Introduction
Rural communities confront greater difficulties than urban areas in maintaining an effective health workforce. Rurality is associated with higher levels of physical risk, lower population densities, scarcity of services and threats to the sustainability of services1. These characteristics are accompanied by shortages of qualified professionals2, transport difficulties, long waiting lists, lack of after-hours services and high fixed costs per service. Though much research has focused on doctors, and there are some questions regarding the validity of conclusions regarding strategies3-5, relevant research indicates the difficulties that confront mental health professionals in rural areas. These difficulties include professional isolation6,7, limited access to professional development and training8, inadequacies of management support in the government system9 and sole practice10, and lack of professional support11,12, interagency cooperation13 and teamwork10. Rural professionals also confront personal isolation7, cultural strangeness14, lack of spousal employment, housing and quality schooling14. They report heavy workloads and high levels of distress and burnout10,15,16.
The strength of the workforce literature is that it focuses on the perspective of the worker. The literature highlights issues such as attractors and reasons for workers to extend work in rural and remote areas (eg social and community attractiveness), barriers to remaining and reasons for leaving and issues of supervision and support. An important weakness, however, is that very few studies have examined the viewpoint of mental health managers, CEOs of non-government agencies, regional policy personnel or senior mental health practitioners/clinicians as key informants. Only three previous studies sought the perspective of senior mental health leaders in rural areas. The single Australian study13 focused on general issues for rural and remote health providers rather than those of mental health recruitment and retention. Two US studies by Glassen et al17 and McDowell et al18 examined the perceptions of rural hospital CEOs regarding the barriers to and strategies in the recruitment and retention of healthcare professionals. In these studies, CEOs suggested that a community needs to be 'attractive' to health professionals, implying the extent of the community's support for families and extent of professional cooperation. The second study, by MacDowell et al18 found that the single most important positive factor in the recruitment of health professionals was their favourable perception of the public school system. Although outlining the views of CEOs, the questions in the survey instrument were based on the results of past research with workers and, therefore, the answers were framed by practitioners' interpretations and did not provide managers' views unqualified by the survey instrument. The study was not focused on mental health or Australia.
The lack of senior mental health leaders' perspectives is a serious gap in the rural mental health literature. It was thought that the views of such leaders from across Gippsland as key regional informants would provide broad and well-founded understandings of central challenges facing the mental health workforce in the region, particularly in terms of the recruitment, retention and training of professional staff. The current study was accordingly designed as a phenomenological study, focused on gaining those managers' views of the mental health workforce in Gippsland, a large and fairly sparsely settled area of south-eastern Victoria12, with a population of approximately 240 00019. Scores on the ARIA+ scale, the 'standard Australian Bureau of Statistics endorsed measure of remoteness ... derived from measures of road distance between populated localities and five] service centres'20, range from 0 (major city) to 12 (very remote area). In 2006, Statistical Local Areas in Gippsland ranged from a low index of 0.91 for Latrobe (C, Moe) to a high of 5.97 for East Gippsland (Orbost)20. On the SIEFA Index for Relative Socio-Economic Disadvantage, on which a low score indicates a high level of disadvantage, four of the seven Gippsland Local Government Areas - Latrobe (at number 8), East Gippsland (15), Wellington (26) and Bass Coast (28) - rank in the lowest one-third of 80, and Baw Baw and South Gippsland rank at around the mean (47 and 48, respectively) (Table 121).
In addition, the study focused on the mental health workforce overall and not specific professional groups. It did this for several reasons. First, like many rural areas, there is a shortage of mental health professionals such as psychiatrists, mental health nurses, psychologists, allied health and social welfare workers. Second, the study was initiated by Monash University's regional Department of Rural and Indigenous Health, whose remit includes all mental health professions. Finally, as became evident in the study, the reality of rural recruitment is that employers often have to consider taking 'whatever they can get' rather than choosing a particular profession to fill a job vacancy.
Methods
Potential participants from the primary health and NGO sector, representing different professional backgrounds, tiers of management and locations, were recruited by an initial phone call. With the support of the Director of Mental Health at Latrobe Regional Hospital, those from the clinical mental health service self-nominated. Each potential participant was subsequently sent a detailed background information sheet and further arrangements for interview made by phone. The total of 24 participants included 17 females and seven males, representing agencies from all areas and shires of Gippsland, including the clinical mental health service, Psychiatric Disability Rehabilitation and Support Services (PDRSS), community health, Divisions of General Practice, small rural health services, non-government agencies, professional groups (eg Australian Psychological Society, Australian Association of Social Workers) and private practitioners. Their professional backgrounds included nursing, psychiatry, medicine, welfare, social work and psychology, and each had between 10 and 30 years' experience in mental health and/or the Gippsland region.
Each participant was interviewed in their place of work during work hours, according to a semi-structured interview that explored issues related to recruitment, retention and training in general, in Gippsland and the particular organisation and locale. Interviews were recorded and transcribed. The research was approved by the Monash University Human Research Ethics Committee.
Following transcription, initial intra- and cross-interview analyses identified central themes in each interview. These analyses were undertaken by the first and second authors independently, seeking to preserve the integrity of participants' meaning and impose as little interpretation as possible. In order to strengthen their validity, the themes and a brief summary of interview were returned to each respondent for comment, correction and refinement22. The first and second authors then checked the validity of their analyses across transcripts, and through discussion, identified a number of recurrent themes that exhibited internal consistency and distinction from each other23, regarding participants' understandings of the issues they face. They also used conventional qualitative content analysis24 to break each transcript into 'units of meaning' consisting of single or grouped phrases and sentences. The number of these units of meaning contributed to the emergence of the themes (Table 1). Occasional comments that differed from those of the majority informed the researchers of issues not otherwise identified or interpreted differently. An example was the insight of one participant, who said that 'I am not so sure that there is a shortage of workers' which differed from the bulk of commentary indicating outright shortage. Interpretation of the data was aided by such comparison and reference to the research literature. Some early findings were discussed with a meeting of nine of the original participants, and the content of this discussion informed and is included in what follows.
Results
The major themes were categorised at a higher order level according to issues either external or internal to the organisations (Table 1). The table also indicates the number of units of meaning that contributed to the emergence of each theme. This weighting was used to suggest a crude hierarchy of informants' perceptions of the urgency of recruitment and retention. The interviews reveal that recruitment, retention and training are conceptually distinct and intertwined, with the issues impacting directly on retention also impacting in a less immediate way on recruitment, and training a significant factor in both recruitment and retention. Findings regarding issues of recruitment and retention are followed by a consideration of training issues.
Issues of recruitment and retention
The issues external to organisations are those of personnel, environment, nature of mental health work and rural location, and issues internal to the organisations those of management and organisational structure and culture. The weightings suggest that recruitment is regarded by managers as a matter of greater urgency than retention or training and that the organisations themselves are of a second order of significance in terms of perceived workforce difficulties. However, to the extent that the organisations are acknowledged, management is critical.
External issues: Informants indicated that the pool of available and potential mental health personnel is limited by global, national and state shortages of suitable workers, competition with metropolitan and intra-regional organisations, inadequacy of specialist training, and the choices of qualified people to work in other careers. The difficulties are heightened in some specialist areas like Child and Adolescent Mental Health Services (CAMHS) and social work, and by the move to tertiary training, and they aggregate to mean that small organisations are often unable to find staff, even to provide temporary relief. Informants indicated that the workforce is predominantly female and divided into younger ('Generation Y') and older ('Baby Boomer') generational cohorts, with the latter dominant in terms of number and authority but ageing and nearing retirement. These cohorts have differing career and personal motivations that influence their decision to take a job, opinion regarding the quality and opportunities offered by the job and decision to stay or leave. Shortages, in particular of medical personnel, mean that psychiatric care relies on overseas workers, many of whom are unfamiliar with the dominant national culture and language, the subtleties of colloquial English and contemporary rural cultures, which as one commented, can be 'very ocker [colloquial Australian English], very Aussie, very country ... not so open minded'.
Table 1: External and internal themes according to recruitment, retention and training issues
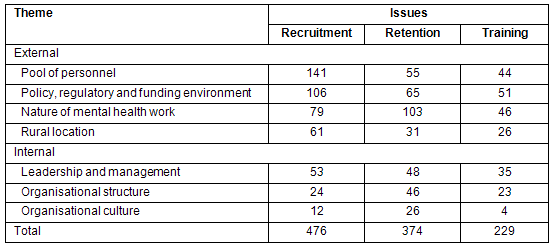
The policy, regulatory, funding and industrial relations environment is dominated by the processes of de-institutionalisation, decentralisation and privatisation on the one hand, and some continuing disciplinary and regulatory structures and industrial relations awards setting workplace responsibilities, salaries and conditions on the other. The juxtaposition produces a system characterised by uneven change, gaps in service and 'all sorts of conflicts in terms of philosophies of care, models of care, [discrepancies between]what a manager or a DHS might consider an indicator of success[and] a clinician may not'. The difficulties are evident to participants in the disparity between award rates for clinical workers and those in the PDRSS sector. As one said:
I think Aldi shelf-packers get more than what this crew [gets] a day.
They are also evident, as another said:
...in a review of family services [that] required a change in the qualifications ... and [that] the people we had ... didn't meet that.
Several informants indicated that funding is a constant problem for small organisations struggling to meet growing need, cover service gaps and overcome confusion surrounding treatment regimes and lines of responsibility. Monies are often provided in 'little buckets', tied like the Medical Benefits Schedule to procedural outcomes that are less appropriate to mental than other health care, rarely sufficient to employ properly qualified workers, and insufficiently flexible to cater to the demands of rural service. It was further suggested that organisations are subject to regulation imposed by professional registration and accreditation regimes that limit their capacity to recruit sufficient numbers of adequately trained people.
Some incentives, like the remote area allowance and Medical Specialist Outreach Assistance Program (MSOAP), are implemented to entice workers to rural regions but thought to have little impact. Others, like Medicare rebates to psychologists, are intended to make psychological services more widely available but can unexpectedly entice professionals away from the public sector.
Informants suggested that mental health is considered a 'not ...particularly appealing speciality to go into', that it rarely provides immediately gratifying outcomes; they also suggested that ignorance and stigma surrounding mental health are a difficulty, as is a relative lack of understanding by professionals of some recently developed programs. The latter is partly a problem, they say, of the fragmentation of state and federally funded services and those provided through private health insurance. They indicate that these factors make mental health a particularly demanding field for their workers, with tension surrounding the challenging and high risk nature of the client group, and the need to deal with suicide and travel alone to clients' sometimes isolated homes. Mental health workers also face an increasing workload, amount of paperwork and constant change. Where it is difficult to find relief staff, these pressures impose on those workers pressure to decide to:
...prioritise those that you think have the highest need and risk [and] being crisis driven, rather than being able to do some of that preventative work.
These pressures, imposed on organisations by the uneven and imperfectly managed change in mental health care in rural localities, are visited on individual workers, producing an enervating sense of hopelessness and 'burnout'.
Participants indicate that these difficulties are magnified where issues of rurality combine with local historical and geographical factors. Rurality means that most services are small, that workers need generalist skills, are required to travel to clients and that opportunities for career progression are limited. It therefore imposes extra demands on workers and costs per employee, and in turn greater demand on the organisation's capacity to recruit and train. Where these additional and peculiar demands are not systemically accounted for, as in regulations and funding guidelines determined according to what are known in the region as 'metropolitan' formulae, organisations' ability to recruit workers, particularly specialists, and retain the more career oriented, is limited. Organisations find that, as some said, they are poaching or 'sucking from each other'.
Rurality can also mean that access to amenities, services and personal opportunities are reduced and professional isolation and exposure to 'ocker' culture increased. These factors are said to influence different professional and demographic groups differently, precipitating change for those with young families as their children reach high school age or spouses find other work. They mean that young people are not expected to stay in the region for long periods, that older workers are more focused on quality of life than career, and that overseas trained professionals rarely stay in the region after gaining Australian qualification. The mix of these issues varies by location and service sector, with difficulties retaining social workers reported in East Gippsland and the area mental health service having a relatively stable workforce in the Latrobe Valley but difficulties in south and west Gippsland. Many issues are shaped by distance from Melbourne, modified by locale-specific factors such as proximity to the railway/highway transport corridor, coastal attraction and size/amenity of town or sub-region.
Internal issues: The weight of commentary in Table 1 suggests that internal issues of leadership and organisational structure and culture are considered less significant to recruitment than external issues. However, leadership was the most important internal factor influencing recruitment, insofar as any management shortcomings made retention problematic, and in turn created a recruitment problem. Participants said that organisational structures can create problems, including the dispersal of some teams that leaves individuals distanced from administration and without direction, while organisational size can limit their capacity to provide professional support and make it difficult to keep and attract specialist staff. Problems of retention that become problems of recruitment were reported to include the practice of restricting executive structures to discipline rather than opening them to skill and ability, the tendency of senior staff to remain for longer periods and so restrict others' opportunities for career advancement, the quality of orientation and induction programs and (in larger organisations) of coordination, lack of workforce planning, and failing to conduct exit interviews. The comment that, 'if you've got a crap culture it won't take long to see your gaps in terms of recruitment and retention' indicated the intimate connection between organisational structure and culture and retention and recruitment. In both recruitment and retention, organisations have limited capacity to provide material incentives to outweigh the disincentives or to meet the needs of potential recruits and current employees.
Training issues: Informants consistently indicated that training was highly important but in a troubled state, that the increasingly complex nature of mental health work is making training ever more important to the provision of effective care and that it is becoming a critical factor in many individuals' decisions to seek and remain in positions. The example of new and emerging models of care such as dual diagnosis were used to demonstrate that effective care now requires a far greater integration of knowledge than previously. It was also reported that workers must now consider a range of issues such as those of risk management, rehabilitation and recovery, culturally-appropriate practice, dual professional and training roles, changing scope of practice, more sophisticated treatment/therapeutic modalities and inter-professional competence. Furthermore, to be effective in rural environments, all personnel, particularly new graduates and overseas psychiatrists, require careful induction in colloquial rural cultures and languages, and support and further training after appointment. Changes in practice and in the policy, funding and regulation environment mean, as a participant said, that you 'require a different knowledge base and skill set when compared to practitioners of just ten years ago'. The centrality of ongoing professional development in these circumstances is reflected in the fact that proof of such development is a requirement for maintenance of registration for a number of professions in the field. This complexity confronts many older workers with cultural and social tensions.
At the same time, there is a shortage of training positions, limited exposure of students to rural work and confused pathways into mental health work. Although there is, as participants suggested, 'quite of bit of mental health education out there', it has been fragmented by the change from earlier more centralised and standardised training regime in the apprenticeship mode, so that some courses and qualifications are not formally accredited and others are inadequate to emerging workplace roles. Some graduates are entering the workforce with inadequate skills, with some courses not 'leading to anything' and others not providing pathways: 'there is [now] no avenue, no direct pathway' into mental health work. The current training arrangements do not provide for direct entry into mental health nursing, and the time out of the workforce involved with university training limits the number of new entrants to the field. Basic and continuing training appropriate to this new work environment tends to be siloed within disciplines, professions and sectors. Many participants indicated that the funding available to organisations is similarly not sufficiently malleable to meet training needs that are both newly emerging and locally specific, and is most often one-off, not sufficient and pre-scribed for use in particular ways.
In addition, continuing professional education and training is reported to be difficult to provide in rural areas where funding inadequately meets needs, and there is really 'not a broad inter-professional approach' and very few 'off-the-shelf inter-professional training packages available'. It was suggested that it was difficult for organisations to identify quality training from the mass available and then manage the costs of sourcing, travel and backfill and organisational adjustment to accommodate it. A consequence is that continuing in-service training is, though vitally important to delivery of service and workforce maintenance, very difficult to implement. These difficulties occur because there is a paucity of training packages that suit needs and it is difficult to get a critical mass for local professional development, so it is mainly held in Melbourne. It was also suggested that the circumstances lead organisations to employ part-time workers, who require the same level of skill and training as full time, which further inflates costs. The costs and time involved in travel to training and the need to provide relief, contribute to the additional costs and tensions imposed by rurality that are not adequately covered in standard funding formulae.
Discussion
The perspective of mental health leaders provided above makes an important contribution to the rural mental health workforce literature. It confirms the difficulties of workforce shortages, rurality and attitudes to mental health work found in other studies2,6,7, highlights a complexity currently confronting mental health service providers, and provides a new understanding of the workforce challenges that that complexity poses, particularly for organisations in rural areas. The complexity centres on a core tension between a growing and increasingly complex mental health demand and a limited capacity to meet that demand. The study indicates that this tension is at the centre of difficulties in attracting and retaining skilled employees, and that managerial leadership is crucial to the capacity of rural mental health organisations to negotiate the tension in a way that ensures both effective delivery of care and a stable workforce.
On the one hand, organisations face an expansion of demand associated with increasing popular and governmental recognition of rural mental health concerns, technologically and evidence-based changes in practice, constantly emerging training needs, changing expectations on the part of workers, and a more diversified rurality (associated with the transport corridor through the region) that is producing locally-specific needs. On the other hand, they face a declining capacity to meet that demand due to factors beyond their control. These factors include the on-going processes of de-centralisation and privatisation of state administrative and regulatory structures, service provision, workforce development and training that are producing fragmentation, dislocation and gaps in service. Together with changing expectations of work-life balance among generational cohorts, tensions at the interface of older and emerging organisational cultures, an expansion of roles and (other than in psychology25) declining numbers entering mental health careers in general, it is more difficult for organisations to meet the need. Though these factors are impacting widely, they are particularly acute in rural and regional areas.
This core tension manifests differently and poses different problems for organisations in different locations. Large regional organisations experience it differently from small NGOs in small centres. All organisations nevertheless share a limited capacity to account for the mental health stigma, cover for the absence of colleagues in training, or provide the kind of professional support and pastoral care that will entice people to apply and remain in positions. The study has highlighted the fundamental importance of innovative leadership in creating the organisational structures and cultures that can do so. Such leadership must focus on nurturing organisational flexibility, in the form for example, of supporting dual work practices to accommodate the different training backgrounds and preferences of different cohorts of workers, or cobbling together funding from several sources to provide training that can ensure workers' adaptability. Management must also be enlightened insofar as it is responsive to individual needs, productive for the organisation and aware of the good of the local and regional community as a whole.
These conclusions make an important addition to the literature. They highlight the centrality of quality leadership and management to the retention of workers and with a flow-on effect to recruitment. The many comments regarding the stigmatised nature of mental health work and relative lack of understanding of the profession (eg among general nurses) are consistent with those of Robertson et al26, who found that among medical students psychiatry is perceived as unattractive and does not command the respect afforded other specialities. The confirmation in this study suggests a need to promote this area of the health workforce to de-stigmatise mental health as a profession.
Conclusion
The focus in this study on senior mental health leaders' perspectives fills a gap in the rural mental health literature. While the views of these key regional informants added another voice to previous literature regarding workforce shortages, issues of rurality and stigma, their viewpoints highlighted the important role of quality leadership and management in the retention and ongoing recruitment of mental health workers in rural areas.
References
1. Australian Institute of Health and Welfare. Rural, regional and remote health: a study on mortality, 2nd edn. Canberra, ACT: AIHW, 2007.
2. Aisbett DL, Boyd CP, Francis KJ, Newnham K, Newnham K. Understanding barriers to mental health service utilization for adolescents in rural Australia. Rural and Remote Health 7: 624. (Online) 2007. Available: www.rrh.org.au (Accessed 9 September 2010).
3. Lea J, Cruickshank M, Paliadelis P, Parmenter G, Sanderson H, Thornberry P. The lure of the bush: do rural placements influence student nurses to seek employment in rural settings? Collegian 2008; 15(2): 77-82.
4. Wilson NW, Couper ID, De Vries E, Reid S, Fish T, Marais BJ et al. A critical review of interventions to redress the inequitable distribution of healthcare professionals to rural and remote areas. Rural and Remote Health 9: 1060. (Online) 2007. Available: www.rrh.org.au (Accessed 9 September 2010).
5. Grobler L, Marais BJ, Mabunda SA, Marindi PN, Reuter H, Volmink J et al. Interventions for increasing the proportion of health professionals practising in rural and other underserved areas. Cochrane Database of Systematic Reviews 2009(1): CD005314.
6. Kowalenko N, Bartik W, Whitefield K, Wignall A. Rural workforce development and staff support: Remodelling service provision for early intervention in child and adolescent mental health. Australasian Psychiatry 2003; 11(Suppl1): S110-S116.
7. Eley D, Young L, Shrapnel M. Rural temperament and character: A new perspective on retention of rural doctors. Australian Journal of Rural Health 2008; 16(1): 12-22.
8. Hodgins G, Judd F, Davis J, Fahey A, Hodgins G, Judd F et al. An integrated approach to general practice mental health training: the importance of context. Australasian Psychiatry 2007; 15(1): 52-57.
9. Bärnighausen T, Bloom DE. Financial incentives for return of service in underserved areas: a systematic review. BMC Health Services Research 2009; 9: 66; doi:10.1186/1472-6963-9-86.
10. Gibb H, Livesey L, Zyla W. At 3 am who the hell do you call? Case management issues in sole practice as a rural community mental health nurse. Australasian Psychiatry 2003; 11(Suppl1): S127-S130.
11. Gardiner M, Sexton R, Durbridge M, Garrard K. The role of psychological well-being in retaining rural general practitioners. Australian Journal of Rural Health 2005; 13(3): 149-155.
12. Hodgins G, Murray G, Donoghue A, Judd F, Petts A, Hodgins G et al. Introducing a professional development programme to a rural area mental health service: the importance of context. Australasian Psychiatry 2004; 12(2): 153-160.
13. Eley RM, Baker PG. Rural and remote health research: Key issues for health providers in southern Queensland. Australian Journal of Rural Health 2007; 15(6): 368-372.
14. Roger AR, Andrilla CHA, Thomas C, Hart LG. Shortages of medical personnel at community health centers: implications for planned expansion. JAMA 2006; 295(9): 1042.
15. Gardiner M, Sexton R, Kearns H, Marshall K. Impact of support initiatives on retaining rural general practitioners. Australian Journal of Rural Health 2006; 14(5): 196-201.
16. Perkins D, Larsen K, Lyle D, Burns P. Securing and retaining a mental health workforce in Far Western New South Wales. Australian Journal of Rural Health 2007; 15(2): 94-98.
17. Glassen M, Peters K, MacDowell M. Rural Illinois hospital chief executive officers' perceptions of provider shortages and issues in rural recruitment and retention. Journal of Rural Health 2006; 22(1): 59-62.
18. MacDowell M, Glasser M, Fitts M, Fratzke M, Peters K. Perspectives on rural health workforce issues: Illinois-arkansas comparison. Journal of Rural Health 2009; 25(2): 35-140.
19. Australian Bureau of Statistics. Local Government Area (LGA) by Age 10 Year Age Groups (AGEP). Canberra, ACT: ABS, 2006.
20. The University of Adelaide. GISCA. (Online) 2010. Available: http://gisca.adelaide.edu.au/projects/category/about_aria.html (Accessed 30 September 2010).
21. The University of Adelaide. ARIA+ by statistical local area. (Online) 2001. Available: http://www.spatialonline.com.au/gisca02/aria_sla/viewer.htm (Accessed 30 September 2010).
22. Lincoln Y, Guba E. Naturalistic inquiry. London: Sage, 1985.
23. Marshall C, Rossman G. Designing qualitative research, 3rd edn. Thousand Oaks, CA: Sage, 1999.
24. Hsieh H-F, Shannon SE. Three approaches to qualitative content analysis. Qualitative Health Research 2005; 15(9: 277-1288.
25. Mental Health Workforce Advisory Committee. Mental health workforce: supply of psychologists. Melbourne, VIC: MHWAC, 2008.
26. Robertson T, Walter G, Soh N, Hunt G, Cleary M, Malhi G. Medical students' attitudes towards a career in psychiatry before and after viewing a promotional DVD. Australasian Psychiatry 2009; 17(4): 311-317.



