Dear Editor
Mycobacterium ulcerans disease, commonly called Buruli ulcer (BU), is a neglected and emergent tropical disease1. Buruli ulcer is endemic in the rural wetlands of the tropical countries/regions of Africa, The Americas, Asia, and Australia but is uncommon in non-African countries1. Infection with M. ulcerans often leads to extensive destruction of skin and soft tissue with the formation of large ulcers2. Ulcerative and non-ulcerative forms of the disease exist. The non-ulcerative lesions may be papules, nodules, plaques, edemas or osteomyelitis2. The disease often occurs in people who live or work close to rivers and stagnant bodies of water3. The disease is more severe in impoverished inhabitants of remote rural areas. Approximately 70% of those affected are children under the age of 15 years2. The characteristic skin ulcers have undermined edges and are usually painless.
A 24 day-old female newborn from the village of Nkamuna (an endemic area for BU in Songololo Territory, Bas-Congo Province, Democratic Republic of Congo), presented on 28 May 2007 to the Nkamuna Medical Centre with an extensive ulcerated lesion on her abdomen and back with satellite ulcers (Fig1). Typical of BU, edema had appeared on her back 2 weeks prior to presentation. The edematous area deteriorated and an ulcer with undermined edges formed, also typically observed in BU. The patient presented no symptoms of a bacterial infection (fever, enlarged lymph nodes etc). An initial diagnosis of BU was based on the clinical and epidemiological findings.
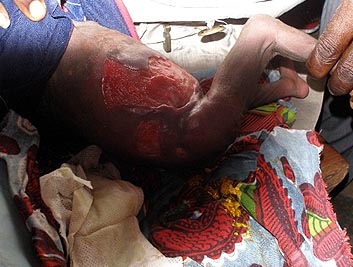
Figure 1: The large cutaneous ulcer resembling a Buruli ulcer found in the 24 day-old newborn.
Tissue specimens were submitted to the mycobacteriology laboratory of the Institute of Tropical Medicine, Antwerp, Belgium. Smear, culture and PCR tests for M. ulcerans were negative. Histopathologic analysis of formalin-fixed tissue performed at the Armed Forces Institute of Pathology, Washington, USA, revealed acute and chronic inflammation with small areas of necrosis and gram-positive cocci. Histopathological examination concluded that the specimen could represent an old BU infection suprainfected with gram-positive cocci. Neither culture nor drug sensitivity testing was performed. HIV infection was excluded following negative results from the rapid tests Determine HIV-1/2 (Abbott; Tokyo, Japan), Uni-Gold (Biotech; Bray, Ireland) and Genie II HIV-1/HIV-2 (Bio-Rad; Marnes-la-Coquette, France).
The combination rifampicin-streptomycin recommended by WHO for BU treatment4 was not prescribed because streptomycin was contraindicated in this 24 day-old newborn. Surgery (large excision) under general anesthesia and medical transfer to the nearest provincial hospital were not possible due to logistical constraints. Consequently, the patient was treated with oral ampicillin. The dressings were changed daily with an aqueous solution of chloramines-metronidazole-nitrofurandoïne5. Unfortunately, the patient died 2 weeks later.
In a rural zone, the following ulcerative lesions may be confused with BU: necrotizing fasciitis, phagedenic ulcer, ulcer of vascular origin, ulcerative cutaneous tuberculosis, African histoplasmosis, ulcerated carcinoma. Histopathologic examination clarifies differential diagnosis and allows diagnosis of the ulcer.
Buruli ulcer is rare to unknown in newborns. This case illustrates the difficulties physicians encounter in rural areas in making a diagnosis of BU and choosing treatment on the basis of history and physical examination. Added to this, in our case, a precise diagnosis was not possible even after medical investigations. This case report demonstrates that in a rural area the clinical diagnosis of large ulcers, including differential diagnosis, may be more difficult than is usually reported.
Kapay Kibadi, MD
Department of Surgery, Faculty of Medicine,
University of Kinshasa, Democratic Republic of Congo
Acknowledgements
The author thanks Professor Francoise Portaels (Institute of Tropical Medicine, Antwerp, Belgium) and Professor Wayne M Meyers (Armed Forces Institute of Pathology, Washington, USA) for microbiologic and histopathologic analysis. Also thanked are Kayinua (General Hospital of Nsona-Mpangu, RDC) and Belly (MC of Nkamuna, RDC) for their cooperation and participation in the study.
References
1. World Health Organization. Buruli ulcer: progress report, 2004-2008. Weekly Epidemiological Record 2008; 17: 145-156.
2. Portaels F, Silva MT, Meyers WM. Buruli ulcer. Clinics in Dermatology 2009; 27: 291-305.
3. Kibadi K, Panda M, Muyembe-Tamfum JJ, Fraga GA, Filho AL, Anyo G et al. New foci of Buruli ulcer, Angola and Democratic Republic of Congo. Emerging Infectious Diseases 2008; 14: 1790-1792.
4. World Health Organization. Provisional guidance on the role of specific antibiotics in the management of Mycobacterium ulcerans disease (Buruli ulcer). WHO/CDS/CPE/GBUI/2004.10. Geneva: WHO, 2004.
5. Kibadi K. Ulcère à Mycobacterium ulcerans: prise en charge chirurgicale dans 102 observations en République Démocratique du Congo. Médecine Tropicale 2005; 65: 444-448. (In French)
