The prevalence of childhood overweight and obesity in the Canadian population has increased remarkably compared with the child populations of other countries1. In Canada, the rate of increase in obesity has been greater in children than in adults2, and in rural youth populations compared with urban3. While evidence clearly suggests that overweight and obesity is a growing concern for all Canadians, it may be an even greater concern for youth and for those living in rural areas.
Changes in patterns of behaviors, such as physical activity, sedentary behavior, and dietary practices have been found to contribute to the rise in childhood obesity4. Recent national studies have reported that 26% of Canadian children (2-17 years) are classified as overweight5 and many Canadian children are not meeting the national guidelines for physical activity6, are engaged in too much 'screen time'6 (eg watching television, using a computer for games or other activities), and are not eating the recommended servings of dairy, fruit, or vegetables7. There are limited data on the health behaviors of children aged 8 to 13 years living in Saskatchewan, particularly those children living in rural settings. Of the 10 Canadian provinces, Saskatchewan ranks fifth for prevalence of childhood obesity, with 29% of children (aged 2-17 years) classified as overweight5. A similar proportion (28.8%) of children and youth (2-17 years) living in rural Saskatchewan have been classified as overweight or obese8. Studies examining the physical activity patterns of children (aged 8-13 years) living in rural Saskatchewan have reported that many children (46.3%) were not physically active enough for health benefits9, and that these children are less aerobically fit than children living in urban settings in the province10. A study conducted with Saskatchewan rural adolescent youth in grades 7-12 reported that most youth watched between one and 2 hours of television daily, consumed less than the recommended amounts of fruit and vegetables, and few were active for a minimum of one hour every day11. As young children are in the process of developing health behaviors and beliefs about health, health promotion efforts that focus on this age group may be effective in influencing health behaviors that could continue into adolescence and beyond. To guide and tailor interventions and health promotion strategies, further research is needed into the health characteristics of young children living in rural areas, and on associated factors that may influence their patterns of behavior. The purpose of this study was to explore the health behaviors and weight status of a group of rural children aged 8-13 years living in central Saskatchewan.
Quantitative methods (ie health questionnaire, anthropometric measures) were used to examine weight status and health behaviors of a group of pre-adolescent children living in rural Saskatchewan. This article reports the weight status, physical activity, sedentary behaviors, dietary patterns, and perception of health of the boys and girls who participated in the study.
The study was approved by the University of Saskatchewan's Behavioral Research and Ethics Board and by the Director of Education and principal of the participating school. Both parental consent and child assent were obtained for completing the questionnaire and measuring height and weight.
The study was conducted in an agriculturally based rural town (pop. 1743) in a western Canadian prairie province located approximately 100 km from the nearest urban center. All children in grades 1-7 (n = 194) were invited to participate in the study and were recruited through short classroom presentations conducted by a researcher. Of the 194 questionnaires distributed through the classrooms, 99 were returned completed for a response rate of 51%. There were no significant differences in gender between respondents and non respondents.
A cross-sectional health questionnaire based on portions of the Health Behavior in School Aged Children (HBSC) Survey (1997-1998)12 was used to gather information on children's physical activity, sedentary behaviors, dietary patterns, and perceptions of health status. In particular, sedentary behaviors were measured by self-reported hours of screen time, and time spent commuting by car or bus to school or other activities. Children's physical activity patterns were assessed by self-reported frequency of their participation in organized (eg volleyball, football, soccer, swimming), unorganized (eg biking, spontaneous sports games, rollerblading), or class like activities (eg gymnastics, karate, dance). Perception of health status was measured by self-report of how healthy children thought they were (very healthy, quite healthy, not very healthy).
The HBSC questionnaire was developed by an international research network of multidisciplinary experts and used to gather information on health and health behaviors of youth aged 11-15 years12. Reliability and validity of the dietary and activity portions of the HBSC survey have been established by previous studies13,14. Additional questions relating to the rural environment were specifically developed for the present study and added to the end of the HBSC survey. A pilot test of the entire questionnaire took place prior to the commencement of the study. Students completed the questionnaire at home with their parent or guardian and returned it in a sealed envelope to a designated container in their classroom.
Height and weight measurements of each child were collected by the researcher. Measurements followed the procedures suggested by Cole & Rolland-Cachera15. The children were asked to remove shoes or any heavy clothing such as a jacket or sweater. Height was measured twice to the nearest 0.1 cm using a standardized stadiometer (Health o meter Professional model 500KL; www.homescales.com). Weight was measured twice to the nearest 0.1 kg using a digital scale (Taylor electronic scale #7335EF; Toronto, Canada; www.taylor.ca). The measurements of height and weight were averaged and recorded to the nearest 0.1 cm or kg. The final height and weight measurements were used to calculate BMI (kg/m2) for each child. Using the international standards for calculating childhood obesity16, children were classified by their BMI as a healthy weight or an unhealthy weight (overweight or obese). Obesity and overweight were defined for the study based on the child's age and sex-specific BMI cut off for obesity and overweight, respectively, according to international standards established by Cole et al16.
All data from the questionnaire was cleaned (obviously erroneous values checked and deleted), entered, and analyzed using SPSS v16.0 (www.spss.com.au). Categorical variables (eg age, gender, grade) were analyzed descriptively using frequency distributions and percentages. The χ2 test was used to examine distributions of variables across grade level, and between boys and girls and town and farm residents. Statistical significance was indicated by p ≤ 0.05.
In this sample, 34% of children were categorized as either overweight (23.7%) or obese (10.3%) (Table 1). Overall, 42.9% of boys were overweight (28.7%) or obese (14.3%) and 25% of the girls were overweight (18.8%) or obese (6.2%).
A significantly higher proportion of boys aged 6-8 years were categorized as having an unhealthy weight compared with girls of the same age (χ2 [1, N = 34] = 6.2, p = 0.046). There was a tendency for the proportion of children with an unhealthy weight to increase by age (Fig1). Interestingly, regardless of weight status, the majority of children (99.9%) reported that they were 'quite healthy' or 'very healthy'.
Table 1: Health characteristics of the children by gender
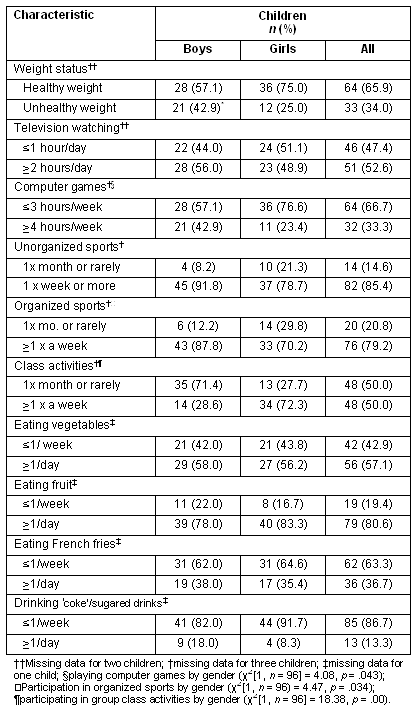
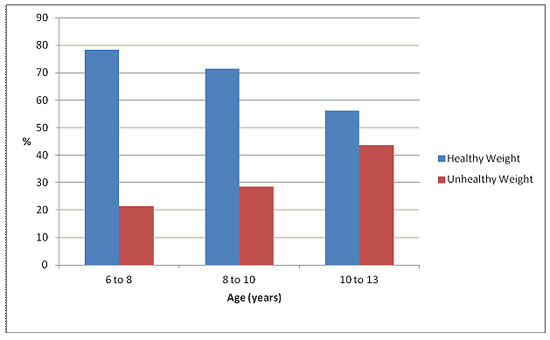
Figure 1: Proportion of healthy weight and unhealthy weight children by age
Compared with the girls, a significantly higher proportion of boys reported playing computer games for 4 hours or more a week (Table 1). Many children (52.6%) reported watching television for 2 hours or more a day. A significantly higher proportion of children living in town compared with children living on a farm or acreage reported watching two hours or more of television a day (χ2 [1, N = 97] = 5.28, p = .021). There were no significant differences between place of residence and time spent using a computer for games or other activities.
Twenty-five percent (n = 27) of the children commuted to school daily by school bus and reported a minimum mean time of 29.5 min (SD = 16.2) traveling one way to or from school. Additionally, 40% of the children reported spending a relatively short time being driven to school (M = 4.2 min, SD = 3.9) or from school most days of the week. The majority of children (70%) reported being driven to other activities (eg sports, clubs, visit friends), spending a minimum mean time of 23.8 min (SD = 34.8) traveling one way to or from activities on a weekly basis.
A significantly greater proportion of boys participated in organized sports while a significantly greater proportion of girls participated in non-competitive class activities, such as gymnastics, dance, or karate (Table 1). Although not statistically significant, there appeared to be a trend for a higher prevalence of boys participating in unorganized sports compared with girls. There were no significant differences between participation in organized, unorganized or class-like activities and living in a town or on a farm. While there were no significant differences in dietary patterns between boys and girls, 80.6% of children reported eating fruit one or more times a day and 57.1% reported eating vegetables one or more times a day. Most children (86.7%) drank 'coke' or sugared drinks only once a week or less while 63.3% reported eating French fries once a week or less (Table 1).
Discussion
Study results show that 34% of all children responding to the survey were either overweight (23.7%) or obese (10.3%). While direct comparisons with other studies are difficult due to differences in methodologies and populations, these findings are a slightly higher than a regional study of 504 children conducted in rural Ontario, Canada where 28.6% of children were classified as overweight (17.7%) or obese (10.9%)17. The Canadian Community Health Survey reported 26% of children aged 6-11 years living in rural Saskatchewan as overweight (18%) or obese (8%)8, lower than what was found by the current study. A study conducted in the USA with 3416 rural and urban children aged 8-12 years reported that 46.9% of rural children were at risk for overweight (21.8%) or were overweight (25.1%)18, with the terms 'at risk for overweight' and 'overweight' corresponding to the Canadian terms of overweight and obese, respectively19.
This study found a significantly higher prevalence of overweight and obesity in boys aged 6-8 years compared with girls of the same age, supporting the findings from a study conducted in rural Ontario where a significantly greater prevalence of obesity (but not overweight) was found in boys (15%) aged 7 and 10 years of age compared with similar aged girls (6.8%)17. Inconsistent with these, are studies of rural children living in the USA18 and of urban children living in Canada20 that report no significant gender differences in the prevalence of overweight and obesity. Further research is needed to more clearly distinguish if gender differences exist in the prevalence of overweight or obesity in rural children. Should gender differences be found to exist, further exploration of potential reasons for differences may provide valuable information for the development of early health promotion programs tailored specifically to gender.
National recommendations suggest that children and youth spend 2 hours a day or less watching television21. Only 47.4% of children in the present study met this recommended guideline. This finding is similar to other studies of Canadian children that have reported 44% of children in grades 6-1222 and 36% and 33% of 11 year-old boys and girls, respectively, reported meeting the recommended guideline for television watching23. A study of 954 rural high school students (grades 7-12) reported that 53.7% of youth watched between one and 2 hours of television on an average school day11.
Interestingly, in this research, place of residence (ie living in town) was significantly associated with more hours of television watching. There are limited data that examine and compare the patterns of behaviors between farm and non-farm rural residents, particularly in children. One study that compared cardiovascular risk factors between farm and non-farm rural women reported a higher prevalence of smoking in non-farm rural residents but a higher prevalence of obesity and hypertension in farm residents24. Similarly this research suggests that differences in behaviors may exist between farm and non-farm rural residents. Further exploration of these factors may reveal variations in these populations that require specific approaches to health promotion and intervention strategies.
Children in this study were involved in inactive modes of transportation (eg transported by vehicle to and from activities). Many children reported being driven to school (40%), to activities (70%) and/or riding a school bus (25%) on a regular basis. The use of inactive transportation in this rural setting results in children potentially accumulating several additional hours a week (ie approximately 60 min/day to and from school and/or 60 min/week to and from extracurricular activities) of sedentary behavior. There are few studies that explore the amount of time rural children spend commuting; however, these findings are similar to those found in children in grades 6-12 living in New Brunswick where 77% of children reported using inactive modes of transportation (eg getting a ride or taking a bus)22. Even though some commuting (ie busing to school) cannot be avoided in rural settings, decreasing unnecessary commuting (when safe to do so) may provide additional opportunities for rural children to be active, thereby counteracting the necessary commuting in this setting.
The consumption of sugared drinks has been associated with displacing nutrients25 and the development of overweight and obesity in children26. The daily intake of sugared drinks in this study (18% for boys and 8.3% for girls) is similar to those found in a Canadian study that reported 14% of boys and 10% of girls drank sugared drinks on a daily basis23. A study conducted with rural children living in the USA reported that 32.3% of school age children consumed 180 mL (9 ounces) or more of soft drinks every day27. The finding in the present study suggest that rural children have reasonable access to sugared drinks; thus, a reduction in soft drink consumption would be a worthy focus of health promotion efforts for rural child populations.
Regardless of weight status almost all children (99.9%) reported they were 'quite healthy' or 'very healthy'. This finding is in contrast to a previous study that reported a decrease in children's quality of life (ie physical, emotional, social, and school functioning) with increasing BMI28. For this sample of children, one explanation may be that health was associated with happiness rather than physical functioning and body shape. Therefore, the children may have believed that if they were happy then they were healthy.
Limitations
The response rate and data collection methods contributed to the limitations of this research. Although several strategies were used to improve participation, the low response rate (51%) limits generalizability beyond the study sample. The health questionnaire was based on the HBSC questionnaire which was designed for adolescents. To address this limitation, children were asked to take the questionnaire home and complete it with a parent or guardian, thus decreasing the possibility of children's potential lack of understanding of the questions. To limit the influence of the validity of the HBSC tool, questions related to the rural environment were added to the end of the validated tool.
This study responded to the recommendation of Tremblay29 for the need of more studies using directly measured heights and weight for the assessment of overweight and obesity. Although a contribution of this study was the directly measured heights and weights, a limitation remained in the self-report of the health behaviors. Potential inaccuracies have been reported in proxy and self-report data, suggesting that even though these methods provide some benefits (eg ease of collection), relying exclusively on these methods is not recommended30,31. In this study, obtaining objective measures of physical activity, sedentary activity, commuting times, and dietary recalls would add to the accuracy of data and thus our overall understanding of these behaviors.
The findings of this study suggest that the health of pre-adolescent children living in rural Saskatchewan is being influenced by physical inactivity and a high prevalence of overweight and obesity. Additionally, boys may be at higher risk for overweight and obesity than girls, and this risk may begin at a very young age. Differences may also exist in the preferences of activities between boys and girls and between the behaviors of children living in town and farm settings. An interesting finding and one that requires further exploration is that children's perceptions of their health status were not influenced by their weight or health behaviors.
This study has provided additional information about the health of children aged 8-13 years living in rural Saskatchewan and has confirmed the urgent need for health promotion efforts specifically tailored to this population.
Acknowledgement
This research was supported in part by CIHR Strategic Training Program in Public Health and the Agricultural Rural Health Ecosystem (PHARE). The authors especially thank the school officials of the participating school and, specifically, the rural children and parents whose knowledge and participation was most valuable.
References
1. Janssen I, Katzmarzyk PT, Boyce WF, Vereecken C, Mulvihill C, Roberts C et al. Comparison of overweight and obesity prevalence in school-aged youth from 34 countries and their relationships with physical activity and dietary patterns. Obesity Reviews 2005; 6(2): 123-132.
2. Tremblay MS, Katzmarzyk PT, Willms JD. Temporal trends in overweight and obesity in Canada, 1981-1996. International Journal of Obesity Related Metabolic Disorders 2002; 26(4): 538-543.
3. Brunner M, Lawson J, Pickett W, Boyce W, Janssen I. Rural Canadian adolescents are more likely to be obese compared with urban adolescents. International Journal of Pediatric Obesity 2008; 3(4): 205-211.
4. Anderson P, Butcher K. Childhood obesity: trends and potential causes. The Future of children 2006; 16(1): 19-45.
5. Statistics Canada. Nutrition: findings from the Canadian community health survey. Measured obesity: overweight Canadian children and adolescents. Report 82-620-MWE. Ottawa: Statistics Canada; 2005.
6. Active Healthy Kids Canada. The Active Healthy Kids Canada report card on physical activity for children and youth. (Online) 2010. Available: www.activehealthykids.ca (Accessed 2 August 2011).
7. Garriguet D. Nutrition: Findings from the Canadian community health survey. Overview of Canadian's eating habits. Report 82-620-XIE. Ottawa: Statistics Canada. 2006.
8. Shields M, Tjepkema M. Regional differences in obesity. Report 82-003. Ottawa: Statistics Canada; 2006.
9. Bilinski H, Semchuk K, Chad K. Understanding physical activity patterns of rural Canadian children . Online Journal of Rural Nursing and Health Care 2005; 5(2): 73-82.
10. Tremblay MS. Conquering childhood inactivity: is the answer in the past? Medicine and Science in Sports and Exercise 2005; 37(7): 1187-1194.
11. Martz D, Wagner A. Saskatchewan rural youth healthy lifestyles and risk behavior project fact sheet. Report: Health Canada DSCIF Study # 6558-08-2005/3480566. Saskatoon, SK: University of Saskatchewan, 2008.
12. HBSC. Health behaviors in school-aged children homepage. (Online) 2009. Available: http://www.hbsc.org/index.html (Accessed 25 January 2009).
13. Booth M, Oakely A, Bauman A. The reliability and validity of the physical activity questions in the WHO health behavior in schoolchildren (HBSC) survey: a population study. British Journal of Sports Medicine 2001; 35(4): 263-267.
14. Vereecken C, Maes L. A Belgian study on the reliability and relative validity of the health behavior in school-aged children food-frequency questionnaire. Public Health Nutrition 2003; 6(6): 581-588.
15. Cole T, Rolland-Cachera F. Measurement and definition. In: W Burniat, T Cole, I Lissau, E Poskitt (Eds). Childhood and adolescent obesity: causes, consequences, and prevention. New York: Cambridge University Press, 2002; 3-22.
16. Cole TJ . Establishing a standard definition for child overweight and obesity worldwide: international survey. BMJ 2000; 320(7244): 1-6.
17. Galloway T . Obesity rates among rural Ontario schoolchildren. Canadian Journal of Public Health 2006; 97(5): 353-356.
18. Joens-Matre R, Welk G, Calabro M, Russell D, Nicklay E, Hensley L. Rural-urban differences in physical activity, physical fitness, and overweight prevalence of children . Journal of Rural Health 2008; 24(1): 49-54.
19. Plotnikoff RC . Physical activity, smoking, and obesity among Canadian school youth. Comparison between urban and rural schools. Canadian Journal of Public Health 2004; 95(6): 413-418.
20. Haque F, Rocha A, Horbul B, Desroches P, Orrell C. The prevalence of childhood obesity. Canadian Journal of Dietetic Practice and Research 2006; 67(3): 143-147.
21. American Academy of Pediatrics. children , adolescents, and television. Pediatrics 2001; 107(2): 423-426.
22. The New Brunswick student wellness survey. Homepage. (Online) 2009. Available: http://www.unbf.ca/education/herg/wellness/elementary-wellness-project.php (Accessed 25 January 2009).
23. WHO. Inequalities in young people's health: HBSC international report from the 2005/2006 survey. Report: Health Policy for children and Adolescents 5. Edinburgh: Child and Adolescent Health Research Unit, 2008.
24. McCarty C, Chyou PH, Ziegelbauer L, Kempf D, McCarty D, Gunderson P et al. A comparison of cardiovascular disease risk factors in farm and non-farm residents: The Wisconsin Rural Women's Health Study. Wisconsin Medical Journal 2002; 101(7): 34-39.
25. Mrdjenovic G, Levitsky DA. Nutritional and energetic consequences of sweetened drink consumption in 6- to 13-year-old children. Journal of Pediatrics 2003; 142(6): 604-610.
26. Ludwig DS, Peterson KE, Gortmaker SL. Relation between consumption of sugar-sweetened drinks and childhood obesity: a prospective, observational analysis. Lancet 2001; 357(9255): 505-508.
27. Harnack L, Stang J, Story M. Soft drink consumption among US children and adolescents: nutritional consequences. Journal of the American Dietetic Association 1999; 99(4): 436-441.
28. Williams J, Wake M, Hesketh K, Maher E. Health-related qualtiy of life of overweight and obese children . JAMA 2005; 293(1): 70-76.
29. Tremblay M. The need for directly measured health data in Canada. Canadian Journal of Public Health 2004; 95(3): 165-168.
30. Elgar FJ, Stewart JM. Validity of self-report screening for overweight and obesity. Evidence from the Canadian community health survey. Canadian Journal of Public Health 2008; 99(5): 423-427.
31. Shields M. Proxy reporting in the national population health survey. Report 82-003. Ontario: Statistics Canada, 2000.


