Context
Nigeria is a West African country with a 2008 population of approximately 140 million. Despite substantial petroleum resources, at least 70% of Nigerians subsist on less than $US1.25 per day, and have a life expectancy at birth of 46 years. Approximately 52% of Nigerians live in rural areas1. Gross domestic product (GDP) per capita in 2007 was estimated at $US1118. As at 2005, health expenditure per capita in Nigeria was $US31, and health expenditure as percentage of GDP declined from 5% in 2002 to 3.9% in 20052,3. Nigeria's national health indices and human development index (2009 HDI rank: 158) are disproportionately poorer than health funding shortfalls would suggest, indicating a systemic failure of health policy. For example, in 2007 Nigeria's senior public sector physicians and nurses earned, on average, $US1800 and $US500 per month, respectively, significantly above the average salaries of these health professionals in Africa and Asia4. However, compared with developing countries such as the Philippines (2009 HDI rank: 105) and Indonesia (2009 HDI rank: 111), which pay lower salaries to health workers and also experienced recent declines in government health expenditure3, Nigeria's life expectancy at birth is at least 15 years lower5. Paralleling the situation in most African nations, Nigeria's health sector is chronically understaffed at all levels (Table 1)1,6.
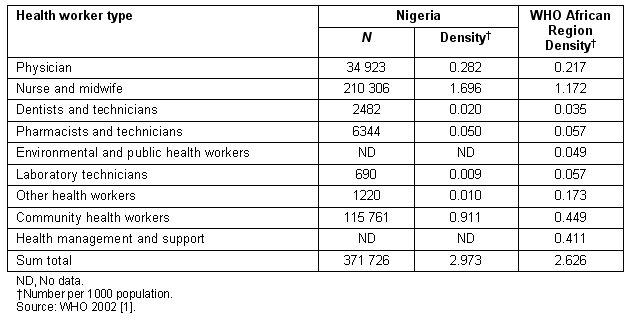
Table 1: Number and density of health workers in Nigeria, compared with 2002 WHO African region statistics
Issues
A recent modelling study asserted that numerical inadequacy of health workers has become 'the binding constraint in implementing many priority health programs in Africa'7. The proportion of households within 10 km of a health centre, clinic or hospital is 50% higher in urban regions, compared with rural areas8. Morbidity and preventable mortality trends worsen in direct correlation with ease of access to health services. For example, although Nigeria's overall maternal mortality is, at 1100 per 100 000 live births, among the highest in the world9, and within-country analyses indicate that maternal mortality is significantly higher in the largely rural regions of Nigeria10,11. Such findings are in accord with global findings that demonstrate 'rural residence' is a strong risk factor for increased maternal mortality12. Similar inequalities in health trends that disadvantage rural residents have been documented for infant mortality13. This article discusses factors hindering efficient health workforce development in Nigeria's rural and remote regions, and suggests feasible solutions.
Obstacles to recruitment and retention
One factor unlikely to be hindering Nigeria's efforts to recruit and retain health workers in rural and remote areas is the out-migration of doctors and nurses. This is because almost all migrating Nigerian doctors and nurses come from urban areas and so are unlikely to work in rural areas, even if their migration efforts were unsuccessful14,15. More important encumbrances are now discussed.
Spartan living standards in rural and remote areas: Open defecation, severely limited access to electricity, primitive social amenities, chronic poverty, poor quality educational or communication facilities, fragile health systems and the inadequacy of potable water (Fig1) characterise the rural regions of Nigeria16-18. Such adverse living conditions create formidable lifestyle challenges for skilled health personnel and their families.

Figure 1: Rural women and children near a neighbourhood well in Katsina State, northern Nigeria.
Inadequate numbers of trained health staff and limited employment capacity in the public sector: The numbers of all cadres of health staff in Nigeria need to be at least doubled in order to provide enough health workers to address the nation's current health needs6. Although some progress is being made in expanding the Indigenous training of Nigerian health workers19, frequent industrial action in the tertiary education sector and limited employment opportunities due largely to public sector budgetary constraints have practically neutralised Nigeria's training expansion initiatives. Few effective incentives currently exist to encourage educationally disadvantaged rural-based Nigerians to undergo training in the health professions, despite credible evidence that healthcare trainees from rural backgrounds are significantly more likely to work in rural areas after graduation20,21.
Inadequate remuneration: Inflation and the progressive devaluation of Nigeria's currency over the past 2 decades have made public sector salaries and allowances for health workers other than physicians increasingly inadequate for comfortable living. There are greater opportunities for income supplementation in urban rather than rural areas. Approximately 60% of Nigeria's states provide financial incentives to entice workers to relocate to rural areas19. Ironically, although states such as Taraba and Jigawa are severely deficient in Indigenous health workers and rural social infrastructure, their governments do not usually give non-Indigenous staff pensionable appointments, making it unattractive for needed non-Indigenous health workers to relocate19.
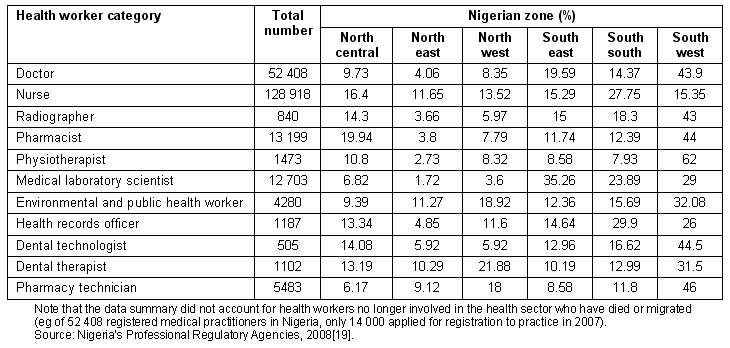
Sub-optimal mix and distribution of healthcare workers: The density of all registered cadres of health workers (Table 1) falls short of international recommendations for minimum ratios of health workers per 1000 population6,22. The distribution of Nigeria's health workers favours urban regions such as the South-West Zone, compared with the arid North-East Zone (Table 2). Although modest progress has been made in training community health officers, enrolments for such training must be significantly expanded. This is especially so for trainees drawn from rural regions where their skills are more appropriate to the communities' health needs23. In resource-poor countries such as Tanzania, staff trained for less technically demanding healthcare positions are less difficult to recruit and retain in rural and remote regions.
Table 2: Distribution of health workers in Nigeria by zone, 2007
Burnout of staff: Due to the enormity of unmet health needs, many dedicated staff working in Nigerian rural and remote areas are at risk of being overwhelmed by excessive workload24. It is not unusual for Nigerian rural general hospital doctors' daily outpatient clinic lists to contain over 100 patients. Such excessive workload, coupled with relatively poor remuneration, inadequate clinical facilities and limited opportunities for professional development, hinder efforts to recruit and retain skilled health staff in rural and remote areas.
Lessons learned
Proposals for improving recruitment and retention
Improve health governance: Although Nigeria has more health workers than most African countries, Nigeria's health indicators compare poorly with countries with a smaller health workforce, such as Eritrea, Mozambique, Tanzania and Uganda. One of the major shortcomings of Nigeria's health sector is inadequate health governance25. In Uganda, for example, nationwide health district performance is currently ranked and published. This represents an attempt at transparency regarding health worker performance after years of issues with public sector health workers which adversely the public health system26. Few benchmarks currently exist to monitor and compare the performance of Nigeria's public sector health workers.
Develop rural and remote health workforce recruitment and retention strategy: Despite acknowledgment of a severe shortage of healthcare workers in rural and remote areas27, Nigeria currently has no comprehensive rural and remote health workforce improvement strategy. Strategy 4.2 of the National Human Resources for Health Strategic Plan 2008-2012 (NHRFHSP) provides a perfunctory, non-evidence-based approach to addressing a complex health management problem. A useful strategic framework should provide a detailed situational analysis of the health systems and health needs in rural and remote areas, living conditions, funding gaps and sources, private and public sector healthcare providers and the mix of health worker requirements to meet identified needs28.
Fund incentives to motivate the retention of rural health workers: Rural and remote communities require basic facilities, such as electricity, sewerage systems and potable water supplies (Fig1), primarily for residents' wellbeing but also for making communities habitable for and attractive to urban-origin staff. For the individual health worker, additional financial remuneration might be impractical in the context of public service guidelines ocncerning pay scales. Rural non-governmental health organizations' payment to staff of a 'welfare package' (for relocation, housing, transport and meal subsidies) has motivated staff to work in the Nigerian rural private sector, as well as in the rural health sector of several other African countries29. Non-monetary incentives such as recognition, facilitating safe working environments, and creating professional development opportunities are equally important30.
Consider low-cost overseas recruitment: It is difficult to recruit and retain health workers in rural and remote areas, even in advanced countries like Australia. In Ghana, 65% of doctors and 40% of nurses work in Greater Accra and Kumasi, although about 33% of Ghana's population live in these cities. As a result, the Ghanaian Government recruited 184 Cuban doctors to work in underserved rural areas from 2006. This strategy has also be used in South Africa in recent years14. Less expensive sources of overseas recruitment include long-term bilateral agreements with international non-governmental health agencies such as Medecins Sans Frontieres (MSF). One untapped source of overseas health workers is the substantial population of Nigerians working overseas. According to Government records, in 2003, 29% of Nigeria's 35 000 registered doctors, and 20% of 10 364 registered pharmacists had either emigrated or were working in other professions. At least 16 300 nurses emigrated from Nigeria between 2004 and 200719.
It is probable that many Nigerian-born overseas-based health workers would return to work for short periods in underserved regions of Nigeria if a scheme was developed to facilitate volunteer activities. For example, in the USA, 35 000 practitioners and 10 000 students are members of the American Association of Physicians of Indian Origin, which provides volunteers for health service provision in India14.
Strengthen rural and remote health impact of National Youth Service Corps Program: The primary objective of Nigeria's National Youth Service Corps (NYSC) Scheme31 is to achieve national unity through the mobilization of new graduates to areas of need in Nigeria that are outside the graduate's cultural origin. This program guarantees a regular supply of low-cost, newly trained doctors, pharmacists and university trained nurses who may be compelled to work in rural and remote regions of Nigeria for 12 months. This represents a predictable and substantial source of skilled Indigenous health workers for rural and remote health workforce planers. Recently, nursing and midwifery graduates have become eligible for participation in the NYSC Scheme, and both groups are highly sought rural health workers. Incentives (such as free high-quality accommodation, transport allowances, and relocation and on-call allowances) for rural-based NYSC staff would facilitate optimum performance and also encourage continuation in rural and remote employment after compulsory national service32.
Improve strategic training of health workers more suited to rural and remote regions: In view of universal trends that indicate highly trained Nigerian health workers are unlikely to improve healthcare provision in rural areas on a long-term basis, it makes sense to adequately fund the nations' 13 schools for training community health officers and 43 schools for training community health extension workers. This may facilitate the availability of high quality community health officers, community health assistants and laboratory technicians for positions in rural and remote health services.
A comparison of the curriculum of Nigeria's Community Health Officer training program with that of Tanzania's Assistant Medical Officer's program indicates that Nigeria's program curriculum is inferior in scope and depth. For example, the Tanzanian training entails theoretical and practical lessons in internal medicine, pediatrics and child health, surgery, obstetrics and gynecology at a substantially higher standard than those in the Nigerian community health officers' curriculum19,33-36.
Improve management training cadre: Health management and leadership in Nigeria currently operates by default, rather than by design. In most health organizations senior clinicians are usually 'promoted' to senior management positions, irrespective of their management training. Not only do such practices deprive Nigeria's health system of experienced clinicians, but effective health leadership is also compromised if such senior doctors, nurses and midwives have yet to develop effective leadership skills37. No well-regarded Nigerian university currently offers training courses in health services management, and master of public health training courses in leading Nigerian universities are restricted to medical graduates only. Such a parochial approach to public health training deprives the sector of the necessary mix of skills required in the interdisciplinary field of health management38.
Link recruitment and retention to performance: Successful recruitment and retention process are vital for improving the performance of health systems in rural and remote regions of Nigeria. Performance measurement focuses on healthcare delivery outputs and outcomes from at least 4 dimensions: (i) availability (distribution and attendance); (ii) competence (technical knowledge, skills and behaviour); (iii) responsiveness (courtesy and positive client orientation); and (iv) productivity (ability to provide maximally effective services and outcomes with minimum possible input). Fritzen found that, in developing countries, high-performing health systems exhibited the following features33:
- a strong sense of mission and sense of commitment to organizational mission by staff
- a relatively high level of prestige and social status accorded to those who work in the organization
- culture oriented towards results both individually and organizationally
- the organization constantly evaluates its performance against external objectives and benchmarks
- lines of feedback from the end-users of services are open and actively used to improve service delivery.
Most of these characteristics are currently missing from Nigeria's rural and remote health service organizations.
Cultivate a culture of operational research: Rural health systems research receives inadequate attention in Nigeria. The culture of 'more of the same' needs to be replaced with one that supports a rapid and yet comprehensive assessment of key health system functions, and utilizes this knowledge to improve the quality and coverage of health services39. Nigeria's budgetary allocation for operational research on important public health problems (such as tuberculosis and malaria) are usually 'diverted' to other uses (including embezzlement), leading to stunted opportunities for innovation and improved health service delivery, particularly in rural regions.
Facilitate collaborative approach to health improvement with residents of rural and remote communities: Health workforce planning for rural and remote settings requires substantial collaboration with opinion leaders in rural and remote communities, including traditional healers and religious leaders. Retention problems are commonly caused by hostility to non-Indigenous health staff deployed to work in rural and remote regions without prior consultation with local authorities. With the protracted inadequacy of modern health services, herbalists and religious leaders have assumed leading roles as 'healthcare providers' in their regions, and must be co-opted as allies in efforts to improve rural health services. For example, the opposition of Muslim clerics to polio immunization in northern Nigeria may be attributable to a deep-seated suspicion about the motives of substantial numbers of local and international health providers, who focused on a single health issue while other health problems perceived as more important by local communities were disregarded40.
Develop and fund mobile health teams based in regional regions of rural and remote areas: The reality of living conditions in most rural and remote areas of Nigeria is that there are so few basic facilities that they are incompatible with long-term wellbeing, particularly for health workers accustomed to urban living. An approach to meeting both community needs for rural health workers and the lifestyle needs of skilled health workers can be found in createing 'hubs' in Nigerian regional areas. From these hubs, teams of highly skilled health workers could travel regularly to remote regions for brief periods. The regional hubs would have adequate social amenities, as well as work and schooling opportunities for the spouses and children of health workers. Health posts in rural areas served by mobile health teams could be staffed by local community health officers and assistants. These local health workers could manage common ailments, organize consultations for patients with more complex health problems, and follow up patient treatment after consultation with the specialist health staff in mobile teams. In developed countries like Australia, mobile health teams such as the Royal Flying Doctor Service have made a significant contribution to rural and remote health care while operating from regional hubs41.
Improve health sector funding: Nigeria's health sector funding relative to GDP is, at 3.9%, one of the lowest in the world. Item 26 of the 2001 Abuja Declaration, to which Nigeria was host and signatory, proposes that 15% of the GDP of African nations should be allocated to health care42. Less than half of the $US180 million (N27.8 billion) requested to implement the NHRFHSP in 2008 was allocated by the Federal Government. The lack of political will, corruption and mismanagement severely encumber well-intentioned initiatives to improve the Nigerian rural workforce. Health budget funding for human resource development should be clearly targeted to addressing the current situation where a significant number doctors, nurses and community health officers are unemployed due to poor health planning and blanket employment embargoes in the public sector19.
Conclusion
Diminishing political will for effectively addressing Nigeria's health problems is exemplified by the fact the current Federal Government took 9 months to appoint a new health minister following the resignation of the first government ministerial appointee (as sequel to a corruption scandal).
Chronic neglect of health management as a related but separate discipline from clinical training, systemic corruption, severely limited opportunities for non-medical graduates to participate at senior levels of public health planning, and sub-optimal collaboration with international non-governmental organizations, deprive Nigeria's public health system of genuinely entrepreneurial capital and skills which are urgently required to implement strategies for addressing recruitment and retention shortfalls in rural and remote regions of Nigeria. Only a coordinated intersectoral approach that begins with strong political commitment and adequate funding, and is embraced by local communities, is likely to reverse the steady deterioration in human resources management for rural and remote health services in Nigeria.
References
1. World Health Organization. Country health systems fact sheet - Nigeria. Brazzaville: WHO, 2006. Available: http://www.afro.who.int/home/countries/fact_sheets/nigeria.pdf (Accessed 12 November 2009).
2. International Observatory on End of Life Care. Country Report - Nigeria. Lancaster: Lancaster University, United Kingdom, 2005.
3. World Health Organization. Statistical information system. Geneva, WHO, 2005. Available: http://www.photius.com/rankings/total_health_expenditure_as_pecent_of_gdp_2000_to_2005.html (Accessed 16 November 2009).
4. McCoy D, Bennett S, Witter S, Pond B, Baker B, Gow J et al. Salaries and incomes of health workers in sub-Saharan Africa. Lancet 2008; 371: 675-681.
5. United Nations Development Program. Human Development Report 2009. Fact Sheets Indonesia and Philippines. New York: UNDP, 2009. Available: http://hdr.undp.org/en/media/HDR_2009_EN_Complete.pdf (Accessed 14 November 2009).
6. World Health Organization. The World Health Report: working together for health. Geneva, WHO; 2006.
7. Scheffler RM, Mahoney CB, Fulton B, Dal Poz MR, Preker AS. Estimates of health care professional shortages in sub-Saharan Africa by 2015. Health Affairs 2009; 28: w849-w862.
8. Uneke C, Ogbonna A, Ezeoha A, Onwe F, Ngwu B and the Innovative Health Research Group. The Nigeria health sector and human resource challenges. The Internet Journal of Health 8(1). (Online) 2008. Available: http://www.ispub.com/journal/the_internet_journal_of_health/volume_8_number_1_5/article/the_nigeria_health_sector_and_human_resource_challenges.html (Accessed 12 January 2008).
9. Maternal Mortality in 2005. Estimates developed by WHO, UNICEF, NUFPA and the World Bank. Geneva: WHO, 2007. Available: http://hdr.undp.org/en/media/HDR_2009_EN_Complete.pdf (Accessed 10 November 2009).
10. Wall LL. Dead mothers and injured wives: the social context of maternal morbidity and mortality among the Hausa of northern Nigeria. Studies in Family Planning 1998; 29: 341-359.
11. Umeora OUJ, Esike COU, Egwatu VC. Maternal mortality in rural Nigeria. International Journal of Gynecology and Obstetrics 2005; 88: 321-322.
12. Ronsmans C, Graham WJ on behalf of the Lancet Survival Series Steering Group. Maternal mortality: who, when, where, and why. Lancet 2006; 368: 1189-2000.
13. De Poel EV, Donnell OO, Doorslaer EV. What explains the rural-urban gap in infant mortality - household or community characteristics? Tinbergen institute discussion paper TI 2007/3. (Online) 2007. Available: http://www.tinbergen.nl/discussionpapers/07067.pdf (Accessed 15 November 2009).
14. Skeldon R. Of skilled migration, brain drains and policy responses. International Migration 2008; 47: 3-29.
15. Bach C. International mobility of health professionals - brain drain or brain exchange? World Institute for Development Economics Research. Research paper No. 2006/82. URL: http://www.wider.unu.edu/publications/working-papers/research-papers/2006/en_GB/rp2006-82/ (Accessed 13 November 2009).
16. Anyanwu JC. Rural Poverty in Nigeria: profile, determinants and exit paths. African Development Review 2006, 17: 435-460.
17. Porter G. Living in a walking world: rural mobility and social equity issues in sub-Saharan Africa. World Development 2002; 30: 285-300.
18. Bird K, Hume D, Moore K, Shepherd A. Chronic poverty and remote rural areas. CCRC Working Paper 13. (Online) 2002. Available: http://www.chronicpoverty.org/uploads/publication_files/WP13_Bird_et_al.pdf (Accessed 17 November 2009).
19. Labiran A, Mafe M, Onajole B, Lambo E. Health workforce profile for Nigeria, 1st edn. (Online) 2008. Available: http://www.afro.who.int/hrh-observatory/country_information/fact_sheets/Nigeria.pdf (Accessed 14 November 2009).
20. Wilson NV, Couper ID, De Vries E, Reid S, Fish T, Marais BJ. A critical review of interventions to redress the inequitable distribution of healthcare professionals to rural and remote areas. Rural and Remote Health 9: 1060. (Online) 2009. Available: http://www.rrh.org.au (Accessed 15 November 2009).
21. Laven G, Wilkinson D. Rural doctors and rural backgrounds. How strong is the evidence? A systematic review. Australian Journal of Rural Health 2003; 11: 277-284.
22. Awofeso N, Schelokova I, Dalhatu A. Training of frontline health workers for tuberculosis control: lessons from Nigeria and Kyrgyzstan. Human Resources Health 2008; 6: 20. Available: www.hrhresourcecenter.org/node/2169 (Accessed 15 November 2009).
23. Munga MA, Maestad O. Measuring inequalities in the distribution of health workers: the case of Tanzania. Human Resources Health 2009; 7: 4.
24. Gerein N, Green A, Pearson S. The implications of shortages of health professionals for maternal health in Sub-Saharan Africa. Report on Health Matters 2006; 14: 40-50.
25. Khemeni S. Local government accountability for health service delivery in Nigeria. Journal of African Economies 2005; 15: 288-312.
26. McPake B, Asiimwe D, Mwesigye F, Ofumbi M, Ortenblad L, Streefland P et al. Informal economic activities of public health workers in Uganda: implications for quality and accessibility of care. Social Science and Medicine 1999; 49: 849-865.
27. Federal Republic of Nigeria. National Human Resources for Health Strategic Plan 2008-2012. Abuja: Federal Ministry of Health, 2007. Available: http://www.docstoc.com/docs/4026583/FEDERAL-REPUBLIC-OF-NIGERIA-NATIONAL-HUMAN-RESOURCES-FOR-HEALTH-STRATEGIC (Accessed 15 November 2009).
28. Pong RW, Russell N. A review and synthesis of strategies and policy recommendations on the rural health workforce. Ontario: Centre for Rural and Northern Health Research, Laurentian University, 2003. Available: http://portal.laurentian.ca/NR/rdonlyres/93AB730E-5D37-4E50-B490-12E80F3433A1/0/TORC_RuralhealthworkforcesynthesisfinaldraftMay.pdf (Accessed 11 November 2009).
29. Harries AD, Zachariah R, Bergstrom K, Blanc L, Salaniponi FM, Elzinga G. Human resources for control of tuberculosis and HIV-associated tuberculosis. International Journal of Tuberculosis and Lung Disease 2005; 9: 128-137.
30. Hungoro C, Normand C. Health workers: building and motivating the workforce. The World Bank. Disease control priorities in developing countries. Washington, DC: The World Bank, 2006. Available: http://www.ncbi.nlm.nih.gov/bookshelf/picrender.fcgi?book=dcp2&part=A10283&blobtype=pdf (Accessed 13 November 2009).
31. Marenin O. Implementing deployment policies in the National Youth Service Corps of Nigeria: Goals and Constraints. Comparative Political Studies 1990; 22: 397-436.
32. Kotzee TJ, Couper ID. What interventions do South African qualified doctors think will retain them in rural hospitals of the Limpopo province of South Africa? Rural and Remote Health 6: 581. (Online) 2006. Available: http://www.rrh.org.au (Accessed 11 January 2010).
33. Fritzen SA. Strategic management of the health workforce in developing countries: what have we learned? Human Resources for Health 2007; 5: 4.
34. Mullan F, Frehywot S. Non-physician clinicians in 47 sub-Saharan African countries. Lancet 2007; 370: 2158-2163.
35. Bryan L, Garg R, Ramji S, Silverman A, Tagar E, Ware I. Investing in Tanzanian human resources for health. (Online) 2006. Available: http://touchfoundation.org/uploads/assets/documents/mckinsey_report_july_2006_5nYbVVVS.pdf (Accessed 10 November 2009).
36. Pemba SK. Training of assistant medical officers in Tanzania. (Online) 2008. Available: http://www.healthtrainingifakara.org/AMO/amoprofile08.pdf (Accessed 13 November 2009).
37. World Health Organization. Strengthening health leadership and management: the WHO framework. Available: http://www.who.int/management (Accessed 14 November 2009).
38. El Ansari W, Russell J, Wills J. Education for health: case studies of two multidisciplinary MPH/MSc public health programmes in the UK. Public Health 2003; 117: 365-376.
39. Islam M (Ed.). Health systems assessment approach: a how-to manual. U.S. Agency for International Development in collaboration with Health Systems 20/20, Partners for Health Reformplus, Quality Assurance Project, and Rational Pharmaceutical Management Plus. Arlington, VA: Management Sciences for Health, 2007. Available: http://www.who.int/pmnch/topics/continuum/hsassessmentapproach/en/index.html (Accessed 13 January 2010).
40. Yahya M. Polio vaccines - 'no thank you!' : barriers to polio eradication in northern Nigeria. African Affairs2007; 423: 185-204.
41. Harvey DJ, Williams R, Hill K. A flying start to health promotion in remote north Queensland, Australia: the development of Royal Flying Doctor Service field days. Rural and Remote Health 6: 485. (Online) 2006. Available: http://www.rrh.org.au (Accessed 11 January 2010).
42. Abuja Declaration. African summit on HIV, AIDS tuberculosis and related infectious diseases. April 2001; Abuja, Nigeria; 2001. Available: http://www.un.org/ga/aids/pdf/abuja_declaration.pdf (Accessed 13 November 2009).
