Introduction
According to Rioja et al.1 and Ostry2, in different nations, differences over time between rural and urban mortality have varied in intensity and direction. In the late 19th century, when infectious disease mortality was high, worse sanitary hygiene and over-crowding in cities led to higher mortality rates than in the countryside. With the epidemiological transition, the more rapid pace of modernization in the cities has led to a faster decline in urban mortality relative to rural places so that now, in some (but not all) developed nations, mortality rates in rural places for many causes of death are higher than they are in urban places3,4.
The extent of the difference in mortality across the rural-urban continuum varies, in some cases quite markedly, from nation to nation3,5 and by specific cause of death3,4,6,7. Increasingly researchers recognize that, even in developed nations where rural and urban mortality is similar5, rural areas have higher (in some cases much higher) morality among children and young adults. In developed nations such as Canada and Australia where age-adjusted rural mortality tends to be much greater than rural mortality, deaths from unintentional injuries, poisoning, motor vehicle trauma, and suicide, causes of death which are disproportionately high among the young, also tend to be higher in rural places3,4,8,9.
Several studies in recent years have demonstrated a consistent deficit in health status among rural compared with urban Canadians3,4,6,7,9-11. The most comprehensive of these recent studies was conducted by the Canadian Institute for Health Information (CIHI)4 utilizing morbidity data from the 2002 Canadian Community Health Survey (CCHS) and mortality outcomes obtained from the Canadian Mortality Database (CMD) for the years 1986-1996.
This recent CIHI study utilized a more sophisticated definition of 'rural' than has been used in previous investigations of rural health in Canada12. In most health studies rural places have been defined crudely on the basis of population size. However, CIHI investigators in their 2006 study used Statistics Canada's Metropolitan Influenced Zone (MIZ) system to classify rural places into four sub-groups based, not only on population size, but also on their proximity to urban places, and the extent to which rural places are 'influenced' by nearby urban centers.
The CIHI analysis, using this more finely graded definition of rural places, demonstrated fairly consistent gradients in health outcomes, including mortality, along both the urban-rural continuum and this more finely subdivided rural continuum. This new definition of rurality (fairly well described in the original CIHI study), was operationalized with administrative data and furthers our understanding of the impact of place on health.
The primary purpose of this article is to illustrate the use of an age, gender, and place based re-analysis of data from an existing study4 in order to more clearly demonstrate the role of these three factors in rural-urban differences in mortality, in order to better develop policy to reduce this gap.
The article is organized as follows. The methods section reviews the way 'rural' and 'urban' are defined, and the methods used to gather and analyze data in the original CIHI study. The approach of the present study is outlined, whereby the original study results were re-visited, re-synthesized and presented in such a way that age, gender, and place are integral to the analysis of the mortality gap between urban and rural residents in Canada. The results of the re-analysis are presented in the results section. This is followed by a discussion of the results and suggestions for how this type of age/gender/place analysis might be used to better develop policy targeted to reducing the current gap in mortality along the urban-rural continuum in Canada.
Methods
In the original investigation4, CIHI researchers aggregated records from the CMD to the Census Sub-division (CSD) level for each year in the period 1986-1996. Because some census district boundaries changed over this period, mortality data from each of these years was fitted to 1996 CSD boundaries.
Next, each CSD was categorized into one of 7 possible MIZs (Table 1)12. These MIZs characterize rural areas according to population size and proximity and influence exerted by nearby urban areas. The MIZs offer a more sophisticated way of defining 'rural' than is found in typical analyses where rural areas are defined solely in terms of population size or density. Statistics Canada's MIZ system estimates the level of influence exerted by nearby urban areas by assessing the proportion of residents in a rural CSD who commute on a regular basis to nearby urban areas. While this is a fairly crude measure of urban 'influence' on a rural CSD, it is a vast improvement when compared with traditional 'size-only' measures of rurality.
Table 1: Standard Area Classification codes (MIZ system)
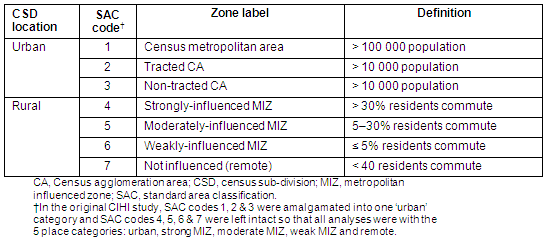
Once mortality data was made available for all CSDs in Canada for each of the years and CSD was categorized into one of the 7 MIZ categories, statistical comparisons of mortality outcomes for major causes of death were made across 5 MIZ categories for different age groups and by gender. Causes of death were extracted from the International Classification of Diseases (ICD) 9 codes found in the CMD.
Complete census data were not available for approximately 20% of the 5984 CSDs in 1996 due to their small population size. In addition, the share of the CSDs included in the CIHI study varied by MIZ: 75.3% for CMAs/CAs, 99.1% for strong MIZ, 93.9% for moderate MIZ, 82.3% for weak MIZ and 50.1% for no MIZ. The suppression of data for CSDs with small populations explains the unavailability of some census data at the CSD level as well. It is clear therefore that sub-populations, particularly those living in very small communities in remote places, were under-ascertained using this sampling framework.
The results section of the original CIHI report and the appendix contained a number of tables with data on mortality rates for major causes of death by MIZ regions, age group, and gender. The original report presented general results with discussion based on each major causes of death. Results were tabulated for each cause of death by gender and age groups (usually years 0-4, 5-19, 20-44, 45-64 and ≥65).
In the present study calculations were performed to determine the proportion of excess deaths occurring in each of the four different types of rural places, relative to deaths in urban places. These calculations were performed for different gender and age groups. In this way, the age, gender, and rural place-specific characteristics of mortality gradients for major causes of death were highlighted. This re-analysis provides a new set of insights into the gender and place dimensions of the mortality gap between urban and rural Canadians, and can be used to more effectively to develop prevention policy in rural Canada.
Results
All-cause mortality by gender and across the urban-rural continuum
In all causes of death (except cancer) age-standardized mortality rates are higher in rural compared with strong MIZs, and male mortality for all causes of death and within each place category is always greater than female mortality (Table 2).
Table 2: Annual mortality rates (per 100 000) in Canada by residence and gender
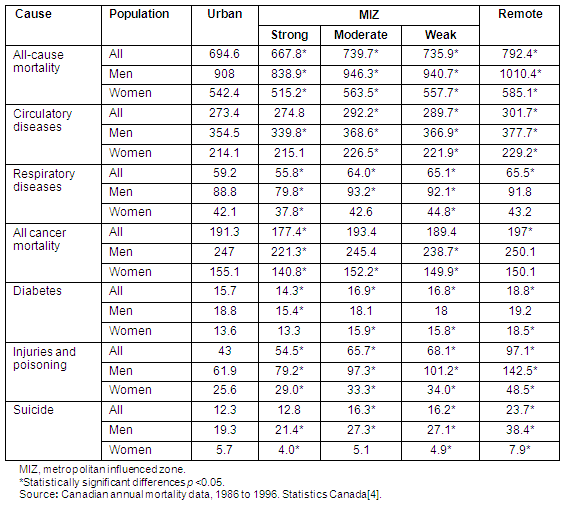
Figure 1 illustrates the presence of a rough gradient in all-cause mortality for both genders moving from strong MIZs through to remote regions. All-cause mortality rates for both men and women are approximately 20% greater in remote compared with strong MIZ regions.
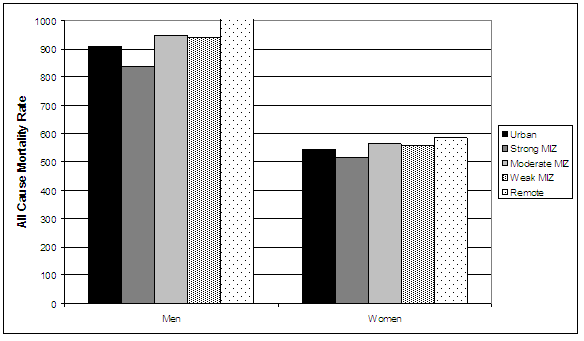
Figure 1: Age-standardized all-cause mortality rates (per 100 000) by place of residence and gender, Canada 1986 to 1996. MIZ, metropolitan influenced zone.
In order to better understand the drivers of this gradient in mortality along the urban-rural continuum it is necessary to look more closely at its age and gender structure.
Variation in all-cause mortality between residents of urban compared with rural regions in Canada by age and gender
Sub-analyses were conducted separately for males and females with age groups 0-4, 5-19, 20-44, 45-64 and over 65 years. As shown in Figure 2 there is only a slight gradient in age-standardized all-cause mortality along the rural-urban continuum for men and women over age 45. In contrast, a strong gradient exists for all-cause mortality among girls and women and boys and young men (Figure 3).
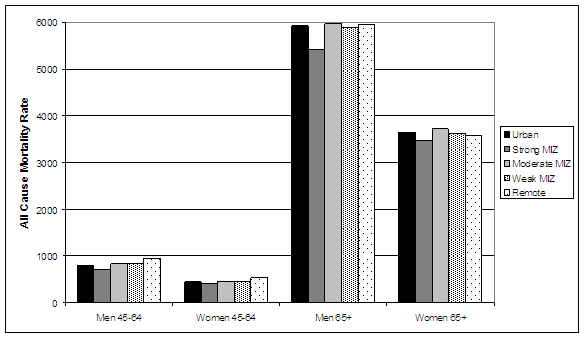
Figure 2: Age-standardized all-cause mortality rates (per 100 000) among women and men (over age 44 years), by place of residence, Canada 1986 to 1996. MIZ, metropolitan influenced zone.
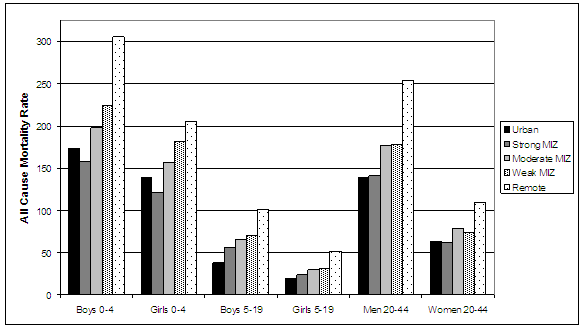
Figure 3: Age-standardized all-cause mortality rates (per 100 000) among boys men, girls and women (less than age 45 years) by place of residence, Canada 1986 to 1996. MIZ, metropolitan influenced zone.
These data demonstrate that the seemingly small gradient in all-cause mortality along the urban-rural continuum observed for the entire population (Fig1) is driven by steep gradients in mortality among people less than age 45. In addition, the highest all-cause mortality rates for males and females under age 45 are found in age groups 0-4 years.
The effect of place on the gradient between urban and across rural places
All-cause mortality in urban places for those less than age 45 was compared with mortality in strong, moderate, weak, and remote places to illustrate the excess all-cause mortality in each of these rural places (Fig4).
Excess mortality in rural compared with urban places was highest for boys and girls age 5 to 19 and lowest for boys and girls age 0-4. For boys and girls age 5-19 living in remote communities, all-cause mortality rates were, respectively, 164% and 157% higher for boys and girls the same age living in urban places.
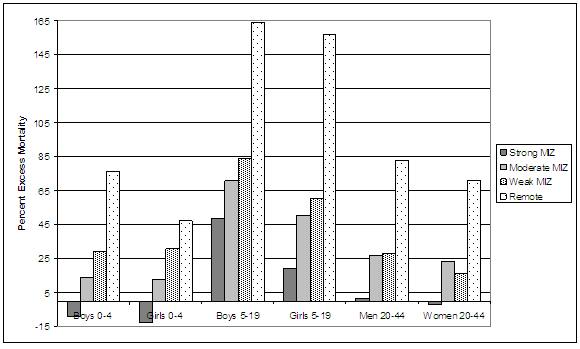
Figure 4: Excess all cause rural relative to urban mortality by age and gender. MIZ, metropolitan influenced zone.
Given that deaths from injury/poisoning, suicides, and motor vehicle accidents (MVAs) make up the bulk of deaths occurring in those under age 45 the gradients across place, in mortality for these causes of death are next explored.
The effect of gender and age on mortality gradient between urban and across rural places for suicide, injury/poisoning, and motor vehicle accidents
Excess suicide mortality for girls and boys age 5-19 living in remote places is, respectively, 533% and 329% greater than for girls and boys of the same age residing in urban places. In weak MIZs excess suicide mortality for 5-19 year-olds is similar for girls and boys and is 'only' 50% greater than those of the same age living in urban places (Fig5).
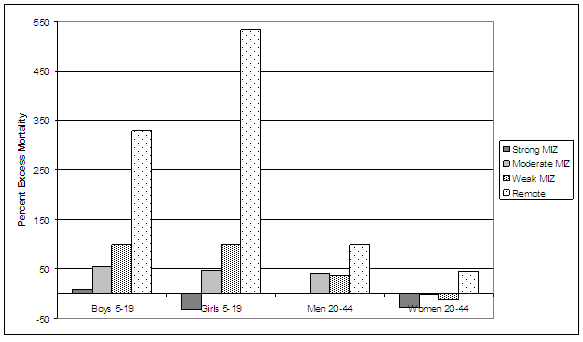
Figure 5: Excess rural suicide relative to urban mortality by age and gender. MIZ, metropolitan influenced zone.
As in the case of suicide mortality, excess rural compared with urban injury/poisoning deaths tend to increase with decreasing age. In remote places injury/poisoning deaths among boys aged 0-4 are 374% greater than they are for boys of the same age residing in urban places. Compared with the same age groups in urban places, excess deaths due to injury/poisoning for girls age 0-4, girls age 5-19 and boys age 5-19 in remote places were approximately 250% greater than in urban places (Fig6).
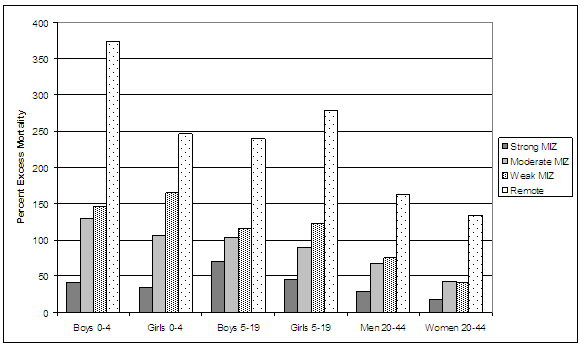
Figure 6: Excess rural injury/poisoning relative to urban mortality by age and gender. MIZ, metropolitan influenced zone.
Mortality from MVAs are higher in all rural compared with urban places. Unlike suicide and injury/poisoning mortality, for MVAs there is relatively little difference in the observed patterns of excess rural mortality among age groups. Excess MVA mortality in remote places is in the 175-225% range for all age groups. In weak MIZs, excess MVA mortality for girls age 0-4 is 275%, compared with being in the 125% range for boys and girls and men and women in other age groups (Fig7).
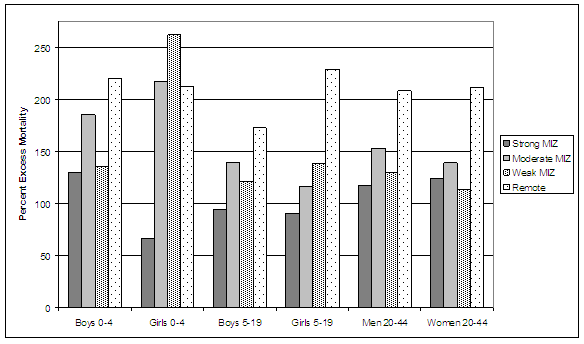
Figure 7: Excess rural motor vehicle accident mortality, relative to urban mortality by age and gender. MIZ, metropolitan influenced zone.
Discussion
Five main conclusions are drawn from this research. First, mortality tend to be worse moving from urban to remote regions, except in the case of strong MIZs where rates tend to be lower than they are in urban places and in other rural MIZs. Second, these differences in mortality along the urban-rural continuum are mainly driven by those under age 45 and particularly deaths caused by injury and poisoning, MVA and suicide. Third, the proportion of excess deaths relative to urban places for those under age 45 increases with decreasing age. Fourth, remote places have the highest excess in mortality for suicide, MVA, injury and poisoning, relative to urban places.
Fifth, although absolute mortality for all age groups and in all regions is higher for males than it is for females, the relative impact of place (in terms of proportion of excess deaths) in rural relative to urban Canada is remarkably consistent regarding gender for the 3 major causes of death for those under age 45. In other words, it doesn't matter much if one is male or female, the relative impact of living increasingly further away from Canadian cities is, in general, equally adverse.
Thus, while it is well known that riskier male behaviour may be behind much of the higher absolute mortality for males, this re-analysis shows that for both rural boys and girls, life outside Canadian cities is much more dangerous than it is for age counterparts resident in urban places. This observation has implications for policy. In particular, there is a need for prevention policies being targeted at both boys and girls for the prevention suicide, injury/poisoning, and MVAs. Such policies should be especially prominent in remote places where excess deaths, relative to urban places, are astoundingly high.
The original CIHI study4 showed that the differences in health status along the rural-urban continuum are small for those over age 45; therefore, the rural health disadvantage is largely a problem for children, youth, and young adults. Given that poverty among children and youth in Canada (in all regions) is very high relative to other industrial nations13, child and youth health must be a specifically articulated priority for health policy-makers in this country.
The results for suicide are alarming, particularly for boys and girls aged 15-19. Research from Australia, Norway, and the United Kingdom have found the largest increases in suicide rates for young adults since the 1970s have occurred among residents in rural regions4,14-16. The high suicide rates in rural Canada identified in this study may also reflect recent increases. It is well known that in Canada suicide rates among Aboriginal youth are higher than for non-Aboriginal youth17,18. Given the often high proportion of Aboriginal people living in remote regions of Canada this could explain, to some extent, the extremely high rates observed in these regions.
Conclusion
The relative mortality for young girls living in rural compared with urban places in Canada is similar to the relative mortality for young rural boys. There is, therefore, a need for prevention policies targeted at both boys and girls to prevent suicide, injury/poisoning, and MVAs in rural, and especially remote places.
Acknowledgements
The author is a Canada Research Chair and Senior Scholar with British Columbia's Michael Smith Foundation for Health Research. He acknowledges the contribution that these two organizations have made to this work.
References
1. Rioja L, Redondo R, Aboitiz R. Death in town and country: an analysis of urban-rural differences in mortality. Sociologia Ruralis 2007; 141(4): 454-474.
2. Ostry A. An exploration of the gap in health status between urban and rural Canadians. In: J Kulig, A Williams (Eds), Rural health: a Canadian perspective. Toronto: University of Toronto Press, 2010.
3. Lagace C, Mesmeules M, Pong R, Heng D. Non-communicable disease and injury-related mortality in rural and urban places of residence. Canadian Journal of Public Health 2007; 98(Supp1): 562-569.
4. Canadian Institute for Health Information. How healthy are rural Canadians? An assessment of their health status and health determinants. Ottawa: Canadian Institute for Health Information, 2006.
5. O'Reilly G, O'Reilly D, Rosato M, Connolly S. Urban and rural variations in morbidity and mortality in Northern Ireland. BMC Public Health 2007; 7: 123.
6. Pohar S, Majumdar S, Johnson J. Health care costs and mortality for Canadian urban and rural patients with diabetes: population-based trends from 1993-2001. Clinical Therapeutics 2007; 29: 1316-1324.
7. Boland M, Staines A, Fitzpatrick P, Scallan E. Urban-rural variation in mortality and hospital admission rates for unintentional injury in Ireland. Injury Prevention 2005; 11: 38-34.
8. Paulozzi L, Yongli X. Recent changes in drug poisoning mortality in the United States by urban-rural status and by drug type. Pharmacoepidemiology and Drug Safety 2008; 17: 997-1005.
9. Ostry A, Maggi S, Hershler R, Louise A, Chen L, Hertzman C. A case control study of differences in non-work injury and accidents among sawmill workers in rural compared to urban British Columbia, Canada. BMC Public Health 2009; 9: 432, 2009.
10. Mitura V, Bollman RD. The health of rural Canadians: a rural urban comparison of health indicators. Rural and Small Town Canada Analysis Bulletin 4: 6. (Online) 2003. Available: http://www.statcan.gc.ca/pub/21-006-x/21-006-x2003003-eng.pdf (Accessed 7 August 2009).
11. Mitura V, Bollman RD. Health status and behaviours of Canada's youth: A rural-urban comparison. Rural and Small Town Canada Analysis Bulletin 5: 3. (Online) 2004. Available: http://www.statcan.gc.ca/pub/21-006-x/21-006-x2003003-eng.pdf (Accessed 7 August 2009).
12. McNiven C, Puderer H, Janes D. Census metropolitan area and census agglomeration influenced zones (MIZ): a description of the methodology. Cat no. 92F0138MIE2000002. Ottawa: Statistics Canada, 2000.
13. Conference Board of Canada. How Canada performs: a report card on Canada. Ottawa: Conference Board of Canada, 2009.
14. Dudley M, Kelk N, Florio T, Waters B, Howard J, Taylor D. Coroners' records of rural and non-rural cases of youth suicide in New South Wales. Australian and New Zealand Journal of Psychiatry 1998; 32(2): 242-251.
15. Kelly S, Charlton J, Jenkins R. Suicide deaths in England and Wales, 1982-1992: The contribution of occupation and geography. Population Trends 1995; 80: 16-25.
16. Mehlum L, Hytten K, Gjertsen F. Epidemiological trends of youth suicide in Norway. Archives of Suicide Research 1999; 5(3): 193-205.
17. Chandler MJ, Lalonde CE. Cultural continuity as a protective factor against suicide in First Nations youth. Horizons 2008; 10(1): 68-72.
18. Lalonde CE. Identity formation and cultural resilience in aboriginal communities. In: RJ Flynn, P Dudding, J Barber (Eds), Promoting resilience in child welfare. Ottawa: University of Ottawa Press, 2006; 52-71.
Abstract
Introduction: The primary purpose of this article is to demonstrate the role that age, gender, and place play in rural-urban differences in mortality, in order to better develop policy to reduce these differences.
Methods: In 2006, the Canadian Institute for Health Research published a major epidemiological investigation into the morbidity and mortality experience of Canadians, using mortality data as well as the 2004 Canadian Community Health Survey. Using these data, gender differences in mortality across the rural-urban continuum were further explored. The proportion of excess deaths occurring in each of the four different types of rural places, relative to deaths in urban places, were calculated for different gender and age groups.
Results: Differences in mortality across the urban-rural continuum are mainly driven by people under 45 years, and are particularly due to deaths caused by injury and poisoning, motor vehicle accident (MVA) and suicide. The proportion of excess deaths relative to urban places for those under 45 years increases with decreasing age. Remote places have the highest excess in mortality for suicide, MVA, injury and poisoning, relative to urban places.
Conclusion: The relative mortality for young girls living in rural compared with urban places is similar to the relative mortality for young rural boys. There is, therefore, a need for prevention policies targeted at both boys and girls to prevent suicide, injury/poisoning, and MVAs in rural, and especially in remote, places.
Key words: Canada, gender, mortality.
You might also be interested in:
2013 - Dental education in the rural community: a Nigerian experience
