Introduction
Despite varied cultural, historical, geographical and genetic backgrounds, many Aboriginal populations around the world are experiencing dramatic increases in diabetes prevalence1. In Canada, approximately 5% of the population has been diagnosed with diabetes2. There are ethnic differences in diabetes prevalence1,3-6, and Canadian Aboriginals (First Nations, Métis [those of mixed blood] and Inuit) are considered a high-risk population7. Prevalence rates are reportedly 2 to 5 times higher among First Nations individuals than the general Canadian population8-10. Although the eruption of diabetes has been relatively well-characterized in First Nations and the general Canadian population from administrative or survey methodology1,9,11, there is much less information with respect to diabetes risk-factors or the prevalence of undiagnosed diabetes.
In the province of Alberta we accessed databases of three separate community-based diabetes and diabetes-risk screening projects12-14, creating a unique subject pool of First Nations, Métis and non-Aboriginal adult individuals without diabetes. In Alberta approximately 40 000 First Nations (treaty or status) individuals live on reserves negotiated by federal treaties, while another 60 000 live off reserves15. Approximately 8000 Métis individuals live on Métis Settlements with distinct land bases in rural northern Alberta. The Métis have a unique cultural identity different from First Nations. Many other Métis (approximately 75 000) do not live on settlements and have no land base (these individuals identify with the Métis Nation)15. We tested whether ethnicity was a factor contributing to differences in diabetes risk-factors, or to the prevalence of undiagnosed diabetes in rural Alberta.
Methods
Screening projects
The 'Screening for Limb, I-Eye, Cardiovascular, and Kidney complications of diabetes' (SLICK) project has travelled to each of the 44 Alberta First Nations communities (most of which are remote or rural) since 2001 providing diabetes risk assessment, diabetes complications screening and community-based care13. Since 2003, the Mobile Diabetes Screening Initiative (MDSi) has travelled to rural Aboriginal 'off-reserve' and remote Alberta communities providing diabetes screening14. Approximately 50% of MDSi clients live in Métis settlements. Finally, Believing we can Reduce the Aboriginal Incidence of Diabetes (BRAID) has been screening the on-reserve population of a single rural Alberta First Nation for diabetes since 200312. Each project received approval from the Ethics Review Board of the University of Alberta. The data presented in this article were collected between October 2003 and June 2007.
Subjects
Adult subjects (≥18 years old) without known diabetes were referred or self-referred from within the Aboriginal communities or rural towns by local bookers (community members who helped to arrange for potential subjects to engage with the screening program) and health professionals, with help from local advertising. A total of 3148 subjects were included (1037 males and 2111 females). Off-reserve subjects self-defined their ethnicity, and on-reserve subjects were assumed to be First Nations (status or non-status) unless otherwise noted. The following groups resulted: First Nations (n = 1790), Métis (867) and non-Aboriginal (491).
Measurements
Each project deploys mobile clinics equipped with healthcare personnel and portable technology into the communities. Detailed methodology has been reported elsewhere13. All subjects were counseled on-site regarding testing results, and encouraged to follow up with their physicians, particularly with respect to re-assessment or confirmation of abnormalities of fasting plasma glucose (FPG; ideally with an oral glucose tolerance test). Age, reported history of gestational diabetes (GDM) or babies over nine pounds (females only), body mass index (BMI), waist circumference, hemoglobin A1c (A1c), FPG and random plasma glucose (RPG) were measured. We assessed the presence of overweight (BMI 25-29.9), obesity (BMI >30), abnormal waist circumference (>102 cm males, >88 cm females)16, undiagnosed diabetes (FPG >6.9 or RPG >11.0 or A1c >7.0%) and pre-diabetes (according to both the Canadian [CDA] and American Diabetes Association [ADA] criteria: FPG 6.1-6.9 and FPG 5.6-6.9, respectively)7,17.
Blood pressure (BP) and serum lipids, as well as the prevalence of hypertension (BP >140/90), hypercholesterolemia (total cholesterol >5.24 mmol/L), high total to high-density lipoprotein (HDL) cholesterol ratio (>3.94), hypertriglyceridemia (fasting value >1.44 mmol/L) and metabolic syndrome16 were also assessed (because information about anti-hypertensive and lipid-lowering medications was not always reliably collected these data were not a focal point of our interpretation).
Statistical analysis
The statistical significance of differences between groups was assessed using overall χ2 tests. Additional χ2 tests were performed to test the significance of differences between: (i) First Nations and Métis; and (ii) First Nations and non-Aboriginal. Logistic regression analyses were used to assess the statistical significance of between group differences after adjusting for age and gender. Odds ratios (OR) were determined relative to First Nations.
Results
The ratio of males : females did not differ between groups. The non-Aboriginal group was older (48.8 ± 15.4 mean years) and had the lowest mean values for waist circumference (97.6 ± 16.7 cm), BMI (30.0 ± 6.4) and RPG (6.3 ± 1.5 mmol/L) (p<0.01). The highest mean values for waist circumference (104.7 ± 15.6 cm), BMI (31.2 ± 6.6) and RPG (6.7 ± 1.9 mmol/L) were found in First Nations subjects (p<0.01). Despite group differences in mean RPG, there were no differences in FPG or A1c levels.
Prevalence results are listed (Table 1). The proportion of individuals who were overweight/obese or who had abnormal waist circumferences was highest in the First Nations group (84.4% and 76.8%, respectively; p< 0.01). The highest prevalence of a history of gestational diabetes (GDM) was found in First Nations women (9.0%), compared with 4.5% and 5.2% of the Métis and non-Aboriginal groups, respectively (p<0.01). Significant differences (p<0.01) were apparent when using the ADA criteria for pre-diabetes, with Métis having the highest prevalence (43.9%). There was no difference in the prevalence of undiagnosed diabetes. Individual p-values for comparisons between First Nations/Métis, as well as First Nations/non-Aboriginal are given in Table 1 for statistically significant overall comparisons. First Nations were more likely to be obese (p<0.01), whereas Métis were more likely to be overweight (p = 0.04).
Table 1: Prevalence of anthropometric and clinical variables
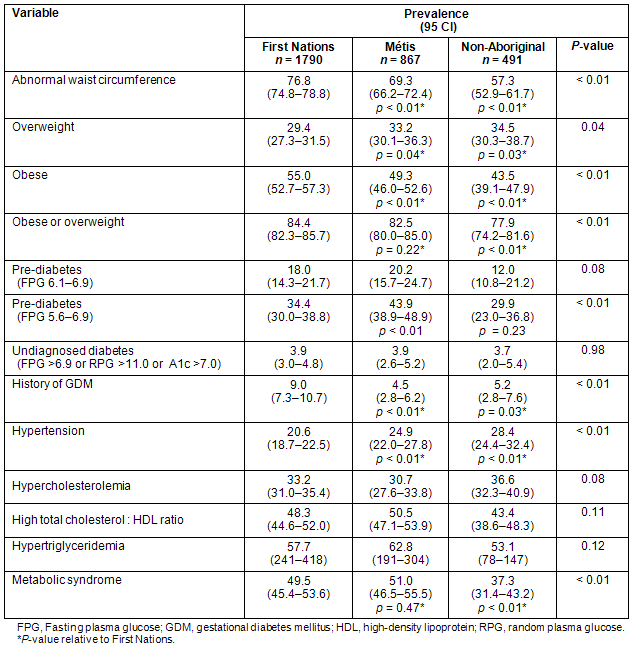
After age and gender adjustments, the First Nations group were still more likely to be obese and to have high waist circumferences; however, there was a gradient whereby the Métis had intermediate values and the non-Aboriginal group had the lowest values (OR 0.8, p = 0.01 for Métis obesity, OR 0.7, p<0.01 for Métis abnormal waists, compared with non-Aboriginals OR 0.62 and 0.35, p<0.01 for both obesity and abnormal waists respectively). Métis women were less likely to have a history of GDM (OR 0.46; p<0.01) compared with the First Nations group. There was also a trend for First Nations and Métis to be more likely to have metabolic syndrome than non-Aboriginals (OR 0.63 for non-Aboriginals, 1.07 for Métis, p = 0.03). Finally, individuals in the non-Aboriginal group were less likely to have pre-diabetes (OR 0.50; p = 0.01) and Métis were more likely to have pre-diabetes (OR 1.39; p = 0.03).
Discussion
We have shown that rural First Nations individuals have more risk factors for diabetes, including higher RPG, higher rates of obesity and of abnormal waist circumferences, and higher prevalence of self-reported GDM compared with rural Métis and non-Aboriginal individuals. A gradient whereby Métis individuals have some intermediate results emerged. Additionally, our results reveal high rates of obesity, undiagnosed diabetes and pre-diabetes among rural adults, regardless of ethnicity.
According to survey data, approximately 58% of the adult Canadian population was overweight or obese in 200518. First Nations, Métis and rural non-Aboriginals groups reported on here had much higher rates (84%, 83% and 78%, respectively), although interpretation requires caution as individuals were self-referred or selected because of presumed risks (such as obesity or family history of diabetes). Regardless, the advantage of this data is that anthropometrics were measured (self-reports tend to be an underestimate). Other reports have confirmed a higher prevalence of obesity in rural Canada19-21, and high rates of undiagnosed diabetes were related to obesity among First Nations individuals8,22. From administrative database analysis it was also recently shown that the greatest increases in diabetes incidence are among rural men (compared with rural women, or urban men or women), regardless of ethnicity23. However, urban/rural differences in the prevalence of obesity and its related co-morbidities do not appear to be universal; in-fact, in many countries the prevalence rates of both diabetes and obesity are slightly higher in urban compared with rural areas1,24.
Even after age and gender adjustment, First Nations subjects tended to be more overweight/obese and had higher waist circumferences. Moreover, First Nations individuals had the highest prevalence of reported GDM. There is increasing evidence that pre-gestational or GDM contributes to the high prevalence of diabetes among First Nations individuals8-10,25, a phenomenon also seen in non-Aboriginal populations.
From 2005 administrative data, the prevalence of diabetes in First Nations and non-First Nations individuals in Alberta was 12% and 5%, respectively9. No comparable data on the Métis is available, but survey data estimated a prevalence rate of 6% in 200026. Taken together, differences we observed in weight, waist circumference, metabolic syndrome and GDM are therefore consistent with known differences in diabetes prevalence between First Nations, Métis and non-Aboriginals. This is consistent with international data, showing higher rates of obesity and diabetes for many Aboriginal populations in the United States, Australia, Polynesia and other countries in comparison with respective general populations1,27-30.
Potential reasons for our reported differences found cannot be determined from this study, but may include genetics and/or socioeconomic factors. For example, a single nucleotide polymorphism was discovered in transcription factor HNF-1α among the Oji-Cree of northwestern Ontario and Manitoba that was associated with increased type 2 diabetes risk31. However, nothing is known about this mutation in Alberta First Nations populations. Numerous other susceptible genes associated with type 2 diabetes have been identified in different populations, and recent research suggests that these genetic factors may need to be modified by environmental factors for overt diabetes to develop32,33. A 2004 report by the Canadian Institute for Health Information revealed that Aboriginals experience inferior social, economic and environmental conditions compared with other Canadians, leading to increased disease burden34. Low household income has been associated with higher diabetes prevalence35, and census data found 40% of First Nations and 28% of Métis were in a low income bracket, compared with 16% for other Canadians in 200034.
An important limitation was that subjects were not from a population-based sample and may have been those most health-concerned; however, this would have been true for all groups. Although our results may not be representative, they provide novel community-based information comparing obesity and diabetes risk among rural First Nations, Métis and non-Aboriginal individuals.
Conclusion
In conclusion, rural First Nations adults have more diabetes risk-factors compared with rural Métis and non-Aboriginal adults, but there seems to be a gradient whereby Métis have intermediate risk.
Acknowledgments
The authors thank all of the subjects and leaders who welcomed SLICK, MDSi and BRAID into their communities. Thanks are also due to the field team members, the Alberta Aboriginal Diabetes Initiative committee, and to Sheri Pohar for providing data analysis. Funding was provided by CIHR (Canadian Institutes of Health Research), the University of Alberta, Health Canada (Canadian Health Information Partnership Program - CHIPP) and Alberta Health and Wellness.
References
1. Yu CH, Zinman B. Type 2 diabetes and impaired glucose tolerance in Aboriginal populations. A global perspective. Diabetes Research and Clinical Practice 2007; 78(2):159-170.
2. Statistics Canada. Diabetes care in Canada: Results from selected provinces. (Online) 2005. Available: http://www.statcan.ca/bsolc/english/bsolc?catno=82-621-X20060029224 (Accessed 12 December 2008).
3. Harris MI, Flegal KM, Cowie CC, Eberhardt MS, Goldstein DE, Little RR et al. Prevalence of diabetes, impaired fasting glucose, and impaired glucose tolerance in US adults. The third national health and nutrition examination survey, 1988-1994. Diabetes Care 1998; 21(4):518-524.
4. Anand SS, Yusuf S, Vuksan V, Devanesen S, Teo KK, Montague PA et al. Differences in risk factors, atherosclerosis and cardiovascular disease between ethnic groups in Canada: The study of health assessment and risk in ethnic groups (SHARE). Indian Heart Journal 2000; 52(Suppl7):S35-S43.
5. Narayan KM, Boyle JP, Thompson TJ, Sorensen SW, Williamson DF. Lifetime risk for diabetes mellitus in the United States. Journal of the American Medical Association 2003; 290(14):1884-1890.
6. Wild S, Roglic G, Green A, Sicree R, King H. Global prevalence of diabetes: estimates for the year 2000 and projections for 2030. Diabetes Care 2004; 27(5):1047-1053.
7. Canadian Diabetes Association. Canadian Diabetes Association. 2008 Clinical practice guidelines for the prevention and management of diabetes in Canada. Canadian Journal of Diabetes 2008; 32(Suppl1). Available: http://www.diabetes.ca/files/cpg2008/cpg-2008.pdf (Accessed 25 May 2009).
8. Young TK, Reading J, Elias B, O'Neil JD. Type 2 diabetes mellitus in Canada's First Nations: Status of an epidemic in progress. Canadian Medical Association Journal 2000; 163(5): 561-566.
9. Alberta Diabetes Surveillance System. Alberta diabetes atlas. Edmonton, Alberta: ADSS, 2007.
10. Dannenbaum D, Kuzmina E, Lejeune P, Torrie J, Gangbe M. Prevalence of diabetes and diabetes-related complications in First Nations communities in northern Quebec (Eeyou Istchee), Canada. Canadian Journal of Diabetes 2008; 32(1): 46-52.
11. National Diabetes Surveillance System. Diabetes in Canada, second edition. Ottawa, Ontario: NDSS, 2002.
12. Kaler SN. The BRAID study: believing we can reduce the Aboriginal incidence of diabetes. University of Alberta, Edmonton; 2005. (Thesis)
13. Virani S, Strong D, Tennant M, Greve M, Young H, Shade S et al. Rationale and implementation of the SLICK project: Screening for limb, I-eye, cardiovascular and kidney (SLICK) complications in individuals with type 2 diabetes in Alberta's First Nations communities. Canadian Journal of Public Health 2006; 97(3): 241-247.
14. Kaler SN, Ralph-Campbell K, Pohar S, King M, Toth E. High rates of the metabolic syndrome in a First Nations community in Alberta: prevalence and determinants in adults and children. International Journal of Circumpolar Health 2006; 65(5): 389-402.
15. Statistics Canada. Aboriginal peoples in Canada in 2006: Inuit, Métis and First Nations, 2006 census. (Online) 2006. Available: http://www12.statcan.ca/english/census06/analysis/aboriginal/first.cfm (Accessed 5 June 2008).
16. Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults. Executive summary of the third report of the National Cholesterol Education Program (NCEP) expert panel on detection, evaluation, and treatment of high blood cholesterol in adults (adult treatment panel III). JAMA 2001; 285(19): 2486-2497.
17. American Diabetes Association. Diagnosis and classification of diabetes mellitus. Diabetes Care 2008; 31(Suppl1): S55-S60.
18. Statistics Canada. Canadian community health survey: Obesity among children and adults. (Online) 2005. Available: http://www.statcan.ca/bsolc/english/bsolc?catno=82-621-X20060029224 (Accessed 12 December 2008).
19. Reeder BA, Chen Y, Macdonald SM, Angel A, Sweet L. Regional and rural-urban differences in obesity in Canada. Canadian heart health surveys research group. Canadian Medical Association Journal 1997; 157(Suppl1): S10-S16.
20. Plotnikoff RC, Bercovitz K, Loucaides CA. Physical activity, smoking, and obesity among Canadian school youth. Comparison between urban and rural schools. Canadian Journal of Public Health 2004; 95(6): 413-418.
21. Bruner MW, Lawson J, Pickett W, Boyce W, Janssen I. Rural Canadian adolescents are more likely to be obese compared with urban adolescents. International Journal of Pediatric Obesity 2008; 3(4): 205-211.
22. Harris SB, Gittelsohn J, Hanley A, Barnie A, Wolever TM, Gao J et al. The prevalence of NIDDM and associated risk factors in Native Canadians. Diabetes Care 1997; 20(2): 185-187.
23. Johnson JA, Vermeulen SU, Toth EL, Hemmelgarn BR, Ralph-Campbell K, Hugel G et al. Increasing incidence and prevalence of diabetes among status Aboriginal men in rural and urban Alberta, 1995 - 2006. Canadian Journal of Public Health 2009; 100(3): (in press).
24. Mascie-Taylor CG, Goto R. Human variation and body mass index: a review of the universality of BMI cut-offs, gender and urban-rural differences, and secular changes. Journal of Physiological Anthropology 2007; 26(2): 109-112.
25. Franks PW, Looker HC, Kobes S, Touger L, Tataranni PA, Hanson RL et al. Gestational glucose tolerance and risk of type 2 diabetes in young Pima Indian offspring. Diabetes 2006; 55(2): 460-465.
26. Statistics Canada. Aboriginal peoples survey 2001 - initial findings: Well-being of the non-reserve aboriginal population. (Online) 2003. Available: http://www.statcan.gc.ca/bsolc/olc-cel/olc-cel?catno=89-589-X&CHROPG=1&lang=eng (Accessed 12 December 2008).
27. King H, Rewers M. Global estimates for prevalence of diabetes mellitus and impaired glucose tolerance in adults. WHO Ad Hoc Diabetes Reporting Group. Diabetes Care 1993; 16(1): 157-177.
28. Centers for Disease Control and Prevention: Morbidity and Mortality Weekly Report. Diabetes Prevalence Among American Indians and Alaska Natives and the Overall Population - United States, 1994-2002. JAMA 2003; 290(12): 1571-1573.
29. O'Dea K, Rowley KG, Brown A. Diabetes in Indigenous Australians: possible ways forward. Medical Journal of Australia 2007; 186(10): 494-495.
30. New Zealand Ministry of Health. A Portrait of Health: Key results of the 2002/03 New Zealand Health Survey. (Online) 2004. Available: http://www.moh.govt.nz/moh.nsf/0/3D15E13BFE803073CC256EEB0073CFE6/$File/aportraitofhealth1.pdf (Accessed 08 April 2009).
31. Hegele RA, Cao H, Harris SB, Hanley AJ, Zinman B. The hepatic nuclear factor-1alpha G319S variant is associated with early-onset type 2 diabetes in Canadian Oji-Cree. Journal of Clinical Endocrinology & Metabolism 1999; 84(3): 1077-1082.
32. Florez JC. Clinical review: the genetics of type 2 diabetes: a realistic appraisal in 2008. Journal of Clinical Endocrinology and Metabolism 2008; 9(12): 4633-4642.
33. Adeghate E, Schattner P, Dunn E. An update on the etiology and epidemiology of diabetes mellitus. Annals of the New York Academy of Sciences 2006; 1084: 1-29.
34. Canadian Institute of Health Information. Improving the health of Canadians: Aboriginal peoples health. Ottawa, Ontario: CIHI, 2004.
35. Kelly C, Booth GL. Diabetes in Canadian women. Women's Health 2004; 4(Suppl1): S16.

