Introduction
Intimate partner violence (IPV) is a major public health problem in Africa and internationally1-7. Its consequences among women may include death8, physical injury and disability, depression, post-traumatic stress syndrome9, suicidal ideation10, high blood pressure11, unwanted pregnancy12,13, miscarriage and low birth weight babies10,12,14 and sexually transmissible infections3,15.
Previous studies have identified some associated factors: for the male perpetrator alcohol use2,6,7,17 and having multiple sexual partners4; for the woman, HIV-positive status3,6,15, low education/ socioeconomic status2,6,7 and pregnancy7, being in a cohabitating or short-duration relationship.
The Rwandan 2005 Demographic and Health Survey (DHS) reported18 the prevalence of IPV among pregnant women as 10.2%, but there were limited data on the determinants of IPV in Rwanda. If the health status of women is to be improved, effective interventions against IPV must be provided. Interventions will be most effective if local data on the prevalence of and factors associated with IPV are identified.
The aim of this study was to determine IPV-associated factors among rural, pregnant Rwandese women.
Methods
Study population and questionnaire
In January 2006, trained research staff from the School of Public Health, National University of Rwanda administered a survey questionnaire to 387 pregnant women attending for prenatal care services at Kabutare, a rural area in the South Province, Rwanda. The questionnaire included items on demographics, domestic violence, alcohol use by male partner, and HIV status. To assess IPV, consecutive HIV-infected and HIV-negative women were recruited into the study from antenatal clinic attendees. Study participants were asked specific questions (Fig1).

Figure 1: Questions used to ascertain prevalence of intimate partner violence.
Statistical methods
The measures used in this study were based on items from the questionnaire. The outcome of interest was self-reported history of IPV defined as having any of the listed experiences (Fig1). The demographic characteristics of interest were age, education (no formal education, elementary education, high school and beyond), marital status, length of relationship with male partner, alcohol use by male partner, and HIV status.
Mean age, and proportions with lifetime IPV and IPV in the last 12 months were assessed. Both univariate and multivariate odds of IPV exposure were estimated using logistic regression analysis. All data analysis was performed using SAS 9.1 (SAS Institute Inc; Cary, NC, USA).
Ethics considerations
The Institutional Review Board of the National University of Rwanda and the National Ethics Committee approved the study protocol. Informed verbal consent was obtained before administering the survey to participants. Consenting women were interviewed in private by trained research assistants. There was no identifier on the response form.
Results
The mean age of the 387 participants was 29.4 years (SD 6.3 years). Most of the sample was married (79.7%). More than one in two participants were married to an occasional alcohol drinker (58.1%), and 66.9% had elementary education. Almost one in two respondents (47.0%) were HIV positive and 54.7% reported lifetime IPV (Table 1).
Most participants reported lifetime experience of verbal abuse (53.7%). Other forms of lifetime IVP included pulling hair (9.4%), slapping (18.2%), choking (6.5%), punching with fists (19.3%), throwing to the ground and kicking with feet (12.8%), and burning with hot liquid (3.1%) (Table 2).
Table 1: Demographic characteristics of the study population
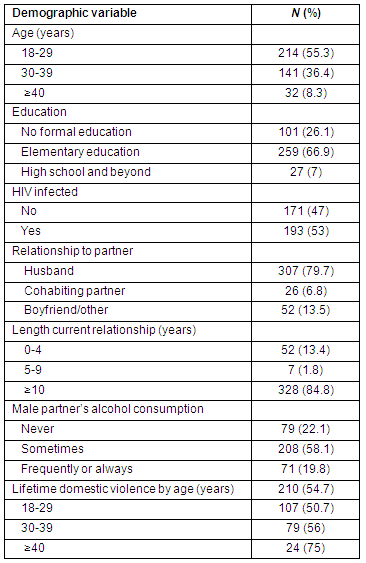
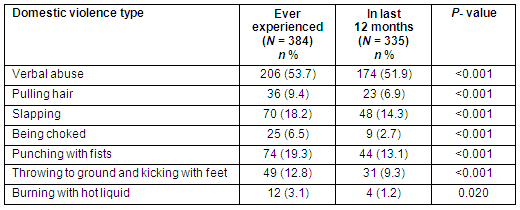
Table 2: Frequency of intimate partner violence among rural Rwandan pregnant women, 2006
Results from univariate and multivariate analyses are reported (Table 3). Compared with women who had no education, women with elementary education were less likely to report lifetime IPV (OR = 0.24; 95% CI [0.10, 0.59], and OR = 0.34; 95% CI [0.13, 0.88] for high school or beyond]). Participants who were in a cohabitating relationship were more than twice as likely to report lifetime IPV as those who were married (OR = 2.30; 95% CI [1.38, 3.82]). Compared with those who had lived with their male partner for 10 years or more, those who were in a relationship for 4 years or less were more likely to report lifetime IPV (OR = 3.25; 95% CI [1.73, 3.09]). Respondents whose male primary partners used alcohol were more likely to report lifetime IPV than those whose partners did not drink alcohol (OR = 2.66; 95% CI [1.48, 4.77] for occasional drinkers and OR = 4.01; 95% CI [2.00. 8.05] for heavy drinkers). There was no significant association between HIV-positive status and IPV.
Table 3: Lifetime experience of intimate partner violence among rural Rwandan pregnant women, 2006, according to demographic variables
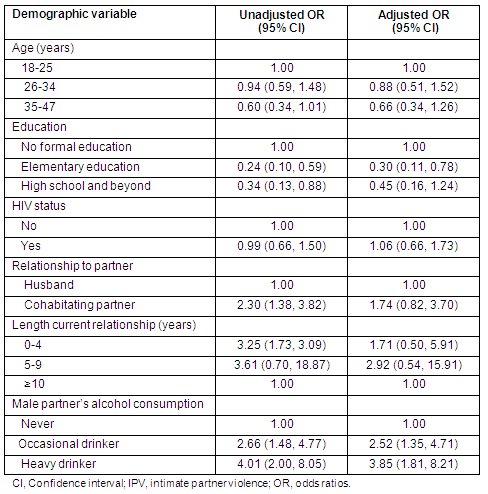
As shown in the multivariate analysis, odds ratios were unchanged for elementary education and alcohol drinking of male partners. The association between cohabiting with a male partner and lifetime IPV was no longer significant in the multivariate analysis.
Discussion
This study aimed to determine factors associated with IPV among rural pregnant women in Rwanda. The high rate of HIV-positive status in this study (47% compared with the national average of 3.2%) was due to participants being recruited from consecutive HIV-positive and HIV-negative women. Findings from this study indicate that more than one in two participants had experienced at least one form of IPV (verbal abuse) from their male partners (53.7% for lifetime IPV, and 51.9% for IPV in the last 12 months). These results are similar to reports from Soweto, South Africa (51%)19, but higher than those reported in Uganda (30%)2 and Tanzania (45.7%)3. The Rwandan Demographic Health Survey (DHS) 2005 reported the prevalence of physical violence during pregnancy at 10%18.
The present study found alcohol use by a male partner to be positively associated with IPV. Previous studies have reported a positive association between IPV and alcohol abuse by either perpetrator or victim7,17,20. A positive correlation between IPV and partner's alcohol use was found in a study conducted among Turkish women7. In New Mexico, female trauma patients who were screened and found positive for alcohol problems were five times more likely to have experience IPV in the previous 12 months compared with those without alcohol problems17. A Polish study reported that perpetrators who drank alcohol were more likely to be physically violent than those who did not drink alcohol20.
This study found no association between HIV and IPV, which differs from previous studies in Rwanda and elsewhere3,15,16. In a sample of 600 Rwandan women from two urban and two rural antenatal clinics, Ntaganira et al found that HIV-positive participants were more likely to report IPV than those who were HIV negative16. In a 3 month follow-up study of 245 Tanzanian women, Maman et al found that those who were HIV positive were more likely to report IPV than those who were HIV negative3. That risk was 10 times higher among young subjects. An explanation for the lack of association between IPV and HIV-positive status in the present study may relate to social support mechanisms being more protective in rural areas but this requires further research.
Results from this study indicate that education (positively associated with socioeconomic status) was inversely associated with lifetime IPV. Previous studies have reported a similar finding in other countries6,12,21,22. In a cross-sectional study conducted among Turkish pregnant women, abused women were less educated and had lower income than non-abused women21. A Bangladeshi study found the less educated the woman, the greater her risk of IPV12.
The limitations of this study are that its results cannot be used to assume causality. Second, it is possible that recall bias or deliberate mis-reporting may affect the accuracy of the self-reported data. However, this study used a standardized questionnaire that enables comparisons of IPV. The sample also had much higher prevalence of HIV-infected persons than would be the case in a community study. The prevalence of HIV in the general community is estimated at 3.2% among women 15-49 years23. Finally, the underlying reasons for IPV were not explored. Future qualitative studies using in-depth interviews are recommended to obtain data on cultural and societal factors associated with IPV in rural Rwanda.
Conclusion
The prevalence of IPV among pregnant rural Rwandan women indicates an urgent need for specific protective measures, such as public awareness campaigns, social policy and legal reform. The identified associated factors may be useful in developing public health programs to address IPV among rural Rwandan women.
Acknowledgements
The authors acknowledge the professional assistance provided by Shakila Bishumba, Fanette Umuraza, Immaculée Mukashema and Laurette Rudasingwa in field work supervision. Grateful thanks are also given to the women who participated in the survey. This project was made possible by the financial support of the Rwanda National Aids Control Commission.
References
1. World Health Organization. World report on violence and health. Geneva: WHO, 2002. Available: www.who.int/violence_injury_prevention/violence/world_report/en/full_en.pdf (Accessed 23 September 2007).
2. Koenig MA, Lutalo T, Zhao F, Nalugoda F, Wabwire-Mangen F, Kiwanuka N et al. Domestic violence in rural Uganda: evidence from a community-based study. Bulletin of the World Health Organisation 2003; 81: 53-60.
3. Maman S, Mbwambo JK, Hogan NM, Kilonzo GP, Campbell JC, Weiss E et al. HIV-positive women report more lifetime partner violence: findings from a voluntary counseling and testing clinic in Dar Es Salaam, Tanzania. American Journal of Public Health 2002; 92: 1331-1337.
4. Andersson N, Ho-Foster A, Mitchell S, Scheepers E, Goldstein S. Risk factors for domestic physical violence: a national cross-sectional household survey in eight southern African countries. BMC Women's Health 2007; 16: 11.
5. Parish WL, Wang T, Laumann EO, Pan S, Luo Y. Intimate partner violence in China: national prevalence, risk factors and associated health problems. International Family Planning Perspectives 2004; 30: 174-181.
6. Malcoe LH, Duran BM, Montgomery JM. Socioeconomic disparities in intimate partner violence against Native American women: a cross-sectional survey. BMC Medicine 2004; 2: 20.
7. Deveci SE, Gulbayrak C, Tokdemir M, Ayar A. Prevalence of domestic violence during pregnancy in a Turkish community. Southeast Asian Journal of Tropical Medicine and Public Health 2007; 338: 754-760.
8. Campbell JC, Glass N, Sharps PW, Laughon K, Bloom T. Intimate partner homicide: review and implications of research and policy. Trauma Violence Abuse 2007; 8: 246-269.
9. Rosen D, Seng JS, Tolman RM, Mallinger G. Intimate partner violence, depression, and posttraumatic stress disorder as additional predictor of low birth weight infants among low-income mothers. Journal of Interpersonal Violence 2007; 22: 1305-1314.
10. Hurwitz EJ, Gupta J, Liu R, Silverman JG, Raj A. Intimate partner violence associated with poor health outcomes in U.S. South Asian women. Journal of Immigrant Minor Health 2006; 8: 251-261.
11. Silverman JG, Decker MR, Reed E, Raj A. Intimate violence victimization prior and during pregnancy among women residing in 26 U.S. states: associations with maternal and neonatal health. American Journal of Obstetrics and Gynecology 2006; 195: 140-148.
12. Silverman JG, Gupta J, Decker MR, Kapur N, Raj A. Intimate partner violence and unwanted pregnancy, miscarriage, induced abortion, and stillbirth among a national sample of Bengladesh women. British Journal of Obstetrics and Gynaecology 2007; 114: 1246-1252.
13. Pallitto CC, O'Campo P. The relationship between intimate partner violence and unintended pregnancy: analysis of a national sample from Columbia. International Family Planning Perspectives 2004; 30: 165-173.
14. Collado Pena SP, Villanueva Egan LA. Relationship between familial violence during pregnancy and risk of low weight in newborn. Ginecologia y Obstetricia De Mexico 2007; 75: 259-267.
15. Jewkes R. Intimate partner violence: causes and prevention. Lancet 2002; 359: 423-1429.
16. Institut National de la Statistique du Rwanda (INSR) and ORC Macro. Rwanda Demographic and Health Survey 2005. Calverton, MA: INSR and ORC Macro, 2006.
17. Dunkle KL, Jewkes RK, Brown HC, Yoshihama M, Gray GE, McIntyre JA et al. Prevalence and patterns of gender-based violence and revictimization among women attending antenatal clinics in Soweto, South Africa. American Journal of Epidemiology 2004; 160: 230-239.
18. Makara-Studzinska M, Gustaw K. Intimate violence by men abusing and non-abusing alcohol in Poland. International Journal of Environmental Research in Public Health 2007; 4: 76-80.
19. Ntaganira J, Muula AS, Masaisa F, Dusabeyezu F, Siziya S, Rudatsikira E. Intimate partner violence among pregnant women in Rwanda. BMC Women's Health 2008; 8: 17.
20. Weinsheimer RL, Schermer CR, Malcoe LH, Balduk LM, Bloomfield LA. Severe intimate partner violence and alcohol use among female trauma patients. Journal of Trauma 2005; 58: 22-29.
21. Sahin HA, Sahin HG. An unaddressed issue: domestic violence and unplanned pregnancies among pregnant women in Turkey. European Journal of Contraceptive and Reproductive Health Care 2003; 8: 93-98.
22. Roche M, Moracco KE, Dixon KS, Stern EA, Bowling JM. Correlates of intimate partner violence among female patients at a North Carolina emergency department. North Carolina Medical Journal 2007; 68: 89-94.
23. UNAIDS. Uniting the World Against AIDS. Rwanda country HIV estimates. (Online) no date. Available: www.unaids.org/en/CountryResponses/Countries/rwanda.asp (Accessed 4 January 2009).
Abstract
Introduction:
Intimate partner violence (IPV) is a major public health problem in Africa and internationally, with consequences that include physical injury, significant morbidity and even death. The Rwandan 2005 Demographic and Health Survey (DHS) reported a national prevalence of IPV among pregnant women of 10.2% but there were limited data available on the factors involved. The aim of this study was to determine the factors associated with and prevalence of IPV among pregnant Rwandese women in the rural southern province of Kabutare.Methods: A total of 387 pregnant women attending antenatal clinics in the South Province of Rwanda answered a questionnaire which included items on demographics and IPV. Mean age and prevalence of IPV in the previous 12 months as well as lifetime IPV were assessed. Both univariate and multivariate odds of IPV exposure were estimated using logistic regression analysis.
Results: The mean age of the 387 participants was 29.4 years (SD 6.3 years). More than one in two participants reported lifetime verbal abuse (53.7%). Other forms of lifetime IPV included pulling hair (9.4%), slapping (18.2%), choking (6.5%), punching with fists (19.3%), throwing to the ground and kicking with feet (12.8%), and burning with a hot liquid (3.1%). In the multivariate analysis, alcohol use by male partner was positively associated with lifetime IPV (OR = 2.52; 95% CI [1.35, 4.71] for occasional drinkers, and OR = 3.85; 95% CI [1.81, 8.21] for heavy drinkers). Compared with subjects with no formal education, women who had elementary education were less likely to report lifetime IPV (OR = 0.30; 95% CI [0.11, 0.78]).
Conclusion: Alcohol use by male partner and low education of women were positively associated with lifetime IPV. The high rates of IPV among Rwandan pregnant women indicate the need for urgent measures to prevent and curb domestic violence using public health education, an awareness campaign and policy advocacy.
Key words: intimate partner violence (IPV), partner violence, Rwanda, women's health.
You might also be interested in:
2020 - A bitter pill to swallow: registered nurses and medicines regulation in remote Australia




