This article presents the validation analysis of a research-based conceptual model for developing palliative care in rural communities. Kelley's model uses a community capacity development perspective to articulate the process of developing palliative care in rural communities where care of dying people is normally provided by local generalist healthcare providers, and not palliative care specialists1. The model was developed based on focus group data from interdisciplinary rural healthcare providers across Canada. The purpose of the validation research described in this article is to evaluate whether the theoretical model accurately explains the palliative care development experiences of rural services providers in diverse communities. Further, this research refines the model, evaluating the potential of the model as a theoretically explanatory and predictive tool which has the ability to distinguish between those communities that demonstrate the capacity to move to the next phase of palliative care development and those communities that do not. It was determined that an additional variable should be included in phase 1 of the model, this research has further defined three integrative processes that are applicable across all four phases of the model.
Developing rural palliative care: a conceptual model
Due to the aging population, more people are living longer with chronic and terminal illnesses, and the demand for palliative care is increasing steadily2-5. Indeed most deaths in developed countries result from the kinds of illnesses that would require palliative care services, such as cancer, coronary heart disease, dementia and diabetes1,6, and the need for palliative care services is expected to rise increasingly as the population continues to age1,7. Despite the increasing need for palliative care services, it is well recognized that the people who are dying in rural and remote areas have less access to palliative care services than their urban counterparts8-11. It is also recognized that people dying in rural communities want to remain in their home communities and do not want to travel to urban centers for end-of-life care12-15.
Development of the model
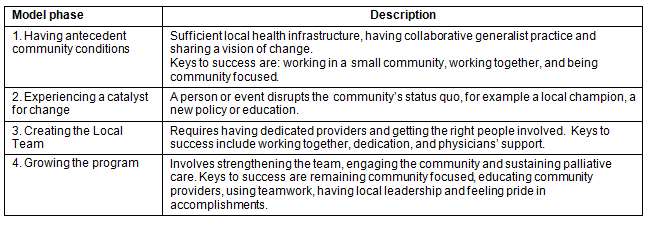
The development of the detailed model, along with its theoretical and empirical underpinnings is outlined elsewhere1. Briefly, the model was initially created from empirical, qualitative data to conceptualize rural communities' process of developing local palliative care programs from the perspective of rural healthcare providers, using a theoretical perspective of community capacity development. The model outlined four phases of rural palliative care development: (i) having required antecedent community conditions; (ii) experiencing a catalyst for change; (iii) creating a local palliative care team; and (iv) growing the palliative care program. Each phase had several tasks that must be accomplished, culminating in phase four which was the delivery of a program that provides clinical care, education, advocacy and is characterized as having created strong linkages both within the community and with outside resources. The model depicted a 'bottom-up' community development approach that built on existing community resources and remained community focused. It further illustrated how rural providers manage the challenges of lack of resources, community resistance to palliative care, bureaucracy, and the nature of the rural environment and described the overarching keys to success for developing rural palliative care as working together, building on existing resources and remaining community focused. The model uses the organic metaphor of a tree (Fig1) to represent developing palliative care in a rural community, and identifies the keys to success in each of the four sequential phases (Table 1).
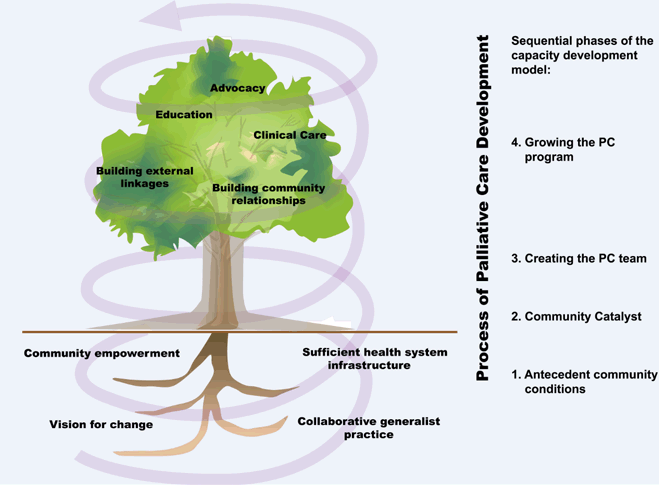
Figure 1: Developing a rural palliative care model adapted with new antecedent condition.
Table 1: Overview of the four-phase model
Method
Ethics approval
Prior to data collection the research protocol was reviewed and approved by the ethics review board at Lakehead University, McMaster University and one of the two participating health regions.
Data collection
The data for the study were derived from seven semi-structured focus groups with 32 rural palliative care providers in 7 communities in 2 provinces in Canada throughout the period 2007-2008. Validation and refinement of the model involved returning to one rural community in Province 1 where data were initially collected in 1999-2000 as part of the original research to develop the model. This was done in order to gather longitudinal data of their palliative care program progress over 8 years and evaluate whether the theoretical model accurately explains the palliative care development experiences of rural services providers.
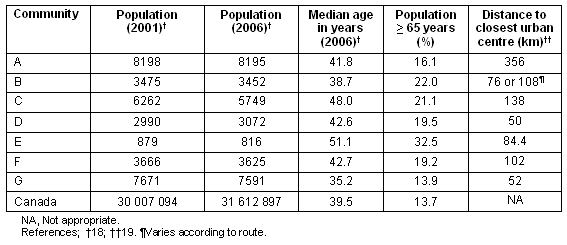
In addition, data were collected in Province 2 from 6 diverse rural communities in one health authority not previously involved in the development of the model. The medical director of palliative care and the program manager of the health region in this province were requested to identify communities appropriate for the research that had less than 10 000 inhabitants, and had healthcare providers who provided palliative care. The population of 10 000 or less was chosen as the inclusion criteria to be consistent with the Statistics Canada definition of 'Rural and Small Town Canada' used in the earlier phase of the research16. A summary is provided of demographic information for all participating communities (Table 2). Further, they were asked to select communities that were at various stages of developing palliative care services in order to examine the explanatory power of the model across the four phases. This sampling also allowed for comparative analysis of community capacity development dynamics in 6 different communities within one geographic region and health authority, providing comparable data to examine the predictive power of the conceptual model. Comparing communities in the same region and health authority minimizes the impact of much of the health system variability that could possibly influence the process and development of palliative care programming. Information about each community's stage of development was withheld from the researchers in order to test the model's ability to theoretically predict without bias. Once the appropriate communities were identified, the medical director of palliative care and the program manager of palliative care created a list of potential participants that included all interprofessional healthcare professionals who were involved in providing palliative care in the selected communities at the time of the study. A letter of invitation was created by the researchers and this letter was sent to all of these identified healthcare providers by the program manager's secretary. Providers who received letters were also invited to identify any others that they knew of who were involved in palliative care and these people were also invited. Therefore, a purposeful sampling strategy was used for this study in order to obtain information-rich sources. Patton explains that 'information-rich [sources] are those from which one can learn a great deal about issues of central importance to the purpose of inquiry' (p230)17. The focus group participants were healthcare providers who worked in a variety of care settings and represented a wide range of healthcare professions and roles: nurses, managers or consultants, occupational therapists, social workers, physicians, pharmacists and volunteers.
Table 2: Rural community demographics18,19
The focus groups served as the method for obtaining expert reviews to validate the conceptual model20. The focus group sessions averaged 55 min duration with a range of 34 min to 2 hours, and were precipitated by a presentation of Kelley's model1. The focus groups were semi-structured in nature, and guided by questions aimed at eliciting participants' impressions of the model (Fig2). All focus groups were audio-taped, transcribed verbatim, and checked for accuracy. The thematic approach used was constant comparative analysis21. Data were coded inductively using the framework for community capacity development, specifically the phases and themes making up the model; this ensured that any new themes that emerged were easily noted. All transcripts were coded manually by two members of the research team. Data from both Provinces 1 and 2 were used to validate and refine the model using the following process of theory development.
Carlson et al. outline a systematic process of theory development and evaluation that consists of theory development, field testing and refinement22. The model validation approach taken in this research was consistent with this process. Using the qualitative data collected during this research, the original conceptual model for developing palliative care was compared with and evaluated against the new data collected. Changes in the model were made where needed to make the model consistent with the new data. Through an iterative process, the data were analyzed and the model was refined where required. The refined model represents the theoretical best fit between the data generated in the field and the existing conceptual model.

Figure 2: Sample questions from focus group interview schedule.
Results
Validation of the model
Overall, the model was validated. As mentioned, the second visit to Community A in Province 1 was to determine whether or not the model reflected the experience of further developing the palliative care team. When thinking retrospectively about their process, participants identified a palliative care educational event as the initial catalyst to their progress and recognized the model as verifying their local experience:
I mean for me, definitely, when I look at where we were then, when we first started this research project with you [Kelley] and where we are now, certainly, you can follow through the model and look at examples all along the way of the different steps that we experienced... But I think that's where we had our beginning [the educational event] was right from the very roots and I think that's why we've done as well as we have.
Participants also elaborated on the fact that, in spite of having formed a team, their progress was sometimes disrupted by external events such as the introduction of government initiatives and the formation of new partnerships with healthcare associations.
In addition, the model was able to theoretically predict that 3 communities in Province 2 had local capacity to develop palliative care and three had not. The major factors that contributed to whether or not local capacity had developed were: the reaction of the community healthcare providers to the regionalization process; the relationship between the palliative care consultant and the local community providers; and the sense of local community empowerment, commitment and vision for change.
Results
Refinement of the model
In addition to the data collected in Province 1, the 6 communities in Province 2 were reviewed as a set, given the common experience with respect to the contextual factors previously mentioned. Themes from this data set include: palliative care development being shaped by internal and external forces, proceeding in a non-linear fashion, requiring an ongoing catalyst, and having a sense of local empowerment. This latter theme was determined to be a fourth antecedent condition, as will be discussed. Further, the first three themes operate across all phases and are illustrated in Figure 1 by the yellow arrows reaching upwards; these themes can be defined as processes which have been further defined as a result of this research.
New antecedent condition: a sense of local empowerment
The 3 communities that began the regionalization process demonstrated strong professional relationships between local community providers and the regional palliative care consultant assigned to their community, as well as all having a community environment that includes a strong sense of local empowerment, and willingness and commitment to improve palliative care services to dying people in their community. In contrast, the communities that had not yet begun to develop palliative care did not have these three characteristics. They may have accepted the regional program and have established good working relationships with the palliative care consultant, but demonstrated no community with vision for change and a lack of commitment to taking local responsibility for community palliative care. A participant alluded to regionalization as interrupting the momentum and dynamics of the informal palliative care team that existed prior to regionalization:
Our palliative care has evolved exactly as you have just stated here over the last 10 years and [then] we had it slightly imposed upon us through the region because the region felt strongly about it.
The communities that had not yet begun to develop palliative care services were also more likely to identify barriers that they felt inhibited them from moving forward. For instance, one participant mentioned that there was a lack of human and financial resources to draw upon:
I think it will also boil down to the volunteering of your services... like the way it stands now, I don't think we could financially have a palliative care team. It just wouldn't work. I mean there is no money in the budgets...
On the contrary, the communities that had begun to develop palliative care demonstrated a clear sense of local community empowerment and resourcefulness. The emergence of this theme from the data led to revising phase 1 of the model to include a fourth antecedent community conditions - a sense of empowerment and community control over local palliative care development. A clear example of community empowerment was displayed in one community when several occupational therapists came together to provide direction to caregivers on how to properly use a piece of equipment. As one participant explains:
[The caregivers] were coming in to do the palliative care assessment care on this lady; they had never been trained on how to use a lift and we were horrified. The vendor was not big on doing the training and so we did the training.
This same participant remarked that in order to deliver palliative care services it is necessary to 'not [be] afraid to try something that nobody has tried yet'. A participant from this same community attributed community control and self-sufficiency as unique and specific to each community:
I do think that each rural community is so different that it needs to be individual and needs to have its own strong place I don't think that we should... have to go to the region for help. I think it should be self-contained in each rural community.
It also became evident that a sense of empowerment and local control facilitated palliative care development in the community from Province 1. According to one of the participants, local providers did not want palliative care in to be as formalized as it was in the regional centre. In effect, local providers were motivated to maintain their independence in the process:
... the meetings started and one of things that we said a number of times was that we don't want this to be formal, we want it to be informal... We really don't want to take minutes and don't want to be moving motions and that... I mean we certainly fought for a long time to keep our autonomy...
The three integrative thematic processes of concern across all phases of the model will be discussed in detail.
Integrative process 1: shaped by internal and external forces
The 6 communities in Province 2 had recently experienced external events, mainly the effects of healthcare restructuring given the regionalization of palliative care services by the health region. The regionalization process led to several changes in the delivery of palliative care services, including the implementation of palliative care nurse consultants in every community. One of the palliative care consultant participants, who discussed palliative care from both a regional and local perspective, described how all of the communities concerned had had their own informal teams before regionalization and how restructuring had upset much of the groundwork that had already been laid by the community:
But there has been that resistance... groups that they had started to organize...when they started to be regionalized, all that got uprooted and it's been a long journey back to bring some of that back.
The themes that emerged from the discussion related to the catalyst phase, the first in the developmental model. Themes related to 'getting started' were collapsed into three main categories: (i) community reaction to the regionalization process; (ii) the relationship between the palliative care consultant and the local community providers; and (iii) commitment and vision for change in palliative care, along with a sense of local community empowerment. Whether or not communities had started to develop palliative care depended on these dynamics, in addition to the response to regionalization. The model theoretically predicted that 3 communities had the core capacity and had begun to develop local palliative care while the other 3 communities lacked the antecedent conditions for change and had not yet begun the process. The medical director of palliative care and the program manager of the health region verified these results as being accurate.
Through the discussions, several key forces were recognized as having an effect on the development of palliative care that were not elaborated on in the initial model. Both spatial and socio-demographic characteristics were found to influence the development of palliative care services. For instance, communities that were farther away from regional centers were more likely to develop local palliative care. The majority of communities that developed palliative care teams were more than 100 km from the closest regional centre (Table 2). The exception here is Community G where palliative care development was strongly influenced by a local champion - the medical director of palliative care for the region was a physician and resident of Community G. The remaining communities were perhaps more reliant on accessing palliative care services through their regional centre due to easier accessibility. As a participant from confirmed:
[Community F] has to be a little more self-sufficient than us, definitely because even with weather conditions... [Community F] you know, is probably only about 4000 people but they are 1 hour away from a regional hospital and in the winter it could be about 2 or 3 hours.
Other forces that were considered to interfere with the delivery of palliative care were the actions of external community or health associations. For example, the policies and protocols of paramedics and community police in responding to home deaths do not tend to recognize that palliative deaths should be treated differently from non-palliative deaths. For instance, paramedics may commence resuscitation efforts and police may start to investigate whether foul play was involved in the death. In addition, new strategies put in place by health associations may temporarily disorganize local activities. This was the case in Community A when a provincial health association established palliative care guidelines:
Through [a provincial health organization] getting more involved in palliative care, they came out with these community action teams and then our supportive care team became that team and now it has encompassed the palliative care team.
Yet it is also possible for external policies or procedures to serve the goals of palliative care teams. This occurred in Community A when, in order for the community hospital to receive accreditation, they were required to improve coordination with community agencies that provided care and support to patients outside of the hospital. The notion of an external policy having the potential to be either a support or constraint was also evident in terms of how the communities in Province 2 responded to regionalization and the implementation of palliative care nurse consultants. As a participant from Community F explains, the 6 communities responded in different ways:
The regional program was a hard sell to rural communities for a long time so it was a negative catalyst for some time and it became more positive as time went on.
In addition, participants from all of the communities agreed that one of the positive effects of regionalization was the rearrangement of services and office space which led to the centralization of services in a single building. According to a participant from Community G:
That kind of happened with regionalization as well - it rearranged where we all were; home care ... came ... into this facility and it made it so that everyone was more accessible to each other. So communication improved immediately.
From yet another geographical perspective, interestingly, the acceptance of palliative care nurse consultants was more likely to occur if the individual was 'internal' to the community - a community resident. Participants from Community F discussed the importance of having a local palliative nurse consultant on the team as it facilitated communication with informal networks in the community and residents. The team members expressed that having a local palliative care nurse consultant increased accessibility to information and resources:
[The nurse consultant] is like three steps from our office.... It's just that fact that we see her everyday that she's here, if you have something to bounce off, it's not a matter of 'gee we should call so and so in [the regional centre] and next time they're out we'll have them see this person'.
However not all of the communities were privy to having a local community member as their local palliative care consultant. Some of the consultants worked in more than one community and as a result were only available certain days of the week or via telephone.
Integrative process 2: non-linear nature of development
Participants from the community in Province 1 also noted that despite their efforts, their progress varied in its focus and pace over time through the influence of factors both internal and external to the community. Metaphorically, the growing tree may lose a branch and need to re-grow it. Variations in progress suggest 'seasonal' differences in a tree's existence: spring (rapid growth), summer (stable), fall (decline) and winter (dormant). The emergence of this theme led to revising the model to elaborate that the development of palliative care is non-linear in nature. The non-linear nature of growth was vividly conceptualized by one of the participants:
Sometimes the branches for any number of reasons may die back and you may end up getting a change of person, an increase in funding, which is like getting more light, those things all cause the tree to maybe reshape, or there is some retrenching right now, a change in the process so the tree is being trimmed back and it's going to grow, but the essentials are there with the knowledge and the desire and the community resources are there... You get a palliative care client and you have the tree functions and working and all of a sudden there [are] very few people there. You have a group of people ready to do something that doesn't need to be done at that particular time and then the flow of your client numbers for example will have an effect on your tree and you feel that there is a die back and then all of a sudden the numbers increase and the tree seems to blossom.
Another participant from this same community added that while one part of the tree might experience a stagnant period of growth, other parts might continue to thrive. She explained that the loss of a team member such as a physician may disrupt the clinical care, however, during that same time the volunteer and advocacy functions will continue to move forward with educational initiatives and campaigns. The communities in Province 2 also elaborated on internal and external forces that had an effect on the development of palliative care. These external and internal forces were perceived as both supports and barriers. For instance, locums and new physicians, in particular, international medical graduates, were perceived as barriers to palliative care. Because locums were not familiar with palliative patients or staff, they are often unwilling to prescribe narcotics for pain and symptom management without doing lab work, even if the patients were palliative. For example, a foreign-trained physician had taken over after the retirement of a local physician. His lack of knowledge about palliative care, according to a participant, impeded the delivery of care:
There are other doctors that have come here that may not necessarily be familiar with the way that we even do things in our country you know... but they are culturally different and so sometimes that's a little bit of a barrier...
Physician involvement was regarded as an essential component to have in place in order to deliver palliative care. However, a nurse participant in Province 1 was quick to point out that physician involvement from a distance was also possible but that it required commitment. She recounted a case where the palliative patient was receiving home care and the physician was involved through telemedicine.
Integrative process 3: ongoing nature of catalyst
Internal and external forces contributed to the non-linearity of palliative care development but were also perceived as catalysts to changing the ways in which care was being delivered. As a result, the model was refined whereby experiencing a catalyst could occur on an ongoing basis during all phases of the process. In this regard, the catalyst for change occurs in the community when there is a disruption in their current approach to caring for dying people. The catalyst can be the implementation of palliative care services by the regional health region, as was the case in Province 2.
A participant from Community B conceptualized palliative care development to wax and wane over the course of time and to be rejuvenated by a variety of catalysts over time, thus acting as a feedback loop. She explained that feedback, for example from a family member of a palliative patient, will lead the team to re-evaluate their practices and to make changes to how care is delivered in the future. To help illustrate her point, she used the metaphor of fruit falling from the tree and decomposing to help replenish the soil. In essence, the outcome of the feedback, be it positive or negative, manifests itself as a learning experience which may change how care is delivered from that point onwards.
This study demonstrated that Kelley's model1 is applicable for understanding/explaining and describing/predicting rural community experiences of palliative care program development. The model was validated and further refined as a result of the research, determining a new antecedent condition and 3 additional integrative processes. Communities without antecedent conditions outlined in the model did not develop palliative care programs; therefore, prior to developing palliative care services, attention needs to be given to developing infrastructure, the vision for change, promoting collaborative practice and enhancing community empowerment.
Insight was also gained about the differences between communities that developed palliative care programs and those that did not. These differences elaborate the phase of the catalyst by adding a fourth antecedent condition - a sense of local empowerment and also have implications for regional health authorities which aim to develop local palliative care services in rural communities. Results indicate that successful development is a local, internal community process. This was evidenced by communities who failed to develop a local vision for change when palliative care was implemented by external forces such as through government initiatives rather than by local efforts. Regional programs and consultants can contribute greatly to development if they are incorporated into local processes and accepted by local providers.
In addition to nurturing the numerous antecedent conditions required for the development of palliative care services in rural communities, this research has a number of other implications; these include the recognition that the process through which regionalization of palliative care programs occurs in health regions needs to be responsive to local initiative, resources and culture if it is to build on what exists to support local capacity development. Further, this research suggests that that regional palliative care consultants need to work at becoming 'insiders' to the local processes, focusing on education and support of local providers; and finally, that respecting and supporting local commitment, and vision will empower communities to use available resources and build their own programs. Policy-makers can benefit from understanding the sequential and localized community development process and adopt a method of promoting change to enhance community capacity and not impose solutions from outside. Ultimately, having local palliative programs available in rural communities increases access and quality of care for those who are dying.
The research team will conduct the next phase of the project that will involve applying the conceptual model prospectively over three years as a guideline to developing palliative care in rural communities. This next phase will work with communities using the model as an intervention in rural sites across a number of Canadian provinces.
Acknowledgement
The CIHR ICE grant HOA-80057 entitled 'Timely Access and Seamless Transitions in Rural Palliative/End-of-Life Care' was funded through CIHR Institute of Cancer Research and CIHR Institute of Health Services and Policy Research to A Williams and D Wilson (Co-PIs), and Co-Investigators K Brazil, D Brooks, N Chappell, W Duggleby, R Fainsinger, L Fillion, D Cloutier-Fisher, D Goodridge, C Justice, S Kaasalainen, ML Kelley, K Kovacs-Burns, M MacLean, D Marshall, V Menec, JL Richards, C Ross, A Taniguichi, R Thomas, C Truman and K Willison.
References
1. Kelley ML. Developing rural communities' capacity for palliative care: a conceptual model. Journal of Palliative Care 2007; 23(3): 143-153.
2. Robinson CA, Pesut B, Bottorff JL, Mowry A, Broughton S, Fyles G. Rural palliative care: a comprehensive review. Journal of Palliative Medicine 2009; 12(3): 253-258.
3. Wilson DM, Justice C, Sheps S, Thomas R, Reid P, Leibovici K. Planning and providing end-of-life care in rural areas. Journal of Rural Health 2006; 22: 174-181.
4. Davies E. Higginson IJ. Better palliative care for older people. World Health Organization. (Online) 2004. Available: http://www.euro.who.int/__data/assets/pdf_file/0009/98235/E82933.pdf (Accessed 1 February 2011).
5. Wilson DM, Truman CD, Thomas R, Fainsinger R, Kovacs-Burns K, Froggatt K et al. The rapidly changing location of death in Canada, 1994-2004. Social Science & Medicine 2009; 68: 1752-1758.
6. McMichael T. Human frontiers, environments and disease: past patterns, uncertain futures. Cambridge, UK: Cambridge University Press, 2001.
7. Carstairs S. Still Not There, Quality End-of-Life Care: a progress report. Ottawa, ON. (Online) 2005. Available: http://www.sen.parl.gc.ca/scarstairs/PalliativeCare/Still%20Not%20There%20June%202005.pdf (Accessed 1 February 2011).
8. Phillips JL, Davidson PM, Jackson D, Kristjanson L, Bennet M, Daly J. Enhancing palliative care delivery in a regional community in Australia. Australian Health Review 2006; 30: 370-378.
9. Ministerial Advisory Council on Rural Health. Rural health in rural hands: strategic directions for rural, remote, northern and Aboriginal communities. Ottawa, ON. (Online) 2002. Available: http://dsp-psd.pwgsc.gc.ca/Collection/H39-657-2002E.pdf (Accessed 1 February 2011).
10. Evans R, Stone D, Elwyn G. Organizing palliative care for rural populations: a systematic review of the evidence. Family Practice 2003; 20(3): 304-310.
11. Crooks VA, Schuurman N. Reminder: palliative care is a rural medicine issue. Canadian Journal of Rural Medicine 2008; 13(3): 139-140.
12. Gilbar O, Steiner M. When death comes: where should people die? Hospice Journal 1996; 11(1): 31-49.
13. Romanow RJ. Building on values: the future of health care in Canada. Final report of the commission on the future of health care in Canada. Ottawa, ON. (Online) 2002. Available: http://dsp-psd.pwgsc.gc.ca/Collection/CP32-85-2002E.pdf (Accessed 1 February 2011).
14. McRae S, Caty S, Nelder M, Picard L. Palliative care on Manitoulin Island. Views of family caregivers in remote communities. Canadian Family Physician 2000; 46: 1301-1307.
15. Magilvy JK, Congdon JG. The crisis nature of health care transitions for rural older adults. Public Health Nursing 2000; 17(5): 336-345.
16. du Plessis V, Beshiri R, Bollman RD, Clemenson H. Definitions of Rural. Rural and Small Town Canada Analysis Bulletin 3(3). Cat no 21-006-XIE. Ottawa, ON: Statistics Canada, 2001.
17. Patton, MQ. Qualitative research and evaluation methods, 3rd ed. Thousand Oaks, CA: Sage, 2002.
18. Statistics Canada. 2006 Community Profiles. Ottawa, ON. (Online) 2008. Available: http://www12.statcan.ca/census-recensement/2006/dp-pd/prof/92-591/index.cfm?Lang=E (Accessed 1 February 2011).
19. Google Maps. Canada. (Online) 2009. Available: http://maps.google.ca/maps (Accessed February 1 2011).
20. DeVellis RF. Scale development. Newbury Park, CA: Sage, 1991.
21. Thorne S. Data analysis in qualitative research. Evidenced Based Nursing 2000; 3: 68-70.
22. Carlson ED, Engebretson JC, Chamberlain RM. The evolution of theory: a case study. International Journal of Qualitative Methods 2005; 4(3): 1-17.


