full article:
Introduction
In Canada there is a general shortage of family physicians (general practitioners), particularly in rural areas1. Sixteen percent of the family physicians in Canada practice in rural areas, serving 21% of the population1. Both urban and rural family physicians face a number of challenges in their work place, such as high workloads and the business demands of setting up and running a private practice2. However, some issues are specific to the geographical area of their workplace. Urban and inner-city family physicians have reported seeing higher numbers of patients with complex disease profiles such as co-morbidities and emotional and mental health problems, compared with their suburban and rural colleagues3. In the same study, urban family physicians felt that they dealt with more issues per visit and had longer patient visits than their sub-urban and rural counterparts. In another study, urban family physicians felt that they had less autonomy and worked under greater pressure to see more patients than their rural colleagues2.
Rural family physicians have reported major challenges in their work environment. These challenges range from professional isolation4,5 to trying to establish professional/private boundaries6,7 or workload issues8. Professional isolation was exacerbated for rural family physicians during medical emergencies. A cross-sectional survey of rural physicians in a western Canadian province, British Columbia, examined the impact of practicing in a rural community on psychological wellbeing and intention to relocate. The results of the study demonstrated that of the 131 rural physicians, almost one-third suffered from mild to severe depression and 80% reported 'moderate to severe emotional exhaustion'9. Of the rural physicians who participated in the study, half of the respondents reported that they were considering relocating to a different community9. Length of stay in these communities did not have an impact on depression scores10.
Rural areas are faced with the challenge of attracting and retaining family physicians1. Various strategies ranging from targeted medical school and resident training, professional development, regional collaborations and financial compensation have been used to enhance recruitment and retention11,12. Others argue that personal and professional integration is the key to improving retention of rural practitioners5. Integration and support for rural family physicians may serve as a buffer against the challenges of rural practice.
Despite the many recruitment and retention strategies over the years, the success of recruitment and retention in rural areas continues to be problematic. The data source for this article is a separate qualitative study that was conducted on 48 family physicians examining the impact of the feminization of family medicine in New Brunswick. While the initial focus of the study was the issue of feminization, the interviews centered on workplace issues. This article is based on 21 of those interviews conducted on rural family physicians regarding their workplace issues in the eastern Canadian province of New Brunswick. The results of the study will contribute to our knowledge of issues that have a significant impact on the retention of rural family physicians.
The setting for this research, the province of New Brunswick, has a small population of just under 750 000 people. Half the population lives in rural areas or small towns (<10 000)13. New Brunswick has three cities and their immediate adjacent communities have populations ranging from 100 000 (Greater Moncton) to 70 000 (Fredericton). The next three largest towns have populations ranging from 12 700 to 18 200, and all other areas have smaller populations14. For comparison purposes, New Brunswick is 72 908 km2 with a population density of 11 people per km2, while the Netherlands is 41 452 km2 with 491 people per km215.
Methods
Interviews
A qualitative, collective case study approach was employed to explore the 'bounded system' of multiple cases through in-depth interviews16. This approach allowed exploration of the context of the work environment (bounded system) of family physicians. The study was reviewed by two university research ethics boards. We recruited 48 family physicians from across the province. In this collective case study approach, each case consisted of two individuals, for a total of 24 cases based on language (French/English), gender, location of practice (urban/rural), and year of graduation from medical school (<10 years, between 10-20 years and >20 years of practice) as criteria. An example of a case would be female/rural/middle-aged/English. All participants received an honorarium ($120) for completing the interview.
Recruitment
Participants were recruited using the College of Physicians and Surgeons of New Brunswick website information. The website lists physicians' primary specialty, date of graduation from medical school and location of practice. The sex of the physicians was inferred from the names and all physicians practicing outside the 6 largest cities and towns in New Brunswick were considered rural. We used a targeted recruitment strategy, sending letters of invitation explaining the study to potential participants in 8 separate mailings, each designed to target physicians fitting our case study criteria. A reply card was included with the invitation package, along with a self-addressed, stamped return envelope and a fax number for sending responses. All information in the recruitment package was in both French and English and potential participants were given the option to indicate their language of preference for the interview.
Research team
The multidisciplinary, bilingual research team consisted of three co-investigators - a sociologist, a family physician and a philosopher/ethicist - and three research assistants trained in qualitative research methods. Prior to the interview, participants' consent was sought for permission to audiotape the interview. All but two participants agreed to have their interview recorded. For the two exceptions, the research assistant took detailed notes and made an audiotaped recap after the interview was completed. Interviews were conducted face-to-face in either the physician's home or office.
Analysis
All audiotaped interviews were transcribed verbatim and analyzed thematically using a categorical aggregation approach. In this type of analysis, 'the researcher seeks a collection of instances from the data, hoping that issue-relevant meanings will emerge'16. Each member of the team read and analyzed two transcripts, making notes to help generate initial codes. At a preliminary team meeting, comparisons were made both within and across transcripts, further contributing to the development of thematic categories. Related themes were then compared and collapsed into major substantive themes. The team was in agreement for most codes; however, in cases where there was a difference of opinion, consensus was obtained by further team discussion. After the development of the initial coding scheme, minor revisions and additional codes were discussed during telephone and email correspondence. A second team meeting took place in order to finalize the coding scheme. A bilingual research assistant used the English coding scheme to analyze the French transcripts. Dependability and confirmability of the data were achieved by sending a summary of the analysis back to the interviewees for comment. No participants sent back comments. This article only reports the experiences and themes that emerged from the data for rural family physicians practicing in New Brunswick.
Results
Response rate
For each of the mailings the average response rate was 35%. We were unable to fill all cases because there were few physicians for some of the specific criteria. We therefore chose to have some cases overrepresented when it became obvious that the pool of potential candidates was going to be small in some specific cases. There were a total of 12 rural cases with underrepresentation in four cases (two male, two female) and overrepresentation in one (female). This made a total of 21 rural physicians.
The transcripts of all urban participants were also analyzed for references to rural practice; and indeed four of the 27 urban participants also discussed rural practice.
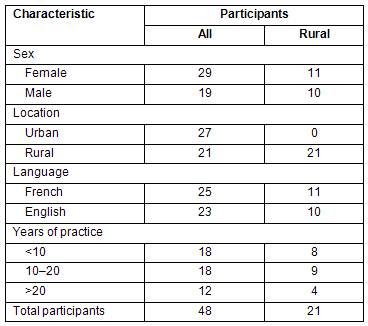
Table 1: Characteristics of all and rural participants
The major themes that emerged from the data were: benefits of rural practice, professional isolation, complex patient profiles and maintaining professional boundaries.
Benefits of rural practice
A number of rural family physicians felt that the benefits of rural practice outweighed the disadvantages. This seemed to be particularly the case for physicians who had grown up in rural areas. One family physician appreciated the fact that he knew his patients and their families well. He said:
What was interesting was the degree to which your care of patients, or your diagnosis, was enhanced by knowing the patient. When I saw my patients in the ER, usually I had some background that other people wouldn't have as, opposed to when I saw other people's patients. Rural male middle-aged English (interview 6)
Others chose to practice in a rural area because of the lifestyle.
...we wouldn't be able to have the lifestyle we wanted in the city... I grew up in rural New Brunswick ... and I really wanted to return to a less urban area.... Rural male middle-aged English (interview 7)
Professional isolation
Although some discussed the benefits of rural practice, many more rural physicians discussed the challenges. One such challenge was that of professional isolation. Many physicians felt that they had little opportunity to consult with other family physicians or specialists regarding medical diagnosis or management problems. Further, after treating patients with unusual medical conditions or emergencies, they did not have a chance to debrief with colleagues. As one physician described it:
I think the more rural you go the harder it gets because you begin to have professional isolation issues and things like that, not only on a personal level, everybody I know in town is my patient, but also in a sense that I've got no one to bounce ideas off: 'What should I do with this case of heart failure?' Rural male young English (interview 1)
For rural family physicians whose patients need specialist care, it was not always easy to access such care. Rural family physicians complained that specialists were sometimes dismissive of their skills, questioned their judgment or couldn't understand why the treatment could not be offered locally. This situation typically occurred when the family physician had exhausted all specialist care venues in the local setting. Several family physicians reported that they had some trepidation about making referrals to specialists whom they did not know, or with whom they had little contact. As one physician said:
Rural people know that not all services are available; however, some specialists do not want to take more patients if it is not convenient. Rural female middle-aged French (interview 2)
Yet another physician complained about the lack of diagnostic services as a problem. This physician said:
Our biggest lack any time... there's been no X-ray... This summer the lab was cut... Rural female older English (interview 4)
However, the same physician felt that she had a great working relationship with one specialist colleague and that working to build this strong relationship was certainly of benefit to her rural practice. She said:
If I need a patient transferred to the regional hospital, I can call them. So it has been wonderful. Rural female older English (interview 4)
Complex patient profiles
In addition to professional isolation, several rural family physicians described their feeling that the rural patient is more complex than the urban patient. One physician attributes this to rural lifestyle and the fact that rural citizens do not seek medical help as easily as their urban counterparts. She said:
A lot of these patients are sort of older people with a lot of multiple medical problems so they're fairly challenging and they are probably the type of people who would be in every week or two anyway because they're pretty sick. ....[M]ore rural people seem to drink and smoke and party a heck of a lot more... and they tend to not really take care of their hearts and they don't complain until things get really, really bad, so, I just see, the patients seem to be a lot sicker, more demanding. Rural female young English (interview 5)
Another physician suggested that when patients come with psychosocial problems there is a paucity of community resources to refer them for appropriate counseling or other services. He said: 'I don't always have assistance from family resources. They don't have enough employees to support those families' (rural male young French; interview 8). The lack of comprehensive medical support in small communities makes the family physician feel as though it is his/her job to fill the gaps left by inadequate services and little specialist support.
Maintaining professional boundaries
Perhaps the biggest challenge facing rural family physicians was not in the professional, but rather in the private sphere. Setting and maintaining professional and private boundaries was mentioned by many as the most challenging aspect of having a rural practice. The challenges ranged from systematic ones (few physicians in the community), to patients not recognizing the physicians' privacy. A system-related issue was work pressure. This male physician said:
...there is a lot of pressure of, you know, 'We need someone to cover the ER this day'.... You feel bad 'cause, you know, you don't want people to not have a doctor, and not be able to access health care. Rural male young English (interview 3)
The work pressures of a rural practice make it difficult for a family physician to establish personal boundaries and to practice proper self-care. The health of the patients is often considered more important than the health of the physician.
Other boundary issues were related to patients' inability to respect the physicians' privacy. Some rural family physicians talked about being approached by patients outside work for medical advice. Whether at the grocery store, a child's hockey practice or shopping in the mall, rural patients seemed to easily cross the professional/private boundary. One physician summed it up as follows:
So, I'd be in the grocery store, the drive thru at Tim's and people would be asking about their mother, or their son and stuff. People would be at your door and sometimes we had people in the house, like on a Sunday morning, coming up the stairs saying: 'I'm one of your patients...' Rural male middle-aged English (interview 6)
This physician has made the decision to move to a bigger centre and now commutes to his rural practice; he said: '...I purposely made that decision to commute'. Another physician had left family medicine and was now working in a rural ER full-time because, while in private practice she could not set boundaries. She said, '...I knew everyone, it was difficult to set limits, I could not say no' (Rural female middle-aged French; interview 2).
Discussion
Rural family physicians in New Brunswick face challenges such as professional isolation, workload issues and social isolation similar to those faced by other rural physicians5,8,17. Physicians also spoke of the lack of support from colleagues, often specialists in the larger centers, regarding the acceptance of referrals and requests for consultations. In addition, many felt that their patient profile was more complex than the patient profile of their urban colleagues. This perception is not supported by Blankfield et al3; however, other studies suggest that rural patients are older, financially poorer, more likely to smoke, less educated and in poorer overall health than their urban counterparts18.
The paramount challenge for the rural family physicians in this study was the establishment and maintenance of professional and private boundaries. Rural family physicians feel that these boundaries are continuously crossed by themselves, due in part to such issues as work pressure or guilt - and by patients. If these boundary violations are experienced often or profoundly enough, rural physicians may consider leaving the community or changing their practice setting, as a number of physician participants had done or were considering. While it has been documented in the literature that work pressure and work isolation is a significant challenge, what has not been well documented is the struggle of maintaining professional and private boundaries by physicians, and the seeming ease with which patients cross these boundaries in rural communities. Patients and rural communities need to take some responsibility for respecting the rural family physician's privacy or the trend toward physicians moving away from their practice locations will continue. Although some older physicians felt that they could cope better with patients crossing boundaries, not one mentioned it as a positive experience.
It is important that rural family physicians express clearly what intrusions into their private lives they will tolerate. It is also important that patients and communities respect physicians' professional boundaries. Not recognizing these boundaries by both physicians and patients may lead to depression, burnout and eventually loss of the physician to the community10. One participating family physician felt that patients who meet their physicians outside the office or medical setting, need to be 'aware of appropriate and inappropriate questions' (Rural male middle-aged; interview 6).
Contemporary rural family physicians have moved beyond the traditional, romanticized, old-fashioned male country doctor who has a supportive wife at home and is always on call for his patients, day or night. The majority of the new family physicians are female, and a large number have significant child-rearing responsibilities19,20. Other rural medical specialists also struggle with maintaining professional boundaries between patients and themselves. Psychiatrists and other mental health workers also face unique patient-physicians/practitioner relationships6.
Despite the challenges of rural practice, several of the rural family physicians were satisfied to live and work in rural areas. Consistent with the literature, rural physicians who grew up in rural areas are most likely to enjoy living and working in such an environment21,22.
The recruitment of rural family physician participants to this study was based on age, gender and language. Our analysis revealed that these family physicians' characteristics did not have any influence on the experienced challenges and rewards of rural practice.
Conclusion
Understanding the challenges faced by rural physicians may serve as a pathway to increasing retention in rural areas. In our view, retention of rural family physicians needs to include also the non-clinical, non-medical and non-technical issue of privacy. Rural patients and rural communities need to understand that their physician needs privacy and 'downtime' that is free from intrusion. In order to develop effective retention strategies, it is important to pay attention to the issue of professional and personal boundary formation and maintenance. Both patients and physicians need to be educated on the importance of these issues, and also on the impact that violation of these boundaries may ultimately have on the retention of physicians in rural communities.
References
1. Canadian Institute for Health Information. Geographic distribution of physicians in Canada: Beyond how many and where. Ottawa: Canadian Institute for Health Information, 2009.
2. Luman K, Zweifler J, Grumbach K. Physician perceptions of practice environment and professional satisfaction in California: from urban to rural. Journal of Rural Health2007; 23(3): 222-228.
3. Blankfield RP, Goodwin M, Jaen CR, Stange KC. Addressing the unique challenges of inner-city practice: a direct observation study of inner-city, rural, and suburban family practices. Journal of Urban Health 2002; 79(2): 173-185.
4. Smith DM. Barriers facing junior doctors in rural practice. Rural Remote Health 5: 348. (Online) 2005. Available: www.rrh.org.au (Accessed 5 May 2009).
5. Hays R, Wynd S, Veitch C, Crossland L. Getting the balance right? GP's who choose to stay in rural practice. Australian Journal of Rural Health 2003; 11: 193-198.
6. Simon RI, Williams IC. Maintaining treatment boundaries in small communities and rural areas. Psychiatric Services 1999; 50(11): 1440-1446.
7. Rourke J, Rourke L, Goertzen J, Brown JB, Smith L. Physician-patient relationships: patients as friends and patients who harass. Canada Medical Association Journal. 1996; 154(8): 1149; author reply 50.
8. Bowman RC, Crabtree BF, Petzel JB, Hadley TS. Meeting the challenges of workload and building a practice: the perspectives of 10 rural physicians. Journal of Rural Health 1997; 13(1): 71-77.
9. Thommasen HV, Lavanchy M, Connelly I, Berkowitz J, Grzybowski S. Mental health, job satisfaction, and intention to relocate. Opinions of physicians in rural British Columbia. Canadian Family Physician 2001; 47: 737-744.
10. Thommasen HV, Connelly I, Lavanchy M, Berkowitz J, Grzybowski S. Short report: burnout, depression, and moving away. How are they related? Canadian Family Physician2001; 47: 747-749.
11. Chaytors RG, Spooner GR. Training for rural family medicine: a cooperative venture of government, university, and community in Alberta. Academic Medicine 1998; 73(7): 739-742.
12. Rabinowitz HK, Diamond JJ, Markham FW, Hazelwood CE. A program to increase the number of family physicians in rural and underserved areas: impact after 22 years. JAMA 1999; 281(3): 255-260.
13. Government of Canada. Canadian Rural Information Service. (Online) 2008. Available: http://www.rural.gc.ca/cris/faq/pop_e.phtml (Accessed 10 January 2009).
14. Government of New Brunswick. Population. (Online) 2006. Available: http://www.gnb.ca/cnb/nb/Population-e.asp (Accessed 20 February 2009).
15. MSN Encarta. Facts and figures. (Online) 2008. Available: http://encarta.msn.com/encnet/refpages/RefEdList.aspx?refid=210117935 (Accessed 20 February 2009).
16. Creswell JW. Qualitative inquiry and research design: choosing among five traditions. London: Thousand Oaks: Sage, 1997.
17. Barley GE, Reeves CB, O'Brien-Gonzales A, Westfall JM. Characteristics of and issues faced by rural female family physicians. Journal of Rural Health 2001; 17(3): 251-258.
18. Goertzen J. The four-legged kitchen stool. Recruitment and retention of rural family physicians. Canadian Family Physician 2005; 51: 1181-1183, 4-6.
19. Gautum M. Women in medicine: stresses and solutions. Western Journal of Medicine 2000; 2001(174): 37-41.
20. Riska E. Towards gender balance: but will women physicians have an impact on medicine? Social Science & Medicine 2001; 52(2): 179-187.
21. Chan BT, Degani N, Crichton T, Pong RW, Rourke JT, Goertzen J et al. Factors influencing family physicians to enter rural practice: does rural or urban background make a difference? Canadian Family Physician 2005; 51: 1246-1247.
22. Rourke JT, Incitti F, Rourke LL, Kennard M. Relationship between practice location of Ontario family physicians and their rural background or amount of rural medical education experience. Canadian Journal of Rural Medicine 2005; 10(4): 231-240.




