Introduction
Women in rural and remote settings face unique geographical, social economic and political challenges. They have diverse needs and health issues, which have historically been neglected by the healthcare system1-3. Studies in women's health have shown that health concerns the totality of women's experiences throughout the life span, with the implication that overall health includes, but is not only defined by, reproductive health4,5. The health concerns and life circumstances of women in different age cohorts are not the same, and as a result health systems work unevenly for women, failing to address specific needs across life spans, geographical circumstances and socio-cultural economic divisions6. Young and older women, for example, face age-group specific issues that constrain their access to appropriate care7. It is necessary to understand and provide support for women's health at critical stages in the life cycle when support may be required.
Globally epidemiological research has increased public awareness of risk factors associated with disease and has provided invaluable evidence in several areas of public health, for example: studies on intimate partner violence in multiple countries8 and data from large scale mortality studies in post-conflict nations9. However this is limited in its capacity to reveal a holistic picture of health, especially young women's health10. Attention is often focused on individual-based risk factors and epidemiological studies are decontextualized from the social relationships within which these risk factors occur11,12. In addition, the studies do not portray the social, material and structural factors that influence risk behaviours and ultimately health.
Young women in rural Papua New Guinea
Young women's health in Papua New Guinea (PNG) is synonymous with discussions about HIV transmission and reproductive health. Current statistics reveal that the 15-24 year age group make up over 50% of the HIV prevalence, with females in this age group having an estimated prevalence of 0.9%13,14. As a result, reproductive and sexual health programs respond to adolescent health in relation to specific behavioural, social and environmental 'risk factors' and HIV and sexually transmitted infection transmission risks. Young women are constructed as a risk group and this has lead to stigmatization, scapegoating while it overlooks differences among young women as a group15. There is also little examination of how these risks and relationships might be historically and economically driven processes that constrain individual agency and are rooted in a life of nutritional deficiency, illness burdens, heavy workloads, poverty, gender discrimination and unequal access to educational and other opportunities16,17. Although health related behaviour is to some extent within the control of an individual young woman, many of the social determinants of health are not, and her agency is constrained by the situations and statuses that are conferred on her18.
Risk factors and young women in Papua New Guinea
Women in PNG face unequal opportunities in education, income generation and access to economic resources and property19. Widespread and entrenched gender inequity leaves girls particularly vulnerable to abuse, exploitation and violence. Intimate partner violence has reached unacceptable levels19 and regional surveys have revealed that 67% of rural women have experienced violence from a spouse or intimate partner20,21. More recently the Government of PNG stated that 'young women all over the country are at high risk of rape, gang rape and other forms of violent sexual assault'22. Female literacy is only 46% and only 6% of the female rural population reach an education level of grade 10 or above23. The low status of women perpetuates patterns of early marriage and frequent childbearing, seen in the total fertility rate of 4.0 (women 15-49 years), one of the highest in the Pacific14. Early marriage increases a woman's vulnerability, and disrupts educational opportunities and social ties. The prevalence and social acceptability of violence against women are major factors contributing to the poor health of young women in PNG19.
The research question - understanding women's health beyond risk factors
It is easy to see solutions as either medical or matters of health education (M Macintyre; pers. comm., 2009). Problems specific to women's health are complex and not attributable to either lack of knowledge or absence of services. Instead she argues that the health status of women reflects the complex and changing social and structural conditions of women's lives. Little is known about rural PNG women's perceptions of their health needs, and even less is known about women's health issues across the lifespan. This is a serious issue in a country where over 80% of the population lives in a rural area. In order to provide an alternative to the current biomedical discourse on rural young women's health in PNG it was necessary to understand the health-related experiences of young women, as shared and narrated by the women themselves, and to examine health as it is situated within the socio-cultural context of women's lives.
Aim and objectives
The overarching aim of the larger study of which this article is one aspect was to undertake an ethnographic assessment of women's health within the socio-historical context of PNG to: (i) identify if there are critical points in the lifespan affecting positive change in the health status of women; and (ii) ascertain if the gap between the perceptions of service providers and the real needs of women can be bridged. The objectives of this article were to examine young women's perceptions of health and health-related experiences using a gender analytic framework, and to identify priority areas for public service interventions.
Method
Use of the qualitative approach
This study used rapid ethnographic assessment, a modification of traditional ethnography which accommodated a combination of qualitative and interpretive methods and a shortened period of time in the field. Rapid ethnographic assessment and interpretive methods enable researchers to learn about what is happening to individuals and groups of people within a specific setting, and to gain meaningful contextual data by paying necessary attention to social and economic factors, cultural practices and local ecological circumstances24. The methods create space for shared dialogue between researcher and participant25. Ten in-depth interviews (IDI), 2 ranking exercises (RE), 2 focus group discussions (FGD) and 2 photo narrative (PN) exercises were conducted. Questions centered on young women's personal narratives and perspectives of their health-related concerns, with particular attention to understanding these perspectives within the social context.
In FGD and IDI, open-ended questions sensitive to the context were used to reveal what being healthy meant to young women:
- Tell me about everyday life. What is a woman's life like here?
- When you say are healthy what do you mean?
- What can you do to stay healthy? What is the most important thing you do to stay healthy?
- Do you often think about your health? If no, what brings 'health' to mind? If yes, what makes you think about it?
- What are the (health) problems women (your age) face here? What problems are worse than others? How?
- Does your mother face the same problems as you? If no, how are they different?
- Is there something you do to overcome the problem of (name problem)? If no, how do you think this problem could be overcome?
Photo narratives added an extra dimension to focus group discussions26, with photos of women at different stages of their lives (child, adolescent adult) used to stimulate discussion. Participants were shown pictures of women from a similar rural PNG context and undertaking specific tasks or responsibilities (eg a young woman selling food at the market, a mother sitting with her children). Participants were asked to describe each photo, who was in it and what she was doing. They were asked to think of some of the girls/women of a similar age in their village and to consider what their life might be like. Further questions relating to the photo included, what sort of (health) problems might she have and what do you suggest could be done to help her? Participants were also asked to consider what the girl's/woman's hopes might be for the future. Discussions also attempted to address issues of resilience, hope, aspirations, healing and empowerment.
Ranking and scoring exercises provided a useful means for young women to prioritize, compare and discuss their main health issues. A maximum of 10 health problems were identified collectively. Each issue was represented by an agreed item from the local setting, placed in a row on the ground. For example violence against women was represented by a stick. Each health issue was ranked using pebbles, and attributed various numerical values (free-scoring) that indicated relative importance. Values ranged from 5 (most important issues) to 1 (least important). Emphasis was put on group interaction and consensus regarding identified health problems. Most of the young women who participated in an FGD or PN exercise participated in an RE. This provided the opportunity to gain feedback, and cross-check and validate some of the preliminary findings.
The first author (RH) carried out the majority of discussions in tok pisin (Melanesian Pidgin), the local lingua franca, with the assistance of a local research assistant. The local assistant was from the area and had been working as a health researcher at the study site for several years. Several young women chose to speak their first language (Ndu) and in these cases the discussion was facilitated by the research assistant with the support of a local field assistant. The research assistant assisted in the interpretation of cultural understanding and meanings, and emerging themes were discussed with the local field assistant. Cultural interpreters increased reliability of the data collected as they clarified terms and local nuances, assisted the first author with translations where needed, conducted 'member checks' with key informants, and were able to respond to participants' questions in a meaningful and sensitive way27.
The study site
The research site was a village in the Wosera District, East Sepik Province of PNG. The research was carried out from mid-2005 to February 2006 and was part of a larger study examining rural women's health within the context of women's lives at critical stages in the life cycle.
The Wosera District is part of Abelam territory, an ethnolinguistic group occupying an area between the southern foothills of the Torricelli Range and the Sepik River. Abelam clans are patrilineal kin groups and several clans are represented within each village28. In the Wosera it is common for women to perform the majority of daily domestic duties and subsistence work. Women's health and social development statistics are poor due to entrenched inequalities, multiple role responsibilities and because the status of women is lower than that of men. The payment of a 'brideprice' in which a woman's fertility and labour are acquired from her father, entails husbandly authority over a woman19 (M Macintyre; pers. data, 2009). Of the rural population in the East Sepik in 2000 only 43% of women were literate23. There is a heavy reliance on subsistence production for household consumption. Cash earning opportunities are limited, evidenced by low per capita incomes29-31. In 2004, the antenatal coverage of five health centres in the Wosera was 48%32, below the 2006 national average of 58%13.
Participant recruitment
Snowball and purposive sampling were predominantly used to recruit participants. Women were identified following a community information session and by word of mouth. Recruiting and gaining access to young women was initially challenging because many young women did not attend the community meeting. With the help of a local field assistant young women were targeted specifically, the nature of the study explained and existing misunderstandings clarified.
Single and married participants, unmarried mothers, school leavers and current school attendees were approached and made aware of the study. The snowball recruitment technique allowed for this diversity and the four-month study period ensured there was ample time for participants to talk of their experience with others and encourage some of the more uncertain young women to take part.
Although the study classified young adults as 18-24 years, it became more relevant to rely on social relationships and groupings, rather than actual ages. Self-identification and social acceptance underpinned the sampling process and six women under the age of 18 and six women over the age of 24 self-classified as a young adult. Oral parental consent was obtained by 8 participants under the age of 18. There was an even spread of the socio-demographic groups of young women who participated in each method. For example, of the 2 FGD, 1 was conducted with young women who were married (with and without children) and aged mid- to late 20s, while the second was conducted with single women in their late teens, either currently attending school or no longer enrolled. Eight of the 10 IDI were conducted with single women, one of whom had a child. Three young participants were currently in high school.
Ethical considerations
The participants knew the purpose of the study before discussions took place and were assured of confidentiality. Consent was given orally and participants were not asked to sign a consent form. This was less obtrusive and also took into account high illiteracy levels. This informal process contributed to the establishment of rapport and trust with participants. Ethical approval was obtained in accordance with the requirements of Curtin University's Human Ethics Committee and the PNG Medical Research Advisory Council.
The authors were also aware of their own positions at all times. The first author who undertook the research has lived and worked for several years in PNG. She is sensitive to the social setting and understands the importance of presenting narratives that reveal women's voices and are embedded in landscapes in which they live. The second author is from the developing world and works extensively with participatory and empowerment methodologies.
Data analysis
All IDI, PN exercises and FGD were audio-taped and transcribed verbatim for analysis. The process of analysis involved a deep immersion in the collected data. The first author and local research assistant read, re-read and discussed participants' accounts for emerging themes and issues requiring further questioning33. From emerging themes, codes were generated and applied to segments of transcribed data to identify common categories of importance as well as unanticipated findings. The emerging themes were also communicated to the local field assistant for her consideration, input and cultural contextualisation. The software program Atlas-ti v 4.1 (Atlas-ti; Germany; http://www.atlasti.com/) was used to manage the data analysis process34.
Results
Socio-demographic characteristics
The socio-demographic characteristics of the sample are presented (Table 1). Thirty-three young women participated in the study and ranged in age from 15 to 29 years. Participants had an average education level of grade 6. Four young women were enrolled in grade 6 or above during the study period. One-third of the participants (n = 11) were married and nine of these young women had one or more child. Three of the single young women had a child. Five of the 11 married young women had a village of origin outside the study site; two were from neighboring villages, two from a village within 1 hour's walk and one from another province, accessible only by air or sea. This diversity offered interesting insights and nuances into the ways young women's health needs were framed and prioritized in the context of their marital status and associated roles and responsibilities.
Table 1: Demographic characteristics of 33 young adult women participants
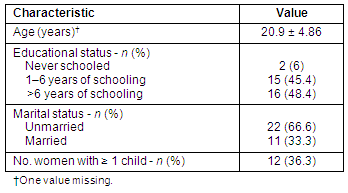
Young women's definitions of health
Young women typically spoke about 'being healthy' by drawing on descriptions from the social and material circumstances of their lives and their daily activities. Young women expressed the need to 'have money' to be healthy, identified during RE as their most pressing health priority and a point discussed at length by all young women.
Angela: If I don't have kerosene I will worry. When I don't have money I find it really hard. If I don't have salt or kerosene, I will sit down and think a lot. How will I get money to buy these things? How will I look after my family? Women have a lot of problems finding money. (FGD, 29 years)
The nature of women's social relationships and access to social support to mediate workload demands and economic constraints also determined good health, and discussions centered on a desire for cooperative and caring spousal, friendship and kinship relations.
Leslie: I'm a young woman and I want to do my own thing. If I want to collect water, cook or go to the garden and harvest vegetables or cut firewood, I will do it. If my parents or in-laws force me then I won't want to do it. I have learnt how to do it already and so I do it when I see there is a need. If they press me to do chores I tell them that I'm not a child, I'm a grown woman. Then if others hear what they say to me they will think that I am disobedient and then they might ruin my name and say that I don't like to work. (PN, 29 years)
All young women expressed similar sentiments for independence. However a desire for increased independence was mediated by their dependence on parental and social support to meet their personal and material needs. Young women's discussions of independence highlighted 3 interrelated sub-themes: (i) the balance between dependence and independence; (ii) the value of financial dependence; and (iii) building healthy relationships. The following quote by Sylvia provides a good illustration of the interplay between the 3 themes, and each is examined in greater detail in the discussion below.
I live with my parents and they don't tell me off. They both give me money. When I want to go around with my friends they give me money. Sometimes when I want to go out they get cross. But generally, I have a good life. But if I go out with my group of girl friends at night my parents do get cross. (IDI, 19 years)
The balance between dependence and independence
A woman's workload was perceived to be unchanging and physically demanding. It involved water collection; the weeding, planting and harvesting of crops; the sourcing and cutting of fire wood; food preparation and cooking; and the washing of clothes and cooking utensils in the river. Unlike adult women or young married women, young women who lived with their parents had fewer workload responsibilities, although most were expected to help their mothers with domestic duties and the care of younger siblings. Amy claimed she had the freedom to choose whether to work or not:
When it comes to sago for example, sometimes I help my mother to harvest it, but sometimes I can't be bothered so I just stay at home. (IDI, 19 years)
All single young women discussed that despite depending on their parents for care and emotional support, they wanted to establish themselves as independent and separate beings from their parents. Young women recognised their security was synonymous with their parents' care. They wanted to be provided for, fairly treated and assigned few responsibilities by their parents, which in turn would give them the opportunity to seek other pastimes. They did not want to seize independence by rebellion but by negotiating with their parents for greater latitude and freedom, as Michelle explained, 'I do a lot of the work, I help my parents and then in return my parents give me money'. Their independence and desire for autonomy therefore was conditional on parental acquiescence. Everlyn expressed the link clearly:
Sometimes we help our mothers to cook. When they are tired we cook. Or if our mothers cook we can do other chores for them. And then they don't get angry and they are happy with us. Then we get on well with our parents and they give us money if we ask for it and they let us go out. (FGD, 22 years)
Parental provision of social and material support would show a single young woman she was respected and cared for, and the result would be compliance and obedience. If a young woman felt neglected by her parents, she was tingting bai bagarap (unable to think straight) and in desperation could seek alternative avenues of support from outside the family. Young women believed this could lead to high risk behaviour, such as substance abuse and transactional sex, and exploitative personal relationships. Parental care and support was also valued by married young women. A mother was required to prepare her daughter for marriage by teaching her the fundamental domestic skills to manage her own household and family.
The act of engaging in a struggle between dependence and independence has been identified as a necessary developmental step towards adulthood10, but for single adolescent mothers, the absence of parental emotional and practical support could have serious mental and physical consequences. Two of the three single adolescent mothers were particularly vocal about the independence they sought from their parents. Adolescent mothers expressed their anger and frustration at the treatment they received from their parents, and the degree to which their life had changed for the worse. They faced the early cessation of education, abandonment by their boyfriends and a stigmatized child. As with the stigma associated with HIV transmission in PNG, there was a pervasive retributive logic that laid the blame on pregnant adolescents because they had defied traditional customs35. They were forced to take on multiple workload tasks and, because the young women were not in formalized relationships such as marriage, they had limited opportunities for help and support.
Michelle: If my brothers can help me to build a house my life will be good as I'll have my own house. Like, now I live with my parents I face a lot of problems. If I had my own house I'd be in a good position. I'd have my own garden and I would go to the market and earn some money and I'd be able to provide for myself. (IDI, 21 years)
These participants also described considerable emotional and physical violence in their lives, as is evidenced by Elsie's account:
I don't respond when he [father] yells. If I talk back then I will get hit and be in a lot of pain. So I just close my mouth and let him yell at me. That's what I do, I don't talk back. (PN, 21 years)
The value of education and financial independence
During interview, all but one young woman discussed money in relation to their autonomy and as a requisite for good health. The search for independence by having access to money was expressed in different ways. The economic needs of married young women were directly related to their new role and accessing the essentials necessary to maintain a household: food, kerosene, soap, clothing and their children's school fees.
Single young women spoke about how having money created opportunities to connect with friends, family and peers, to access market resources, or to buy and share items such as betel nut and cigarettes. The connection between money and the opportunity to purchase items according to the standards set by their peers ran through several interviews. It was important to keep up with the latest style of dress, or to accessorize with hair products and nail polish, and personal items such as clothing, laundry and body soap were a constant issue of concern. Jane explained that she wanted to have the means 'to look after myself.'
If you have money you will think about buying good food, spending time with friends at the market. Money is our support. If I have money I will be healthy, I'll feel happy. If I go to school I know that I will have everything I need. (IDI, 19 years)
The perceived social and economic opportunities that a completed high-school (grade 10) or secondary (grade 12) education offered young women were seen as integral to health. Education was identified as a key strategy to improve current and future wellbeing and to create socioeconomic opportunities. Eight of the single participants, however, discussed the precarious nature of their financial dependence on parents to continue their education. Only 4 of the 8 were currently enrolled in some form of education, with the remaining 4 excluded, mainly due to high education costs and the parental preference for investing in male education. Access to secondary and tertiary education is limited, and even where access is not a problem, the quality of the education provided is often low. Furthermore, an increasing number of youths leave school after completing grades 6, 8, 10 and 12, and cannot find formal employment ether in rural or urban areas due to a lack of experience or qualification36.
Building healthy relationships
Another aspect of the struggle for independence involved young women having the freedom to develop healthy relationships with their female and male friends. Young women described the value of being part of a wider support network of trusted allies who were experiencing the same struggles and concerns. Participants talked about the strong ties they shared with their friends, and that there was a strong correlation between spending time with friends and their sense of happiness.
Sylvia: When I go out with my friends I feel healthy, I feel happy. If I can't go out and have to stay in the house I feel fed up. (IDI, 19 years)
Being happy was interrelated with all three of the themes discussed, and was often heard in conjunction with mi fri long... (I'm free to...). Happiness was associated with autonomy - being free to socialize, free from economic constraints and free from parental influence.
Sue: When I spend time with my friends, I feel really happy. We tell stories about ourselves, we talk to each other, and I feel really happy. (IDI, 18 years)
Many single young women stressed the importance of spending time with their boyfriend. Socializing with an unrelated young man was regarded as an undesirable modern practice by parents and male siblings, as was wearing revealing modern clothing, drinking alcohol, smoking marijuana or going to a 'six to six' disco party. Young women avoided gossip, criticism and cultural expectations through secrecy, which allowed them to have boyfriends without getting caught37. Open affairs were likely to result in a young woman being beaten by her male kin because of the shame of her behavior, which reflected badly on them. Although the exercise of these meetings was often difficult, with go-betweens used to pass messages, young women made a clear link between having the opportunity to nurture an intimate relationship and a sense of wellbeing. This link was expressed as a necessity, mi mas lukim boi fren blong mi na mi bai pilim hamamas (I must see my boyfriend and then I will feel happy), and it was one aspect of their desire for independence that was most difficult to achieve.
Young women were aware that the pursuit of romantic courtship had its risks. Fear of pregnancy was a common health-related concern in young women's accounts of their relationships with young men. As they negotiated the tension between desire for romance, companionship and assessing a potential husband, and the fear of stigma if discovered, the hidden status of the relationship ensured a lack of access to information and contraception13. Young unmarried women in this study were frequently refused family planning information or access to contraception by health workers and volunteers engaged in community-based reproductive and sexual health education activities. Several health workers and volunteers justified their actions to the first author explaining that they did not want to facilitate the promiscuity and sexual activity of young women outside the confines of the marital relationship.
Young married women's struggles to build healthy relationships were discussed in terms of the types of relationships they had with their husband, kin and in-laws, and the different avenues of support available to them to in order to meet the demands of their multiple responsibilities. In spite of her own desire to be cared for, Doreen now had the full responsibilities of an adult and she spoke about her need to be supported in this new role:
If we work together, if my husband follows me to the sago garden and we do the work together, or he looks after the baby while I do the work, when we come back to the village we get on together well. I feel happy. (IDI, 25 years)
All married young women recognized that their physical and emotional wellbeing could be enhanced by having a 'good' husband. This meant a husband who was non-violent and did not seek to control his wife's movements and socialization.
Beryl: A big thing is when we want to go a play sport or socialize with friends, our husbands stop us and we don't feel that this is a good attitude. We ask ourselves, why do they stop us from doing what we want to do? That's what we think about and we worry about it. It's a big thing for us. (RE, 26 years)
Angela: Sometimes men hit their wives. They make us bleed. They use their knives on us and beat us badly. Or some beat their wives with cane. A lot of problems occur because of this and we find it hard to respond. But we do consider leaving our husbands. (RE, 29 years)
Young women desired a man who listened to the requests of his wife, assisted in childcare and other workload activities, and who supported the family financially by sharing or saving any earnings. Married women ranked a supportive husband as their second most important health concern. Anna explained that having a supportive husband was an aspect of life that was integral for creating a sense of wellbeing.
From my perspective, I feel really good when my husband helps me and we work together. I feel encouraged and I think, because of his help, I am able to have some time to rest in the village. (IDI, 21 years)
In PNG a husband who worked regularly in the gardens and assisted with childcare was not typical, however, and in order to cope with the new roles and responsibilities associated with marriage, most of the young women still sought support from their maternal family. Although young woman expressed a desire for independence that could be achieved by marrying and living away from the familial household, they felt that residing in a different province, district and even village, could be an isolating and demanding experience in terms of their daily life and existence with no kin to support them. However, as the marriages of the young women in the present study were contracted between partners in different sections of the same village or neighboring village, most were never far from their natal homes38. This gave Anna much needed access to social, material, emotional and physical support at a challenging stage of her life cycle.:
My mother comes and visits me here. Anything I need she gives me, like sago, vegetables, bananas. She goes and gets it from her garden and gives it to me. (IDI, 21 years)
Discussion
Understanding the links between health and lived experiences
Good health - a social and cultural experience: Good health in rural PNG, as voiced by the young women of this study, is a social and cultural experience, not an isolated or individual condition. All the young women viewed health in the context of their social world. The meaning of health was always embedded in descriptions of women's connection with others, the demands of their gender roles and responsibilities, and their capacity to meet pressing economic and material concerns, and motivated by their efforts at independence. There are similarities between the descriptions of health by the women in this study and those mentioned by women in different cultural contexts, such as Cameroon39, United Arab Emirates3, Wales40 and Ecuador41. The voices and narratives of young women in this study have drawn similar attention to the relationship of health to wider life experiences. It is these narratives that are absent in the current political and public health discourse in PNG.
Contrary to the current discourse on young women's health in PNG that is focused on risk factors and behavioural determinants of sexual and reproductive health, young women's health needs were articulated in response to what Bannister and Schreiber term 'struggles for independence' in daily life, and their connectedness to others most important and closest to them10. Thus, the current approach that addresses risk behaviour has the potential to be perceived as alien and irrelevant to the real life experiences of adolescent women10.
Connectedness and good adolescent health
The link between connectedness and good adolescent health has been extensively considered and documented41-44. Being well connected to significant other persons (or institutions) can provide a sense of belonging, an absence of loneliness and a perceived bond with socialization agents, and is protective against problematic behaviour and poor health outcomes. If young people have mutually beneficial relations with the people and institutions of their social world they have a greater chance of a future marked by positive contributions to self, family, community and civil society43.
The young women in this study expressed their desire to be connected to others, their family and peer groups. Connectedness to the school institution and school friends was discussed as important for good health for some young women, and supports other studies that have examined school connectedness as a protective factor for adolescent health45,46. Happiness was associated with affectionate and communicative interaction and supportive and fair parenting. In the domestic environment this meant having parents that did not intrude on, exploit or manipulate a young woman's independent self43.
Developing healthy relationships with boyfriends and in marriage
Participants romanticized and favoured love-match marriages to the traditional practice of kin-arranged or preferred marriage. These relationships were discussed in terms of respect and cooperation, as well as psychological intimacy. The social and cultural context of these young women's lives, however, impacted on their ability to develop these types of relationships. Young women, for example, took great care to hide their pre-marital relationships from male siblings and parents, as well as from public view. The social and emotional consequences of premarital pregnancy have been documented47, and as evidenced by the accounts of the young women in this study, manifest in low self-esteem, feelings of social isolation, helplessness and powerlessness. It is now well known that being abandoned or stigmatized can force women into casual and commercial forms of sexual networking, adding extra health and social burdens48.
Married participants expressed frustration that their expectation of marriage as companionate and supportive was often not met. Respondents' descriptions highlight the importance of understanding the effect of gender expectations on young women's lives, their growing economic responsibilities, as well as the new responsibility for the primary care of their families49. The married women in this study sought healthy and supportive relationships with their own kin, husband and in-laws in response to their gendered roles, financial insecurity and heavy workloads.
Health and the socioeconomic status of women
The link between health and the socioeconomic status of women is receiving more attention50,51,41. The circumstances of want created an oppressiveness in young women's lives and they struggled to meet their basic needs on severely restricted budgets. Continued access to education was tenuous for some and impossible for most. Unmarried mothers were particularly disadvantaged without a husband to assist in child rearing, subsistence labor or through paid work. Some security was felt in the support young married women received living close to their natal family.
Conclusion
This study has shown that rural young women have distinct health-related perceptions and experiences related to the social, economic and cultural circumstances of their lives. The results document that health is related to the gendered roles and responsibilities of women within their families and communities, and not limited to the reproductive cycle and child-bearing. These findings are consistent with a recent study of Indigenous adolescents in Australia that shows vulnerabilities to ill-health are embedded in the social and cultural context, and related to educational constraints, drugs and alcohol and racial discrimination52.
Recommendations
To deliver effective health care, we argue that is not enough to focus only on reproductive and maternal health. It is essential that there is an examination of the challenges facing young women at various phases of their lives - when they are single, married or single mothers. The WHO strategic approach to improving reproductive health policies and programs provides a useful framework for the development of evidence-based policymaking for women's health in PNG53. This three-stage approach - strategic assessment and action research; identifying and addressing management, technical and socio-cultural resource issues that affect service delivery and quality of care; and participatory and collaborative decision-making among a variety of stakeholders - provides the scope to assess and manage women's health within a broader context of health, to explore viable program alternatives and to encourage multidisciplinary stakeholder involvement. The methodology, with its systems framework and participatory process, has proven useful for assisting countries such as Bolivia and Ethiopia in the process of identifying health priorities and in the design and strengthening of health policies and programs.
The study revealed the intricacies and complexities of the lives of young women, their agency and struggle for independence against entrenched communal and institutional practices. There is also the need to evaluate the impact of the challenges faced on self-esteem, resilience, pro-social behaviors such as sharing, generosity and helping and problem behaviour avoidance - aspects that build agency45. Further exploration is required to understand the ways in which young women prioritize different relationships and health at various points in their lives.
Policymakers and practitioners should be required to identify and respond to key factors in women's health experiences54. Given the role of connectedness, for example, in young women's lives there is a need to further examine and communicate a small number of basic conditions parents, teachers, peers, health educators should attempt to facilitate in their relationships with young women43. This provides the opportunity to enhance parenting and teacher training skills in support of adolescent autonomy, respect for individuality, mutual trust and respect and positive discipline. Peers and family members could also be trained as mentors to act as role models and to motivate and spend time with young women. This could enhance the established mentor-type relationships that some young women experienced with key family members. Mohajer et al. noted that mentoring programs can provide a medium for family members to engage with youth, build their self-esteem and empower young people in a culturally acceptable way52.
An alternative approach to women's health would be to value women's own accounts of their health, and to examine gender roles and responsibilities as they affect health. To ensure a better balance between the treatment of disease and infirmity, and health promotion and prevention efforts, greater consideration must be given to the many factors beyond clinical health services that contribute to rural women's health. Health professionals in PNG must take up the challenge to reshape their understanding of how young women's experiences and life circumstances influence their health and wellbeing.
References
1. Leipert B, Reutter L. Developing resilience: how women maintain their health in northern geographically isolated settings. Qualitative Health Research 2005; 15(1): 49-65.
2. Wathen CN, Harris RM. 'I try to take care of myself.' How rural women search for health information. Qualitative Health Research 2007; 17(5): 639-651.
3. Winslow W, Honein G. Bridges and barriers to health: her story - Emirati women's health needs. Health Care for Women International 2007; 28(3): 285-308.
4. Moss N. Gender equity and socioeconomic inequality: a framework for the patterning of women's health. Social Science and Medicine 2002; 54(5): 649-661.
5. Weisman CS. Changing the definitions of women's health: implications for health and health care policy. Maternal and Child Health Journal 1997; 1(3): 179-189.
6. Wyn R, Solis B. Women's health issues across the lifespan. Women's Health Issues 2001; 11(3): 148-159.
7. World Health Organization. Gender sensitivity and gender-based analysis in women's health development. Historical outlines and case studies of best practice. Kobe, Japan: Women and Health Program, Centre for Health Development, 2003.
8. Garcia-Morena C, Jansen HA, Ellsberg M, Watts CH. Prevalence of intimate partner violence: findings from the WHO multi-country study on women's health and domestic violence. Lancet 2006; 368(9543): 1260-1269.
9. Coghlan B, Brennan R, Ngoy P, Dofara D, Otto B, Clements M et al. Mortality in the Democratic Republic of Congo: A nationwide survey. Lancet 2006; 367(9504): 44-51.
10. Bannister E, Schreiber R. Young women's health concerns: revealing paradox. Health Care for Women International 2001; 22(7): 633-647.
11. Link B, Phelan J. Social conditions as fundamental causes of disease. Journal of Health and Social Behaviour 1995; 36: 80-94.
12. Schulz AJ, Lempert LB. Being part of the world: Detroit women's perceptions of health and the social environment. Journal of Contemporary Ethnography 2004; 33(4): 437-465.
13. World Health Organization/Western Pacific Regional Office. Country health information profile. Papua New Guinea. Western Pacific region health databank. (Online) 2008. Available: http://www.wpro.who.int/countries/countries.htm (Accessed 20 August 2008).
14. UNAIDS/WHO. Epidemiological fact sheet on HIV and AIDS core data on epidemiology and response. Papua New Guinea 2008 update. Geneva: UNAIDS/WHO Working Group on Global HIV/AIDS and STI Surveillance, 2008.
15. Hewat S. Love as sacrifice. The romantic underground and beliefs about HIV/AIDS in Manokwari, Papua. In: L Butt, R Eves (Eds). Making sense of Aids: culture, sexuality and power in Melanesia. Honolulu, Hawaii: University of Hawaii Press, 2008; 150-167.
16. Cohen M. Towards a framework for women's health. Patient education and counselling 1998; 33(3): 187-196.
17. Wong G, Li V, Burris M, Xiang Y. Seeking women's voices: setting the context for women's health interventions in two rural counties in Yunnan, China. Social Science and Medicine 1995 41(8): 1147-1157.
18. McDonald C, McIntyre M. Women's health, women's health care: complicating experience, language and ideologies. Nursing Philosophy 2002; 3(3): 260-267.
19. Amnesty International. Papua New Guinea: violence against women: not inevitable, never acceptable! AI index: ASA 34/002/2006. London: International Secretariat., 2006.
20. Bradley C. Why male violence against women is a development issue: reflections from Papua New Guinea. In: M Davies (Ed.). Women and violence . London: Zed, 1994; 10-26.
21. Toft S. Domestic violence in Papua New Guinea, Law Reform Commission PNG occasional paper no.19. Port Moresby: Law Reform Commission of Papua New Guinea, 1986.
22. Committee on the Rights of the Child. Consideration of reports submitted by State Parties Under Article 44 of the Convention, Papua New Guinea, UN Doc. CRC/C/28/Add.20, para. 172. (On line) 2003. Available: http://daccessdds.un.org/doc/UNDOC/GEN/G03/431/76/PDF/G0343176.pdf?OpenElement (Accessed 4 November 2009).
23. National Statistics Office. Papua New Guinea 2000 National Census - East Sepik Provincial Report. Port Moresby: National Statistics Office, 2002.
24. Bentley M, Pelto G, Straus W, Schuman D, Adegbola C, De La Pena E et al. Rapid ethnographic assessment. Social Science and Medicine 1988; 27(1): 107-116.
25. Denzin N, Lincoln Y. Handbook of qualitative research, (2nd edn). San Francisco, CA: Sage, 2008.
26. Ulin P, Robinson E, Tolley E, McNeill E. Qualitative methods: a field guide for applied research in sexual and reproductive health. Research Triangle Park, NC: Family Health International, 2002.
27. Liamputtong P. Researching the vulnerable. London: Sage, 2007.
28. Winkvist A. Water spirits, medicine-men and witches: avenues to successful reproduction among the Abelam. In: R Cecil (Ed.). The anthropology of pregnancy loss. Oxford: Berg, 1996; 59-74.
29. Curry G. Markets, social embeddedness and precapitalist societies: the case of village tradestores in Papua New Guinea. Geoforum 1999; 30(3): 285-298.
30. Curry G. Doing 'Business' in Papua New Guinea: the social embeddedness of small business enterprises. Journal of Small Business and Entrepreneurship 2005; 18(2): 231-246.
31. Curry G, Koczberski G. The risks and uncertainties of migration: an exploration of recent trends amongst the Wosera Abelam of Papua New Guinea. Oceania 1999; 70(2): 130-145.
32. National Department of Health. District reporting. Maternal Health Report January to December 2004. Port Moresby: Information System, Monitoring and Research Branch, National Department of Health, 2005.
33. Dageid W, Duckert F. Balancing between normality and social death: Black, rural, South African women coping with HIV/AIDS. Qualitative Health Research 2008; 18(2): 182-195.
34. Muhr T. Atlas.ti - The knowledge workbench. Visual qualitative data analysis management model building. Berlin: Scientific Software Development, 1997.
35. Eves R, Butt L. Introduction. In: L Butt, R Eves (Eds). Making sense of Aids: culture, sexuality and power in Melanesia. Honolulu, HI: University of Hawaii Press, 2008; 1-23.
36. Serawe S. Situation analysis on young men in Port Moresby, Papua New Guinea. Port Moresby: Foundation for People and Community Development, 2006.
37. Buchanan-Aruwafu H, Maebiru R. Smoke from fire: Desire and Secrecy in Auki, Solomon Islands. In L Butt. R. Eves (Eds). Making sense of Aids: culture, sexuality and power in Melanesia. Honolulu, HI: University of Hawaii Press, 2008; 168-186.
38. Scaglion R. Spare the rod and spoil the woman? Family violence in Abelam Society. Pacific Studies 1990; 13(3): 189-203.
39. Defo B. Effects of socioeconomic disadvantage and women's status on women's health in Cameroon. Social Science and Medicine 1997; 44(7): 1023-1042.
40. Walters V, Charles N. I just cope from day to day: unpredictability and anxiety in the lives of women. Social Science and Medicine 1997; 45(11): 1729-1739.
41. Schoenfeld N, Juarbe TC. From sunrise to sunset: an ethnography of rural ecuadorian women's perceived health needs and resources. Health Care for Women International 2005; 26(10): 957-977.
42. Barber BK, Schluterman JM. Connectedness in the lives of children and adolescents: a call for greater conceptual clarity. Journal of Adolescent Health 2008; 43(3): 209-216.
43. Lerner M, Almerigi JB, Theokas C, Lerner JV. Positive youth development: a view of the issues. The Journal of Early Adolescence 2005; 25(1): 10-16.
44. Roth JL, Brooks-Gunn J. Youth development programs: risk, prevention and policy. Journal of Adolescent Health 2003; 32(3): 170-182.
45. Blum RW, McNeely C, Nonnemaker J. Vulnerability, risk, and protection. Journal of Adolescent Health 2002; 31S: 28-39.
46. Libbey HP. Measuring student relationships to school: attachment, bonding, connectedness, and engagement. Journal of School Health 2002; 74(7): 274-283.
47. Bennett L. Single women's experiences of premarital pregnancy and induced abortion in Lambok, Eastern Indonesia. Reproductive Health Matters 2001; 9(17): 37-43.
48. Hammar LJ. Fear and loathing in Papua New Guinea: sexual health in a nation under siege. Making sense of Aids: culture, sexuality and power in Melanesia. Honolulu, HI: University of Hawaii Press, 2008; 60-79.
49. Avotri J, Walters V. You just look at our work and see if you have any freedom on earth: Ghanian women's accounts of their work and health. Social Science and Medicine 1999; 48(9): 1123-1133.
50. Farmer PE. Infections and inequalities: the modern plagues. Berkley, CA: University of California Press, 2001.
51. Hildebrandt E, Kelber ST. Perceptions of health and wellbeing among women in a work-based welfare program. Public Health Nursing 2005; 22(6): 506-514.
52. Mohajer N, Bessarab B, Earnest J. There should be more help out there! A qualitative study of the needs of Aboriginal youths in rural Australia. Rural and Remote Health 9: 1137. (Online) 2009. Available: http://www.rrh.org.au (Accessed 15 May 2009).
53. Fajans P, Simmons R, Ghiron L. Helping public sector health systems innovate: the strategic approach to strengthening reproductive health policies and programs. American Journal of Public Health 2006; 96(3): 435-440.
54. World Health Organization. Women, ageing and health: a framework for action. Focus on gender. Geneva: WHO, 2007.

