Introduction: The poverty, poor environmental living conditions and poor health standards experienced by Aboriginal Australians in some communities in rural and remote Australia have been described recently as 'fourth world'1. For more than a century Aboriginal people have suffered the effects of dispossession of their land; destruction of their traditional culture and values; and exposure to infectious diseases, alcohol and the Western diet that is high in fat and sugar. Collectively these factors have contributed to the prevalence of chronic disease that afflicts Aboriginal people. In particular, renal disease has emerged during the last decade as a major contemporary health problem for Aboriginal Australians.
Several recent studies have highlighted the cultural and financial burden of this disease2-5. According to the latest age- and sex-adjusted figures, Aboriginal people now have approximately nine-fold the risk of non-Aboriginal Australians of developing end-stage renal disease6. In parts of Australia's Northern Territory, where Aboriginal people represent over 20% of the Territory's population, the rates of end-stage renal disease have been described as 'epidemic', reaching 2700 per million in the Tiwi Islands7-8. Calls for the introduction of community-based screening programs for the early detection of renal disease have been widely promulgated4-9.
In response to a request from the Umoona Tjutagku Health Service in mid 1997, the Renal Unit at Flinders Medical Centre, Adelaide, South Australia, formed a partnership with the health service to conduct a renal-disease screening program for adult members of the Umoona Community at Coober Pedy, a town 850 kilometres north of Adelaide. The partnership was later expanded to include screening for children (conducted by the Renal Unit at the Women's and Children's Hospital, Adelaide, South Australia). The community named the program 'The Umoona Kidney Project'.
The Umoona community had recently experienced the dislocation of a number of its older people who suffered from advanced renal disease and were undergoing dialysis in a variety of centres in South Australia and the Northern Territory. As a result, the community had suffered social trauma. Consistent with the community's overall holistic approach to healthcare, the community wanted the renal program to provide a focus for community awareness of and knowledge about chronic disease, as well as to complement existing health programs.
Pathologically, end-stage renal disease among Aboriginal people has been shown to be mainly glomerular in nature10. Renal biopsy studies indicate Aboriginal people have increased rates of glomerulomegaly, mesangiocapillary glomerulonephritis, diabetic nephropathy and non-IgA proliferative glomerulonephritis, compared with the non-Aboriginal population11. Glomerular damage is characterised by albuminuria10. As an integral part of The Umoona Kidney Project, the point-of-care DCA 2000 machine (Bayer Australia, Melbourne, Australia) was used for the first time in an Aboriginal community to detect albuminuria12. The small, portable DCA 2000 (dimensions, 24 x24 x27 cm; 5 kg) measures the urine albumin : creatinine ratio (ACR) on 40 mL urine with an on-site result available in 7 min. Prior to its use in the field, the DCA 2000 underwent a full scientific evaluation13.
This article describes the results of the adult screening program from 1 June 1998 to 31 December 2000, examines the associations between albuminuria and other risk factors for renal disease, and discusses the application of the DCA 2000 point-of-care technology for renal screening in the remote clinical setting.
Methods
Community consultation, program ownership and direction
Prior to commencing the adult screening program, clinical and scientific staff from the Renal Unit at Flinders Medical Centre undertook 6 months of community consultation with the Board of the Umoona Tjutagku Health Service and Umoona community members. This consultation was facilitated by a series of open community forums held during field visits to Coober Pedy. At these meetings the community expressed its concerns about renal disease and its aspirations for the program, resulting in the clearly defined aims and objectives of The Umoona Kidney Project. These aims and objectives included the early detection of renal disease among community members by the implementation of a renal screening program. Ownership of the program resided with the community and the Flinders Medical Centre renal team was responsible to, and directed by, the Board of the Umoona Tjutagku Health Service.
Personnel
The Flinders Medical Centre renal team consisted of a scientist-program manager, two nephrologists, a data manager and a nutritionist. The renal team conducted 20 field visits to the community during the project's three-year duration. The Umoona health team consisted of Aboriginal health workers (with four health workers working on the program across its duration), supported by a clinical nurse. The local medical officer at the Coober Pedy Hospital, the town's general practitioner and nursing staff at the hospital also assisted the program.
Participants
The adult screening program was open to community members who were 18 years or older, and participation was entirely voluntary. Each of the 158 participants gave prior, signed and informed consent.
Screening
At the request of the community, screening was conducted at the health service clinic and began in June 1998. The Aboriginal health workers recorded each participant's height and weight (for calculation of body mass index [BMI]) and measured their blood glucose using a glucose meter (Medisense; Abbott Diagnostics, Sydney, NSW, Australia). Following these test, participants underwent an initial consultation with one of the visiting nephrologists, during which family and personal medical histories were recorded and a medical examination took place, which included lying and standing blood pressure (BP) measurement.
Each participant brought with them a first-morning urine specimen collected in a 75mL sterile container. The urine was tested qualitatively using Multistix (Bayer Australia) dipsticks on the Clinitek 50 Urine Analyser (Bayer Australia) for the presence of protein, glucose, blood, nitrites and leucocytes. Provided the urine specimen was negative for blood, leucocytes and nitrites, the urine was tested on-site with the DCA 2000 for urine ACR. The urine ACR result was handed to the nephrologist during the initial consultation. The nephrologist then provided the participant with immediate feedback on his or her overall risk-factor profile.
Each participant's baseline screening data was recorded on a single-page proforma and the information was transferred electronically on-site to a patient data-management program (designed using Microsoft Access software).
Risk factor assessment
The following parameters were considered risk factors for renal disease:
- Persistent hypertension (>140/>90 mmHg on at least two separate occasions)
- Random blood glucose greater than 11.1 mmol/L (at least twice)
- Persistent albuminuria (urine ACR >3.4 mg/mmol on a first morning specimen14 on at least two separate occasions, with the specimens being negative for leucocytes and nitrites)
- Obesity (BMI >30 kg/m2)
- 'Positive' family or personal medical history, notably a current smoker or consumer of amounts of alcohol greater than 50 g per day for males or greater than 20 g per day for females
- A history of recurrent skin infections.
Repeat measurements necessary to confirm persistent hypertension or albuminuria were conducted either by the Umoona health team between field visits, by the renal team, or by the nephrologist at the next available field visit. The use of first morning specimens for measuring urine ACR was considered preferable to a random sample, which is subject to the potential false-positive effects of posture and exercise and has greater within-person biological variation15-18.
Following initial clinical review, an action plan was developed for each participant and recorded electronically. This action plan detailed further investigations to be performed (notably repeat BP and urine ACR tests), as well as other clinical information to be collected prior to the next field visit (eg current medications).
Ethics approval
Ethics clearance to conduct The Umoona Kidney Project was obtained from the Aboriginal Health Research Ethics Committee of South Australia and the Flinders Medical Centre Committee on Clinical Investigation.
Results
Participation
By January 2001, 158 adults (approximately 65% of the community's total adult population) had undergone a complete screening assessment. Those screened were 58 males (37%; mean age = 43.8 years, range 23-78) and 100 females (63%; mean age = 39.6 years, range 18-72 years).
Overview of screening results
During the three-year screening program, the team's nephrologists conducted 328 patient encounters: 82 people were seen once, 14 people were seen twice, 66 people were seen three times and five people were seen four times. A total of 232 on-site urine ACR measurements were performed.
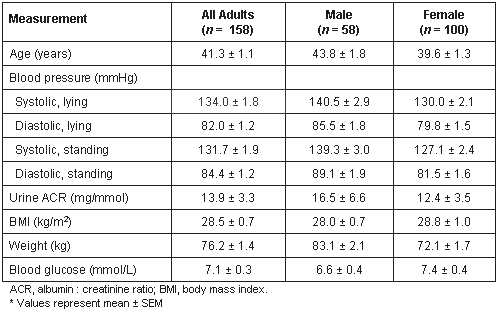
The overall mean (± standard error) of measurements conducted during screening is shown for all adults, as well as by gender (Table 1). Diastolic and systolic BP (lying and standing) and weight were higher in males than in females (p < 0.03 in all cases, unpaired t-test). Blood glucose levels were higher in female participants than in males but the trend was not significant.
Table 1: Summary of measurements conducted during screening of adult population*
Prevalence of risk factors
The overall prevalence of individual risk factors found during community screening is shown (Figure 1).
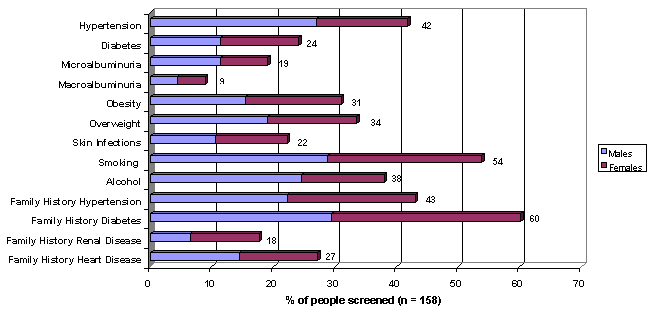
Figure 1: Overall community prevalence of risk factors split by gender. The male : female split shown for each risk factor reflects the relative contribution of gender to the total % of people screened who had positive risk.
Greater than 25% of all adults screened (n = 42/149) had previously undiagnosed persistent microalbuminuria (urine ACR between 3.4 and 34 mg/mol) or macroalbuminuria (>34 mg/mmol). The mean, standard error and range of ACR values found was 16.0 ± 1.8 mg/mmol (3.6-33.1 mg/mmol) for the microalbuminuric group and 114 ± 24 mg/mmol (range 37-349 mg/mmol) for the macroalbuminuric group. Hypertension was found in greater than 40% of the participants (n = 62/148) with a significantly higher rate observed in males (59%) compared with females (32%; p = 0.02, Chi-squared trend analysis). Fifty-eight per cent of participants with hypertension (n = 86/148) were undiagnosed prior to screening. Approximately 25% of all people screened (n = 35/145) had non-insulin dependent (type 2) diabetes mellitus (as assessed by personal history or random blood glucose), and greater than 50% of participants screened also had a positive family history for this condition. Three participants were discovered to have non-insulin dependent diabetes mellitus during screening. Two-thirds of the population surveyed (n = 96/148) was either obese (BMI ³30 m/kg2) or overweight (BMI between 25 and 30 m/kg2). Rates of alcohol and tobacco consumption were high, with greater than 50% of all males drinking to excess and smoking tobacco.
Association between albuminuria and co-existing risk factors
As shown (Table 2), the progression of albuminuria was significantly associated with the following continuous variables: age, diastolic and systolic BP in both lying and standing positions, and blood glucose (p < 0.01 in all cases, ANOVA). These differences remained significant when controlling for age and sex.
Table 2: The association between measured risk factors and ACR category
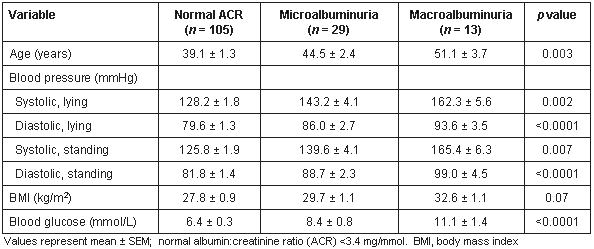
In addition, the categoric variables hypertension, diabetes and obesity all showed strong associations with stratified ACR levels (p<0.02 in all cases, logistic regression analysis, data adjusted for age and sex). An association was also observed between albuminuria and an increasing number of these coexisting categoric risk factors (Figure 2). The proportion of people whose ACR was normal decreased as the number of coexisting risk factors increased. The risk of microalbuminuria was significantly increased in the presence of one or more risk predictors while the risk of macroalbuminuria increased significantly in the presence of two or more coexisting risk factors (Chi-squared trend analysis).
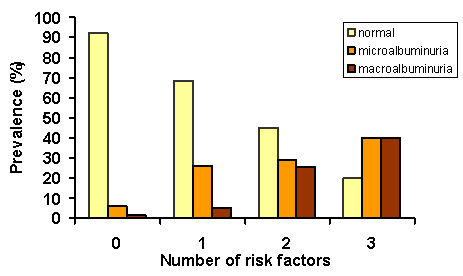
Figure 2: Association between albuminuria and an increased number of coexisting risk factors
Other observations during screening
The screening program also identified non-renal conditions including heart failure (n = 1), angina/myocardial infarction (n = 1), hepatitis B (n = 1), pregnancy (n = 1), bronchiectasis (n = 1), active scabies (n = 1), chronic leg ulcers (n = 1) and sub-mandibular abscess (n = 1).
Discussion
This article details the results of the first comprehensive screening program for renal disease undertaken in a remote Aboriginal community in South Australia, using a point-of-care instrument (the Bayer DCA 2000) as the primary screening tool for quantifying microalbuminuria. The program has identified a significant burden of incipient and established renal disease among adult members of this rural Aboriginal community. The high rates of microalbuminuria (n = 29; 19%) and macroalbuminuria (n = 13; 9%) found in this study are the first reported for an Aboriginal community in South Australia. They are generally consistent with rates reported in Aboriginal communities in other parts of Australia. For example, a study of approximately 1100 Aboriginal adults (> 15 years) from eight communities in central Australia, the Kimberley and Cape York areas in northern Australia reported microalbuminuria rates of 22% for men and 27% for women, while the prevalence of macroalbuminuria was 10% for men and 13.5% for women19. Microalbuminuria rates of 27% have been observed in a large northern Australian community of approximately 700 people5,20.
Albuminuria, if left untreated, may progress from microalbuminuria to macroalbuminuria and renal insufficiency arising from overt albuminuria10,21. Screening for albuminuria using a simple non-invasive urine test, such as urine ACR, is therefore critical because the earlier albuminuria is detected the greater the chance of modifying the progression of the disease. All community members identified with incipient or overt renal disease in The Umoona Kidney Project were offered and accepted the opportunity to participate in tailored clinical and community-based intervention programs that were aimed not only at reducing the burden of renal disease, but also the high rates of associated hypertension, diabetes and obesity found in this community22,23. The clustering of these risk factors with albuminuria is part of the overall metabolic syndrome, and all factors need to be addressed concurrently if an impact is to be made on reducing the chronic disease burden of the community.
Indeed, the screening phase of The Umoona Kidney Project was conducted as part of a broad, family-orientated holistic approach to addressing chronic disease within the Aboriginal community setting. Community awareness programs about renal health, the importance of good nutrition and exercise, and strategies to reduce alcohol and tobacco consumption were conducted at different levels for both Aboriginal Health Workers and adults and children in the community23. The Flinders and Women's and Children's renal teams also formed partnerships with a number of community groups including the Umoona Aged Care Services, the Aboriginal Meals Program, the Coober Pedy Area School and the Tjapa Tjuta Child Care Centre. At the request of the Aboriginal health-worker team, a nutrition training program was developed by the team's nutritionists specifically for the health workers; the content, level, timing and length of this training program determined by the health workers themselves23.
The point-of-care DCA 2000 instrument was the cornerstone of the renal screening program. It proved robust and reliable in a remote clinical setting and demonstrated sound analytical performance characteristics during 30 months of regular field use12. The purchase price of the DCA at approximately $AU6500 and the cost of ACR reagent cartridges at approximately $AU9 each, means the DCA point-of-care technology is a cost competitive, practical alternative to the pathology laboratory for remote communities. The ability of the DCA 2000 to generate an on-site result in 7 min provided an improved service for community members and greater client satisfaction, because results could be discussed with the doctor during the consultation. In the early stages of the screening program, a scientist or technician from the visiting renal team operated the DCA to perform the urine ACR tests. However, following an education and training program in September 1999, Umoona's Aboriginal health-worker team assumed full responsibility for performing urine ACR tests in the latter stages of the program. By performing the tests themselves, health workers have been empowered to take greater responsibility for renal screening in their community, while sustainability and community control and ownership of the program has been ensured. The Umoona Kidney Project was formally handed over to the community in December 2000, with the Flinders renal team still providing clinical, scientific, technical and data management support when appropriate.
Conclusion
The practicability, clinical usefulness and cultural appropriateness of using point-of-care technology in the remote Aboriginal health setting has been clearly demonstrated in The Umoona Kidney Project, and further opportunities exist to broaden the scope and application of point-of-care instruments in community-based screening and management programs.
Acknowledgements
The Umoona Kidney Project was supported by grants from the South Australian Health Commission (1998), the Office for Aboriginal and Torres Strait Islander Health in the Commonwealth Department of Health and Aged Care (1999-2000), Servier Laboratories Australia Pty Ltd, the Australian Kidney Foundation and Janssen-Cilag Pty Ltd. The authors give particular thanks to Barry Young, Managing Director of Servier, who ensured The Umoona Kidney Project came to fruition. All members of the Umoona community are thanked for their participation and long-term support of the program. Maryanne Hudson and Cissie Riessen worked as Aboriginal health workers in the early stages of the program and are acknowledged for their contribution, along with Vicki McCormack and Chris Durden (clinical nurses at Umoona). Ian Crombie (former Chairman of the Board of the Umoona Tjutagku Health Service), Waluwe Simpson-Lyttle and Janice Braun (former Directors of the Umoona health service) all had major input to the program at community level. The dedication and commitment of Karan Lavender (administrative assistant, Renal Unit at Flinders Medical Centre) and our close friends and colleagues at the Women's and Children's Hospital, Adelaide, South Australia (Dr Ken Juriedini, Dr Margie van Renen and Sandra Harris), who worked tirelessly on the concurrent children's-screening arm of the project, is gratefully and sincerely acknowledged.
References
1. O'Donoghue L. Indigenous health: hopes for a new century. John Chalmers Oration. Presented at Flinders Medical Centre, 6 July 2000.
2. Van Buynder P,Gaggin J, Mathews J. Renal disease patterns in Aboriginal Australians. Medical Journal of Australia 1993; 159: 82-87.
3. Hoy W, Mathews J, Pugsley D. Treatment of Aboriginal Australians with end-stage renal disease in the top end of the Northern Territory:1978-1993. Nephrology 1995; 1: 307-313.
4. Thomas MAB. Kidney disease in Australian Aboriginals: time for decisive action. Medical Journal of Australia 1998; 168: 532-533.
5. Hoy W. Renal disease and the environment: lessons from Aboriginal Australia. Nephrology 2001; 6: 19-24.
6. Cass A, McDonald S, Wang Z. Australians with renal disease: a new national survey. Medical Journal of Australia 1999; 171: 444.
7. Hoy W, Baker P, Kelly A et al. Reducing premature death and renal failure in Aboriginal Australians. Medical Journal of Australia 2000; 172: 473-478.
8. Spencer JL, Silva DT, Snelling P et al. An epidemic of renal failure among Australian Aboriginals. Medical Journal of Australia 1998; 168: 537-541.
9. Hoy W. Renal disease in Australian Aboriginals. Medical Journal of Australia 1996; 165: 126-127.
10. Hoy W. Screening for renal disease and other chronic diseases in Aboriginal adults and preliminary experience of a medical intervention program. Nephrology 1998; 4: S90-S95.
11. Seymour AE. Glomerular disease in whites versus Australian aboriginals. 'Last of a race of ruin.' Nephrology Dialysis and Transplantation 1995; 10: 769-770.
12. Shephard M, Allen G. Screening for renal disease in a remote Aboriginal community using the Bayer DCA 2000. Australian Journal of Medical Science 2001; 22: 164-170.
13. Shephard MDS, Barratt L, Simpson-Lyttle W. Is the Bayer DCA 2000 acceptable as a screening instrument for the early detection of renal disease? Annals of Clinical Biochemistry 1999; 36: 393-394.
14. Bennett PH, Haffner S, Kaisiske BL et al. Screening and management of microalbuminuria in patients with diabetes mellitus: recommendations to the scientific advisory board of the National Kidney Foundation from an ad hoc committee of the council on diabetes mellitus of the National Kidney Foundation. American Journal of Kidney Disease 1995; 25: 107-112.
15. Sacks DB, Bruns DE, Goldstein D et al. Guidelines and recommendations for laboratory analysis in the diagnosis and management of diabetes mellitus. Clinical Chemistry 2002; 48: 436-472.
16. Howey JE, Browning MC, Fraser CG. Biologic variation of urinary albumin: consequences for analysis, specimen collection, interpretation of results, and screening programs. American Journal of Kidney Disease 1989; 13: 35-37.
17. Mogensen CE, Keane WF, Bennett PH et al. Prevention of diabetic renal disease with special reference to microalbuminuria. Lancet 1995; 346: 1080-1084.
18. American Diabetes Association. Diabetic nephropathy. Diabetes Care 2002; 25: S85-S89.
19. Rowley KG, Isler DM Best JD et al. Albuminuria in Australian Aboriginal people: prevalence and associations with components of the metabolic syndrome. Diabetologia 2000; 43: 1397-1403.
20. McDonald SP, Wang Z, Hoy WE. Physical and biochemical predictors of death in an Australian Aboriginal cohort. Clinical and Experimental Pharmacology and Physiology 1999; 26: 618-621.
21. Hoy W. Renal disease as a metaphor: towards a more integrated view of Aboriginal health. Clinical and Experimental Pharmacology and Physiology 1998; 25: 1038-1042.
22. Shephard MDS, Brown M, Hudson M, Riessen C, Braun J. The Umoona Kidney Project. Aboriginal Health Worker Journal 2000; 24: 12-15.
23. Zeunert S, Cerro N, Boesch L et al. Nutrition project in a remote Australian Aboriginal community. Journal of Renal Nutrition 2002; 12: 102-106.
Published 8 February 2003; modified 19 August 2003.

