Approximately 42% of the Irish population live in rural areas1; however, there is limited knowledge of their health status and sense of wellbeing2-4 because urban populations are more researched5. Certain health advantages have been reported to be associated with living in a rural setting. For instance, rural inhabitants are less likely to report poor mental health3 and have been shown to be generally healthier than their urban counterparts, with lower mortality rates from cancer, and circulatory and respiratory diseases2. Compared with urban communities, traditional rural communities have been associated with strong social and family networks, and such dense social networks have been positively correlated with life satisfaction and protective effects on health6. An individual's environment also has a role, for people living within a 1 or 3km radius of a natural, green environment have been reported to have better self-perceived health compared with those living in urbanised areas7, possibly due to reduced stress and fatigue, sustained attention, promotion of physical activity and facilitation of social cohesion8.
The disadvantages of living in a rural setting have also been reported, including higher mortality rates among children and young people in rural areas of Northern Ireland2, and higher rates of stress, anxiety and depression in farmers and farming families in Northern Ireland9. Evidence of higher suicide rates in rural areas, especially among males10, is alarming. These trends may be related to higher rates of deprivation of11 or geographical inaccessibility to health and emergency services12. In addition, the rural environment may contribute to higher rates of obesity due to less opportunity for physical activity related to long commuting distances and lower access to formal leisure facilities5.
In Canada, Australia and the USA, for example, higher mortality rates have been reported among rural populations13-15; while in Ireland and the UK the opposite is has been found2,16. Thus, studies on the health status of rural inhabitants compared with their urban counterparts have yielded mixed and sometimes conflicting results. Furthermore, within rural areas variations in self-rated health and mental health outcomes have been reported5, suggesting the existence of positive and negative determinants of health status and wellbeing.
There is scarce international data and no data from rural communities in Ireland exploring these conflicting issues from the perspective of the inhabitants themselves. Therefore, the aim of the present study was to identify the determinants of health, health needs, and healthcare services in a rural community in the west of Ireland.
Community under study
The rural community under study is served by the Ballyvaughan medical practice, which has an 85 year history as a single-handed rural practice located in the Burren region of North Clare. The main practice centre is in the village of Ballyvaughan; a satellite clinic is operated once a week 16 km (10 miles) away in the village of Fanore. The practice caters for a population of approximately 2500 people spread over a wide geographical area of 500 km2 approximately17.
Irish health system
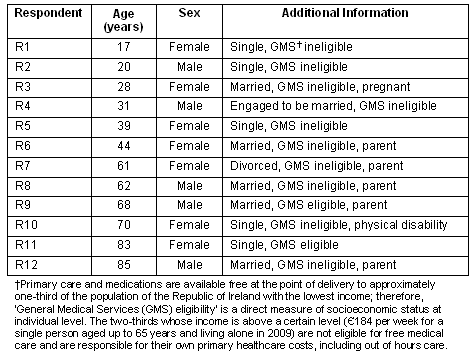
Primary care and medications are available at the point of delivery without cost to the approximate one-third of the population of the Republic of Ireland with the lowest income. Therefore 'general medical services (GMS) eligibility' is a direct measure of individual-level socioeconomic status. The two-thirds of the population whose income is above a certain threshold (?184 per week for a single person aged up to 65 years who lived alone in 2009) are ineligible for free medical care and are responsible for their own primary healthcare costs, including out of hours care.
Design
Ethical approval was obtained from the research ethics committee of the Irish College of General Practitioners.
Consecutive patients attending the practice during a designated 14 day period during May 2010 were asked to consent to participate in the study, after a brief explanation of the study aims and objectives. From these patients, a purposeful sample of 12 participants was chosen to partake in semi-structured one-on-one interviews with one of the investigators. The sample was chosen as an accurate representation of the practice population in terms of age, sex, and GMS eligibility. All interviews were tape recorded with participants' permission.
The framework for the topic guide for interviews is shown (Fig1). This was generated from the study aims and objectives and a review of the literature. In keeping with the iterative nature of qualitative research, the topic guide was modified during the data collection stage in order to capture and re-visit emerging themes, as appropriate18.

Figure 1: Interview topic guide for semi-structured interviews.
Following verbatim transcription, data were analysed according to the principles of framework analysis19. Framework analysis involves the following 5 key stages19:
- Familiarisation - preliminary examination of the data entailing an initial reading of all data.
- Developing a thematic framework - producing analytical categories from respondents' statements or responses to the researchers enquiries and other key areas identified by respondents themselves.
- Indexing the material - identifying instances of analytical categories involving searches for key words or phrases.
- Charting - grouping instances under headings or particular research questions.
- Mapping and interpretation to inform the key objectives of the research - synthesising the range of views under particular themes to produce an overall picture on a range topics and relating this to other relevant research and theoretical perspectives.
Each author read the collected qualitative data several times. To identify conceptual themes they independently and systematically reduced the text, making comparisons with the research literature19. This process was carried out independently by the four researchers to enhance reliability19. Themes were shared and debated within the multidisciplinary team of authors (a medical student, a family doctor, a dietician and a research scientist), which is known to heighten reflexivity in the interpretation process20. A concordance of views on common themes was reached after discussion and debate.
Respondents were assigned a numerical code during data input to ensure anonymity, and these codes are used throughout the results section. Any references to names in respondents' answers have been changed.
During the 14 day study period, 564 patients from the total practice population of 2130 patients attended the practice. The demographic profiles of the 12 participants were chosen as a purposeful sample of attendees (Table 1). From the analysis of data, 5 key themes emerged: community, environment, familiarity, accessibility, and expectation.
Table 1: Demographic characteristics of study participants (n=12), who are listed in increasing order of age.
Community
A central theme 'community' emerged, with several respondents acknowledging the value of being able to talk to and confide in a large network of family or friends. Many participants highlighted as advantages the strong sense of community, close family ties, and the idea of knowing your neighbours:
I'm delighted to have a baby in a rural environment. It's really like a big family, you know everyone is looking out for you. My nearest neighbour is maybe two fields away, but we all know one another and look out for one another. I like the idea that I know my neighbours and they can keep an eye on the family. (R3, 28 year-old married female)
However, some patients admitted that integrating into a rural community was difficult, especially with regard to social isolation. However, there was also the suggestion that interaction was obtainable if one wished:
The opportunities are there, it's up to you to get up and go if you want to get involved. I think you are as isolated as you want to be; if you want to go and visit people or whatever or if you want to stay on your own and be a hermit you can do that too. (R6, 44 year-old married female)
Involvement in the community varied. Some participants described a desire to give something back to organizations from which they benefited. Others were involved in organizations of interest to their children or themselves, or for the sake of the community. In general, the strong sense of community was identified as a positive reason factor to living in a rural area. Furthermore, these dense social and family networks appeared to have a positive influence on the mental health and wellbeing of rural inhabitants.
Environment
The consensus among patients was that they liked many aspects of living in the rural environment, including the open spaces, the ocean, local flora and fauna, fresh air, and peace and quiet. Some respondents also highlighted the ability of the environment to influence their health:
I do have down times, we all do. I just get through this or go for a walk or go down by the sea. (R7, 61 year-old divorced female)
Health-wise, it's very good...I appreciate the very clean air. (R11, 83 year-old single female)
It was suggested that events in the town reflect the natural seasons, for instance foods such as fruits, vegetables, and seafood were expected and prepared at certain times of the year. There were also negative comments about the environment, especially related to social isolation, an particularly in winter:
It's like living in two completely different places in the one year - in summertime it is really, really busy - then in wintertime, nothing is happening at all. So it's a little bit schizophrenic. I think the village goes into hibernation in winter. You are quite expended during the summer season and then the winter it's just time to re-group and maybe come into yourself a little bit more - rest. (R3, 28 year-old married female)
Although some patients indicated that working locally could be a challenge due to the limited employment opportunities, there were also examples of advantages:
On your own farm, you are your own boss, you're out in the fresh air every day - 'tis grand. You learn the value of hard work. (R2, 20 year-old single male)
Many of the patients interviewed included walking as their major form of exercise. Other patients suggested that their major form of physical activity was the physical labour involved with their farm work. There were some comments about the lack of local facilities, such as exercise gyms or local dance classes which might assist in increasing their level of activity.
In addition, many commented on the importance of healthy foods in the community and highlighted the local farmer's market as a major attraction, with its added advantage of the social benefits of a community gathering. Some patients indicated that it was an advantage to have a limited selection of foods available, especially highlighted was the absence of fast food restaurants locally. There was also general consensus that while healthy foods were available locally, it was difficult to complete grocery shopping locally, either due to lack of availability or high cost:
If you had a family, you couldn't buy all the food locally - it's just too dear. So that's why a lot of people would go [to the supermarket] to buy in bulk; it's a lot cheaper. (R5, 39 year-old single female)
On the whole, all participants acknowledged that the proximity to nature and fresh air were advantages to living in the area and that such factors had a positive influence on their physical and mental health.
Familiarity
There was a sense of familiarity with the doctors in the local practice, and most patients indicated that they felt they could confide in them with most issues. However, the young patients interviewed seemed less likely to discuss problems with their family physician:
I don't really talk to people when I'm feeling down. I think I can cope with things myself but if I couldn't I'd talk to somebody. I'd never come to the doctor to talk about it, no matter how bad it was, but I'd definitely talk to a friend or someone very close. (R1, 17 year-old single female)
Furthermore, when asked about overall wellbeing, a number of participants acknowledged that they usually tried to deal with issues alone or didn't want to 'trouble' others with their problems. Of particular concern was that young men were less likely to confide in their GP concerning mental health issues:
I don't think younger guys would [come to the family doctor for depression], I don't think younger guys understand it. (R4, 31 year-old male, engaged to be married)
Although most participants reported having a very good relationship with their family doctor, a small number, particularly males and young people, would not confide personal mental health concerns to their family doctor.
Accessibility
Another key theme was 'accessibility'. It was commented that people with limited mobility may have difficulty accessing services, or that GMS-eligible patients may be more aware of the accessible services. It was also suggested that access to various facilities, such as clothes shops, public libraries, cinema, swimming pool or fitness clubs was poor. Comments about transportation were very much related to accessibility, with many mentioning the need to own a car, and the large travelling distance to access services:
I just think of my father, he died at home of a heart attack. The ambulance had to come from... about 40 minutes away. By the time you'd phoned...and gone through all the different channels you had to go through, I said: 'Look, the man is dying like, he's probably gone now anyway'. I suppose I panicked. It's very easy to say not to panic but you do. So that was a hard situation. (R5, 39 year-old single female)
Some of the younger participants described a lack of suitable activities, including an active nightlife, and this was given as an explanation for why young people leave the community:
I think it's very important just to get away, to experience life in the city, then you actually realise what you're missing in the country. (R4, 31 year-old male, engaged to be married)
There was general agreement that the health services available locally were of high quality, comprehensive and accessible to all. While some patients were happy to get their medications from the medical practice, others highlighted the lack of a local pharmacy as a shortcoming, as well as the lack of local access to allied health services such as speech therapy.
Expectation
'Expectation' has been shown to be a key determinant of satisfaction with healthcare services21. The statement below exemplified the fact that participants from this rural community did not seem burdened with unrealistic or complex sets of expectations about local health services, or indeed life in general, which may have contributed to participants' generally positive outlook:
As long as we eat well and sleep well - we're kind of very happy that way. We don't demand an awful lot of ourselves. (R3, 28 year-old married female)
Discussion
Study design and limitations
This study illustrated a number of important determinants of health and wellbeing in a rural population. Strengths in the design included the semi-structured format of the interviews and the process of purposeful sampling of patients which facilitated a broad representation of patients views. Studies have shown that 90% of a community consult their GP within a year; therefore, sampling consecutive patients presenting to the practice may be an accurate reflection of members of the community22. In addition, the multidisciplinary team of authors heightened reflexivity in the interpretation process.
Limitations of the study included poor representation of young males presenting to the practice. In addition, the population studied had a lower than average national deprivation score, which makes generalization to all rural communities difficult. It was also difficult to define the term 'rural' with reference to studies in other countries, and with the intent of ruling out urbanised areas in this study. Much of the data regarding the health needs of people living in rural areas originate from Canada, Australia and USA13-15; areas in which rural living differs significantly in many aspects to life in rural Ireland. For example, people living in rural areas of Ireland and the United Kingdom have been shown to experience better health overall than their urban counterparts; whereas, the opposite is true in the other countries mentioned. Finally, one of the researchers (LG) worked in the practice studied, which was a potential source of bias. In order to reduce this potential bias, this researcher did not have any input into the patient selection or interview process.
Main findings
The strongest theme to emerge from this study was the sense of community and family connections among participants from this rural area. These social and family networks were a significant source of psychosocial support for several of the participants. This finding is consistent with numerous studies which reported that traditional rural communities have much stronger family and social relationships compared with urban communities, and this has a positive, protective effect on their health and life satisfaction6,23. There is growing recognition of the importance of rural social networks, many of which have been undermined by rural de-population and poor employment prospects in rural areas. Recent initiatives such as the Irish organization Maicre na Feirme ('the Elite of the Land'), represent an effort to facilitate and galvanize such networks24. An inverse relationship between depression and the strength of informal, intimate social relationships has been reported25, while social support has been emphasised as a strong predictor of health and subjective wellbeing for older rural adults23. This is also important for the wellbeing of children, which was reported to be enhanced by strong cohesion in the neighbourhood, and crucially affected by factors such as school, the natural environment and sporting associations26.
There was a general consensus among participants that being surrounded by the natural environment was beneficial to their health and wellbeing. This suggestion is supported by research showing a lower prevalence of asthma and respiratory symptoms in rural communities, which may be related to environmental factors such as less air pollution27. It has also been shown that the percentage of 'green space' in a persons' living environment has been positively correlated with self-perceived health7, neighbourhood satisfaction and time spent on physical activity28, as well as lower mortality rates29. In contrast, one study showed no relationship between the amount of green space and the level of physical activity during leisure time30. The suggestion that long commuting distances and a lack of indoor leisure facilities may contribute to lower levels of physical activity in rural areas5 is in agreement with the current study, where several participants reported a lack of and need for indoor leisure facilities in the community. Finally, the natural environment was beneficial in providing seasonal fresh produce and natural products at the local farmers' market, and this was universally mentioned by respondents. However, the ease of obtaining 'healthy' food was also questioned, being frequently reported as too expensive to buy from the local shop. Therefore, it is not only the availability of healthy foods in small communities that are an issue, but if such foods are judged to be too expensive to purchase, they will not form part of rural diets.
Familiarity with and continuity of the local family doctors and health service was also identified as having a positive influence on respondents' health and wellbeing. However, there was a general reluctance among younger patients to present to doctors, which is not unique to rural areas and is reported to involve issues of confidentiality and access31. A review of a large database revealed that young people who readily expressed concerns by email had difficulties disclosing concerns about their health to parents and doctors face-to-face32. As in traditional rural communities, the family doctors who live in the rural area under study are in a unique position to develop long-term relationships with patients and their families, remember important life events and provide support during emotionally difficult times. Providing continuity of care is fundamental to the GP role, and this is particularly evident in rural communities where GPs hold the patient's 'lifetime clinical record', as the doctor-patient therapeutic relationship develops over years and multiple encounters33,34. With this positive relationship in mind, it must also be noted that significant resources have been directed to recruitment, training and retention of doctors in rural Irish settings35; however, shortages of rural doctors remain in countries such as Australia36 and Canada37.
Of particular interest were the expectations and the general attitude that people in the community were happy with the basic necessities of life, and also appeared to be satisfied with the health care they received. In stark contrast, in parts of the USA more is spent on health care per capita than in any other country, but residents do not show consistent evidence of being more satisfied with the quality of their health care38. Furthermore, studies have shown that rural inhabitants often have functional views of health and illness, differentiating between health problems that can be endured for a while, compared with those that interfere with daily functioning39. Further studies have postulated that such 'health resilience' and low expectations may be enhanced by geographical inaccessibility of services and a 'frontier' mentality with inherent connections to 'the land'40.
Rural areas are at a disadvantage in terms of the geographical inaccessibility of a number of services, and this appears to be a negative determinant of health and wellbeing41. Geographical isolation and the need for a good public transport system, as well as poor access to emergency services were emphasized in the study. These findings are supported by a study showing that in rural communities, poor access to emergency services such as ambulance or fire services, rather than health care specifically, affected inhabitants most1. Other highlighted services included the need for a local pharmacy and the availability of alternative therapies and speech therapy at the medical centre. Despite these findings, participants were consistently happy with the services available locally and, in general, believed their health needs were met. This is inconsistent with numerous studies, which reported that access to services, particularly medical services, was much worse in rural communities41. The positive view of health services may be a reflection of the type of people who make up the community, or may also be related to the structure of health care in the region under study. The establishment of a primary care team in 2004 in the area under study, as part of the Irish national primary care strategy42, may be significant in this regard. The primary care teams in Ireland consist of multidisciplinary health professionals who work together (in the case of this community under the one roof) to deliver health and personal social services accessible to the community served, which leads to better continuity of care and service co-ordination42.
A cause of concern that emerged in assessing the mental health status of respondents was the finding that many people were more likely to deal with mental issues alone, not wanting to 'trouble' others with their problems. This is a particularly worrying finding in view of the high rate of suicide in rural communities10, combined with the fact that rural mental health services are overstretched, and that rural people are very suspicious and wary of contacting those that do exist38. In comparison with younger people living in urban areas, the limited educational and employment opportunities, and recreational activities of rural inhabitants have been suggested as impacting on mental health outcomes and contributing to risk-taking behaviour43. The unwillingness to consult with others may be a consequence of living in a small community, where anonymity can be difficult, and a person may be concerned about the stigma associated with mental health issues. Stigma and discrimination have been highlighted as underlying causes of social exclusion44, and this can have an even greater effect on the person's life than a mental health issue. The consistently high rates of death by suicide in Ireland over the past 20 years have paralleled qualitative changes to Irish society, which is now more time pressured, less caring and more materialistic45. Interestingly, the loss of a sense of community in many regions of the country has contributed to some of these changes. These findings highlight a need to focus on mental health in rural environments, and to increase public awareness and attitudes. The factors that determine mental health are complex, and although the social support and contact available in close-knit rural communities may be protective, rural isolation and the inaccessibility of services may have a negative effect on mental health. Efforts in this regard have been made recently, with The National Office for Suicide Prevention's public advertisement campaign and website46. This promotional campaign was aimed at young people and discusses isolation as a common problem. Although efforts such as these begin to address mental health issues in young people, further efforts and research are required.
Implications
Important implications for determinants of health in this study include the strength of the community and its level of affluence. The importance of the community was a central theme in this study, and it has been shown previously that the personal and social quality of human relationships is relevant to health and longevity22. In a pioneering study in a small American town, inhabitants focused on family, cooperation, lack of distinction between rich and poor, as well as greeting, enjoying and helping neighbours, and there was clinical evidence that coronary artery disease was significantly lower than in the two neighbouring control towns, despite similar prevalence of conventional risk factors, including high serum cholesterol, high fat diet, and smoking47.
In addition, the affluence of a community has been shown to impact on health. Although much of the variation in health outcomes among individuals remains unexplained, the most powerful social determinants of adult health are contained within the elements of individual socioeconomic status44. In the case of the people interviewed in the present study, the majority described some type of work or activity to 'keep themselves busy', and when they were questioned specifically about 'making ends meet' financially, none described difficulties. Thus, these factors together may produce similar effects for the inhabitants of this small community that was not unmasked in this study.
In the present qualitative analysis of the determinants of health in a rural community in the West of Ireland, emerging themes underlined the advantages of living in a rural environment, including the strong sense of community, the benefits of the natural environment, familiarity, and lower sense of expectation. Issues concerning geographical inaccessibility and hesitation in confiding mental health issues with medical professionals highlight that a great deal of work is needed in order to increase public awareness and change attitudes towards mental health issues. This is particularly important considering the dominant urban focus in previous research on the social geographies of mental health, which have obscured the experiences of people with mental health problems living in rural localities48.
Acknowledgement
The authors thank the patients and staff of the rural primary care centre and community for their assistance and participation in this project.
References
1. Tay JB, Kelleher CC, Hope A, Barry M, Nic Gabhainn S, Sixsmith J. Influence of sociodemographic and neighbourhood factors on self rated health and quality of life in rural communities: findings from the Agriproject in the Republic of Ireland. Journal of Epidemiology and Community Health 2004; 58: 904-911.
2. O'Reilly G, O' Reilly D, Rosato M, Connolly S. Urban and rural variations in morbidity and mortality in Northern Ireland. BMC Public Health 2007; 7: 123.
3. Fitzsimon N, Shiely F, Corradino D, Friel S, Kelleher CC. Predictors of self-reported poor mental health at area level in Ireland: a multilevel analysis of deprivation and social capital indicators. Irish Medical Journal 2007; 100(8Suppl): S49-S52.
4. Kelleher CC, Friel S, Nic Gabhainn S, Tay JB. Socio-demographic predictors of self-rated health in the Republic of Ireland: findings from the National Survey on Lifestyle, Attitudes and Nutrition, SLAN. Social Science & Medicine 2003; 57: 477-486.
5. Riva M, Curtis S, Gauvin L, Fagg J. Unravelling the extent of inequalities in health across urban and rural areas: evidence from a national sample in England. Social Science & Medicine 2009; 68: 654-663.
6. Yoon DP, Othelia Lee E-K. The impact of religiousness, spirituality and social support on psychological well-being among older adults in rural areas. Journal of Gerontological Social Work 2007; 48(3-4): 281-298.
7. Maas J, Verheij RA, Groenewegen PP, de Vries S, Spreeuwenberg P. Green space, urbanity and health: how strong is the relation? Journal of Epidemiology and Community Health 2006; 60: 587-592.
8. Groenewegen PP, van den Berg AE, de Vries S, Verheij RA. Vitamin G: effects of green space on health, well-being, and social safety. BMC Public Health 2006; 6: 149.
9. Magee S. Farmers and Farm Families in Northern Ireland: the results of a social survey of farmers and farm families conducted in 2001/02. Norwich: Department of Agriculture and Rural Development Economics and Statistics Division, National Statistics, 2002.
10. Singh GK, Siahpush M. Increasing rural-urban gradients in US suicide mortality, 1970-1997. American Journal of Public Health 2002; 92(7): 1161-1167.
11. Stark C, Hopkins P, Gibbs D, Belbin A, Hay A. Population density and suicide in Scotland. Rural and Remote Health 7: 672. (Online) 2007. Available: www.rrh.org.au (Accessed 20 July 2011).
12. Ryan-Nicholls K. Health and sustainability of rural communities. Rural and Remote Health 4: 242. (Online) 2004. Available: www.rrh.org.au (Accessed 20 July 2011).
13. Australian Institute of Health and Welfare. Rural, regional and remote health. A study on mortality. Rural Health Series, no 8. Canberra, ACT: AIHW, 2007.
14. Eberhardt MS, Pamuk, ER. The importance of place of residence: examining health in rural and non-rural areas. American Journal of Public Health 2004; 94: 1682-1686.
15. Pampalon R, Martinez J, Hamel D. Does living in rural areas make a difference for health in Quebec? Health & Place 2006; 12(4): 421-435.
16. Connolly S, O'Reilly D, Rosato M. Increasing inequalities in health: is it an artefact caused by the selective movement of people? Social Science & Medicine 2007; 64(10): 2008-2015.
17. HSE Mid-Western Area. Primary Care Team Mapping Exercise. Limerick: HSE Mid-Western Area, 2006.
18. Greenhalgh T, Taylor R. How to read a paper: papers that go beyond numbers (qualitative research). BMJ 1997; 315(7110): 740-743.
19. Carter Y, Shaw S, Thomas C. An introduction to qualitative methods for health professionals. London: Royal College of General Practitioners, 1999.
20. Barry CA, Britten N, Barber ND. Using reflexivity to optimize teamwork in qualitative research. Qualitative Health Research 1999; 9: 26-44.
21. McKinley RK, Stevenson K, Adams S, Manku-Scott TK. Meeting patient expectations of care: the major determinant of satisfaction with out-of-hours primary medical care? Family Practice 2002; 19: 333-338.
22. Mant D. Principles of prevention. In: R Jones, N Britten, L Culpepper, D Gass, R Gro, D Mant, C Silagy (Eds). Oxford Textbook of Primary Medical Care. Oxford: Oxford University Press, 2005; 369-372.
23. Mair CA, Thivierge-Rikard RV. The strength of strong ties for older rural adults: regional distinctions in the relationship between social interaction and subjective well-being. The International Journal of Aging and Human Development 2010; 70(2): 119-143.
24. Macra na Feirme. Rules and constitution. Macra na Feirme. (Online) no date. Available: http://www.macra.ie (Accessed 6 November 2010).
25. Bosworth HB, Steffens DC, Kuchinbbatla MN, Jiang WJ, Ariasm RM, O'Connor CM et al. Relationship of social support, social networks and negative events with depression in patients with coronary artery disease. Aging & Mental Health 2000; 4(3): 253-258.
26. Eriksson U, Asplund K, Sellstrom E. Growing up in rural community-children's experiences of social capital from perspectives of wellbeing. Rural and Remote Health 10: 1322. (Online) 2010. Available: www.rrh.org.au (Accessed 20 July 2011).
27. Iversen L, Hannaford PC, Price DB, Godden DJ. Is living in a rural area good for your respiratory health? Results from a cross-sectional study in Scotland. Chest 2005; 128: 2059-2067.
28. Bjork J, Albin M, Grahn P, Jacobsson H, Ardo J, Wadbro J et al. Recreational values of the natural environment in relation to neighbourhood satisfaction, physical activity, obesity and wellbeing. Journal of Epidemiology and Community Health 2008; 62: 1-7.
29. Takano T, Nakamura K, Watanabe M. Urban residential environments and senior citizens' longevity in megacity areas. The importance of walkable green spaces. Journal of Epidemiology and Community Health 2002; 56: 913-18.
30. Maas J, Verheij RA, Spreeuwenberg P, Groenewegen PP. Physical activity as a possible mechanism behind the relationship between green space and health: a multilevel analysis. BMC Public Health 2008; 8: 206.
31. McPherson A. ABC of adolescence: adolescents in primary care. BMJ 2005; 330: 465-467.
32. Harvey K, Churchill D, Crawford P, Brown B, Mullany L, Macfarlane A et al. Health communication and adolescents: what do their emails tell us? Family Practice 2008; 25(4): 304-311.
33. Scott-Jones J. Defining the role of the GP in a primary health care team: the GP genome and phenotype 2009-2020. Wellington: The Royal New Zealand College of General Practitioners New Zealand, 2009.
34. Royal College of General Practitioners. Curriculum statement 3.3: Clinical ethics and value-based practice. (Online) 2007. Available: http://www.rcgp-curriculum.org.uk/pdf/curr_3_3_Clinical_ethics.pdf (Accessed 30 July 2011).
35. Nic Gabhainn S, Murphy AW, Kelleher C. A national general practice census: characteristics of rural general practices. Family Practice 2001; 18: 622-626.
36. Hoyal FM. Retention of rural doctors. Australian Journal of Rural Health 1995; 3: 2-9.
37. Collier R. Medical school admission targets urged for rural and low-income Canadians. Canadian Medical Association Journal 2010; 182: E327-E328.
38. Davis K, Schoen SC, Doty MM, Holmgren AL, Kriss JL, Shea, KK. Mirror, Mirror on the wall: an international update on the comparative performance of American health care. New York: The Commonwealth Fund, 2007.
39. Long KA. The concept of health: rural perspectives. Nursing Clinics of North America 1993; 28: 123-130.
40. Veitch C. Impact of rurality on environmental determinants and hazards. Australian Journal of Rural Health 2009; 17: 16-20.
41. Borders TF, Aday LA, Xu KT. Factors associated with health related quality of life among an older population in a largely rural western region. Journal of Rural Health 2004; 2(1): 67-75.
42. Department of Health and Children. Primary care: a new direction. Quality and fairness - a health system for you. Dublin: The Stationary Office, 2001.
43. Quine S, Bernard D, Booth M, Kang M, Usherwood T, Alperstein G et al. Health and access issues among Australian adolescents: a rural-urban comparison. Rural and Remote Health 3:245. (Online) 2003. Available: www.rrh.org.au (Accessed 20 July 2011).
44. Ziembroski JS, Breiding MJ. The cumulative effect of rural and regional residence on the Health of Older Adults. Journal of Aging and Health 2006; 18: 631-659.
45. Department of Health and Children. A vision for change; report of the expert group on mental health policy. Dublin: The Stationary Office, 2006.
46. The National Office for Suicide Prevention. (Online) 2009. Available: http://www.letsomeoneknow.ie (Accessed 5 November 2010).
47. Wolf S, Bruhn JG. The power of clan: the influence of human relationships on heart disease. New Jersey: Transaction, 1993.
48. Parr H, Philo C, Burns N. Social geographies of rural mental health: experiencing inclusions and exclusions. Transactions of the Institute of British Geographers 2004, 29(4): 401-419.


