Measles is a highly contagious and vaccine preventable respiratory paramyxovirus infection, and a major cause of child morbidity and mortality. The incubation period is 10-12 days from exposure to the virus to the onset of fever, and a rash usually appears at around day 14 (range 7-18 days). Patients are contagious from about 4 days before eruption of the rash until 4 days after the eruption1. The severity of measles varies widely, depending on a number of host and environmental factors. The risk of developing severe or fatal measles increases for those aged less than 5 years, living in overcrowded conditions, who are malnourished (especially with vitamin A deficiency); and those with immunological disorders, such as advanced HIV infection.
In developing countries, case-fatality rates among young children may reach 5-10%. The complications of infection, including, severe diarrhoea, protein-energy malnutrition, respiratory infection and encephalitis, are often the ultimate causes of mortality in developing countries1. Worldwide, the number of reported measles cases declined 67%, from 852 937 in 2000 to 278 358 in 2008, and reported measles mortality declined from 733 000 deaths in 2000 to 164 000 in 20082. Improvements in measles control is reflected in a remarkable drop in the number of measles cases reported globally, from 278 358 in 2008 to 222 408 by the end of 2009. However, the dissonance between the estimated case-fatality rate of 5-10%, and the apparent case-fatality rate of over 60% between 2000 and 2008 suggests under-reporting of clinical measles cases, because mortality reports are relatively more reliable.
Measles vaccination coverage is used as an indicator of progress towards the Millennium Development Goal 4 of reducing infant mortality, because the infection contributes significantly to increased child morbidity and mortality, and because vaccination coverage provides an indication of the level of access to child health services. Measles vaccination provides a safe, efficacious and cost-effective method for disease prevention, and is credited with preventing over 2 million infant deaths per year, accounting for a 78% decrease in measles-related deaths between 2000 and 20083. Effective measles vaccination programs may also help to ease resource constraints in healthcare systems by preventing infection and, therefore, the number of cases presenting to hospitals for medical care4.
Indonesia is the fourth most populous nation in the world with an estimated 228 million population in 2008. Approximately 52% of the population resides in urban areas. Despite steady economic growth over the last three decades, Indonesia's measles vaccination coverage is lower than that of other South-East Asian nations. Estimates from Indonesia's Demographic and Health Survey 20075 (IDHS) show that measles vaccination coverage for Indonesian children aged below 6 years was 72.8% (based on mother's report or health card records), compared with 84% in the South-East Asian region in the same year4. In 2007, approximately 0.9 million eligible Indonesian children were not vaccinated against measles, and 19 456 measles cases were reported among Indonesian children, the second highest caseload in the South-East Asian region after India. Indonesia's measles incidence of 6.73 cases per 100 000 people is the third highest in South-East Asia6.
The primary aims of this study were to: (i) use the nationally representative IDHS dataset to determine if rural residence is a significant determinant of measles vaccination uptake in Indonesia; and (ii) explore other factors presumed to influence the likelihood of children in rural and urban areas receiving the first dose of measles vaccination.
Data
The IDHS is a cross-sectional survey administered by Statistics Indonesia, with financial assistance from the Government of Indonesia, the United Nations Population Fund, the Ford Foundation and UNICEF. Datasets are produced by Macro International for the Measure DHS (Demographic and Health Surveys) Project, which is funded by the US Agency for International Development. Measure DHS permitted download and use of the 2007 IDHS datasets for this study.
The household questionnaire was completed by 40 701 out of 42 341 sampled households (99% response rate)5. The objectives of the DHS include measurement of child health indictors such as vaccination coverage and nutritional status, assessing coverage of maternity services and investigating the direct and indirect factors that influence maternal and child health. The DHS is considered a reliable benchmark for comparison of vaccination data. Investigations of the quality of DHS methodologies concluded that it is nationally representative and relatively free of systematic bias7. Information about living children aged between 0 and 59 months was collected through the 'married women's questionnaire' and separated into a children's dataset by DHS.
Variables
The dependent variable of interest was the likelihood of measles vaccination among children under 5 years of age. The question on measles vaccination was asked of every mother with a child aged under 5 years. The IDHS provided five response options: 'yes (marked on vaccination card)', 'yes (date recorded on vaccination card)', 'yes (mother's recall)', 'no' and 'don't know'. Because only 21% of the sample had their vaccination history recorded on a vaccination card, measles vaccination was re-coded into a dichotomous (no/yes) variable, with vaccinated children recorded as 'yes' regardless of the source of the information. Children whose mother indicated that they did not know whether measles vaccination had been given (1.33%) were classified as not having received the vaccination because it was likely to reflect that the child was not vaccinated and fits better with the 'no' response. In addition, the small size of the 'don't know' sample indicates that there is little likelihood of a bias in combining this group with the 'no' responses. All other vaccinations from the Indonesian childhood vaccination schedule that were considered in this study (Bacillus Calmette-Guérin vaccine [BCG], Diphtheria Tetanus and Pertussis vaccine [DTP], polio and hepatitis B) were also measured using dichotomous (no/yes) variables.
Type of residence was defined as either urban (reference category) or rural location. There is no universally accepted definition of rurality8. In the IDHS, 'urban areas' refer to large cities (capital cities and cities with populations greater than one million), smaller cities (more than 50 000 people) and towns. All 'countryside' areas are considered rural9. The region of residence variable indicates in which of the 33 Indonesian provinces the respondent resided at the time of the survey.
Household economic status is defined using the DHS wealth index quintiles, ranging from poorest (reference category) to richest. The wealth index is calculated by ORC Macro and is produced by combining as many indictors of household assets and utilities as possible. Indicators are any variable that may reflect the household's economic status, including, but not limited to, type of flooring, water supply, television, persons sleeping per room and ownership of agricultural land. Indicator variables are then weighted and an index is produced. The index is divided into quintiles (poorest, poorer, middle, richer, richest) based on the household population, and each member of a household receives the household's quintile category. The DHS wealth index is considered more stable, reliable and accurate compared with traditional measures of economic status, such as household income and expenditure, which are difficult to collect in developing countries10.
To investigate the relative importance of household wealth in urban and rural areas, the measles vaccination coverage rates for poor and wealthy children were compared in rural and urban areas of Papua, South Kalimantan, East Java and West Sumatera provinces. Papua, South Kalimantan and West Sumatera were selected because they have been identified since 2006 as priority areas for improving measles vaccination by the Indonesian Ministry of Health. East Java was chosen because this province has above average measles vaccination coverage.
Maternal education was included in the analysis because this is a well-established determinant of vaccination coverage11. The influence of maternal education on vaccination uptake was measured using categorical variables indicating the highest level of schooling attained by the child's mother (ie no education [reference category], primary, secondary or higher education). Paternal education level was defined using the same 5 categories.
The presence of a skilled birth attendant during delivery was used as a proxy for the availability of skilled health workers in the community12. Skilled attendance at birth is considered an indicator of general access to health services and is closely linked to overall health system capacity13. Skilled attendants included doctors, nurses, midwives or village midwives. Women who indicated that they were not assisted by skilled attendants but who reported that they had received informal assistance (ie from a friend, family member, traditional birth attendant), 'other', 'no one' or 'don't know' were coded as 'no' for this variable. For the purposes of this article, a traditional birth attendant is defined as someone who has not received formal medical training12. The 10 women who indicated that they did not know whether a skilled attendant was present at the birth of the child were also coded as 'no', because it is unlikely that a skilled attendant was present and only a small number (0.07%) of cases was affected. The IDHS also contained data relating to the place of birth (eg at home, hospital or private clinic). The presence of a skilled birth attendant was selected over place of delivery, because many women may prefer to give birth at home and with the advent of skilled village midwives, home delivery does not necessarily mean that a skilled attendant was not present. The continuous variable 'total children ever born' from the DHS was used to investigate differences in average parity between urban and rural areas and among wealth quintiles.
Analysis
Contingency table analysis was used to investigate the urban-rural differences in the socio-demographic characteristics of the sample, including maternal age, child age, mean total children ever born per woman, sex of the child, measles vaccination coverage, access to skilled birth attendants, wealth and maternal and paternal education. For categorical variables, Pearson's χ2 tests were used to establish the significance of differences in socio-demographic and measles vaccination coverage across groups at the 5% level. Independent sample t-tests were used to assess significance of urban-rural differences in the continuous variables (maternal and child age, total children ever born) at the 5% level.
Bivariate analysis was used to further investigate the education and wealth the characteristics of women who did not give birth with the assistance of a skilled birth attendant. Pearson's χ2 tests were again used to establish the significance of differences between groups at the 5% level. Significant differences in mean children ever born among urban and rural residents and wealth quintiles were assessed using independent sample t-tests.
Bivariate analyses were used to investigate the pattern of vaccination coverage across urban and rural areas for measles and the 11 other vaccinations in the Indonesian childhood vaccination schedule. Regional differences in measles vaccination uptake across the 33 Indonesian provinces were also investigated using bivariate analysis. Significance testing was again conducted using Pearson's χ2 tests.
Contingency table analysis was used to compare the measles immunisation coverage rate for poor and rich children residing in rural and urban areas of Papua, South Kalimantan, East Java and West Sumatera provinces. Chi-square tests were again used to establish the significance of differences in measles vaccination coverage for poor and rich groups in each area at the 5% level. For this analysis respondents were classified as 'poor' if they were in the poorest or poorer DHS wealth quintiles and 'rich' if they were in the middle, richer or richest wealth quintiles.
Multivariate logistic regression analysis was used to investigate whether rural-urban differentials remained after controlling for sex of the child, maternal age, maternal age squared, maternal and paternal education, household wealth and the presence of a skilled birth attendant. Maternal age was measured as a continuous variable; all other variables were included as categorical variables. A binomial logistic regression model was developed with measles vaccination as the outcome variable. All independent variables were entered simultaneously into the model. The results are reported as odds ratios (OR) and the 95% confidence intervals (CI) for the odds ratios. All data analysis was conducted using PASW v17 (http://www-01.ibm.com/software/analytics/spss/).
The sample contained 15 065 living children aged 9-59 months. The socio-demographic characteristics of the sample are presented according to location of residence (Table 1). A greater proportion of the sample resided in rural areas (61.9%). Overall, 72.8% of children in the sample had received measles vaccination. The mean age of children was 33.9 months in urban and rural areas, and the number of males and females was similar.
Table 1: Cross tabulation of the relationship between location of residence and socio-demographic characteristics (N = 15 065 living children aged under 5 years)
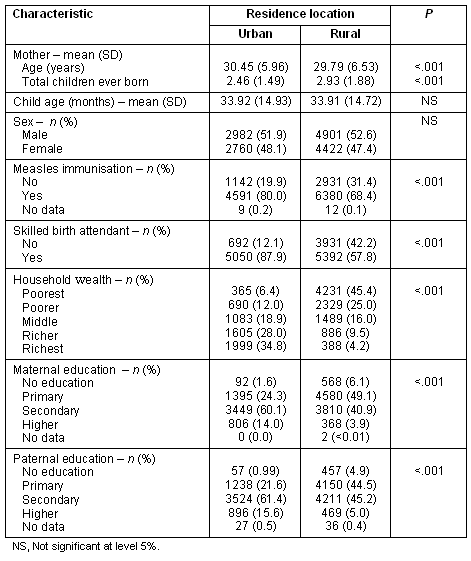
When socioeconomic status was analysed across urban and rural areas, 70% of rural residents fell into the poor or poorest wealth quintiles compared with 18% urban residents. A significantly higher proportion of rural mothers were in the poorest and poorer wealth quintile (p<0.05). The proportion of mothers in the middle, richer and richest wealth quintiles was significantly higher in urban areas (p<0.05).
The proportion of children delivered with the assistance of a skilled birth attendant was used as a proxy for rural-urban disparities in the availability of skilled health workers12. Rural-urban differentials in skilled birth attendants were significant under bivariate analysis, with skilled attendance at 57.8% of births in rural areas compared with 87.9% of births in urban areas (χ2 = 1514.915; p<0.001). Analysis of the 4623 women who gave birth without any skilled assistance, showed that they were also likely to have lower levels of education and wealth. Of those who were not assisted by a skilled attendant, 70.9% had primary or no education. In addition, 80.6% were in the poorest or poorer wealth quintiles.
The mean number of children ever born among women in the sample was 2.75 with a standard deviation (SD) of 1.758. The mean number of children ever born per woman was significantly higher in rural areas and for poorer wealth quintiles. The mean total children ever born to rural mothers was 2.93 (SD = 1.881) compared with 2.46 (SD = 1.492) for urban women (t = -16.755; p<0.001). The mean number of children per woman for the poorest and poorer wealth quintiles combined was 3.05 (SD = 1.946). This was significantly higher (t = 21.275; p<0.001) than the mean number of children for the middle, richer and richest quintiles combined, which was 2.45 (SD = 1.481).
Bivariate analysis revealed that measles vaccination coverage was significantly higher (p<0.001) among urban children (80.1%) compared with rural children (68.5%). As is shown, the rural-urban differential was not unique to the measles vaccination (Table 2). Vaccination coverage was significantly higher (p<0.001) among urban children for all 12 vaccinations listed in the Indonesian vaccination schedule.
Table 2: Vaccination coverage among rural and urban children for 12 vaccinations listed on the Indonesian vaccination schedule
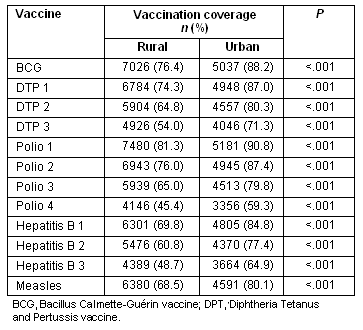
Investigation of rural-urban differences in vaccination coverage by province (Table 3) shows that measles vaccination coverage is significantly higher in urban areas for 16 of the 33 Indonesian provinces. The eastern provinces of Indonesia, such as Maluku and Papua, showed the greatest rural-urban differentials. These are predominantly rural regions with high poverty levels14. In Papua, where the rural-urban differential is greatest, coverage was 47.3% among rural children and 81.0% among urban children.
Table 3: Measles vaccination coverage among rural and urban children in each of the 33 Indonesian provinces
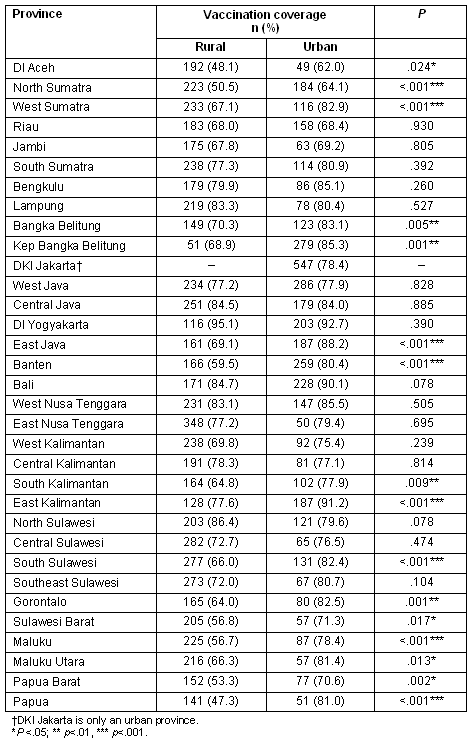
To further examine the influence of economic status, measles vaccination coverage among the poorest 2 wealth quintiles and the richest 3 quintiles was examined in urban and rural areas of Papua, South Kalimantan, East Java and West Sumatera. The results show that for all 4 provinces, measles vaccination coverage was not significantly different between the poorest 2 wealth quintiles and wealthiest 3 quintiles in urban areas (Table 4). In rural areas, measles vaccination coverage was significantly higher among the wealthier group. This was most significant in Papua and East Java (p<0.001), followed by South Kalimantan (p = 0.003) and West Sumatera (p≤0.03).
Table 4: Measles vaccination coverage according to economic status for rural and urban children in 4 Indonesian provinces
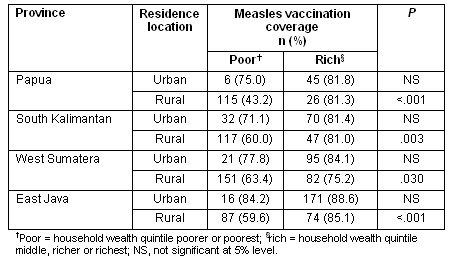
Multivariate logistic regression analysis was performed to assess the independent effect of rural-urban residence on measles vaccination coverage, while controlling for sex of the child, maternal age, maternal age squared, maternal and paternal education, household wealth and the presence of a skilled birth attendant.
The odds of measles immunisation were not significantly different for male and female children (Table 5). Maternal age was positively correlated with measles vaccination. Maternal age squared was also found to be significant, suggesting that the relationship between maternal age and measles vaccination is curved. Further analyses showed that the percentage of children immunised increased as maternal age group increased up to the 30-34 year age group and then decreased for the combined and rural samples. For the urban sample, the proportion of children immunised increased with each successive maternal age group up to 35-39 years and then began to decline.
Table 5: Logistic regression results for measles vaccination coverage after controlling for sex and residence location of the child, maternal age, maternal and paternal education, wealth and the presence of a skilled birth attendant
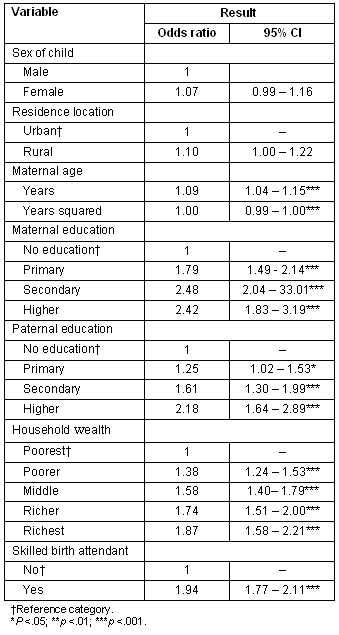
After controlling for all other variables, the rural-urban differential in measles vaccination coverage was marginally significant (OR = 1.10, 95% CI [1.00-1.10]).The main variables found to adversely influence rural-urban variations in measles vaccination in Indonesia were low maternal and paternal education, higher poverty and inadequacy of skilled birth attendants. Maternal and paternal highest education levels were significantly correlated with measles vaccination after adjusting for all other examined variables. The greatest increase in the odds of vaccination was found when mothers and fathers had reached secondary level education or higher, compared with no education (p<0.001). Household wealth quintile was a significant and positive correlate of measles vaccination after adjusting for all other variables in the model. The odds of measles vaccination were increased for each level of wealth compared to reference quintile (poorest; Table 5). The odds of vaccination among the richest quintile were almost two-times higher (OR = 1.87, 95% CI [1.58-2.21]) compared with the reference group. The presence of a skilled attendant at the child's birth significantly increased the odds of measles vaccination after adjusting for all other variables in the model (OR = 1.94, 95% CI [1.77-2.11]).
Discussion
Measles vaccination coverage in rural regions of Indonesia appears weakly associated with place of residence after controlling for sex of the child, maternal age, maternal age squared, maternal and paternal education, household wealth and the presence of a skilled birth attendant. Although education, wealth and access to skilled birth attendants were strongly correlated with measles vaccination, the marginally significant result obtained for place of residence means that it is not possible to exclude rural location per se as a determinant of vaccination uptake.
Ordinarily it would be expected that low education, higher birth rates, poverty and inadequate vaccination health staff in rural areas would lead to highly significant lower vaccination rates. The Millennium Development Goals Report 2011 indicates a pronounced rural disadvantage, with rural children remaining at greater risk of dying, even in countries were child mortality rates are low overall15. A study of vaccination coverage among Indian children concluded that rural residence alone did not have a significant effect, but if coupled with poverty and minority status, rural residence amplified disparities in coverage16.
The findings presented here, however, suggest slightly higher adjusted-odds of measles vaccination coverage in rural areas. This may be explained by Indonesia's targeted approach to reducing the impact of rural residence on health. Indonesia's village based health clinics, or Puskesmas, and the village midwife program were established to improve access and reduce health inequalities among disadvantaged groups, including rural and remote communities17. Village midwives provide immunisation, as well as other maternal and child health services via the extensive POSYANDU (integrated health services post) network, which has significantly improved access to health care and health outcomes in Indonesia18. Outreach activities such as special vaccination days tend to target those villages that have reported poor vaccination coverage in the past. Therefore, more resources are directed towards activities to improve coverage and reduce drop out in rural and remote villages19,20. Nevertheless, as this result was only marginally significant, the cumulative effects of several other determinants of vaccination in rural areas, such as poverty, low maternal education and limited access to skilled health workers, provide an important starting point for addressing rural-urban disparities in measles vaccination uptake.
Higher poverty in rural areas adversely impacts on measles vaccination in several ways. First, deprived neighbourhoods generally have inferior social amenities which create disincentives for skilled health staff to relocate to such areas21. Poverty reduces the capability of mothers to take children to vaccination centres. Ironically, the uptake of childhood immunization offsets the detrimental effects of poverty and low maternal educational attainment22,23. Given that poverty in Indonesia is concentrated among households in the rural agricultural sector, it is important to ensure that poverty reduction activities are targeted appropriately. A 2006 study found that growth in the urban services sector has the largest effect on poverty reduction for all sectors except urban agriculture. In addition, growth in rural agriculture strongly reduces poverty in the rural agriculture sector, which is the largest contributor to overall poverty in Indonesia. This implies that the most effective way to accelerate poverty reduction in Indonesia is by focusing on integrated and sustained support of urban services, as well as rural agriculture24.
Although Indonesia has, particularly in the past decade, implemented poverty alleviation programs such as healthcare subsidy cards for the poor, a considerable leakage continues to flow to the non-poor. Conditional on ownership, the middle wealth quintiles were more likely to use the subsidized health cards than the poorest quintiles25. Improved governance of this and related initiatives to improve access to health care for poor Indonesians is urgently required.
This study found that maternal education was a significant determinant of measles vaccination coverage. Maternal education has also been found to influence a mother's ability to recall whether their child has received vaccinations, and the likelihood that a vaccination card has been kept for the child5. This implies that education enhances a mother's understanding of the importance of immunisation and child health care. Ensuring access to education for females in rural areas could, therefore, help to reduce disparities in vaccination coverage. Improvements in female education in rural areas must address two impediments: cultural antipathy towards female education26, and relatively high parity27 among women.
The proportion of children delivered with the assistance of a skilled birth attendant was significantly lower in rural areas. This trend reflects the rural-urban distribution of skilled health workers in Indonesia and most developing nations28. Although the first dose of measles vaccine is not administered until 9 months after birth, the availability of skilled birth attendants at birth appears to predict vaccination coverage; as such, the availability of quality health staff is likely to be continued into early childhood. Furthermore, the availability of skilled birth attendants is strongly influenced by factors known to directly influence measles vaccination. For example, a study into inequalities in maternal and child health in the Asia-Pacific found that the overall geographical, socioeconomic context and socioeconomic position contributed to 75% of the inequalities in skilled birth attendance in Indonesia13. Specifically, wealth contributed 27% and maternal education 12% to inequalities13. These determinants reflect the major determinants of inequalities in measles vaccination identified here.
A national strategy is required to improve the current inadequate distribution of health workers in rural regions. Good health infrastructure and a suitable mix of health workers in rural regions will help to restore the confidence of rural residents in the health system28. In relation to improving vaccination in rural regions, a study in India found that revitalization of rural health systems has a positive effect on improving vaccination rates. However, the study also found that small incentives have large positive impacts on the uptake of vaccination services in resource-poor areas and are more cost-effective than purely improving supply29.
Improvements in the quality and accessibility of rural health services could also overcome issues relating to vaccination drop out. The 2009 report on Expanded Program on Immunisation (EPI) immunisations in Indonesia indicated the complete drop-out rate for DTP as 4%, but partial dropout as 'significantly higher in all regions'30. Thus, given that the measles vaccination is scheduled one month before the second DTP vaccination, it is possible that urban-rural differences in measles vaccination coverage are influenced by drop out.
Over and above the need to reduce the urban-rural gap in measles vaccination coverage is the need to raise the national vaccination coverage at least to the current global measles vaccination coverage average of 83%. In addition to concomitantly targeting the socio-demographic determinants identified in this study, an effective initiative is a national measles supplementary vaccination program, such as the pilot supplementary vaccination program organised in 3 Indonesian provinces with assistance from UNICEF in 200931. The ability of these programs to actively seek out children for vaccination, particularly the socioeconomically disadvantaged, will assist in raising national coverage by increasing coverage in these groups13.
The results presented here must be interpreted in light of several limitations. There are limitations to the use of skilled birth attendance as a proxy for access to health care. As not all skilled birth attendants provide immunisation services, it is possible that the positive correlation found here is due to the outreach and education activities of skilled birth attendants rather than the direct provision of immunisation services. Furthermore, EPI operations are restricted in their ability to provide outreach to rural areas by the need to maintain the cold chain of vaccination storage. Rural-urban differences in access to health care may also be influenced by other factors, such as the distance to a health facility and not wanting to attend unaccompanied. These were investigated in the IDHS, but were not considered here because they related specifically to the woman's ability to access health care for herself and, therefore, may not extend to obtaining health care for children5.
The logistic regression analysis conducted here was carried out at the individual level. The type of residence by classifying respondents as urban or rural residents, was collected at the individual level; however, it may also be considered a community or contextual level variable. Two limitations of our statistical approach in relation to type of residence are that statistically significant results may be confounded by the higher-level variable and when the hierarchical nature of the data are not considered, potentially important community level effects may be overlooked32,33. This model does not take into account contextual effects on decision-making, such as social learning and social influence34, which can lead individuals in a similar social setting to act similarly, and the effect of location on the availability of public health infrastructure. The policy implications of this being that interventions must target community, as well as individual determinants of vaccination coverage35. However, we believe that these limitations will have minimal impact on our findings because type of residence is has not been consistently treated as a community-level variable in studies of DHS data35,36.
In addition to providing sustainable initiatives to increase measles vaccination coverage globally, it is important to close the rural-urban gap in Indonesia's measles vaccination uptake. Addressing the critical determinants of inferior measles vaccination coverage in Indonesia's rural regions will facilitate major improvements in Indonesia's child health trends. Three such critical determinants for attention in Indonesia's rural areas highlighted in this study are poverty, parental education and access to skilled health workers.
References
1. World Health Organization. Measles. Fact sheet 286. (Online) 2009. Available: http://www.who.int/mediacentre/factsheets/fs286/en/ (Accessed 2 December 2010).
2. Dabbagh A, Gacic-Dobo M, Wolfson L, Featherstone D, Strebel P, Okwo-Bele JM, et al. Global Measles Mortality 2000-2008. Morbidity and Mortality Weekly Review 2009; 58: 1321-1326.
3. World Health Organization. Measles vaccines: WHO position paper. Weekly Epidemiological Record 2009; 84(35): 349-360.
4. United Nations. The Millennium Development Goals Report 2009. (Online) 2009. Available: http://www.un.org/millenniumgoals/pdf/MDG_Report_2009_ENG.pdf (Accessed 2 December 2010).
5. Statistics Indonesia (Badan Pusat Statistik-BPS), Macro International. Indonesia Demographic and Health Survey 2007. (Online) 2008. Available: http://www.measuredhs.com/pubs/pdf/FR218/FR218[27August2010].pdf (Accessed 23 February 2010).
6. World Health Organization. SEAR EPI Fact Sheet. (Online) 2008. Available: http://www.searo.who.int/vaccine/LinkFiles/EPI2008/SEAR08.pdf (Accessed 2 December 2010).
7. Murray CJL, Shengelia B, Gupta N, Moussavi S, Tandon A, Thieren M. Validity of reported vaccination coverage in 45 countries. The Lancet 2003; 362(9389): 1022-1027.
8. Muula S. How do we define 'rurality' in the teaching on medical demography? Rural and Remote Health 7: 653. (Online) 2007. Available: www.rrh.org.au (Accessed 19 December 2007).
9. Measure DHS. Description of the Demographic and Health Surveys Individual Recode Data File. (Online) 2008. Available: http://www.measuredhs.com/pubs/pdf/DHSG4/Recode4DHS.pdf (Accessed 1 May 2011).
10. Rutstein SO, Johnson K. The DHS Wealth Index. DHS Comparative Reports 6. (Online) 2004. Available: http://www.measuredhs.com/topics/wealth/start.cfm (Accessed 2 May 2011).
11. Hobcraft J. Women's education, child welfare and child survival: a review of the evidence. Health Transition Review 1993; 3(2): 159-173.
12. Wirth ME, Balk D, Delamonica E, Storeygard A, Sacks E, Minujin A. Setting the stage for equity-sensitive monitoring of the maternal and child health Millennium Development Goals. Bulletin of the World Health Organization 2006; 84(7): 519-527.
13. Rannan-Eliya R. Review of the situation of equity in access to maternal and child health care in the AsiaPacific region: consultation on equity in access to quality health care for women and children. (Online) 2008. Available: http://www.unicef.org/eapro/Unicef_VN_MNCH_Review_04-22.pdf (Accessed 15 May 2011).
14. Hill H, Resosudarmo BP, Vidyattama Y. Indonesia's changing economic geography. Bulletin of Indonesian Economic Studies 2008; 44(3): 4 07-435.
15. United Nations. The Millennium Development Goals Report 2011. (Online) 2011. Available: http://www.un.org/millenniumgoals/11_MDG%20Report_EN.pdf (Accessed 15 July 2011).
16. Som S, Pal M, Chakrabarty S, Bharati P. Socioeconomic impact on child immunisation in the districts of West Bengal, India. Singapore Medical Journal 2010; 51(5): 406-412.
17. Hatt L, Stanton C, Makowiecka K, Adisasmita A, Achadi E, Ronsmans C. Did the strategy of skilled attendance at birth reach the poor in Indonesia? Bulletin of the World Health Organization 2007; 85(10): 774-782.
18. Halabi SF. Participation and the Right to Health: Lessons from Indonesia. Health and Human Rights. (Online) 2009; 11(1): 49-59.
19. Tandiara N. Improving immunization coverage: a review of EPI coverage in West Sulawesi province, Indonesia. In: Proceedings, 45th International Course in Health Development; 11-22 September 2008; Amsterdam; KIT (Royal Tropical Institute/Vrije Universiteit Amsterdam; 2009 Available: http://www.search4dev.nl/document/185348 (Accessed 30 August 2011).
20. Government of Indonesia. Indonesia Progress Report on the Millenium Development Goals. (Online) 2004. Available: http://www.undp.or.id/pubs/imdg2004/English/MDG-IDN_English_Goal4.pdf (Accessed 7 July 2011).
21. Shankar PR. Attracting and retaining doctors in rural Nepal. Rural and Remote Health 10: 1420. (Online) 2010. Available: www.rrh.org.au (Accessed 30 December 2010).
22. Bawah AA, Phillips JF, Adjuik M, Vaughan-Smith M, Macleod B, Binka FN. The impact of immunization on the association between poverty and child survival: Evidence from Kassena-Nankana District of northern Ghana. Scandinavian Journal of Public Health 2010; 38(1): 95-103.
23. Semba RD, de Pee S, Berger SG, Martini E, Ricks MO, Bloem MW. Malnutrition and infectious disease morbidity among children missed by the childhood immunization program in Indonesia. Southeast Asian Journal of Tropical Medicine and Public Health 2007; 38(1): 120-129.
24. Suryahadi A, Suryadarma D, Sumarto S. The effects of location and sectoral components of economic growth on poverty: Evidence from Indonesia. Journal of Development Economics 2009; 89(1): 109-117.
25. Sparrow R. Targeting the poor in times of crisis: the Indonesian health card. Health Policy and Planning 2008; 23(3): 188-199.
26. Mellington L, Cameron N. Female education and child mortality in Indonesia. Bulletin of Indonesian Economic Studies1999; 35(3): 115-144.
27. Schoemaker J. Contraceptive use among the poor in Indonesia. International Family Planning Perspectives and Digest 2005; 31(3): 106-114.
28. Rokx C, Giles J, Satriawan E, Marzoeki P, Harimurti P, Yavuz E. New insights into the provision of health services in Indonesia: a health workforce study. Washington, DC: The International Bank for Reconstruction and Development/ World Bank, 2010.
29. Banerjee AV, Duflo E, Glennerster R. Kothari D. Improving immunisation coverage in rural India: clustered randomised controlled evaluation of immunisation campaigns with and without incentives. BMJ 2010; 340: c2220.
30. BASICS III. Improving child health in Indonesia: Millennium Challenge Corporation Indonesia Immunisation Project. (Online) 2009. Available: http://www.basics.org/reports/FinalReport/Immunization-Final-Report_BASICS.pdf (Accessed 15 May 2011).
31. UNICEF Indonesia. A supplementary measles immunization campaign. (Online) 2009. Available: http://www.unicef.org/indonesia/media_11607.html (Accessed 4 December 2010).
32. Bardenheier BH, Shefer A, Barker L, Winston CA, Sionean CK. Public Health Application Comparing Multilevel Analysis with Logistic Regression: Immunization Coverage among Long-Term Care Facility Residents. Annals of epidemiology 2005; 15(10): 749-755.
33. Li J, Alterman T, Deddens JA. Analysis of Large Hierarchical Data with Multilevel Logistic Modeling Using PROC GLIMMIX. In, Proceedings: Thirty-first Annual SAS Users Group International Conference; 26-29 March 2006; San Francisco. Cary NC: SAS Institute Inc; 2006.
34. Ionnides YM, Topa G. Neighborhood effects: Accomplishments and looking beyond them. Journal of Regional Science 2010; 150(1): 343-362.
35. Boco AG. 2010. Individual and community level effects on child mortality: an analysis of 28 demographic and health surveys in Sub-Saharan Africa. DHS Working Papers 73 (Online) 2010. Available: http://www.measuredhs.com/pubs/pdf/WP73/WP73.pdf (Accessed 20 February 2010).
36. Mahy M, Neeru G. Trends and differentials in adolescent reproductive behavior in Sub-Saharan Africa. DHS Analytical Studies 3 (Online) 2002. Available: http://www.measuredhs.com/pubs/pdf/AS3/AS3.pdf (Accessed 20 February 2011).


