Effective decentralization of healthcare financing and the implementation of a sector-wide approach to health care in Sub-Saharan Africa (SSA) require sound planning based on an understanding of national patterns of morbidity and mortality in all regions1. Just as SSA mortality data are deficient relative to that of other world regions2, so data from the more remote areas of SSA are deficient when compared with that of the more easily accessible and readily researched zones3.
Sub-Saharan Africa is still predominantly rural, with the majority of its population living far from urban centres4. Knowledge of the morbidity and mortality patterns in these more remote areas is essential when health priorities are set and interventions planned. For example, the treatment of trachoma only became a priority for the Cameroon Ministry of Public Health after the publication of data on its extremely high prevalence in a rural area of northern Cameroon5. The failure to gather health information from remote areas can also lead to the wastage of public funds, as exemplified by the mass de-worming campaigns that continue in the same area despite the fact that intestinal worms have been unknown there for at least a generation6. Despite the importance of published data on morbidity and mortality in this part of Africa, little information is available.
The study site
Kolofata District in the Far North Region of Cameroon is 1000 km from the capital city. The district's west and north sides share a highly porous border with Nigeria's Borno State. There are no paved roads in the district, the supply of mains electricity is intermittent, and most water comes from wells and boreholes. The population is predominantly Muslim. Most residents are illiterate and speak neither of the country's two official languages. The local economy is based on subsistence farming, herding and small trading. The district's climate consists of 3 seasons: a hot dry season from February to June; a rainy season from July to September; and a cooler dry season from November to January (the transitional month of October may be wet or dry).
The Kolofata District Hospital is the referral hospital for 7 primary healthcare centres, serving a rural population of 122 000. Approximately one-third of the hospital's out-patients come from Nigeria. Since its establishment in 1993, the hospital has had no more than two physicians serving concurrently; since 2005 one of these has been a general surgeon.
All admissions to and deaths in the Kolofata District Hospital from 1993 to 2009 were recorded manually in hospital registers. The patient information in the registers included: dates of admission and discharge or death; name, address, age, sex and ethnic group; main illness, duration of symptoms, a summary of physical examination; and presenting diagnosis or diagnoses. In the case of death, the probable cause was recorded.
Included in this descriptive, retrospective record study were all patients who died in the hospital from 1 January 1993 to 31 December 2009. No community deaths were included. Data that included the patients' date of admission, address, age, sex, ethnic group, duration of symptoms, diagnosis or diagnoses, date of death and probable cause of death were transcribed by hospital personnel into an Excel spreadsheet. Hospital personnel then analysed the data using EpiInfo v 3.5.1 (CDC Atlanta; http://wwwn.cdc.gov/epiinfo/) and OpenEpi v 2.3 (Open Source Epidemiologic Statistics for Public Health; www.openepi.com). Where Bartlett's test indicated normally distributed data, ANOVA was used to compare two groups. Where variance was not homogeneous, the Mann-Whitney/Wilcoxon (Kruskal-Wallis H) test was used. The mid-p exact test was used to calculate odds ratios (OR) and confidence intervals (CI).
Diagnosing the cause of death was performed by a physician or clinical officer, based on the patient's history, physical examination, and the results of relevant laboratory or imaging investigations. Where patients with AIDS died of opportunistic infections, AIDS was given as the cause of death. Death was attributed to 'intoxication' for patients with no clear lethal diagnosis other than a recent history of ingestion of a toxic medicine or substance. Neonatal sepsis was identified as the cause of death for children less than 1 month of age with persistent fever and circulatory collapse in the absence of other identifiable diagnoses such as tetanus, malaria, respiratory infection, or gastroenteritis.
In this study, patients under 15 years were classified as a child, and those over 15 years an adult, in accordance with WHO conventions2.
In total, 1281 deaths were recorded for hospitalised patients from 1 January 1993 to 31 December 2009.
Age, sex and district of residence
Of all deaths, 63.9% were children and 56% were male. More males died in every age group except for those 15-44 years (Fig1). Regarding deaths before the age of 5 years, 46.9% were in children 0-11 months. Of all deaths, 37.4% were among patients from outside Kolofata District.
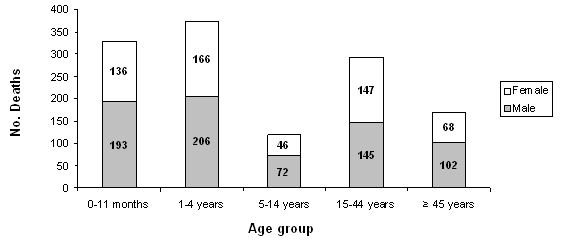
Figure 1: Comparison of male and female deaths by age group.
Cause of death
Overall, acute lower respiratory tract infection (LRI) was given as the cause for the greatest number of deaths (167), followed by malaria (152) and diarrhoeal diseases (133; Table 1). Anaemia, malnutrition and AIDS were ranked fourth, fifth and sixth, both overall and for each sex.
Among adults, AIDS was the most frequent cause of death in both men and women (Table 2). After AIDS, the complications of pregnancy and LRI were the next most frequent causes of death for women, as were LRI and urinary tract pathology for men.
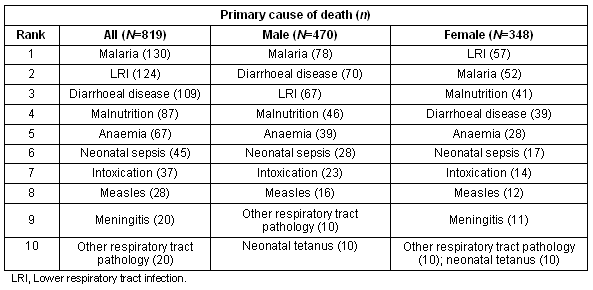
Malaria, diarrhoea and LRI were the 3 most common causes of death among boys; LRI, malaria and malnutrition were the leading causes of death among girls (Table 3).
Table 1: Overall leading primary causes of death
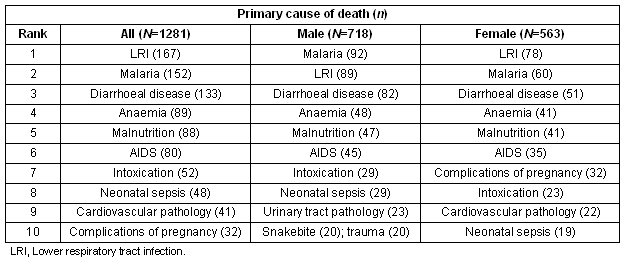
Table 2: Leading primary causes of death in adults (aged ≥15 years)
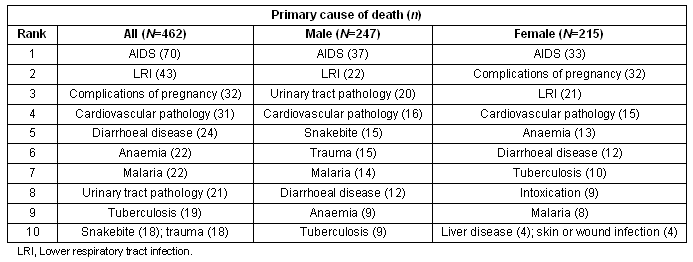
Table 3: Leading primary causes of death in children (aged <15 years)
Seasonality
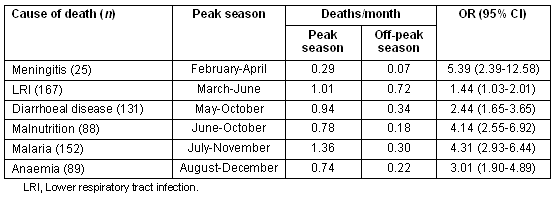
Causes of death varied with the seasons, and peak and off-peak seasonal trends were noted (Table 4), as were other patterns. Anaemia was the most frequent cause of death in December and January, then LRI from February to the end of April, diarrhoeal diseases in May and June, malnutrition in July, and malaria from August to the end of November. Death due to respiratory tract infections was more common during the dry season, while death from diarrhoeal diseases and malnutrition was more frequent during the rainy season. Deaths due to malaria and anaemia were most common during and just after the rains.
Table 4: Seasonality of leading primary causes of death
Time from symptom onset to admission and death
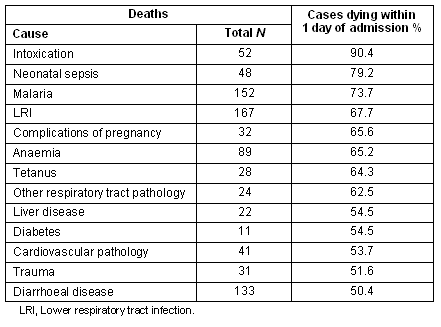
Symptom duration was recorded for 1041 patients (Fig2). The average time from symptom onset to admission was 18.5 days for children and 68.5 days for adults (p<.001); however, 697 patients (74.2% children and 53.4% adults; OR 2.50, 95% CI 1.91-3.28, p<.001) presented within 1 week of symptom onset or earlier. The average time from admission to death was 2 days for children and 5.2 days for adults (p<.001). A total of 56.8% of deaths (64.2% of children and 43.7% of adults; OR 2.31, 95% CI 1.83-2.92, p<.001) occurred on or before the day following admission. For 13 causes of death, at least 50% of patients died within 1 day of admission (Table 5). There was no difference between males and females regarding symptom duration or the frequency of rapid death.
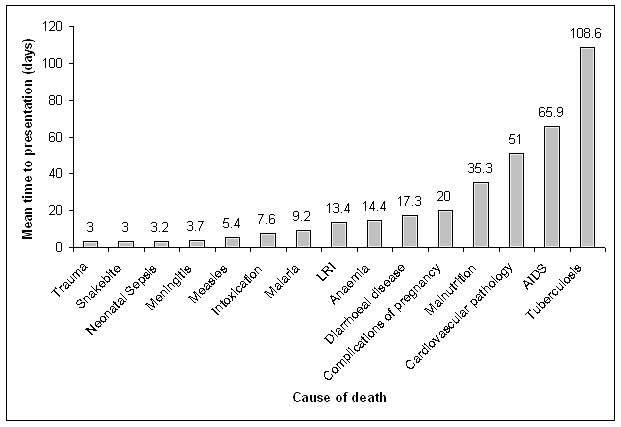
Figure 2: Most common 15 causes of death with mean time from onset of symptoms to presentation at hospital in patient-reported days (12 outlying cases with symptom duration >365 days excluded). LRI, Lower respiratory tract infection.
Table 5: Causes of death associated with ≥ 50% of deaths occurring within 1day of hospital admission
Causes of death over time
Hospital deaths due to malaria, AIDS and complications of pregnancy increased over time, relative to other causes (Fig3). Relative to other causes, AIDS was more often a cause of death during later (2004-2009) than earlier years (OR 10.6; 95% CI 5.1-25.2; p<.001) as were malaria (OR 1.7; 95% CI 1.2-2.5; p<.01), and complications of pregnancy (OR 4.1; 95% CI 1.7-11.0; p<.001).
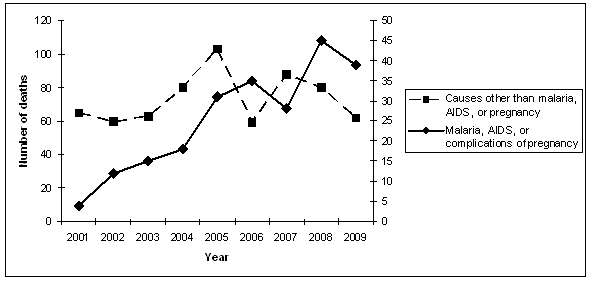
Figure 3: Deaths due to malaria, AIDS or complications of pregnancy (right axis scale) compared with deaths due to other causes (left axis scale), 2001-2009.
Vaccine-preventable diseases
From 2000 to the end of 2009 there were 10 deaths due to measles; 5 of these patients were from a Kolofata District village, and 2 of these were children under 9 months (too young to have been vaccinated). In the same period, 1 of the 6 children who died of measles was from Kolofata District while the other 5 were from bordering villages in Nigeria. The last Kolofata District death due to measles occurred in 2005. In the 5 years from 2005 to 2009, only 1 Kolofata District death was recorded as due to neonatal tetanus.
Deaths due to chronic non-transmissible diseases
Of all deaths, 4.3% were due to cardiovascular pathology, diabetes or cancer but there was no trend observed over the 17 year period (Fig4); relative to other causes of death there was no significant difference in deaths due to chronic non-transmissible diseases during earlier (1993-2003) and later years (OR 1.2; 95% CI 0.69-2.1; not significant).
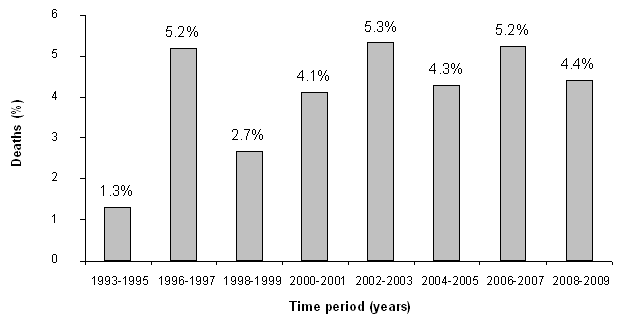
Figure 4: Deaths attributed to cardiovascular pathology, diabetes, or cancer as percent of all deaths.
Discussion
This study of deaths in a district hospital in northern Cameroon over a 17 year period is the first of its kind from this part of Africa. It revealed that in this region:
- infectious diseases continue to be prominent causes of death in hospitalized patients
- chronic non-communicable diseases are not increasing relative to other causes of death in hospital
- the majority of patients who die in hospital are children, and male (except in those of reproductive age)
- there is a strong seasonal variation to deaths in hospital
- among hospital inpatients, deaths due to AIDS, malaria or the complications of pregnancy have been increasing relative to other causes
- death due to measles and neonatal tetanus, illnesses long covered by the national vaccination program, have become rare
- a substantial proportion of all hospital deaths occur rapidly, on or before the day following admission.
These findings are similar to other studies performed in Africa. In a case-control, community-based study of children under 5 years in the Gambia from 2003 to 2006, Rutherford et al reported that fever of unknown origin, diarrhoea and pneumonia were responsible for 55% of deaths; 54.3% of deaths occurred within 2 days of hospitalisation, and 49.3% of deaths occurred in children 0-11 months7. Hammer et al found that malaria was the most frequent diagnosis in childhood death in north-western Burkina Faso8, and in the same region Ramoth et al found no evidence of a decrease in malaria mortality from 1999 to 20049. In a community-based survey of mortality in western Kenya, van Eijk et al attributed 74% of deaths to infectious causes, with AIDS, tuberculosis, malaria, respiratory tract infections being most common10. The WHO estimates approximately half of all deaths in SSA occur in children under 15 years, with infectious diseases being the major cause2. Among adults, AIDS is the most frequent cause of death, followed by trauma among men and complications of pregnancy among women2. Although a 1997 study from South Africa demonstrates the historically high proportion of deaths due to infectious diseases11, the increasing prominence of non-communicable diseases as a cause of death in such relatively developed settings12 is not evident here.
Despite a decade of heavily funded AIDS and malaria control programs in SSA, AIDS and malaria continue to increase relative to other causes of death. A reduction of malaria mortality depends in part on treatment availability13. The increase in malaria deaths in this part of northern Cameroon coincided with a nation-wide change in government policy to replace the widely available chloroquine with artermisinin-based combination therapy (ACT) as first-line treatment. Although chloroquine resistance was a concern in southern Cameroon as early as the mid-1980s14, this was not so in the far north of the country15 where patterns of resistance have been markedly different16. While chloroquine was removed from the market abruptly, ACT was not made available in adequate quantities for some years. This may have contributed to the rise in malaria deaths. Deaths from AIDS have been increasing as more HIV-positive patients have been identified, and the only treatment available in the district is first-line. Resistance to first-line treatment has begun to occur, measured by genotyping resistance studies on samples taken from Kolofata Hospital patients.
An increase in hospital deaths due to the complications of pregnancy coincided with the arrival of a surgeon in 2005, following which seriously ill patients who would previously have remained at home or been managed elsewhere were referred to Kolofata Hospital.
Study limitations
The study has some limitations. Given the retrospective, records-based design of the study, it is not possible to validate the data for accuracy or completeness of records. Hospital-based data have been shown to provide useful information for public health priority setting17, but they may or may not be a reflection of circumstances outside the hospital. Data for this in this part of Africa do not exist, but in western Kenya, van Eijk found hospital death to be associated with younger age, higher education and socioeconomic status, non infectious cause, and shorter duration of illness compared with community death10.
Where diagnostic tools are relatively scarce, diagnoses are susceptible to error. Before 1996, for example, AIDS was not cited as a diagnosis in this district because HIV testing was unavailable. Incomplete data or a practitioner's bias or inexperience would introduce diagnostic errors. Nevertheless, trained healthcare personnel working with live patients will provide more reliable diagnostic information than those not involved in patient care. Verbal autopsies, the other method frequently used to ascertain cause of mortality in resource-poor zones, have their own limitations18,19. The gender bias evident in a higher proportion of males suffering hospital death may reflect a higher proportion of males in the population, a higher proportion of males who fall sick and subsequently die, or a higher proportion of males who are brought for health care. This issue should be explored.
Study significance
This study is of practical significance in several ways. On a district level, it describes the burden of mortal disease that must be dealt with in a hospital in this rural, remote part of Africa. The implications with regard to staffing, equipment, medicines, education, and preventive activities are generalisable to any district hospital in a similar setting. The study has suggested that to reduce mortality, priority should be given to the prevention and management of LRI in all age groups; of malaria, LRI and diarrhoeal diseases in children; and also of AIDS and the complications of pregnancy in adults.
Planning for the provision of medicines, supplies and health education should take into account the seasonal influences on causes of death. The reasons for the high number of deaths due to malnutrition during the rainy season should be studied and managed. And the finding that over half the deaths occurred on or before the day following admission suggests that some patients are presenting to hospital too late in their illness, and/or that emergency care is not optimal.
When setting public health priorities, partial data can be worse than no data at all3, and this is certainly so if government decision-makers base decisions that will affect an entire country on data collected from only part of it. In the absence of data from all areas affected, national and international decision-makers should be wary of applying single solutions to problems in countries characterized by the extreme diversity that is typical of many countries in Africa.
The results of this study suggest that to reduce mortality in this world region, priority should be given to the prevention and management of LRIs, malaria, diarrhoeal diseases, AIDS, and the complications of pregnancy. The planning of health resources and activities should take into account seasonal variations. Improvements to emergency services and community education that emphasises presentation early in an illness should reduce the number of deaths that occur soon after hospital admission. That death due to measles and neonatal tetanus has become rare is a reflection of the effectiveness of the national vaccination program in this area.
References
1. Hutton G, Tanner M. The sector-wide approach: a blessing for public health? Bulletin of the World Health Organization 2004; 82: Online (2004). Available: http://www.who.int/bulletin/volumes/82/12/893.pdf (Accessed 26 July 2011).
2. Mathers CD, Boerma T, Fat DM. Global and regional causes of death. British Medical Bulletin 2009; 92: 7-32.
3. Cooper RS, Osotimehin B, Kaufman JS, Forrester T. Disease burden in sub-Saharan Africa: what should we conclude in the absence of data? Lancet 1998; 351: 208-210.
4. The World Bank Group. Agriculture and rural development: regions. (Online) 2011. Available: http://go.worldbank.org /RF3070S7F0 (Accessed 31 January 2011).
5. Bensaid P, Huguet P, Goldschmidt P, Einterz E. Le trachome au Cameroun: résultats d'une enquête épidémiologique dans le district de Kolofata dans la province de l'Extrême-Nord. Revue Internationale du Trachome et de Pathologie Oculaire Tropicale et Subtropicale et de Santé Publique 2007; 84: 79-90.
6. Einterz EM, Bates ME. Infant disease patterns in northern Cameroon. Transactions of the Royal Society of Tropical Medicine and Hygiene 1993; 87: 418-420.
7. Rutherford ME, Dockerty JD, Jasseh M, Howie SRC, Herbison P, Jeffries DJ et al. Access to health care and mortality of children under 5 years of age in the Gambia: a case-control study. Bulletin of the World Health Organization 2009; 87: 216-224.
8. Ramroth H, Ndugwa RP, M?ller O, Yé Y, Sié A, Kouyaté B et al. Decreasing childhood mortality and increasing proportion of malaria deaths in rural Burkina Faso. Global Health Action 2009; Apr 15;2. DOI:10.3402/gha.v2i0.1909.
9. Hammer GP, Somé F, Müller O, Kynast-Wolf G, Kouyaté B, Becher H. Pattern of cause-specific childhood mortality in a malaria endemic area of Burkina Faso. Malaria Journal 2006; 5: 47. Available: http://www.malariajournal.com/content/5/1/47 (Accessed 2 September 2010).
10. van Eijk AM, Adazu K, Ofware P, Vulule J, Hamel M, Slutsker L. Causes of deaths using verbal autopsy among adolescents and adults in rural western Kenya. Tropical Medicine and International Health 2008; 13(10): 1314-1324.
11. Couper I, Walker AR. Causes of death in a rural hospital in South Africa. Central African Journal of Medicine 1997; 43(8): 219-222.
12. Tollman SM, Kahn K, Sartorius B, Collinson MA, Clark SJ, Garenne ML. Implications of mortality transition for primary health care in rural South Africa: a population-based surveillance study. Lancet 2008; 372(9642): 893-901.
13. Chuma J, Okungu V and Molyneux C. Barriers to prompt and effective malaria treatment among the poorest population in Kenya. Malaria Journal 2010; 9: 144. Available: http://www.malariajournal.com/content/9/1/144 (Accessed 25 August 2010).
14. Sansonetti PJ. Chloroquine-resistant Plasmodium falciparum in Cameroon. Lancet 1985; 1: 1154-1155.
15. Lavoue V, Lavoue P, Turk P, Brasseur P, Druilhe P. Low prevalence of P. falciparum in-vivo resistance to chloroquine in northern Cameroon in 1986. Tropical Medicine and Parasitology 1988; 39(3): 249-250.
16. Brasseur P, Kouamouo J, Moyou RS, Druilhe P. Mefloquine resistant malaria in Cameroon and correlation with resistance to quinine. Memórias do Instituto Oswaldo Cruz 1992; 87(Supp III): 271-273.
17. Tornheim JA, Manya AS, Oyando N, Kabaka S, Breiman RF, Feikin DR. The epidemiology of hospitalized pneumonia in rural Kenya: the potential of surveillance data in setting public health priorities International Journal of Infectious Diseases 2007; 11: 536-543.
18. Maude GH, Ross DA. The effect of different sensitivity, specificity and cause-specific mortality fractions on the estimation of differences in cause-specific mortality rates in children from studies using verbal autopsies. International Journal of Epidemiology 1997; 26(5): 1097-1106.
19. Chandramohan D, Maude GH, Rodrigues LC, Hayes RJ. Verbal autopsies for adult deaths: issues in their development and validation. International Journal of Epidemiology 1994; 23(2): 213-222.

