Introduction
A large of amount of literature exists on the factors that influence the recruitment and retention of rural GPs in Australia and other countries ranging from: professional factors such as rural exposure during training and backup1-5, personal and family factors such as rural background and spouse preferences6, community factors such as climate and recreational and cultural opportunities2,6 and economic factors such as income and practice costs7,5.
However, much of the work undertaken in this area has not yet been updated to reflect the attitudes and preferences of the new generation of potential rural GPs. It is already acknowledged that the Generation X (born between 1962 and 1977) and Generation Y (born between 1978 and 1994) doctors have different perceptions of workload, lifestyle and the support required to practise, as well as different defining values and attitudes8-11. They have different expectations on what is expected of a medical practitioner and place greater importance of balancing career and personal life11. For rural practice, the Generation X and Y GPs are likely to be more selective in the type and location of the practice they join in order to achieve a feasible work-life balance.
The aim of this study was to explore, from a Generation X perspective, the factors deemed important by general practice graduates in selecting a rural practice at the completion of their training. The study also aimed to identify the process general practice graduates use to identify a potential rural practice.
Methods
Fifteen out of a potential of 41 rural pathway GP registrars in their final year of training in 2006 were recruited for the study from 2 South Australian regional training providers (RTPs): the Adelaide to Outback General Practice Training Program and Sturt Fleurieu General Practice Education and Training. Recruitment was by a letter of invitation disseminated by the 2 training providers. Participants received a small honorarium for their time.
Participants were interviewed using a semi-structured interview schedule (Table 1). Topics in the interview schedule included: their ideal rural practice and community, source of information on potential practices, and when they commenced looking. The interviews were digitally recorded and transcribed. Ethical approval was gained from the University of Adelaide Human Research Ethics Committee and all data remained confidential.
Table 1: The semi-structured interview schedule used in the study

Interview bias was reduced by recruiting an interviewer from a different discipline with no previous knowledge of the research area. Drawing the many factors identified back to the experience of participants improved external validity.
Thematic analysis was conducted on all transcripts and key ideas were coded and grouped into keywords, categories, sub-themes and, finally, themes. This phenomenological hermeneutic thematic analysis was guided by the ideas of Max van Manen12. The thematic analysis followed 4 phases. Phase 1 involved combing through each interview for key words and concepts. Key concepts were coloured in different font colour and code words placed next to these. Phase 2 involved collating the separate interviews and joining all the highlighted quotes and phrases together into categories, key words, and concepts, leading up to sub-themes. These key words and concepts were further developed in discussions between the 2 authors (CL and VW) who independently conducted their own reading of the data and discussed the analysis with the intention of creating a solid inter-rater reliability. An example of this phase of the analysis is included (Table 2). Phase 3 analysis involved choosing key quotes, which were considered to be the best examples of each idea put forward by the participants. From these, sub-themes were developed. Phase 4 analysis involved the breaking up of one document with collated data into 4 tables of grouped sub-themes.
A fifth phase was the final stage of the qualitative analysis. The 4 sub-themes were collated into the 2 final themes, and these 2 themes and 4 sub-themes will be described fully in the results section below.
Table 2: Example of phase 2 analysis used in the study

Results
Participant characteristics
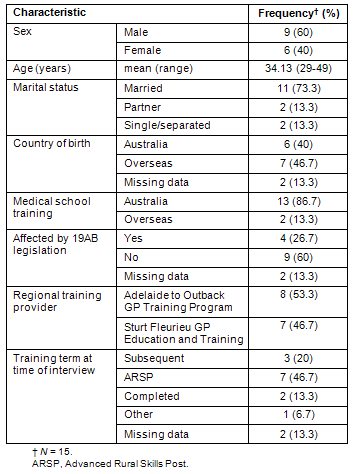
The characteristics of the participants in the study are summarised (Table 3). The mean age of participants was 34 years. The majority of participants classified Generation X were male (60%) and either married or with a partner (87%). Most of the participants (47%) at the time of the interview were undertaking an Advanced Rural Skills Post (ARSP: GP registrars with an interest in rural general practice can apply to do an additional year of GP training. Training posts in Advanced Rural Skills offer intensive training in procedural skills and other disciplines which have a particular relevance for GPs working in a rural and remote setting).
Table 3: Summary of participant characteristics
Key themes
The key results of the qualitative analysis were broken into 2 major themes:
- The Ideal Rural General Practice, which contains 2 sub-themes: The Practice and The Community.
- Word of Mouth, which contains 2 sub-themes: Advice and Source of Knowledge.
Concepts related to these themes and sub-themes are shown (Table 4).
Table 4: Key themes, sub themes and concepts identified in the analysis

Theme one: the ideal rural general practice: This theme consisted of 2 sub-themes, The Practice (related to a wish list for an ideal practice to work in) and The Community (related to a wish list for the most desirable community to live in). The Practice was by far the largest sub-theme with the greatest amount of detail provided by participants.
The Practice The registrars interviewed described the ideal rural practice as one giving scope for skills development and maintenance. It was a priority for them, as one stressed:
It's important that [a practice] offers me opportunities to do anaesthetics because that's crucial... I did the training and I'd just like to upkeep those skills, so obstetrics and obstetric anaesthesia...I don't want to work in a place where I won't get an opportunity to do anaesthetics. (Dr P2: lines 191-200)
Others saw rural practice as an ideal opportunity to expand their skills:
One of the reasons why I've chosen rural practice is because of the training opportunities in the GP training itself, in that if I'm doing rural practice rather than urban practice, the support that I get in doing courses and expanding my skills is paramount, it's got an amazing level of support. That's a really important factor in me choosing it. (Dr P15: 580-6)
As almost half the participants were still training, and helpful supervision, solid back up from fellow doctors and knowledgeable allied health personnel were also deemed important. They especially valued:
...good relationships with specialists that visit...you could phone for advice at any time and they'd be very happy and willing to ring you back and give you any advice over the phone and see people at short notice. (Dr P11: 285-90)
An appropriate number of doctors in a practice, somewhere from four to 10, was also considered a way to facilitate good support. Practice size also related to on-call and after hours work. One participant believed the correct number of doctors in a practice was four, adding that 'more than that and it gets a bit too much; less than that and the on-call and other things become a bit onerous.' (Dr P6: 152-3). Another participant needed a larger group of:
...around 10 partners... as you get bigger you get a little bit less control - a little bit less friendly and as you get smaller you get more friendly and it's a much tighter team but you've got twice as much on-call.' (Dr P11: 238-40).
While registrars accepted on-call work was part of rural practice, they wanted this to be reasonable and believed a larger practice would offer this.
The business side of an ideal practice was also important. The registrars valued a capable practice manager who ensured an efficiently run business, particularly as it would allow them to focus on medicine. As one registrar stated:
A practice manager who has skills in business development, that would be more ideal for me: to know that it's happening, but to not have the responsibility to make it happen. (Dr P3: 278-9)
Emphasis on skilled staff also included nursing staff and they particularly emphasised the importance of practice nurses and valued 'the team approach' (Dr P11: 201-12).
Registrars also sought a welcoming and positive working atmosphere in the practice structure with their fellow doctors and clients, and a sense of community with their colleagues. One registrar remarked that the friendliness of their fellow staff members was essential:
... Because it is a business and the patients are clients and they don't have to see you. It's their choice to see you but if your staff are friendly... efficient, booking the patients well and greeting them nicely when they come...if you've got really grumpy staff or people who don't answer the phone, you might be missing clients and people might leave you because they don't like the atmosphere.(Dr P5: 372-8)
Ethical practice was important for these future rural GPs. They were passionate about medicine and saw it as a vocation and therefore it was important that the rural practice met these needs. One registrar said she:
...would not work for an organisation that was like a chain, like a supermarket sort of system that we're starting to see arise in some of the more urban areas where you have a chain of medical practices and people are employed. (Dr P7: 264-6)
This attitude transferred into the style of practice they sought. They had no desire to be part of a practice emphasising income which did not allow them to provide the best possible care for their patients. Whether this was appointment scheduling or the choice to bulk-bill patients, the type of practice they refused to join was described as:
... [where you] see a patient every 10 minutes. GPs never really speak to each other because they just rush in and see their patients...no social interaction...no Friday night drinks, there's no lunches together.(Dr P3: 363-67)
Well equipped work spaces, access to related services and electronic medical records mattered to these registrars. Solid back-up with a hospital close by was also essential:
...my ideal situation would be a medical practice co-located with a 5- to 10-bed acute hospital with a casualty department with, say, a 20- or 30-bed nursing home and a 20- to 30-bed hostel place run by doctors with minimum of top-heavy management with ready access to specialists in general medicine, general surgery, obstetrics and paediatrics, and a major teaching hospital within about 45 minutes. (Dr P6: 147-51)
The Community This second sub-theme involved the ideal rural community. The registrars interviewed said this ideal community involved characteristics such as a sense of community in the township, being a place where they could belong, one that felt like a home to them. Some registrars felt comfortable in larger regional centres, others needed a small town, some needed quieter towns, others were drawn to more vibrant areas, but all sought a place where they were included and felt welcome:
I like working in rural areas rather than urban areas, and that's just because I like the sense of community. I like knowing where people work and... a sense of placement within a community, I look for that. (Dr P 15: 183-6)
It's...the feel of the town itself too when you drive into it. It's a different feeling...It's a very subjective thing - the surrounds - it's the friendliness of even the people just walking down the street and when you go into the shop to buy a drink and that sort of thing... I suppose it's the welcoming or the warmth of the town. (Dr P5: 456-61)
Registrars sought communities with a lively tourism aspect and some social life. They also wanted amenities such as a gym, a restaurant and shops. Experiencing the town as a place where they were treated with respect, were safe and had access to good facilities for both themselves and their families was also important to the registrars interviewed. One registrar with young children sought:
...somewhere nice to bring up a family...I don't want to be in a desert...I don't want to be in a place that's not suitable for bringing up a small child really, a place where it's polluted and where there's crime.(Dr P13: 288-90)
Many of the registrars' concerns related to family issues, such as jobs for their partners and quality schooling and childcare. One registrar explained that what he wanted was:
...a good school, for my children and also that my wife can get a job. Otherwise they get depressed with each other and then I'm the one in trouble! (Dr P1: 276)
For some, closeness to extended family was important. One registrar explained, ' If I ruled any practice out it would be based on the fact that it was too far away from our family (Dr P7: 371-2).
The physical landscape also mattered when selecting a location, not only in visual appeal, but also in terms of opportunities to participate in activities such as surfing or bushwalking. One registrar described the influence of the physical landscape on his decision:
I was actually attracted by the fact that it was green and...there were hills and that's the agricultural part of me...the land was the influence rather than the population or the people. It is surprising because I thought I would probably end up more remote...but there's certain influencing factors along the way that it's just how I've ended up in 'Latte rural' as I call it rather than 'remote rural. (Dr P11: 451-8)
Registrars also discussed the environment in terms of opportunities to participate in other activities outside medicine, such as hobbies or recreational activities.
Theme two: word of mouth: 'Word of mouth' described the information shared between registrars when identifying potential rural practices. This theme contained 2 sub-themes: Advice and Source of Information.
Advice In this sub-theme the registrars considered the advice they would give a GP about to follow in their footsteps and take a rural path. They valued reasonable pay but balanced this against a positive lifestyle. Money talks, was their message, but not always - and not in every way. One doctor put it simply: '...if I like a place, I'm willing to compromise less pay for better quality of life, I guess, and better work environment' . (Dr P2: 178-9).
They stressed that it was important to study and explore a work place ahead of time. They gave such advice as visiting a clinic of interest first, working there for a while, getting to know the people, and learning of any practical limitations. One suggested that an early visit examining a contract was a good idea:
Go and see the clinic for yourself before you actually make any commitments and get all the terms laid out in front of you...know what you can expect and maybe not get disappointed...you don't want to make a rash decision just going to one place and signing up and finding later down the track that that's not what you want. (Dr P13: 387-92)
The experience of working in a potential practice was used by several registrars to identify potential practice locations, and this was either through training or locum work. As one registrar suggested:
Do the rural locum stuff, where you do two weeks at a time in a different place...that would be a fantastic job for a registrar for six months and have a look at half-a-dozen; a dozen different practices and you'd just gain so much in how different practices work [then] you can find your own practice and take all these different little bits and pieces with you. (Dr P7: 439-44)
Source of Knowledge This second sub-theme covered the source of knowledge for rural doctors about locating ethical practices and congenial workplaces. Most of this knowledge came by word of mouth, especially from GP friends and colleagues. As one registrar remarked:
Word of mouth is a source [of knowledge]...friends... who have worked in the area give me some background... [I] get the information about a workplace and I'd prefer it from a colleague or someone who did the same job [as me] to give me the information... (Dr P2: 74 -90)
The rural GP grapevine was also useful ' ....you do share a lot... hear good and bad things of what's been happening...' (Dr P10: 470). The registrars occasionally looked for information in appropriate medical journals, the newspapers, or websites but these were less important than word of mouth.
Timing of decision
The majority of registrars reported that they commenced the process of finding a practice in the last 6 months of their training, after they had undertaken the fellowship exam. A couple of the registrars had made their decision much earlier and had been influenced by programs such as the John Flynn Scholarship Scheme or other work experiences.
Discussion
This study focused on exploring the type of rural practice and factors deemed important by a group of registrars about to enter rural practice on the completion of their training. This Generation X group of registrars were looking for practices with the following characteristics:
- a medium size practice, with 4-6 GPs, allowing for sufficient time off and less on-call work
- a well-structured practice with an experienced practice manager
- potential to practise and maintain current skills, particularly procedural skills
- a well-equipped practice, with access to practice nurses and a local hospital
- an ethical practice that allowed autonomy in patient management
- a team environment
- a supportive professional environment.
Like the previous generation, this group of participants placed importance on tangible factors such as professional support and back up1,13, access to continuing education1,13, and the availability of support facilities14. However, what these registrars also emphasised was the importance of a team environment, access to nursing staff and the ability to practise as they choose. Intangible factors, such as the ethics of a practice and practice culture, were also important in choosing a rural practice.
This study, like that of Riley et al's6 USA study, found that the opportunity to practise skills developed during training was important to the graduates and played a key role in the selection of a practice. After hours and on-call arrangements were also of concern. While they understood the requirement of after hours and on call work in rural general practice, they also sought practices allowing reasonable hours, which tended to be larger group practices.
An agreeable relationship between colleagues and a pleasant work atmosphere was also inportant. Good role models with ethical practices mattered and were important in their practice choices.
For these participants, financial considerations were not the major factor in the selection of a practice; lifestyle and a positive work environment were more important. This is interesting in the light of the number of financially based strategies to attract and retain rural GPs in Australia15 and other countries16. It suggests that when commencing in rural practice financial considerations are not a major issue for registrars, and that these may be less important in the recruitment of rural GPs.
Community factors, as with the previous generation of rural GPs1,2, were important in selecting the location of a practice for this group of registrars. This included the both tangible and intangible factor such as physical environment, culture and the 'feel of the town'. The term used by one of the participants sums up their desired type of rural community: latte rural, which offers a lifestyle with possible hobbies such as farming, fishing, bushwalking or water sports. The results are similar to studies tracking health students in the Australian states of New South Wales, Western Australia and Victoria17-19. These studies found that the attractiveness of the rural town and size of community were important influences on location choice.
Family factors are known to influence the recruitment and retention of rural GPs2. This study identified issues of schooling and work opportunities for the spouse as another influence on practice selection.
Distance to metropolitan areas were not emphasised by this group and could be foregone, although some participants wanted locations closer to metropolitan areas to maintain links with their extended families, particularly if they planned to have children.
Finding a rural practice
In selecting a practice, participants identified a number of sources of information on a potential practice. The most important sources of information came by word of mouth, referrals by colleagues and contact made through their training. As has been found in other research6, this study emphasised the importance of referrals by colleagues, an informal but vital part of a registrar's selection of a place of work in a rural area.
This study also highlighted the role of exposure to practices during training in determining what type of practices registrars seek after completing training. It also suggests that the marketing of future practice locations should commence in the last year of registrar training because this is when they begin the selection process.
Limitations of the study
Several limitations were identified in this research. First, this small sample of GP registrars was restricted to those from 2 RTPs in South Australia. However, this study used qualitative methodology in order to explore in-depth the factors GP registrars deemed important and data saturation was reached.
Second, being a South Australian (SA) based study, the views may not be generalisable to other states and territories. However, the goal was to inform the development of policy for the Rural Doctors Workforce Agency, an SA based organisation and, therefore, focusing on SA registrars was appropriate.
The higher number of male participants (60%) may have influenced the responses given. However, the rural registrars training pathway has a majority (62%) of male registrars nationally.
Conclusion
This group of Generation X rural registrars identified tangible and intangible factors important to them in selecting a rural practice. Many of these factors were similar to those identified by the previous generations, such as professional support, reasonable on-call work, access to hospital and the ability to use the skills they had gained during training. However, they also identified factors such as a team environment, and positive and ethical practice as influential.
The results provide an insight into the type of practice and rural community where a Generation X group of doctors want to work and live. They also illustrate the importance of lifestyle in selecting a rural practice or community. This has implications for the future rural medical workforce and also provides evidence that can be used to target future policy initiatives.
Acknowledgements
This study was funded by the Rural Doctors Workforce Agency Inc in South Australia. The authors acknowledge and thank the GP registrars who participated, Sarah Dugdale for undertaking the interviews and Beth Nixon for transcribing them.
References
1. Hays R, Veitch C, Cheers B, Crossland L. Why doctors leave rural practice. Australian Journal of Rural Health 1997; 5: 198-203.
2. Humphreys J, Jones J, Jones M, Hugo G, Bamford E, Taylor D. A critical review of rural medical workforce retention in Australia. Australian Health Review 2001; 24(4): 91-102.
3. Brooks R, Mardon R, Lewis M, Clawson A. The roles of nature and nurture in the recruitment and retention of primary care physicians in rural areas: a review of the literature. Academic Medicine 2002; 77(8): 790-798.
4. Ozolins I, Greenwood G, Beilby J. Keeping women doctors in the country. Rural and Remote Health 4: 268. (Online) 2004. Available: www.rrh.org.au (Accessed 7 May 2004).
5. Godsen T, Bowler I, Sutton M. How do general practitioners choose their practice: preferences for practice and job characteristics. Journal of Health Services, Research and Policy 2000; 5(4): 208-213.
6. Riley K, Myers W, Schneeweiss R. Recruiting physicians to rural practice: suggestions for success. Western Journal of Medicine 1991; 155: 500-504.
7. Pope A, Grams G, Whiteside C, Kazanjian A. Retention of rural physicians: tipping the decision-making scales. Canadian Journal of Rural Medicine 1998; 3(4): 209-216.
8. Eley D, Young L, Shrapnel M, Wilkinson D, Baker P, Hegney D. Medical students and rural general practitioners: congruent views on the reality of recruitment into rural medicine. Australian Journal of Rural Health 2007; 15: 12-20.
9. Laurence C, Elliott T. The when, what and how South Australian pre-registration junior medical officers' career choices are made. Medical Education 2007; 41(5): 467-75.
10. Schofield D, Page S, Lyle D, Walker T. Ageing of the baby boomer generation: how demographic change will impact on city and rural GP and nursing workforce. Rural and Remote Health 4: 604. (Online) 2004. Available: www.rrh.org.au (Accessed 24 October 2006).
11. Gavel P, Evans J, Young J. Who are the doctors of tomorrow? - some Australian perspective and thoughts. In: Proceedings, 9th International Medical Workforce Conference; 15-19 November 2005; Melbourne, Australia; 2005.
12. Van Manen M. Researching lived experience. New York: SUNY, 1990.
13. Hoyal F. Retention of rural doctors. Australian Journal of Rural Health 1995; 3: 2-9.
14. Strasser R. How can we attract more doctors to the country. Australian Journal of Rural Health 1992; 1(1): 39-44.
15. Lennon B. Programs and policies to redistribute physicians to high need areas - Australia. In: Proceedings, 8th International Medical Workforce Collaborative; 6-9 October 2004; Washington, DC, USA; 2004.
16. Council on Graduate Medical Education. Tenth report: physician distribution and health care challenges in rural and inner-city areas. Washington, DC: US Department of Health and Human Services, Public Health Service, Health Resources and Services Administration, 1998.
17. Larson A, Playford D, Wheatland B. Whither rural health students? Methodology and preliminary analysis of the student tracking project, Western Australia. Geraldton, WA: Combined Universities Centre for Rural Health, 2004.
18. Schofield D, Fletcher S, Fuller J, Birden H, Page S. Where do students in the health professions want to work? Human Resources for Health 2009; 7: 74.
19. Schoo A, McNamara K, Stagnitti K. Clinical placement and rurality of rural career commencement: a pilot study. Rural and Remote Health 8: 964. (Online) 2008. Available: www.rrh.org.au (Accessed 19 April 2010).



