Introduction
Worldwide, injuries represent a substantial public health issue, accounting for approximately 5 million deaths in 2000, a mortality rate of 83.7 per 100 000 population1. In Australia, injury is the leading cause of death for individuals aged 1 to 44 years2 and is the fifth leading cause of hospitalisation for all age groups3. However, the rate of injury differs for urban and rural residents. For example, the rate of hospitalised injury for rural residents is 1.4 times higher than that of urban residents4. This urban-rural difference in injury rates is common in other countries5-7.
In 2005, Australia's National Injury Prevention Plan was released, in which the prevention of injury in rural and remote Australian populations was declared a national priority4. In order to identify where injury prevention strategies for rural populations should be targeted in New South Wales (NSW), Australia's most populous state, information is required about the patterns and causes of injury-related hospitalised morbidity and mortality. This article provide this by identifying and comparing the pattern of hospitalised injury morbidity and injury mortality for urban and rural residents in NSW.
Method
Hospital admission data
Hospitalisation data were obtained from the NSW Admitted Patients Data Collection (APDC) from 1 July 2000 to 30 June 2005. The APDC includes information on inpatient separations from NSW public and private hospitals, private day procedures and public psychiatric hospitals. Information collected includes patient demographics, diagnoses and clinical procedures. Hospitalised morbidity data were coded using the ICD, 10th revision, Australian Modified (ICD-10-AM)8-10.
Injury-related hospitalised morbidity was identified using the following criteria:
- the hospitalisation was for a resident of NSW
- a principal diagnosis was in the ICD-10-AM range S00-T98
- an external cause code was in the ICD-10-AM range V00-Y98.
The NSW hospitalisation data include information on episodes of care in hospital that end with the discharge, transfer or death of the patient, or when the service category for the admitted patient changes. Also included within the APDC are hospitalisations of NSW residents that occurred in another state or territory of Australia.
Hospitalisations relating to transfers or statistical discharges were excluded from the analysis in order to partly eliminate 'multiple counts', which occur when an individual has more than one episode of care for an injury. These exclusions refer to transfers between hospitals or changes in the service category (eg a change from acute to rehabilitation care) for a patient during one episode of accommodation in a single facility11.
Mortality data
Mortality data were obtained from the Australian Bureau of Statistics (ABS) mortality data file from 1 January 2000 to 31 December 2004. Deaths in NSW are registered with the NSW Department of Births, Deaths and Marriages and information collected from death certificates (certified by a medical practitioner or pathologist) includes demographic data and the cause of death. This information is provided to the ABS and mortality data is coded using the International Classification of Diseases (ICD) v1012.
Injury-related mortality was identified using the following criteria:
- the deceased was a resident of NSW and the death occurred in Australia
- an external cause code was in the ICD-10 range V00-Y98.
Urban-rural classification
The enhanced Accessibility/Remoteness Index of Australia, classification, ARIA+13, was used to define urban and rural locations. The ARIA+ is a continuous varying index with values ranging from 0 (high accessibility) to 15 (high remoteness). The ARIA+ measures access in terms of remoteness determined on road distance measurements from 11 914 populated localities to the nearest 5 categories of service centre, based on population sizes of more than 250 000 persons; 48 000 to 249 999 persons; 18 000 to 47 999 persons; 5000 to 17 999 persons; and 1000 to 4999 persons. Localities that are more remote have less access to service centres; those that are less remote have greater access to service centres. The 5 ARIA+ scores are classified into 5 groups: major cities, inner regional, outer regional, remote and very remote.
Data analysis
Analysis was performed using SAS v9.1 (SAS Institute. Cary, North Carolina, USA). For hospitalisation and mortality data, age- and sex-specific population estimates as at 31 December and 30 June 2001 were used as the standard population, respectively, obtained from the NSW Health Department. These estimates are based on the ABS population estimates14. Direct age standardised rates were calculated using the estimated Australian residential population at 30 June 2001 as the standard population. Standardised mortality ratios (SMR) and standardised admission ratios (SAR) were calculated for specific injury mechanisms. Indirect age standardised rates were used to calculate the SMR and SARs using the age-specific rate for urban residents as the standard rate. Ninety-five percent confidence intervals (95% CI) were calculated assuming a Poisson distribution15,16. P-values were generated using the method of exact confidence intervals of the SMRs17. For the analysis, the statistical local area (SLA) of residence of the injured person was used to identify the geographic location, the ARIA+ classification groups of 'major cities' and 'inner regional' were defined as 'urban', while the classification groups of 'outer regional', 'remote' and 'very remote' were defined as 'rural'.
There were 609 970 injury-related hospital admissions identified, 1986 (0.3%) of which did not have a SLA code and for 3633 (0.6%) SLAs an ARIA+ code could not be defined. A total of 12 331 injury-related deaths were identified from the mortality data. There were 131 (1.1%) deaths that did not have an SLA code and for 623 (5.1%) SLAs an ARIA+ code could not be defined. These cases with missing data were excluded from the analyses. In addition, the gender of five hospitalised individuals and the age of 542 hospitalised and nine deceased individuals was unknown and these cases were excluded from the gender-based and age-specific analyses, respectively.
Results
Hospital admissions
There were 604 351 injury-related hospitalisations during the period 1 July 2000 to 30 June 2005, giving an overall rate of 1805.6 per 100 000 population. Of these hospitalisations, 544 322 (90.1%) were of urban (1754.6 per 100,000 population) and 60 029 (9.9%) were of rural (2481.8 per 100,000 population) residents. Rural males had the highest hospitalisation rate (3023.6 per 100 000 population) and this rate was almost 1.5 times the rate of urban males (2117.4 per 100 000). Rural females had a hospitalisation rate higher than urban females (1871.8 per 100 000 and 1377.1 per 100 000, respectively). Hospitalised injury rates for both sexes were higher in rural compared with urban residents over time (Fig1).
Males aged 15-29 years had the highest rates of hospitalised injury and for rural males the rate was twice as high as the hospitalisation rate for urban males. The highest hospitalised injury rates for rural females were for those aged 65 years and over (Fig2).
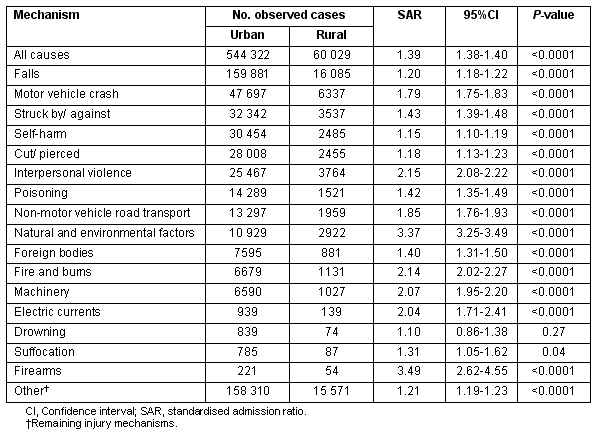
Rural residents had an increase likelihood of being hospitalised for each injury mechanism, except drowning (Table 1). Incidents involving firearms or natural and environmental factors were at least 3 times more likely to involve rural rather than urban residents. Incidents involving interpersonal violence (IPV), fire and burns, machinery, and electric currents were at least twice as likely to involve a rural resident being admitted to hospital than an urban resident.
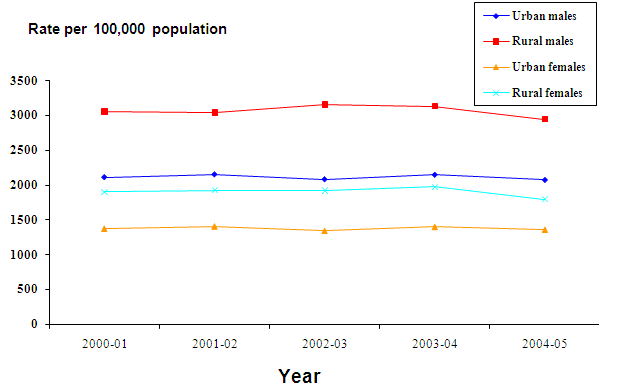
Figure 1: Injury-related hospital admissions (age-standardised hospitalisation rates) in New South Wales for urban and rural residents by gender, 1 July 2000 to 30 June 2005.
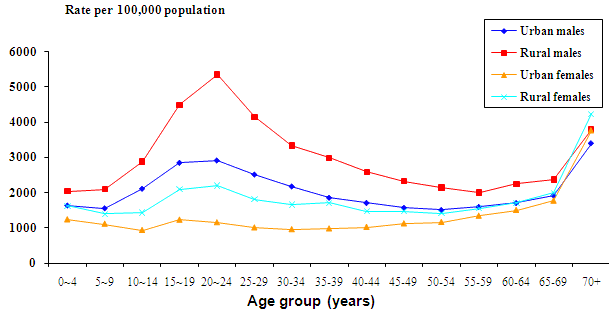
Figure 2: Injury-related hospital admissions (age-standardised hospitalisation rates) in New South Wales for urban and rural residents by gender and age group, 1 July 2000 to 30 June 2005.
Table 1: Urban and rural indirect standardised hospital admission ratios for injury-related admissions in New South Wales by injury mechanism, 1 July 2000 to 30 June 2005
Mortality
There were 11 577 injury-related deaths during the period 2000 to 2004, giving an overall rate of 34.2 per 100 000 population. Of these, 10 421 (90.0%) were of urban (33.2 per 100 000 population) and 1156 (10.0%) were of rural (48.1 per 100 000 population) residents. Rural males had the highest injury mortality rate (69.9 per 100 000 population) and this was 1.5 times higher than the rate of urban males (48.1 per 100 000). Rural females had an injury mortality rate approximately 1.3 times higher than their urban counterparts (26.0 per 100 000 and 19.3 per 100 000, respectively). Injury mortality rates were higher in rural compared with urban residents over time (Fig3). Males aged 70 years and over and 20-34 years had the highest rates of injury mortality. Rural females aged 15-34 and rural and urban females aged 70 years and over had the highest injury mortality rates for females. Rural children aged less than 5 years had injury mortality rates twice as high as urban children (Fig4).
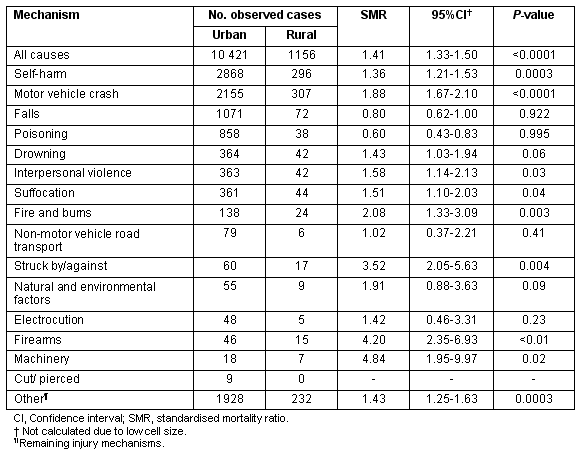
Rural residents had an increase likelihood of being fatally injured by each injury mechanism, except falls, poisoning, drowning, non-motor vehicle road transport, natural and environmental factors and electrocution (Table 2). Fatal incidents that involved machinery, firearms, and struck by/struck against objects were between 3 and 4 times more likely to involve rural than urban residents.
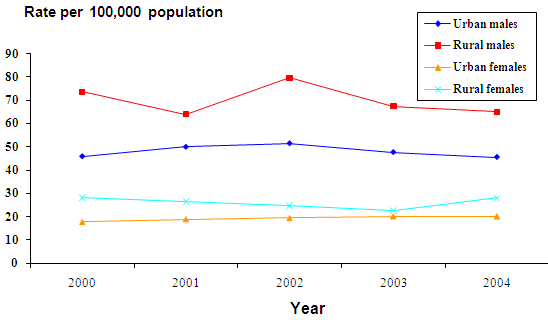
Figure 3: Injury-related mortality (standardised mortality rates) in New South Wales for urban and rural residents by gender, 2000-2004.
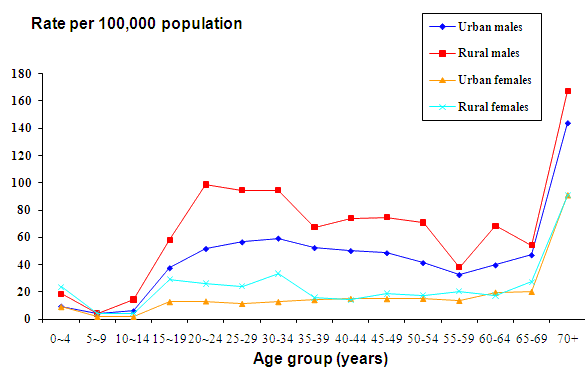
Figure 4: Injury-related mortality (age-standardised mortality rates) in New South Wales for urban and rural residents by gender and age group, 2000-2004.
Table 2: Urban and rural indirect standardised mortality ratios for injury-related deaths in New South Wales by injury mechanism, 2000-2004
Discussion
Injuries represent a substantial public health issue in many countries18, with some sections of a population identified as being more at risk of injury than others19. This study found that despite only 10% of rural residents in NSW being hospitalised for an injury or being fatally injured, injury-related hospitalisation and mortality rates were almost 1.5 times higher for rural compared with urban residents. Other studies have also identified higher injury6,20,21 and injury mortality6 rates in rural versus urban locations. There are numerous factors that could play a part in the higher rates of hospitalised injury and injury mortality in rural locations in NSW, such as different environmental conditions and an increased likelihood of a rural residents' exposure to some injury mechanisms, particularly mechanical agents, such as firearms and machinery22.
Rural males had the highest injury hospitalisation and mortality rates in the current study. Likewise, males in both small and large rural areas were found to have the highest injury hospitalisation rates in the USA in 2004, compared with males in small urban areas and females in any location23. In a prior US study during 1997 to 2001, rural males were found to have higher injury rates compared with males in suburban, small and large urban locations and females in any location20. In NSW, rural males are more likely to be employed in rural high risk industries, such as agriculture, forestry and logging, and mining industries. These industries have all been shown to have higher work-related fatal injury rates in Australia when compared to the all-industry average23.
In the current study, the high injury mortality rates of rural children aged less than 5 years compared to urban children is of concern. For children living in rural areas, their home and playground is often also a workplace. Studies in Colorado24 and the USA21 also showed higher rates of injury for children residing in rural compared with urban localities, due to the dual nature of locations as worksite and an area for recreation25. Recommended strategies for the prevention of injury to young children have focused on limiting their exposure to hazards found on rural properties, such as through the creation of designated safe play areas, the establishment of guidelines for children's work in agriculture, and the restriction of access to farm machinery26-28.
Injury mechanisms differed between the rural and urban population, with rural residents experiencing higher SARs for almost all injury mechanisms. Mechanisms, such as firearms and machinery, generally had high SMRs and SARs for rural residents. Machinery, such as tractors and related equipment, are common agents of fatal injury on rural properties, often involving tractor rollovers and run overs29-33. Prevention strategies such as fitting roll over protective structures (ROPS) have shown demonstrable reductions in fatalities due to tractor rollover34. In order to reduce the incidence of tractor run overs, tractor safety access platforms have been recommended35.
Other fatal mechanisms, such as fire and burns, motor vehicle crashes (MVCs), and natural and environmental factors were almost twice as likely to involve rural rather than urban residents. For hospitalised injuries, IPV, fire and burns, machinery, and electric currents, were all twice as likely to involve rural residents. In part, the higher SMRs and SARs for mechanisms, such as MVCs, natural and environmental factors, and machinery are due to increased exposure to these mechanisms compared with urban residents. In particular, for MVCs, factors such as travel distance, vehicle speed, lighting conditions and a lack of road safety features, have all been found to contribute to higher injury mortality and hospitalisation rates in rural compared with urban residents5,6. Other possible reasons for higher injury mortality rates in rural residents have included an increased time to discovery and poorer access to rescue and retrieval and/or medical services5. However, these factors alone do not explain the increase in hospitalised injury morbidity among rural residents.
Study limitations
There are several limitations to the current study. These included the absence of information regarding the geographic location of the fatal or non-fatal injury in the mortality and hospitalisation data collections. Instead, an assumption was made that residents were injured in the location in which they resided. It is possible that admission practices may differ between more urban compared to more remote locations. However, incidentally, the home has been found to be a common location of injury36, particularly for children37. It is recommended that the feasibility of collecting information regarding the geographic location of the injury should be assessed. Approximately 1% of injury-related hospital admissions and 6% of deaths could not be allocated an ARIA+ code due to missing or inadequate SLA information. However, these proportions are relatively small and would not have changed the findings of the current study. The quality of the hospital morbidity and mortality data in NSW is largely unknown and it is possible that poor data validity might have affected the study's results.
Conclusion
This article has quantified the difference in the experience of hospitalised injury and injury mortality between rural and urban residents in NSW, with rural residents experiencing a higher injury burden. Mechanisms of injury that have demonstrably higher SMRs and SARs in rural compared with urban locations should be targeted for injury prevention activity. This has implications for policy-makers who are charged with implementing the National Injury Prevention and Safety Promotion Plan in NSW, particularly because there has been little change in the incidence rates of mortality and hospitalised injury over time in NSW during the time periods examined.
Acknowledgements
The authors were supported by the NSW Injury Risk Management Research Centre, with core funding provided by the NSW Health Department, the NSW Roads and Traffic Authority and the Motor Accidents Authority. The authors thank the Centre for Epidemiology and Research at the NSW Health Department for providing access to the Health Outcomes and Information Statistical Toolkit (HOIST) to obtain data analysed in this study. The HOIST system refers to a data access, analysis and reporting facility established and operated by the Centre for Epidemiology and Research, Population Health Division, NSW Department of Health.
References
1. Peden M, McGee K, Sharma G. The injury chart book: a graphical overview of the global burden of injuries. Geneva: World Health Organization, 2002.
2. Kreisfeld R, Newson R, Harrison J. Injury deaths, Australia 2002. Injury research and statistics series no.23. Vol. INJCAT 65. Adelaide, SA: AIHW, 2004.
3. Berry J, Harrison J. Hospital separations due to injury and poisoning, Australia 2003-04. Injury research and statistics series no. 30. Adelaide, SA: AIHW, 2007.
4. National Public Health Partnership. The National Injury Prevention and Safety Promotion Plan: 2004-2014. Canberra, SA: National Public Health Partnership, 2004.
5. Kmet L, Macarthur C. Urban-rural differences in motor vehicle crash fatality and hospitalization rates among children and youth. Accident Analysis & Prevention 2006; 38: 122-127.
6. Boland M, Staines A, Fitzpatrick P, Scallan E. Urban-rural variation in mortality and hospital admission rates for unintentional injury in Ireland. Injury Prevention 2005; 11(1): 38-42.
7. Macpherson AK, To TM, Parkin PC, Moldofsky B, Wright JG, Chipman ML, Macarthur C. Urban/rural variation in children's bicycle-related injuries. Accident Analysis & Prevention 2004; 36(4): 649-654.
8. National Centre for Classification in Health. ICD-10-AM, 1st edn. Sydney, NSW: National Centre for Classification in Health, 1998.
9. National Centre for Classification in Health. ICD-10-AM 2nd edn. Sydney, NSW: National Centre for Classification in Health, 2000.
10. National Centre for Classification in Health. ICD-10-AM, 3rd edn. Sydney, NSW: National Centre for Classification in Health, 2002.
11. Population Health Division. The Health of the People of NSW. Report of the Chief Health Officer. Sydney, NSW: NSW Health Department, 2004.
12. World Health Organization. International statistical classification of diseases and related health problems, v10. Geneva: World Health Organization, 1992.
13. Glover J, Tennant S. Remote areas statistical geography in Australia. Notes on the Accessibility/Remoteness Index of Australia (ARIA+ version). Working paper series no. 9. Adelaide, SA: Public Health Information Development Unit, 2003.
14. Centre for Epidemiology and Research. Health Outcomes and Information Statistical Toolkit (HOIST). Sydney, NSW: NSW Department of Health, 2006.
15. Ulm K. A simple method to calculate the confidence interval of a standardized mortality ratio. American Journal of Epidemiology1990; 131(2): 373-375.
16. Greenland S. A simple method to calculate the confidence interval of a standardized mortality ratio. American Journal of Epidemiology 1990; 133(2): 212-213.
17. Sun J, Ono Y, Takeuchi Y. A simple method for calculating the exact confidence interval of the standardized mortality ratio with an SAS function. Journal of Occupational Health 1996; 38(4): 196-197.
18. Krug E. Injury surveillance is the key to preventing injuries. The Lancet 2004; 364: 1563-1566.
19. Dixon J, Welch N. Researching the rural-metropolitan health differential using the 'social determinants of health'. Australian Journal of Rural Health 2000; 8: 254-260.
20. Tiesman H, Zwerling C, Peek-Asa C, Sprince N, Cavanaugh J. Non-fatal injuries among urban and rural residents: The National Health Interview Survey, 1997-2001. Injury Prevention 2007; 13: 115-119.
21. Coben J, Tiesman H, Bossarte R, Furbee P Rural-Urban differences in injury hospitalizations in the US, 2004. American Journal of Preventive Medicine 2009; 36(1): 49-55.
22. Denis W. Causes of health and safety hazards in Canadian agriculture. International Journal of Health Services 1988; 18(3): 419-436.
23. Driscoll T, Mitchell R, Mandryk J, Healey S, Hendrie L, Hull B. Work-related fatalities in Australia, 1989 to 1992: an overview. Journal of Occupational Health and Safety - Australia and New Zealand 2001; 17(1): 45-66.
24. Hwang HC, Stallones L, Keefe TJ. Childhood injury deaths: rural and urban differences, Colorado 1980-8. Injury Prevention 1997; 3(1): 35-37.
25. Lexau C, Kingsbury L, Lenz B, Nelson C, Voehl S. Building coalitions: a community wide approach for promoting farming health and safety. American Association of Occupational Health Nurses 1993; 41(9): 440-449.
26. Mitchell R, Franklin R, Driscoll T, Fragar L. Farm-related fatalities involving children in Australia, 1989-1992. Australian & New Zealand Journal of Public Health 2001; 25(4): 307-314.
27. Cameron D, Bishop C. Farm accidents in children. BMJ 1992; 305: 22-25.
28. Strueland D, Lee B, Nordstrom D, Layde P, Wittman D. A population based case-control study of agricultural injuries in children. Injury Prevention 1996; 2: 192-196.
29. Franklin R, Mitchell R, Driscoll T, Fragar L. Agricultural work-related fatalities in Australia, 1989-1992. Journal of Agricultural Safety and Health 2001; 7(4): 213-227.
30. McCurdy S, Carroll D. Agricultural injury. American Journal of Industrial Medicine 2000; 38: 463-480.
31. Crandall C, Fullerton L, Olson L, Sklar D, Zumwalt R. Farm-related injury mortality in New Mexico, 1980-91. Accident Analysis & Prevention 1997; 29(2): 257-261.
32. Gerberich S, Gibson R, French L, Lee T, Carr W, Kochevar L, Renier C, Shutske J. Machinery-related injuries: regional rural injury study - I (RRIS-1). Accident Analysis & Prevention 1998; 30(6): 793-804.
33. Pollock K, Fragar L, Morton C. Traumatic deaths in Australian agriculture: the facts 2007, Rural Industries Research and Development Corporation and Australian Centre for Agricultural Health and Safety: Canberra.
34. Day L, Rechnitzer G, Lough J. An Australian experience with tractor rollover protective structure rebate programs: process, impact and outcome evaluation. Accident Analysis & Prevention 2004; 36(5): 861-867.
35. Day L, Rechnitzer G. Safe tractor access platforms: from guidance material to implementation. Journal of Agricultural Safety and Health 2004; 10(3): 197-209
36. Runyan C, Perkis D, Marshall S, Johnson R, Coyne-Beasley T, Waller A, Black C, Baccaglini L. Unintentional injuries in the home in the United States Part II: Morbidity. American Journal of Preventive Medicine 2005; 28(1): 80-87.
37. Williams K, Schootman M, Quayle K, Struthers J, Jaffe D. Geographic variation of pediatric burn injuries in a metropolitan area. Accident and Emergency Medicine 2003; 10(7): 743-752.
