Context
Introduction
Australia is considered one of the 'safest countries in the world in which to give birth or be born' (p.3)1. However, there are wide disparities in maternal infant health (MIH) outcomes for Aboriginal and Torres Strait Islander Australians and women in remote and rural areas of Australia when compared with other Australians. There are many contributing factors including: the enduring effects of colonisation, a higher burden of disease, and poverty reflected in poor housing, lack of employment and reduced access to services. This article reviews current services, national initiatives and international examples and proposes strategies to address the disparities. It is argued that strategies to address MIH in other comparable countries, particularly where Indigenous populations have also suffered from colonisation, should be applied in Australia. Specifically we argue for a greater recognition of the public health role of midwifery, and changing the way midwives work to enable 'birthing on country' for Indigenous women. Successful Inuit models have incorporated traditional knowledge and onsite midwifery training and have shown extraordinary results. This article also argues for an increased emphasis on the collection, analysis and reporting of maternal deaths in Australia to have more accurate reporting of the maternal mortality ratio (MMR).
Primary maternity services
Australia has committed to extending and enhancing Primary Maternity Services as the 'preferred approach to providing pregnancy and birthing services to women with uncomplicated pregnancies'(p.1)2. Primary maternity services include antenatal, birth and postnatal care for women with low-risk pregnancies. The safety and effectiveness of these services relies on them having networks with timely referral to, and treatment in, secondary and tertiary services, if required. The provision of culturally appropriate care as close to home as possible is also now supported by government2. This is a significant shift in direction for Australia. The logistics of how and where these services will be established and supported are currently being debated.
National reforms
The healthcare reform agenda of the current Australian National Government has a strong emphasis on community based services, primary care and improving care for rural and remote areas and Indigenous communities (Closing the Gap, National Health and Hospitals Reform Commission, Primary Maternity Services in Australia: A Framework for Implementation and the Report of the Maternity Services Review. One resultant initiative will promote a much stronger community profile for midwives by enabling 'eligible' midwives access to Medicare Benefits Scheme (MBS) and the Pharmaceutical Benefits Scheme.
These Government initiatives present an opportunity to increase midwifery services with a new funding stream to rural and remote areas where health expenditure has never equalled urban areas nor matched the need3. However, the current eligibility criteria has the potential to make the Medicare reforms unworkable. Of particular concern is the successful lobbying from the Australian Medical Association (AMA) for Medicare registered midwives to have 'collaborative arrangements' with one or more named medical practitioners. The combination of an extraordinary turnover of doctors in some settings (locums may relieve for as little as 2 weeks); doctors' fear of being held responsible for midwives' practice and resistance to a perceived expanded role for midwives from the AMA and some rural doctors organisations could jeopardise the workability of this reform. We propose a flexible model where midwives can consult and transfer to any maternity service, thus reducing the risk of delay to care when needed (detailed below and similar to the model in many Canadian provinces) (Fig1).
 Figure 1: A workforce model for primary maternity services in rural and remote areas, reproduced with permission S Kildea and C Cliffe.
There are a number of issues that currently influence the delivery of maternity services and the experiences of women accessing the services in Australia. These issues will now be outlined with recommendations provided to each issue.
Issues
Issue 1: Measuring progress
Maternal mortality is commonly used as an indicator of a country's development status and as a measurement of the safety and quality of maternity services. The relative safety of birth in Australia has fostered a shift in reporting, from survival, to other indicators such as interventions in birth and fetal outcomes4. Our latest triennial Maternal Deaths Report (2003-2005) announced a considerable drop in deaths with the MMR reported to have reduced from 84 (11.1 per 100 000) in the previous triennium to 65 (8.4 per 100 000)5. However, maternal mortality data are poorly collected, reported and analysed in Australia6. Each state and territory does this differently with some jurisdictions lacking formal committees and review processes. Additionally, in the 2003-2005 report there was no reported validation of data from the Australian Bureau of Statistics Mortality Database or the National Hospital Morbidity Database5. When this validation occurred in 2000-2002 an extra 18 deaths were found. If a similar number were underreported in 2003-2005 then the number of deaths would have been almost the same. Thus in this article we have used the 2000-2002 report as a more reliable source of data. Legislative changes and targeted funding are required in Australia to allow robust, non-punitive processes to be implemented such as the Confidential Enquiries in the United Kingdom (Recommendation 1) (Table 1). At a minimum, the data must be validated prior to publication.
Table 1: Policy, practice and research recommendations to advance Closing the Gap in Australia, based on the synthesis of current literature and research presented in this article
Figure 1: A workforce model for primary maternity services in rural and remote areas, reproduced with permission S Kildea and C Cliffe.
There are a number of issues that currently influence the delivery of maternity services and the experiences of women accessing the services in Australia. These issues will now be outlined with recommendations provided to each issue.
Issues
Issue 1: Measuring progress
Maternal mortality is commonly used as an indicator of a country's development status and as a measurement of the safety and quality of maternity services. The relative safety of birth in Australia has fostered a shift in reporting, from survival, to other indicators such as interventions in birth and fetal outcomes4. Our latest triennial Maternal Deaths Report (2003-2005) announced a considerable drop in deaths with the MMR reported to have reduced from 84 (11.1 per 100 000) in the previous triennium to 65 (8.4 per 100 000)5. However, maternal mortality data are poorly collected, reported and analysed in Australia6. Each state and territory does this differently with some jurisdictions lacking formal committees and review processes. Additionally, in the 2003-2005 report there was no reported validation of data from the Australian Bureau of Statistics Mortality Database or the National Hospital Morbidity Database5. When this validation occurred in 2000-2002 an extra 18 deaths were found. If a similar number were underreported in 2003-2005 then the number of deaths would have been almost the same. Thus in this article we have used the 2000-2002 report as a more reliable source of data. Legislative changes and targeted funding are required in Australia to allow robust, non-punitive processes to be implemented such as the Confidential Enquiries in the United Kingdom (Recommendation 1) (Table 1). At a minimum, the data must be validated prior to publication.
Table 1: Policy, practice and research recommendations to advance Closing the Gap in Australia, based on the synthesis of current literature and research presented in this article
 Issue 2: Australian maternal infant health outcomes
The following statistics highlight the enormous disparity between Aboriginal and Torres Strait Islander and non-Indigenous health outcomes, and build a case for doing things differently in Australia. In 2000-2002, the MMR for Aboriginal and Torres Strait Islander women was 5.3 times greater than other Australian women: 45.9 versus 8.7/100 0007. It is possible that this is an undercount as 27% of cases did not record Indigenous status. This rate of death is greater than both Sri Lanka (19/100 000) and Malaysia (18/100 000)(Fig2), two countries that have strived to ensure locally based skilled attendant care at the primary care level and successfully and dramatically reduced their MMR in consecutive years8.
Issue 2: Australian maternal infant health outcomes
The following statistics highlight the enormous disparity between Aboriginal and Torres Strait Islander and non-Indigenous health outcomes, and build a case for doing things differently in Australia. In 2000-2002, the MMR for Aboriginal and Torres Strait Islander women was 5.3 times greater than other Australian women: 45.9 versus 8.7/100 0007. It is possible that this is an undercount as 27% of cases did not record Indigenous status. This rate of death is greater than both Sri Lanka (19/100 000) and Malaysia (18/100 000)(Fig2), two countries that have strived to ensure locally based skilled attendant care at the primary care level and successfully and dramatically reduced their MMR in consecutive years8.
 Figure 2: Maternal deaths per 100 000.
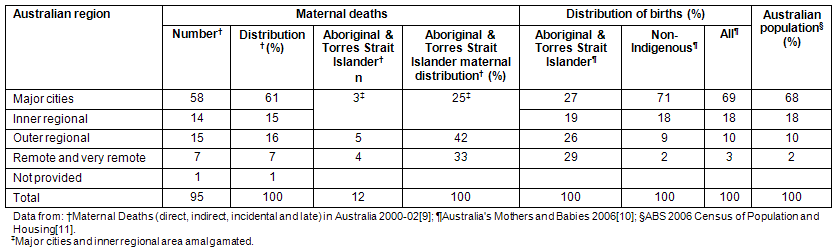
Although there is no demonstrated causal pathway and the numbers are small, Table 2 shows that the proportion of maternal deaths to women who were resident in remote areas (7%) was higher than the proportion of women who gave birth from these areas (3%). Outer regional Australia accounted for 16% of maternal deaths and 10% of births. It can also be seen that 29% of Aboriginal and Torres Strait Islander births are to women living in remote and very remote areas compared with 2% of non-Indigenous births.
Table 2: Distribution of births and maternal deaths in Australia by remoteness area of usual residence and Indigenous status9-11
Figure 2: Maternal deaths per 100 000.
Although there is no demonstrated causal pathway and the numbers are small, Table 2 shows that the proportion of maternal deaths to women who were resident in remote areas (7%) was higher than the proportion of women who gave birth from these areas (3%). Outer regional Australia accounted for 16% of maternal deaths and 10% of births. It can also be seen that 29% of Aboriginal and Torres Strait Islander births are to women living in remote and very remote areas compared with 2% of non-Indigenous births.
Table 2: Distribution of births and maternal deaths in Australia by remoteness area of usual residence and Indigenous status9-11
 Perinatal mortality rates are also considerably higher for Aboriginal and Torres Strait Islander babies (2-3 times) compared with non-Indigenous Australians12, with double the percent of low birth weight infants (13.2% vs 6.1%) and preterm births (13.9% vs 7.9%)13 (based on the 2005 report because this was the most comprehensive available data). Families from rural and remote areas experience higher rates of fetal and neonatal deaths (1.5-2.9)14.Research and trend data in Western Australia, however, shows increasing disparity in recent years in the infant mortality rate (RR: 4.4) for Aboriginal women compared with non-Aboriginal women, with higher rates in remote areas and teenage mothers under 16 years15. Research in Queensland and Western Australia has identified that the majority of perinatal deaths are due to antenatal factors16 and significantly more potentially preventable deaths in Aboriginal infants are due to infection, preterm birth and sudden infant death syndrome15. These are all amenable to targeted interventions with the Queensland study recommending primary healthcare initiatives to reduce the prevalence of low birth weight and preterm birth and a public health approach inclusive of a domestic violence focus16.
'Close the Gap' campaign: In 2007/2008 the Council of Australian Governments (COAG) committed to 'Overcoming Indigenous Disadvantage' setting six targets with a regular reporting framework against key indicators17. Indicators relating to maternity services include antenatal care; smoking in pregnancy; teenage birth rate and low birth weight17. The 2009 report17 showed the proportion of low birth weight babies, preterm births and perinatal deaths increased as antenatal visits decreased. Indigenous women are more likely to smoke in pregnancy (52 vs 16%) and had a higher teenage pregnancy rate (18 vs 3.2%) than non-Indigenous women, both modifiable factors associated with poor outcomes. With 55% of Aboriginal and Torres Strait Islander new mothers living in outer regional through to very remote areas (Table 2) it is clear that strategies must be employed to reduce the significant disparity in maternal and infant health outcomes between these women and other Australians. We contend that the MMR should be added as a key indicator for measuring Indigenous disadvantage in Australia and accorded the same importance as the MMR is receiving internationally (Millennium Development Goal Five: to reduce the MMR by three-quarters by 2015) and other 'Close the Gap' indicators nationally (Recommendation 2). We acknowledge this would require an increased investment in maternal death investigation, monitoring and reporting in Australia.
Issue 3: Workforce
Globally, skilled attendants are thought to be crucial to improving maternal infant health outcomes18. The term 'skilled attendant' has been debated at length, the accepted definition:
Perinatal mortality rates are also considerably higher for Aboriginal and Torres Strait Islander babies (2-3 times) compared with non-Indigenous Australians12, with double the percent of low birth weight infants (13.2% vs 6.1%) and preterm births (13.9% vs 7.9%)13 (based on the 2005 report because this was the most comprehensive available data). Families from rural and remote areas experience higher rates of fetal and neonatal deaths (1.5-2.9)14.Research and trend data in Western Australia, however, shows increasing disparity in recent years in the infant mortality rate (RR: 4.4) for Aboriginal women compared with non-Aboriginal women, with higher rates in remote areas and teenage mothers under 16 years15. Research in Queensland and Western Australia has identified that the majority of perinatal deaths are due to antenatal factors16 and significantly more potentially preventable deaths in Aboriginal infants are due to infection, preterm birth and sudden infant death syndrome15. These are all amenable to targeted interventions with the Queensland study recommending primary healthcare initiatives to reduce the prevalence of low birth weight and preterm birth and a public health approach inclusive of a domestic violence focus16.
'Close the Gap' campaign: In 2007/2008 the Council of Australian Governments (COAG) committed to 'Overcoming Indigenous Disadvantage' setting six targets with a regular reporting framework against key indicators17. Indicators relating to maternity services include antenatal care; smoking in pregnancy; teenage birth rate and low birth weight17. The 2009 report17 showed the proportion of low birth weight babies, preterm births and perinatal deaths increased as antenatal visits decreased. Indigenous women are more likely to smoke in pregnancy (52 vs 16%) and had a higher teenage pregnancy rate (18 vs 3.2%) than non-Indigenous women, both modifiable factors associated with poor outcomes. With 55% of Aboriginal and Torres Strait Islander new mothers living in outer regional through to very remote areas (Table 2) it is clear that strategies must be employed to reduce the significant disparity in maternal and infant health outcomes between these women and other Australians. We contend that the MMR should be added as a key indicator for measuring Indigenous disadvantage in Australia and accorded the same importance as the MMR is receiving internationally (Millennium Development Goal Five: to reduce the MMR by three-quarters by 2015) and other 'Close the Gap' indicators nationally (Recommendation 2). We acknowledge this would require an increased investment in maternal death investigation, monitoring and reporting in Australia.
Issue 3: Workforce
Globally, skilled attendants are thought to be crucial to improving maternal infant health outcomes18. The term 'skilled attendant' has been debated at length, the accepted definition:
'...an accredited health professional - such as a midwife, doctor or nurse - who has been educated and trained to proficiency in the skills needed to manage normal (uncomplicated) pregnancies, childbirth and the immediate postnatal period, and in the identification, management and referral of complications in women and newborns.'18
It is recognised that skilled attendants, and other key professionals, must be supported by an enabling environment including policy support, access to basic supplies, drugs, transport and relevant emergency obstetric and newborn services for timely management of complications18. In Australia, professionals who fit the WHO definition of skilled attendants are midwives, general practitioners with obstetric training and specialist obstetricians.
International reports highlight a health workforce crisis with critical shortages in some areas, inappropriate skill mix and maldistribution both within and between countries19. In particular, the World Health Report20 noted the MIH workforce was one of the most serious concerns of our time, with 700 000 midwives needed to provide skilled care across the world. Shortages of maternity service providers in Australia reflect the international situation with an uneven distribution of the medical workforce evident and predictions showing this will continue well into the future20,21. Critically for rural and remote maternity services there is a shortage of procedural GPs and those with obstetrics skills with trends suggesting these shortages are worsening22.
Workforce shortages imply multiple strategies are needed to ensure all women receive care from a skilled attendant23 (Recommendation 3). Given international shortages, recruiting internationally is not the answer; Australia has an obligation to train, and if anything, export skilled providers. Expanding strategies that have been shown to be successful is a logical place to start. For example the Commonwealth Government funded Specialist Outreach Program, Obstetric and Medical Locum Schemes; and the Northern Territory funded Midwifery Outreach Program could all be expanded across Australia with the expansion to include a locum scheme for midwives (Recommendation 4). Increasing incentives to encourage the workforce to live in remote areas and increasing bonded scholarships, though not popular with some students, are necessary. Another strategy, proposed by Duckett24, is to move beyond the notion of workforce supply and focus the response on workforce flexibility. The current maternity reforms involving MBS 'eligible' midwives appear to offer promise in this area.
One earlier national strategy aimed at increasing the flexibility of the workforce and the provision of antenatal care in rural Australia is likely to be deleterious. In 2006 a new MBS Item (16400) was introduced by the Department of Health and Ageing25 and supported by the AMA and the Royal College of Nursing of Australia, despite vigorous opposition from eight other professional organisations26. The item allows doctors, who are not required to have obstetric qualifications, to claim MBS for nurses, not required to have midwifery qualifications, to provide antenatal care on their behalf. This rebate only applies to rural and remote areas. Here many doctors do not have obstetric qualifications, have trained overseas, and never previously worked in the Australian maternity care system. Using inappropriately prepared doctors to 'supervise' inappropriately prepared nurses fails to provide Australia's most 'at risk' pregnant women with suitable access to 'skilled attendants'. Thus we argue that this Medicare Item must be modified to remove nurses, who are not midwives, from the eligible list of antenatal care providers (Recommendation 5).
Issue 4: Inefficient use of the midwifery workforce
Of the three professional groups that match the definition of a skilled attendant in Australia, midwives are the only group where the distribution across Australia proportionately matches births across the country20,27,28. However, in many rural and remote areas midwives are also required to provide acute nursing care and have little opportunity to work solely in midwifery or to provide holistic midwifery care. Where women are receiving 'antenatal check ups' the biophysical focus of care fails to maximise opportunities to work with women to increase their health in pregnancy and their capacity to be socially, emotionally and environmentally ready for parenthood. The largest Australian study into the midwifery workforce reported one of the major reasons midwives leave the profession is that they are unable to work to their full scope of practice. This is a particular problem in rural and remote areas, and in the area of antenatal care29,30.
Like many other countries, Australia has commenced a three-year Bachelor of Midwifery (BMid) degree which will see a decline in the number of midwives who are also nurses. The BMid graduates meet the international definition of a midwife with a stronger emphasis on community based care and reproductive health than the 12 month Graduate Diploma for nurses to train as midwives. The introduction of the BMid in New Zealand resulted in increasing numbers of the midwifery workforce attaining midwifery qualifications without holding an initial nursing qualification31. In New Zealand, the BMid graduates are now the largest group of practising midwives (31%), outside overseas trained midwives (37%) in the country (Dr Sally Pairman, Chair, NZ Midwifery Council; pers. comm; 2009). Although qualified midwives can add the study of nursing to their midwifery education if they wish, few choose this option in New Zealand. Many are providing care across rural and remote areas over the childbirth continuum. New Zealand has also significantly increased the number of Maori midwives being educated and returning to their own communities to provide services. This has been supported through Nga Maia, a national organisation supporting Maori in pregnancy and childbirth32.
The recognition of professional skills in a more flexible manner24 would see BMid qualified midwives working effectively in innovative caseload models or midwifery group practices with caseloads adjusted for complexity and distances traveled (currently in urban models one midwife usually cares for 40 women). Other than time spent attending pregnant and childbearing women in hospital, care would be enhanced through home visiting and providing education and care in community settings. Midwives providing labour and birth care can be supported by registered nurses or assistants who have skills in managing maternity emergencies, particularly neonatal resuscitation. The Maternity Emergency Care Course for non-Midwives could provide the education to support this33.
Such re-organisation of the midwifery workforce matches activity to need, rather than servicing the needs of rosters based on hospital practices (Recommendation 6).
The rural midwives working in this new model should also support student positions, funded by the National Workforce Taskforce as student midwives, assistants in midwifery or Aboriginal health workers (similar to the assistant in nursing pay scale), thus growing the rural workforce (Recommendation 7). Additional support must be made available for Aboriginal and Torres Strait Islander women to undertake the BMid (Recommendation 8). In 2010 a partnership between the Northern Territory Department of Health and Families (NT DHF) Congress Alukura Aboriginal Medical Service and Australian Catholic University has seen five Aboriginal women commence their BMid in 2010. All are employed full time and studying concurrently with four embedded in a local midwifery group practice.
More effective utilisation and flexibility of the midwives' role would affect the health workforce in several ways. It could lead to more midwives being attracted to work in remote and rural Australia and free up the time of GPs thereby reducing waiting time for GP appointments. Disadvantages of this model include: lack of flexibility of staff in small units and it is in contradiction to the 'more generalized, less specialized' workforce being recommended by some34. Midwife-only positions lead to less capacity for managers to use midwifery staff to fill nursing vacancies.
Where midwives have made the change to caseload practice, some of the key principles to sustainability are reported as: the ability to make meaningful relationships with women, offering continuity of carer, the occupational autonomy and flexibility and support at home and work35. Midwives opting for caseload practice also recognise the need to engage in continuing education and some would require mentoring until they become familiar with managing the change of practice.
Mentoring midwives who are starting out in caseload models has been successfully implemented in New Zealand and Australia (eg Royal Hospital for Women and Ryde Hospital). Other support models include the statutory supervision model in the UK that provides support and guidance to all midwives. If a mentoring model were to be successfully implemented in Australia, funding for program development and experienced midwives to provide mentoring to rural or remote colleagues, particularly through telecommunication and electronic methods would be needed (Recommendation 6).
The Northern Territory Government (NTG) is currently making significant changes to midwifery services including the introduction of midwifery only positions in five remote communities and an expansion of outreach midwifery positions to provide skilled care where there are no midwives. A further innovation by the NTG, aiming to increase support for women being relocated to regional centres to await birth, is the introduction of the Midwifery Group Practice (MGP) for remote women in Alice Springs and Darwin. The Darwin model has an Aboriginal health worker and a senior Aboriginal Elder embedded as core components and is being evaluated within an NHMRC funded health services program aimed at strengthening the year before and the year after birth (all authors are investigators). The challenge of the remote based midwife positions will be to work differently to maximize their impact. A community development approach, working side-by-side with community workers, to strengthen families and support pregnant women and new mothers is needed.
Issue 5: Relocating women to regional centres to birth
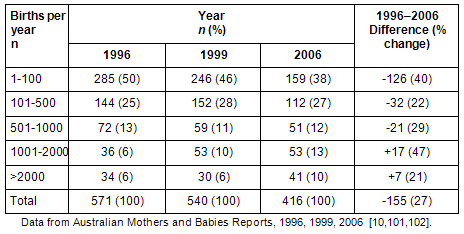
In the last 15 years Australia has seen the closure of 158 birthing services that performed less than 500 births per annum with more than 50% (130) of rural units closed36 (Table 3). These closures have been based on the belief that the loss of medical services makes them unsafe and unviable rather than a national planning approach. This ad hoc approach resulted in some communities of less than 50 births a year retaining birthing services versus other communities with over 100 births a year loosing services. Workforce shortages, lack of access to on-site emergency caesarean section, concerns about safety and perceived higher costs have contributed to these closures37,38. This is despite studies that show there is no evidence that birth for 'low-risk' women is safer in the large hospital setting when compared with birth at home or in small units where skilled attendants work in integrated systems39-48. Research into the impact of the closure of small units highlight the subsequent loss of maternity care providers, the de-skilling of those who stay and the cost shifting that has occurred to families (fuel, childcare, takeaway food, mobile phone etc) who are traveling further for all maternity care49-51. Additionally there is mounting evidence that health outcomes for women and babies worsen following the closure of local units38,52 with some women risking dangerous road travel and babies born on the side of the road53. We believe a reversal of this trend is warranted.
Table 3: Hospitals and birth centres by number of women who gave birth in 1996, 1999 and 200610,11,101,102
 Issue 6: Planning services
The primary maternity services framework will be challenging to implement in the context of ad hoc non-evidence based closure and reopening services will require a new approach. There is little published work to guide the planning process for commencing or re-establishing primary maternity services. The WHO targets of a minimum of five emergency obstetric facilities (including at least one comprehensive facility) for every 500 000 population54, refer to the developing world context and are not easily transferred to the vast distances of rural Australia or the '4th world' context of our remote Aboriginal and Torres Strait Islander communities.
Clearly there is a need to establish a formula or other standardised method for determining the maternity services needs of communities. Researchers from British Colombia in Canada have developed the Rural Birth Index (RBI) to provide such a formula55. The RBI measures birthing numbers, population vulnerability and distance to surgical services to estimate the appropriate maternity services necessary for any population under 25 000. The RBI could be an appropriate policy and planning tool for the Australian setting to assist in planning services based on population need. An Australian workshop, facilitated by Dr Stefan Grzybowski (Centre for Rural Health Research), was held in August 2009 to explore and progress the Australian applicability, testing and modification56. It was well supported by a wide range of clinicians, policy-makers, health planners and academics as worthy of testing in an Australian setting however funding is yet to be sourced (Recommendation 10).
Debates around the minimum number of births for both individuals and facilities to provide competent safe care are occurring57. A number of countries similar to Australia continue to support primary maternity services without surgical capability and with low throughput (Canada, New Zealand, America, Scotland)58-62. Rather than focusing only on numbers, experts are now promoting other strategies to maintain clinicians' competency including continuing skills development and management of emergencies through simulation and drills63,64.
The distance birthing services can be provided from surgical facilities without compromising health outcomes has also been debated with the answer still not clear. The critical time known as the 'decision to incision/delivery' interval (D-D), from when the need for a caesarean section is recognised to when it occurs is thought to be 75 min, but the evidence is mostly based on research in the tertiary setting65. Evidence regarding safe transfer time in the rural and remote setting is slowly becoming available with evaluations of units operating many hours from tertiary services, sometimes completely cut off in bad weather, demonstrating excellent results61,66. This evidence suggests that early identification of problems is mostly possible and that many emergencies can be well managed in the primary setting until transfer to larger units occurs. Thus we suggest that the location of primary maternity services may not have to be based on the D-D distance of 75 min and further research in this area is recommended (Recommendation 11).
A challenge facing both policy-makers and health professionals in Australia is balancing the need for safety with the community pressure for primary level birthing facilities. We are seeing the re-establishment of primary units in some settings (Ryde in Sydney, Belmont in Newcastle, Mareeba in Queensland) with evaluations showing impressive results67,68. Currently a National Health and Medical Research Council funded study to determine the outcomes and costs of providing care in primary level maternity units in both Australia and New Zealand is in progress and will report in 2010 (ID: 571901) (authors 3 and 4) with similar costing work being undertaken for remote NT communities in another NHMRC funded grant aimed at improving continuity of care the year before and the year after birth (all authors are investigators, ID: 422503).
Issue 7: Culturally safe services
Over the last 30 years there have been repeated consultations with Aboriginal and Torres Strait Islander women across remote and rural Australia that have recommended changes to improve the cultural responsiveness of centralised hospital birthing services37,69-75 but little improvement has resulted. Women have repeatedly identified birthing on country as something they believe will improve maternal and perinatal health outcomes37,69-71. These women have stated that their relationship to the land is compromised by birthing in hospitals where many also feel culturally unsafe37,50,69-71,73,76,77. Some women also worry about the safety of the children they must leave behind and believe that the relationship between baby, siblings and father would be better if they were nearby for the birth37,69,71,76,78. This data has again been reported in our NT NHMRC study showing little change over time.
The health of Aboriginal and Torres Strait Islander Australians is integrally linked to their culture and the land79, a link that is strengthened by birthing on their land70,78. Enforced relocation to distant hospital facilities breaks this link, precludes the integration of traditional attendants and practices and continues cultural disconnection into the next generation. The disconnection between social, cultural and spiritual risk and Western medical biophysical risk is a critical and understudied phenomenon that needs to be investigated and better understood. Aboriginal and Torres Strait Islander leaders feel strongly that the cultural risk of not birthing on their land must be acknowledged and included in the risk assessment process80. Some women are performing their own risk assessment. In three of the largest remote communities in Australia where women are routinely relocated for birth (Wadeye, Maningrida and Palm Island), research and reports demonstrate a problematic maternity system81-83. In these communities, every year between 2003 and 2008, 5-22% of women by-passed the system and birthed in their remote communities, some having little antenatal care and birth support as a result. Many of these women had experienced the Western model of evacuation for birth and chosen to avoid it, either hiding their pregnancy or returning to the community, following transfer to the regional centre between 36-38 weeks gestation82.
Social and psychological problems which produce stress, ineffective self-management and a lack of control over circumstances in life are thought to be greater determinants of health in disadvantaged populations than a lack of access to medical care84-86. Yet the current Australian processes to measure risk and address safety in birth do not include the social, emotional and cultural risks that have been identified by Aboriginal and Torres Strait Islander women themselves, nor do they offer women choice or control50. The links among the in-utero experience, birth weight and the child's environment in the first years of life, with long term social, emotional and physical health are well established87,88. Intrauterine stress, preterm birth and low birth weight are linked to chronic disease in adulthood including diabetes, cardiovascular disease and renal failure, all of which are over represented in the Indigenous population89,90.
Some Australian strategies to improve Aboriginal MIH outcomes have started to make a difference with important factors identified as: flexibility, community based, continuity of care, outreach and home visiting, a partnership approach with Aboriginal and non-Indigenous workers and integration with other services91. Two of the better known programs are the NSW Aboriginal Maternal Infant Health Strategy92 and the Strong Women, Strong Babies, Strong Culture Program which employs wise elders in local communities, recognises cultural knowledge as a core principal, is highly valued and has been shown to make a difference to MIH outcomes93. This program could be implemented across remote Australia (Recommendation 4). Although both programs target improved antenatal and postnatal care within a primary healthcare approach, neither incorporate birthing services, a critical missing component. The key components of successful programs are often poorly understood and under-researched, particularly in remote Australia (Recommendation 12).
Lessons learned: Inuit experience
Research from Northern Canada has shown that childbirth in very remote areas can offer a safe, culturally acceptable and sustainable alternative to routine transfer of women to regional centres66,94,95. In one community (Puvirnituq), a primary maternity service opened in 1985 with a 6-8 hour transfer time (in ideal circumstances) to the nearest surgical services. The perinatal mortality rate has fallen significantly and is now better (9/1000) than other comparable Indigenous populations across Canada: Northwest Territories (19/1000) and Nunavut Territory (11/1000)62. Additionally, when comparing 1983 (when there was regular transfer to the regional centre) with 1996 outcomes there has been a reduction in inductions of labour (10% to 5%), episiotomies (25% to 4%), transfers (91% to 9%) and the caesarean section rate (2%) compares favourably to the Quebec rate of 27%66. Since Puvirnituq opened, smaller, more remote communities (eg Inukjuak: population 1184; Salliut: population 1143) have commenced both on-site birthing and training of midwives94,96. A further 7 years evaluation data from these three remote communities contains data on 3500 live births and shows improved trends across all MIH outcomes (V Wagner, pers. comm., 2010).
Reports from these communities describe a community development approach that links the establishment of the local birthing centre to greater social functioning, a decrease in domestic violence and sexual assault, and increasing numbers of men being involved in the care of their partners and newborns66,94,97. The regaining of dignity and self-esteem has also been reported92. A key factor supporting the change process appears to have been the open dialogue and debate around risk in childbirth98 with a recognition that:
Issue 6: Planning services
The primary maternity services framework will be challenging to implement in the context of ad hoc non-evidence based closure and reopening services will require a new approach. There is little published work to guide the planning process for commencing or re-establishing primary maternity services. The WHO targets of a minimum of five emergency obstetric facilities (including at least one comprehensive facility) for every 500 000 population54, refer to the developing world context and are not easily transferred to the vast distances of rural Australia or the '4th world' context of our remote Aboriginal and Torres Strait Islander communities.
Clearly there is a need to establish a formula or other standardised method for determining the maternity services needs of communities. Researchers from British Colombia in Canada have developed the Rural Birth Index (RBI) to provide such a formula55. The RBI measures birthing numbers, population vulnerability and distance to surgical services to estimate the appropriate maternity services necessary for any population under 25 000. The RBI could be an appropriate policy and planning tool for the Australian setting to assist in planning services based on population need. An Australian workshop, facilitated by Dr Stefan Grzybowski (Centre for Rural Health Research), was held in August 2009 to explore and progress the Australian applicability, testing and modification56. It was well supported by a wide range of clinicians, policy-makers, health planners and academics as worthy of testing in an Australian setting however funding is yet to be sourced (Recommendation 10).
Debates around the minimum number of births for both individuals and facilities to provide competent safe care are occurring57. A number of countries similar to Australia continue to support primary maternity services without surgical capability and with low throughput (Canada, New Zealand, America, Scotland)58-62. Rather than focusing only on numbers, experts are now promoting other strategies to maintain clinicians' competency including continuing skills development and management of emergencies through simulation and drills63,64.
The distance birthing services can be provided from surgical facilities without compromising health outcomes has also been debated with the answer still not clear. The critical time known as the 'decision to incision/delivery' interval (D-D), from when the need for a caesarean section is recognised to when it occurs is thought to be 75 min, but the evidence is mostly based on research in the tertiary setting65. Evidence regarding safe transfer time in the rural and remote setting is slowly becoming available with evaluations of units operating many hours from tertiary services, sometimes completely cut off in bad weather, demonstrating excellent results61,66. This evidence suggests that early identification of problems is mostly possible and that many emergencies can be well managed in the primary setting until transfer to larger units occurs. Thus we suggest that the location of primary maternity services may not have to be based on the D-D distance of 75 min and further research in this area is recommended (Recommendation 11).
A challenge facing both policy-makers and health professionals in Australia is balancing the need for safety with the community pressure for primary level birthing facilities. We are seeing the re-establishment of primary units in some settings (Ryde in Sydney, Belmont in Newcastle, Mareeba in Queensland) with evaluations showing impressive results67,68. Currently a National Health and Medical Research Council funded study to determine the outcomes and costs of providing care in primary level maternity units in both Australia and New Zealand is in progress and will report in 2010 (ID: 571901) (authors 3 and 4) with similar costing work being undertaken for remote NT communities in another NHMRC funded grant aimed at improving continuity of care the year before and the year after birth (all authors are investigators, ID: 422503).
Issue 7: Culturally safe services
Over the last 30 years there have been repeated consultations with Aboriginal and Torres Strait Islander women across remote and rural Australia that have recommended changes to improve the cultural responsiveness of centralised hospital birthing services37,69-75 but little improvement has resulted. Women have repeatedly identified birthing on country as something they believe will improve maternal and perinatal health outcomes37,69-71. These women have stated that their relationship to the land is compromised by birthing in hospitals where many also feel culturally unsafe37,50,69-71,73,76,77. Some women also worry about the safety of the children they must leave behind and believe that the relationship between baby, siblings and father would be better if they were nearby for the birth37,69,71,76,78. This data has again been reported in our NT NHMRC study showing little change over time.
The health of Aboriginal and Torres Strait Islander Australians is integrally linked to their culture and the land79, a link that is strengthened by birthing on their land70,78. Enforced relocation to distant hospital facilities breaks this link, precludes the integration of traditional attendants and practices and continues cultural disconnection into the next generation. The disconnection between social, cultural and spiritual risk and Western medical biophysical risk is a critical and understudied phenomenon that needs to be investigated and better understood. Aboriginal and Torres Strait Islander leaders feel strongly that the cultural risk of not birthing on their land must be acknowledged and included in the risk assessment process80. Some women are performing their own risk assessment. In three of the largest remote communities in Australia where women are routinely relocated for birth (Wadeye, Maningrida and Palm Island), research and reports demonstrate a problematic maternity system81-83. In these communities, every year between 2003 and 2008, 5-22% of women by-passed the system and birthed in their remote communities, some having little antenatal care and birth support as a result. Many of these women had experienced the Western model of evacuation for birth and chosen to avoid it, either hiding their pregnancy or returning to the community, following transfer to the regional centre between 36-38 weeks gestation82.
Social and psychological problems which produce stress, ineffective self-management and a lack of control over circumstances in life are thought to be greater determinants of health in disadvantaged populations than a lack of access to medical care84-86. Yet the current Australian processes to measure risk and address safety in birth do not include the social, emotional and cultural risks that have been identified by Aboriginal and Torres Strait Islander women themselves, nor do they offer women choice or control50. The links among the in-utero experience, birth weight and the child's environment in the first years of life, with long term social, emotional and physical health are well established87,88. Intrauterine stress, preterm birth and low birth weight are linked to chronic disease in adulthood including diabetes, cardiovascular disease and renal failure, all of which are over represented in the Indigenous population89,90.
Some Australian strategies to improve Aboriginal MIH outcomes have started to make a difference with important factors identified as: flexibility, community based, continuity of care, outreach and home visiting, a partnership approach with Aboriginal and non-Indigenous workers and integration with other services91. Two of the better known programs are the NSW Aboriginal Maternal Infant Health Strategy92 and the Strong Women, Strong Babies, Strong Culture Program which employs wise elders in local communities, recognises cultural knowledge as a core principal, is highly valued and has been shown to make a difference to MIH outcomes93. This program could be implemented across remote Australia (Recommendation 4). Although both programs target improved antenatal and postnatal care within a primary healthcare approach, neither incorporate birthing services, a critical missing component. The key components of successful programs are often poorly understood and under-researched, particularly in remote Australia (Recommendation 12).
Lessons learned: Inuit experience
Research from Northern Canada has shown that childbirth in very remote areas can offer a safe, culturally acceptable and sustainable alternative to routine transfer of women to regional centres66,94,95. In one community (Puvirnituq), a primary maternity service opened in 1985 with a 6-8 hour transfer time (in ideal circumstances) to the nearest surgical services. The perinatal mortality rate has fallen significantly and is now better (9/1000) than other comparable Indigenous populations across Canada: Northwest Territories (19/1000) and Nunavut Territory (11/1000)62. Additionally, when comparing 1983 (when there was regular transfer to the regional centre) with 1996 outcomes there has been a reduction in inductions of labour (10% to 5%), episiotomies (25% to 4%), transfers (91% to 9%) and the caesarean section rate (2%) compares favourably to the Quebec rate of 27%66. Since Puvirnituq opened, smaller, more remote communities (eg Inukjuak: population 1184; Salliut: population 1143) have commenced both on-site birthing and training of midwives94,96. A further 7 years evaluation data from these three remote communities contains data on 3500 live births and shows improved trends across all MIH outcomes (V Wagner, pers. comm., 2010).
Reports from these communities describe a community development approach that links the establishment of the local birthing centre to greater social functioning, a decrease in domestic violence and sexual assault, and increasing numbers of men being involved in the care of their partners and newborns66,94,97. The regaining of dignity and self-esteem has also been reported92. A key factor supporting the change process appears to have been the open dialogue and debate around risk in childbirth98 with a recognition that:
the cultural aspect of birth is not a mere 'nicety' that can be appended to the care plan once all other acute obstetrical techniques are in place. It is essential to perinatal health... it is from within the culture and community that real positive changes in the health of the people begins'99.
Some of the key factors in the success of these services are the collaborative community development approach to care; local employment; on-site midwifery training; integration of Inuit knowledge with western knowledge; the involvement of men; a risk screening process that includes social and cultural risks in addition to biomedical risks; and the interdisciplinary perinatal committee. This committee reviews each woman's case 32-34 weeks gestation for all risks, and creates a care plan for birth100. Conclusion In conclusion, there are increasing rather than decreasing challenges to the delivery of safe maternity services in rural and remote areas of Australia. Changing the way care is delivered could promote substantial improvements. Maternity providers must demonstrate the competencies required of skilled birth attendants. The midwifery workforce should be enabled to work to their full scope of practice with referral support from general practitioners with obstetric skills and specialist obstetric services, neither of which need to be 'named' or on site. With changes to the funding model in Australia, the provision of skilled, culturally appropriate care as close to home as possible for all women must be seen as a non-negotiable national priority. With slow progress being made towards closing the gap in MIH outcomes and culturally acceptable maternity care across Australia, and likely underreprting of poorer outcomes, it would seem appropriate to learn from others. Comparable counties, particularly Canada and New Zealand, have made substantial progress towards closing this gap. These countries come from similar colonial histories yet are leading the way, both in innovation of service models, midwifery in primary care settings and health outcomes for their Indigenous peoples103. Providing primary maternity services 'on country' must be explored. This should be done within a rigorous research framework using a community development approach that incorporates the training of Indigenous women as midwives and is led by the Indigenous community itself with support from an integrated network (Recommendation 13). We can no longer ignore the extraordinary results from the remote based Inuit models, particularly the unpredicted effects that are contributing to building community capacity and resilience. Communities that self identify this as a goal must be supported even when obstacles are described as insurmountable by service providers. We also believe Australia must take note of the millennium development goal and aim to reduce the MMR for Indigenous Australians from 45.9 per 100 000 (2000-2002) to 11.5 per 100 000 by 2015. Acknowledgments Sue Kildea is the Current Vice President of the CRANAplus, an organisation supporting and advocating for remote Australia and the provider of the MEC course. This article was supported by data from two NHMRC funded studies: (ID: 422503, all authors; ID: 571901, authors 3 and 4). References 1. Department of Health and Aging. Improving maternity services in Australia: A discussion paper from the Australian Government. Canberra, ACT: Commonwealth of Australia, 2008. 2. NSW Department of Health on behalf of the Maternity Services Inter-jurisdictional Committee. Primary maternity services in Australia: A framework for implementation. Canberra, ACT: Australian Health Ministers Advisory Council, 2008. 3. Australian Government. Steering Committee for the Review of Government Service Provision, Overcoming Indigenous Disadvantage Report. Canberra, ACT: Commonwealth of Australia: 2009. 4. Laws P, Sullivan E. Australia's mothers and babies 2007, Perinatal Statistics Series no. 23. Sydney, NSW: AIHW National Perinatal Statistics Unit, 2009. 5. Sullivan E, Hall B, King J (Eds). Maternal deaths in Australia 2003-2005. Sydney, NSW: AIHW National Perinatal Statistics Unit, 2008. 6. Kildea S. Maternal deaths high for Indigenous women. Women and Birth 2008; 21: 175-176. 7. Kildea S, Humphrey M, Sherwood J, Paterson B, Finn M, Black D et al. Maternal mortality in Aboriginal and Torres Strait Islander women. In: J King, E Sullivan (Eds). Maternal Deaths in Australia 2000-2002. Canberra, ACT: AIHW, 2006; 75-81. 8. Ronsmans C, Graham WJ for Lancet Maternal Survival Series Steering Group. Maternal mortality: who, when, where and why. Lancet 2007; 368(9543): 1189-1200. 9. Sullivan E, Kildea S, Black D. Epidemiology of Maternal Deaths. In: J King, E Sullivan (Eds). Maternal Deaths in Australia 2000-2002. Canberra, ACT: AIHW, 2006; 8-31. 10. Laws P, Hilder L. Australia's mothers and babies 2006, Perinatal Statistics Series no. 22. Sydney, NSW: AIHW National Perinatal Statistics Unit, 2008. 11. Australian Bureau of Statistics. 4102.0 - Australian Social Trends, 2008. Population Distribution. (Online) 2008. Available: http://www.abs.gov.au/AUSSTATS/abs@.nsf/Lookup/4102.0Chapter3002008 (24 March 2009). 12. Trewin D, Madden R. The Health and Welfare of Australia's Aboriginal and Torres Strait Islander Peoples. Canberra, ACT: Australian Bureau of Statistics, Australian Institute of Health and Welfare, 2005. 13. Laws P, Abeywardana S, Walker J, Sullivan E. Australia's mothers and babies 2005, Perinatal Statistics Series no. 20. Sydney, NSW: AIHW National Perinatal Statistics Unit, 2007. 14. Australian Bureau of Statistics, Australian Institute of Health and Welfare. The Health and Welfare of Australia's Aboriginal and Torres Strait Islander Peoples 2005. Canberra, ACT: Australian Bureau of Statistics and the Australian Institute of Health and Welfare, 2005. 15. Fremantle C, Read A, de Klerk N, McAullay, Anderson I, Stanley F. Patterns, trends and increasing disparities in mortality for Aboriginal and non-Aboriginal infants born in Western Australia, 1980-2001: population database study. Lancet 2006; 367: 1758-1766. 16. Johnston T, Coory M. Reducing perinatal mortality among Indigenous babies in Queensland: should the first priority be better primary health care or better access to hospital care during confinement? Australian and New Zealand Health Policy 2005; 2(11). Available: http://www.anzhealthpolicy.com/content/2/1/11. 17. Steering Committee for the Review of Government Service Provision. Overcoming Indigenous Disadvantage Report. Canberra, ACT: Commonwealth of Australia, 2009. 18. WHO. Making Pregnancy Safer: The critical role of skilled attendants: Joint statement by World Health Organisation, International Confederation of Midwives, International Federation of Gynecology and Obstetrics. Geneva: WHO, 2004. 19. WHO. The World Health Report 2006: Working together for health. Geneva: WHO, 2006. 20. Australian Health Workforce Advisory Committee. The Midwifery Workforce in Australia 2002-2012, AHWAC report 2002.2. Sydney, NSW: AHWAC, 2002. 21. AHWAC. The Australian Nursing Workforce - An Overview of Workforce Planning 2001-2004. Sydney, NSW: Australian Health Workforce Advisory Committee (AHWAC), National Health Workforce Secretariat, 2004. 22. Loy C, Warton R, Dunbar J. Workforce trends in specialist and GP obstetric practice in Victoria. Medical Journal of Australia 2007; 186(1): 26-30. 23. Koblinski M, Matthews Z, Hussein J, Mavalankar D, Mridha M, Anwar I et al. Going to scale with professional skilled care. Lancet 2006; 368: 1377-1386. 24. Duckett S. Interventions to facilitate health workforce restructure. Australia and New Zealand Health Policy 2005; 2(14). Available: http://www.anzhealthpolicy.com/content/2/1/14. 25. Commonwealth Government. Item No. 16400, Extract from Medical Benefits Schedule. Canberra, ACT: Commonwealth Government, no date. 26. Australian Nursing Federation, Australian College of Midwives, Australian Nursing and Midwifery Council, Royal Australian and New Zealand College Obstetricians and Gynaecologists, The College of Nursing, Australian Practice Nurses Association, Council of Remote Area Nurses of Australia and The Association of Australian Rural Nurses. Consensus Statement. Commonwealth Government Medicare Item 16400: Antenatal care in rural and remote communities. (Online) 2006. Available: http://www.anmc.org.au/userfiles/file/Consensus_Statement.pdf (Accessed 13 July 2010). 27. Australian Medical Workforce Advisory Committee. Commonwealth Government, The Specialist Obstetrics and Gynaecology Workforces in Australia, An Update: 2003 to 2013. Sydney, NSW: AMWAC, 2004. 28. Pflaum M, Wall C, Slatyer B, Boutchard C, Jolly R, Harris K. The Australian Medical Workforce Occasional Paper. Canberra, ACT: Department of Health and Aged Care, 2001. 29. Barclay L, Brodie P, Tracy S, Leap N. Australian Midwifery Action Project Final Report. Sydney, NSW: Centre for Family Health and Midwifery, University of Technology Sydney, 2002. 30. Brodie P. Addressing the barriers to midwifery - Australian midwives speak out. Australian Journal of Midwifery 2002; 15(3): 5-14. 31. Midwifery Council of New Zealand. Midwifery Workforce Data, 2006. (Online) 2006. Available: http://www.midwiferycouncil.org.nz/main/Workforce/ (Accessed 10 August 2009). 32. Nga Maia. Nga Maia New Zealand. (Online) 2009. Available: www.ngamaia.co.nz (Accessed 10 August 2009). 33. Kildea S, Kruske S, Bowell L. MEC: A short course in maternity emergencies for remote area health staff with no midwifery qualifications. Australian Journal of Rural Health 2006; 14: 111-115. 34. Duffield C, Roche M, O'Brien-Pallas L, Diers D, Aisbett C, King M et al. Glueing it together: nurses, their work environment and patient safety. Sydney, NSW: Centre for Health Services Management UTS, 2007. 35. Brodie P, Warwick C, Hastie C, Smythe L, Young C. Sustaining midwifery continuity of care: perspectives for midwives. In: C Homer, P Brodie, N Leap (Eds). Midwifery continuity of care. A practical guide. Sydney, NSW: Elsevier, 2008; 149-164. 36. Rural Doctors Association of Australia. Governments Must Heed the Evidence: Small Maternity Units are Safer, media release. (Online) 2005. Available: http://www.rdaa.com.au (Accessed 7 December 2005). 37. Hirst C. Re-Birthing, Report of the Review of Maternity Services in Queensland. Brisbane, QLD: Queensland Health, 2005. 38. Australian College of Rural and Remote Medicine and Rural Doctors Australia. Joint ACRRM / RDAQ submission to the Review of Maternity Services in Queensland, November 2004. Brisbane, QLD: Australian College of Rural and Remote Medicine and Rural Doctors Australia, 2004. 39. Cameron B. Outcomes in rural obstetrics, Atherton Hospital 1981-1990. Australian Journal of Rural Health 1998; 6: 46-51. 40. Cameron B, Cameron S. Outcomes in rural obstetrics, Atherton Hospital 1991-2000. Australian Journal of Rural Health 2001; 9(Suppl): 39-42. 41. Edwards A, Gale J. Rural Maternity Initiative Evaluation, Final Report. Kyneton, VIC: Kyneton District Health Service, 2007. 42. Campbell R, Macfarlane A. Where to be born? The debate and the evidence, 2nd edn. Oxford, UK: National Perinatal Epidemiology Unit, 1994. 43. Wiegers T, Keirse M, van der Zee J. Outcome of planned home and hospital births in low risk pregnancies: prospective study in midwifery practice in the Netherlands. BMJ 1996; 313(7068): 1309-1313. 44. Johnson K, Daviss B. Outcomes of planned home births with certified professional midwives: large prospective study in North America. BMJ 2005; 330: 1416-1423. 45. Tracy SK, Dahlen H, Caplice S, Laws P, Wang YA, Tracy MB et al. Birth Centers in Australia: A National Population-Based Study of Perinatal Mortality Associated with Giving Birth in a Birth Center. Birth 2007; 34(3): 194-201. 46. Tracy S, Sullivan E, Dahlen H, Black D, Wang Y, Tracy M. Does size matter? A population-based study of birth in lower volume maternity hospitals for low risk women. British Journal of Gynaecology 2006; 113: 86-96. 47. Lumley J. The Safety of Small Maternity Hospitals in Victoria 1982-84. Community Health Studies 1988; X11(4): 386-393. 48. Olsen O, Jewell M. Home birth versus hospital birth. Cochrane Database of Systematic Reviews 1998; issue 3: CD000352. DOI: 10.1002/14651858.CD000352. 49. Dietsch E, Davies C, Shackleton P, Alston M, McLeod M. 'Luckily We Had a Torch': Contemporary Birthing Experiences of Women Living in Rural and Remote NSW. Wagga Wagga, NSW: Charles Sturt University, 2008. 50. Kildea S. Risky business - contested knowledge over safe birthing services for Aboriginal women. Health Sociology Review 2006; October: 387-396. 51. May J, Kent S, Guppy M. Obstetric care in rural Australia: the evidence is right under our noses-but what direction are we heading? Standing up for Rural Health: Learning from the past, Action for the future. In: Proceedings, 9th National Rural Health Conference; 7-10 March; Albury, VIC, 2007. 52. Kornelsen J, Grzybowski S. Safety and community: the maternity care needs of rural parturient women. Journal of Obstetrics and Gynaecology Canada 2005; 27: 554-561. 53. Dietsch E, Shackleton P, Davies C, Alston M, McLeod M. 'Mind you, there's no anaesthetist on the road': women's experiences of labouring en route. Rural and Remote Health 10:1371. (Online) 2010. Available: www.rrh.org.au (Accessed 12 July 2010). 54. WHO, UNFPA, UNICEF, AMDD. Monitoring emergency obstetric care, A Handbook. Geneva: WHO, 2009. 55. Grzybowski S, Kornelsen J, Schuurman N. Planning the optimal level of local maternity service for small rural communities: A systems study in Btitish Columbia. Health Policy 2009; 92(2): 149-157. 56. Kildea S, Stratagos S. A rural birth Index for Australia? Australian Journal of Rural Health 2010; 18(2): 85-86. 57. Society of Obstetricians and Gynaecologists of Canada, College of Family Physicians of Canada, Society of Rural Physicians of Canada. Number of births to maintain competence. Candian Family Physician 2002; 48(4): 751. 58. Matheson D, Borman B. The Patterns of Use of Facilities and Obstetric Outcomes for Women Living in Rural Areas, 2001. Otago: University of Otago, 1999. 59. Rosenblatt R, Reinken J, Shoemack P. Is obstetrics safe in small hospitals, evidence from New Zealand's regionalised perinatal system. Lancet 1985; 2(8452): 429-432. 60. Health Funding Authority. Maternity services: A reference document. Hamilton: Health Funding Authority, 2000. 61. Leeman L, Leeman R. Do all hospitals need cesarean delivery capability?: An outcomes study of maternity care in a rural hospital without on-site cesarean capability. The Journal of Family Practice 2002; 51(2): 129-134. 62. British Columbia Reproductive Care Program. Consensus Symposium Summary. Vancouver, BC: British Columbia Reproductive Care Program, 2000. 63. Grzybowski S, Kornelsen J, Cooper E. Rural maternity care services under stress: the experiences of providers. Canadian Journal of Rural Medicine 2007; 12(2): 1-6. 64. National Health Service. The National Framework for Service Change in NHS Scotland, Rural Access Action Team, Final Report. Scotland: National Health Service, 2005. 65. Thomas J, Paranjothy S, James D. National cross sectional survey to determine whether the decision to delivery interval is critical in emergency caesarean section. BMJ 2004; 328(7441): 665. 66. Van Wagner V, Epoo B, Nastapoka J, Harney E. Reclaiming Birth, Health, and Community: Midwifery in the Inuit Villages of Nunavik, Canada. Journal of Midwifery & Women's Health 2007; 52(4): 384-391. 67. Scherman S, Smith J, Davidson M. The first year of a midwifery-led model of care in Far North Queensland. Medical Journal of Australia 2008; 188(2): 85-88. 68. Tracy S, Hartz D. Final Report: The Quality Review of Ryde Midwifery Group Practice, September 2004 to October 2005. Sydney, NSW: Northern Sydney and Central Coast Area Health Service, 2005. 69. Biluru Butji Binnilutlum Medical Service. Women's Business Meeting, Darwin, November 2-3, Report and Recommendations. Darwin, NT: Danila Dilba, 1998. 70. Carter B, Hussen E, Abbott L, Liddle M, Wighton M, McCormack M et al. Borning: Pmere Laltyeke Anwerne Ampe Mpwaretyeke, Congress Alukura by the Grandmothers Law. Australian Aboriginal Studies 1987; 1: 2-33. 71. Kildea S. And the women said... Report on birthing services for Aboriginal women from remote Top End communities. Darwin, NT: Territory Health Service, 1999. 72. NSW Health Department. The NSW Aboriginal Perinatal Health Report. Sydney, NSW: NSW Health Department, 2003. 73. NT DHCS. Review of Birthing Services in the Northern Territory of Australia. Darwin, NT: Department of Health and Community Service,1992. 74. Senate Community Affairs References Committee. Rocking the Cradle, A Report into Childbirth Procedures. Canberra, ACT: Commonwealth of Australia, 1999. 75. Banscott Health Consulting. Maternity Services Review in the Northern Territory. Darwin, NT: Department of Health and Community Services, 2007. 76. Fitzpatrick J. Obstetric health services in Far North Queensland: is choice an option? Australia Journal of Public Health 1995; 19(6): 580-588. 77. Fitzpatrick J. Birthing Choices in Far North Queensland. Brisbane, QLD: Department of Health, Housing and Community Service, 1993. 78. Kildea S, Wardaguga M. Childbirth in Australia: Aboriginal and Torres Strait Islander Women. In: H Selin, P Stone (Eds). Childbirth across cultures, ideas of pregnancy, childbirth and the postpartum period in many of the worlds cultures. Amherst: Springer, 2009, 275-287. 79. National Aboriginal and Torres Strait Islander Health Council. National Aboriginal and Torres Strait Islander Health Strategy, Consultation Draft. Canberra, ACT: National Aboriginal and Torres Strait Islander Health Council, 2000. 80. Wardaguga M, Kildea S. Bring Birthing Back to the Bush. Aboriginal Health Worker Journal 2005; 29(5). Available: http://search.informit.com.au/documentSummary;dn=132125806405061;res=IELHEA. 81. Barclay L, Kildea S, Gao Y. 1+1= A Healthy Start to Life - Research Report no.5. Darwin, NT: Graduate School for Health Practice, 2008. 82. Ireland S, Wullili Narjic C, Belton S, Kildea S. Niyith Niyith Watmum the quiet story: Exploring the experiences of Aboriginal women who give birth in their remote community. Midwifery 2010; doi:10.1016/j.midw.2010.05.009 (In press). 83. Gosden A. A report on the development of a midwifery model of care for the Joyce Palmer Health Service (Palm Island). Townsville, QLD: Townsville Health Service District, Queensland Health, 2008. 84. Pincus T, Esther R, De Walt D, Callaghan L. Social Conditions and Self-management Are More Powerful Determinants of Health and Access to Care. Annals of Internal Medicine 1998; 129(5): 406-411. 85. Wilkinson R, Marmot M (Eds). The Solid Facts, Social Determinants of Health. Geneva: World Health Organisation, 1998. 86. Wallerstein N. Powerlessness, empowerment, and health: implications for health promotion programs. American Journal of Health Promotion 1992; 6(3): 197-205. 87. McCain M, Mustard F. The Early Years Study, Reversing the real brain drain. (Online) 1999. Available: http://www.children.gov.on.ca/ (Accessed 12 July 2010). 88. Shonkoff J, Phillips D. Rethinking nature and nurture In: J Shonkoff , D Phillips (Eds). From Neurons to Neighborhoods, the Science of Early Childhood Development. Washington, DC: National Academy Press, 2000; 39-56. 89. Barker D. Fetal nutrition and cardiovascular disease in later life. BMJ 1997; 53(1): 96-108. 90. Hoy W, Rees M, Kile E, Mathews J, Wang Z. A new dimension to the Barker hypothesis: Low birth weight and susceptibility to renal disease. Kidney International 1999; 56(3): 1072-1077. 91. Herceg A. Improving health in Aboriginal and Torres Strait Islander mothers, babies and young children: a literature review. Canberra, ACT: Australian Government Department of Health and Ageing, 2005. 92. NSW Health. NSW Aboriginal Maternal and Infant Health Strategy Evaluation Final Report 2005. Sydney, NSW: NSW Health, 2006. 93. Mackerras D. Birthweight changes in the pilot phase of the Strong Women Strong Babies Strong Culture Program in the Northern Territory. Australian and New Zealand Journal of Public Health 2001; 25(1): 34-40. 94. Houd S, Qinuajuak J, Epoo B (Eds). The outcome of perinatal care in Inukjuak, Nunavik, Canada 1998-2002. In: Proceedings, 12th International Congress on Circumpolar Health; 10-14 September 2003; Nuuk, Greenland, 2003. 95. Chamberlain M, Barclay K. Psychosocial costs of transferring women from their community for birth. Midwifery. 2000; 16(2): 116-122. 96. Tookalak N. Birthing in Puvirnituq in remote Artic Canada. Birthplace Magazine 1998; Summer: (no pp). 97. Rawlings L. Birth Rites. In: Gheradi J (Ed). Perth, WA: Jag Films, 2002. 98. Kaufert P, O'Neil J. Analysis of a dialogue on risks in childbirth: clinicians, epidemiologists, and Inuit women. In: S Lindenbaum, M Lock (Eds). Knowledge, Power and Practice, The Anthropology of Medicine and Everyday Life. Berkeley, CA: University of California Press, 1993; 32-54. 99. Stonier J. The Innulitsivik Maternity. In: J O'Neil, P Gilbert (Eds). Childbirth in the Canadian North: Epidemiological, Clinical and Cultural Perspectives. Manitoba: Northern Health Research Unit, 1990; 61-74. 100. Couchie C, Sanderson S. A Report on Best Practices for Returning Birth to Rural and Remote Aboriginal Communities. Journal of Obstetrics and Gynaecology Canada 2007; 29(3): 250-254. 101. Day P, Sullivan E, Lancaster P. Australia's mothers and babies 1996. Sydney, NSW: Australian lnstitute of Health and Welfare National Perinatal Statistics Unit, 1999. 102. Nassar N, Sullivan E. Australia's Mothers and Babies 1999, Perinatal Statistics Series no.11. Sydney, NSW: AIHW National Perinatal Statist, ic, , , , , , s, Unit, 2001. 103. Ring I, Brown N. The health status of Indigenous peoples and others, the gap is narrowing in the United States, Canada, and New Zealand, but a lot more is needed. BMJ 2003; 327(7412): 404-405.



