Introduction
Services to rural areas are treated as just that, 'services'. However, the role of services can be more than just 'provision of service' because more often than not services bring with them infrastructure and professional personnel. Professionals can be, and often are, major assets for economic, social and cultural sustainability1-6. The problem is that professionals are often 'visitors' to rural areas and their retention and recruitment is difficult for a range of reasons7-13.
Governments do develop policies and programs to support allied health in rural Australia, such as the Australian Federal Government's Rural Allied Health Undergraduate Scholarship Scheme, Rural Allied Health Clinical Placement Grants, and the past Rural Private Access Program. In Victoria a suite of local, regional and state-wide workforce projects have been initiated by the Department of Human Services. These include the 'Region of Choice', 'Mentoring Works' and 'Statewide Allied Health Workforce Education Program' that aim to attract and retain health professionals in rural areas. However, the retention of allied health practitioners (AHPs) is still problematic and, with the exception of medical practitioners in the primary healthcare setting, governments predominantly focus on the 'public sector' when developing rural health policies. The general focus on retention policies for rural and regional AHPs in Australia has been 'employment' of personnel in pre-existing structures of public delivery (eg hospital or community health setting). This has been reinforced by workforce studies that focus on managing allied health professionals within public health hierarchical structures14-18. These studies focus almost exclusively on public sector employees. The role of private AHPs is rarely mentioned.
Professionals need flexibility in the way they perform relevant tasks and apply their skills in rural areas. The need for 'flexibility' is a common attribute among professionals in rural settings19. The application of rigid management controls, especially under strict funding guidelines, will often clash with this need for flexible arrangements in rural settings20. The issue of more flexible funding models for rural health has been raised in the literature by researchers looking for alternative models of management or funding, in order to establish clinical leadership and improved rural career options20-22. The focus is still very much on restructuring funding models for the public sector. Research has shown that private AHPs generally remain longer in rural areas than those working in the public sector12,23,24. Little recognition is given to re-thinking models that help to integrate the private sector into the allied health workforce policy mix. However, before policy-makers consider changes to the present system, analysis is required of what private practitioners think about their own role in broader policy for retention of practitioners in rural areas.
This article reports on the thoughts and perceptions of an important group of private AHPs in rural areas using data from a survey about inclusion into a broader rural health policy and programs. The focus of this article is on 'rehabilitation therapists' (RTs; physiotherapy, occupational therapy and speech pathology)25. For the purposed of this discussion, the term 'public' means health services that belong to the state, and 'private' refers to services that are 'for profit' outside of the state.
Method
Participants
The target group for the surveys included private RTs working in rural and regional areas of Victoria. Because the project is exploratory and funding was limited, only those private RTs who had an email address were chosen. Email addresses were obtained from lists on the internet, and were thus limited to RT professions that made such lists publicly available (physiotherapy, occupational therapy and speech pathology). The number of email addresses obtained was 198, of which 14 were returned as invalid or rejected by spam protectors. Of the remaining 184, 72 surveys were completed (40%). This completion rate is considered a good response rate for online surveys26.
Instrument
The survey consisted of 29 questions: eight related to the perceived place occupied by RTs in rural areas; eight related to their professional practice; seven related to retention policies; two related to education and training; and four were demographic questions (Appendix I). The questions in the survey were drawn from previous research into the retention of allied health practitioners in rural areas24,25,27. The survey was constructed using an online survey program (Zoomerang).
Procedure
Ethics approval for the survey was granted by Deakin University, Victoria, and consent by respondents was assumed if the survey was returned. A URL for the survey was included in the email and sent to participants. Data from completed surveys went directly into a database so that all responses were anonymous and confidential. The sample was purposive rather than representative, because the study design was intended to be exploratory rather than definitive.
Results
Of the 72 respondents 66 reported their occupation: 23 were speech pathologists, 22 were physiotherapists and 21 were occupational therapists. The overwhelming majority of respondents who reported their sex were female (77%, n=55). The majority (52%, n=31) were aged between 36 and 50 years, while 28% (n=17) were 35 and below, and 20% (n=12) were over 50 years. Of those who reported the number of years working in rural/regional areas (n=53), 64% had worked for 10 years or less. One respondent had worked for 38 years in rural/regional areas. Of the 60 who reported where they began their careers, 63% (n=38) reported rural and 37% (n=22) indicated urban. The overwhelming majority (n=50, 79%) began their careers in the public sector, 11% (n=7) began in non-government organization (NGO) sector, while only 10% (n=6) began in the private sector.
More than a quarter of the rural private RTs (n=19) reported working in partnership with the public sector for part of the time. The majority of those practitioners worked as clinical practitioners in the public sector (on a salary) and their hours of work varied from 2 to 38 per week. The individual who indicated 38 hours also worked another 16 hours in private practice. Others (n=5) reported that they also acted in an advisory role for the public sector. A smaller number (n=11) worked in the NGO sector in a clinical as well as an advisory role. Thirty practitioners also worked in a voluntary capacity for one or more sporting organizations, welfares groups, charities or schools. Their activities varied among clinical, advisory, governance or training roles. There was a considerable number (n=45) who indicated that they worked with practitioners of other than their own profession. This varied from cross referrals to team work with other practitioner groups both within and without their own professions.
Of the 65 who answered the question 'Is there benefit for rural or regional health professionals having partnerships between private and public practice in rural and regional areas?' all but one answered 'yes'. When asked how partnerships would be of benefit, the answers from 59 respondents covered a wide range of areas including:
- mentoring and professional development
- helping to alleviate waiting lists
- better access to and local coordination of service delivery
- better use of shared interdisciplinary knowledge in the local community
- wider array of allied health skills to share, mentor and utilize in the local community
- more efficient use of resources in the community through sharing
- better use of staff time through rostering between public and private facilities
- a more comprehensive approach to primary health care.
A total of 62 respondents answered 'yes' to the question 'Do you think governments need to develop programs in rural and regional areas to facilitate partnerships between private, public and community practices?' When asked whether governments should facilitate such partnerships, the response was varied. There was a general feeling that such facilitation would be beneficial as long as it did not involve increased paperwork and regulation.
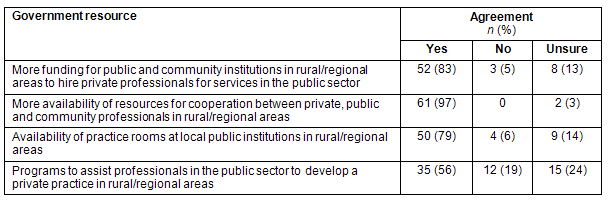
Respondents were then asked whether they agreed or not with the propositions outlined (Table 1). The RTs agreed to more funding for public and community institutions, more availability of resources (such as availability of practice rooms at local places), and extra programs to assist professionals in the public sector to develop a private practice in rural/regional areas.
Table 1: Agreement or not with government resources
The respondents also made a number of general and particular suggestions about ways to assist private RTs to sustain their practices in rural areas. Some of these included:
- educational support, for example lower costs for access to or use of local in-house public professional development programs
- compensation for hours spent on roads to visit more remote clients
- grants to assist with practice development
- funding for private practitioners to mentor/support public clinicians if they have a skill area the local public clinicians do not have
- tax incentives to attract and maintain health professionals
- improved streamlining of public and private practices to facilitate better client outcomes
- scholarships to support the training and development of private pratitioners to fill service gaps.
When asked whether there was any emphasis placed on how to run a business in their professional education, 61 of the 66 who answered the question (92%), said 'no'. When asked whether there should be business training, 21 (32%) answered 'no'. Those who answered 'no' were more inclined to argue that business training could be undergone later in post-graduate work or through their professional organisations. Others argued that practitioners should think about business skills once they had become more experienced in their profession. However, the 44 who replied 'yes' indicated that learning business skills is not incompatible with delivering good care. Skills within the human resource field such as recruiting and retaining staff, staff management, documentation and record keeping, were considered to be easily transferable to good professional practice. Others argued that many aspects of business practice such as finance, tax, work care, staff employment and obligations, were all skills that could be easily employed in the public sector as well. There was support for government and professional assistance for small business training when practitioners were seeking to establish their businesses.
The respondents were divided on the question of whether governments should provide incentives for private practitioners to relocate to rural areas. Those who thought that incentives for relocation was good policy (56%, n=36) suggested initiatives such as:
- adjusting the enhanced primary care (EPC) program fees for practitioners in rural areas
- providing access to rooms/clinical space or set up grants
- development of diagnosis/issue specific clinics
- reduction in Higher Education Contribution Scheme (HECS) fees
- access to salary packaging
- grants or scholarships for private practitioners
- tax rebates for costs of travel, relocation and accommodation.
However there was some caution from those who replied 'no' to the question. They said that it depended on whether there was a shortage of specific professionals in the area. They generally wanted more policy recognition for existing practitioners so retention problems could be overcome. In this respect there was support for more scholarships and grants to attract practitioners into the existing private practices. There was some hesitation about government support for setting up clinics that had their home base in large urban centres like Melbourne. Such an approach was seen as a way of channelling funding into urban clinics while sustaining minimal practice in rural areas.
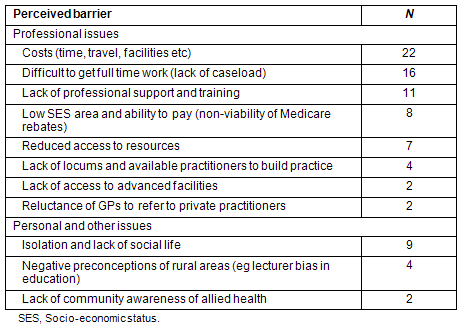
When the respondents were asked about the major barriers to working in rural areas there was a range of responses (Table 2). Many of the issues had been foreshadowed in previous questions but the leading barriers were seen as cost, small numbers of available clients, lack of access to professional training and the low socio-economic status (SES) of many of their clients.
Table 2: Perceived barriers to working in rural areas
When respondents were asked whether having a private practice widened their social network in their location, 52% (n=31) indicated that it did. This included mixing with other business people in the area, and especially for women through business training. For those in small towns the business was an entrée into social networks as the professionals in the public facilities were generally in larger regional centres. There was also the opposite reaction from the 48% (n=29) who felt their social network was limited because many of the local population were clients, either through their private practice or in partnership with public facilities.
There were 55% (n=32) who felt that they had a positive role to play in local economic development. This included their role in hiring people to work for them, investing and spending money in the locality, contributing to other local developments as community members and providing an essential service to the locality that makes it more attractive for others to invest in the area. In their professional role many considered themselves to be the means for keeping local people healthy through primary health care, and supplying rehabilitation processes, which both add to the vitality of the local area and create a better environment for economic development.
When asked to comment further, there was some indication that public perceptions of private RT practice in rural and regional areas was not always very positive. For example:
Philosophical perspectives can have a negative impact (ie workers in public sector may believe that private practitioners are only in it for the money).
Private practice professionals need to make a profit and this does not always sit well with the public purse.
There is often the perception that we are making oodles of money from the fees we charge, however nothing could be further from the truth.
This was supported by other comments that indicate that working in rural areas is not a 'goldmine' for RTs:
I personally do not feel I can charge anywhere near what I know is charged by my colleagues in Melbourne, despite offering at least an equal service. This makes it hard to make a living on private practice alone.
Discussion
It has been recognised that the need to develop a more systematic approach to healthcare delivery in rural areas requires the involvement of all sectors of the health community29. Among the medical profession in Australia, there is a history of private practitioners working closely with the public health system and this is acknowledged in various funding processes. This has generally not been the case for private RT practitioners.
While the term 'public' is usually reserved for health services that belong to the state, and 'private' is used to describe services that are 'for profit' outside the state, Giusti et al.29 states that:
...the public health sector should be supported by public money and protected by a series of privileges regulated by law, while the private health sector should operate on private funding, obtained through fees, donations or other means in the arena of a market oriented provision of service and of competition. This understanding is based on the assumption that the private sector is homogeneous and financially self-sustaining whereas, in reality, a remarkable heterogeneity exists in the private/non-government sector.
This description applies as much to rural Australia as it does to developing countries. As reported in this survey, many private RTs in rural areas of Victoria are not financially self-sustaining. The difficulties of obtaining a full time caseload and the costs associated with travel over large distances means that income from private fees alone leaves many private RTs at a disadvantage when compared with their urban counterparts. Some clinical care partnerships already exist with the public sector (26%) and a smaller percentage (15%) with the NGO sector. However, there are also practices in many public facilities that charge direct fees to the public for service access. For example, regional hospitals charge a means tested fee for clients who use their allied health care facilities. Thus, the charging of fees does not in itself relate only to the private sector.
If the term 'public health services' is re-defined not as an as administrative division based on fee delivery, but according to 'the objectives and output of that service' then the perceived prejudices encountered by some of the survey respondents could be overcome29. Many of the respondents perceived that collaboration with the public sector may lead to better health outcomes, such as helping to alleviate waiting lists, better use of shared interdisciplinary knowledge in the local community, a wider array of allied health skills to share, mentor and utilize in the local community and better use of staff time through rostering between public and private facilities. Such perceptions could be used as the basis for place based delivery of healthcare services to specific rural communities.
A considerable majority of private RTs in this survey indicated that it would be beneficial for governments to make resources more available for cooperation among private, public and community professionals in rural/regional areas. This is not unexpected because there are many private RTs who would gain if a broader range of clients was made available to them. Nevertheless if there are already existing programs in place for other health professions that target private practitioners then it is not unreasonable for private RTs to have those extended to their professions. Existing programs such as the Rural Retention Program for GPs and the Rural Pharmacy Maintenance Allowance/Start up and Succession Allowances are examples from other health professions that could be extended to health professions like RTs. There could also be extensions of the Practice Nurses and/or Allied Health Workers for Urban Areas of Workforce Shortage (which includes the three professions in this survey) to rural areas that make use of private practitioners. Furthermore, the Victorian Government has released a framework for Managed Clinical Networks (MCNs), which are defined as 'interested groups and individuals working across organisations and professions to solve complex problems we couldn't solve on our own, with a focus on clinical variation'30. While there is mention of 'private consultants' in the document this is in the context of the medical profession and not private RTs or other private allied health professions30. The MCNs may be a future path to the development of further partnerships for private RTs in rural areas.
Beyond retention, there are also issues of recruitment for RTs in rural areas. Over half of the respondents (56%, n=36) indicated that they would like to see incentives such as adjusting the EPC program fees for practitioners in rural areas. Private RTs can now treat public patients under Medicare (the state subsidised healthcare scheme), although with access restricted to 5 visits per year. While this requires communication with the medical practitioner who refers, it is not known what effect this has on the viability of private practitioners in rural areas. One of the barriers mentioned by respondents was that many of their clients were of low SES and any adjustment in the rates and number of visits would certainly improve access for those clients.
While some respondents proposed other incentives (such as development grants for setting up new practices, access to salary packaging and various rebates for travel, relocation or accommodation) there were also those who urged caution in the way that such incentives could be accessed and administered. It was suggested that care needed to be taken to ensure that 'outpost clinics' of urban based companies were not established as a means of channelling funding back into urban clinics while sustaining minimal practice in rural areas. Many thought that before any policies for recruitment of new private practitioners were put in place, more should be done to develop policies that assist retention of existing practitioners.
The arguments raised by respondents for support for private practice in rural areas were not based on a model for the 'privatisation' of publicly funded allied health care. Rather they argued for the expansion of public provision of allied health services in rural areas through partnerships with 'private' providers. Their perceived aim is to make more efficient use of resources in the community through sharing. As generators of local economic development, these private practices could call on other government programs that focus on rural development (such as small business development funds or regional development money). Furthermore, as indicated by the survey respondents, many of the business skills learned by private practitioners are valuable not only in the business world, but are also applicable to their professional practice. In this process they not only bring much needed professional and business expertise but also make a major contribution to the social capital of rural towns through their voluntary contributions to local community organisations31.
Limitations
The study has limited focus because it includes only the RT professions of physiotherapy, occupational therapy and speech pathology. Nevertheless, other research indicates that the professions of physiotherapy and occupational therapy are generally found to have a high proportion of private practitioners28. Furthermore, while the number of respondents is relatively small, much of what of they have to say provides a range of responses on both positive and negative aspects of various policy options.
Conclusion
So far much of the contribution of RTs to rural health service, which is supported by enhanced retention rates for private AHPs, has gone comparatively unnoticed. The results of this research indicate that many private RTs in Victoria perceived their greater involvement in the delivery of public health in rural areas in a positive manner. Already there are some private RTs involved in supplying support for the public sector through their partnerships with local public agencies. Since the evidence shows that the retention rate for private AHPs is better than for their colleagues working in the public sector, it would seem appropriate that policy-makers take some note of the perceptions of these RTs.
References
1. Banner G. Community governance and the new central-local relationship. International Social Science Journal 2002; 54(172): 217-231.
2. Cocklin C, Alston M. Community sustainability in rural Australia: a question of capital. Canberra, ACT: Academy of the Social Sciences in Australia, 2003.
3. Everingham C. Reconstituting community: social justice, social order and politics of community. Australian Journal of Social Issues 2001; 36(2): 105-122.
4. Fuller T, Pletsch C. The Community Futures Program in Canada: good governance in successful rural development programming. Guelph, ON: University of Guelph, 2005.
5. Halseth G, Bruce D, Sullivan L. Leading and lagging: the long run role of institutions and social capital in fostering community economic development. In: G Halseth, R Halseth (Eds). Building for success: explorations of rural community and rural development. Brandon: Rural Development Institute, 2004.
6. Howe B, Cleary R. Community building: policy issues and strategies for the Victorian Government. Melbourne, Vic: Centre for Public Policy, University of Melbourne and Anglicare, 2001.
7. Belcher S, Kealey J, Jones J, Humphreys J. The VURHC Rural Allied Health Professionals Recruitment and Retention Study. Melbourne, Vic: VURHC, 2005.
8. Denham LA, Shaddock AJ. Recruitment and retention of rural allied health professionals in developmental disability services in New South Wales. Australian Journal of Rural Health 2004; 12(1): 28-29.
9. Gillham S, Ristevski E. Where do I go from here: we've got enough seniors? Australian Journal of Rural Health 2007; 15(5): 313-320.
10. Knudsen HK, Johnson JA, Roman PM. Retaining counseling staff at substance abuse treatment centers: effects of management practices. Journal of Substance Abuse and Treatment 2003; 24(2): 129-135.
11. Rourke J. Increasing the number of rural physicians. Canadian Medical Association Journal 2008; 178(3): 322-325.
12. Stagnitti K, Schoo A, Reid C, Dunbar J. Retention of allied health professionals in the south-west of Victoria. Australian Journal of Rural Health 2005; 13(6): 364-365.
13. US Department of Health and Human Services. Factors influencing retention and attrition of Alaska community health aides/practitioners: a qualitative study. Anchorage, AK: US Department of Health and Human Services, 2004.
14. Akroyd D, Mulkey W, Utley-Smith Q. The impact of work rewards on radiographers' organizational commitment. Radiological Management 1995; 17(2): 51-68.
15. Collins K, Jones ML, McDonnell A, Read S, Jones R, Cameron A. Do new roles contribute to job satisfaction and retention of staff in nursing and professions allied to medicine? Journal of Nursing Management 2000; 8(1): 3-12.
16. Hughes R. An omnibus survey of the Australian rural health dietetic workforce. Australian Journal of Nutrition & Dietetics 1998; 55(4): 163-169.
17. Kraeger MM, Walker KF. Attrition, burnout, job dissatisfaction and occupational therapy managers. Occupational Therapy Health Care 1993; 8(4): 47-62.
18. Stagnitti K, Schoo A, Dunbar JA, Reid C. An exploration of issues of managment and intention to stay: allied health professionals in South West Victoria, Australia. Journal of Allied Health 2006; 35(4): 226-232.
19. Blue I. Characteristics of Australian rural health care professionals. In: D Wilkinson, I Blue (Eds). The new rural health. Melbourne, Vic: Oxford University Press, 2002; 190-203.
20. Larson A. Health services and workforce. In: D Wilkinson, I Blue (Eds). The new rural health. Melbourne, Vic: Oxford University Press, 2002; 190-203.
21. Humphreys J, Hegney D, Lipscombe J, Gregory G, Chater B. Whither rural health? Reviewing a decade of progress in rural health. Australian Journal of Rural Health 2002; 10(1): 2-14.
22. Southon G. Health service structures, management and professional practice: beyond clinical management. Australian Health Review 1996; 19(1): 2-16.
23. Cuss K. Allied Health Recruitment and Retention Project, Phase 1 report. Wangaratta, Vic: Central Hume Primary Care Partnership, 2005.
24. O'Toole K, Schoo A, Stagnitti K, Cuss K. Rethinking policies for the retention of allied health professionals in rural areas: a social relations approach. Health Policy 2008; 87: 326-332.
25. Wilson R, Lewis S, Murray P. Trends in the rehabilitation therapist workforce in underserved areas: 1980-2000. Journal of Rural Health 2009; 25(1): 26-32.
26. Braun M. Online survey response rates and times. (Online) 2009. Available: http://www.supersurvey.com (Accessed 31 March 2010).
27. Cuss K. Central Hume Allied Health Recruitment and Retention Project interim learnings, evaluation report, directory of services and 12 month strategy plan 2006-2007. Wangaratta, Vic: Central Hume Primary Care Partnership, 2006.
28. Smith T, Cooper R, Brown L, Hemmings R, Greaves J. Profile of the rural allied health workforce in Northern New South Wales and comparison with previous studies. Australian Journal of Rural Health 2008; 16(3): 156-163.
29. Giusti D, Criel B, De Bethune X. Viewpoint: public versus private health care delivery: beyond the slogans. Health Policy and Planning 1997; 12(3): 193-198.
30. Victorian Government Department of Human Services. Clinical networks: a framework for Victoria. Melbourne, Vic: Victorian Department of Human Services, 2008.
31. Reimer B. The rural context of community development in Canada. Journal of Rural and Community Development. 2006; 1(2): 155-175.
______________________


