institute. Zenkoku Todofuken Shikuchoson-betsu Menseki Shirabe [Report of areas by prefectures and municipalities]. (Online) 2006. Available: http://www.gsi.go.jp/KOKUJYOHO/MENCHO/200610/opening.htm (Accessed 3 March 2009). (In Japanese)
22. Hirose M, Imanaka Y, Ishizaki T, Evans E. How can we improve the quality of health care in Japan? Learning from JCQHC hospital accreditation. Health Policy 2003; 66(1): 29-49.
23. Otaki J. Considering primary care in Japan. Academic Medicine 1998; 73(6): 662-668.
24. Ministry of Internal Affairs and Communications of Japan. Kasochiiki Jiritsu Sokushin Tokubetsu-sochi Hou [Law concerning self-sustaining for rural areas]. (Online) 2007. Available: http://law.e-gov.go.jp/htmldata/H12/H12HO015.html (Accessed 3 March 2009). (In Japanese)
25. Ministry of Internal Affairs and Communications of Japan. Chiho Zaisei [Local government finance]. (Online) no date. Available: http://www.soumu.go.jp/c-zaisei/index.html (Accessed 3 March 2009). (In Japanese)
26. Ministry of Health, Labor and Welfare of Japan, Ministry of Education, Culture, Sports, Science and Technology of Japan. Ekigaku Kenkyu Ni Kansuru Rinri-shishin [Ethical guidelines for epidemiologic research]. (Online) 2007. Available: http://www.mhlw.go.jp/general/seido/kousei/i-kenkyu/ekigaku/0504sisin.html (Accessed 3 March 2009). (In Japanese)
27. Ministry of Internal Affairs and Communications of Japan. Kokusei Chosa [Population Census]. (Online) 2005. Available: http://www.stat.go.jp/english/data/kokusei/index.htm (Accessed 8 July 2009).
28. Japan Statistics Bureau. Jinko Suikei [Report of estimated population]. (Online) 2006. Available: http://www.stat.go.jp/data/jinsui/index.htm (Accessed 3 March 2009). (In Japanese)
29. Ministry of Land, Infrastructure, Transport and Tourism of Japan. Doro-Kotsu Sensasu [Census of transportation]. (Online) 2006. Available: http://www.mlit.go.jp/road/census/h17/pdf/gaiyo.pdf (Accessed 3 March 2009). (In Japanese)
30. Blumenthal D, Glaser J. Information technology comes to medicine. New England Journal of Medicine 2007; 356(24): 2527-2534.
31. Chaudhry B, Wang J, Wu S, Maglione M, Mojica W, Roth E et al. Systematic review: impact of health information technology on quality, efficiency, and costs of medical care. Annals of Internal Medicine 2006; 144(10): 742-752.
32. Makowsky MJ, Schindel TJ, Rosenthal M, Campbell K, Tsuyuki RT, Madill HM et al. Collaboration between pharmacists, physicians and nurse practitioners: A qualitative investigation of working relationships in the inpatient medical setting. Journal of Interprofessional Care 2009; 23(2): 169-184.
33. Zazzali JL, Alexander JA, Shortell SM, Burns LR. Organizational culture and physician satisfaction with dimensions of group practice. Health Services Research 2007; 42(3pt1): 1150-1176.
34. Tajima K. The 4th nation-wide study of adult T-cell leukemia/lymphoma (ATL) in Japan: estimates of risk of ATL and its geographical and clinical features. The T- and B-cell Malignancy Study Group. International Journal of Cancer 1990; 45(2): 237-243.
Abstract
Introduction:
The uneven distribution of physicians in Japan disadvantages rural and remote patients with hematological malignancies to the extent that they may not receive standard treatments. There are 7 core regional medical centers in Tokushima Prefecture. A Tokushima rural medical center's clinical hematology division experienced difficulty in treating patients due to a lack of physicians despite an increasing number of patients with hematological malignancies. The aim of this pilot study was to investigate the regional medical supply and demand associated with newly diagnosed hematological malignancies in Tokushima Prefecture, Japan.Methods: The study investigated the home addresses of patients with newly diagnosed acute leukemia, malignant lymphoma and multiple myeloma who were hospitalized in the 7 core Tokushima centers in 2006. The surveyed patients were compared with the estimated number of patients with those diseases that were newly developed, based on a calculation of incidence and population by age group. The survey also investigated the number and distribution of hematologists.
Results: A total of 248 patients were newly hospitalized in the 7 core centers in Tokushima Prefecture during the 1 year period. The surveyed number of patients was similar to the estimated number of patients in all secondary medical areas, except for one area where there was active traffic to and from adjacent prefectures. More than 70% (median 80%; range 72-100%) of the patients received their treatments within a radius of approximately 25 km from their homes. There were 24 hematologists in November 2006 and 63% of these worked in the city with the largest population. The mean estimated number of patients per unit population was significantly higher in rural and remote areas than in urban areas (p <0.01). Three regional centers had only one or two hematologists.
Conclusions: Most patients with newly developed hematological malignancies in Tokushima Prefecture received treatment from intra-prefectural hematologists within a 25 km distance of their homes. Rural areas had a shortage of hematologists who were localized in urban areas. It is recommended that functions of core medical centres and rural clinics are redesigned according the availability of specialized treatments, and to maximize cooperation between physicians at rural clinics and hematologists at urban hospitals.
Key words: hematological neoplasms, Japan, public health, rural health services.
You might also be interested in:
2020 - Household financial contribution to the health system after Iran's Health Transformation Plan
2006 - A breastfeeding study in a rural population in South Australia

