Introduction
The study of contraception use is an important topic of research for multiple disciplines, including sociology, demography, epidemiology, public health and medicine. By examining patterns of contraception choices made by sexually active adults, insights about population control and family planning1-5, intentionality regarding pregnancy5-7 and sexually transmitted disease prevention8 are forged. Much of the current research on birth control choices overall has been conducted on non-US populations9-11, with the majority of the research performed on populations in developing countries1-3,12. This is doubly true when examining contraceptive choices made by rural in comparison with urban populations1-4,13-14.
Even though sexually active US adults have a wide variety of birth control methods to choose from, there is limited population-based research comparing the contraceptive choices of non-metropolitan or rural US adults with metropolitan or urban US adults. There are two exceptions. The first is the research of Hartlagea et al4 which examined by urban/rural place of residence the contraceptive choices made by mid-western US women aged 13-55 years. This study is limited, however, by the choice of studying a single region in the country and by excluding men. The second exception is the research of Rosenfeld and Everett14 in which women aged 18-50 years in rural Tennessee and in suburban-urban Baltimore were interviewed about their memories of early contraceptive use. This study was limited by the same issues because it studied regional groups and excluded men.
The study reported here sought to address the gap in the current literature on contraception choice by comparing the birth control choices made by US rural adults with urban ones. This research should help reduce the paucity of studies in this important area of inquiry.
The analyses undertaken in this study involved a number of social variables including: race/ethnicity, household income, gender, educational attainment and marital status. Health service variables (health insurance status, whether or not children less than 18 years were living in the household, deferring medical care because of cost and having a personal healthcare provider) were also included in the analyses.
As a comparative analysis of urban and rural adult populations, this research effort joins a recently formed dialog in population health focused on assessing health-related differences between rural and urban populations to detect whether these are indicative of health disparities. Education and healthcare delivery may need to be adjusted to respond to differences identified.
Methods
The database
Data were obtained from the 2004 Behavioral Risk Factor Surveillance System (BRFSS) database. The BRFSS is a cross-sectional, random digit telephone survey that was a collaborative project of the Centers for Disease Control and Prevention (CDC), and all US states and territories, targeting adults from age 18 to 99 years. The survey's objective wais to collect uniform, state-specific data on non-institutionalized adult's preventive health practices and risk behaviors. Data are self-reported responses to mostly forced-choice questions.
The 2004 data were used because they were the most recent data collected where the family planning module questions were asked of all respondents from all states. Reported analyses were performed on weighted data to provide a stratified representation of the US adult population15. A detailed description of the BRFSS survey design and sampling measures can be found elsewhere16.
Preparing data for analysis
Six original BRFSS variables (age, education, annual household income, marital status, race/ethnicity, and birth control method used) were re-coded for the analyses presented here. Since the data were collected in multiple categories, in order to have more meaningful analyses, this approach required collapsing the multiple response categories into fewer ones. For each of the re-coded variables, respondents refusing to answer the questions were coded as missing and removed from the analysis. Table 1 displays the re-coded variables according to their original format and response categories, their re-coded format and the rationale supporting the re-coding decision.
Table 1: Original variables and response categories with re-coded response categories and rationale for changes, 2004 BRFSS data17
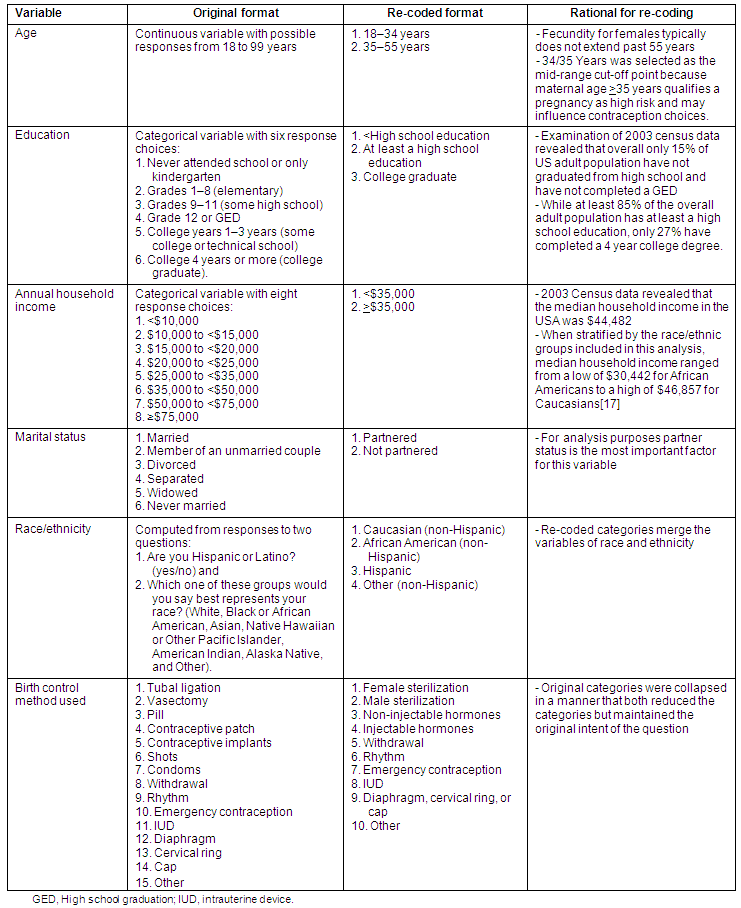
Urban or rural place of residence was determined by computing a single state/county FIPS code from individual state and county FIPS codes and then re-coding the state/county FIPS code as either urban or rural, based on the 2003 Rural-Urban Continuum Codes from the US Office of Management and Budget. Only respondents with both a state and county FIPS code were included in the analyses conducted. All analyses were performed on weighted data.
Statistical analysis
In addition to univariate and bivariate descriptive analyses, a multivariate regression model was performed with rural or non-metropolitan adults using 'birth control' as the dependent variable. The independent variables entered into the model were: birth control choices, race/ethnicity, age, sex, education, household income, health insurance status in the past 12 months, having an identified healthcare provider, deferring medical care in the past 12 months because of cost, marital status, have children less than 18 years living at home, and feelings about having a child. Alpha was set at .05 for all tests of statistical significance. The Statistical Package for Social Scientists Complex Samples v17.0 (SPSS, Chicago, IL, USA) was used to complete the analyses to account for the complex survey design. The research was approved by the Institutional Review Board of the University of Illinois-Chicago College of Medicine at Rockford.
Results
In 2004, 29 311 adults (unweighted), identifiable as rural, aged 18-55 years responded to the BRFSS survey. Weighted they represented 8222, 794 people. Slightly more that 64% of these respondents reported using contraception of some sort. Table 2 displays demographic and health services information about this population.
Table 3 presents the aggregated data of the rural group who reported using contraception, compared with their urban counterparts. There were three relationships emergent from the bivariate analysis worth noting. First, when comparing adults using contraception by place of residence and gender, non-metropolitan adults using contraception were more likely to be have an income of less than $35,000 (OR 1.367, 95% CI 1.364-1.369). Second, when comparing adults using contraception by place of residence and deferring medical because of cost, rural adults using contraception were more likely to have deferred medical care because of cost (OR 1.210, 95% CI 1.207-1.213). Third, when comparing adults using contraception by place of residence and health insurance status, rural adults using contraception were less likely to have health insurance (OR .784, 95% CI .783-.786).
Table 4 shows the comparison of contraception choices and preferences of rural and urban adults. The most frequently reported choice for urban adults was non-injectable hormones ('the pill'); whereas, for rural adults it was female sterilization closely followed by non-injectable hormones. For males and females alike, rural residents were more likely to use permanent sterilization than their urban counterparts. Urban adults were more likely to use condoms than rural adults. Surprisingly, neither group reported a high use of intrauterine devices (IUD).
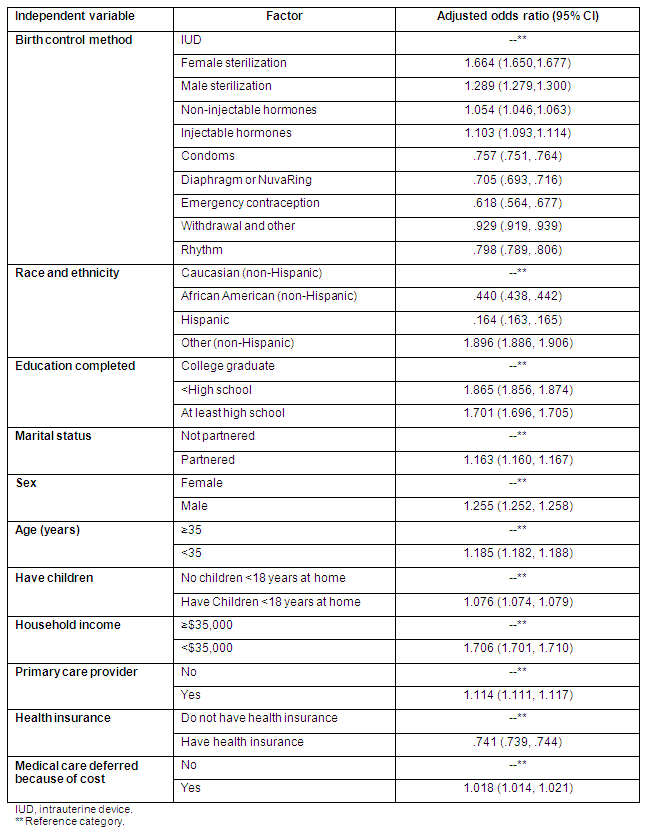
Multivariate regression analysis performed with 'rural adult use of birth control' as the dependent variable is presented in Table 5; it confirmed that rural adults were more likely to use sterilization and less likely to use condoms for birth control. They were also less likely to use: a diaphragm or NuvaRing® (see footnote to Table 4), emergency contraception, and/or withdrawal or rhythm methods. This analysis also confirmed that rural individuals using contraception were more likely to have an income less than $35,000 or to be without healthcare insurance. In addition, they are more likely to have a primary or a personal healthcare provider.
Table 2: Rural adult population aged 18-55 years, 2004 BRFSS data (weighted n = 8222794)
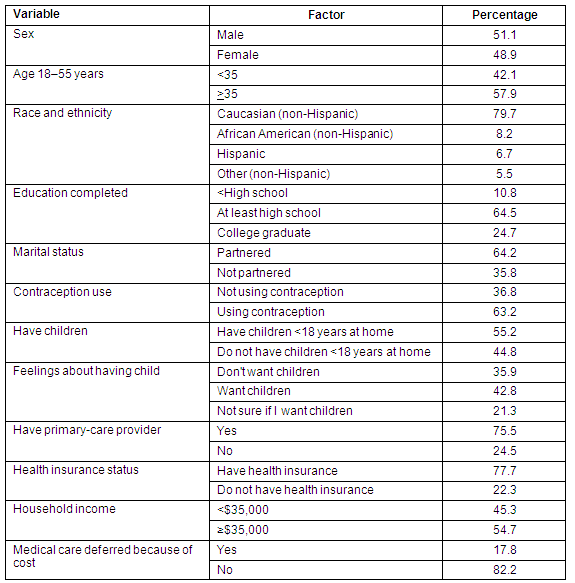
Table 3: Comparison of urban and rural adults aged 18-55 years using contraception, 2004 BRFSS data
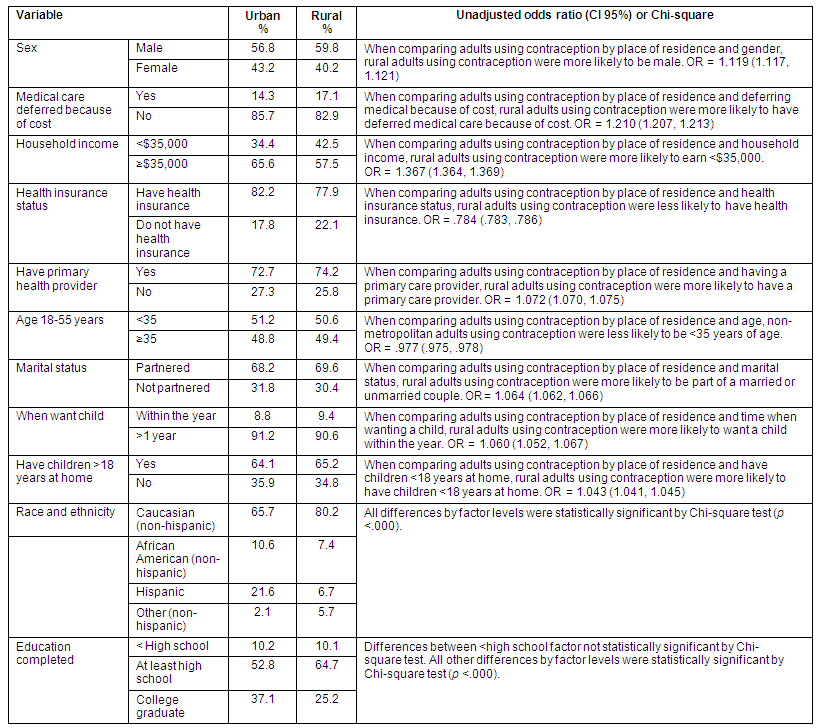
Table 4: Comparison of contraception choice preferences of urban and rural adults aged 18-55 years, 2004 BRFSS data
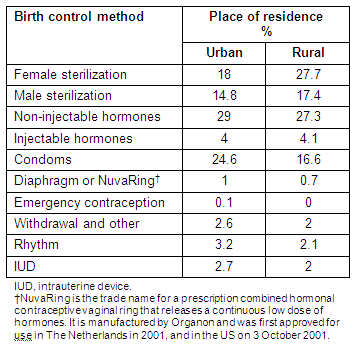
Table 5: Logistic regression analysis: rural adults aged 18-55 years using contraception, 2004 BRFSS data
Discussion
Since rural or more remote areas of the USA are perpetually faced with difficulties accessing general healthcare services such as providers, pharmacists and pharmacy services18,19, rural adults could find their choices of contraceptive methods limited. These recognized limitations to healthcare service access might lead rural adults to choose birth control methods not requiring medication prescription or frequent office visits. Adults faced with these challenges would more likely use rhythm or withdrawal methods, or over the counter (OTC) products such as condoms or spermacide.
The results of this study highlight some differences in contraceptive choices between rural and urban US adults. Rural adults were more likely to choose sterilization, either male or female, as a preferred form of contraception. This finding is somewhat similar to that of an earlier, more limited study that found that rural Illinois women of childbearing years were more likely to choose sterilization for birth control than their urban counterparts4.
Our study found that rural adults were also less likely to use condoms as a form of contraception. This finding was unexpected, not consistent with other studies4,12 and does not seem consistent with limitations in access to health care. However, lack of healthcare access may lead those adults who have completed their planned families to seek out the most permanent form of contraception, namely sterilization, because they would no longer require continued care from healthcare providers, prescriptions or trips to the pharmacy.
Furthermore, in rural communities people are very likely to personally know and possibly be friends of their physicians, pharmacists and other healthcare providers and, as a result, may feel that their privacy is being compromised when having to regularly purchase prescription or OTC products. This factor may lead to more individuals seeking permanent sterilization for contraception. Further study may help determine the reasons behind these choices.
Our results also indicated that even though rural adults were more likely to choose either female or male sterilization, injectable hormones were the next most likely choice of a contraception method. This is a prudent choice for young adults who have not completed their families and who also want to avoid frequent office or pharmacy visits.
Socioeconomic factors, in particular healthcare insurance and income levels, also appeared to influence contraception choices of rural adults. In particular, higher income levels and the presence of health insurance have been associated with greater use of contraception. Interestingly, when compared with their urban counterparts, rural adults making less than $35,000 or without healthcare insurance were more likely to use contraception. Awareness of the costs associated with both pregnancy and raising children may explain why rural adults with limited financial resources seek out reliable means of contraception. Further study may provide insight to explain these differences between rural and similar urban adults.
Limitations
There are several potential limitations to this study. First, the survey is based on telephone-derived data and may be skewed if those who did not participate were less likely to use contraceptives or to use contraception methods in proportionally different ways to those who did respond. For example, persons of lower socioeconomic status are less likely to be included because of poorer phone access. Becuase lower socioeconomic status correlated with different contraception choices, our findings could underestimate the use of birth control reported. However, the fact that the vast majority of the US population live in households with telephones minimizes this bias.
A second limitation is that the survey consists of self-reported answers to close-ended questions. This format is subject to recall bias. A different format to the survey may have yielded different results. Third, the survey was only conducted in either English or Spanish. While English and Spanish are the most commonly spoken languages in the USA, other minority groups who do not use these languages may be under-represented.
Finally, although the survey may be conducted in Spanish, new immigrant Hispanics who might not speak English, or have access to a phone or have health insurance could have inflated the selection bias. Also, a number of newly arrived immigrants may not be willing to participate in a phone survey if they fear their immigration status could be jeopardized.
On the positive side, a strength of this study is the large number of individuals surveyed yielding a nationally representative sample.
Conclusion
The analysis presented here suggested that there were identifiable differences between urban and rural adults in terms of the contraceptive methods they chose. In addition to the influence of primary care provider preferences, other areas for future research include closer examination of socioeconomic factors that are associated with contraceptive choices. These data could assist healthcare providers as well as public health family planning programs when providing counseling to different groups.
Acknowledgement
An earlier draft of this article was presented to the 36th North American Primary Care Research Group (NAPCRG) Annual Meeting at San Juan, Puerto Rico in November 2008.
References
1. Vlassoff C. Fertility intentions and subsequent behavior: a longitudinal study in rural India. Studies in Family Planning 1990; 21: 216-225.
2. Allman J, Nhan VQ, Thang NM, San PB, Man VD. Fertility and family planning in Vietnam. Studies in Family Planning 1991; 22: 308-317.
3. Goodkind D. Abortion in Vietnam: measurements, puzzles, and concerns. Studies in Family Planning 1994; 25: 342-352.
4. Hartlagea SA, Breauxa C, Gehlertb S, Fogg L. Rural and urban Midwestern United States contraception practices. Contraception 2001; 63: 319-323.
5. Mosher WD. Fertility and family planning in the United States: Insights from the National Survey of Family Growth. Family Planning Perspectives 1988; 20: 207-217.
6. Forrest JD, Frost JJ. The family planning attitudes and experiences of low-income women. Family Planning Perspectives 1996; 28: 246-255,277.
7. Dryfoos JG. Contraceptive use, pregnancy intentions and pregnancy outcomes among US women. Family Planning Perspectives 1982; 14: 81-94.
8. Harvey SM, Henderson JT, Branch MR. Protecting against both pregnancy and disease: predictors of dual method use among a sample of women. Women and Health 2004; 39: 25-43.
9. Toulemon L, Leridon H. Contraceptive practices and trends in France. Family Planning Perspectives 1998; 30: 114-120.
10. Yusuf F, Siedlecky S. Patterns of contraceptive use in Australia: analysis of the 2001 National Health Survey. Journal of Biosocial Sciences 2007; 39: 735-744.
11. Skouby SO. Contraceptive use and behavior in the 21st century: a comprehensive study across five European countries. The European Journal of Contraception and Reproductive Health Care 2004; 9: 57-68.
12. Ozumba BC, Obi SN, Ijioma NN. Knowledge, attitude and practice of modern contraception among single women in a rural and urban community in Southeast Nigeria. Journal of Obstetrics and Gynaecology 2005; 25: 292-295.
13. Lindstrom DP, Hernández CH. Internal migration and contraceptive knowledge and use in Guatemala. International Family Planning Perspectives 2006; 32: 146-153.
14. Rosenfeld JA, Kevin Everett K. Teenage women's use of contraceptives in two populations. Journal of the American Board of Family Practice 2001; 14: 1-6.
15. Mokdad AH, Stroup DF, Giles WH. Public Health surveillance for behavioral risk factors in a changing environment: recommendations from the Behavioral Risk Factor Surveillance Team. MMWR 2003; 52(RR09): 1-12.
16. US Centers for Disease Control and Prevention.: Behavioral risk factors: surveillance system users' guide. Atlanta, GA: US Department of Health and Human Services, Centers for Disease Control and Prevention, 1998.
17. DeNavas-Walt C, Proctor BD, Lee CH. Income, Poverty, and Health Insurance Coverage in the United States: 2004. US Census Bureau, Current Population Reports, P60-229. Washington, DC: US Government Printing Office, 2005.
18. Hart LG, Salsberg E, Phillips DM, Lishner D. Rural health care providers in the United States. Journal of Rural Health 2002; 18: 211-232.
19. Casey MM, Klingner J, Moscovice I. Pharmacy services in rural areas: is the problem geographic access or financial access? Journal of Rural Health 2002; 18: 467-477.
Abstract
Introduction: Although sexually active US adults wanting to prevent pregnancy have a wide variety of birth control methods readily available, there is little research that documents the contraceptive choices of rural adults in comparison to urban adults. This study compared the contraceptive choices of rural with urban adults. The comparative analysis joins the recent dialog in population health focused on assessing health related differences to detect if these are indicative of rural health disparities.
Methods: Design: This was a cross-sectional study analyzing 2004 Behavioral Risk Factor Surveillance Survey (BRFSS) data. Place of residence was ascertained by re-coding the state/county FIPS code as either urban or rural, based on 2003 Rural-Urban Continuum Codes from the US Office of Management and Budget (setting: US households; participants: US adults 18-55 years). Main outcome measures: characteristics and contraceptive method choice of rural adults using birth control.
Results: A multivariate regression model performed with 'use of birth control' as the dependent variable yielded that rural in comparison with urban adults 18-55 years were more likely to use female or male sterilization, non-injectable and injectable hormones for birth control. They were less likely to use: condoms, a diaphragm or NuvaRing®, emergency contraception, withdrawal or rhythm methods. Additionally, in comparison with urban adults, rural persons younger than 35 years, those who had children younger than 18 years living with them, those who were partnered, males and those living in households with an income of less than US$35,000 were more likely to report using some form of contraception.
Conclusion: There were differences in the contraception choices of urban and rural adults. How much primary care provider preferences explains the differences is not known and bears further exploration. These results should prove useful to healthcare providers as well as public health family planning programs.
Key words: Behavioral Risk Factor Surveillance System (BRFSS), contraceptive choices, rural US adults, USA.








