Introduction
Rural areas in the USA are facing a myriad of challenges on a variety of levels. Family owned farms are being sold off or foreclosed upon. Small towns are losing their college-educated children to larger cities where there are greater opportunities for employment. Rural schools are being consolidated and closed, and medical care is vanishing from small towns, causing residents to travel further than ever before for their medical needs1-2. In particular, adequate health care continues to be a major concern for rural America. There is a well-documented need for physicians in rural areas3.
Today, as in the past, osteopathic physicians continue to play a major role in meeting the health care needs of America's rural population. While allopathic physicians continue to significantly outnumber osteopathic physicians (in 2004 there were five allopathic students for every one osteopathic student), a high number of osteopathic physicians (approximately 60%) practice primary care as opposed to specialties4. Osteopathic physicians have approximately 1.5 times greater probability of practicing in a rural area compared with other physicians in the USA5-6. Even though many have responded to the needs of rural areas, there remains a serious shortage of physicians, and the future of health care in these areas is in a precarious position2. Fewer medical students entering the field of primary care, increasing levels of student debt, and lower levels of income for primary-care physicians have all contributed to this shortage7-8.
Physician scarcity in rural areas is not a novel topic. There have been many publications focused on the characteristics of physicians who practice rural medicine. Many publications have shown that the influence of a rural background or upbringing has been one of the single strongest predictors of future practice in a rural area9-11. Studies have also examined rural practice retention rates, assessed the role of medical education on practice choice, and looked at demographic factors that influence practice location12-14.
Several of these factors, including age, gender, and ethnicity, have been evaluated with somewhat mixed findings. For example, studies by Rabinowitz, Diamone, Hojat and Hazelwood, as well as Horner, Samsa, and Rickets found no statistically significant impact for these characteristics12-13. However, a study by Fryer, Stine, Vojir, and Miller found that being a male and of older age has a positive influence on rural practice14. Similarly, a study of 1987 to 2000 graduates demonstrated that graduates over the age of 29 years have over 30% greater rural location rates after using the appropriate controls for origins, training type, and career choice. The study uses complete populations of US physicians and may be more reliable than most regarding the age factor6.
Residency and medical school curricula are additional factors that have been shown to positively influence physicians and medical students to practice medicine in a rural area, although the majority of these studies have been performed in allopathic settings15-16. Once again, studies of complete populations using secondary data indicate the important contribution of training type. Both allopathic public and osteopathic training is associated with a 30 to 50% greater production of rural workforce6. All of these findings deserve attention, especially by medical schools and residency programs interested in producing physicians who will practice in rural areas.
Although numerous studies have been published regarding the aforementioned factors, very few direct studies have focused on osteopathic physicians or students on this important issue. In fact it appears that no studies have directly compared osteopathic students with residents according to their intention to practice in a rural area, a shortcoming the present study aims to address.
This study is ultimately concerned with exploring the issue of rural health disparities. Namely, determining what factors play a role in the location decision as the careers of osteopathic medical students and physicians-in-training progress. It is important for organizations such as the American Osteopathic Association (AOA), American Association of Colleges of Osteopathic Medicine (AACOM), hospitals, and government agencies to understand the current level of interest in rural medicine in order to project the future of the osteopathic profession in rural health care. To effectively recruit future generations of physicians interested in working in rural areas, it is crucial to document historical relationships between a physician's demographic characteristics and background (age, gender, race, and the type of community in which they have spent most of their life) and their willingness to practice in a rural area. An understanding of these issues is integral to being able to appeal to this demographic and positively influence their choice of a life in rural medicine.
Methods
Data
An electronic, web-based survey was developed and implemented by the Office of Educational Development at the Oklahoma State University Center for Health Sciences. The survey web page was active from June to July 2007. The survey and paperwork were forwarded to appropriate personnel at AACOM who then sent a survey web-link to their respective residents and fellows. Thus, all participants were either osteopathic medical students or osteopathic physicians currently in training (ie residents). Completion of the survey was voluntary, and no incentives were used to increase response rates.
Two distinct forms of the survey were used to collect data, one for the osteopathic medical students and one for osteopathic physicians-in-training. The survey was designed in such a way to be easily completed within 10 min. No personal identifiers were present in the surveys in an effort to maintain confidentiality. Data captured from the survey included: year in school/residency; age; gender; race; population of the community in which the participant had spent more than half his or her life; population of the community in which the participant intended to practice; and a host of questions regarding attitudes about practicing medicine in a rural area. 'Rural' was defined as a community of less than 50 000 people, which is common in the health literature17.
Statistical methods
Characteristics were summarized for both numbers and percentages of students and residents. Differences between the two groups were calculated by comparing means and using appropriate t-tests. Logistic regression was then used to determine factors associated with a positive response to the question regarding intent to practice in a rural area. Analyses were performed using both SPSS (SPSS Inc, Chicago, IL, USA) and Stata (StataCorp; College Station, TX, USA) statistical software packages, using varying levels of statistical significance (p = 0.10, 0.05, and 0.01).
Results
A total of 161 students from two osteopathic colleges which had a combined enrollment of 1386 students completed and submitted the survey, as well as 51 residents/fellows from a variety of training programs. Although the student response rate of approximately 12% is relatively low, some research suggests this is a fairly standard rate for web-based surveys where the distributor has no personal contact with the survey-takers18. The demographic characteristics and opinions regarding practicing in a rural location are divided into student and resident groups, including statistics only for those who plan on practicing in a rural area (Tables 1 and 2, respectively). These tables also include t-tests for significant differences between students' and residents' responses. Results of the logistic regression are also reported (Table 3), with reported coefficients designating the odds ratios associated with a respondents' intent to practice in a rural location.
Table 1: Descriptive statistics of survey respondents: osteopathic students and residents (values are frequencies of different categories)
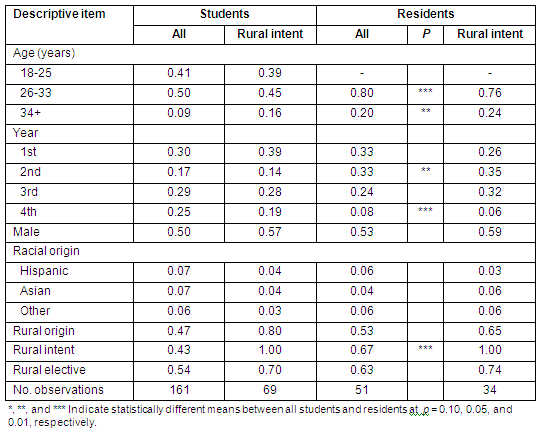
Table 2: Opinions regarding rural practice by osteopathic students and residents (values are frequencies of different categories)
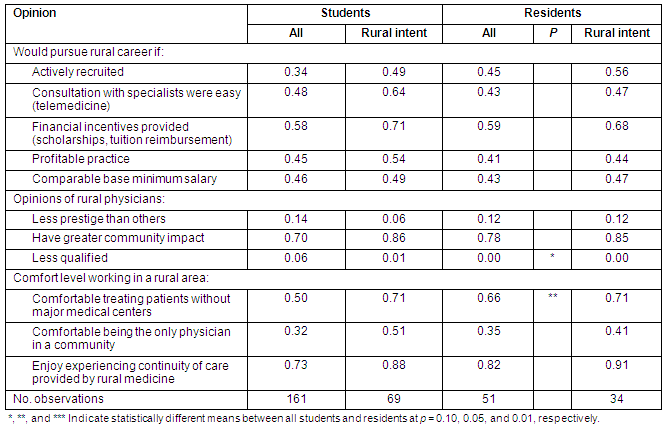
Table 3: Logistic regression results for factors associated with interest in practicing in a rural area (values correspond to β)
Student survey
Approximately 41% of the respondents were between the ages of 18 and 25 years, 40% were aged 26-33 years, and 9% were 34 years and older. The distribution between 1st, 2nd, 3rd, and 4th year students was relatively even. As expected, these characteristics varied significantly from resident's responses, with students more likely to be younger, less likely to be in their 2nd year of study, but more likely to be in the 4th year at their respective institutions. Approximately 43% of students expressed the intention to practice rural medicine, which was significantly lower than the percentage of the residents (53%). Approximately 47% of students were raised in a rural area. Approximately 54% took a rural elective or planned to take a rural elective during their osteopathic education. Of those seeking rural practice, over 80% were raised in a rural area, and 70% took or planned to take a rural elective course.
In terms of opinions on rural practice (Table 2), more students indicated that receiving financial incentives was more important in their decision to pursue a rural career than other motivations. While being generally positive about rural physicians, it is worth noting that 6% felt that rural physicians were less qualified than their urban counterparts - which was statistically significantly higher than the opinions of residents (of whom none felt that way). This occurs despite the relatively similar percentage of student /residents with rural origin (Table 1, 47% and 53%, respectively; not statistically different in these samples). The only other significant difference between the 2 groups came in their comfort level in treating patients without a major medical center. Fewer students (50%) were (understandably) comfortable working in such conditions than residents (66%). This may be simply due to the additional time practicing medicine of the residents.
Our logistic regression uses intent of practicing in a rural area as the dependent variable. The overall fit of the model for students is quite good, with a pseudo R2 of 0.38 and almost 80% correctly predicted for those with both rural and urban intent. As expected, having a rural upbringing has a positive and significant impact. Strikingly, however, as time in school increases, the likelihood of maintaining an intention of rural practice appears to decline. This negative relationship is significant for year 2 at p = 0.05, and in years 3 and 4 at p = 0.01. Additional findings include the positive influence of being relatively older (≥34 years) and taking a rural elective. Gender and race did not play a role in students' decision to pursue rural medicine.
Resident and fellow survey
The majority of the respondents to the resident survey were aged between 26 and 33 years, with only 20% over the age of 33. Only 8% of the responding residents were in their 4th year of postgraduate work, with approximately two-thirds of the sample in either their 1st or 2nd year. It was found that 67% of all respondents expected to practice rural medicine (which, as previously noted, is statistically significantly higher than the rate for students), 53% were raised in a rural area, and 63% took a rural elective as part of their undergraduate education. Of those seeking a rural practice, only 65% were raised in a rural area (compared with 80% of students).
The opinions on rural practice of residents are similar to those of students. As might be expected, the residents' influences were more likely to involve financial incentives for rural practice location. Approximately 78% of residents felt that rural physicians have a greater community impact than their urban counterparts, and no residents felt that rural physicians are less qualified than those in urban areas. However, 12% did feel that rural physicians had lower prestige. It was found that 66% of respondents were comfortable treating patients away from major medical centers, and 82% indicated that they enjoyed providing the continuity of care required by rural medicine.
Resident responses were similar to students regarding the positive impact of rural upbringing and taking a rural elective as an undergraduate (p = 0.10 and p = 0.05, respectively). However, unlike the student survey, residents were actually more likely to be interested in rural medicine during their 2nd and 3rd post-graduation years. The default age category was over 34 years (because there were no observations from residents between 18 and 25 years), and Hispanic, Asian, and other race are grouped together due to a smaller number of observations. However, none of these variables is significant. Again, the model provides a relatively good fit because the percentage correctly predicted is quite high for both categories and is much more accurate than a naive model that simply predicts the alternative with the highest frequency.
Discussion
Student survey
The overall response given to the survey was fairly well balanced across all years of undergraduate medical training. High levels of third- and fourth-year student participation were unexpected, due to their diverse and time-consuming schedules. The relatively high levels of students expressing interest in practicing in an area with less than 50 000 population (43%) could potentially introduce some self-selectivity bias, because a national-level survey indicated that only approximately 20% of graduating osteopathic students answered this question affirmatively in 200419. The potential for bias indicates that the parameter estimates associated with the regression results should be treated with caution.
The opinions of the students indicate that financial incentives are the best way to attract students to rural areas. Approximately 58% of students said they would pursue a rural career if these incentives were made available, compared with only 45% who would pursue a rural career if they were guaranteed a profitable practice, or 34% who would pursue a rural career if actively recruited. Interestingly, while 70% felt that rural physicians had greater community impact than urban physicians, 6% still felt that rural physicians were less qualified. This was one of the few areas where statistically significant differences in opinion occurred between students and residents. The other area of difference was in the comfort level in treating patients away from a major medical center, where only 50% of students expressed comfort. This may be due to their training at that point in time (because approximately 50% of the respondents were in their first 2 years of medical school).
One of the most studied factors influencing medical students to practice medicine in a rural location is a rural upbringing9-11. This study also found rural upbringing to be a positive factor, with strong levels of statistical significance for students (p = 0.01). This illustrates the high importance of 'rural upbringing' in recruitment by schools wanting to produce practitioners interested in rural practice. However, the recruitment of such students may be difficult, given the small number of students who are interested in health careers, gain access to higher education and perform well enough to obtain admission into medical school.
Students taking or planning to take a rural elective did have greater interest in a practice location with less than 50 000 people (p = 0.01). Notably, while many osteopathic schools require some rural rotations, this study found that impact on rural practice was strictly from elective rotations. Institutional dedication to rural medicine has been shown to serve as one predictor of rural physician recruitment20-22. Rural rotations can be important indicators.
In the present study, gender and race did not play a role in students' decisions to pursue rural medicine, and this is consistent with most other studies12-14. However, an interesting finding of this study is that as time in school increases, the likelihood of choosing rural practice declines. Several explanations include decreasing idealism, rising student debt, and perhaps even a potential lack of rural physician role models as students move through their training. The rapid decline in rural practice interest parallels the decline in interest in family medicine in osteopathic medical students in the last 20 years, with more rapid declines in the past decade. When students do not choose family medicine, the probability of rural practice declines greatly. Further, students not choosing family medicine realize that their practice locations are limited to larger locations. Several studies show an overall decrease idealism has been shown to occur throughout medical school and even into internship23-26. Rising student debt has also played a role in students' decisions to avoid primary-care medicine, especially in rural areas27-28. This high level of debt can be dealt with by physician 'loan forgiveness' programs offered to those interested in primary-care medicine.
As the number of rural practitioners declines, there is a corresponding loss of physician role models. Role models are an important component of a medical students' education and future practice intentions29-31. These results suggest a need to continually reinforce the benefits of practicing in a rural area throughout a student's career, perhaps with site visits to well-regarded rural practicing physicians or discussions about loan forgiveness programs.
Resident and fellow survey
There have been numerous programs designed to recruit physicians, including government sponsored initiatives and rural hospital physician recruitment32-33. The popular strategy to locate residency programs in rural areas has decreased in number over the past several years34-35. This study shows that resident exposure to rural medicine as a medical student (ie has taken a rural elective) is a positive influence on interest in setting up practice in a rural area (p = 0.05), along with the continuing positive influence of rural upbringing (p = 0.10).
A primary difference between osteopathic medical students and resident physicians is that medical students appear to have an interest in practicing in a rural area in the early years of medical school, whereas residents appear to have increased interest in rural health later in residency, during the 2nd and 3rd years. It is interesting to note that residents have a generally higher opinion of rural physicians than do students, although only one opinion (that rural physicians are less qualified) is statistically significant.
Limitations
The study has several limitations. As with all regression analysis, establishing causality is difficult, and suggested policy prescriptions are tempered by proposing that they may be effective only if the causality runs from the independent to dependent variables. In particular, there may be some concerns about the direction of causality for the rural elective variable, because those more interested in rural medicine may be more likely to select these electives (as opposed to seeing participation in the elective drive an interest in rural medicine). The response rate to the web-based survey was relatively low and, as previously noted, the potential for bias exists because individuals with an interest in rural medicine may have been more likely to complete the survey. Finally, the use of a population base of 50 000 as the definition of rural has been consistently applied in this analysis and may be a limitation. Other studies may use lower numbers or different designations, such as Rural-Urban Commuting Area (RUCA) codes, which could impact the results.
Conclusion and recommendations
Osteopathic medicine will remain an important contributor to the rural workforce, but this will be a function of admission of the medical students most likely to choose rural practice, osteopathic emphasis on rural practice during training, and graduation rates of the family physicians most likely to choose rural practice. United States health policy also limits rural workforce contributions as policy fails to support primary care and fails to assist rural patients to overcome financial access barriers. The goal of this study was to assist osteopathic programs in their successful recruitment and placement of physicians into underserved rural areas. The results found that positive factors impacting on rural interest include: having a rural background, being an older student, and participating in rural clinical elective experience for both medical students and residents. This suggests that osteopathic schools can improve their placement of rural physicians by targeting recruitment programs on candidates who fit these descriptions, and by offering incentives for participation in rural electives.
An additional goal of this study was to evaluate the similarities and differences of osteopathic medical students and physicians undergoing postgraduate training. One striking similarity was that both students and residents ranked financial incentives as the most influential motivator for pursuing rural practice. No significant differences were found for various types of incentives, indicating that separate methods of promoting rural careers among students and residents are not necessary. In particular, expanding loan forgiveness programs or scholarships for students to decrease student debt may be effective in encouraging both students and residents to pursue rural careers.
The results also indicated that residents have higher opinions of the qualifications of rural physicians, and that they feel more comfortable treating patients in rural areas. While this discrepancy is partly explainable by residents' increased experience, implementing programs that focus on rural physician 'success stories' (such as interviews with well-known rural physicians) or encouraging solo practice of procedures typically found in rural areas may provide additional benefit. Schools seeking to promote rural physicians should emphasize education about rural practice prior to the point at which a student can select family medicine (which is generally a permanent choice).
Acknowledgements
The authors thank Chaunda Capers for critically evaluating the survey. They also thank Tom Levitan and Machelle Davison EdD for their help in disseminating the survey. The manuscript has been greatly improved thanks to the helpful comments of three anonymous referees.
References
1. Mills B, Hazarika G. The migration of young adults from non-metropolitan counties. American Journal of Agricultural Economics 2001; 83: 329-340.
2. Agency for Healthcare Research and Quality. 2004 National Healthcare Disparities Report. (Online) 2004. Available: http://www.ahrq.gov/research/ruraldisp/ruraldispar.pdf (Accessed 18 February 2008).
3. Gazewood J, Rollins L, Galaska S. Beyond the horizon: The role of academic health centers in improving the health of rural communities. Academic Medicine 2006; 81: 793-797.
4. Miller T, Hooker RS, Mains DA. Characteristics of osteopathic physicians choosing to practice rural primary care. Journal of the American Osteopathic Association 2006; 106(5): 274-279.
5. American Osteopathic Association. Fact sheet 2006. (Online) 2006. Available: www.osteopathic.org/pdf/ost_factsheet.pdf (Accessed 2 July 2009).
6. Bowman RC. They really do go. Rural and Remote Health 8: 1035. (Online) 2008. Available: http://www.rrh.org.au (Accessed 25 June 2009).
7. Whitcomb M. The challenge of providing doctors for rural America. Academic Medicine 2005; 80: 715-716.
8. Association of American Medical Colleges. Association of American Medical Colleges Matriculation Questionnaire 2008: All Schools. (Online) 2008. Available: http://www.aamc.org/data/msq/msq2008.pdf (Accessed 1 September 2009).
9. Laven G, Wilkinson D. Rural doctors and backgrounds: how strong is the evidence? A systematic review. Australian Journal of Rural Health 2003; 11: 277-284.
10. Azer SA, Simmons D, Elliott SL. Rural training and the state of rural health services: effect of rural background on the perception and attitude of the first-year medical students at the University of Melbourne. Australian Journal of Rural Health 2001; 9: 178-185.
11. Australian Medical Workforce Advisory Committee (AMWAC). Doctors in vocational training: rural background and rural practice intentions. Australian Journal of Rural Health 2005; 13: 14-20.
12. Rabinowitz HK, Diamond IJ, Hojat M, Hazelwood CE. Demographic, educational and economic factors related to recruitment and retention of physicians in rural Pennsylvania. Journal of Rural Health 1999; 15: 212-218.
13. Horner RD, Samsa GP, Ricketts TC. Preliminary evidence on retention rates of primary care physicians in rural and urban areas. Medical Care 1993; 31: 640-648.
14. Fryer GE, Stine C, Vojir C, Miller M. Predictors and profiles of rural versus urban family practice. Family Medicine1997; 29: 115-118.
15. Chan B, Degani N, Crichton T, Pong R, Rourke J, Goertzen J et al. Factors influencing family physicians to enter rural practice. Does rural or urban background make a difference? Canadian Family Physician 2005; 51(9): 1247.
16. Rosenthal T, McGuigan M, Anderson G. Rural residency tracks in family practice: graduate outcomes. Family Medicine 2000; 32(3): 174-177.
17. Ricketts T, Taylor P, Johnson-Webb K. Definitions of rural: a handbook for health policy makers and researchers. Federal Office of Rural Health Policy Health Resources and Services Administration, United States Department of Health and Human Services, 1998. Available: http://www.shepscenter.unc.edu/research_programs/rural_programs/pub_reports.html (Accessed 10 March 2009).
18. Marcussen CH. Response rates in internet surveys. In: Proceedings, Innovations in Online Market Research Conference. 11-12 September 2001; Amsterdam, 2001.
19. Teitelbaum HS. Osteopathic medical education in the United States: improving the future of medicine. Washington, DC: American Association of Colleges of Osteopathic Medicine-American Osteopathic Association, 2005.
20. Potter JM. Characteristics of Alaskan family physicians as determinants of practice location. Alaska Medicine 1995; 37(2): 49-52,79.
21. Rabinowitz HK, Diamond JJ, Markham FW, Hazelwood CE. A program to increase the number of family physicians in rural and underserved areas: impact after 22 years. Journal of the American Medical Association 1999; 281(3): 255-260.
22. Wheat JR, Higginbotham JC, Yu J, Leeper JD. Physicians for rural America: the role of institutional commitment within academic medical centers. Journal of Rural Health 2005; 21(3): 221-227.
23. Crandall SJ, Volk RJ, Loemker V. Medical students' attitudes toward providing care for the underserved: are we training socially responsible physicians? Journal of the American Medical Association 1993; 269: 2519-2523.
24. Griffith CH, Wilson JF. The loss of student idealism in the 3rd year clinical clerkships. Evaluation and the Health Professions 2001; 24: 61-71.
25. Griffith CH, Wilson JF. The loss of idealism throughout internship. Evaluation and the Health Professions 2003; 26: 415-426.
26. Woloschuk W, Harasym PH, Temple W. Attitude change during medical school: a cohort study. Medical Education 2004; 38: 522-534.
27. Xu G, Veloski JJ. Debt and primary care physicians' career satisfaction. Academic Medicine1998; 73: 11.
28. Hadley J, Cantor JC, Willke RJ, Feder J, Cohen AB. Young physicians most and least likely to have second thoughts about a career in medicine. Academic Medicine 1992; 67: 180-190.
29. Cutchin MP. Community and self: concepts for rural physician integration and retention. Social Science and Medicine 1997; 44(11): 1661-1674.
30. Brooks RG, Walsh M, Mardon RE, Lewis M, Clawson A. The roles of nature and nurture in the recruitment and retention of primary care physicians in rural areas: a review of the literature. Academic Medicine2002; 77(8): 790-798.
31. Senf JH, Campos-Outcalt D, Kutob R. Factors related to choice of family medicine: a reassessment and literature review. Journal of the American Board of Family Practice 2002; 16(6): 502-512.
32. Fleetwood J. Improving physician recruitment for rural hospitals. The Quality Letter for Healthcare Leaders 1999; 11(11): 8-9.
33. Gorsche R, Hnatuik J. Additional skills training for rural physicians. Canadian Family Physician 2006; 52(5): 601-604.
34. Rosenthal TC, McGuigan MH, Anderson G. Rural residency tracks in family practice: graduate outcomes. Family Medicine 2000; 32(3): 174-177.
35. Longenecker R, Rosenthal T, Stearns J, Woods M. Graduate medical education for rural practice. Joint statement. Washington, DC: National Rural Health Association and the American Academy of Family Physicians, 2008.

