Context
In order to achieve the 'Health for All' proposed by the Alma-Ata Declaration, a fair allocation of physicians among the entire population of each society is required1. In reality, however, the geographical distribution of physicians is far from even. In both developed and developing countries, the disproportionate concentration of physicians in urban areas, and the shortage of physicians in rural areas, is a serious healthcare problem. Both national and international political action has been suggested to solve this problem2.
Physician shortage and maldistribution in post-World War II Japan
Article 25 of the Constitution of Japan states that all people have a right to medical service of equal quality. The provision of fair healthcare access for the entire population, including those who live in rural or remote areas, is recognised as the responsibility of the national and local governments. This sense of 'governmental responsibility' among the Japanese is the basis of the physician workforce strategies of post-war Japan.
During World War II, Japan produced a large number of military physicians. The number of new licensed physicians in 1940 was 2074; however, by 1950 this figure had risen to 73933. Due to this rapid increase, the shortage of physicians was not recognised as a major social issue for some decades after the end of the war. However, during the period of the American occupation, General Headquarters of the Allied Forces limited medical education to university-level schools, which had only comprised a small part of the pre-war medical school sector in Japan. This substantially decreased the number of graduating physicians. As the number of medical school entrants dropped from 10 533 in 1945 to 2800 in 1951, by 1954 only 2798 new physicians were licensed3. This low level of physician supply lasted until 1970.
In 1953 the number of physicians per 100 000 population in Japan was 103, markedly lower than that in comparable industrialised countries, such as the USA (150), West Germany (151), and Italy (173). At the same time, the demand for medical services increased dramatically due to the establishment of the national health insurance system in 1961, and the rapid economic development of the 1950s and 1960s. Between 1955 and 1967, the number of patient visits to medical institutions doubled. The decrease in supply and the increase in demand created a serious shortage of physicians. The shortage of physicians was especially severe in rural and remote areas. In 1967 the number of physicians per 100 000 population in 7 metropolitan cities was 149, 126 in other cities, and 63 in towns and villages4. There were more than 2900 nationally-certified 'non-physician communities' (muichiku), which were defined by the government as areas of more than 50 residents within a 4 km radius where daily access to a physician was difficult or impossible5.
Issue
In Japan the mal-distribution of physicians that severely disadvantaged rural populations has been addressed by the concerted, cooperative efforts of the three public sectors: national government, local governments and medical schools. Over the past half century, Japan has established and managed:
- The national health insurance system (which covers everyone regardless of their place of residence)6.
- A special medical school for producing rural physicians7.
- Many public clinics and hospitals in rural areas8.
These public-sector-led countermeasures to the mal-distribution of physicians have had some effect on the issue5-8, and these strategies will now be described in detail. The transferability of the Japanese-style rural health strategy to developing countries, now struggling to build up their physician workforce in rural areas, will also be discussed.
Actions
Strategies of the national government: The national government planned and executed an ambitious strategy in 1960s and 1970s, 'one medical school in each prefecture' (similar to states in the USA), to solve the physician shortage and the unequal distribution of physicians simultaneously. Under this strategy, public medical schools were founded in (mainly rural) prefectures where none existed. The number of medical schools in Japan increased from 46 to 79 in the years 1950 and 1980, respectively. The number of medical school entrants rose from 3560 to 8260 in 1965 and 1980, respectively9. This was followed by a rapid increase in the number of physicians per 100 000 population, from 100 in 1950 to the government's 1960s target of 150 in 1984. The national government implemented the 'Rural Healthcare Plan' in 1956. The plan is enacted every 5 years to improve rural health delivery and has been revised every five years since.
Local government strategies: Municipalities (cities, towns and villages) are the basic geographic units of administration and, in 2009, there were 1779 municipalities among the 47 prefectures. While the national government increased the number of medical schools and physicians, the governments of rural prefectures and municipalities that are directly responsible for providing health care to their residents, struggled to recruit physicians.
Japan adopted a fee-for-service healthcare system after World War II, and most of Japan's medical institutions are for-profit private clinics and hospitals6. It was, however, difficult for rural communities with small populations to attract private medical institutions due to their requirement for high profitability. And attracting physicians to rural areas was particularly difficult due to the following factors. Japanese physicians have the right to practice wherever they choose. There is no area quota for physicians, and no financial incentive for rural practice. In addition, most physicians have an urban background10,11.
It was therefore necessary for rural municipal governments to establish their own public clinics and hospitals - and to provide financial incentives for physicians to work there. Substantial amounts had to be allocated from rural municipal government budgets for physician incentives and the purchase of equipment for clinics and hospitals. As a result, the salaries of rural physicians are generally higher than for their urban counterparts.
If the municipalities could not afford to have their own public hospitals, prefectures owned them on behalf of the municipalities. Thus the more rural the location, the higher the proportion of public hospitals in Japan. In 2005, for example, the percentage of public hospitals among all hospitals in large cities was 4%, but 16% elsewhere12. The percentage is likely to be more than 50% in the most rural or remote areas.
The massive financial support from public budgets has reportedly elevated the quality of hospital equipment and the satisfaction of physicians with their salaries8,13,14. However, despite these municipal and prefectural efforts, physician posts in rural medical institutions remained unfilled, with an occupancy rate of only 56% in 196715. Some municipalities recruited international physicians from countries such as Korea and Taiwan16.
Jichi Medical University: The governments and residents of rural municipalities and prefectures that still experienced difficulty in recruiting physicians learned they could neither rely on physicians' voluntarism nor the national government's policies to end the physician shortage in rural areas. In December 1970, the Union of Prefecture Governors submitted a petition calling for a new medical school to produce rural physicians. This petition was immediately accepted by the national government and the new school, Jichi Medical School (currently Jichi Medical University [JMU]), was founded in April 197215.
Half of the budget for this special medical school was provided by the national government with the remainder divided equally among the 47 prefectural governments. The annual management of JMU is supported by pooled funds from the equal contributions of the 47 prefectures. Each prefectural government, in cooperation with JMU officials, selects two or three local high school graduates for admission to JMU. Each student's educational and living expenses are borne by his/her home prefecture. In exchange, the student is required to work for public medical institutions in their home prefecture for 9 years after graduation and licensure. The nine-year obligation period consists of 2-3 years clinical training as a primary-care generalist, followed by 6-7 years in rural service.
The JMU has thus two unique characteristics: free medical education in exchange for obligatory rural service; and close, long-term cooperation of national and local governments, and the medical school over the period from pre-entrance selection to completion of the nine-year obligation for each student. Figure 1 shows this interaction among the public sectors.
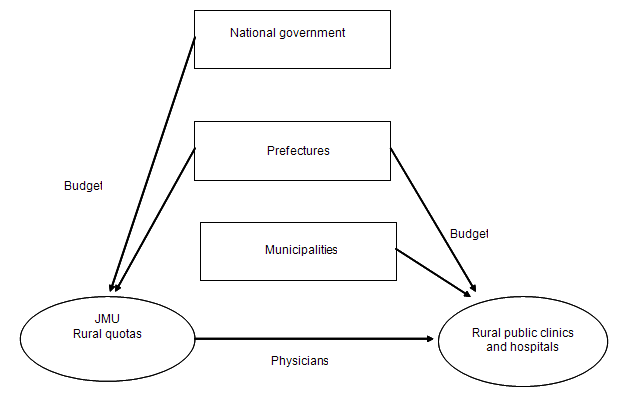
Figure 1: The structure of public sectors to secure health care in rural areas (JMU, Jichi Medical University; rural quotas: financial incentive programs for producing rural physicians in other public medical schools).
Thirty-eight years after its foundation, JMU has considerable achievements. By 2006 it had produced 2962 physicians, 97% of whom have completed or are completing their obligation17. The percentage of JMU graduates under obligatory service who work in municipalities with a population of less than 50 000 is 85%; while those who remain 'after obligation' is 50%. These figures are substantially higher than for non-JMU physicians in Japan (19%)18. The retention rate of JMU graduates in their home prefectures after obligation is 70%19.
Consequences of the physician increase policy in Japan
The 'one medical school in each prefecture' policy induced a rapid increase in the number of physicians. The number of physicians per 100 000 population rose from 150 to 218 in 1984 and 2006, respectively. The growth of the number of physicians and JMU graduates dramatically decreased the number of 'non-physician communities' (muichiku), which the government considered its highest priority (Fig2)5.
However, despite an increase in the absolute number of physicians in rural areas, the relative gap between the number of physicians in urban and rural areas has reportedly remained unchanged20,21. Although the number of physicians per unit population increased by 60% between 1980 and 2000, the Gini coefficient (level of equity) of physician distribution against population distribution has consistently been 0.3322. While the contribution of JMU physicians to rural and remote municipalities is substantial, they comprise only 1% of all physicians in Japan, and the impact of the JMU initiative on the distribution of all physicians in Japan is not as large as was expected.
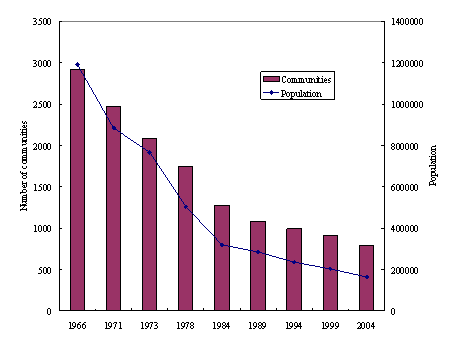
Figure 2: Transition of the number of 'non-physician communities' and their populations (government definition of 'non-physician community' is an area with >50 residents within a 4 km radius, where daily access to a physician is difficult or impossible)5.
The supply of physicians has not yet met demand. The progressive specialisation and technologisation of medicine, population aging and the demand for medical services has greatly increased. In addition, after a rapid growth in the number of students admitted to medical school in the 1960s and 1970s, the government reduced the number of entrants by 7%, contending that physicians were oversupplied9. As a result, the number of physicians per unit population in Japan is still among the lowest five of the 30 OECD countries23.
The situation has been exacerbated by government-led mergers of municipalities since 2004, with the total number of municipalities decreasing by 45% (from 3212 to 1779) between 2003 and 2009. In addition, the economic recession of the 1990s and early 2000s has led to a decline in financial status for most municipalities, and placed the less profitable rural public clinics and hospitals in a difficult predicament. Merged municipalities were often forced to close these public clinics and hospitals in the interest of 'financial streamlining'. This aggravated the shortage of physicians in rural areas, and equity in the geographic distribution of physicians according to population has clearly declined since 200424.
The Jichi Medical University replication policy
Responding to the absolute shortage of physicians nationwide, the government increased medical school admissions in 2007. This was the first increase since adoption of the 1986 government suppression policy. However, the way in which this increase was implemented was new.
Following the success of JMU, the government determined to increase physicians by imposing a 'rural quota' on one medical school in each prefecture of five students every year (except for Hokkaido where the quota is 15 students). These rural quotas increase the number of medical school entrants in all 47 prefectures by 245 annually. These physicians are produced in a similar fashion to the JMU system, with most of the quota students recruited from the prefecture where the medical school is located. Similarly, their tuition fees are waived in exchange for a nine-year period bonded to the prefecture's public medical institutions (Fig1). In addition to the government-led rural quotas, some medical schools have set 'community quotas' for students who are willing to work in the prefecture, preferably in a rural community, without obligation.
By 2008, 80% of all medical schools had adopted quotas of some sort, and 24% had adopted rural quotas25. If the 245 annual rural quota physicians follow the pattern of JMU graduates, it is predicted that the number of physicians in rural municipalities will increase by 6.5% 9 years after the first students graduate (excluding the increase effect of growth in the total number of physicians and JMU graduates). If these rural quota physicians remain in rural areas after their obligation at a similar proportion to JMU graduates, the increase rate will be even higher. The policy to replicate JMU has the potential to make a substantial impact on the nationwide distribution of physicians in Japan.
The rural quota policy, however, could present problems that distort the intended outcome. First, most 'community quotas' do not impose an obligation and depend on students' desire to practice in their home prefecture or in rural communities, and students can change their minds in the course of their undergraduate and residency training. Second, while the rural quotas impose an 'obligation' on students, each school has its own penalty charges for breach of this obligation. The quota students of schools where breach of contract penalties are relatively light may be more likely to pay the charges for release. Finally, the scheme's structure may undermine the motivation of quota students to serve rurally. For example, if five rural quota students to spend 6 years with 100 non-quota colleagues, who have no obligation and a free choice of speciality and practice, their commitment to rural service could be eroded, resulting in a substantial proportion breaching their obligation.
Lessons learned
Contractual rural service programs in other countries
There are various existing international JMU-like financial incentive programs to attract physicians to rural and underserved areas. The programs are, in most cases, conducted on the basis of binding scholarships for medical students, and loan forgiveness programs for young physicians26. Other than JMU, such programs exist, for example, in the USA27, Australia28, Canada29, New Zealand30, South Africa31 and Mexico32. Some of these programs are reportedly effective in increasing the number of physicians in their target areas26.
Transferability of the Japan-style rural health manpower policies
The public sector-led physician securing system in rural areas, which has been maintained consistently in post-war Japan, was only possible because the government, prefectures, municipalities and JMU had strong ties. This Japan-style system has some advantages and disadvantages. The greatest advantage of this type of socialised health manpower securing system is that, in contrast to a system that relies on the market economy for physician distribution, it can attract physicians to rural areas. Another advantage is that a binding medical education system like JMU offers an opportunity to talented young people who hope to be physicians but cannot afford medical school fees. A disadvantage is that the Japan-style system imposes a financial burden on national and local governments. A potential disadvantage is that JMU-like binding programs cause a conflict between the student's social obligation and his or her freedom to choose where to practice. In this regard, the conflict may become more obvious as Japanese society becomes more Westernised and individualistic.
The Japan-style rural health manpower policies, therefore, would be most effective in countries where the public sector has the greatest responsibility for providing rural health care. Japan-style policies would also work in societies where many young people have to abandon their plans to attend medical schools for financial reasons, and in societies where attachment to freedom of location choice does not prevail over the sense of obligation to society. Many developing countries meet these criteria.
In many developing countries, the exodus of physicians abroad and the shortage of physicians in rural areas are serious problems. Based on the experience of Japan, concerted efforts from the public sector and a strong rural physician production system are the keys to solving these problems.
References
1. International Conference on Primary Health Care. Declaration of Alma-Ata. (Online) 1978. Available: http://www.who.int/hpr/NPH/docs/declaration_almaata.pdf (Accessed 15 April 2009).
2. WONCA Working Party on Rural Practice. Health for all Rural People: The Durban Declaration. (Online) 1997. Available: http://www.globalfamilydoctor.com/aboutWonca/working_groups/rural_training/durban_declaration.htm (Accessed 31 July 2009).
3. Ministry of Health and Welfare. Ishi shikaishi yakuzaisho chosa 1971 [The national physician census 1971]. Tokyo, Japan: The Ministry, 1972.
4. Ministry of Health and Welfare. Ishi shikaishi yakuzaisho chosa 1967 [The national physician census 1967]. Tokyo: The Ministry, 1968.
5. Ministry of Health, Labour and Welfare. Muichiku tou chosa [Survey of non-physician communities]. Tokyo, Japan: The Ministry, 2004.
6. Ikegami N, Campbell JC. The art of balance in health policy: maintaining Japan's low-cost, egalitarian system. Japanese edition. Tokyo: Chuko-shinsyo; 1996.
7. Inoue K, Hirayama Y, Igarashi M. A medical school for rural areas. Medical Education 1997; 31: 430-434.
8. Matsumoto M, Okayama M, Inoue K, Kajii E. High-tech rural clinics and hospitals in Japan: a comparison to the Japanese average. Australian Journal of Rural Health 2004; 12: 215-219.
9. Asano N, Kobayashi Y, Kano K. Issues of intervention aimed at preventing prospective surplus of physicians in Japan. Medical Education 2001; 35: 488-494.
10. Takayashiki A, Okayama M, Mise J, Kajii E. The birthplaces of medical students and their intentions of rural practice [Igakusei no syusshinchi to syourai no hekichikinmu kibou.] Primary Care (Tokyo) 2003; 26(Suppl): 142. (in Japanese)
11. Matsumoto M, Inoue K, Kajii E. Characteristics of medical students with rural origin: implications for selective admission policies. Health Policy 2008; 87: 194-202.
12. Ministry of Health, Labour and Welfare. Iryo-sisetsu chosa 2005 [Health Facility Census 2005]; Tokyo, Japan: The Ministry, 2005.
13. Matsumoto M, Inoue K, Kajii E. Rural practice evaluation: how do rural physicians evaluate their working conditions? Australian Journal of Rural Health 2001; 9: 64-68.
14. Matsumoto M, Okayama M, Kajii E. Rural doctors' satisfaction in Japan: a nationwide survey. Australian Journal of Rural Health 2004; 12: 40-48.
15. Union of Prefectural Governors and Jichi Medical School. Jichi ikadaigaku no ayumi [Footsteps of Jichi Medical School]. Tochigi, Japan: The Union and the School, 1974.
16. Anon. A series: Taiwanese in Japan (11th Story). In: Asahi Shinbun Newspaper; 30 March 2010. Available: http://www.asahi.com/special/kajin/TKY201003300340.html (Accessed 2 April 2010).
17. Matsumoto M, Kajii E. Medical education program with obligatory rural service: analysis of factors associated with obligation compliance. Health Policy 2009; 90: 125-132.
18. Matsumoto M, Inoue K, Kajii E. Contract-based training system for rural physicians: follow-up of Jichi Medical University graduates (1978-2006). Journal of Rural Health 2008; 24: 360-368.
19. Matsumoto M, Inoue K, Kajii E. Long-term effect of the home prefecture recruiting scheme of Jichi Medical University. Rural and Remote Health 8:930. (Online) 2008. Available: www.rrh.org.au.org (Accessed 27 May 2010).
20. Kobayashi Y, Takaki H. Geographic distribution of physicians in Japan. The Lancet 1992; 340: 1391-1393.
21. Inoue K, Matsumoto M, Toyokawa S, Kobayashi Y. Transition of physician distribution (1980-2002) in Japan and factors predicting future rural practice. Rural and Remote Health 2009; 9: 1070.
22. Kobayashi Y. Ishisu to ishi no bunpu [The number of physicians and their distribution]. Iryokeizai Kenkyu 2006; 18: 142-146.
23. Organisation for Economic Co-operation and Development. OECD health data. Paris, France: OECD, 2006.
24. Toyabe S. Trend in geographic distribution of physicians in Japan. International Journal for Equity in Health 2009; 8: 5.
25. Imamichi H. Igakubu chiikiwaku nyugaku eno teigen: naigai no chiken oyobi chosa kara [Proposals to medical school rural quota admission: review of past literature and a survey report]. Kousei roudou kagaku kenkyuhi buntanhoukokusyo. Tokyo: Ministry of Health, Labour and Welfare, 2009.
26. Barnighausen T, Bloom DE. Financial incentives for return of service in underserved areas: a systematic review. BMC Health Services Research 2009; 9: 86.
27. Weaver DL. The National Health Service Corps: a partner in rural medical education. Academic Medicine 1990; 65: S43-44.
28. Department of Health and Ageing, Australian Government. Medical Rural Bonded (MRB) Scholarships. (Online) 2008. Available: http://www.health.gov.au/mrbscholarships (Accessed 12 May 2008).
29. Anderson M, Rosenberg MW. Ontario's underserviced area program revisited: an indirect analysis. Social Science & Medicine 1990; 30: 35-44.
30. Dunbabin JS, McEwin K, Cameron I. Postgraduate medical placements in rural areas: their impact on the rural medical workforce. Rural and Remote Health 6:481. (Online) 2006. Available: www.rrh.org.au.org (Accessed 27 May 2010).
31. Ross AJ. Success of a scholarship scheme for rural students. South African Medical Journal 2007; 97: 1087-1090.
32. Nigenda G. The regional distribution of doctors in Mexico, 1930-1990: a policy assessment. Health Policy 1997; 39: 107-122.


