The effect of trauma on an individual or group can be devastating1:
Traumatic events confront people with both an external and internal reality which attack ideals and beliefs about safety and personal control. The external reality is of danger and uncontrollable events that may kill, maim, brutalise or destroy. Disaster, war, rape, assault, motor vehicle accidents and predatory violence also generate an internal reality of fear, horror and helplessness. The person is often affected more by the harrowing memories than the event itself. This leads to a sense of recurrent trauma, triggered by even the most subtle of stimuli.
Aboriginal Australians are arguably one of the most traumatised people in the world. The consequences of exposure to traumatic events experienced by generations of Aboriginal people include poor health outcomes with compounding psychiatric disorders and complex psychosocial health problems2,3. Documenting and understanding traumatic events and prevalence of Posttraumatic Stress Disorder (PTSD) will lead to a comprehensive understanding of issues affecting the current health and welfare of Indigenous people, and assist the development of effective strategies to address the health concerns of this historically marginalised and traumatised population.
Abundant literature indicates that Aboriginal people have been exposed to a variety of traumatic events associated with official policies of successive governments4:
Aboriginal culture is a history of brutality and bloodshed. The assault on Aboriginal people includes massacres, diseases, dispossession and dispersal from the land. Aboriginal people were not only dispossessed of the land, but also much of the traditional culture and language was taken from them. For many years in many parts of Australia, Aboriginal people were herded onto reserves and missions.
The impact of trauma is worsened when a traumatic event is designed, planned and systematically executed by the very people looked to for protection5,6. This was the case for Aboriginal Australians, for the attack on Aboriginal culture, family and communities was planned and executed systematically. Aboriginal people's exposure to traumatic events and its effect was then maintained through moving them into missions and reserves with escapees being killed7-10. This was disguised as being 'for their own welfare'(p14)4:
...until very recently, Aboriginal children were taken away from their mothers, placed in institutions and in some states [were] used as cheap labour. I cannot overstate the traumatic consequences of policy and the destruction of Aboriginal culture and community life that resulted. It seems incredible now, but it was the policy of successive governments to destroy Aboriginal family life under the banner of assimilation.
The impact of this policy on direct victims and their offspring has been long lasting psychosocial health and emotional sequelae. One survivor described the consequences of being a Stolen Child in her adult life(p17)11:
...all I focused on was looking after my children. You see the word welfare was still indented in my brain, and I made a pact with myself that nobody was going to take my children away.
The damage is not limited to those who were removed, but has been passed on to their descendants in transgenerational trauma and complex traumatic effects. This has manifested in form of avoidance, hypervigilance and intrusive thoughts in some cases, and in others it may be complicated by alcohol and substance abuse, violence against self and others, with the potential for misdiagnosis ultimately resulting in ineffective therapeutic interventions.
Other impacts of trauma include a high level of domestic violence and other offences resulting in the higher than national average imprisonment of Aboriginal people12,13. The level of violence and aggression reported in Aboriginal communities bears no relationship to Aboriginal culture and history. In particular, reports of child abuse is contrary to the gentleness, kindness and generosity of Aboriginal people reported by the first settlers and missionaries14,15.
The complexity and extent of exposure to traumatic events by Aboriginal people suggests a potentially high rate of PTSD and other psychiatric disorders. However, mainstream health professionals pay little attention to PTSD when assessing an Aboriginal patient who may be overwhelmed by prominent psychiatric symptoms such as psychosis, depression, and drug and alcohol ingestion16. Another factor influential in health professionals' non-recognition of PTSD when assessing Aboriginal clients is the limitation of the current diagnostic criteria, which do not account for types of historical traumatic events experienced by generations of Aboriginal people4,8,9,16.
Both the International Classification of Diseases (ICD) code ICD-10 and Diagnostic and Statistical Manual of Mental Disorders (DSM) code DSM-IV descriptions of traumatic events are similar in meaning. The ICD-10 criterion 'A' for PTSD describes traumatic event as '...a stressful event or situation (either short- or long-lasting) of exceptionally threatening or catastrophic nature, which would be likely to cause pervasive distress in almost anyone'17. The DSM-IV criterion '(A)1' for PTSD states it to include '...event or events that involved actual or threatened death or serious injury, or a threat to the physical integrity of self or others'18. Based on ICD-10 and DSM-IV descriptions of traumatic events, some argue that the traumatic experience of historically disadvantaged people should not be regarded as a traumatic event that could result in PTSD or other psychiatric disorders19. This argument further asserts that PTSD is 'malingering' and a chosen expression aimed at financial or other form of gains20. However, such opponents of PTSD as a clinical diagnosis fail to understand the reality of the condition(p6)21:
...the critical element that makes an event traumatic is the subjective assessment by victims of how threatened and helpless they feel. So, although the reality of extraordinary events is at the core of PTSD, the meaning that victims attach to these events is as fundamental as the trauma itself.
Therefore, meaning and perception can result in PTSD, rather than an event. And while it is understood that a PTSD is the end result of exposure to traumatic events, not everyone exposed to traumatic events develops PTSD22-24. 'The development of PTSD is dependent on a complex interaction of pre-trauma, peri-trauma, and post-trauma variables' (p164)22. Pre-trauma variables include previous traumatic exposure, such as childhood physical and/or sexual abuse, and pre-existing psychiatric illnesses increase the likelihood of developing PTSD22,25,26. Peri-trauma risk factors are the severity of the trauma, the degree of threat and duration of exposure and intensity of the victim's response22,27,28. Post-trauma variables relate to a poor social network, absence or lack of family support, physical disability from trauma and the degree of loss; these are identified as determinants of the development of PTSD following exposure to a traumatic event29-33. Other mediating factors include pre-morbid personality, social class and socio-economic status, educational status, cultural background and ethnicity, and gender. All these risk factors are synonymous with the experience of Aboriginal people4,14,31,34,35.
The study
This is a population study conducted in Central West Region of Western Australia. The study targeted all who were eligible (see inclusion and exclusion criteria), and a total of 221 participants took part, all of whom were Aboriginal.
Ethical considerations
As part of the research ethics standard requirement for any research on human, this study was given community-wide consent following extensive consultation. Community support was required by the University of Adelaide Ethics Committee and Western Australian Aboriginal Health Information and Ethics Committee (WAAHIEC). Upon fulfilment of the above requirements, the study was approved by the Ethics Committee of the University of Adelaide and WAAHIEC (#H-58-2001).
Careful consideration was given to avoid any item that may lead to the identification of participants in the report and related publications. Prior to administering of the instrument, participants were given detailed information about the study including their right to withdraw at any time and without advance notice. Prior to the commencement of the interview participants were asked to sign a consent form.
Selection of participants: inclusion and exclusion criteria
As this was a population study, three Aboriginal communities were selected on the basis of observable level of traumatic events, accessibility, prior connection with the author and community leaders' indication of support for the study. Inclusion criteria for an individual participant were: Aboriginality, being resident in these communities and aged 18 to 65 years. Aboriginality and residency status were established through Aboriginal Health Workers.
Exclusion criteria were those with a cognitive impairment, severe physical illness causing current symptoms, and intoxication at the time of interview. A non-Aboriginal person was excluded from participating in the study regardless of their marital or other relationship to an Aboriginal person and community. As a population study, it was aimed to gain a maximum participation of eligible residents in the selected communities.
Instruments
A structured clinical interview and survey questionnaire were used to collect quantitative data. Four modules were administered: Anxiety disorders, Depression, Alcohol, Drug abuse and PTSD, of Composite International Diagnostic Interview (CIDI) Auto v2.1; Impact of Events Scale (IES); Alcohol Use Disorder Identification Test (AUDIT); and Indigenous Trauma Profile (ITP).
The ITP was developed to address the inability of the CIDI to elucidate some of the traumatic events experienced by generations of Aboriginal people. The Division of Mental Health of the World Health Organisation (WHO) developed the CIDI for clinicians to apply in community settings36,37. The CIDI was used in ICD-10 and DSM-IV to validate the PTSD diagnostic criteria and was found applicable in differing cultural settings, which is the basis for its use in this study36-38.
The validity, reliability and linguistic and semantic, cross-cultural conceptual and content equivalence of CIDI have been established via numerous studies conducted on various cultural groups36,37. The IES and AUDIT validity and reliability have been established in research on various groups in culturally diverse communities39,40. The IES also has been used in several studies involving combat veterans, assault victims, motor vehicle accident survivors, fire fighters and victims of natural disasters39. The AUDIT reliability and validity was established in a study carried out to identify alcohol related disorders and comorbidity40.
Data collection
Each subject was visited at home and given written information explaining the study. In addition, the explanatory note was read out by a health worker or researcher prior to the participant signing the consent form. Following the explanation of the study, those subjects who consented to participate were given survey questionnaires containing the IES, AUDIT and ITP. The CIDI was administered at the time of the visit, or an appointment was made for a more convenient time. The CIDI was administered by the author because it requires specific clinical skills to interpret and enter data correctly. The interview was conducted in an environment where the subjects felt comfortable and data was entered into a laptop. This was to ensure confidentiality because attending a designated centre may have exposed subjects to unwelcome attention. In this way any negative consequences were avoided for participants.
Demographic characteristics of the study population
For reasons of confidentiality, this article deliberately omitted information identifying the communities involved and participants' tribal background. The three towns are located in the Murchison Health District of the Central West Region of Western Australia. Of the participants, 47% (n=104) were male and 53% (n=117) female; their average age was 38 and is presented according to age groups (Table 1).
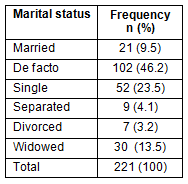
The marital status of the participants was classified according to 6 categories: married; de facto; single; separated; divorced; and widowed (Table 2). The majority of participants, 46.2% (n=102), were identified as being in a de facto relationship, followed by 23.5% (n=52) who identified as single.
Table 1: Participants' age distribution
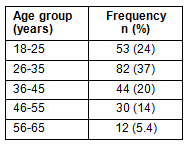
Table 2: Participants' marital status
Key findings
Rate of exposure to traumatic events, PTSD and alcohol use: The rate of life time exposure to traumatic events was 97.3% (n=215). A total of 55.2% (n=122) participants met DSM-IV diagnostic criteria for PTSD. Of participants who met diagnostic criteria for PTSD, 91% (n=111) also met diagnostic criteria for alcohol abuse. Alcohol abuse without PTSD and other psychiatric disorders accounted for 21.26% (n=47) (Fig1).
Other significant findings include depressive and anxiety disorders (Table 3). While major depression accounted for 22.3% (n=49) of participants, dysthymic disorder was found to be 2% (n=4).
As shown (Table 3), a total of 17.2% (n=38) participants met diagnostic criteria for anxiety disorders. Of this group, 7.9% (n=3) met DSM-IV diagnostic criteria for agoraphobia; 26.3% (n=10) for generalized anxiety disorder (GAD); 7.9% (n=3) for panic disorder; 47.4% (n=18) for a specific phobia; and 10.5% (n=4) for social phobia.
Age of onset of PTSD and alcohol abuse: The PTSD onset age indicates that traumatic events occurred at an early age and have disrupted adult life (Fig2). There is a strong association between PTSD and alcohol abuse onset age. The PTSD onset age started as early as 5 years of age and steadily increased, while alcohol abuse disorder onset started at the earliest at 15 years of age and had escalated by the late teens and early twenties. Both disorders showed the same trend.
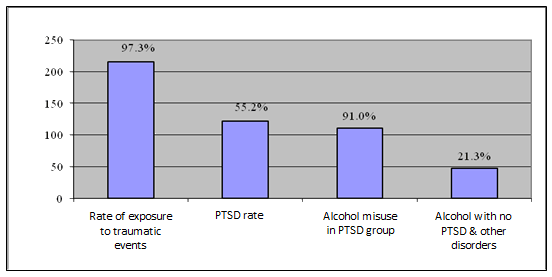
Figure 1: Participants' traumatic exposure, PTSD and alcohol abuse.
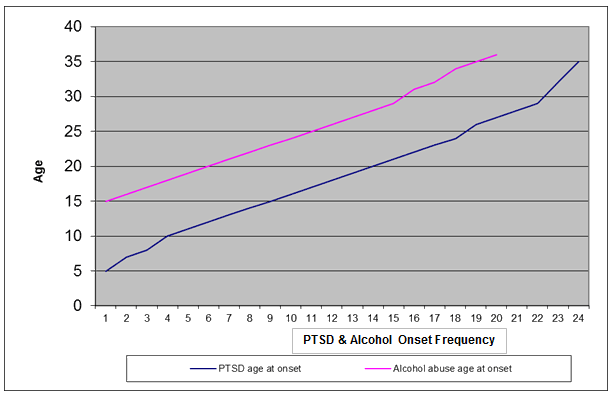
Figure 2: Age of onset for PTSD and alcohol abuse.
Table 3: Psychiatric disorders identified
(composite international diagnostic interview [CIDI] result)

Comparison of findings with another study
A comparison of the findings of this study with the Australian National Wellbeing and Mental Health Survey (ANWMHS) shows interesting contrasts28. A comparison is made of the types of traumatic events and life time prevalence of exposure reported in this study with the ANWMHS report (Table 4). However, only selected and similar variables reported in both studies were compared because the rate of exposure and types of traumatic events reported in this study are numerous and may be specific to the population studied.
A comparison was made of the life time prevalence of PTSD, alcohol abuse/dependence and cannabis use found in this study with prevalence in the general population reported in the ANWAMHS (Table 5).
Table 4: Comparison of lifetime prevalence of traumatic experiences
with Australian National Wellbeing and Mental Health Survey results28
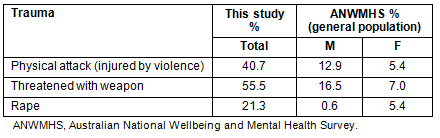
Table 5: Comparison of this study with Australian
National Wellbeing and Mental Health Survey results28
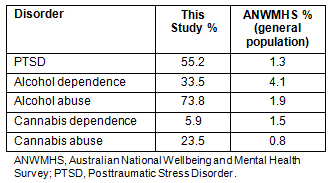
The rate of exposure to traumatic events found in this study was compared with the ANWMHS rate, and a higher rate of exposure to traumatic events was found in individuals in the communities studied here than the national average. Again, only selected and similar variables reported in both studies were compared because the rate of exposure and some types of traumatic events reported in this study were not reported in the ANWMHS.
Discussion
In a critical review of the findings of this study the following questions may be asked. What are the implications of these findings? Does clinical practice reflect the higher than national average PTSD rate found in this study? Can the findings of the present study be replicated elsewhere in a similar population? The study focused on a remote Aboriginal population, and explored the lived experience of the participants. The lived and shared experience of Aboriginal people is traumatic so the high rate of PTSD is not surprising. Because this experience is shared by all Aboriginal people across the nation, it is likely that the same instruments would produce similar results if used in a similar population. A number of previous studies using different instruments have also reported high rates of exposure to traumatic events, and a high rate of PTSD and alcohol misuse related disorders in the Aboriginal population2,3,35.
However, while this study found a high rate of exposure to traumatic events which has translated into a high rate of PTSD, this relationship is not reflected in clinical settings. Possible reasons include misinterpretation of PTSD symptoms. Core PTSD symptoms such as intrusion, avoidance and hypervigilance are also manifestations of other clinical conditions such as psychotic and depressive disorders. This both poses challenges and presents an opportunity to review current clinical approaches to Aboriginal mental health41. In the current clinical environment, it is widely reported that alcohol misuse related disorders, and depressive and psychotic disorders are common diagnoses given to Indigenous patients in clinical settings. However, there is no evidence of PTSD as a common diagnosis in spite of the well-documented collective and individual exposure of Aboriginal people to traumatic events2,41-43.
The fact that those who met DSM-IV diagnostic criteria for PTSD are a non-treatment-seeking population indicates that PTSD is an important public health concern. The higher rate of PTSD in this historically disadvantaged population justifiably suggests the argument offered by opponents to PTSD as a diagnosis, who link it to social and economic status and propose that the poor and disadvantaged shouldn't be diagnosed with PTSD19,20. However, the reality is that this population is not seeking treatment from professionals - instead they are self-medicating with alcohol and other substances. The majority of PTSD-positive participants (91% [n=111]) met alcohol related disorder criteria, which offers an explanation for the fact that they are not seeking professional assistance. The higher rate of exposure to traumatic events is consistent with findings of a Northern Territory study2; and a higher rate of PTSD is reported in another study41. The silence on Aboriginal PTSD in the clinical setting was demonstrated by a study that reported psychiatric disorders among Aboriginal Western Australians without reference to PTSD, either in its older or in current terms42. This silence on PTSD in the clinical environment requires further study to ascertain whether PTSD in Aboriginal patients is mistaken for other clinical conditions. The DSM-IV and ICD-10 diagnostic criteria present a narrow window to diagnose Aboriginal persons with PTSD, dismissing some of the key traumatic events experienced by Aboriginal people4,11,14,41.
Although PTSD is not at the centre of current mental health practice, alcohol misuse is attracting much attention in the clinical setting, at policy level and is also a major concern for Aboriginal people due to its immediate effects of violence, accidents, and neglect of children. This has resulted in a 'quick fix' approach with little effort to address the underlying issues such as the need for education, employment and housing; and the effects of financial hardship and social injustice. Without addressing these core issues any approach will achieve little or no significant outcome.
There is a well established understanding among Aboriginal people about why their people are misusing alcohol. Furthermore, there is a well established understanding about effects of trauma, including re-traumatisation and the complex problems associated with it41-43. While Aboriginal people are trying to make sense of and deal with the effects of alcohol on the community and especially on the future of younger generations, interventions appear to be generate by panic at the policy level and are, at best, aimed at producing short-term effects rather than long-term outcomes. In spite of the historical evidence of the negative impact of banning Aboriginal people from drinking alcohol, this currently appears to be a favoured approach of both policy-makers and some sectors of the Aboriginal communities. This is only an emergency solution.
In this study, 97.35 (n=215) of participants reported exposure to a traumatic event. A total of 55.2% (n=122) met the DSM-IV diagnostic criteria for PTSD. An overwhelming 96% (n=212) reported consuming alcohol, and of these 73.8 (n=163) met the diagnostic criteria for an alcohol related disorder. The interplay of exposure to traumatic events, resultant PTSD and alcohol misuse have severe consequences for the health and wellbeing of Aboriginal people. Compounded by socio-economic disadvantages, the consequences of exposure to traumatic events contribute to complex psychosocial health problems and physical comorbidity. They increase the vulnerability of Aboriginal people to overall poor health outcomes.
The current approach of specialised mental health services that focus on the treatment and rehabilitation of an individual rather than the family and community contradicts the Aboriginal philosophy and view of mental health. The fact that Aboriginal people see mental health as the social and emotional wellbeing of not only an individual but also family, community and environment explains the philosophical differences. The current provision of specialised mental health services to Aboriginal people is not utilised sufficiently because it generates stigma and also contradicts their fundamental belief system on health and wellbeing. It also fails to tackle the issue of transgenerational trauma; by so doing, it leads to a poor understanding of currently occurring traumatic events, which are the effects of transgenerational trauma. Such misunderstanding leads to misdirected interventions, focusing on the identification and treatment of symptoms without addressing causative factors. When trauma and its effects are continuously misunderstood and not acknowledged, the effect on individuals, family and community is magnified. If it is not dealt with appropriately, unacknowledged trauma can have a devastating impact on those who are directly affected and spread to the next and following generations. Put simply, what is being witnessed in Aboriginal communities in relation to mental health issues and concerns is due to the misunderstanding of the traumatic events that have been affecting generations of Aboriginal people. Clinical practice must consider and focus on PTSD as a central issue when clinicians assess Aboriginal patients.
Acknowledgement
The author acknowledges academic and research support provided by Professor Alexander McFalane and his team of researchers and academics of the Department of Psychiatry, the University of Adelaide. Without Professor McFarlane's support it would have been not possible to complete the study.
References
1. McFarlane AC, Raphael B. Trauma and its effects. In: S Bloch, BS Singh (Eds). Foundations of clinical psychiatry (2E). Melbourne , VIC: Melbourne University Press, 2001; 149-161.
2. Holmes C, McRae-Williams E. An investigation into the influx of Indigenous "visitors" to Darwin's Long Grass from remote NT communities - phase 2: being undesirable: law, health and life in Dariwin's long grass. Canberra, ACT: Commonwealth of Australia, 2008.
3. Havemann P. Denial, modernity and exclusion: Indigenous placelessness in Australia. Macquarie Law Journal 2005; 5: 57-79.
4. 4. O'Donoghue L. Aboriginal families and ATSIC. Family Matters 1993; 35: 14-15.
5. Sochting I, Corrado R, Cohen IM, Ley RG, Brasfield C. Traumatic Pasts in Canadian Aboriginal people: Further support for a complex trauma conceptualization? BC Medical Journal 2007; 49(6): 320-326.
6. McFarlane AC. Avoidance and intrusion in posttraumatic stress disorder. Journal of Nervous & Mental Disease 1992; 180(7): 439-445.
7. Clarke C, Harnett P, Atkinson J, Shochet. Enhancing resilience in indigenous people: the integration of individual, family and community intervention. Aboriginal and Islander Health Worker Journal 1999; 23(4): 6-10.
8. O'Shane P. The psychological Impact of White Settlement on Aboriginal People. Aboriginal and Islander Health Worker Journal 1995; 19(3): 24-29.
9. Franklin M, White I. The history and politics of Aboriginal Health. In: J Reid, P Trompf. Health of Aboriginal Australians. Sydney, NSW: Harcourt Brace Jovanovich, 1991; 1-35.
10. Broome R. Aboriginal Australians, black response to white dominance: 1788-1980. Sydney, NSW: Allen & Unwin, 1982.
11. Peters L. The years that never were. Aboriginal and Islander Health Workers Journal 1995; 19(3): 16-19.
12. Crime Research Centre. Rural crime and safety in Western Australia. Perth, WA: The University of Western Australia, 1997.
13. Crime Research Centre. Mapping crime, offenders and socio-demographic factors. Perth, WA: The University of Western Australia, 1999.
14. Reynolds H. Aboriginal sovereignty: reflections on race, state and nation. Sydney, NSW: Allen Unwin, 1996.
15. Cripps K. Indigenous family violence pathways forward. In: N Puradie, P Dudgeon, R Walker. Working together: Aboriginal and Torres Strait Islander Mental Health and Wellbeing Principles and Practice. Canberra, ACT: Commonwealth of Australia, 2010; 145-154.
16. Parker R. Australian Aboriginal and Torres Strait Islander mental health: an overview. In: N Purdie, P Dudgeon, R Walker, Working Together: Aboriginal and Torres Strait Islander Mental Health and Wellbeing Principles and Practice. Canberra, ACT: Commonwealth of Australia, 2010; 3-11.
17. World Health Organization. Classification of Mental and Behavioural Disorders, (ICD-10): with glossary and Diagnostic Criteria for Research, 10th edn. Washington DC: American Psychiatric Press, 1994.
18. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorder (DSM-IV-TR), 5th edn. Washington, DC: American Psychiatric Association, 2000.
19. Summerfield D. The invention of post-traumatic stress disorder and the social usefulness of a psychiatric category. BMJ 2001; 322: 95-98.
20. Dillon A. Posttraumatic stress strength. Aboriginal and Islander Health Worker Journal 2009; 33(1): 22-25.
21. Van der Kolk BA, McFarlane AA. The black hole of trauma. In: BA van der Kolk, AC McFarlane, L Weisaeth; Traumatic stress: the effects of overwhelming experience on mind, body, and society. New York: Guilford Press, 1996; 3-23.
22. Creamer M, O'Donnell M. Post-traumatic stress disorder. Current Opinion in Psychiatry 2002; 15: 163-168.
23. Yehuda R. Current concepts: post-traumatic stress disorder. New England Journal of Medicine 2002; 346(2): 108-114.
24. Orcutt HK, Erickson DJ, Wolfe J. A prospective analysis of traumatic exposure: the mediating role of PTSD symptomatology. Journal of Traumatic Stress 2002; 15(3): 259-266.
25. Hill J. Childhood trauma and depression. Current Opinion in Psychiatry 2003; 16: 3-6.
26. Kessler RC, Sonnega A, Bromet E, Hughes M, Nelson CB, Breslau N. Epidemiologic risk factors for trauma and PTSD. In: R Yehuda (Ed.), Physiological trauma. Washington DC: American Psychiatric Press, 1999.
27. Creamer M, Burgess P, McFarlane AC. Posttraumatic stress disorder: findings from the Australian National Survey of Mental Well-being. Psychological Medicine 2001; 31: 1237-1247.
28. Australian Bureau of Statistics. Mental Health and Wellbeing of Adults. Canberra, ACT: ABS, 2000.
29. Begic D, Jokic-Begic N. Violence, behaviour and post-traumatic disorder. Current Opinion in Psychiatry 2002; 15: 623-626.
30. Begic D, Jokic-Begic N. Aggressive behaviour in combat veterans with post-traumatic stress disorders. Military Medicine 2001; 166: 671-676.
31. Maes M. Risk and preventative factors of Post-traumatic stress disorder and its co-morbid disorders. Current Opinion in Psychiatry 2000; 13: 587-589.
32. Ford JD, Kidd P. Early childhood trauma and disorders of extreme stress as predictors of treatment outcome with chronic posttraumatic stress disorder. Journal of Traumatic Stress 1998; 11(4): 743-761.
33. Australian Bureau of Statistics. Mental health and wellbeing, Australia. Canberra, ACT: AGPS, 2002.
34. Hunter E. Considering trauma in an indigenous context. Aboriginal and Islander Health Worker Journal 1998; 22(5): 10-18.
35. Mattingley C, Hampton K. Survival in our own land. Aboriginal experiences in South Australia since 1836. Melbourne, VIC: Australian Scholarly Publishing, 1998.
36. Peters L, Andrews G, Cottler LB, Chatterji S, Janca A, Smeets R. Composite International Diagnostic Interview Posttraumatic Stress Disorder Module: preliminary data. International Journal of Methods in Psychiatric Research 1996; 6: 167-174.
37. World Health Organization. Composite International Diagnostic Interview (CIDI). Core Version 2.1. Geneva, WHO, 1997.
38. Keane TM, Kaloupek DG, Weathers FW. Ethnocultural Considerations in the assessment of PTSD. In: AJ Marsella, MJ Friedman, ET Gerrity, RM Scurfield (Eds). Ethnocultural aspects of posttraumatic stress disorder: issues, research, and clinical applications. Washington, DC: APA, 1996, 183-205.
39. Green BL. Cross-national and ethnocultural issues in disaster research. In: AJ Marsella, MJ Friedman, ET Gerrity, RM Scurfield; Ethnocultural aspects of posttraumatic stress disorder: issues, research, and clinical applications. Washington, DC: APA, 1996, 341-361.
40. Bush K, Kivlahan DR, McDonell MB, Fihn SD, Bradley KA. The AUDIT alcohol consumption questions (AUDIT-C). Archives of Internal Medicine 1998; 58: 1789-1795.
41. Atkinson J, Nelson J, Atkinson C. Trauma, transgenerational transfer and effects on community wellbeing. In: N Purdie, P Dudgeon, R Walker; Working Together: Aboriginal and Torres Strait Islander Mental Health and Wellbeing Principles and Practice. Canberra, ACT: Commonwealth of Australia, 2010; 135-144
42. Atkinson J. Making sense of the senseless: feeling bad, being mad, getting charged up. In: M Tehan, D Chong (Eds); Proceedings, Having it Both Ways: dual diagnosis, alcohol, drugs and mental illness national conference, 1998. Melbourne, VIC: Jesuit Social Services, 1998.
43. Atkinson J, Ober C. We al-ali 'fire and water': a process of healing. In K Hazelhurst (Ed.); Popular justice and community regeneration: pathways of indigenous reform. Westport, CT: Praeger, 1995; 201-218.
