African Americans living in rural areas of the USA experience multiple health disparities as a result of both race and rural geography. African Americans have the highest age-adjusted death rates of any race for heart disease, cancer, diabetes, and AIDS; they also experience higher incidence of hypertension and obesity1,2. Rural residence in the USA is linked to increased risk of type 2 diabetes, obesity, poor oral health, suicide, and tobacco use3. As such, rural African Americans are particularly vulnerable to ill health, but they are often overlooked in the literature.
An increasing body of research suggests that social factors, or social determinants of health, are key predictors of health outcomes and are critical contributors to health disparities4-6 . The WHO defines social determinants of health as 'the conditions in which people are born, grow, live, work and age, including the health system'6. Quality of, and access to, the healthcare system has been the focus of most US rural health research. However, studies have found the healthcare system to make a minimal contribution to health outcomes, which has been found to be as low as 3.5% in some studies7,8. Therefore, there is a need for health disparities research that explores the social determinants of rural health beyond the healthcare system7,9. There is a paucity of rural health studies that incorporate this concept of social determinants7,9,10.
Qualitative, ethnographic approaches are ideal for studies of rural social determinants7,9. They allow researchers to address the 'variability and complexity'7 of rural communities' cultures, environments, and politics. Such studies can be used to probe the roots of health disparities, and to develop contextually appropriate interventions to eliminate them.
There is increasing use of ecological theory to inform public health research and intervention. Ecological theory embraces a multilevel view, positing that health is contingent on a plurality of interacting contexts11,12. If offers a valuable way of looking at complex community conditions, and exploring potential links between social determinants and health. The few studies in rural health that have employed ecological theory have focused on single, pre-determined health issues, such as infant mortality and oral health13,14.
The specific ecological model utilized here is an adaptation of the model developed by Sweat and Denison15. This multi-level model organizes potential social determinants of health at five levels:
- The individual (traits and behaviors)
- The relational (relationships, social support)
- The environmental (built environment)
- The structural (laws, policies, and politics)
- The superstructural (social justice issues such as racism, disadvantage due to low socioeconomic status, sexism).
This exploratory study blended a community-based, qualitative approach with the use of Sweat and Denison's ecological theory, with the objective of identifying potential social determinants of health among African Americans in a rural community in the Deep South, from the perspectives of African American community members.
This study was conducted as part of a larger qualitative community health assessment in a county in rural southeastern Georgia (A Scott A, pers. data 'Ethnographic Community Health Assessment of Evans County', 2007). The researchers worked with a citizens' health collaborative to conduct the study. The Institutional Review Board at Georgia Southern University reviewed the study, and all participants provided written informed consent.
The researchers conducted in-depth interviews with 18 African American community members ranging in age from 24 to 70 years. Interviewees were purposefully sampled to incorporate a range of perspectives. Tabular summaries of interviewee characteristics aided in maximizing variability in sampling. A key informant, the director of the local health department, suggested initial interviewees; later interviewees were identified through snowball sampling and through referrals from a range of community organizations. All interviewees were long-time African American residents of the community. They included pastors, retirees, school teachers and principals, coordinator of a youth resource center, President of the local National Association for the Advancement of Colored People (NAACP), young adults, the high school band director, and Director of the local Concerted Services service organization, among others.
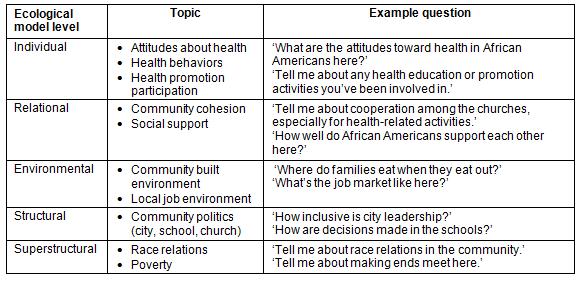
Interviews were conducted between January and April 2007. Interviews were conducted in person in the home or community setting of the interviewee's choice, and interview lengths ranged from 20 min to 2 hours. Interview guides were used to conduct the interviews. Examples are given of interview topics and questions at each level of the ecological model (Table 1). Interviews were recorded and transcribed. Iterative content analysis of interview transcripts and field notes was performed to identify potential social determinants of health. A strategy similar to the 'editing' approach to content analysis described by Crabtree and Miller16 was used. Segments of text in transcripts and notes were sorted and grouped by ecological level, and then analyzed by level. Inductive coding within each level was conducted to identify potential social determinants of health, which were expanded into themes using reflexive memo-writing17 and through data display in matrices18. Triangulation was achieved by having both researchers involved in the analysis. Analysis quality was also tested through member checking, by sharing results with community coalition members19.
Table 1: Selected interview topics and questions for each level of the ecological model
Results
Study community
The study community was a rural town in southeastern Georgia, USA. Approximately 40% of its 2200 residents were African American. The majority lived in poverty. Almost three-fourths of households with children (74%) lived under the poverty line (US$17,463 for a family of four in 2000)20.
Interviewees were asked to list, in their views, the community's most pressing health concerns. The most frequent response was HIV, along with diabetes, high blood pressure, and other chronic diseases related to overweight and obesity.
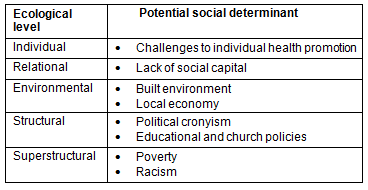
Potential social determinants of health were identified at all five levels of the ecological framework. These issues are summarized (Table 2), and discussed in depth in the following sections.
Table 2: Potential social determinants of health identified at each ecological level
Individual ecological level
Competing needs and fatigue: 'I want to see change so bad': Lack of engagement with personal health and health promotion was a recurring theme, and potential individual-level social determinant of health, that emerged in interview transcripts. This idea was voiced by interview participants who had been involved with community health education and promotion activities. As expressed by one such community member, 'You have to get a gun and say [to community members] "Get in here!".' Attendance at these events was reported to be chronically low, no matter what the location or topic. Interviewees agreed that many of their friends and family members didn't pay attention to health issues until they were sick.
The reasons for this passivity are doubtless complex. It was suggested that more immediate concerns were weighing on people's minds, rather than theoretical health risks. Commenting about a recent health fair, one participant reflected that 'Lots of people wanted food help, but none wanted to learn about health'. Information about hypertension seemed of limited value, perhaps, to those struggling to put food on the family table in this community of high poverty and limited opportunity. Focusing on current rather than future needs is congruent with the theory of time preference described in economics, whereby people will show a preference for 'immediate over delayed utility'21. In this case, food has clear immediate utility.
In turn, this lack of response to community health efforts has led to a sense of frustration and fatigue among planners and volunteers. The director of a local social service organization expressed that 'I have had migraines since 1996... It's from stress... but I want to see change so bad - so bad'. Their passion for improving their community's health is tested by the lack of interest in, and impact of, their efforts. At the same time, they lack the training and capacity to identify other strategies, or to put people's behavior into context. Together, the sense of defeat and lack of capacity puts future individual-level health promotion efforts at risk.
Relational ecological level
Social capital: 'It's just got no togetherness': Social capital has been identified as a significant social determinant of health22,23. Social capital has been defined as the collective value of social relationships, or networks, and the mutual reciprocity they foster24. Social networks may enhance wellbeing by connecting individuals to emotional, financial, instrumental, and other types of support that contribute to physical and mental health. Isolation and community fragmentation, however, are associated with ill health25.
Community social capital emerged as a potential social determinant at the relational level in this study. Interviewees complained of fractiousness among the African American churches, which are key institutions in the community. Rather than presenting a unified front for health activities or other efforts, churches were described as 'territorial', reaching out to, and socializing with, their own members only. One mother commented:
It's about ninety-nine thousand different churches, and all of 'em have their own little center, but it's basically just for those... that go to their church. It's just got no togetherness.
In this sense, the African American churches were rich in bonding social capital, which is generated by strong support within groups, but poor in social capital bridging them to other groups that may have additional resources or supports to offer. One result of this is that redundant events were planned, and opportunities for collaborations were missed; health fairs, for example, are put on separately by different African American churches and organizations.
At another level, interviewees described a generational 'fissure', with the old and the young often estranged and oppositional. However, interview participants referred to a 'network of old retired people' that was very active in the community. A retiree observed that:
I guess it's just we old retired people. We know what needs to be done so we're doing it... Just a few of us be part of everything, and every meeting you go to... There's so much hostility within our young people... either they don't like us or they just don't trust us, you know.
'Seniors' described growing up in a 'connected' African American community with strong ties, familial and otherwise. As put by one elderly woman:
Our parents were connected... we had this big extended family. My grandparents and my uncles and my aunts and all of us and our teachers and our neighborhoods were like this huge extended family.
This was contrasted to the current situation, which has evolved with the economic deterioration of the town. High unemployment and underemployment, a new and thriving drug trade, low high school graduation rates, and high rates of incarceration characterize the lived realities of many younger African Americans in the community. Older interviewees expressed despair at the decline they see in the younger generation, and chastised their lack of engagement with the community and sense of responsibility to one another. Younger participants didn't challenge this portrayal. One young woman commented that:
With the older community the bond is strong. The young generation, they're more interested in tearing each other apart.
In sum, the intergenerational relationships were portrayed as frayed and weak, another source of social capital that was compromised, limiting its potential to 'transmit' emotional, social, financial, and informational support within the African American community.
Environmental ecological level
The built environment: recreation and isolation: At the level of the physical environment, the composition and layout of a community, or the built environment, is a key social determinant of health26,27.The built environment is of particular importance to physical activity and good nutrition, both key to fighting obesity and associated chronic diseases28,29. In this rural community, interviewees identified multiple aspects of the built environment that had potential implications for physical activity and nutrition, many of them negative. A common complaint expressed by parents, teachers, counselors, and community leaders alike was the lack of accessible venues for people to recreate and be active. There is no community swimming pool, bowling alley, ice rink, or other gathering place. There are few sidewalks and bike paths. The town is home to a central park. However, in recent years the park has been closed at 14.30, limiting its availability and blocking access to once-crowded basketball courts and playing fields. The community has a recreation center that sponsors sports activities for children. However, interviewees pointed out that activities had a participation fee, and were geared toward younger children. In addition, this facility was constructed several miles west of the town center in an undeveloped area, off a two-lane highway with no sidewalks, making transport an issue for many families.
In addition, the community also had limited options for accessing healthy food options. The town had one grocery store and multiple convenience stores that sell packaged food. With the lack of competition, the grocery store 'can set... its own prices', and had limited selections of produce and other healthy, fresh foods. Restaurant options largely include fast food chain restaurants, barbecue restaurants, and buffets serving a traditional array of energy-dense, high-fat foods. In sum, the community's built environment is not conducive to maintenance of healthy weight, a key public health concern.
The local economy: 'People without a dream': The community job environment emerged as an additional concern. Given the strong links between income and health, a weak economy can be a powerful social determinant of health. Job options were few in the community, save fast food jobs, other minimum-wage service jobs, and a poultry processing plant largely staffed by immigrants. Much of this economic deterioration has occurred in last 30 to 40 years. Along with the loss of farming work (mainly picking cotton) as agriculture became more mechanized, local textile factories closed or relocated. In addition, interviewees said that as the local economy weakened, illegal drug activity exploded. This change has contributed to the sense of 'generational decline'. Many seniors in the African American community received high school diplomas (and some went on to college); after graduation they were able to find steady employment with manufacturers in the community. Some of these individuals were active in the Civil Rights movement in the 1960s, and were imbued with a sense of activism and ambition to produce change. Interviewees held them in contrast to the younger, current generation, which struggles with unemployment, drugs, and a sense of futility. A woman in her 20s described it this way:
You see that a lot of our kids are hanging out on the corners every day... I can come in from work and see the same people hanging out on the street corner all day long. It's like they haven't even moved.
Seniors in the community were caring for grandchildren whose parents were incarcerated, addicted, or employed in jobs that didn't allow them to afford child care. A senior citizen with a long history of Civil Rights activism described trying to reach out to young people on the corners as the President of her Neighborhood Watch, and her frustration at their disconnection from the recent past:
[I tell them it's] disrespectful to stand on the corners. Back in the 30s, 40s, and 50s, the Klan would come into Black neighborhoods. In fact they did some marches back here in the early days; I have some articles to back me up. They would come into Black neighborhoods and terrorize the neighborhood. It was a form of terror, and what I say to [the young people on the corner] is that 'you doing the same thing, except you don't have your hoods and sheets!'
At the same time, interviewees acknowledged that opportunities in the community were slim now, leaving few avenues for economic success other than escape and the drug trade. In this context, a pastor interviewed described the younger members of the African American community 'people without a dream'. More concretely, the economic environment also left many of them without suitable income to care adequately for themselves and their families.
Structural ecological level
Political cronyism and educational policy: 'Who-you-know' and tracking: Social determinants of health at the structural level include laws and policies that impact health. These policies can be enacted at any level, national, state, or local. Structural determinants can have effects on health that are direct (such as prohibiting smoking in restaurants) or indirect (such as raising the minimum wage, which increases income, which is associated with improved health). Interview participants highlighted structural issues in their community with the potential to function as social determinants of health. Access to political positions where many local policies are made was, according to interviewees, more about family connections than ability; one participant described this as the 'who-you-know syndrome'. It had structural ramifications in the disproportionate control it gave this group, the majority of whom are White, over many local decisions, such as the location of the recreation center (as discussed). It also impacted local funding allocations. One health department employee confided that she could not risk disagreeing with local council members about race issues, because the council controlled a portion of health department funding.
In addition, a number of interviewees expressed concerns with the 'tracking' policy utilized by the local public schools. As students enter the upper grades, they are funneled into either a 'college prep' track or a 'vocational' track. Interviewees expressed the concern that African American youth, especially boys, were disproportionately shunted off into the vocational track. One graduate of the system was upset about this, saying:
We have a lot of people that should be in college prep that's in vocational track... they just throw them anywhere. ... It's harder for them to go to college, because they don't have the classes they need. ...They say, 'Oh, no. You don't have the credits. You might wanna try [name of local technical school]'. ...They done fell into the trap that [county] has set for them, and they have no choice but to go to a trade school.
A tiny proportion of African American young men from the community go to college, and many end up unemployed or underemployed, or incarcerated for drug offenses. Given that education level is associated with a variety of health outcomes30, educational policies that hinder educational attainment may be strong social determinants of health.
The limits of the 'law': churches and health promotion: An additional theme that emerged as a potential social determinant of health at the structural level involved local pastors and churches. In rural communities in the Deep South, pastors are extremely influential figures. As described by the President of the local NAACP, 'A pastor's word is almost law in a rural community'. So, while not lawmakers in the strict sense of the word, pastors' and churches' policies have a significant impact on communities. The church is central to community life in the study town, especially given the lack of other venues for social interaction. Many health education and promotion events are sponsored by churches, and churches are frequently the 'go-to' venues for public health professionals wishing to reach community members about health issues. In addition, parishioners look to their pastors and churches for guidance on how to live, and to decide what constitutes appropriate behavior. In some instances, these messages may serve to confound health.
For example, HIV was identified as a critical health concern for the community, and interview participants stressed the need to educate community members about HIV prevention. However, frank discussions about condoms are taboo if the church is involved. One pastor explained this, saying, 'We can't have the church handing out condoms. The body is the temple of the Holy Spirit. So we deal with abstinence'. One retiree commented that her pastor would 'have a fit' if she mentioned condoms. For her HIV education that included discussion of condoms, she was relegated to the local park. In order to reach congregants, therefore, important messages about protection have to be eliminated.
Superstructural ecological level
Poverty and weathering: Beyond the policies and political milieu of the community are the social justice issues that shape these policies, and that shape experiences at every other ecological level. Class was one such issue with profound importance in community life, according to interview participants.
Poverty is a pivotal social determinant of health, functioning both directly and indirectly to compromise health status. Poverty rates were extremely high in the African American community. Three-fourths of African American families (74%) lived under the poverty line in 2000; the median household income for African Americans was $13,64920. As a result of this, many African Americans lived in substandard housing, including trailers scattered in fields accessible only via dirt roads with the tendency to flood. Some were covered for health care costs by Medicaid, but others described having too much income to qualify for Medicaid, but not enough to purchase their own health insurance. To earn money, some African Americans turned to selling drugs, putting them at increased risk of addiction and violence. The drug industry affected whole neighborhoods, creating a sense of threat for others in the community. Many could not afford to pay heating bills in the winter, and assistance funds were insufficient to assist people more than once a season. There is little public transportation so cars are a necessity, and cheap cars in ill-repair may produce an increased threat of injury in auto-accidents. In short, the potential direct links between poverty and ill health are myriad in the community. This doesn't take into account the additional risks associated with chronic stress, or 'weathering', caused by poverty31.
Racism: 'It's Black and White': Racism and other forms of discrimination can serve as determinants of health at the superstructural level5,9. Experiences of racism have been shown to contribute to poor health, especially poor mental health, both directly and through chronic stress pathways32. Racism was a salient theme in interviews. For example, a few interviewees perceived that White patients were treated better at local doctor's offices, even if 'it's done a little more discreetly than it was in the past'. (Another woman commented that she received good treatment because her mother worked for a prominent local White politician, a case of social connections overcoming the race divide.) In this form, racism could have direct implications for health. More indirectly, as with poverty, racism can be seen as a form of chronic stress.
Interviewees described their community as de facto segregated by race, with the majority of African Americans living on the south side of town, and the majority of Whites living on the north side. The community's churches and civic organizations are mainly segregated as well. As expressed by a former School Board member, the sole African American representative at the time:
You stay on your side of the tracks... change is slow. ... It's Black and White, Black and White.
A young woman agreed, commenting that White people only came to her neighborhood to buy narcotics:
If you see a White person driving through on this street, it's mostly for drugs. Like White people don't just come through here.
All acknowledged that there has been headway in the race relations, but the battle scars run deep. Recent issues have included a community-wide debate over having separate Black and White prom courts, class presidents, and student councils.
Discussion
This exploratory study sought to identify potential social determinants of health among African Americans in a rural community in the Deep South. The study employed an inductive, formative approach and thick description of contextual issues in the community, with the ultimate aim of designing community-based interventions at multiple ecological levels. The social determinants identified had the potential to impact a variety of health behaviors and health outcomes. This breadth is congruent with the wide range of health disparities experienced by rural African Americans.
At the individual ecological level, lack of engagement in health and health promotion was identified an issue of concern. The reasons for this, in part, may relate to the poor local economy and high poverty rates, powerful social determinants in and of themselves. Stresses over meeting basic needs are potent barriers to engaging people in health education and prevention efforts with a long-range focus. The community environment presented additional challenges to health with its limited access to healthy foods (and plethora of unhealthy food options), as well as lack of venues for physical activity.
At the relational level, African American community cohesion was compromised at several levels, limiting the benefits to health and wellbeing that can come from positive social capital. Once again, this issue can be linked in with poverty and the economic deterioration of the town. The limited opportunities available to the younger generation have brought with them frustration and alienation, as well as a new and thriving drug trade. A sense of tight connection among blue-collar families working at local textile plants has been replaced by unemployment, incarceration, and disrupted relationships and family lives. A high school diploma, if it is attained, can no longer bring potential for a living wage and a settled life; this further discourages efforts to obtain diplomas. In addition, local school tracking policies make a college education seem out of reach. Without resources to secure well-paying jobs, the health risks of poverty enter in.
Issues of race and discrimination emerged as potential social determinants of health at the superstructural level. Interviewees described a community life that is largely segregated (de facto), with race 'in play' at the doctor's office, the schools, and in civic life. Studies have linked the ongoing stress caused by discrimination to increased risk of such diseases as hypertension, obesity, and heart disease, through physiological mechanisms related to the hypothalamic-pituitary-adrenal (HPA) axis33. Similar to this finding, a study by Larson et al identifies racism as a key social determinant of health in rural Aboriginal populations34.
In addition, race entered into social determinants identified at other ecological levels. At the relational level, lack of social capital amongst African Americans was exacerbated by lack of connections to the White community, who holds most of the human, built, and financial capital in the town, including control of jobs at local businesses. In sum, the social determinants of health identified here do not function discretely, but in complex interaction with one another. The forces at work at more distal ecological levels (structural and superstructural) are key contributors to, and explicators of, social determinants at the individual and relational levels.
No other published studies have addressed rural social determinants of health using an ecological framework. Dixon and Welch, however, quantitatively explored the rural-urban health differential in Australia using the social determinants approach, and concluded that it provides a powerful tool for gaining insight into rural health disparities35. The findings of the present study support that conclusion, and demonstrate the value of qualitative approaches for exploring the complexities of rural health issues. Limitations of the study include the small number of young male participants, and the lack of participants from the local prison. In addition, there is a growing Hispanic population in the community, and this study cannot address potential social determinants of health from their perspective.
This study is descriptive and exploratory, and not intended to determine causal relationships. However, studies of this sort are critical to illuminating 'the conditions in which people are born, grow, live, work and age' in rural America, and how these conditions may contribute to health disparities. These findings may be transferable to other rural community settings with health disparities related to race, class, and geography. Further work is needed to explore each of these potential social determinants quantitatively, to assess their relationships with specific health behaviors and outcomes. These findings suggest the need for context-specific, community-based interventions that include capacity building for local health promoters, network building within the African American community, collaboration with city planners to influence local development, and advocacy skills. It also speaks to the vital importance of interventions that support community economic development and educational attainment, as well as dialogue across racial lines.
References
1. Center for Disease Control and Prevention (CDC). Highlights in minority health & health disparities. Office of Minority health & Health Disparitie. (Online) 2008. Available: http://www.cdc.gov/omhd/highlights/2008/hfeb08.htm (Accessed 20 December 2010).
2. Office of Minority Health, Office of the Director, CDC. Health disparities experienced by black or African Americans - United States. Morbidity and Mortality Weekly Report 2005; 54(1): 1-3. Available: http://www.cdc.gov/mmwr/preview/mmwrhtml/mm5401a1.htm (Accessed 20 December 2010).
3. Gamm L, Hutchison L, Bellamy G, Dabney BJ. Rural healthy people 2010: identifying rural health priorities and models for practice. Journal of Rural Health 2002; 18(1): 9-14.
4. Marmot M. Social determinants of health inequalities.The Lancet 2005; 365(9464): 1099-1104.
5. Wilkinson R, Marmot M. Social determinants of health: the solid facts, 2nd edn. Geneva: World Health Organization, 2003.
6. World Health Organization. Programmes and Projects: Social determinants of health. (Online) 2010. Available: http://www.who.int/social_determinants/en/ (Accessed 27 August, 2010).
7. Hartley D. Rural health disparities, population health, and rural culture. American Journal of Public Health 2004; 94(10): 1675-1678.
8. Smedley BD, Syme SL. Promoting health: intervention strategies from social and behavioral research. American Journal of Health Promotion 2001; 15: 149-166.
9. Johnson S, Abonyi S, Jeffery B, Hackett P, Hampton M, McIntosh T et al. Recommendations for action on the social determinants of health: a Canadian perspective. The Lancet 2008; 372(9650): 1690-1693.
10. Mukhopadhyay A. Tackling health determinants in rural India: the KHOJ initiative. Global Health Promotion 2010; 17(1): 69-72.
11. McLeroy KR, Bibeau D, Steckler A, Glanz K. An ecological perspective on health promotion programs. Health Education Quarterly 1988; 15(4): 351-357.
12. Burke NJ, Joseph G, Pasick RJ, Barker JC. Theorizing social context: rethinking behavior theory. Health Education and Behavior 2009; 36(5Suppl): 55S-70S.
13. Baffour TD, Chonody JM. African-American women's conceptualizations of health disparities: a community-based participatory research approach. The American Journal of Community Psychology 2009; 44(3-4): 374-381.
14. Powell W, Hollis C, de la Rosa M, Helitzer DL, Derksen D. New Mexico community voices: policy reform to reduce oral health disparities. Journal of Health Care for Poor and Underserved 2006; 17(1Suppl): 95-110.
15. Sweat MD, Denison JA. Reducing HIV incidence in developing countries with structural and environmental interventions. AIDS 1995; 9(Suppl A): S251-257.
16. Crabtree BF, Miller WL. Doing qualitative research: research methods for primary Care, 2nd edn. Thousand Oaks, CA: Sage, 1999.
17. Birks M, Chapman Y, Francis K. Memoing in Qualitative Research. Journal of Research in Nursing 2008; 13(1): 68-75.
18. Miles MB, Huberman AM. Qualitative data analysis. Thousand Oaks, CA: Sage,1994.
19. Lincoln Y, Guba EG. Naturalistic inquiry. Thousand Oaks, CA: Sage,1999.
20. US Census Bureau. American factfinder 2000. Fact sheet report. (Online) no date. Available: http://quickfacts.census.gov/qfd/states/13/13109.html (Accessed 30 August 2010).
21. Frederick S, Loewenstein G, O'Donoghue T. 'Time discounting and time preference': a critical review. Journal of Economic Literature 2002; 40(2): 351-401.
22. Baum F. Cracking the nut of health equity: top down and bottom up pressure for action on the social determinants of health. Promotion & Education 2007; 14(2): 90-95.
23. Morrow V. Children's 'social capital': implications for health and well-being. Health Education 2004; 104(4): 211-225.
24. Putnam RD, Leonardi R, Nanetti R. Making democracy work: Civic traditions in modern Italy. Princeton: Princeton University Press, 1993.
25. Cohen S, Syme SL, eds. Social support and health. Orlando: Academic Press, 1984.
26. Northridge ME, Sclar ED, Biswas P. Sorting out the connections between the built environment and health: a conceptual framework for navigating pathways and planning healthy cities. Journal of Urban Health, 2003; 80(4): 556-568.
27. Schulz A, Northridge ME. Social determinants of health: implications for environmental health promotion. Health Education & Behavior 2004; 31(4): 455-471.
28. Gordon-Larsen P, Nelson MC, Page P, Popkin BM. Inequality in the built environment underlies key health disparities in physical activity and obesity. Pediatrics 2006; 117(2): 417-424.
29. Sallis JF, Glanz K. The role of built environments in physical activity, eating, and obesity in childhood. The Future of Children 2006; 16(1): 89-108.
30. Ross C, Wu C. The links between education and health. American Sociological Review 1995; 60: 719-745.
31. Geronimus AT. Understanding and eliminating racial inequalities in women's health in the United States: the role of the weathering conceptual framework. Journal of American Medical Women's Association 2001; 56(4): 133-136, 149-150.
32. Williams DR, Neighbors HW. Jackson JS. Racial/ethnic discrimination and health: findings from community studies. American Journal of Public Health 2008; 98(9 Suppl): S29-S37.
33. Bose M, Olivan B, Laferrere B. Stress and obesity: the role of the hypothalamic-pituitary-adrenal axis in metabolic disease. Current Opinions in Endocrinology, Diabetes, and Obesity 2009; 16(5): 340-346.
34. Larson A, Gillies M, Howard PJ, Coffin J. It's enough to make you sick: the impact of racism on the health of Aboriginal Australians. Australian and New Zealand Journal of Public Health 2007; 31(4): 322-329.
35. Dixon J, Welch N. Researching the rural-metropolitan health differential using the 'social determinants of health'. The Australian Journal of Rural Health 2000; 8(5): 254-260.

