Introduction
Despite rapid economic growth and national development, some segments of the Malaysian population still suffer from malnutrition, particularly protein-energy malnutrition among children. Although severe forms of nutrient deficiency are rare, moderate undernutrition is still widespread in rural communities. The Malaysian Ministry of Health's National Nutrition Surveillance reported the prevalence of severe malnutrition among children under 6 years to be 1.5% in 1983 and 1.1% in 19861. Despite various government interventions over 17 years, this was only reduced to 1% by 2000, with the prevalence of moderate under-nutrition at 13%2. Many of these undernourished children lived in rural communities with a high poverty index. The most affected states are those located on the east coast and northeast areas of peninsular Malaysia, particularly in Kelantan3, which in 2002 had the second highest poverty index with 12% of households below poverty line, compared with the national level of 5%4. Of the 7 counties in this district, Tumpat is ranked as having the third highest level of household poverty (9.6%)5. Tumpat is a low-lying area subject to annual monsoonal flooding. In 2000 its population was 1.29 million consisting of 95% Malay, 3.8% Chinese and 0.9% other ethnic groups6. Its major economic activities concern the provision of services (67.4%), agriculture-paddy planting, aquaculture or cash crops (15.7%), manufacturing (14.1%), construction (2%) and mining (0.9%).
Over the last 50 years, international studies have identified similar factors contributing to under-nutrition among children7. Although diverse and multisectoral, most of these factors are interrelated and encompass family, community and national factors8. Although similar studies have been conducted in Malaysia, there is little information about the way questionnaires are generated, beyond using literature reviews or consultations with colleagues9-12.
There are many methods for developing quantitative questionnaires. One involves the use of qualitative interviews conducted prior to a survey, in order to gather key socio-behavioral information from participants. Indeed, the validity of quantitative research can be enhanced by open interviews conducted in a real-life context. Thus, the present study aimed at developing a questionnaire to determine the factors contributing to malnutrition using both qualitative and quantitative methods. It is hoped that the outcome of the study will assist in providing an intervention that meets local needs. This article concerns the process of questionnaire development and validation.
Method
Phase 1: Qualitative method
An in-depth interview was conducted using a question guide based on Sastry's conceptual framework13; one theme involved identifying factors contributing to malnutrition. A total of 18 nurses and two doctors who worked with malnourished children in Tumpat were interviewed. The findings of the interview were used to construct a conceptual framework and then develop a questionnaire, which included socio-demographic characteristics and anthropometries. The input of a panel of nutrition experts and researchers assisted in further refining the questionnaire content.
Lincoln and Guba's concept of trustworthiness was adopted for content validation of quantitative data14. To ensure dependability of findings, an audit trail included systematic documentation of field notes, and descriptions of the setting, people and location. Methodological decisions and analytic results were recorded, and interviewees confirmed the content of findings before the data were accepted, assuring internal validity. External validity was achieved by ensuring that interviewees were representative of the area studied; in this case, it was determined that the selected health workers were directly involved in the care of children with malnutrition. Finally, confirmability was achieved by documenting procedures used in checking and rechecking using the audit trail method.
Phase 2: Validity and reliability testing
The questionnaire developed in phase 1 was used in phase 2 to collect quantitative data. Phase 2 was conducted in the same district (Tumpat) but with a different population. A sample of 7119 children was identified. Using Statcalc Epi Info v3.5 (CDC; http://www.cdc.gov/EpiInfo/) and the national prevalence of 18% of malnutrition (underweight) among children aged 5 years and under2, 333 children were recruited from 10 randomly selected clinics. Inclusion criteria were for normal children aged 60 months and under who were permanent residents of the area and attended a health clinic, and their mother or caregiver. Respondents comprised two sets: children; and children's mothers or caregivers. Informed consent that conformed to the Malaysian ethical standard for research was obtained from adult respondents. Ethics approval was obtained from the Ethics Committee of the University of Science Malaysia.
All selected children's anthropometric measurements - weight (to the nearest 0.1 kg), height/length and mid-upper arm circumference (to the nearest 0.1 cm) - were recorded. Because some adult respondents were illiterate, a face-to-face interview with the children's mothers or caregivers was conducted using the developed questionnaire. The data obtained were analysed using SPSS for Windows v 14 (SPSS; Chicago, IL, USA).
To determine the questionnaire factorial structure, exploratory factor analysis was performed. Three main stages were involved: first, a correlation matrix was generated using Pearson's r to determine the correlation coefficient between items. An absolute value of rxy between .50 and .79 reflected a moderate to strong relationship between items. Values of more than zero indicated correlation; however, items with very strong relationships (rxy >.80) were deleted15.
Second, the Kaiser-Meyer-Olkin (KMO) and Bartlett's test of sphericity were checked. The KMO test measures sampling adequacy and should be greater than .5 for a satisfactory factor analysis to proceed. Bartlett's test indicates that a correlation matrix is an identity matrix by looking at significant values. Finally, factors were extracted by from the analysis with their eigenvalues, the percent of variance attributable to each factor, and the cumulative variance of the factor and previous factors. A scree plot determined how many factors to retain, and these were rotated to maximize the relationship between variables15. A varimax rotation with a factor loading of .4 was used as lower cut-off value. Varimax rotation was used to maximize variance of the squared loadings of a factor on all variables in the matrix (the most common rotation option for average datasets)15.
Composite reliability was used because it measures overall reliability of a collection of heterogeneous but similar items11. However, because age was the only factor classified as biological, a calculation of composite reliability was not performed.
Results
Phase 1 study - concept elicitation
Qualitative analysis of pooled data revealed 14 concepts. Some had been identified in the preliminary literature review, but were refined in the interviews to obtain a more precise concept description, for example maternal factors (mother's family planning practices); health status (number of hospital admissions, treatment frequency); and diet (percentage calorie intake higher than recommended nutrient intake [RNI], percentage protein intake higher than RNI). The conceptual framework is presented (Fig1).
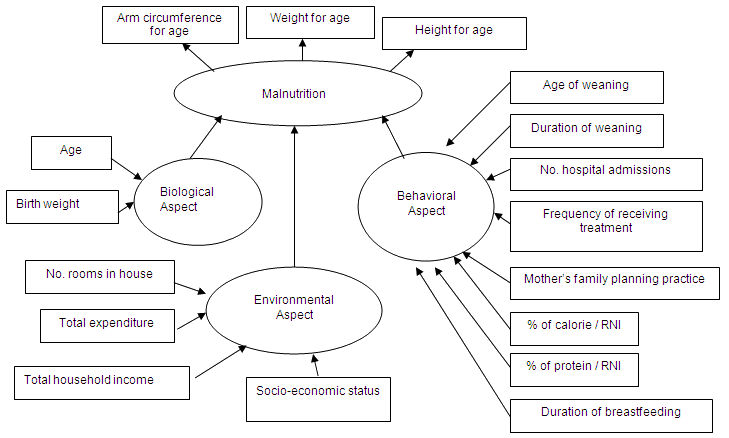
Figure 1: The conceptual framework developed from qualitative data. RNI, Recommended nutrient intake.
Phase 2
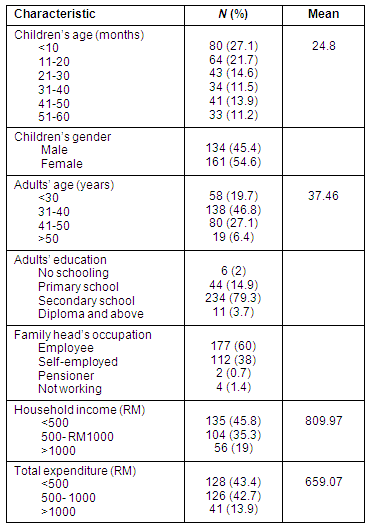
A total of 295 respondents (94% of the targeted response) were recruited, with between 27 and 31 respondents from each of the 10 clinics. The mean children's age was 24.8 months, and that of adult respondents was 37.46 years. Detailed socio-demographic characteristics of the respondents are given (Table 1).
Table 1: Sociodemographic characteristics of the respondents
Factorial structure of the questionnaire
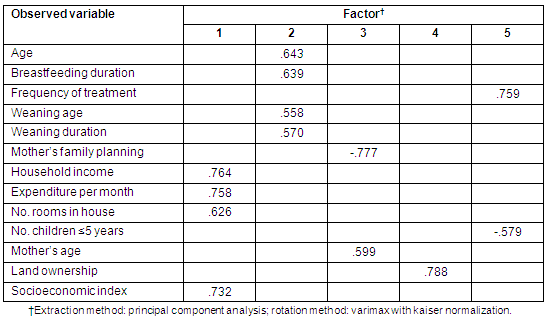
The correlation matrix revealed that rxy for all items were within the range of .15 to .52, therefore no items were rejected. The determinant of the correlation matrix was .209, an indication that there was no linear dependency in the matrix10. The measure of sampling adequacy showed the value of anti-correlation ranged from .531 to .732. Three items (birth weight, percentage of calorie intake based on RNI, and percentage of protein intake based on RNI) were removed due to a value of less than .6010. Barlett's test of sphericity (χ2 = 452.768, p<.001) indicated the correlation matrix was not an identity matrix. Five factors were extracted after rotation using principle component analysis. The total explained variance was 57.6%. Subsequent scree plot analysis revealed that four factors were appropriate. The factor loadings (Table 2) show that four items were loaded on their hypothesized factors, and 5 items were not (mother's family planning, mother's age, land ownership, frequency of treatment, and number of children aged 5 years and under). However, based on Sastry's model13, age was classified as a biological factor; land ownership was classified as an environmental factor; and the remaining items (mother's family planning, mother's age, frequency of treatment and number of children aged 5 years and under) were classified behavioral.
Table 2: Exploratory factor analysis with 13 observed variables for 5 latent variables
Reliability
The composite reliability for environmental and behavioral factors (0.70 and 0.74, respectively) met the basic criteria for reliability set by Raykov16.
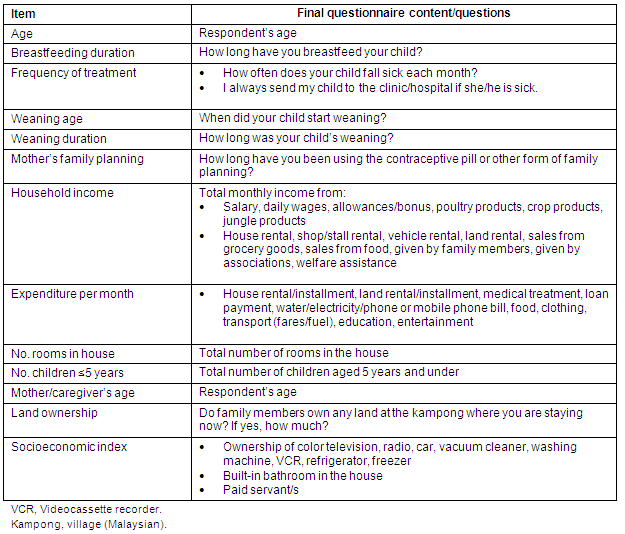
Based on the generated conceptual framework and testing of psychometric properties, the Malay language questionnaire contained 50 items, assessing 7 domains: (i) respondents' background information (race, religion, gender, age, education level, marital status and occupation); (ii) house condition (type of ownership, type of house and number of rooms); (iii) basic necessity and utilities (availability of schools, health facilities, grocery store, water supply, electricity, telephone, toilet, sewage disposal, waste disposal and use of cooking fuel); (iv) property and land ownership (ownership of vehicle and household products, and land ownership); (v) income and expenditure; (vi) child health status (anthropometry status, health history, feeding practices); and (vii) diet (24 hour recall and food preparation). The 13 main questions (translated into English for the purposes of this article) are presented (Table 3).
Table 3: Items and item contents of the final questionnaire
Discussion
The strategy of a 'bottom up' approach to developing the instrument for this study produced good face and content validity. The qualitative methods helped in gaining an understanding of malnutrition among children, especially from phenomena such as directly observable behaviors. In this study, the views of health workers were incorporated at the questionnaire development stage. This was because, as well as acting as screening and referral tools for identifying participant children, the health workers were regarded as partners with the mothers in combating malnutrition among the children17.
The developed questionnaire is easy to use, taking approximately 30-40 min to complete at home or in a clinic. The questions are simple and easy to administer, and suitable for mothers or caregivers who are not highly educated or familiar with health terminology. Although further validation of this approach to studying malnutrition in children in other areas would be ideal, the questionnaire could be used in national surveys to identify malnutrition risk factors and to target related interventions, especially in a rural setting.
One methodological limitation for consideration is the use of purposive sampling to recruit participants for the in-depth interview, which could have introduced sampling bias. However, this was minimized by recruiting health workers from different clinics within the study area.
Based on the exploratory factor analysis, three main contribution factors were identified: biological, environmental and behavioral. The biological factor age was considered a significant indicator of malnutrition because studies18,19 have shown that most affected children are 12 months old and above. This is probably due to poor feeding practices, particularly during the transition from weaning to solid food.
Four environmental items were identified: total household income, total expenditure, number of rooms in the house, and socioeconomic status. Mean household income was RM809.97 with the highest percentage (45.8%) in the income group below RM500 per month. Lower income was very much related to the category of occupation because 60% of the studied population was self-employed, particularly in construction work. Based on the researchers' field survey, self-employment was not a reliable source of income, because these workers depended on the availability of housing projects. Total household expenditure indicated an average of RM659.07 was used at home every month, which was high in relation to the average reported income of RM809.97. Based on a researcher's field observation, although the cost of living was low in the studied areas due to comparatively low food prices, few families could make monthly savings. The number of rooms in the house was associated with income20; where income increased, the number of rooms in the house also increased. The final environmental item, socioeconomic status, was represented by vehicle ownership and basic household products. Households with higher socioeconomic status were usually financially better off. After spending on food and other basic necessities (eg water, electricity), remaining income was spent on purchasing household products (eg televisions, radios, washing machines, DVD players) and on motor vehicles. Households with higher socioeconomic status are likely to have children with a higher weight for age z-score8.
Behavioral factors such as feeding and childcare practices were likely to account for some of this household effect. Feeding and childcare practices are important contributors to the healthy growth and development of children18. Breastfeeding is one of the most important household actions influencing children's nutritional outcomes. Exclusive breastfeeding for at least the first 6 months of life provides a baby with adequate nutrients and antibodies, and eliminates the risk of illness associated with the use of formula feeding utensils. However, prolonged breastfeeding can reduce the total food intake and thus predispose a child to malnutrition18. Prolonged breast-feeding also leads to significant underweight, especially among one year-old children18, particularly those who have not yet commenced weaning. In this case, if the mother is pregnant she is at risk of under-nourishment herself.
This questionnaire was developed in a rural district in Kelantan, therefore generalization can be only be made to other sites with similar characteristics. However, previous studies in this area have only used small samples in questionnaire validation. The major strength of this unique questionnaire is that it has been validated by a qualitative method, followed by systematic testing of its psychometric properties.
References
1. Ministry of Health Malaysia. National Nutrition Surveillance. Report on Family Health Programme Towards Preparation of 6MP. Kuala Lumpur: Family Health Division, Ministry of Health, 1989.
2. Ministry of Health Malaysia. Annual Report 2000. Kuala Lumpur: Ministry of Health, 2000.
3. Zulkifli A, Khairul AA, Atiya AS. The nutritional status of children in resettlement village in Kelantan. Southeast Asian Journal of Tropical Medical Health1999; 30(1): 122-128.
4. Malaysia Five Year Plans. Malaysia quality of life index. Kuala Lumpur: The Government Press, 2002.
5. Government of Malaysia. Mid-term review of the Eighth Malaysia Plan 2001-2005, Kuala Lumpur: The Government Press, 2002.
6. Department of Statistics. Population and housing census of Malaysia: population distribution and basic demographic characteristics. Kuala Lumpur: Department of Statistics Malaysia, 2000.
7. Kikafunda JK, Walker AF, Collet D, James FT. Risk factors for early childhood malnutrition In Uganda. Paediatrics 1988; 102(4): 45.
8. Griffiths P, Madise N, Whitworth A, Matthews Z. A tale of two continents: a multilevel comparison of the determinants of child nutritional status from selected African and Indian regions. Health & Place2004; 10: 183-199.
9. Chee HL, Khor GL, Fatimah A, Wan Abdul Manan WM, Mohd Nasir MT, Nik Shanita S et al. Nutritional assessment of pre-school children in rural villages for the family dynamics, lifestyles and nutrition study (1997-2001). Prevalence of undernutrition and relationship to household socio-economic indicators. Malaysian Journal of Nutrition 2002; 8(1): 33-53.
10. Khor GL, Zalilah MS. Dual forms of malnutrition in the same households in Malaysia - a case study among Malay rural households. Asia Pacific Journal of Clinical Nutrition 2003; 12(4): 427-438.
11. Norhayati M, NoorHayati MI, Mohammod CG, Oothuman P, Azizi O, Fatimah A et al. Malnutrition and its risk factors among children 1-7 years old in rural Malaysian communities. Asia Pacific Journal of Clinical Nutrition 1997; 6(4): 260-264.
12. Zamaliah MM, Mohd Nasir MT, Khor GL, Tee ES. Socio-economic determinants of nutritional status of children in rural peninsular Malaysia. Asia Pacific Journal of Clinical Nutrition 1998; 7(3/4):307-310.
13. Sastry N. Community characteristics, individual and household attributes, and child survival in Brazil. Demography 1996; 33(2): 211-230.
14. Lincoln YS, Guba EG. Naturalistic inquiry. Thousand Oakes, CA: Sage, 1985.
15. Pett MA, Lackey NR, Sullivan JJ. Making sense of factor analysis. The use of factor analysis for instrument development in health care research. London: Sage, 2003.
16. Raykov T. Estimation of composite reliability for congeneric measures. Applied Psychological Measurement 1997; 21: 173-184.
17. Tchibindat F, Martin-Prevel Y, Kolsteren P, Maire B, Delpeuch F. Bringing together viewpoints of mothers and health workers to enhance monitoring and promotion of growth and development of children: A case study from the Republic of Congo. Journal of Health and Population Nutrition 2004; 22(1): 59-67.
18. Caufield LE, Bentley ME, Ahmed S. Is prolonged breastfeeding associated with malnutrition? Evidence from nineteen demographic and health surveys. International Journal of Epidemiology 1996; 25(4): 693-703.
19. Phengxay M, Ali M, Yagyu F, Soulivanh P, Kuroiwa C, Ushijima H. Risk factors for protein-energy malnutrition in children under 5 years: study from Luangprabang Province, Laos. Pediatrics International 2007; 49(2): 260-265.
0. Bendley M, Maureen W, Valerie F, Owen L, Lee C. Determinants of childhood malnutrition in Jamaica. Food and Nutrition Bulletin (Online) 1988; 10(1). Available: http://www.unu.edu/Unupress/food/8F101e/8F101E00.htm (Accessed 24 July 2009).
Abstract
Introduction: Historical data have shown that the factors contributing to and underlying malnutrition among children are diverse, multisectoral and include interrelated biological, social, cultural and economic factors. To determine the these factors in a given population an accurate and reliable questionnaire is essential. This article concerns the process of questionnaire development and validation.
Method: This study was based on a previously described conceptual framework of malnutrition in children and was conducted in two phases. During the first phase, an in-depth interview using a semi-structured questionnaire was conducted of 20 health workers who provide direct care for the malnourished study children in rural Kelantan, Malaysia. Based on these findings a theoretical framework was generated to assist the development of quantitative questionnaire. The developed questionnaire was then tested using a quantitative approach to establish its reliability and validity.
Results: Qualitative analysis of the in-depth interview revealed 17 items that were used to build a conceptual framework for questionnaire development. The questionnaire was then administered to 295 children and their parents/caregivers, with 28.76-35.28% of the children showing signs of malnutrition in the form of stunting, wasting and underweight. Exploratory factor analysis revealed two factors: environmental and behavioral with composite reliability of 0.70, and 0.74, respectively. The quantitative findings identified 14 items which were further tested with factor loadings, showing loading on to 2 factors.
Conclusion: The developed instrument offers a potentially valid and reliable tool to determine the factors contributing to malnutrition among children in rural and poor communities in Tumpat, Kelantan, Malaysia.
Key words: children, Malaysia, malnutrition, questionnaire development.
You might also be interested in:
2013 - Ophthalmological disorders in rural areas of Crete: a geospatial analysis


