Introduction
Respiratory illness is a leading cause of death worldwide, with rates that will continue to escalate into the foreseeable future1,2. Rural residents have an increased risk of dying from some forms of respiratory disease, such as chronic obstructive pulmonary disease (COPD), compared with their urban counterparts3. The manner in which individuals interface with the healthcare system can provide insight into the quality of care they receive4-7, although little is known about the healthcare utilization or location of death for persons with advanced respiratory illness. Equitable access to quality healthcare services for rural residents with advanced respiratory illness will require the development of a sound evidence base. The purpose of this study was to examine rural-urban differences in healthcare utilization and location of death for persons with COPD or lung cancer in the last 12 months of life.
Background
Over 4 million people died worldwide as a result of lung disease in 20021 and this number is projected to increase significantly as the impact of illnesses such as COPD and lung cancer continues to increase. In terms of contribution to global health burden, COPD will assume the position of fifth ranked contributor in 20208. Chronic obstructive pulmonary disease is a chronic and progressive respiratory illness, largely the result of smoking, that causes shortness of breath and activity limitation2. Globally and within Canada, rates of smoking in rural areas have consistently been reported to be higher than rates in urban areas9-12, placing rural populations at higher risk for COPD. Patients with advanced COPD typically have significant interface with the healthcare system, averaging between one and 4 exacerbations per year, accounting for a high number of emergency room visits and being at substantial risk of re-admission to hospital and subsequent poor quality of life2,13. Lung cancer remains the most common cancer worldwide, with 1.2 million new cases diagnosed annually and accounting for 17.8% of all cancer deaths14. These data affirm the need to ensure that high quality end of life care is available for all individuals with advanced respiratory disease in the coming years.
Respiratory-related mortality tends to increase with increasing rurality among both men and women3. There were 47 deaths per 100 000 among men aged 45 to 64 years in the most rural areas (no commuters) compared with 33 deaths per 100 000 in urban areas, representing a 42% higher risk of death. However, the age-standardized mortality rate was lowest among men living in areas with moderate commuter flow (28 per 100 000)3, suggesting that the gradient of effect is not stepwise, that is, the most rural and the most urban areas often have higher rates of adverse health effects15. Failure to account for degrees of rurality may explain discrepancies in reports of the relationship between residence and lung cancer, with one study reporting a lower prevalence of lung cancer for rural residents16 and another reporting a higher prevalence for this group3.
While there is increasing recognition of the ability of population-based indicators available from administrative databases to indirectly measure the quality of end of life care for people with cancer4-7, there has been little work undertaken to identify potential quality indicators for those who die from chronic illness such as COPD. Analysis of indicators such as physician visits, hospitalizations, continuity of care measures (such as the number of care transitions between settings) and location of death are helpful in examining patterns of healthcare utilization near the end of life4-6. Location of death has been used as an indicator of quality of end of life care, given that home death is favored by the majority of terminally ill patients, caregivers, health professionals and the general public17-19. Transfers from home to hospital have been considered an indicator of potentially inappropriate care in the last days of life. Recent work examining transfers to hospital at the end of life by Menec and colleagues20 reported that residents of rural and remote regions of Manitoba, Canada, with lower physician availability and fewer hospital beds had an increased risk of being hospitalized, suggesting that some rural and remote regions were disadvantaged in terms of access to appropriate care at the end of life.
In terms of overall healthcare access and utilization by rural residents, much of the research is inconclusive21. A number of studies have found no differences between rural and urban residents in use of physician services, hospitalization rates22,23, unmet healthcare needs, number of days required to obtain appointments24. Rural residents were more likely than those in urban areas to have a usual source of primary care, but reported fewer visits to healthcare providers25. Fewer home care days were provided to residents of remote areas than metropolitan and other nonmetropolitan locations26.
Laditka and colleagues27 reported that increasing levels of rurality may be positively associated with hospitalizations for ambulatory-care sensitive conditions (ACSC) and concluded this may represent rural-urban disparities in access to primary health care. The ACSC are conditions, including COPD, can be potentially managed and controlled in community settings, possibly avoiding hospital admission28. Hospital admission rates for COPD in Australia were found to be higher in rural than metropolitan areas and were associated with socioeconomic status, smoking rates and remoteness of the area29. The concept of 'distance decay', or decreasing utilization of health services with increasing distance of patients from hospital, may be useful in analysis of healthcare use30.
The purpose of this study was to examine rural-urban differences in healthcare utilization and location of death for persons with COPD or lung cancer in the last 12 months of life using administrative health data.
Methods
Study population and design
This retrospective study within the province of Saskatchewan, Canada (approximately 1 000 000 population) used Saskatchewan Health administrative databases to identify subjects who had either lung cancer (ICD-10 code C34.x) as the underlying cause of death (UCOD) or COPD (ICD-10 code J44.x) as either the UCOD or multiple cause of death (MCOD) and died in 2004. The index date was the date of death. Data related to home care, institutional care, outpatient physician visits, and hospitalizations as well as potential confounders were obtained from the Saskatchewan Health databases. These comprehensive databases31 have been used successfully to conduct large previous epidemiological studies of respiratory health32-34. This study was approved by the University of Saskatchewan Biomedical Research Ethics Board.
Saskatchewan Health databases
Universal health care is provided by Saskatchewan Health to the majority of Saskatchewan residents (approximately 99%) with exceptions being persons insured by the federal government (federal inmates, Royal Canadian Mounted Police and Canadian Forces personnel). The provincial drug plan does not cover Registered Indians, because they receive prescription drug benefits from the federal government, so this population has been excluded from the present study.
Unique identifiers for each individual covered by Saskatchewan Health can be used to link the various databases. Prior to receiving the data from Saskatchewan Health, the unique identifier was de-identified. Saskatchewan Health provided the following databases: subject file, physician services file, physician visits file, hospital services file, home care file, institutional supportive care file and the vital statistics death file.
The subject file contains information regarding demographic variables including sex, year of birth, marital status, area of residence and dates of coverage. The physician services file includes dates of all physician services and fee-for-service codes (FSCs) for FSCs of interest, while the physician visits file includes the date of the visit, diagnosis, location of service and the approved payment amount for a visit. Dates of admission and discharge, diagnoses and diagnoses types, and procedures of interest undertaken during hospitalization are contained within the hospitalization services file.
The home care file includes dates of admission to and discharge from home care, months eligible for services, amount of time spent on specific types of home care duties and costs associated with home care. The definitions of home care were taken from the home care file (Fig1). Although healthcare coverage is considered universal, clients do pay fees for home care services. Saskatchewan home care clients paid user fees of $6.25-$6.36 per service for the first 10 units of services per month in 2004, with the remainder of fees assessed based on income to an annual maximum of $375-38335. No fee for home care services is charged to clients receiving palliative care.

Figure 1: Definitions of home care services.
The institutional supportive care home file includes dates of admission and discharge, program (long term care [LTC], temporary care), purpose of temporary care, level of care and type of facility. Funding to cover approximately 77% of overall LTC costs is provided by Saskatchewan Health, although an income-tested resident charge is applied36. Finally, the vital statistics file includes the date of death, UCOD and MCODs as well as the decedent's residence at the time of death (rural or urban). The independent variable of primary interest was the three-level variable indicating rural/remote (≤9999 population size), small urban (10 000-99 999) or urban (≥100,000) where the urban group was considered the reference group.
Statistical analysis
Prior to analysis, several variables including the number of physician visits, number of hospitalizations and hospitalization length of stay (LOS) were categorized because of a skewed distribution. These variables were dichotomized based on evidence from the literature37 and medians calculated from the present data. The number of physician visits were classified as >24 visits or ≤24 visits in the year representing an average of 2 outpatient visits per month. The number of hospitalizations was categorized as >2 or ≤2 hospitalizations in a year while the mean LOS was categorized as >7 days or ≤7 days representing a full week in hospital. Because it is well-recognized that comorbidities such as cardiovascular disease are often listed on death certificates as the primary cause of death for those with advanced COPD38, UCOD categories included lung cancer, COPD, cardiovascular disease and other conditions, comorbid conditions were classified based on the number of conditions as >1 or ≤1 based on the presence or absence of disease conditions included in the UCOD or MCOD. The number of transfers (discharge from one healthcare institution and same day admission to another) between healthcare settings as classified as <5 or ≥5.
Statistical analysis was completed using SPSS 16.0 (SPSS Inc; Chicago, IL, USA; www.spss.com), with the level of significance (σ) set at 0.05. Descriptive analyses included reporting the mean and standard deviations (SD), medians and inter-quartile range (IQR), and counts and proportions where appropriate. Comparisons between the three groups in terms of demographics and healthcare utilization were completed using analysis of variance (ANOVA) with Scheffe post-hoc tests and χ2 tests of proportion where appropriate. In situations where the assumptions for these tests were not met, the Kruskal Wallis test (with multiple Mann-Whitney tests adjusted with Bonferroni corrections for post hoc analysis) and Fisher's exact tests were used, respectively.
Associations between residence and specific healthcare utilization outcomes were assessed using multivariate logistic regression. The strength of association was measured by the odds ratio (OR) and 95% confidence intervals (CI). Healthcare utilization outcomes of interest included the following binary variables (yes/no): >24 physician visits, any hospitalization, any institutional care, any long term institutional care, any temporary institutional care, any home care, home care services for previous 12 months, palliative home care, 5 or more transitions between care settings, hospital as place of death, LTC institution as place of death, home as place of death, and length of stay (LOS). Interaction terms of clinical importance were assessed and when significant, a stratified analysis was completed.
Results
De-identified data were obtained for 1098 beneficiaries of Saskatchewan Health eligible for prescription drug benefits who had been identified as having either lung cancer (n=483) as their UCOD or COPD (n=615) as their UCOD or MCOD cause of death. Chronic obstructive pulmonary disease was identified as the UCOD for 287 persons (47.7%). Sixty-three decedents had diagnoses of both lung cancer and COPD, leaving 433 with lung cancer only and 602 with COPD only. All cases are reported in this article.
The average age of decedents was 77 years (SD=11 years) and just over half (57%) were male. Most of the population were married or lived common-law (45.5%) and had more than one comorbid condition (52.2%). All decedents with lung cancer had this diagnosis as their UCOD, while the decedents who died with a diagnosis of COPD had UCODs attributed to COPD, cardiovascular disease or another diagnosis. Demographic characteristics, underlying cause of death and number of comorbid conditions were similar between urban, small urban and rural/remote groups (Table 1).
In terms of healthcare utilization in the year prior to death, a number of statistically significant differences among urban, small urban and rural/remote groups emerged (Table 2). Higher proportions of urban residents had 24 or more physician visits within the past 12 months, compared with both small urban and rural/remote counterparts, although urban residents made less use of temporary care than the other groups. While the proportions of persons receiving any home care were similar between the areas of residence in the crude analysis, decedents in rural/remote areas received proportionately more home care of a year's duration than either urban or small urban groups. The number of care transitions between healthcare settings and the place of death were similar for urban, small urban and rural/remote decedents. Hospitals were the most common location of death across all three groups. Home deaths accounted for less than one-fifth of all deaths and were consistent between the groups.
Table 3 provides the bivariate analyses of the specific home care services received by decedents in each of the areas of residence. Significantly higher proportions of urban residents received palliative home care and physiotherapy services than either small urban or rural/remote residents, while significantly lower proportions of urban residents received supportive services and meal preparation than rural/remote residents. Personal nursing service was received by very few urban residents in comparison to either semi-urban or rural/remote residents.
After adjustment for UCOD, age group, sex, marital status, and comorbidity (Table 4), urban, small urban and rural/remote residents were comparable in terms of the likelihood of: any hospitalizations, having had 5 or more transfers between settings, and dying in hospital. Urban residents were more likely to have had 24 or more physician visits in the last year of life compared with small urban (OR=0.52, 95% CI=.37-.74) or rural/remote residents (OR=0.52, 95% CI=.40-.69), while rural/remote residents were more likely to have received any institutional LTC (OR=1.40, 95% CI=1.03-1.90) than the other groups.
Table 1: Demographic characteristics, underlying cause of death and comorbidity by area of residence (percentage)
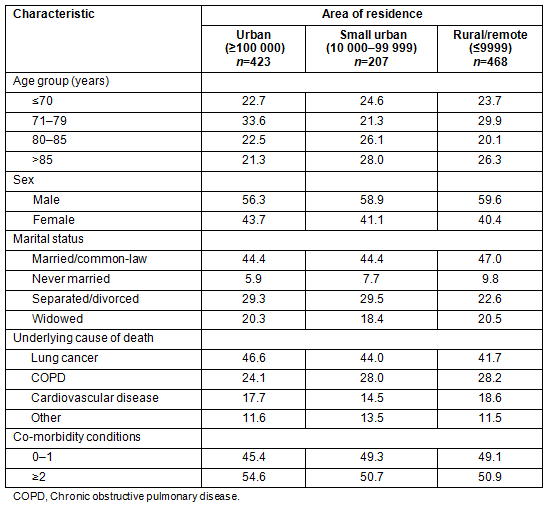
Table 2: Healthcare utilization in the last year of life by area of residence
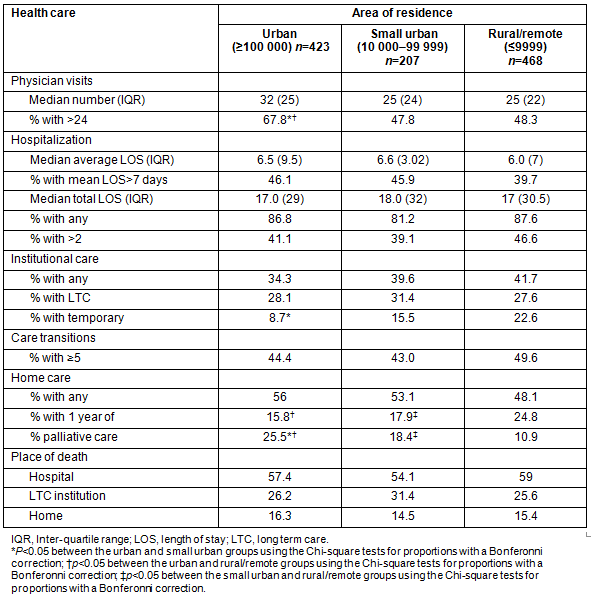
Table 3: Receipt of specific home care services in the last year of life by area of residence
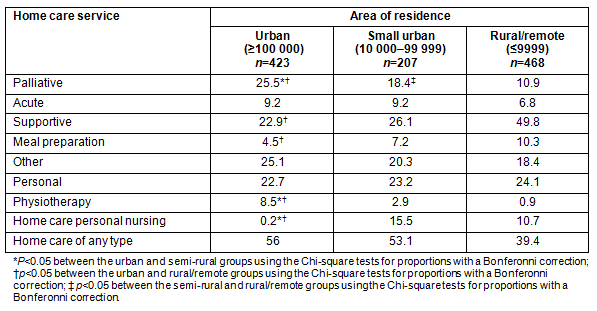
Table 4: Multivariate? analysis examining associations between demographic characteristics, underlying cause of death and comorbidity with physician visits, hospitalization and institutional care (n=1098)
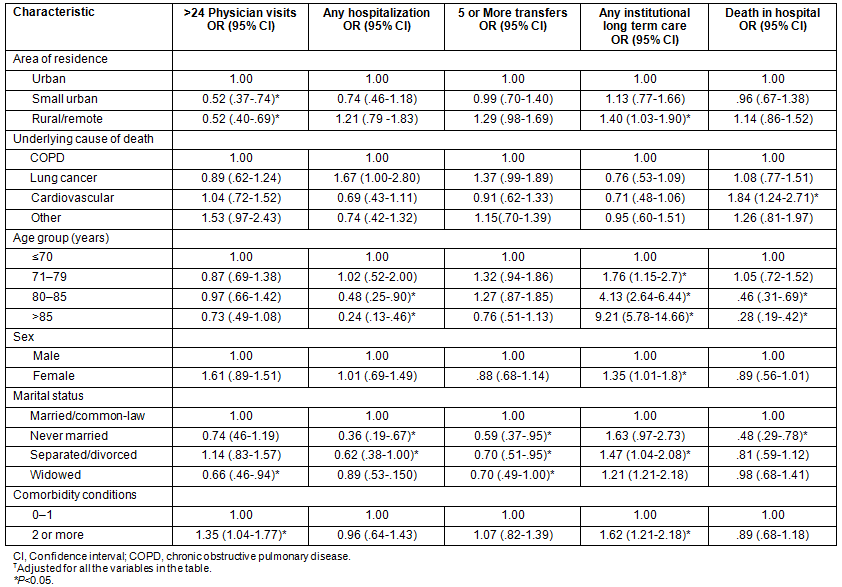
Hospital as a location of death was more likely for those with a UCOD of cardiovascular disease (OR=1.84, 95% CI=1.24-2.71), but was less likely for those aged 80-85 years (OR=0.46, 95% CI=.31-.69), those aged more than 85 years (OR=0.28, 95% CI=.19-.42) and those who had never married (OR=0.48, 95% CI=.29-.78).
Marital status appeared to exert a substantial and independent effect on several types of healthcare utilization. Widowed persons were less likely to have had 24 or more physician visits in the previous 12 months (OR=0.66, 95% CI=.46-.94), while persons who had never married (OR=0.36, 95% CI=.19-.67) or were separated/divorced (OR=0.62, 95% CI=.38-1.00) were less likely to have had any hospitalizations. Married persons had a higher likelihood of having had 5 or more care transitions between settings in the preceding 12 months than any of the other marital status groups. Separated/divorced persons were more likely to have had any institutional long-term care in the previous year (OR=1.47, 95% CI=1.04-2.08) than persons in the other marital status categories, while persons who had never married were much less likely to die in a hospital setting (OR=0.48, 95% CI=.29-.78).
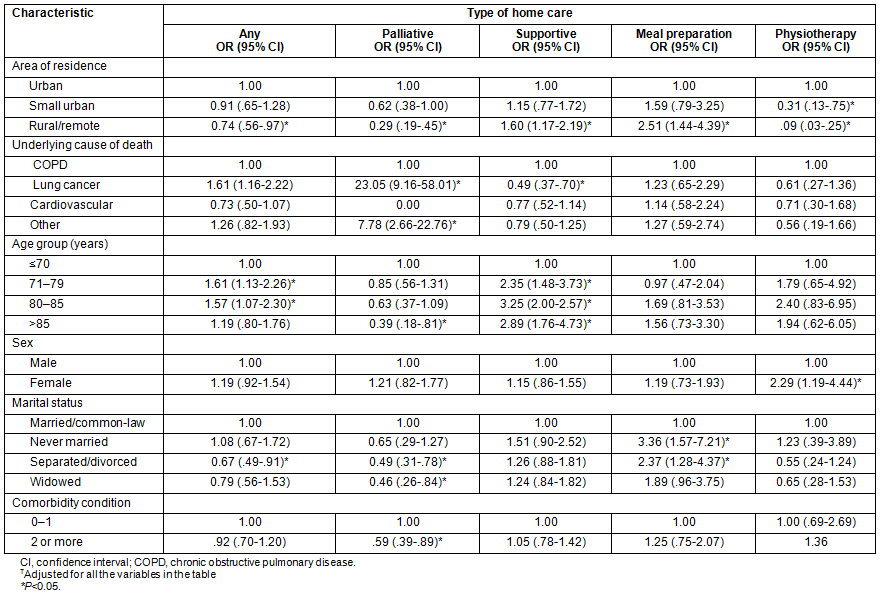
Multivariate analysis was also conducted to examine the associations with type of home care received (Table 5). Residents of rural/remote areas were significantly less likely than those in urban or small urban settings to receive any home care (OR=0.74, 95% CI=0.56-0.97), any home palliative care (OR=0.29, 95% CI=0.19-0.45) or home physiotherapy services (OR=0.09, 95% CI=0.03-0.25). Rural/remote residents were, however, much more likely to receive home supportive care (OR=1.60, 95% CI=1.17-2.19) and home meal preparation (OR=2.51, 95% CI=1.44-4.39).
Table 5: Multivariate? analysis examining associations between demographic characteristics, comorbidity and underlying cause of death with types of home care (n=1098)
Discussion
Our findings demonstrate a number of key differences in health service utilization in the last year of life between persons with respiratory illness living in rural/remote, small urban and urban areas, particularly in terms of physician visits and home care services. Place of death, hospitalizations, and number of care transitions were comparable between the groups.
Hospitals were the place of death for the majority of decedents, regardless of rurality. Only 14.5%-16.3% of all deaths within this study occurred at home, which are lower proportions of home deaths than the 24.3% reported in Flanders39 and 22% in the US40. Given that rural hospitals are often located a significant distance from the patient's home, families of rural residents who die in a hospital may experience a disproportionate burden compared with families in urban settings. Rural families may need to relocate and live in temporary accommodation close to the hospital (often for a protracted period of time) and may experience associated financial burden of accommodations and lost employment income. In addition, the absence of usual social supports in this new environment can represent significant hardships to the families of rural patients who are dying.
Persons residing in rural/remote and small urban settings were significantly less likely than those in urban areas to have a high number of physician visits (24 or more over 12 months), in spite of the fact that their healthcare needs during the last year of life were likely quite similar. There may be several possibilities that help to account for the difference in number of physician visits. One may be Laditka and colleagues'27 assertion that there is a disparity between rural and urban settings in terms of the primary care services available. A second possibility is that there is a differential perception of need and a reduced expectation for primary care among rural residents41,42. Higher levels of community support in rural settings43,44 and rural residents' personal traits of self-reliance and independence45 may also have played a role in reducing the number of physician visits. Access may also be influenced by the ability of older, sicker people to get to the physician, depending on their degree of isolation.
The likelihood of receiving home care, and in particular, specialized services such as palliative care or physiotherapy, was significantly lower for persons in rural/remote areas. Because non-professional home care services such as supportive care and meal preparation were used by a much higher proportion of rural/remote residents compared with small urban and urban residents, proximity to providers per se does not appear to be the primary limiting factor. Physiotherapists and palliative care specialists did not appear to be widely available in the rural/remote areas. Interestingly, urban residents had a much lower likelihood of receiving personal care from a professional nurse than residents in the other two settings. The reason underlying this resource allocation discrepancy between settings is not clear, although it can be speculated that it is the result of distance. Nurses may have been more proximate to clients requiring personal care than non-professional staff and were thus assigned to provide this care. Difficulty recruiting and retaining professional healthcare providers has been a key barrier to delivery of quality palliative care in rural areas noted internationally46,47. Future mixed methods research might examine whether there are differences in the quality of end of life care or subjective perceptions of unmet needs between rural/remote and other settings given the variation in physician visits and differing nature of home care service provided.
Lengths of stay in hospital, number of hospitalizations, number of transfers and location of death were similar across rural/remote, semi-urban and urban settings, suggesting some similarity in end of life care management approaches for respiratory patients with advanced illness. More than half of the deaths of persons with respiratory illness still occurred in hospitals, regardless of area of residence, suggesting there may be quality improvement opportunities in facilitating desired home deaths in all settings. The burden on families that is associated with hospital death may be more onerous than that experienced by urban families who are geographically closer to the hospital. Similarly, close to half of the decedents underwent 5 or more care setting transitions in the last 12 months of life. In the absence of contextual data, these transitions may have been appropriate, although the risks previously discussed bear consideration. Our findings did not support the notion of 'distance decay', in which there is decreasing utilization of health services with increasing distance of patients from hospital.
Strengths and limitations
The strengths of this study included access to 12 months of healthcare data for an entire cohort of decedents in a geographically large and diverse province in 2004, including acute care and home care. The data includes a relatively large number of rural residents. The dataset was robust, with little missing data, and captured care that occurred across multiple settings, thus reflecting the broad nature of treatments provided and care received.
The constraints inherent in using an administrative database, such as potential inaccuracy of coding and lack of contextual detail, were a limitation of this study. The administrative data represent one Canadian province only and regional variation in practice may affect the generalizability of the findings. Further, the data analyzed in this report did not allow for assessment of the quality of life, or the appropriateness and adequacy of care for those who died with respiratory illness.
Conclusion
For persons with respiratory illness in the last year of life, rural-urban differences were apparent in the number of primary care physician visits and in access to and nature of home care services provided. Significantly fewer physician visits were made by residents of small urban or rural remote locations compared with those in urban settings, although additional research is needed to determine the reasons for this discrepancy. From a health systems perspective, the discrepancy in number of physician visits between locations suggests the need to compare health outcomes and patient satisfaction with care between the groups. For example, if outcomes were similar, perhaps fewer physician visits but additional supports for patients at the end of life might result in both cost savings and increased satisfaction.
The likelihood of receiving home care services and specialized home care services such as palliative care and physiotherapy were significantly lower for persons in rural/remote locations. The reduced ability to support patients in their homes may have led to the increased likelihood of admission to institutional LTC noted for the rural remote residents compared with urban and small urban groups.
Novel uses of innovative technologies by specialist home care providers need to be investigated to ensure that care at the end of life is equitable for persons dying with respiratory illness in rural/remote areas. This may include designing healthcare services in such a way as to maximize their efficiency and reach in rural areas, and making greater use of telehealth technology. Further investigation of issues related to differences in quality of care and unmet healthcare needs between rural and non-rural settings will strengthen the evidence base to improve care at the end of life.
Acknowledgements
This project was funded by a Saskatchewan Health Research Foundation New Investigator Establishment Grant awarded to Donna Goodridge. Dr Marciniuk is the recipient of a Lung Association of Saskatchewan Professorship. The authors gratefully acknowledge the assistance of Mary Rose Stang, Analyst, Saskatchewan Ministry of Health. This study is based in part on de-identified data provided by the Saskatchewan Ministry of Health. The interpretation and conclusions contained herein do not necessarily represent those of the Government of Saskatchewan or the Saskatchewan Ministry of Health.
References
1. Yach D, Hawkes C, Gould CL, Hofman KJ. The global burden of chronic diseases: overcoming impediments to prevention and control. JAMA 2004; 291: 2616-2622.
2. O'Donnell DE, Aaron S, Bourbeau J, Hernandez P, Marciniuk D, Balter M et al. State of the art compendium: Canadian Thoracic Society recommendations for the management of chronic obstructive pulmonary disease. Canadian Respiratory Journal 2004; 11 (Suppl B): 7B-59B.
3. Canadian Institute for Health Information. How healthy are rural Canadians? An assessment of their health status and health determinants. Ottawa, ON: Government of Canada, 2006.
4. Earle CC, Park ER, Lai B. Identifying potential indicators of the quality of end-of-life cancer care from administrative data. Journal of Clinical Oncology 2003; 21: 1133-1138.
5. Grunfeld E, Lethbridge L, Dewar R, Lawson B, Johnston G, Burge F et al. Towards using administrative databases to measure population-based indicators of quality end-of-life care: testing the methodology. Palliative Medicine 2005; 20: 769-777.
6. Barbera L, Paszat L, Chartier C. Indicators of poor quality end-of-life cancer care in Ontario. Journal of Palliative Care 2005; 22: 12-17.
7. Grande GE, McKerral A, Addington-Hall JM, Todd CJ. Place of death and use of health services in the last year of life. Journal of Palliative Care 2003; 19: 163-270.
8. Lopez AD, Murray CCJL. The global burden of disease, 1990-2020. Nature and Medicine 1998; 4: 1241-1243.
9. Statistics Canada. Fact sheet on smoking. (Online) 2009. Available: http://www.statcan.gc.ca/pub/82-221-x/2009001/tblstructure/2nm/2hb/hb2tos-eng.htm (Accessed 15 February 2010).
10. Gikas A. Urban-rural differences in smoking prevalence in Greece. European Journal of Public Health 2007; 17(4): 402.
11. Chow CK, Raju K, Raju R, Celermajer DM, Neal BC. Tobacco use and predictors of high smoking rates in rural Andra Pradesh, India. Heart, Lung and Circulation 2007; 16(Suppl 2): S60-61.
12. Yang T, Li F, Yang X, Wu Z, Feng X, Wang Y et al. Smoking patterns and sociodemographic factors associated with tobacco using among Chinese rural male residents: a descriptive analysis. BMC Public Health 2008; 8: 248.
13. Wang Q, Bourbeau J. Outcomes and health-related quality of life following hospitalization for acute exacerbation of COPD. Respirology 2005; 10(3): 334-340.
14. World Health Organization. Global cancer rates could increase by 50% to 15 million by 2020. (Online) 2010. Available: http://www.who.int/mediacentre/news/releases/2003/pr27/en/ (Accessed 5 August 2009).
15. Eberhardt MS, Pamuk ER. The importance of place of residence: examining health in rural and nonrural areas. American Journal of Public Health 2004; 94: 1682-1685.
16. Office for National Statistics. Deaths from lung cancer lower in rural areas. Health Statistics Quarterly (Online) 2010. Available: www.statistics.gov.uk/pdfdir/urmort0808.pdf (Accessed 5 August 2009).
17. Fried TR, Pollack DM, Drickamer MA, Tinetti ME. Who dies at home? Determinants of site of death for community-based long-term care patients. Journal of the American Geriatrics Society 1999; 47: 25-29.
18. De Conno F, Caraceni A, Groff L, Brunelli C, Donate I, Tamburini M et al. Effect of home care on the place of death of advanced cancer patients. European Journal of Cancer 1996; 32A: 1142-1147.
19. Brazil K, Howell D, Bedard M, Krueger P, Heidebrecht C. Preferences for place of care and place of death among informal caregivers of the terminally ill. Palliative Medicine 2005; 19: 492-499.
20. Menec VH, Nowicki S, Kalischuk A. Transfers to acute care hospitals at the end of life: do rural/remote regions differ from urban regions? Rural and Remote Health 10: 1281. (Online) 2010. Available: www.rrh.org.au (Accessed 23 March 2010).
21. Institute of Medicine. Quality through collaboration: the future of rural health. Washington, DC: National Academies Press, 2005.
22. Himes CL, Rutrough TS. Difference in the use of health services by metropolitan and nonmetropolitan elderly. Journal of Rural Health 1994: 10: 80-88.
23. McConnel CE, Zetzman MR. Urban-rural differences in health service utilization by elderly persons in the United States. Journal Rural Health 1993; 9: 270-280.
24. Reschovsky JD, Staiti AB. Access and quality: does rural America lag behind? Health Affairs (Millwood) 2005; 24: 1128-1139.
25. Larson SL, Fleishman JA. Rural-urban differences in usual source of care and ambulatory service use. Medical Care 2003; 41(Suppl7): III65-III74.
26. McAuley WJ, Spector W, Van Nostrand J. Formal home care utilization patterns by rural-urban community residence. Journal of Gerontology and Social Science 2009; 64B: 258-268.
27. Laditka JN, Laditka SB, Probst JC. Health care access in rural areas: evidence that hospitalization for ambulatory-case sensitive conditions in the United States may increase with the level of rurality. Health and Place 2009; 15: 731-740.
28. Canadian Institute for Health Information. Health indicators 2008. Ottawa, ON: CIHI, 2008.
29. Ansari A, Dunt D, Darmage SC. Variations in hospitalizations for chronic obstructive pulmonary disease in rural and urban Victoria, Australia. Respirology 2007; 12: 874-880.
30. Mungall IJ. Trend towards centralization of hospital services and its effect on access to care for rural and remote communities in the UK. Rural and Remote Health 5: 390. (Online) 2005. Available: www.rrh.org.au (Accessed 23 March 2010).
31. Downey W, Stang MR, Beck P, Osei W, Nichol J. Health services databases in Saskatchewan. In: BL Strom (Ed.). Pharmacoepidemiology, 4th edn. Chichester: John Wiley & Sons, 2005; 295-310.
32. Senthilselvan A, Lawson JA, Rennie DC, Dosman JA. Stabilization of an increasing trend in physician-diagnosed asthma prevalence in Saskatchewan, 1991-1998. Chest 2003; 124: 438-448.
33. Suissa S, Ernst P, Benayoun S, Baltzan M, Cai B. Low-dose inhaled corticosteroids and the prevention of death from asthma. New England Journal of Medicine 2000; 343(5): 332-336.
34. Spitzer W, Suissa S, Ernst P, Horwitz RI, Habbick B, Cockcroft D et al. The use of beta-agonists and the risk of death and near death from asthma. New England Journal of Medicine 1992; 326(8): 501-506.
35. Hollander M. Saskatchewan Health, Community Care Branch Home Care program review. Victoria, BC: Hollander Analytical Services, 2006.
36. Marchildon G, O'Fee K. Health care in Saskatchewan: an analytical profile. Regina, SK: Saskatchewan Institute of Public Policy, 2007.
37. Dy SM, Wolff JL, Frick KD. Patient characteristics and end-of-life health care utilization among Medicare beneficiaries in 1989 and 1999. Medical Care 2007; 45: 926-930.
38. Jensen HH, Godtfredsen NS, Lange P, Vestbo J. Potential misclassification of causes of death from COPD. European Respiratory Journal 2006; 28: 781-785.
39. Cohen J, Bilsen J, Hooft P, Deboosere P, van der Wal G, Deliens L. Dying at home or in an institution: using death certificates to explore factors associated with place of death. Health Policy 2006; 319: 319-329.
40. Flory J, Young-Xu Y, Gurol I, Levinsky N, Ash A, Emanuel E. Place of death: U.S. trends since 1980. Health Affairs 2004; 24: 194-200.
41. Mayer ML, Slifkin RT, Skinner AC. The effects of rural residence and other social vulnerabilities on subjective measures of unmet need. Medical Care Research Review 2005; 62: :617-628.
42. Strickland J, Strickland DL. Barriers to preventive health services for minority households in the rural South. Journal of Rural Health 1996; 12: 206-217.
43. Mueller KJ, MacKinney AC. Care across the continuum: access to health care services in rural America. Journal of Rural Health 2006; 22: 43-49.
44. Goodridge D, Duggleby W. Using a quality framework to assess rural palliative care. Journal of Palliative Care 2010; 26(3): (in press).
45. Long KA, Weinert C. Rural nursing: developing the theory base. Scholarly Inquiry for Nursing Practice 1999; 13: 257-269.
46. Evans R, Stone D, Elwyn G. Organizing palliative care for rural populations: a systematic review of the evidence. Family Practice 2003; 20: 304-310.
47. Wilson DM, Justice C, Sheps S, Thomas R, Reid P, Leibovici K. Planning and providing end-of-life care in rural areas. Journal of Rural Health 2006; 22: 174-181.

