Introduction
Planning is defined as a formal process of choosing an organisation's vision, mission and overall goals; devising operational goals and choosing strategies and tactics to achieve these; and allocating resources to achieve the goals1. For the public sector, planning is considered a reasoning process about how an organisation will get where it wants to go2. This position maintains that planning shapes the whole field of public administration, determining the limits of government responsibility, the allocation of resources, distribution of costs, division of labour and the extent of public controls. Additionally, for public healthcare a hierarchical framework as proposed by Green3, outlines broad-based objectives for the future of a health organization. This framework incorporates the values the contextual government holds for the health of the population and the goals of the health sector, and encompasses available resources for health delivery and specific techniques for putting the plans into practice. These long-term objectives are then translated into operational plans with detailed activities, responsibilities, budgets and timetables.
A clear distinction is made between the roles played by planning participants2. Top management, with input from managers at other levels, make broad directional plans, middle management formulate tactical plans and middle and lower management formulate operational plans4. However, this top-down process has been disputed, with the suggestion that plans can emerge from any part of an organisation5. Nonetheless, operational plans function within a specific framework depending on the context, in this case oral health services.
Although such hierarchical planning at strategic, tactical and operational levels is very important for effective healthcare planning, it is often not the practice. Indeed the World Health Organisation, asserted that the adoption of modern methodology for management planning, as utilised in the private sector, was not widely practised in the health sector until the 1990s6. In Lesotho a hierarchical framework is often only used centrally.
About Lesotho
Lesotho is a landlocked, independent, mountainous country completely surrounded by South Africa; more than 80% of the country is 1800 m above sea level and it is located at lat 29°30' S, long 28°30' E. In 2003 the population was 1 802 000 (5% of which was over 65 years and 40% under 15 years) and the population of the national capital Maseru was 373 000. Other large towns include Leribe, Berea and Mafeteng.
Lesotho was the British Basutoland Protectorate until independence in 1966. It currently has multiple developmental challenges including the need to reduce poverty, improve social services, fight HIV/AIDS, accelerate economic growth and consolidate democratic gains made at both central and local level. The Government of Lesotho is committed to decentralisation as a way to address these challenges. The 1994 established Ministry of Local Government and Chieftainship has been instrumental in advancing decentralization, and this has influenced reforms in all sectors, including health care.
Oral health planning in Lesotho
Lesotho health sector administration was a central hierarchical structure until recently; however, the current key institutions for of healthcare services delivery are Health Service Areas (HSA), each based in a government or mission hospital. Each HSA central hospital covers a number of village health centers with resident nurses or nurse practitioners, as well as clinics that are visited regularly by doctors and nurses. The hospital also trains community health workers from individual villages, thus extending health care throughout the whole HSA.
The recent decentralisation dispensation meant that the Lesotho Oral Health Unit is managed within the clinical services department of the Lesotho Ministry of Health and Social Welfare. It comprises a dental clinic with a dentist and at least one dental assistant in each of Lesotho's 10 districts. Each district dentist reports to the district medical officer in the district hospitals, but also to the acting head of the oral health unit monthly. The acting head of the oral health unit coordinates oral health planning at the national level and reports to the director general of the Health Ministry through the head of clinical services. Only the dental clinic in Maseru has additional 'filter clinics' (outreach clinics designed to relieve pressure on the outpatient department of the national referral center, Queen Elizabeth II Hospital [QEII]), with approximately 7 dentists rotating through these and the main QEII dental clinic.
The average district dental clinic provides dental services for one semi-urban and from 20 to 40 rural and remote communities, while the main dental clinic in QEII and its filter clinics provide dental services for Maseru and its contiguous towns. This arrangement provides both opportunities and challenges in planning oral health services. However, as is common in African countries, there is a paucity of published studies on oral health services planning in Lesotho. This study focused on the planning of Lesotho oral health services, using the experiences of dentists in the public sector as the unit of analysis. Such context-specific data may provide the type of information required to address issues in the management function of planning for oral-health service delivery in Lesotho. This prompted the researchers to undertake this study.
Objectives
The objectives of the study were to:
- Describe the experiences of dentists regarding the management function of planning in the rendering of oral health services in Lesotho.
- Make recommendations that will address the emergent research findings.
Methods
Design
The study was carried out using a qualitative research design implementing an exploratory, descriptive and contextual approach, with public sector dentists in Lesotho as the research population.
Sample
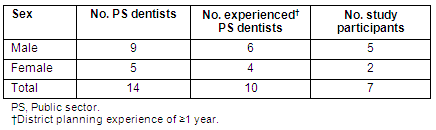
The purposive sample for this study consisted of the 14 public sector dentists in Lesotho at the time of the study. Ten dentists met the criteria for participation (≥1 year of district oral health planning experience and a willingness to share their experiences); however, three of these were inaccessible at the time that time of the study (Table 1).
Table 1: Sample frame and sample according to sex
This approach was used to ensure methodological congruence between the research problem and objectives, and the techniques of data gathering and analysis7,8. Trustworthiness was assured using Guba's Model of Trustworthiness, namely, truth-value, applicability, consistency and neutrality. Data were collected through in-depth, one-on-one interviews with 6 participants, and textual data (a written description detailing the participant's experience) was collected from the seventh. All participants were asked: 'Tell me your experiences in planning services for your dental clinic?'
The six interviews were audiotaped and transcribed verbatim within 24 hours of each interview session. The interview transcripts were complemented with field notes. The collected data were organised and analysed using the Tesch method9, where the researcher obtains a sense of the whole by selecting one document at a time to make meaning of its contents, and then making short notes. Thereafter, topics were listed, clustered according to similarity and abbreviated as codes. The most descriptive wording was then found for the topics and categories formed. A clean set of transcripts and a guideline for coding was presented to an independent coder for analysis and agreement was reached between the researchers and the independent coder on the emergent themes.
Ethics approval
Ethical measures included the voluntary participation and informed consent of participants, privacy of the participants and confidentiality and cross-checking of collected and reported data with the participants individually, through one-on-one briefing or by email. In addition, authorisations were obtained from the Research and Ethics Committee of the Ministry of Health and Social Welfare, Planning and Development Unit in Lesotho, as well as the Technology and Innovation Committee of the Nelson Mandela Metropolitan University, Port Elizabeth, South Africa.
Results
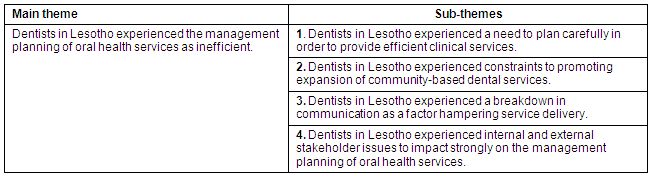
After analysis of the collected data, one major theme and 4 sub-themes emerged (Table 2).
Table 2: Themes and sub-themes regarding the experiences of dentists in the management planning of oral health services in Lesotho
Discussion
The planning of oral health services is inefficient
The main theme, that Lesotho dentists found the management planning of oral health services inefficient, summarizes the issues in the sub-themes. Some specific participant experiences characterized the inefficiency, such as careful planning being hampered by a limitation to information required for decision-making:
...it is good when you are planning... I won't start thinking about a maxillo-facial surgeon, No! it is true that is important, as well as we need more dental assistants, more oral hygienist, more therapists; but all those things will be revealed when we have more information.
Decision-making is a critical managerial activity in the process of planning; no real plan exists until a decision is made to commit resources10. Decision-making theories include sequential and non-sequential models11. The critical aspect of the non-sequential model revolves around the evaluation-choice routine, where alternatives to achieving specific goals are generated and a choice is made using rational analysis of available information. Regarding oral health, such decisions include determination of the needs of the community and the type of oral health services to be provided. Resources may be limited. In oral health care, the required technology may be expensive and is often manufactured outside developing rural and remote communities. Thus healthcare managers' and providers' decisions must mean that the right resources are allocated for the right purpose (allocative efficiency), and also that the resources allocated to specific services will produce the greatest benefit at minimal cost (technical efficiency). For this reason, health authorities such as the Lesotho Government have adopted the primary healthcare strategy12. Oral health-care, one of the basic primary healthcare packages of services offered by the Government of Lesotho, cannot be achieved without baseline-information sufficient for an evaluation-choice routine.
Sub-themes
Need for carefully planning in clinical services: Participants indicated that due to limited basic data (eg the dental caries incidence of the local population), they prioritised basic procedures (eg dental extractions, tooth filling, prophylactic tooth cleaning, treatment of maxillo-facial trauma and acute infections of the head and neck) according to their perceptions of the needs of service users. Thus, curative services were prioritised at the expense of preventive and rehabilitative services:
We all know that most of the treatment we do is extraction...you would at least increase a certain percentage of patients...that really need [dental] filling should be filled rather than have an extraction.
Without adequate information/data, planning and prioritization is impossible. Required baseline data such as population dental caries experience13 and the prevalence of severe oral problems such as noma (gangrenous tissue destruction of the face, especially the mouth and cheek), oral cancer and the oral consequences of HIV/AIDS infection13, is necessary for the efficient commitment of resources.
A health unit is considered efficient when it provides improved health benefits from the use of a given set of resources15,16. Due to the importance of the prioritization process for health planning, the World Bank and the World Health Organisation introduced burden-of-disease criterion for priority-setting, among other such systems proposed14,17,18. When such criteria are used properly in the context of oral health, goals can be reached without neglecting the delivery of preventive and rehabilitative services or referral planning.
Referrals from Lesotho districts often involve patients travelling from rural and remote mountainous communities for uncertain outcomes:
Most of the time we refer them to Maseru, perhaps there are times when they will... they do fabricate dentures at times, ...you refer them, if they are lucky then they may get the service.
Improper planning of referrals may result in the denial of quality specialised care. Patients can be disadvantaged due to such access issues, for there are very limited alternatives outside the public sector in Lesotho.
Constraints to promoting the expansion of community-based services: Participants identified an unmet need to expand community-based dental services within the primary health context, and this had implications for rural and remote patients. While staff shortages and insufficient facilities were identified, transport facilities were important impediments (as was also identified in a South African study19):
Although a lot of the time I had to leave the actual activity in the hands of the public health nurses and health inspectors because often there was the problem of transportation.
It is well and good to sit down and plan in here by yourself as oral health department, but if you need to go somewhere you need to make a good plan with the transport officer, if you need money you need the financial people.
Lesotho is a mountainous country and many rural communities are not easily accessible without effective transport. This constraint to the expansion of community oral health services affects a core primary healthcare strategy: access to care.
Breakdown in communication hampers service delivery: Participants described the breakdown of communication between Lesotho dentists involved in service planning and authorities at district and national levels. This specifically affected human resources procurement and budgeting:
There is a lack of human resources everywhere, the establishment list of the ministry is very old...so it no longer caters for the needs that we have.
Official data corroborate this, indicating a very limited supply of dental personnel in Lesotho (0.07 per 1000 people and 0.4% of all health sector staff)20. Human resources often constitute a significant part of health budgeting in most countries requiring careful planning.
Additionally, participants found the maintenance and procurement of equipment to be inconsistent, a situation reflected in a South African study21. Participants also indicated they were rarely involved fully in budgetary processes that impacted on their services, with a lack of consistent clear, feedback on actual departmental allocations.
Of the 6 major managerial competencies, communication is perhaps the most fundamental because managers cannot accomplish tasks effectively if they cannot manage the vast network of relationships that link them to other people1.
Internal and external stakeholder issues: Participants experienced limitations to their ability to have their views represented at health ministry level. They felt this was due to the organisational structure of the dental department of the Ministry of Health and Social Welfare that lacked a substantive head, and the many unfilled personnel departmental positions. They believed this also limited the development and implementation of national oral health plans.
However, participants identified beneficial, proactive relationships with external stakeholders (staff outside the dental unit, other related ministries, clients, community leaders, for profit and non-profit organisations), and such stakeholders form an important component of healthcare planning22,23.
Limitations
There were several limitations to the study. In terms of subjectivity, the researcher who was an 'insider' was mindful of the need for neutrality, which is difficult to achieve in shared experience. There were appointment scheduling issues with participants, a pitfall of qualitative data collection where direct participants contact is required. Finally, due to the uniqueness of the context, generalisation may be limited, although the detailed description of the context may increase transferability.
Recommendations
The study findings are reinforced by the recommendations of the WHO Africa regional office which encourages developing states to act by strengthening the role of policy and planning in oral health service delivery through research24.
Specific recommendations are made to develop a process for strategic planning to guide dental planning in Lesotho, and to advocate for policies that will make such planning effective. One suggested framework to guide hierarchical planning is to combine a modified Michael, Hitt, Ireland and Hoskisson model25 with the logical framework model to guide the operational phase.
Also recommended is that procurement, transport and human resources management issues are addressed in relation to oral health services, as well as communication gaps between dental unit managers and their authorities locally and centrally and as it relates to the budgeting process.
Important to the sustainability of public oral health services in Lesotho is the need to address fundamental public health requirements for oral health education and oral health promotion in line with WHO and International Dental Federation guidelines14, and the incorporation of this into the public school curriculum, as suggested by participants in the first Lesotho Oral health Conference26.
Conclusion
This study sought to understand the experiences of dentists with regard to the management planning for oral health services in Lesotho. It emerged from the study that the participant dentists experienced the management planning of oral health services as inefficient. This inefficiency, as described by the participants, arose from factors that impair careful planning; constrained the expansion of community based oral health services; caused a breakdown in communication between dentists and their authorities leading to poor services delivery; and was impacted strongly by internal and external stakeholder issues.
The study suggests that dental planning in Lesotho (and other health-care contexts) should take into account priority-setting, procurement management, transport and human resources management as well as stakeholder analysis when embarking on the planning process.
Acknowledgements
In March 2008, just before the study was concluded through the Nelson Mandela Metropolitan University, South Africa, the Lesotho Ministry of Health and Social Welfare appointed a substantive Director of Oral health services and sponsored a management workshop for all unit managers in the dental department. Also the Ministry, in collaboration with the World Health Organisation country office in Lesotho, initiated the process of developing a substantive oral health policy for the country. These activities addresses some of the findings of this study
References
1. Hellriegel D, Jackson SE, Slocum J, Staude G, Amos T, Klopper HB et al. Management. Cape Town: Oxford University Press, 2004.
2. Starling G. Managing the public sector, 7th edn. Belmont, CA: Thomson Higher Education, 2005; 219.
3. Green A. An introduction to health planning for developing health systems, 3rd edn. New York: Oxford University Press, 2007.
4. Smit PJ, Cronje GJ, Brevis T, Vrba MJ. Management principles: a contemporary edition for Africa, 4Th edn. Cape Town: Juta, 2007.
5. Williamson D, Cooke P, Jenkins W, Moreton KM. Strategic management and business analysis. Oxford: Elsevier/Butterworth-Heinemann, 2004.
6. Sapirie SA. WHO and health planning- the past, the present and the future. World Health Forum 1998; 19(4): 382-387.
7. Morse J, Barrett M, Mayan M, Olson K, Spiers J. Verification strategies for establishing reliability and validity in qualitative research. International Journal of Qualitative Methods. (Online) 2002. Available: www.lindafinlay.co.uk (Accessed 24 June 2007).
9. Creswell JW. Research design: qualitative, quantitative and mixed methods approaches, 2nd edn. Thousand Oaks, CA: Sage, 2003.
10. Olum Y. Modern management theories and practices. (Online) 2004. Available: http://unpan1.un.org/intradoc/groups/public/documents/AAPAM/UNPAN025765.pdf (Accessed 12 December 2007).
11. Hansson SO. Decision theory: a brief introduction. Stockholm: Royal Institute of technology (KTH), 2005.
12. Musgrove P, Creese A, Preker A, Baeza C, Anell A, Prentice T (Eds). Health systems: improving performance. The World Health Report. Geneva: WHO, 2000.
13. WHO. The world oral health report 2003. WHO/NMH/NPH/ORH/03.2. Geneva: WHO, 2003.
14. World Dental Federation & World Health Organisation. Nairobi Planning conference for oral health in the African region: conference report. (Online) 2004. Available: http://www.fdiworldental.org/public_health/assets/Activities/Nairobi/Nairobi_Report_en.pdf (Accessed 16 October 2009).
15. Murray JLC, Frenk J. A framework for assessing the performance of health systems. Bulletin of the World Health Organisation, The International Journal of Public Health 2000; 78(6): 717-731
16. Siadat B, Stolpe M. Reforming health care finance: what can Germany learn from other countries. Policy reports, Kiel economic policy papers. Kiel: Kiel Institute for World Economics, 2005. Available: http://www.ifw-kiel.de/pub/kepp/2005/kepp05.pdf (Accessed 21 October 2009).
17. Mooney G and Newberry G. Priority setting in dentistry: putting teeth into the process. NSW Public Health Bulletin 1999; 10(5): 42-43. Available: http://www.publish.csiro.au/?act=view_file&file_id=NB99019.pdf (Accessed 20 October 2009).
18. Gibson JL, Martin DK and Singer PA. Setting priorities in health care organizations: criteria, processes, and parameters of success. BMC Health Services Research. 2004; 4: 25. Available: http://www.pubmedcentral.nih.gov/articlerender.fcgi?artid=518972 (Accessed 22 November 2007).
19. Hall W, du Plessis D, McCoy D. Transport for health care delivery. Durban, South Africa: Health Systems Trust, 2002.
20. Schwabe C, Lerotholi K, McGrath E. Lesotho health sector human resources development & strategic plan 2005-2025. Maseru: Government of Lesotho, 2004.
21. Kachienga M. Assessment of technological investment in the public health sector in South Africa. International Society of Technology Assessment in Health Care. Annu Meet Int Soc Technol Assess Health Care Int Soc Technol Assess Health Care Meet 2003; 19: 92. Available: http://gateway.nlm.nih.gov/MeetingAbstracts/ma?f=102276010.html (Accessed 20 October 2009).
22. Brugha R, Varvasovszky Z. Stakeholder analysis: a review. Health Policy and Planning 2002; 15(3): 239-246.
23. Reich MR. The politics of reforming health policies. IUHPE (Union for Health Promotion and Education European Conference on the Effectiveness and Quality of Health Promotion) 2002; IX/4. Available: http://www.wcfia.harvard.edu/sites/default/files/695__Politics.pdf (Accessed 21 October 2009).
24. WHO. Writing oral health policy: a manual for oral health managers. Brazzaville: WHO Regional Office for Africa, 2005; 3.
25. Kuratko DF, Hodgetts RM. Entrepreneurship: theory, process and practice 7th edn. Mason, OH: Thomson, 2007; 583.
26. Lesotho Government. National policy to achieve oral health for all Basotho (2002-2011). Draft report. Maseru: Government Printers, 2002.


