Introduction
As documented in a recent US Surgeon General's report, secondhand smoke (SHS) exposure causes premature death and disease in children and non-smoking adults1. The home is the primary source of SHS exposure for infants and children, and a major source for non-smoking adults2. Children in households with resident smokers are particularly vulnerable to SHS exposure because adults in the home largely have control over the environment. Indeed, while smokers with a child in the home are much more likely to have home smoking restrictions than other smokers3-5, they are still less likely to have such restrictions than the general population4,5.
Efforts to reduce household SHS exposure face unique challenges in circumpolar regions, due to factors such as living conditions, lifestyles and climate6. Previous studies have documented negative health outcomes in children from SHS exposure7-9. However, relatively few studies in circumpolar regions have estimated the prevalence of children's SHS in the homes of smokers and examined factors related to their exposure. Three studies found were conducted in Nordic countries and the their samples limited to households with three-year-old children10-12.
The goal of the present study was to inform the State of Alaska's comprehensive tobacco control program efforts to reduce SHS exposure. Despite program efforts to date, more than one in four Alaskan smokers with children in the home reported SHS at home during the past 30 days13. The program hypothesizes that there is variability in the burden of children's SHS exposure among sub-populations of households with smokers. Discovering which subpopulations carry the greatest burden is important for program targeting.
The objective of this study was to assess how the prevalence of children's SHS exposure in Alaskan households with an adult smoker varies according to rurality, race/ethnicity, income and education, household age composition, marital status, amount smoked each day, and beliefs in SHS health consequences.
Methods
Setting
The US State of Alaska is located in the extreme northwestern region of North America and has a population of less than 700 00014. Although approximately 50% of Alaskans live in a metropolitan area, it is the least densely populated state in the USA. Alaska Native (AN) people comprise approximately 20% of Alaska's population overall, and 44% of its rural population14. The overall smoking prevalence in 2007 was 21.5% (37% among AN, and 17.8% among non-AN people) with 18-39 year-olds smoking at a rate of 25.4%, 40-59 year-olds at 21.6%, and those over 60 years at 11.1%13.
Study design
The study design was a stratified, random, repeated cross-sectional, population based survey. Data were collected between 2004 and 2007 from the Alaska Behavioral Risk Factor Surveillance System (BRFSS) which is part of a national behavioral risk factor system with standardized validated instrument, methods, and quality control techniques15. The BRFSS is a random-digit-dialed, cross-sectional survey stratified on geographic region. Eligible participants are non-institutionalized, aged 18 years or over, and living in Alaska households with a landline telephone (eligible population size, 480 686)16. Those respondents reached in households outside their primary residence were excluded The interviews were conducted by professionally trained interviewers everyday throughout the day, including evenings, using a standardized protocol and took approximately 20 min to complete per interview16. In 2004-2007, the Council of American Survey Research Organizations (CASRO) response rate (ie definition from the CASRO) ranged from 62% to 68%. This project relied on public health surveillance data and did not require institutional review board approval.
Sample
A total of 10 045 respondents completed the survey during the years examined. Of those, 1121 self-identified as current smokers and reported one or more children under 18 years living at home - the sub-sample representing the group of interest in this analysis. Of those 1119 answered the question on secondhand smoke exposure and comprise the final sample. The average number of children in the home of this sub-sample was 2.1 (standard deviation,1.3).
Measures
A brief description of the measures used in these analyses is given. The specific wording of the questions and response categories can be found at the BRFSS website17.
Secondhand smoke exposure
A 'Yes' response by the adult respondent to the question: 'In the past 30 days, has anyone, including yourself, smoked cigarettes, cigars, or pipes anywhere inside your home?' defined a child's SHS exposure in the home.
Demographics
Information was gathered on the respondent's age, education, income, and ages of children living in the home, and number of adults in household. Low socio-economic status was indexed as a combination of income (less than 185% of poverty level) and education (less than high school). Race/ethnicity was defined as the primary reported race. The BRFSS sampling strata defined geographic regions of the state.
Smoking-related measures
Standard BRFSS measures were used for respondent's smoking status and daily cigarette consumption. Also used were standard BRFSS items measuring belief in the harmfulness of SHS and existence of a home smoking rule17.
Statistical analysis
Bivariate associations between household SHS exposure and each of the potential risk factor variables were examined. Presented for each variable is the raw sample size at each response category level, and the weighted percent of the subpopulation at that level, and the percent of SHS exposure at that level with standard error (SE), and the p-value for the Wald χ2 test of association between the variable and home SHS exposure (Table 1). A multiple logistic regression model was used to examine potential confounding between race and other variables.
To conduct analyses SAS 9.1 (SAS Institute; Cary, NC, USA) procedures were used, which took into account the complex survey sampling methodology. Statistical significance was tested at the 5% alpha level.
Results
The prevalence of SHS exposure estimated from the 1119 respondents in the combined 2004-2007 Alaska BRFSS data is presented (Table 1). In the population of smokers living in homes with children, approximately 25% reported SHS exposure in their homes in the last month.
Demographics
Respondents living with children over 5 years of age reported a significantly (p< 0.05) higher prevalence of SHS exposure in the home, compared with those living with younger children. The respondent's age was also significantly related to SHS exposure in the home, with those 40 years and older reporting more exposure than others. A significantly smaller percentage of AN people reported SHS exposure in the home than Whites and those who reported other races. Respondents in extremely rural regions (North, Southwest, and the Interior) had a significantly lower percentage of reported exposure in the home than those living in other regions. Respondents living with no other adults reported significantly higher exposure in the home than others. Secondhand smoke exposure in the home was not found to vary significantly by gender or socio-economic status measures.
Smoking-related variables
Those smoking more cigarettes per day were significantly more likely to have home SHS exposure. In addition, having a ban on smoking in the home was significantly related to SHS exposure in the home. Only 5% of respondents with a 'not allowed' smoking rule reported home SHS exposure, compared with 81-91% of those with only occasional or no restrictions. A total of 74% of all respondents had a 'no smoking' home rule.
Beliefs in secondhand smoke health consequences
No significant relationship was found between SHS exposure in the home and belief in the general harm of SHS. However, an association was found between believing SHS has an effect specifically on Sudden Infant Death Syndrome (SIDS) and less home SHS exposure. Although a large percentage of respondents believed that SHS was harmful (89%), fewer (50%) knew or believed that SHS effected SIDS.
Examination of confounding
To examine potential confounding between AN race and other variables examined, a multivariate logistic regression analysis was conducted. Candidate confounder variables significantly associated with both race and exposure were rural region and cigarette consumption. A model including race and these variables revealed that being of AN race (odds ratio [OR]=0.54 relative to all others, p=.026), 20 or more cigarettes smoked per day (OR=2.98, relative to 1-19 smoked per day, p<.001) remained independent predictors of exposure. The unadjusted OR for being of AN predicting exposure was 0.47 (p=.004).
Table 1: Bivariate associations of respondent characteristics with secondhand smoke exposure in the home
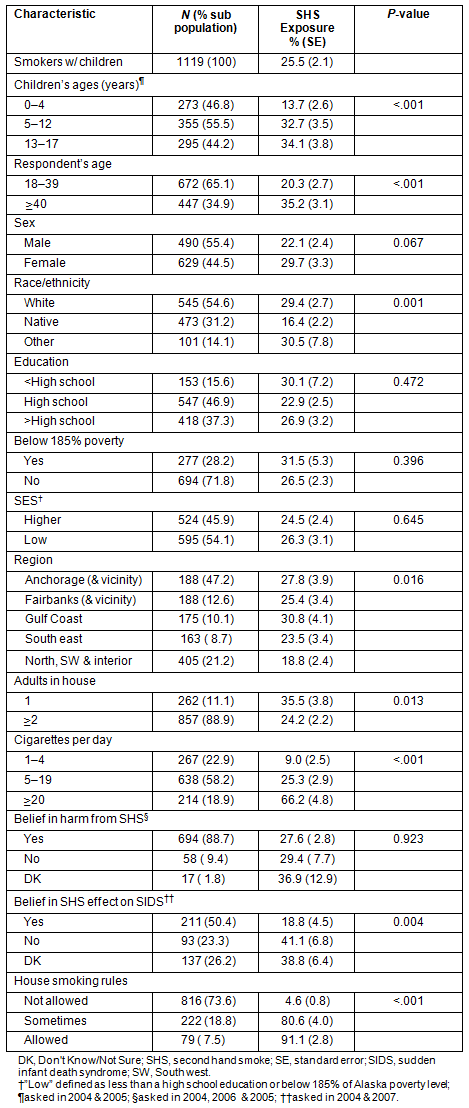
Discussion
In this study over 25% of smokers with children in Alaska reported SHS exposure in their home during the last month, but this estimate varied according to sub-population. Consistent with other studies, children's exposure in the home was found to be associated with their parents being older4, being the only adult in the home3,11,12, and consuming more cigarettes3,11; while having young children in the home was associated with less home SHS exposure3. Alaskan Native households were found to have less home exposures than other races, even after adjusting for other variables. This finding is in contrast to another study of households with a smoker and a child that found Native Americans had as much SHS exposure at home as White households18, but that study was limited to low-income Native American and White households in Oklahoma. Socioeconomic status was not significantly associated with home SHS exposure in our study, regardless of race/ethnicity or region, but has been found to be associated with exposure in other US states5,19 and in Norway10,11.
Limitations
This study has several limitations. First, the data on home SHS exposure are based on a proxy measure of actual child exposures. The survey asked simply if 'anyone' smoked tobacco 'anywhere' inside the home, it did not ask potentially important details related to level of exposure such as the number of persons that smoked or the proximity of the smoker to the children. Moreover, the exposure measure was based on self-report and may have been affected by social desirability. One study in Alaska's Y-K Delta region suggested that SHS exposure among AN may be underreported20, although findings from a study in other northern regions suggested smokers in general accurately report their children's SHS exposure21. Second, although the survey was population based, because the survey was telephone based those people in households without telephones (approximately 3% of households16) could not be reached and are not represented. Third, although multivariate analysis was used to control for several potentially confounding factors, some of the associations found may have been due to other factors not included in these models. Finally, some group categories, such as 'other' race and failure to believe in SHS harm had relatively few respondents, limiting the power to detect an association between those variables and SHS exposure. It was not possible to detect significant associations between SHS and some categories, possibly due to the study lacking sufficient statistical power.
Conclusions
Although it was found that in Alaska most smokers with children believe that SHS is harmful, they should be encouraged to have no-smoking rules in their homes to convert those beliefs into actions. Our finding of low SHS exposure among AN people with children in the home is new and encouraging. Results from this study suggest those with school-aged children, and moderate to heavy smokers should be targeted for intervention, given their high prevalence of home SHS exposure. Future work should examine reasons for low exposure levels among AN people to inform programmatic efforts in other non-indigenous communities.
Acknowledgements
The authors thank Chris Bushore for his insightful comments on the manuscript. This work was supported by the Alaska Tobacco Prevention and Control Program.
References
1. US Department of Health and Human Services. The health consequences of involuntary exposure to tobacco smoke: a report to the surgeon general. Atlanta, GA: 2006.
2. Trosclair A, Babb S, Murphy-Hoefer R, Asman K, Husten C, Malarcher A. State-specific Prevalence's of Smoke-Free Home Rules - United States 1992 - 2003. Morbidity and Mortality Weekly Report 2007; 50(20): 501-504.
3. Berg C, Cox S, Nazir N, Mussulman L, Ahluwalia,J, Ellerbeck E. Correlates of Home Smoking restrictions among rural smokers. Nicotine & Tobacco Research 2006; 8(3): 353-360.
4. Norman G, Ribisl K, Howard-Pitney B, Howard K. Smoking Bans in the Home and Car: Do those who really need them have them? Preventive Medicine 1999; 29: 582-589.
5. Pizacani B, Martin D, Stark M, Koepsell T, Thompson B, Diehr P. Household smoking bans: which households have them and do they work? Preventive Medicine 2003; 36: 99-107.
6. Backer V, Nepper-Christensen S, Porsbjerg C, von Linstow ML, Reersted P. Respiratory symptoms in Greenlanders living in Greenland and Denmark: a population-based study. Annals of Allergy, Asthma and Immunology 2004; 93(1): 76-82.
7. Spengler JD, Jaakkola JJ, Parise H, Katsnelson BA, Privalova LI, Kosheleva AA. Housing characteristics and children's respiratory health in the Russian Federation. American Journal of Public Health 2004; 94(4): 657-662.
8. Lanier AP, Bulkow LR, Novotny TE, Giovino GA, Davis RM. Tobacco use and its consequences in northern populations. Arctic Medical Research 1990; 49(Suppl2): 17-22.
9. Hugg TT, Jaakkola MS, Ruotsalainen RO, Pushkarev VJ, Jaakkola JJK. Parental smoking behaviour and effects of tobacco smoke on childrens health in Finland and Russia. European Journal Of Public Health 2008; 18(1): 55-62.
10. Rise J, Lund KE. Predicting children's level of exposure to environmental tobacco smoke based on two national surveys in Norway in 1995 and 2001. Addictive Behaviors 2005; 30(6): 1267-1271.
11. Lund KE, Skrondal A, Vertio H, Helgason AR. To what extent do parents strive to protect their children from environmental tobacco smoke in the Nordic countries? A population-based study. Tobacco Control 1998; 7(1): 56-60.
12. Helgason AR, Lund KE. Environmental tobacco smoke exposure of young children--attitudes and health-risk awareness in the Nordic countries. Nicotine and Tobacco Research 2001; 3(4): 341-345.
13. Alaska Division of Public Health. Alaska Tobacco Facts, 2009 Update. (Online) 2009. Available: http://www.hss.state.ak.us/dph/chronic/tobacco/alaska_tobacco_facts.pdf (Accessed 23 October 2009).
14. US Census Bureau. Alaska Fact Sheets. (Online) 2009. Available: http://factfinder.census.gov (Accessed 23 October 2009).
15. Nelson DE, Holtzman D, Bolen J, Stanwyck CA, Mack KA. Reliability and validity of BRFSS measures. Preventive Medicine 2001; 46(Suppl1): S3-S42.
16. Alaska Division of Public Health. Behavioral Risk Factor Surveillance System Survey methodology. (Online) 2009. Available: http://www.hss.state.ak.us/dph/chronic/hsl/brfss/method.htm (Accessed 23 October 2009).
17. Centers for Disease Control and Prevention (CDC). Behavioral Risk Factor Surveillance System Survey Questionnaire. (Online) 2004. Available: http://www.cdc.gov/BRfss/questionnaires/english.htm (Accessed 23 October 2009).
18. Kegler M, Malcoe L. Smoking restrictions in the home and car among rural Native American and White families with young children. Preventive Medicine 2002; 35: 344-342.
19. Martinez-Donate A, Hovel M, Hofstetter C, Gonzalez-Perez G, Adams M, Kotay M. Correlates of home smoking bans among Mexican Americans. Tobacco Control 2007; 21(4): 229-236.
20. Helzer LJ, Heitkamp KM, Shein M, Etzel RA. Pilot study of methods to measure saliva cotinine in Alaska Native women during pregnancy. International Journal of Circumpolar Health 2007; 66(Suppl1): 29-38.
21. Patja K, Hakala S, Prättälä R, Ojala K, Boldo E, Öberg M. Adult smoking as a proxy for environmental tobacco smoke exposure among children - comparing the impact of the level of information in Estonia, Finland and Latvia. Preventive Medicine 2009; 49(2-3): 240-244.
Abstract
Introduction: Secondhand smoke (SHS) exposure causes premature death and disease in children and non-smoking adults; the home is the primary source of SHS exposure. The aim of this study was to assess variance in the prevalence of children's SHS exposure in Alaskan households with an adult smoker according to rurality, race/ethnicity, income and education, household age composition, marital status, amount smoked each day, and beliefs in SHS health consequences.
Method: Telephone interviews were conducted between 2004 and 2007 on a population-based random sample of 1119 Alaskan adult smokers with children living in the household.
Results: Respondents living with children over 5 years of age reported a significantly (p <0.05) higher prevalence of home SHS exposure, compared with those living with younger children. Respondents 40 years and older reported significantly more exposure than others. Alaska Native smokers reported significantly lower SHS exposure in their homes than those of other races, as did those living in very rural areas. Respondents' heavier smoking was significantly associated with more SHS exposure. The sub-population of adults living without other adults was approximately 1.5 times more likely to report SHS exposure than those living with other adults. As expected, having a no-smoking rule in the home greatly lowered the risk of SHS exposure in the home.
Conclusions: Although most smokers with children believed that SHS is harmful, some need to convert those beliefs into actions. The results from this study suggest that those with school-aged children, and moderate to heavy smokers should be targeted for intervention, given their high prevalence of home SHS exposure. Future work should examine reasons for low exposure levels among Alaska Native people to inform programmatic efforts in other communities.
Key words: Alaska, child, passive smoking, risk factors, USA.
You might also be interested in:
2016 - Access to chlamydia testing in remote and rural Scotland
2008 - Establishing standards for obstructed labour in a low-income country
2004 - Investigating the health of rural communities: toward framework development
