Introduction
In Jamaica, culturally and traditionally, health has been viewed as being on the other side of the sickness pendulum. This is also the case in many Western societies where health is seen as the 'absence of diseases'1-4, an approach both negative and narrow in scope. According to some scholars, such a concept of health emphasizes the absence of some disease-causing pathogens rather than the presence of health1-3. Such a perspective is in keeping with the traditional biomedical model that views exposure to specific pathogens as the cause of diseases in organisms. This began during the period 130-200 CE in ancient Rome2,5, and despite the efforts of WHO as early as 19464 and Engel6-10 to expand this image of health, it is still widespread in contemporary Jamaica.
Owing to this image of health, healthcare utilization for men can be interpreted as weakness rather than an opportunity for preventative care. With this cultural bias the tern 'sicky sicky' (sickly) is used to describe men who frequently visit healthcare facilities or claim that they are suffering from dysfunction. Men believe they must protect their machoism (masculinity) and will only visit healthcare facilities infrequently in an attempt to display strength; keeping sickness at a distance assists their social survivability. Task specialization is important for Caribbean males and they will not publicly execute certain functions11-14, because gender defines social roles and functions. Masculinity for the Caribbean man is synonymous with power, strength and 'toughness', and he must not show any 'softness' or fragility because these are associated with female behaviour. Therefore Jamaican males generally do not like reading or literature, the English language, home management, child care, nursing or cosmetology, and they cannot appear to be 'sicky sicky' or seek medical care.
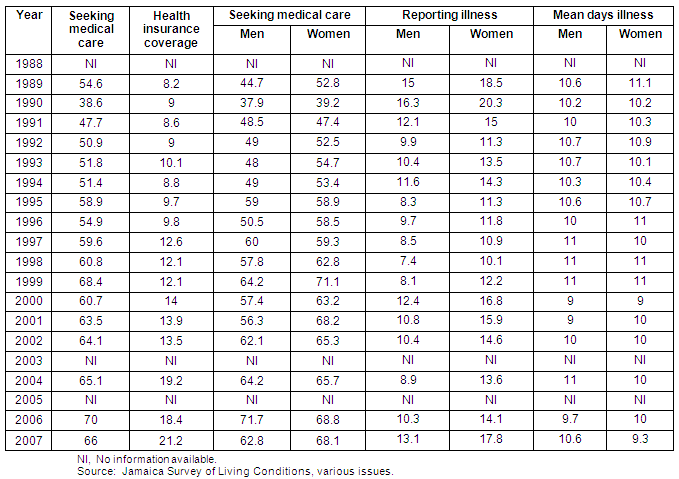
Over the last two decades (1988-2007), statistics from the Planning Institute of Jamaica and the Statistical Institute of Jamaica (in Jamaica Survey of Living Conditions - JSLC)15 have showed that the percentage of Jamaican men reporting illness or ailments to be 16.3% (in 1990), and that 37.9% of these sought medical care. Women, however, reported more dysfunctions and sought more health care, except in 1991, 1995 and 1997 (Table 1). The latest health data available from Jamaica was collected in 2007; this showed that 13.1% of men reported illness and 62.8% of these sought health care. In comparison, 17.8% of women reported ailments and 68.1% visited healthcare facilities for medical care, and spent less time suffering from those illnesses (9.3 days vs 10.6 days for men). This health-gender differential accounts for the disparity in life expectancy between the sexes with women outliving men by 6 years5. Globally, this difference in life expectancy is 8 years more for women than men16,17, emphasizing the role that culture plays in denying men comparatively better health.
Table 1: Percentage of those seeking medical care, self-reported illness, and gender composition of those who report illness and seek medical care in Jamaica, 1988-2007
Although it is not possible to establish that in Jamaica urbanization has resulted in more illness being experienced by rural residents, the Jamaica Survey of Living Conditions (JSLC) revealed that in the period 1988-2007 there were more instances of self-reported illness/injury by rural Jamaicans than urban dwellers. In 2007, 17.3% of rural Jamaicans reported illness compared with 13.9% of those in 'other towns' and 14.1% of those in urban areas. Of those who reported illnesses, 59.9% indicated a chronic recurring ailment. The chronic ailments suffered by rural residents were asthma (8.2%), diabetes (10.8%), hypertension (22.6%) and arthritis (9.3%). The incidence of arthritis and diabetes were higher and lower, respectively, than for those in other geopolitical zones.
Statistics from the Statistical Institute of Jamaica18 indicated that the 5 leading causes of mortality in Jamaican men were cerebro-vascular diseases, diabetes mellitus, ischaemic heart disease, malignant neoplasm of the prostate and hypertensive disease. The rate of cancer in Jamaican men has been said to be greater than that of men in the USA19. If the Jamaican culture means that men are less likely to visit healthcare facilities and more likely to live in rural zones, what determines good health for rural men? A comprehensive review of Caribbean health literature, in particular Jamaican, revealed few relevant studies.
This study examines the social determinants of good health status for rural Jamaican men to assist in health planning. Because Jamaican men make less use of healthcare facilities than women, understanding those with good health may provide an insight into the lives of those with poor health.
Methods
Participants and questionnaire
The current research extracted a sample of 5041 respondents (20.2% of the survey) from a Jamaican national cross-sectional survey of 25 018 respondents20, based on those who lived in rural parishes and were male over the age of 15 years. The original survey used a stratified random probability sampling technique to draw the 25 018 respondents; the non-response rate was 29.7% with 20.5% not responding to particular questions; 9.0% did not participate in the survey and another 0.2% were rejected due to data cleaning. The Jamaica Survey of Living Conditions (JSLC) was commissioned by the Planning Institute of Jamaica (PIOJ) and the Statistical Institute of Jamaica (STATIN) to collect data from Jamaicans on their standard of living in order to assess government policies. These two organizations are responsible for planning, data collection and policy guidelines for Jamaica. The JSLC is an administered questionnaire where respondents are asked to recall detailed information about particular activities. The questionnaire covers demographic variables, health, immunization of children 0-59 months, education, daily expenses, non-food consumption expenditure, housing conditions, inventory of durable goods and social assistance. Interviewers are trained to collect the data, which is prepared by household members. The survey is conducted annually between April and July.
Model
The multivariate model used in the present study is a modification of those of Grossman21, Smith & Kington22 and Bourne5,23, which captures the multi-dimensional concept of health and health status. The current study added some new factors, such as crowding and consumption per person in the household. Another fundamental difference between this and the former models is that the present study is area-specific and focused primarily on rural residence, which includes the majority of the poor in Jamaica. For effective health education and private care to take place, this cohort's health status must be understood.
Measure
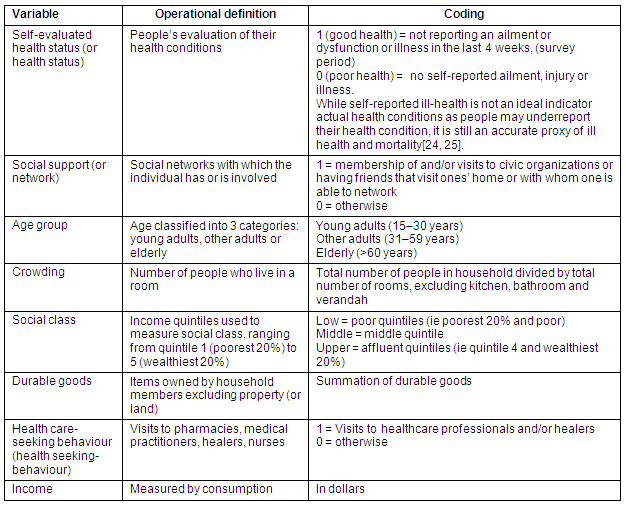
Some critical variables used in this study and their definitions and measurements are provided in Table 2.
Table 2: Operational definitions of particular variables24,25
Statistical analysis
Statistical analyses were performed using SPSS 16.0 for Windows (SPSS; Chicago, IL, USA; www.spss.com). Descriptive statistics included frequency, mean and standard deviation. Logistic regression was used to explore the relationship between the predictor variables and health status. The final model was based on those variables that were jointly statistically significant (p<0.05).
The Hosmer and Lemeshow test26 was used for goodness of fit of the model, and an odds ratio was used to interpret each significant variable27.
Results
Demographic characteristic of sample
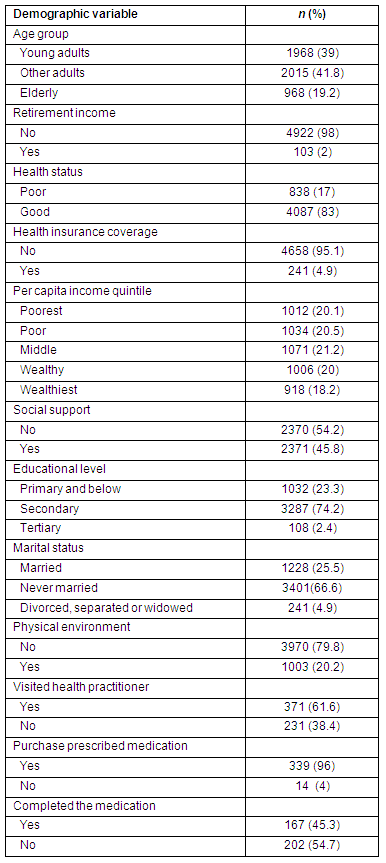
Of the sampled respondents 39% were young adults (15-30 years), 41.8% adults (31-59 years) and 19.2% elderly (≥60 years). In all, 83% reported good health. Only 61.6% (n = 371) of those who indicated poor health had visited a health practitioner in the last 4 weeks. Of those with self-reported health conditions, 96% claimed they had purchased medication, with only 45.3% mentioning that they completed taking the prescribed medication. Of those who responded to the health insurance question, 4.9% (n = 241) had private coverage (Table 3).
Table 3: Demographic characteristics of sampled population, rural residence in Jamaica
Multivariate regression
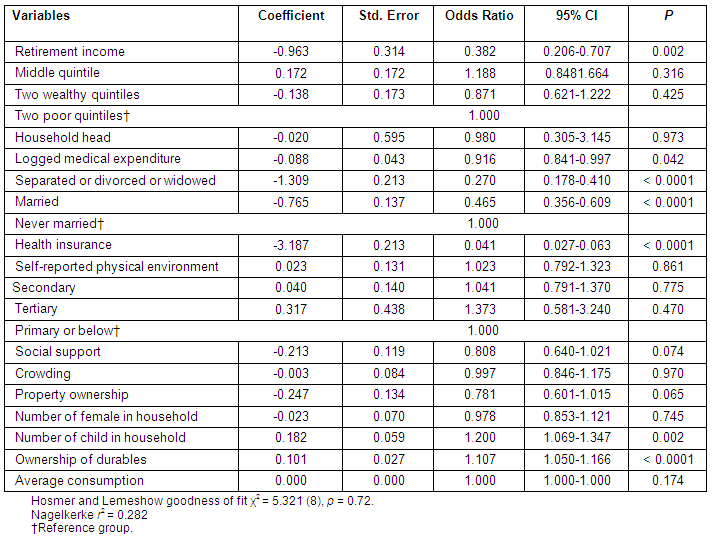
Of the 12 identified variables tested in this study, 6 were found to be statistically significant (p<0.05) for the final model (Table 4). These 6 social determinants are: retirement income, marital status, health insurance, number of children in the household, asset ownership (durable goods), and sex of respondents. The model provided a good fit to the data, based on the Hosmer and Lemeshow test.
Table 4: Logistic regression: explanatory variables of rural health of Jamaican men
Discussion
Jamaica is among those Caribbean societies and developing countries in which men understand health in terms of sickness. They associate sickness with weakness and are less likely to attend healthcare facilities for preventative care because they believe this to be an indicator of weakness. This situation is prevalent in many developing nations. Often these men only become active participants in addressing their health conditions when these have become chronic, incapacitating or life-threatening, affecting their employability, livelihood or sexuality. For instance, men in the Caribbean, and in Jamaica particularly, are less likely to undergo digital prostate examinations; likewise, sexual dysfunctions are not spoken about. This later is not limited to Caribbean men. With Viagra the leading medicine world-wide, sexual dysfunction is not only seen as a weakness in men, but it also suggests how manhood is defined in many societies.
When Jamaican men have an illness their first remedy is self-care or self-medication, compared with women, who seek health care at an early stage in an illness and also for preventive care. It has been found that men are only willing to report life-threatening diseases such as heart disease, and that of those who suffer from erectile dysfunction only 10.5% seek help28. Reasons for barriers to health-seeking behaviour may be embedded in personal beliefs, perceived loss of control, or be related to levels of optimism29, ethnic background and tolerance to risk-taking. This is not limited to Jamaican men; a Malaysian study showed similar health-seeking behaviour, and also reported similarities in Pakistani men28.
Low et al. stated that 'erectile dysfunction (ED) is a common sexual disorder affecting men. Although new treatments for ED have emerged for many years, this does not directly translate into men actively seeking treatment for their ED problem'28. Aspects of this issue include the emphasis placed on biomedical treatment, men's perceptions of issues classified as health related, and even how health information is collected and measured. Low et al. stated 'some men did not see ED as a medical problem, while others accepted it as a normal consequence of ageing'28.
Rural Jamaican men's health
What constitutes good health for rural men in Jamaica? In this study, self-reported health status was used to examine the health of rural men. Is this a good measure? Self-rated health is a complex variable that captures multiple dimensions of the relationship between physical health and other personal and social characteristics. It is consistent in its capacity to predict mortality25,30. It has also been strongly associated with successful aging31. Ringen32 in a paper entitled 'Wellbeing, Measurement, and Preferences' argued that non-welfarist approaches to measuring wellbeing are possible despite subjectivity. The direct approach to establishing wellbeing, according to Ringen, is not better than gathering data by the indirect method (using social indicators). Questions are raised about whether utility is a function of goods and preferences or products and taste. Wellbeing is based on choices, which are a function of individual assets and options. Choices are sometimes 'irrational', which makes for a departure from empiricism32. Hence, self-reported health status (or subjective wellbeing) is a useful way to evaluate people's health.
Self-reported good health in rural Jamaican men is determined by medical expenditure, retirement income, marital status, health insurance, the number of children in the household and ownership of durable goods (excluding property and land). Of the 6 social determinants of rural men's good self-reported health, only 2 positively influence good health: the number of children in the household and ownership of durable goods. The current study revealed that young children (<14 years) not only positively determine the good health of rural men, but that for each additional child in the household, good self-reported health is likely to increase 1.2 times. Good health will also increase 1.1 times if more durable goods are owned by the rural man. Other studies have agreed that wellbeing is increased according to material resources32-35, and that children positively determine good health (or wellbeing).
The impact of number of children: Culturally in Jamaica, children have been seen as futuristic goods for parents (ie income in old age). This cultural reality accounts for the number of children in particular households. In the 1960s, the mean number of people per household was in excess of 6; in the 1970s this had declined to 4, and currently (2007) the figure is approximately 3 per household.
Although the national average is 3.3 people per household (2007), rural households had 3.415. Part of the rationale for more people per household in rural Jamaica is the number of children. Historically, rural people were farmers who owned land. The survivability of the family was based on the farm and the labor available to work it. Poor men who could not afford to hire more workers increased their workforce by using their own children, who would also support their parents in old age. The number of children, and males in particular, were a source of pride for men. The more the farm was worked, the greater the opportunity to acquire possessions. Currently children still provide psychological benefits for rural males, and fatherhood is associated with reduced risky behavior. This accounts for the positive influence of an increased number of children in the household on the wellbeing of rural men in Jamaica.
The impact of poverty: In 1997, the prevalence of poverty in the nation was 19.9%, with rural poverty 2.95 times greater than urban poverty (9.3%), and 1.85 times greater than in 'other towns' (14.8%). By 2007 the nation's poverty had fallen by 50.3% (to 9.9%); however, although rural poverty had fallen by 44.2% (to 15.3%) it was 3.83 times greater than in 'other towns', and 2.47 times greater than urban poverty. It is well established that poverty correlates with ill-health36, but this is not the case for rural Jamaican men for there is no significant statistical association between social class and good health status. It should be noted that rural poverty does not suggest an inability to consume, because the cultural family in rural zones extends beyond heredity to community. Within this social 'family', those who are poor, senior citizens, orphans, ill and children will be assisted by those who have more.
Apart from the labor supply aspect to large rural families, and the pride that children provide, poverty is another motivation for large households. Poverty encourages increased fertility and more children in rural areas, for the future contribution they will make to the economic improvement of the household. A strong association has been found between family size and wellbeing in adult years37, with each additional child in a family increasing future economic wellbeing. In Jamaica, children less than 15 years are unable to work, so their positive influence on rural men's good health is of a psychosocial nature. However poverty alleviation may be seen in terms of investment in a child/children, as equivalent to investing in stocks, bonds, shares.
Other determinants of rural men's good self-reported health
Health insurance coverage: Health insurance is a product people use for future health conditions. In the present study, a rural man was 0.96 times (or 96%) less likely to purchase health insurance. Health insurance coverage cannot be used to measure healthcare-seeking behaviour as it is a precaution, rather than a preventative measure. Rural men buy private health insurance in Jamaica for the high likelihood of ill-health; therefore, health insurance coverage is not a good indicator of preventative health - and rural men's good health is not improved by the purchase of this product. Similarly, those rural men who spent more on medical care were 0.08 times (or 8%) less likely to have good health. Expenditure on medical care is to restore good health and is therefore not a preventative approach to health care for rural men, contrary to previous studies5,23.
Marriage: The literature search suggested that married men have greater wellbeing than those non-married. Smith and Waitzman added that men's gains from marriage were greater than women's38. It has been said that 'many observers have theorized that married individuals have access to more informal social support than do non-married individuals'39, and this explains the higher quality of life of married couples than 'non-married' individuals. Some studies have shown that married people have a lower mortality risk39, and this eplains why they take fewer life-threatening risks38,40.
With a sample of 1049 Austrians aged 14 years and over, Prause et al. found that married individuals reported better subjective health-related quality of life index (8.3) than divorced persons (7.6), or singles (7.7)41. Smock et al. found a direct relationship between married women and economic wellbeing42. Their longitudinal data from the 1987-1988 National Survey of Families and Households (NSHH1) and a follow-up survey (NSFH2) revealed that married women had higher economic wellbeing than those who were divorced, with those who remarried matching their married counterparts and exceeding the wellbeing of single women. For divorced women, as for their married counterparts, educational attainment and work experience were positively associated with wellbeing.
Despite the plethora of studies showing a correlation between marriage and health, Lillard and Panis disagreed43. They found that healthier men were less likely to be married, and that the healthier married men married later in life and postponed remarriage. The study found that unhealthy men entered marriage at an early age, suggesting that these men do so for health reasons43. The results of the present study are consistent with this, finding that rural Jamaican men who had never married were more likely to report good health, compared with married or divorced men.
Retirement income: Another important finding that emerged from this research is the negative correlation of those who rural men who received retirement income with good self-reported health status. This is counter to studies that found increased income to mean greater wellbeing36,44,45. For example, Keister stated (in an article entitled 'Sharing the wealth: the effect of sibling on adult's wealth ownership') that there is 'little doubt that material resources can improve quality of life and wellbeing...'36. It has also been found that material resources have the capacity to improve one's choices, comfort level, state of happiness and leisure, which militates against static wellbeing46,47.
By way of explanation, retirement income is received primarily by those men older than 65 years, a cohort less likely to be in good self-reported health. The current findings were that rural men who received retirement income were 0.382 less likely to report good health in comparison with those who had not received this benefit, and this was the least predictor of good health status of the study.
Conceptual change
It may be that it is necessary to re-culturize health practitioners and health researchers regarding their views and their image of the health and wellness of rural men. Rather than focusing on disease, a positive approach was suggested by a group of Caribbean scholars who stated 'wellness involves the different measures that we use to maintain good health and is geared towards preventing illness and diseases'48. Health is broader than diseases4, and this confirms the use of social determinants in health discussions49-55. However, Davidson et al.'s conceptual framework for good health in Jamaica48 lacks specifics for rural residents or rural men48. Empirical studies have shown that self-reported illness, self-evaluated health status, happiness, and life satisfaction can all be used to measure health21-25,30,49,56, and self-reported illness or health status have been found to be good predictors of objective health (such as mortality or life expectancy)24,25,30.
The Jamaica Survey of Living Conditions collects data from Jamaicans on their living conditions, and among the questions is the item: 'In the last 4 weeks have you had an ailment or illness not caused by injury?'. The current study used the self-evaluated health conditions to measure health status, seeking to model the social determinants of health among rural men.
Since 2000 the WHO and others have discussed the use of social determinants of health in anticipating policy directions53,54,57. Like others before it4,48,57, the present study has shown the role of social determinants in determining good health. However, this study has distinguished factors specific to sex and geographic location, and this is significant in predicting the health (or wellbeing) of a populace or a sub-population1-3,5,21-23,49-55 - in this case rural Jamaican males.
Using self-reported health conditions to measure the self-evaluated health status of rural Jamaicans, Bourne & McGrowder56 found 12 socio-psychological variables that determined good self-reported health (cost of medical care; education; retirement income; health insurance coverage; house tenure; gender; crowding; psychological affective conditions, positive and negative; age; living arrangements; and typology in the number of people who resided in the household - age and sex). Although the current study used the same definition of self-evaluated health, the social determinants of good health for rural men were not necessarily the same. Identifying these for this specific sup-population provides a framework for understanding58-60 and addressing inequalities that exist in the health of males in Jamaica. This also offers a useful approach for future work.
Conclusion
In summary, good self-reported health status in rural men is a function of health insurance coverage, marital status, the number of children in the household, retirement income and ownership of durable goods (excluding property and land). This study provided insights into social factors that determine the good health status of rural men, and within this reality healthcare practitioners can now devise appropriate programs to address the health concerns of this cohort.
One way to improve the level of health in a population is to address the health concerns of the poor - in Jamaica this means rural residents. Men continue to seek less care than women, and when this is added to rurality, poor rural men seek even less health care. Addressing the health gaps that exist in the Jamaica population, particularly among rural men, is an urgent concern.
The present study highlights that social determinants of self-evaluated (or reported) health status may differ among countries, and even within nations and between sexes. Public health practitioners must understand this when seeking to make a difference.
The way forward
Men, in particular rural men, have been understudied in Jamaica. This study has provided an understanding of some issues surrounding health from their perspective. These findings may be used to inform future studies. Policy-makers may also be able to use the information to inform health promotion, interventions and education campaigns specifically for rural men. The results of this study suggest that health status is experienced similarly among the rural men studied, regardless of social determinants. Current health policies may, therefore, not meet the needs of this particular group of men in Jamaica.
The results of this study also challenge the notion that education means people make better health choices, thereby gaining improved health status. This may explain the higher mortality in males as policies fail to reach the target population. Another issue highlighted by this study is the relationship between health and marital status, with married men reporting lower health status than single men, suggesting that rural married men should be included in health promotion campaigns. Further research is needed into the relationship between health and marital status in rural Jamaican men to understand the impact of their value systems, health challenges, health decisions and lifestyle on health inequality.
This study on the social determinants of health does not provide all the answers but it has identified some health inequalities among rural men in Jamaica. More answers are needed to effectively aid policy formulations. Policy implementation in Jamaica needs epidemiological monitoring and analyses over time in order to understand how to guide future research-based policy implementation.
References
1. Longest BB. Health Policymaking in the United States, 3rd edn. Chicago, IL: Health Administration Press, 2002.
2. Brannon L., Feist J. Health psychology. An introduction to behavior and health, 6th edn. Los Angeles, CA: Wadsworth, 2007.
3. Bourne PA. A theoretical framework of good health status of Jamaicans: using econometric analysis to model good health status over the life course. North American Journal of Medical Sciences 2009; 1(2): 86-95.
4. World Health Organization. Preamble to the 1948 Constitution of the World Health Organization as adopted by the International Health Conference, New York, June 19-22, 1946. In: Basic documents, 15th edn. Geneva: WHO; 1948.
5. Bourne PA. Medical Sociology: modelling well-being for elderly people in Jamaica. West Indian Medical Journal 2008; 57: 596-604.
6. Engel G. A unified concept of health and disease. Perspectives in Biology and Medicine 1960; 3: 459-485.
7. Engel G. The care of the patient: art or science? Johns Hopkins Medical Journal 1977; 140: 222-232.
8. Engel G. The need for a new medical model: a challenge for biomedicine. Science 1977; 196: 129-136.
9. Engel G. The biopsychosocial model and the education of health professionals. Annals of the New York Academy of Sciences 1978; 310: 169-181
10. Engel GL. The clinical application of the biopsychosocial model. American Journal of Psychiatry 1980; 137: 35-544.
11. Barrow Christine. Caribbean Gender Ideologies: Introduction and Overview. In: B Christine (Ed.). Caribbean portraits: essays on gender ideologies and identities. Kingston, Jamaica: Ian Randle, 1998.
12. Chevannes B. Learning to be a man: culture, socialization and gender identity in five Caribbean communities. Kingston, Jamaica: The University of the West Indies Press, 2001.
13. Gayle H. Adolescent male survivability in Jamaica. Kingston, Jamaica: The Jamaica Adolescent Reproductive Health Project (Youth Now), 2002.
14. Parry O. Masculinities, myths and educational underachievement: Jamaica, Barbados, and St Vincent and the Grenadines. In: R Reddock (Ed.). Interrogating Caribbean masculinities: theoretical and empirical analyses. Kingston, Jamaica: University of the West Indies Press, 2004.
15. Planning Institute of Jamaica, Statistical Institute of Jamaica. Jamaica Survey of Living Conditions, 1989-2007. Kingston, Jamaica: PIOJ and STATIN, 2008.
16. United Nations. Statistical yearbook, 50th issue. New York: Department of Economic and Social Affairs, Population Division UN, 2006.
17. United Nations. World Population Ageing, 2007 and United Nations. Washington: UN, 2007.
18. Statistical Institute of Jamaica. Demographic statistics 2007. Kingston, Jamaica: STATIN, 2008.
19. Glover FE Jr, Coffey DS, Douglas LL, Cadogan M, Russell H, Tulloch T et al. The epidemiology of prostate cancer in Jamaica. Journal of Urology 1998; 159: 1984-1986.
20. Statistical Institute Of Jamaica. Jamaica Survey of Living Conditions, 2007. Kingston, Jamaica: Statistical Institute of Jamaica, 2007.
21. Grossman M. The demand for health - a theoretical and empirical investigation. New York: National Bureau of Economic Research, 1972.
22. Smith JP, Kington R. Demographic and economic correlates of health in old age. Demography 1997; 34: 159-170.
23. Bourne PA. Health Determinants: using secondary data to model predictors of well-being of Jamaicans. West Indian Medical Journal 2008; 57: 476-481.
24. Idler EL, Kasl S. Health perceptions and survival: do global evaluations of health status really predict mortality. Journal of Gerontology 1991; 46: S55-S65.
25. Idler EL, Benyamini Y. Self-reported health and mortality: a review of twenty-seven community studies. Journal of Health, Society and Behaviour 1997; 38: 21-37.
26. Homer D, Lemeshow S. Applied logistic regression, 2nd edn. John Wiley & Sons, New York, 2000.
27. Hair JF, Black B, Babin BJ, Anderson RE, Tatham RL. Multivariate data analysis, 6th edn. Upper Saddle River: NJ: Prentice Hall, 2005.
28. Low W-Y, Chirk-Jenn NG, Choo W-Y, Hui-Meng T. How do men perceive erectile dysfunction and its treatment: a qualitative study on opinions of men? The Aging Male 2006; 9: 175-180.
29. Clarke VA, Lovegrove H, Williams A, MacPherson M. Unrealistic optimism and the health belief model. Journal of Behavioral Medicine 2000; 23: 367-376.
30. Bourne PA. The validity of using self-reported illness to measure objective health North American Journal of Medical Science 2009; 1(5): 232-238.
31. Roos NP, Havens B. Predictors of successful aging: a twelve-year study of Manitoba elderly. American Journal Public Health 1991; 81: 63-68
32. Ringen S. Wellbeing, measurement, and preferences. Scandinavian Sociological Association 1995; 38: 3-15.
33. Blanchflower DG, Oswald AJ. Well-being over time in Britain and the USA. Journal of Public Economics 2004; 88: 1359-1386.
34. Lima ML, Nova R. So far so good: subjective and social wellbeing in Portugal and Europe. Portuguese Journal of Social Science 2006; 5(1): 5-33.
35. Becker GS, Philipson TJ, Soares RR. The quantity and quality of life and the evolution of world inequality. American Economic Review 2005; 95: 277-291.
36. Alleyne GAO. Equity and health. In: Equity and health: views from the Pan American Sanitary Bureau. Occasional publication no 8. Washington, DC: Pan American Health Organisation; 2001; 3-11.
37. Keister LA. Sharing the wealth: the effect of sibling on adult's wealth ownership. Demography 2003; 40: 521-542.
38. Smith KR., Waitzman NJ. Double jeopardy: interaction effects of martial and poverty status on the risk of mortality. Demography 1994; 31: 487-507.
39. Goldman N. Marriage selection and mortality patterns: inferences and fallacies. Demography 1993; 30: 189-208.
40. Umberson D. Family status and health behaviors: social control as a dimension of social integration. Journal of Health and Social Behaviour 1987; 28: 306-319.
41. Prause W, Saletu B, Tribl GG, Rieder A, Rosenberger A, Bolitschek J et al. Effects of socio-demographic variables on health-related quality of life determined by the quality of life index-German version. Human Psychopharmacology Clinical and Experimental 2005; 20 359-365.
42. Smock P, Manning WD, Gupta S. The effects of marriage and divorce on women's economic wellbeing. American Sociological Review 1999; 64: 794-812.
43. Lillard LA, Panis CW. Marital status and mortality: the role of health. Demography 1996; 33: 313-327.
44. Alleyne GAO. Health and economic growth. In: Equity and health: views from the Pan American Sanitary Bureau. Occasional publication no 8. Washington, DC: Pan American Health Organisation; 2001; 265-269.
45. Oswald AJ. Happiness and economic performance. Economic Journal 1997; 107: 1815-1831.
46. Easterlin RA. Building a better theory of wellbeing. In: Proceedings, Paradoxes of Happiness in Economics; 21-23 March 2003; Milan, Italy; University of Milano-Bicocca; 2003.
47. Easterlin RA. Income and happiness: towards a unified theory. Economic Journal 2001; 111: 465-484.
48. Davidson W, Wright V, Lowe H. The wellness handbook: your guide to healthy living. Kingston, Jamaica: Pelican, 2002.
49. Hambleton IR, Clarke K, Broome HL, Fraser HS, Brathwaite F, Hennis AJ. Historical and current predictors of self-reported health status among elderly persons in Barbados. Revista Panamericana de Salud Publica 2005; 17(5-6): 342-352.
50. Asnani MR, Reid ME, Ali SB, Lipps G, Williams-Green P. Quality of life in patients with sickle cell disease in Jamaica: rural-urban differences. Rural and Remote Health 8: 890. (Online) 2008. Available: www.rrh.org.au (Accessed 12 November 2009).
51. Diener E. Subjective well-being: the science of happiness and a proposal for a national index. American Psychological Association 2000; 55: 34-43.
52. Graham H. Social determinants and their unequal distribution clarifying policy understanding. The MilBank Quarterly 2004; 82(1): 101-124.
53. Wilkinson RG, Marmot M. Social determinants of health. the solid facts, 2nd edn. Copenhagen: World Health Organization, 2003.
54. Kelly M, Morgan A, Bonnefog J, Beth J, Bergmer V. The social determinants of health: developing evidence base for political action. Geneva: WHO, 2007.
55. Pettigrew M, Whitehead M, McIntyre SJ, Graham H, Egan M. Evidence for public health policy on inequalities: 1: the reality according to policymakers. Journal of Epidemiology and Community Health 2004; 5: 811-816.
56. Bourne PA, McGrowder DA. Rural health in Jamaica: examining and refining the predictive factors of good health status of rural residents. Rural and Remote Health 9: 1116. (Online) 2009. Available: www.rrh.org.au (Accessed 12 November 2009).
57. WHO. The social determinants of health. (Online) 2008. Available: http://www.who.int/social_determinants/en/ (Accessed 28 April 2009).
58. Graham H. Intellectual disabilities and socioeconomic inequalities in health: an overview of research patterns, determinants and challenges. Journal of Applied Research in Intellectual disabilities 2005; 18(2): 101-111.
59. Graham H, Kelly MP. Health inequalities: concepts, frameworks and policy. London: Health Development Agency, 2004.
60. Graham H. Tracking health inequalities in England: remedying health disadvantages, narrowing gaps or reducing health gradients. Journal of Social Policy 2004; 33(1): 115-131.
Abstract
Introduction: A comprehensive literature review revealed a gap in health research regarding the determinants of good health for rural men in Jamaica. This study seeks to fill this void by examining cross-sectional survey data to model the social determinants of the self-reported good health status of rural men in Jamaica.
Method: A sample of 5041 males (≥15 years) was extracted from a national cross-sectional survey of 25 018 respondents. A stratified random probability sampling technique was used to draw the sample. Data were stored, retrieved and analyzed using SPSS for Windows 16.0 (SPSS; Chicago, IL, USA). Descriptive statistics were used to provide pertinent socio-demographic characteristics of the sample, and logistic regression was used to establish a predictive model for good self-reported health status in rural Jamaican males.
Results: Seventeen percent of rural men claimed that they had poor health, 4.9% had health insurance, 61.6% visited a healthcare practitioner, 96.0% purchased prescribed medications and 45.3% completed the course of prescribed medications. The social determinants of good health status of rural men in Jamaica are cost of medical care (OR = 0.916, 95% CI = 0.841-0.997); retirement income (OR = 0.0.382, 95% CI = 0.206-0.707); marital status: separated, divorced or widowed with reference to those never married (OR = 0.270, 95% CI = 0.178-0.410), and married with reference to never married men (OR = 0.465, 95% CI = 0.356-0.609); health insurance coverage (OR = 0.041, 95% CI = 0.027-0.063); number of children in household (OR = 1.200, 95% CI = 1.069-1.347); and number of durable goods owned (OR = 1.107, 95% CI = 1.050-1.166).
Conclusion: Children continue to be not only futuristic assets to parents, but they also currently improve the health status of rural men.
Key words: good health, health status, Jamaica, public health, rural men, social determinants of health.
You might also be interested in:
2011 - Barriers to the up-take of telemedicine in Australia - a view from providers
