Introduction
Group A streptococcal (GAS) infections cause significant morbidity and mortality in Aboriginal and Torres Strait Islander people in Australia1. Of particular concern are acute rheumatic fever (ARF) and its sequela rheumatic heart disease (RHD). Both diseases have rates among the highest in the world in Indigenous Australians1 with hospitalisation rates 6 to 8 times higher than for non-Indigenous Australians2. Prophylaxis is available to prevent recurrent episodes of ARF with an intramuscular injection (IMI) of benzathine penicillin G (BPG) administered every 28 days for a minimum of 10 years after diagnosis3.
In the Northern Territory (NT) poor uptake of prophylactic BPG has meant recurrent ARF episodes continue to occur4. Reasons contributing to the poor uptake include: inconvenience, lack of family support, lack of confidence, forgetting, mobility between communities and uncertainty about when the injection is due5. To improve the uptake of prophylaxis RHD programs in Darwin and Alice Springs were established to progressively introduce control strategies4.
The concept of using the full moon as a reminder for penicillin prophylaxis was suggested by both clients and primary care providers in Central Australia. The full moon provides a reliable, timely and readily available reminder that 4 weeks have passed, and this strategy makes use of an appropriate concept for people who have low levels of English literacy, limited access to calendars, and may spend much of their lives outdoors. Thus, the Full Moon Strategy was conceived to complement other strategies aimed at improving the uptake of 4 weekly prophylaxis. The Alice Springs RHD program developed and implemented the Full Moon Strategy, using the full moon as a reminder to both clients at risk of RHD and healthcare workers that the prophylactic BPG is due.
From June 2006, Central Australian RHD program staff began informing and educating clients and healthcare workers about the Full Moon Strategy. The RHD program then collaborated with the Health Promotion, and Media and Corporate Communications Units of Department of Health and Families (DHF) to develop the media campaign and health promotion materials that were in use from June 2007. These included:
- calendar posters for display in a clinic showing the dates of the full moon
- personal calendar cards showing the dates of the full moon
- revision of the RHD flipchart to include the dates of the full moon
- radio advertisements played 6 times each day from 3 days before to 3 days after the full moon from June 2007 to July 2008 (42 broadcasts per full moon cycle).
The evaluation aimed to assess:
- Whether clients requiring BPG and healthcare workers were aware of and understood the Full Moon Strategy.
- Whether there was an impact on the timing and uptake of BPG since the commencement of the Full Moon Strategy.
Methods
The evaluation was conducted in four remote Aboriginal communities, encompassing an approximate population of 3400, and the Alice Springs town camps, population 2000 (unpubl. data; Central Australian Remote Health Services, Department of Health and Families, Alice Springs; 2008)6. Interviews were conducted from February to August 2008 in the remote communities, and from November to December 2008 in the town camps.
Eligible participants were clients in the RHD database who were prescribed BPG and were resident in the communities and camps at the time of the evaluation. Each client was visited at home and invited to participate. Consenting participants or their parent/carers were then interviewed by an Aboriginal researcher from DHF for remote communities, or from Tangentyere Council, one of the major service delivery organisations for people in the town camps. Interviews were written in English and conducted in English and Aboriginal languages as determined by the Aboriginal interviewer. Clinic charts and the RHD database were reviewed to collect information on prophylaxis given to clients who had been interviewed.
Primary healthcare workers were identified during the study visit to the remote communities and invited to participate. They were interviewed by non-Aboriginal researchers who were employed in the RHD Program or Health Promotion Unit.
Data were entered into a Microsoft Access database and analysed using Stata Statistical Software v10 (StataCorp; College Station, TX, USA). Responses to interview questions and BPG doses were reported as percentages. The percentage of participants given prophylaxis was determined by dividing the number of prophylactic doses administered by the total number of doses due for participants that month, using a two-sample test of proportion. The statistical significance of these results was measured using binomial exact 95% confidence intervals (CIs). Dates of the full moon for evaluation of timing of BPG uptake were from the Australian Government Geoscience Australia site7. Ethics approval was received from the Central Australian Human Research Ethics Committee (EC00155).
Results
A total of 110 clients at risk of RHD were identified as being eligible for participation, 55 from the remote communities and 55 from the Alice Springs town camps. Fifty clients (45%; 39 clients at risk of RHD and 11 parents/carers) consented to be interviewed; all were Aboriginal (Table 1). The median age of clients was 28 years (range 8-58) and the majority were female (n = 41; 82%).
Also interviewed were 19 healthcare workers from the remote communities, of whom nine were Aboriginal (47%). Their median age was 38 years (range 23-62) and 13 were female (68%).
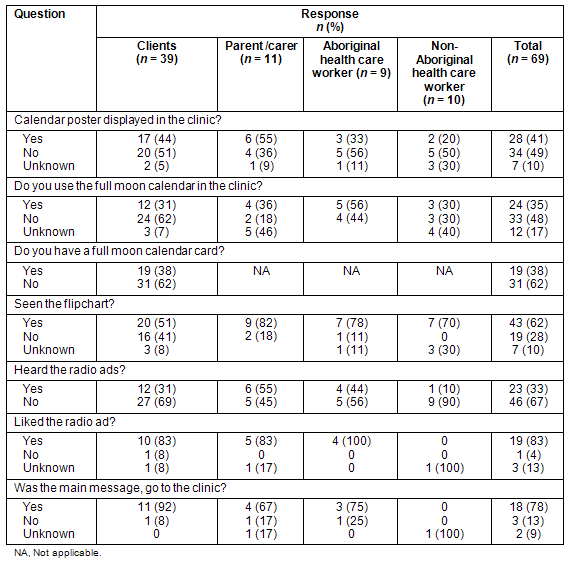
Table 1: Responses to the questions asked about the health promotion tools from clients at risk of rheumatic heart disease, parent/carers and healthcare workers
Calendar poster
Of the 50 clients at risk of RHD or their parents/carers, 23 (46%) had seen the calendar poster at the clinic and 19 of those (83%) knew the purpose was to remind people when BPG was due (Table 1). Having seen the calendar poster, 16 (70%) stated they checked to see when their prophylaxis was due.
Of the 19 healthcare workers asked about the calendar poster, nine said that they had seen it displayed and eight had used it in the clinic. The most common reason the calendar was not displayed, from four healthcare workers, was that they did not have the calendar.
Personal calendar card
Of the 50 clients at risk of RHD or their parents/carers, 19 (38%) had a personal calendar card. Twelve interviewees (24%) had never been given a card while seven (14%) had lost their card. From the 19 healthcare workers interviewed, nine reported giving the calendar cards to all clients who needed BPG prophylaxis.
Flipchart
The flipchart was seen by 29 clients (58%) at risk of RHD or their parents/carers. Questions on the usefulness of the flipchart were asked of clients at risk of RHD. More than one response could be given for each question and the most common of the 66 responses reported that it 'confirmed when you were due to receive your BPG' (n = 23; 35%).
Fourteen healthcare (74%) workers had seen the flipchart, seven stated that they used it sometimes, six said they never used it and one person used it all the time.
Radio advertisements
For the purpose of assessing awareness of the radio advertisements, the responses were combined for all 69 interviewees, of whom 23 (33%) said that they had heard the radio advertisements. Of the 23 participants who heard the radio advertisement, 19 (82%) liked the content and 18 (78%) understood the main message of 'going to the clinic to get your needles'.
Benzathine penicillin injections
Of the 50 RHD clients or their parents/carers who were interviewed, all consented to review of their medical records. Three were excluded from analysis because their prophylaxis ceased before June 2004. From June 2004 to May 2006, before the Full Moon Strategy commenced, 22% (95% CI 18, 27) of penicillin prophylaxis was administered during the week of the full moon but uptake fluctuated widely during this period. Whereas the proportion receiving penicillin prophylaxis during the week of the full moon was not substantially higher for the period June 2006-May 2008 (24%, 95% CI 21, 28), it was notably more consistent (Fig1). The overall uptake of BPG during the latter period (June 2006-May 2008) was 57% (95% CI 56, 60) - an absolute increase of 10% (95% CI 6,15 p <0.01) compared with the June 2004-May 2006 period when overall uptake was 47% (95% CI 44,51).
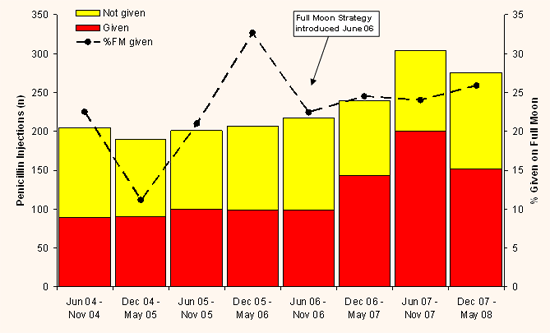
Figure 1: Penicillin prophylaxis due each month and percentage of doses administered during the week of the full moon, June 2004-June 2008.
Discussion
The Full Moon Strategy and the use of its promotional tools appear to have resulted in more consistent receipt of prophylaxis around the full moon but not a dramatic increase in uptake at the time of the evaluation. The overall increase in uptake of monthly prophylaxis to 57% is encouraging but relatively moderate in comparison with the earlier period (47%), highlighting that a substantial improvement is still required before high uptake rates are achieved in this very high risk population.
The limited gains observed may not necessarily be directly attributable to the Full Moon Strategy. Similar moderate gains were reported following the establishment of the RHD register in 2001 where adherence to prophylaxis uptake in four sentinel sites in Central Australia was reported to have increased from 55% in 2000 to 68% in 20028. The uptake of penicillin prophylaxis in Central Australia from the sentinel sites and our study have shown a significant increase in prophylaxis has occurred after each program intervention, although the sentinel site interventions were site specific and not generalized to the region. Other factors that may have influenced the uptake in penicillin prophylaxis during the period of the Full Moon Strategy evaluation include the high rates of changes in staffing in both primary healthcare services and the RHD program. There were also interruptions to the supply of BPG in 2004 and 2006. However neither the staff changes or the interruptions to BPG supply appear to have reduced the number of injections given during this study period9.
The flipchart was the most recognised health promotional tool used in the Full Moon Strategy. It was not a new tool, having first been introduced by the RHD program in 2002; however, the flipchart was adapted to include the full moon calendar. While the radio advertisement was the least known promotional tool, one-third of interviewees recalled the advertisement. In comparison, in a recent media campaign in Queensland, Australia 17% of participants could recall an advertising message without prompting, 83% could recall a television advertisement with prompting and 20% a poster with prompting10. The present results were consistently higher than those experienced in Queensland and support the use of media campaigns as health promotional tools.
Other issues raised in this project are the importance of full implementation of health promotion strategies. Reasons that resources were not used included healthcare workers not being aware of them; and clients not receiving them.
The clients at risk of RHD who were not interviewed were people who were either not in the community at the time the interviewers visited or were not located during the 1-2 day visit. As consent was not obtained to review their records for prophylaxis uptake, it was not possible to make comparisons between those who were interviewed and those who were not. Most of those interviewed were female but this is consistent with the known preponderance of ARF and RHD in Indigenous Australian females11.
The interviews conducted by the RHD program were with available health staff in the remote communities (approximately 5-8 staff per community). While the potential for conflict of interest or information bias for the RHD program interviewers was recognised, this does not appear to have biased the findings with respect to BPG uptake for which the overall gains were modest. The interviewed staff were unaware of the plan to assess coverage relative to the timing of the full moon. Given the high turnover in the RHD program staff during the course of the project, it is thought unlikely that staff would have recruited clients based on their compliance with BPG during the full moon and, in practice, it was expected that most new staff members would be unaware of what education had been given previously.
Multiple interviewers were also used to interview the clients at risk of RHD and/or their parents or carers in the different communities because English is not the first spoken language and a range of local languages are spoken in the communities. The use of multiple interviewers is an acknowledged limitation to this study, providing the potential for inconsistencies among interviewers. The authors endeavoured to ensure the consistency of the interview process by conducting a joint training workshop for all interviewers and involving them in the adaptation of the interview tool. In the authors' view, the clear advantage of having multiple interviewers concerned obtaining informed consent and ensuring that the questions asked were understood (ie the interviewers had knowledge of the local language within their community).
Conclusion
There are a number of clear limitations to this study, including: the small number of participants; the retrospective time period as a comparison of uptake; and the absence of control of other confounding factors. However, the encouraging results suggest the Full Moon Strategy is worth continuing with to observe whether uptake will continue to improve. The significant increase in prophylaxis and a more consistent uptake around the time of the full moon suggest that the Full Moon Strategy may have been effective. While this is an encouraging result, the current uptake of BPG is clearly inadequate to prevent recurrent episodes of rheumatic fever. Innovative control measures and ongoing support and training of RHD staff are still required to make improvements in the rates of heart disease among Aboriginal and Torres Strait Islander people.
Acknowledgements
The authors gratefully acknowledge the involvement of the following Central Australian communities and health services: Hermannsberg, Ti Tree, Yuendumu, Santa Teresa, Central Australian Aboriginal Congress and Alice Springs town camps. We thank the study participants, their families, the health clinics and other community organisations for their support. We also acknowledge the evaluation staff and local health workers for their commitment and contribution: Prue Crouch, Eleanor Hooke, Melissa Fidock, Alan Palmer, Nola Wilson, Jeannie Campbell, Lynette Windsor, Marion Swift, Denise Foster, Vanessa Davis, Audrey McCormack, Dianne Impu and Tiara Foster.
References
1. Carapetis J, Steer A, Mulholland E, Weber M. The global burden of group A streptococcal diseases. The Lancet Infectious Diseases 2005; 5(11): 685-694.
2. Australian Institute of Health and Welfare, Field B. Rheumatic heart disease: all but forgotten in Australia except among Aboriginal and Torres Strait Islander people 2004. Bulletin no 16 (cat no AUS 48). Canberra, ACT: AIHW, 2004.
3. National Heart Foundation of Australia and the Cardiac Society of Australia and New Zealand. Diagnosis and management of acute rheumatic fever and rheumatic heart disease in Australia - an evidence-based review. Canberra, ACT: National Heart Foundation of Australia, 2006.
4. Edwards K. The Acute Rheumatic Fever/Rheumatic Heart Disease Program - an update. The Northern Territory Disease Control Bulletin 2007; 14(2): 26-28.
5. Harrington Z, Thomas D, Currie B, Bulkanhawuy J. Challenging perceptions of non-compliance with rheumatic fever prophylaxis in a remote Aboriginal community. Medical Journal of Australia 2006; 184(10): 514-517.
6. Foster D, Mitchell J, Ulrik J, Williams R. Population and Mobility in the Town Camps of Alice Springs. Alice Springs, NT: Tangentyere Council Research Unit, Desert Knowledge Cooperative Research Centre, 2005.
7. Australian Government Geoscience Australia. Moon Phase Data. (Online) no date. Available: http://www.ga.gov.au/geodesy/astro/moonphases/moonphases.jsp (Accessed 16 January 2008).
8. Brown A, Purton L, Schaeffer G, Wheaton G, White A, Committee ftCARS. Central Australian Rheumatic Heart Disease Program. A report to the commonwealth Novermber 2002. The Northern Territory Disease Control Bulletin 2003; 10(1): 1-8.
9. Currie B. Benzathine penicillin - down but not out. The Northern Territory Disease Control Bulletin 2006; 13(2): 1-3.
10. Queensland Transport. Transport Security Campaign Evaluation Final Report 2007. (Online) 2007. Available: www.transport.qld.gov.au/resources/file/eb04e74283d20a5/01_pages01_13_introduction.pdf (Accessed 29 July 2010).
11. Carapetis J, Wolff D, Currie B. Acute rheumatic fever and rheumatic heart disease in the top end of Australia's Northern Territory. Medical Journal of Australia 1996; 164(3): 146-149.




