full article:
The current pandemic (H1N1) 2009
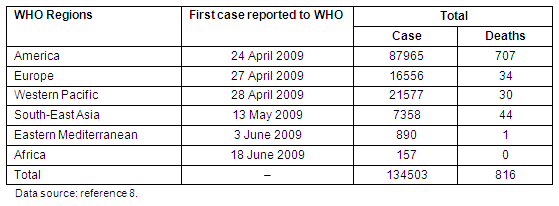
The pandemic (H1N1) 2009 virus has spread from the American continent to other world regions, including Europe, the Middle East, Asia, the Pacific and Africa (Table 1). This complex virus evolved from at least three virus lineages1-3. Genetic analysis of the current H1N1 strain shows it to be a reassortment of six gene segments from the known triple reassorted swine virus, and two gene segments (NA and matrix protein) from the Eurasian influenza A (H1N1) swine virus4. Human-to-human transmission of this reassorted virus has been reported5,6. Based on expert consultation and assessment of all available information, on 11 June 2009 WHO raised the worldwide pandemic alert level to phase 6, indicating that a global pandemic is underway. Within a short time (from April to July 2009), the virus had spread in 160 countries and territories with 134 503 cases and 816 deaths recorded7.
Table 1: Cases of pandemic (H1N1) 2009 worldwide8
Possible impact of current outbreaks in developing countries
To combat and contain the virus, heightened surveillance, the acquisition of up-to-date information, early detection of cases, and the appropriate medical care of cases are crucial. By mid-2009 most pandemic (H1N1) 2009 cases were detected in developed countries but the virus is spreading to developing countries9. Developed countries are better prepared to mitigate the effect of the pandemic than developing countries, with Eduardo et al. suggesting that few developing countries are adequately prepared10. However, studies of previous influenza pandemics suggest that developing countries are disproportionately affected by influenza pandemics11,12. Data from 1918-1920 Spanish Influenza (H1N1) outbreaks suggest the current global influenza pandemic could result in global mortality of approximately 62 million, with 96% of the deaths occurring in the low- and middle-income populations of developing countries12. This prediction is supported by considerable numbers of human deaths in the early stages of the pandemic having occurred in Mexico, a middle-income developing country.
The factors underlying increased mortality in Mexico are not yet clear; however, among contributing factors are the delayed identification of the H1N1 virus (due to a lack of sophisticated laboratory facilities), the absence of early action to block the transmission cycle13 and the virus's greater pathogenicity than the seasonal influenza virus14,15.
Developing countries are characterized by limited access to medical care, undeveloped public health infrastructure, low socio-economic conditions, increased population density, insufficient public awareness and a high prevalence of existing infectious diseases (eg gastrointestinal and respiratory infections, HIV, tuberculosis, malaria, dengue fever and hepatitis). Various host-related factors, such as poor nutritional status, may also influence morbidity and mortality. The currently useful antiviral drugs (oseltamivir and zanamivir) are most available in developed countries such as the USA, Japan and the countries of the European Union16. Vaccines for the current virus are under development in developed countries, where they will be first available. Therefore, additional effort must be made to assist those in developing countries to combat the current pandemic.
Pandemic preparedness plans
The WHO urges all countries to develop and implement national pandemic preparedness plans to prevent, mitigate and minimize the effects of the pandemic (H1N1) 200917. Effective plans for combating any catastrophic infectious disease (such as pandemic influenza) address five issues: (i) surveillance and laboratory services; (ii) communications; (iii) maintenance of community services; (iv) providing medical care; and (v) the supply and delivery of vaccines and drugs18. Social distancing also plays a crucial role in developing countries if one or more of these issues cannot be addressed.
In many developing countries preparedness for combating pandemics is inadequate. However, apart from attempting to follow the approach used in developed countries, inherent capacity in developing countries may assist. Many are regularly subject to natural disasters such as cyclones, floods, famine or earth quakes, and recovery from such events may offer resources useful in combating a pandemic. For example, Bangladesh has suffered from food insecurity for decades; however, that country now produces high-yield rice by planting 2-3 crops each year. Small pox has also been eradicated from this and other developing of countries, and polio vaccine coverage is at almost 100%. In such settings, public health programs have succeeded by integrating the skills of people from differing fields.
To minimize the impact of the current pandemic (H1N1) 2009, immediate preparedness plans should be devised on the basis of local socio-economic conditions. However, some important issues common to most developing countries should be emphasized. The case fatality rate of a pandemic can be reduced substantially by improving the healthcare system. Essential basic supplies such as drugs, masks and gloves should be available to all hospitals and clinics. In case of scarcity, an alternative approach may be developed on the basis of local social realities. A good distribution system is essential and achievable. The gathering of people for festivals and religious meetings should be restricted, if necessary. Also, public health measures, including the provision of clear and timely information, should be undertaken to avoid the spread of panic.
Healthcare personnel require basic understanding of pandemic infection control. Field workers need to be briefed about the nature of the infection, such as the difference between this and the traditional influenza virus, and differing recommendations for management. Indeed, control of the pandemic (H1N1) 2009 is dependent on comprehensive approaches taken by staff of local departments of health, veterinary sciences and animal husbandry. Politicians and policy-makers should play coordinating roles. Information about influenza infection may be new to public health personnel who may be required to collect samples from patients and animals (in conjunction with veterinary workers). In the absence of private facilities, samples may need to be examined at central public health and veterinary laboratories in developing countries.
Public health and veterinary workers may also take the lead in convincing village populations to develop family emergency plans. Such a plan may involve storing food, prescription medicines, face masks, soap, alcohol for disinfection and other essential supplies. This underscores the importance of a larger nationwide mass-media campaign to boost public awareness. And international cooperation with developed countries will assist in establishing and allocating stockpiles of antivirals and other healthcare supplies. International cooperation can also help build capacity in terms of researchers and healthcare workers.
Conclusion
There is every reason for attention to appropriate pandemic preparedness plans in each developing country to prevent, mitigate and recover from this potentially dangerous strain of influenza. In addition, it is important to build capacity for early detection and outbreak control. Using local resources and capacities in each country as well as international collaboration will help achieve essential goals.
References
1. Morens D, Taubenberger J, Fauci A. The Persistent Legacy of the 1918 Influenza Virus. New England Journal of Medicine 2009; 361(3): 225-229.
2. Stein R. Lessons From Outbreaks of H1N1 Influenza. Annals of Internal Medicine 2009; 151(1): 59-62.
3. Trifonov V, Khiabanian1 H, Greenbaum B, Rabadan R. The origin of the recent swine influenza A (H1N1) virus infecting humans. Eurosurveillance 2009; 4: 17.
4. Zimmer S, Burke D. Historical Perspective - Emergence of Influenza A (H1N1) Viruses. New England Journal of Medicine 2009; 361(3): 279-285.
5. Naffakh N, Werf S. April 2009: an outbreak of swine-origin influenza A(H1N1) virus with evidence for human-to-human transmission. Microbes and Infection 11(8-9): 725-728.
6. Peiris J, Poon L, Guan Y. Emergence of a novel swine-origin influenza A virus (S-OIV) H1N1 virus in humans. Journal of Clinical Virology 45(3): 169-173.
7. The World Health Organization (WHO). Influenza A (H1N1) Update 59. (Online) 2009. Available: http://www.who.int/csr/don/2009_07_27/en/index.html (Accessed 27 July 2009).
8. WHO. Pandemic (H1N1) 2009 - update 59. (Online) 2009. Available: http://www.who.int/csr/don/2009_07_27/en/index.html (Accessed 27 July 2009).
9. Kruk M. Emergency preparedness and public health systems lessons for developing countries. American Journal of Preventive Medicine. 2008; 34(6): 529-534.
10. Eduardo A, Nicole S, Raquel G, Sharon D, Marcelle L, Nivaldo L et al. National pandemic influenza preparedness planning. Influenza and Other Respiratory Viruses 2009; 3(4): 189-196.
11. Johnson N, Mueller J. Updating the accounts: global mortality of the 1918-1920 "Spanish" influenza pandemic. Bulletin of the history of medicine 2002; 76(1): 105-115.
12. Murray C, Lopez A, Chin B, Feehan D, Hill K. Estimation of potential global pandemic influenza mortality on the basis of vital registry data from the 1918-20 pandemic: a quantitative analysis. Lancet 2006; 368(9554): 2211-2218.
13. Cohen J. Swine flu outbreak. Out of Mexico? Scientists ponder swine flu's origins. Science 2009; 324(5928): 700-702.
14. Munster V, de Wit E, van den Brand J, Herfst S, Schrauwen E, Bestebroer T et al. Pathogenesis and transmission of swine-origin 2009 A(H1N1) influenza virus in ferrets. Science 2009; 325(5939): 481-483.
5. Maines T, Jayaraman A, Belser J, Wadford D, Pappas C, Zeng H et al. Transmission and pathogenesis of swine-origin 2009 A(H1N1) influenza viruses in ferrets and mice. Science 2009; 325(5939): 484-487.
16. ABC News. Tamiflu stockpiles vary widely throughout world. (Online) 2009. Available: http://abcnews.go.com/International/wireStory?id=7480267 (Accessed 5 August 2009).
17. The World Health Organization (WHO). Pandemic influenza preparedness and response. Phase 5-6 Pandemic. (Online) 2009. Available: http://www.who.int/csr/disease/influenza/pipguidance2009/en/index.html (Accessed 5 August 2009).
18. Gensheimer K, Meltzer M, Postema A, Strikas R. Influenza pandemic preparedness. Emerging Infectious Diseases 2003; 9(12): 1645-1648.



