Australia's dental workforce is unevenly distributed, with 79% working in the large cities of metropolitan areas1. As a result, rural areas are under-supplied with dentists to the extent of there being approximately 1000 dental professionals less than the ideal number2. This disproportionate geographical distribution of dentists was highlighted in a 2005 study that found there were 56.2 dentists per 100 000 population in major cities, while in rural Australia there were less than 33.6 dentists for inner regional, 26.9 for outer regional and 22.9 for remote/very remote areas3.
One way to address this problem is to target the next generation of dentists at university with the intent of encouraging them to consider working in a rural area. There is plentiful evidence from the discipline of medicine that rural outreach placements can positively influence undergraduate students to work in a rural location when they have qualified. For example, one Western Australian study of a medical students' rural clinical placement program found that students' rural background, a placement duration of 1 month or longer, self-reported value of the experience and voluntary participation in the program were the key factors that encouraged students to work in a rural location after graduation4.
A survey of medical students from the University of Otago, New Zealand, found that having a rural background positively influenced a decision to enter rural employment5. Other research on medical students' placement experiences has found that students' career intentions and job opportunities are also important factors in the decision-making process when considering rural employment6,7. James Cook University School of Medicine in northern Australia provided eight-week rural internships and evaluated medical students' responses using questionnaires and interviews. It was identified that good communication and support among the faculty, placement staff and students was vital for a successful placement. The researchers also commented on the importance of preparing students sufficiently with adequate meetings and appropriate literature, and the need for quality placement clinical supervisors8. Lyle et al in a cross-sectional survey of Australian health faculties, including dental, medical and general health students, also found that communication and resource sharing between faculty and rural program staff was critical for a successful program9.
Despite positive evidence in medicine and other health disciplines, a recent literature review suggested there is still insufficient definitive evidence about the effectiveness of rural placements10. The authors recommended that future research should focus on longitudinal rural placement studies with follow up of the students' long-term job locations.
In dentistry there is limited evidence on the value of rural placement programs. One dental undergraduate study involved a three-week, voluntary rural program for 4th year dental students from the University of Western Australia11. The study was conducted over 3 years from 2002 and involved 55% of the 143 students in their final year, with rural dental practitioners acting as clinical supervisors. A multifaceted evaluation approach was adopted using questionnaires and interviews. The questionnaire focused on accommodation, the adequacy of support, value of the learning experience and fulfilment of program aims. The students' intentions to work in a rural area were recorded and their post-graduation work location noted. Over 3 years a positive association was found between the rural placements and new graduates working in a rural location. In the first year of the scheme (2002), 26% worked in a rural area, and the proportion rose to 38% in 2003 and 60% in 2004. The majority of students (95%) were positive in their feedback about the placement and deemed it a valuable learning experience.
The Melbourne Dental School in Victoria included a 4 week rural outplacement in July 2006 for 70 final year undergraduates who were rostered in groups of 6-10 to go to Shepparton (178 km from metropolitan Melbourne)12. All students expressed confidence in performing clinical tasks and reported that the experience helped them prepare for real-life situations. The clinical supervisors and staff were especially valued by students for their support. Several barriers were identified to working in a rural location, the most common being separation from family, professional isolation and the lack of social interaction with friends. The authors highlighted the need for strategies from rural health services and rural practitioners to provide new graduates with professional and personal support in order to help them settle in the rural environment. A study from South Australia provides evidence that dental undergraduates can significantly benefit rural public dental services by providing patient care and reducing public patient waiting lists, while also providing the students with a positive experience which may encourage them to consider working in a rural location post-graduation13.
Internationally, the impact of community-based dental education was assessed by qualitatively analysing 160 dental students' essays at University of North Carolina, USA, between 1998 and 200013. Three common themes were identified in the responses: personal and professional growth, enhanced awareness and commitment to service14. At a recent European Symposium where the challenges of outreach teaching were discussed, the positive aspect of placements were reported as: working in a real-world situation, treating a wider range of patients, acquiring first-hand experience of general health issues in a new environment, and working as part of a clinical team15.
Qualitative research methods were employed in a study of outreach placements of 4th year dental undergraduates in Manchester, UK, who were sent to primary care centres in disadvantaged areas of the city16. The study recorded the students' worries and concerns pre-placement. The most common concerns identified were meeting course requirements, the type of patients and the range of potential clinical tasks. Post-placement the students reported fewer concerns, although some identified the clinical support available and 'time stress' as issues to be addressed. A small number of students believed they had fallen behind in faculty course requirements. Overall the program was deemed a success because it achieved its educational objectives. The main findings were increased confidence in undertaking basic clinical tasks and improved time management skills. This study concentrated on comments received from the students to build a picture of the potential of clinical placements to improve aspects of clinical and non-clinical skills. Although it was not a rural program, the use of student feedback models is an important way to assess the value of a rural initiative.
The Faculty of Dentistry, University of Sydney, New South Wales (NSW), implemented a Rural Placement Program with funding from the Australian Government Department of Health and Ageing. The placement program was modelled on those described by the Universities of Melbourne, Western Australia and Manchester11,12,16. The evaluation utilised self-complete questionnaires with a number of free-answer sections to record the students' views and opinions of the placement. This article focuses on the students' perspectives on the placement, with particular emphasis on factors and barriers which may have influenced their intentions to work in a rural location post-graduation.
In the Rural Placement Program implemented by the Faculty of Dentistry, University of Sydney, NSW in 2009, final (4th) year dental undergraduates were assigned to a NSW rural clinic for 1 month. There were 4 rotations with placements at one of 3 clinical sites: Bathurst (2 students), Orange (2 students) and Bowral (6 students). Of the 80 students in 4th year, 40% (n=32) volunteered for the rural program.
The students worked in pairs and a registered dentist who had received specific faculty induction training was assigned the role of clinical supervisor at each rural clinical location. All clinical procedures undertaken on the placements were recorded and contributed to the undergraduates' final year clinical requirements.
A faculty member was designated liaison officer to deal with issues and correspondence with the students and pre-placement briefing meetings were provided. Information booklets and maps were provided for the students. Travel and accommodation costs were paid by the university, as was a daily student allowance.
A self-completed questionnaire was distributed to the students 2 weeks prior to their rural rotation and a post-placement questionnaire within 10 days of their return. Students who did not respond were followed up via email, with a telephone call or SMS one week later.
A semi-structured questionnaire with some open questions was used to record demographic data, rural background, opinions on clinical supervisors, clinical tasks plus students' expectations, concerns and anxieties about the rural initiative, and their future work intentions. The open questions gathered a considerable amount of data and 'framework analysis' was used to provide a platform for interrogation of these data. In order to assist with the content analysis, seven academic dentists identified themes in the questionnaires' open questions. Each staff member received a random selection of 4 pre- and post-placement questionnaires and was asked to identify common themes in those student responses. The themes were then collated by the two principal researchers (GJ and AB) and these formed the basis of the qualitative analysis (Fig1).
Ethics approval was obtained from the Ethics Review Committee (RPAH Zone Sydney).

Figure 1: Students' identified themes from the questionnaires' free answer sections.
Pre- and post-placement free answers were completed by all students who took part in the Rural Placement Program. The mean age of participants was 27 years, 59% were female and the majority (77%) had been raised in a city.
Students' pre-placement themes
An overview of the students' expectations, hopes and concerns prior to their rural placement is provided (Fig2). The most common expectations varied from 'a new experience', meeting different patients to gaining more clinical dentistry (including extractions, treatment planning and simple restorations). Students hoped to increase their clinical experience, improve their communication skills and gain confidence while experiencing a rural community lifestyle.
The key concerns pre-placement were missing lectures at the university, maintaining clinical quotas while away from the metropolitan teaching hospitals, concerns regarding clinical ability and the supervisors' expectations of students' abilities.
I am a little concerned about losing valuable clinical time at the Sydney Dental Hospital, as I may not be able to get enough experience at the rural clinic, plus missing lectures and having to come back and catch up could well be stressful. (Female, aged 26)
The students perceived the clinical strengths of the program to be treatment planning, being able to undertake extractions, good communication skills, and a strong work ethic (Table 1). Weaknesses across the group were reported as diagnostic skills, prosthodontic experience and poor organisational skills.
More than half the students felt confident and prepared for their rural placement. Common reasons for this were their clinical experience at the university, the pre-placement briefing and the rural booklet that provided information on the rural placement.
Some students stated they would have liked more specific information regarding the supervisor's expectations of their abilities. There was an expectation that students would be treating more patients per day in a rural public clinic than at the teaching hospitals, and students were concerned their clinical time-management skills were not sufficiently developed to allow them to treat all their allocated patients:
Until now, we have had the luxury of having 3 hour appointments to complete treatment. It is a bit daunting to think about having to drastically reduce appointment duration. Also, I am unsure about the expectations that the supervisor will have of our clinical skills and procedural knowledge. (Male, 32 years)
The perception of experiencing a quiet, friendly community was generally seen as positive by the students. The short commute to their designated clinic was a relief to almost all the students who were used to longer journeys in Sydney.
Many reported an intention to use the rural placement to assist in making a decision about working in a rural location post-graduation, but emphasised that partners and family were likely to be major factors in deciding where they would work. However, from a practical perspective, they felt that job opportunities would ultimately dictate their practice location. Just over half the students were considering working in a rural location prior to the rural placement (Fig3).

Figure 2: Participants' pre-placement expectations, concerns and hopes regarding the Rural Placement Program.
Table 1: Participants' self-perceived strengths and weaknesses pre- and post-clinical placement

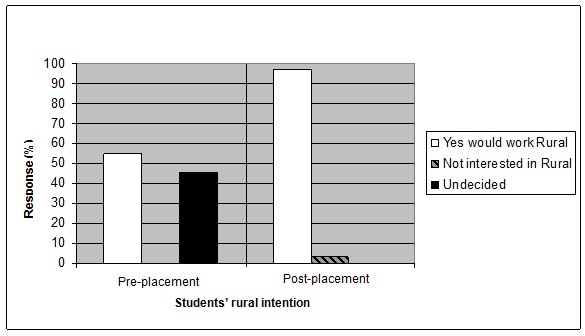
Figure 3: Rural intentions of the students pre- and post-placement.
Students' post-placement themes
Following the rural placement the students were extremely positive about the clinical education received, reporting increased clinical confidence and time-management skills. Restorative care, diagnosis and extractions were the most commonly reported clinical procedures performed. Other procedures mentioned by several students included detecting caries, patient management, root canal therapy, acute care management, dealing with special care patients and crown preparations. The students reported that they had to complete patient treatment at a much faster pace than at the metropolitan teaching hospitals, treating between 6 and 8 patients per day.
The rural clinician supervisors were highly rated by the students, with comments that they had been 'supportive', 'encouraging', 'helpful', 'knowledgeable' and 'professional'. Supervisors' individual techniques varied; however, it was evident that each provided a personal and informative experience for students.
Calm, supportive and really cared about us, a terrific supervisor. (Male, 35 years)
One of the best, greatest clinical supervisors I have ever had. (Female, 25 years)
An excellent clinician and great person; they made the whole experience special. The team were also great, helpful and supportive and need special thanks. (Female, 29 years)
The majority of students felt their relationship with the rural supervisor was better than that with their university supervisors for the following reasons:
- they had more time and interaction in the clinic to build a stronger relationship, leading to a greater level of trust between staff and student.
- there was no changeover of staff during the placement, whereas the university used a large number of supervisors, which reduces personal contact.
Almost all the students enjoyed the rural community setting and aspects noted were: 'pleasant patients', 'a broader range of clinical problems', 'being treated with kindness and respect from the patients and staff', 'the slower pace of life', 'the short commute to work' and 'more relaxed atmosphere'. The living accommodation provided was generally rated positively and many commented that they preferred the rural to the metropolitan community.
There were concerns about some aspects of the placement, mainly: the lack of an effective fast internet connection, lectures not being placed online, cold weather, a lack of communication with the faculty (especially when there were problems), and the stress of catching up on clinical quotas on return to the university. Students in the first rotation, in particular, struggled with reintegrating quickly after their rural placement.
Almost all students were considering working in a rural location after they qualified and quotes from the free-answer questions provided an insight into the way the placement program raised their interest:
Rural is avoided due to the ignorance of the area and people, having a rural experience will allow clinicians to make a more educated choice when choosing where to work. (Female, 24 years)
Experience reminded me why I want to do dentistry, to help people who wanted to be helped and to be in an environment where patient care is the number one priority. (Female, 30 years)
I think it alters my perception about what dentistry is about entirely, moving away from the need to graduate, reach quotas and sit exams. I was exposed to an environment where my primary concern was the person in front of me and that it was my responsibility to provide the best care possible, not to achieve a certain grade. (Female, 27 years)
If I was asked to work in a rural situation similar to that of Bowral I would honestly consider the option, whereas prior to the placement I would not have thought about it. (Male, 25 years)
I'm determined to look for a job in a rural setting. (Female, 30 years)
Themes were identified that may encourage or discourage the students from working in a rural location after graduation (Fig4). Aspects such as the rural community and slower pace of life, a broader range of clinical procedures, kinder patients, good clinical mentors and a shorter commute to work were deemed positive factors in a rural working life.
Barriers identified were that rural life might be too quiet and isolated, and they could miss friends, family and partners. Job opportunities were also noted as a decisive factor.
All the participants would recommend the rural placement to future students and believed it was a great success and, in some cases, one of the best aspects of their undergraduate program. The main reasons for these positive views were 'making new professional contacts', 'the clinical experience acquired', 'the clinical supervisors', 'experiencing rural community life', 'greater independence', 'a clinically and personally rewarding experience'. For example:
Excellent experience both clinically and personally. (Female 25 years)
Best thing I've ever done in my 4 years as a dental graduate. (Male, 28 years)
Experience gained is irreplaceable. (Female, 26 years)
Absolutely - it was awesome and clinically I think it added to my education experience. (Male, 31 years)
I got so much out of it. (Male, 24 years)
Once in a lifetime opportunity! (Female, 28 years)

Figure 4: Factors involved in the decision to work in a rural location.
Discussion
Pre-and post-placement responses were obtained from all students. The majority of the group were female and most were raised in a city environment. Rural background has been found to encourage students to consider working in a rural location post-graduation4; however, in the present study city dwellers really enjoyed the placement and were well-disposed to move to a country area.
Other important elements were the pre-planning of the placement program and the inclusion of factors highlighted in the literature as being an important part of a successful program, namely:
- 1 month placement duration
- trained clinical supervisors
- a dedicated administrator to deal with day-to-day issues and to act as the link between students, clinical supervisors and university faculty
- an advice booklet.
The student views and opinions were collected from semi-structured questionnaires. Self-report was used and this has the potential for judgement error, for participants providing socially desirable responses, and for recall bias. This report focuses on free answers to a questionnaire which were therefore not forced; however, interviews and focus groups may have been a better method. This could have been problematic, for the students' very full curriculum means it would have been difficult to interview all participants, thus compromising the validity of the outcome.
Information packs and pre-placement meetings were provided for the students, as advised by the James Cook University study, and most students were satisfied with the preparation8. However, some mentioned they did not feel entirely prepared and would have liked further information, such as maps of the clinics and surrounding rural locations. Students generally would have appreciated more information about the clinical supervisors and their expectations of students' clinical abilities.
The students were positive about the accommodation provided, the rural locations and community support, with 'kind patients and staff' seen as the most important positive aspects of the program.
The clinical supervisors proved exemplary during the placements and their commitment and professionalism was essential to the program's success. This supports the studies from James Cook and Melbourne Universities, both of which reported that the quality of supervisors is an integral aspect of a successful placement program8,12. The rural supervisors spent more time with the students compared with teaching hospital staff, and felt more at ease with the students. Strong personal relationships were built with trust and respect evident between student and rural supervisor.
Several students felt isolated from the faculty during the placement and were disappointed with the lack of online lectures. Lyle et al stressed the importance of communication and resource sharing between faculty and students9. The Sydney program could have been enhanced if greater attention was paid to communication. Some students felt they were 'falling behind' in course requirements by being away from the university for 1 month, a concern that was also expressed by some participants in the Manchester University outreach scheme16. This issue was addressed in the Sydney program by the Dean confirming that all work completed on the rural placement would contribute to students' clinical requirements.
The students undertook a wide range of primary care clinical activities, especially extractions and basic restorative dentistry; however, some students also undertook more specialist tasks, such as fixed and removable prosthodontics. Participants reported improved confidence in basic clinical skills, time management and their ability to communicate with patients, mirroring the findings from Manchester16 and Melbourne12 Universities. It is of interest that while most participants identified 'time management' and 'diagnosis' as weaknesses pre-placement, post-placement these problems had been addressed (Table 2).
Table 2: Pre- and post-placement questionnaire questions

It was shown that post-placement 97% of the students were more likely to work in a rural setting after graduation, compared with 57% pre-placement (Fig3), indicating that the program had a positive influence on their practice location opinions. The size of the change is consistent with the Western Australian study11. Those researchers also recorded the postgraduate work locations of participants in their placement program and found an increase in the proportion of graduates working in a rural location11. Ranmuthugala et al have highlighted the need for longitudinal follow up when assessing the value of rural placements10. Hence, the students of the present 2009 study will be followed up in 18 months to ascertain their practice location.
The program will be continued and development will be based on the present evaluation, with improvements to include:
- a designated academic staff member will provide assistance to students regarding their concerns and anxieties, and will increase contact frequency to improve communication pathways
- a policy to make allowances for students' clinical quotas on an individual basis (to be confirmed)
- pre-placement information packs will be expanded to include maps of the clinics and surrounding rural locations and other community information
- the debriefing meetings with students will be embedded into the program to enhance students' re-integration post-placement
- the clinical supervisor training will ensure consistency of grading
- a designated clinical staff member will visit the clinics while the students are on placement to offer support.
In this successful undergraduate Rural Placement Program the students valued both the personal and educational components. The students became more aware of the potential advantages of working in a rural location and most reported that they would consider working in a rural location after graduation. Further research is required to monitor the longer-term work plans of the participants. This will provide more robust evidence about the influence of the rural experience on career behaviour.
Acknowledgements
The placement program would not have been possible without the support of Associate Professor Sameer Bhole (Sydney South West Area Health Service) and Ms Jennifer Floyd (Greater West Area Health Service). Dr Sally Clark, Dr Thomas Hasson and Dr Narayan Prasad were the clinical supervisors and their hard work and support along with their staff in both Area Health Services were vital for the success of the program. Professors Chris Peck and Elizabeth Martin ensured the program received faculty support and Ms Antonia Scorciapino was a valuable advisor when managing the budget. Ms Ramona Grimm Department of Population Oral Health made an important contribution to the project's smooth running. Professor Blinkhorn's position is funded by the Centre for Oral Health Strategy, New South Wales Health and he thanks Chief Dental Officer Dr Wright and his staff for their help and guidance with the project. The Rural Placement Program is funded by the Australian Government, Department of Health and Ageing, Commonwealth of Australia, Health Workforce Division, Canberra.
References
1. Teusner DN, Chrisopoulos S, Brennan DS. Geographic distribution of the Australian dental labour force. (Online) 2003. Available: http://www.arcpoh.adelaide.edu.au/publications/report/statistics/pdf_07/dlf_2003.pdf (Accessed 9 May 2011).
2. Australian Research Centre for Population Oral Health. Working papers of the ARCPOH/Australian Institute of Health and Welfare Dental Statistics and Research Unit workshop on the dental labour force. Adelaide, SA: ARCPOH/AIHW,2 002.
3. Australian Research Centre for Population Oral Health. Geographic distribution of the dentist labour force. Australian Dental Journal 2005; 50: 119-122.
4. Playford D, Larson A, Wheatland B. Going country: rural student placement factors associated with future rural employment in nursing and allied health. Australian Journal of Rural Health 2006; 14: 14-16.
5. Williamson M, Gormley A, Bills J, Farry P. The new rural health curriculum Dunedin School of Medicine: how has it influenced the attitudes of medical students to a career in rural general practice? Journal of the New Zealand Medical Association 2003; 116: 1179.
6. Dalton LM, Routley GK, Peek KJ. Rural placements in Tasmania: do experimental placements and background influence undergraduate health science student's attitudes toward rural practice? Rural and Remote Health 8: 962. (Online) 2008. Available: www.rrh.org.au (Accessed 9 May 2011).
7. Orphin P, Gabriel M. Recruiting undergraduates to rural practice: what the students can tell us. Rural and Remote Health 5(4): 412. (Online) 2008. Available: www.rrh.org.au (Accessed 9 May 2011).
8. Sengupta TK, Murray RB, McDonell A, Murphy B, Underhill AD. Rural internships for final year students: clinical experience, education and workforce. Rural and Remote Health 8: 827. (Online) 2008. Available: www.rrh.org.au (Accessed 9 May 2011).
9. Lyle D, Klineberg I, Taylor S, Jolly N, Fuller J, Canalese J. Harnessing a University to address rural health workforce shortages in Australia. Australian Journal of Rural Health 2007; 15(4): 227-233.
10. Ranmuthugala G, Humphreys J, Solarsh B, Walters L, Worley P, Wakerman J et al. Where is the evidence that rural exposure increases uptake of rural medical practice? Australian Journal of Rural Health 2007; 15: 285-288.
11. Bazen JJ, Kruger E, K Dyson, Tennant M. An innovation in Australian dental education: rural, remote and Indigenous pre-graduation placements. Rural and Remote Health 7: 703. (Online) 2007. Available: www.rrh.org.au (Accessed 9 May 2011).
12. Abuzar MA, Burrow MF, Morgan M. Development of a rural outplacement programme for dental undergraduates: students' perceptions. European Journal of Dental Education 2009; 13: 233-239.
13. Richards L, Symon B, Burrow D, Chartier A, Misan G, Wilkinson D. Undergraduate student experience in dental service delivery in rural South Australia: an analysis of costs and benefits. Australian Dental Journal 2002; 47: 254-258.
14. Straus RP, Stein MB, Edwards J, Nies KC. The impact of community-based dental education on students. Journal of Dental Education 2010; 74(10): S42.
15. Eaton KA, de Vries J, Widstrom E, Gait TC, Bedi R, Meyers I et al. 'Schools without walls?' Developments and challenges in dental outreach teaching - report of a recent symposium. European Journal of Dental Education 2006; 10: 186-191.
16. Elkind A, Blinkhorn AS, Blinkhorn FA, Duxbury JT, Hull PS, Brunton PA. Developing dental education in primary care: the student perspective. British Dental Journal 2005; 198: 233-237.

