Rural health workforce issues are a priority area for the Australian Government and substantial funding has been provided for rural education programs to address health workforce disparities across Australia's rural and remote communities1,2. The Australian Government established a Rural Health Strategy in 2001 and there are now 14 Rural Clinical Schools (RCS) in Australia3. The 2008 Urbis Report commissioned by the Australian Government Department of Health and Ageing highlighted the lack of research data on rural programs and workforce outcomes4, essential to ensuring that educational efforts, resources and funding are being concentrated appropriately. In keeping with government policy, the Australian National University (ANU) Medical School aims to have least 25% of each year cohort being students of rural origin, with the same percentage completing half of their clinical training in rural areas as part of a rural stream5.
Most of the preliminary evidence of the success of rural programs is based on positive student evaluation of independent modules and an increase in the number of interns selecting work in regional areas6-8. Further evidence to measure and compare the success of various rural programs will help determine which style of program is most effective in influencing students.
This study examined the ANU Medical School's 4 year rural program in order to understand whether various program components have a direct impact on student intentions to practice in a rural and remote location post-graduation. The study also explores factors that affect student decisions to apply for year-long rural placements.
Background - Australian National University Medical School rural program
The ANU Medical School is a 4 year graduate program that commenced in 2004. Teaching in the first 2 years is problem-based learning, and in the last 2 years students are taught in a clinical environment. The program curriculum covers 4 major themes: (i) medical sciences; (ii) clinical skills; (iii) population health; and (iv) professionalism and leadership. Integrated into these 4 themes are the frameworks of social foundations of medicine, rural experience and Indigenous health.
The ANU RCS was established to deliver an integrated rural training program over Years 1-4 to include both compulsory and elective elements. All students are required to spend a minimum of 8 weeks in structured residential rural placements. In each of Years 1 and 2, students attend 'Rural Week', a compulsory week-long residential session in a rural community. In Year 3, there are two compulsory alternative programs:
- Six week attachment to a medical practice in a south-east (SE) New South Wales (NSW) community or the Northern Territory (NT).
- Elective year-long rural placement, the 'rural stream' in SE NSW.
Students can apply for entry to the Year 3 rural stream program at two admission points: at entry to medical school, or during Year 2. Selection for entry is based on the student's desire to be in this stream for the entire year (expressed through a written statement), and an interview with questions concerning rural life. Incentives provided to students in the rural stream include fully funded accommodation, financial support for relocation, reimbursement of travel expenses and IT equipment/infrastructure at the rural site.
In Year 4, students can choose from 2 to 6 week rural electives in SE NSW in the subject areas of women's health and psychological and addictive medicine. In addition, Year 4 students undertake a 4 week elective which can be in any clinical discipline worldwide.
Survey
The survey in the form of an online, web-based tool was developed for the Year 4 graduating cohort of 2008, with questions based on issues raised in the literature. Participation was anonymous and voluntary during a 4 week period in October 2008.
Students were encouraged to complete the survey by:
- targeted emails to the entire cohort with a link to the survey
- advertisement on student discussion boards and in common rooms
- direct discussion with Year 4 cohort members.
The survey contained 33 forced-answer questions which asked respondents to either select answers from options or to value-rate statements. Where appropriate, comments were permitted to further explain responses. Survey sections covered:
- General information and demographics.
- ANU Rural Program:
- motivations for participating in the year-long placement
- the influence of rural programs on student intention to practice rurally.
- motivations for participating in the year-long placement
- General evaluation:
- Effectiveness of rural program delivery
- Change in student perceptions about rural health and rural issues
- Intention to practice rurally as a direct result of the rural curriculum.
- Effectiveness of rural program delivery
Data analysis
Quantitative data were entered into EpiInfo V3.5.1 (http://wwwn.cdc.gov/epiinfo/) and analyzed for descriptive and frequency statistics. Qualitative data were reviewed and consistent themes among responses extracted.
Ethics clearance
Ethics approval was obtained from the ANU Human Research Ethics Committee. Participant consent was confirmed on entry to the online survey.
Respondent demographics
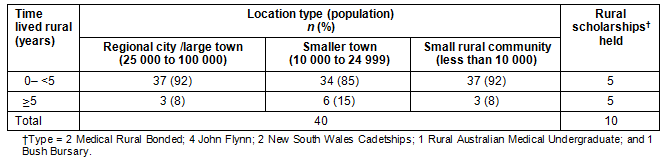
There were 40 survey responses from 88 students, representing 45% of the Year 4 cohort. Most respondents were female (73%), aged 25-29 years (75%) and single (65%) (Table 1). Most respondents (70%) had lived in a metropolitan area for more than 15 years, and up to 15% of respondents had either lived in a regional city, smaller town or small rural community (as defined by the Australian Rural and Remote and Metropolitan Classification [RRMA]) for more than 5 years (Table 2). Respondents held a total of 10 rural scholarships, evenly distributed between students from rural and non-rural backgrounds; 4 respondents (10%) held bonded medical places.
Comparatively, the actual Year 4 cohort comprised of 58 females (66%) and 30 males (34%), with 72% aged under 30 years. The cohort mix included 75% from an urban background, 20% of rural origin and the remainder were international students.
Table 1: Respondent demographic characteristics, according to sex
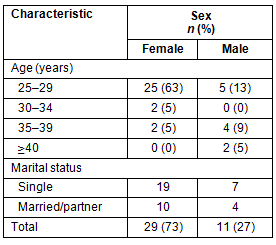
Table 2: Number of years respondents lived in a rural location
Evaluation of Australian National University Medical School rural programs
Rural intention at the commencement and completion of rural programs: In all, 26 of the 40 respondents (65%) indicated that at the commencement of medical school they considered working in a rural and remote area as medical practitioners, and by the end of the course, 33 respondents (82%) indicated their intention to spend time working in an RRMA 3 to RRMA 7 area (large and small rural centre/other rural/remote centre/other remote) during their medical careers. This included 20 respondents (50%) who intended to work between 0 and 5 years, and 13 respondents (32%) for more than 5 years.
Overall, the ANU rural curriculum had a positive effect on 13 respondents (33%) who changed their practice location intention to rural, while 4 respondents (10%) reported that the rural program had a negative effect on their rural practice intention (Table 3). The overall program had no effect on 12 respondents (30%) who were certain of their intentions irrespective of the rural education they received. Although 33 respondents indicated they would spend time working in a rural and remote area, by the end of the survey 11 (28%) were still unsure about eventual rural and remote practive.
Table 3: Influence of overall Australian National University curriculum on respondents, stratified by rural and non-rural origin
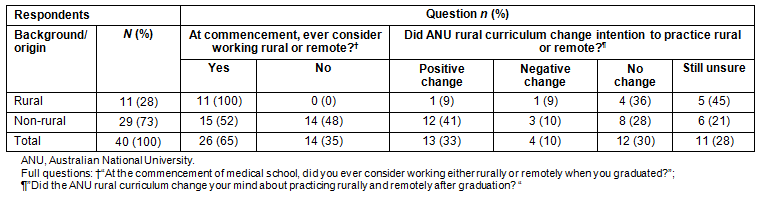
Influence of rural programs on students of rural and non-rural origin: This study defined rural background as living in a non-metropolitan area for more than 5 years. All 11 respondents of rural background indicated that they considered working in rural and remote areas at the commencement of medical school, compared with 15 respondents (52%) of urban background (Table 3). By the end of the overall program, one respondent from a rural background had a positive change in rural practice intention, compared with 12 respondents (41%) of non-rural origin. A larger number of respondents with rural background (36%) were certain about their rural practice intention, compared with those with non-rural background (28%), and more rural background respondents (45%) remained uncertain about rural and remote practice intentions than those of non-rural background (21%).
Direct effects of rural programs: The compulsory components (Years 1 and 2 rural weeks, Year 3 six-week placements) had between 83% and 100% respondent participation (Table 4). From those participating in these programs, 50% indicated they were likely to practice in a rural and remote area as a result of their ANU rural training experience. The proportion of respondents undertaking rural programs on an elective basis ranged from 17% to 25%. Students interested in rural and remote health tended to select these programs, with 75% to 86% of respondents indicating their intention to practice as a direct result of undertaking an elective program.
Table 4: Direct effects of compulsory and elective components of the Australian National University rural program on student intentions to practice in rural and remote areas
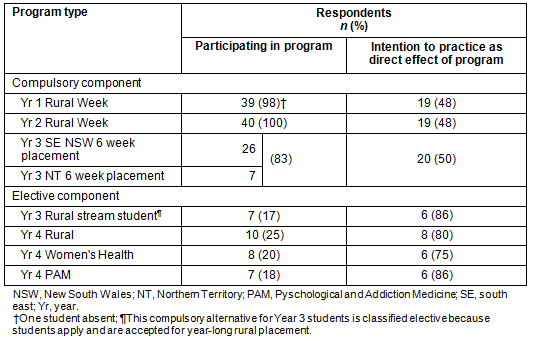
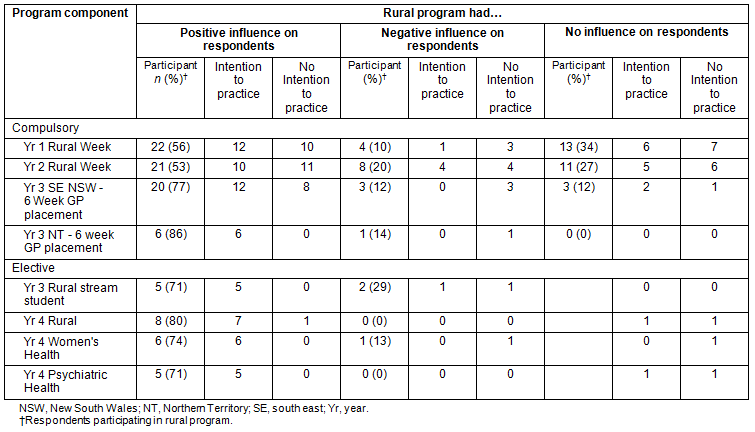
Influence of rural programs on intention to practice: Students were asked whether the rural programs had a positive, negative or neutral influence on their rural intention (Table 5). As a result, 56%, 53% and 77% of students reported the positive influence of Years 1 and 2 rural weeks, and Year 3 placements, but only half had a rural practice intention. In comparison, almost all students who chose a Year 3 year-long placement, 6 week NT placement or a Year 4 elective component reported a positive influence on their intention to practice in a rural and remote area. For both compulsory and elective components, students with negative experiences had no rural practice intention, while for students with neutral experiences, the intentions were evenly divided.
For the 5 respondents who applied to Year 3 rural stream in Year 2, rural weeks were considered very important in encouraging them to apply for or to decide where they would undertake their year long rural program.
There were 6 applications for rural internship among the 40 respondents (15%) and, of these, three had not considered working in a rural or remote area at the commencement of medical school. From this group, two students participated in the year-long placement program. Five of the 6 applicants stated that the ANU rural curriculum changed their intention rural practice, while one applicant always had a rural career intention.
Table 5: Rural program influences and students' intentions for rural and remote practice
Overall evaluation of the Australian National University rural programs: Respondents rated the amount of rural content in the rural curriculum positively, with 29 of the 40 respondents (70%) disagreeing that there should have been less rural focus, and 30 respondents (75%) believing they will be better medical practitioners due to that content. Nearly all respondents, 34 (85%) agreed that the rural programs were delivered in an effective manner.
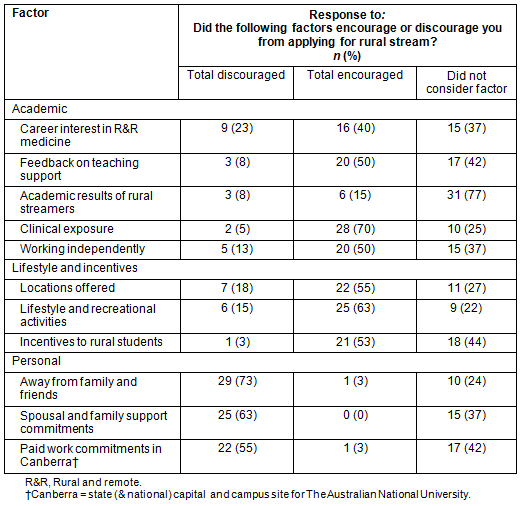
Factors affecting the decision for year-long rural placement (rural stream): Respondents rated factors that encouraged or discouraged their application for a rural stream. The results are presented according to categories of academic, lifestyle/ incentives and personal factors (Table 6). For respondents who considered the factors encouraging, clinical exposure was the most encouraging, followed by rural incentives and feedback on teaching support in deciding whether to apply for rural stream. The personal factors of spending time away from family and friends, work commitments in Canberra and spousal/family support strongly discouraged some respondents from applying for a rural stream. Respondents felt more strongly about discouraging factors associated with personal circumstances than the encouraging factors of academic and lifestyle/incentives when deciding whether to apply for the Year 3 rural stream. Almost 50% of respondents did not consider incentives to rural students, paid work commitments in Canberra and teaching support for rural stream students when deciding to apply for a rural stream.
Table 6: Encouraging and discouraging factors in respondents' applying to the Year 3 rural stream
For the 7 respondents who completed a rural stream, 6 would still have chosen this option, and one was not sure if they would have applied again. There were 6 respondents who were not part of Year 3 rural stream who regretted not applying, and 4 of the 6 respondents commented that family, partner and work commitments were the main reasons that prevented them from applying.
In total, 26 students had no regrets for not applying to rural stream with seven students commenting that family, leaving their partners and work commitments were the main reasons for not applying. Some students felt they received greater exposure to medicine and surgery at the (metropolitan) Canberra Hospital and better overall teaching than rural students. Other students believed they received sufficient rural exposure from their compulsory 6 week rural rotation in either SE NSW or NT.
Discussion
There is evidence that RCS programs across Australian medical schools have a positive effect in increasing interest in rural health career intentions9. Most of the research evaluating the efficacy of RCS programs has focused on examining independent program modules, such as year-long rural placements or rural weeks; however, minimal research has evaluated rural program components comparatively to determine which are most effective at recruiting students for future rural practice6-8.
The ANU Medical School students who have an interest in rural health and voluntarily choose to participate in elective rural programs (eg the Year 3 year-long rural placement and Year 4 rural elective) indicated they are much more likely to practice in a rural and remote area (75% to 86%). However, these students are a minority (between one-fifth and a quarter of respondents) when compared with total respondent numbers.
In comparison, after the compulsory components of the rural program, half of the participating respondents had a rural practice intention. Due to the high participation rate in compulsory programs, the overall yield of those intending to practice rurally is higher in absolute terms than those involved in elective programs. This supports the importance of compulsory rural health experiences in increasing students' interest in rural health careers, and also that all medical students should be targeted by a rural curriculum, not only to those who have a prior interest in rural health10,11.
The structure and timing of compulsory introductory rural components is important. Rural weeks during the early years of medical education are shown to have a strong influence on promoting student interest in rural health and encouraging interested students to then apply for elective rural programs, such as a year-long rural placement program.
Consistent delivery of rural education from year to year has a positive influence on the majority of students12. This study shows that an increase in rural exposure from one to 6 weeks between Years 2 and 3 has a cumulative positive impact on students, even though only half have rural practice intention. In the Year 1 and Year 2 compulsory components, 56% and 53% had positive influences, respectively, and by the completion of the Year 3 compulsory component, this had increased to 77% of respondents. For those respondents involved in the elective programs, almost all reported a positive influence and have an intention for rural practice.
Preliminary reports have outlined the success of rural programs measured by the increasing number of both urban- and rural-origin students selecting regional rather than metropolitan internships6,7. However, this measure focuses on a short term outcome without understanding future graduate rural intentions. In this study, only 15% of respondents chose a rural internship despite 80% indicating future rural work intention. There is, as yet, no evidence of those with a rural intention choosing to train in a metropolitan context before relocation to a regional area. Recognizing this, the Department of Health and Ageing is working with the Committee of Deans of Australian Medical Schools to track the careers of Australian medical school graduates to establish a longitudinal database, and a similar study has been established in Queensland13-15.
The broader aim of exposing students to rural health in a positive manner is consistent with the core ANU Medical School program objective to develop well-rounded future practitioners for all Australians. This has been successfully met, with 75% of respondents believing that they will be better practitioners after completing the rural curriculum. Most importantly, ANU rural programs have had a positive impact on changing student perceptions because more than 80% of student respondents have the intention to work in a rural and remote area by the time of graduation.
Overall, both compulsory and elective rural program components are effective in nurturing the rural interest of all students, both those who may not have a set rural practice intention, and those whose rural experience during medical school reinforces their intention to practice in a rural area.
The Australian National Health and Hospitals Reform Commission report released in July 2009 recommended recruiting more rural-background students and increasing funding for medical schools with a rural focus16. Achieving the right mix of students of both rural and non-rural background is critical16,17. In the present study, the ANU program had a much larger influence on students from non-rural backgrounds (41%) than rural backgrounds (9%) when measuring the positive change in intention for rural practice. This is consistent with evidence from previous research suggesting that the rural training opportunities of rural programs can have a significant and positive impact on urban students' rural career intent7. Because a large proportion of students in medical schools are from urban backgrounds, retaining a commitment to provide rural education to these students is necessary if future workforce demands are to be fulfilled.
With indications that year-long rural placements encourage the retention of students in rural and remote practice, understanding motivating factors in students' decisions to apply for such a placement can help identify factors needing improvement in program delivery7,9,18. In the present study, student respondents felt strongly about their commitment to family and friends. Although the rural program supports the relocation of families by accommodation and employment assistance, the reality of such a major change is still an unattractive option for those with dependents. Respondents who regretted not applying for rural stream, or indicated that they could not apply, stated that their lack of application was due to family reasons. With an emerging trend for medical students to enter the profession at a later age, this factor has implications on the uptake of rural health opportunities and experience because a higher number of older students will have a partner, and possibly dependents, to consider19. Such personal factors are difficult to address, regardless of the assistance that the RCS offers.
Regarding encouraging factors, student motivation to spend a year in a rural location is clearly focused on the advancement of clinical skills, with a perception that training in a rural setting with provide superior clinical exposure. This main factor along with rural incentives and the quality of teaching cement the intentions of students in their decision to apply for a rural stream. Of lesser importance is a career interest in rural health, a disappointing finding because experience in a rural location is fundamental to the objectives of the year-long rural program. However, in this and other studies, the end result is that students are attracted to a rural program for a variety of reasons, and it is the positive experiences gained during their year-long rural stay that encourages future rural intention; the benefit of recruitment can be measured on exit9. Therefore, there may be merit in focusing efforts on 'promoting' aspects of the program that are attractive to students.
Limitations
This initial examination of the ANU program only represents a small number of student respondents based on one cohort year in one university in Australia. The data were collected from students on a retrospective basis over the 4 years, and relied on student recall of experiences. Due to the small number of respondents, firm conclusions cannot be reached about student response patterns and the replicable nature of the results should be tested with subsequent cohort years. The survey was conducted at the completion of the 4 year ANU rural program with recognition that personal and other factors will continue to influence future career intentions and there remains the uncertainty over eventual outcomes. The establishment of the national longitudinal database will soon provide the necessary tracking tool to compare student intentions with actual graduate outcomes.
Rural programs at ANU and student exposure to rural health experiences in medical school is important in influencing students' perceptions of and interest in a career in rural and remote health. This study provides evidence that both compulsory and elective components contribute to a successful holistic rural program that nurtures the rural interest of all students. Overall, students at the ANU medical school were satisfied with the rural curriculum.
The results of this study confirm that there is difficulty in recruiting students with family commitments into year-long rural placement programs, despite incentives. However, those students who select long-term rural study for reasons other than an interest in a career in rural health often end the program with a positive rural practice intention.
Acknowledgement
The authors acknowledge Samantha Egan of the Australian National University Rural Clinical School for her supervisory assistance.
References
1. Productivity Commission. Australia's Health Workforce. Canberra, ACT: Australian Government, 2005.
2. Wilkinson D. Inequitable distribution of general practitioners in Australia: analysis by state and territory using census data. Australian Journal of Rural Health 2000; 8(2): 87-93.
3. Australian Government Department of Health and Ageing. Workforce education and training - Rural Clinical Schools. Available: http://www.health.gov.au/clinicalschools (Accessed 1 June 2009).
4. Urbis Consulting. Evaluation of the University Departments of Rural Health Program and the Rural Clinical Schools Program. Research report. Canberra, ACT: Department of Health and Ageing, 2008.
5. Rural Undergraduate Steering Committee. Rural doctors: reforming undergraduate medical education for rural practice. Final report of the Rural Undergraduate Steering Committee. Canberra, ACT: Department of Human Services and Health, 1994.
6. Wilkinson D, Birks J, Davies L, Margolis S, Baker P. Preliminary evidence from Queensland that rural clinical schools have a positive impact on rural intern choices. Rural and Remote Health 4: 340. (Online) 2004. Available: www.rrh.org.au (Accessed 20 April 2011).
7. Worley P, Martin A, Prideaux D, Woodman R, Worley E, Lowe M. Vocational career paths of graduate entry medical students at Flinders University: a comparison of rural, remote and tertiary tracks. Medical Journal of Australia 2008; 188(3): 177-178.
8. Newbury J, Shannon-S, Ryan V, Whitrow M. Development of 'rural week' for medical students: impact and quality report. Rural and Remote Health 5: 423. (Online) 2005. Available: www.rrh.org.au (Accessed 20 April 2011).
9. Eley D, Baker P. Will Australian rural clinical schools be an effective workforce strategy? Early indications of their positive impact on intern choice and rural career interest. Medical Journal of Australia 2007; 187: 166-167.
10. Critchley J, Dewitt D, Khan M, Liaw S. A required rural health module increases students' interest in rural health careers. Rural and Remote Health 7: 688. (Online) 2007. Available: www.rrh.org.au (Accessed 20 April 2011).
11. Eley D, Young L, Wilkinson D, Chater A, Baker B. Coping with increasing numbers of medical students in rural clinical schools: options and opportunities. Medical Journal of Australia 2008; 188(11): 669-671.
12. Dunbabin JS, Levitt L. Rural origin and rural medical exposure: their impact on the rural and remote medical workforce in Australia. Rural and Remote Health 3: 212. (Online) 2003. Available: www.rrh.org.au (Accessed 20 April 2011).
13. Committee of Deans of Australian Medical Schools (CDAMS). Medical Schools Outcomes Database (MSOD) and Longitudinal Tracking Project. (Online) 2009. Available: http://www.medicaldeans.org.au/msod.html (Accessed 21 April 2011).
14. Australian Research Council, Queensland Health, Royal Australian College of General Practitioners. Doctors E cohort study. (Online) 2007. Available: http://doctors.e-cohort.net/ (Accessed 21 April 2011).
15. Prideaux D. Workforce: the new core curriculum for medical schools. Medical Education 2006; 40(4): 286-287.
16. National Health and Hospitals Reform Commission. A healthier future for all Australians - final report. (Online) 2009. Available: http://www.health.gov.au/internet/nhhrc/publishing.nsf/Content/nhhrc-report (Accessed 21 April 2011).
17. Somers GR, Strasser R, Jolly B. What does it take? The influence of rural upbringing and sense of rural background on medical students' intention to work in a rural environment. Rural and Remote Health 7: 706. (Online) 2007. Available: www.rrh.org.au (Accessed 20 April 2011).
18. Eley D, Baker P. Will Australian rural clinical schools be an effective workforce strategy? Early indications of their positive effect on intern choice and rural career interest. Medical Journal of Australia 2007; 187(3): 166-167.
19. Joyce CM, Stoelwinder J, McNeil J, Piterman L. Riding the wave: current and emerging trends in graduates from Australian university medical schools. Medical Journal of Australia 2007; 186(6): 309-312.


