The rural hospital setting is such that the nurse must be proficient in a variety of specialties with only sporadic opportunities for exposure to these specialized patient situations1. Rural nurses often face limited continuing education opportunities, yet they must know how to interface services between hospital and community based-services and must be comfortable navigating rural social structures2. When new graduates are recruited to rural hospitals, they do not always have a large number of peers to turn to for support in decision-making3,4, yet they may be given a preponderance of responsibility within their first year of practice due, in part, to the unique staffing needs of the rural setting.
While the nursing literature is clear regarding the need for supported transition into the role of registered nurse5-11 (RN), there has been little research related to the unique decision-making experiences of novice nurses in the rural setting. Decision-making is not a solitary activity; it is very much a social activity, shaped by what others bring to the situation, as much as by what the novice nurse brings5. This study revealed that rural novice nurses must be able to engage others in order to make effective clinical decisions in their rural settings. This research also points to concerns regarding how evidence based practice (EBP) does, or does not, have a central part in decision-making in rural critical access hospitals (CAH).
Literature review
The ability to make decisions is underscored in definitions of EBP12-18. In addition to needing a strong knowledge background, new graduates are required to integrate available evidence, clinical judgment, and patient preferences as they plan, implement, and evaluate patient care outcomes17.
Many of the studies designed to investigate decision-making in nursing were conducted using simulations and/or paper scenarios in order to observe the processes of decision-making5,19-26. Decision-making in nursing has been studied using frameworks related to levels of expertise26,27, critical thinking28, judgment5,29, and ethics30. There is a gap in the literature, however, relating to the study of decision-making experiences of rural nurses, and in particular rural novice nurses.
Purpose of the study
Because nurses are often the first to triage and begin treatment, especially in rural areas, an understanding of how they make decisions in patient care is important. The purpose of this study was to explore the decision-making experiences of the rural novice RN.
The interview process was guided by two questions:
- What cues were used by novice rural RNs in order to make clinical decisions?
- What were the sources of feedback which influence subsequent decision-making for processing of cues for these novice nurses?
Research design
Corbin and Strauss's31 grounded theory research design was employed, using two theoretical frameworks: Duchscher's role transition theory10 and the 'naturalistic decision making model'32 to guide the process. Naturalistic decision making (NDM) focuses on how individuals experience decision-making in real life settings with attention to contextual factors such as environment, task complexity, and individual characteristics. Since the introduction of NDM in 1989, new models and theories have developed from the NDM paradigm, including 'situation awareness' (SA). The focus in NDM is typically on the proficient decision-maker who uses past experience in the decision-making process; however, even among experts, individual differences have been reported in the way decisions are made23-28,32-34. Because rural novice nurses are indeed in decision-making positions early in their careers4 the NDM model was used as a framework to explore task, person, and environmental factors related to rural novice nurses' decision-making.
Purposeful participant sampling was guided by Duchscher's10 descriptions of novice nurses, who were just beginning to feel comfortable in the role of nurse at 12 months post-orientation. Thus, they had sufficient confidence in their abilities to be able to answer questions and assist others10.
Participant selection
After receiving ethics approval from a large north central university, as well as the researcher's university, letters of participation were obtained from the directors of nursing in potential CAHs in the state who had employed new graduate RNs in the last year. These were filed with both university internal review boards. The directors of nursing from these CAHs facilitated the researcher making contact with the potential novice RN participants, at which point the participants received a letter of invitation to engage in the study. Because orientations lasted approximately 3-4 months at these CAHs, participants who had completed orientation, but who had not yet reached their two-year anniversary of employment, and had not worked as a licensed nurse (RN or licensed practical nurse [LPN]) in any other healthcare setting, were invited. Using this criteria, 12 interested participants, from 9 of the 36 CAHs were available for the study within the state. Prior to commencing interviews or observations, participants reviewed the consent form with the researcher and were offered the opportunity to withdraw their consent at any time.
Data generation
Over a period of 4 months, face-to-face recorded interviews were conducted with 12 novice registered nurses working in a CAH. The interviews lasted from 40 to 60 min. Nine participants consented to observation as well as interview and were shadowed for a period of 1-2 hours, during which further questions were asked. Observations and interviews were transcribed immediately by the researcher after departure from the site. The participants were interviewed a second time to evaluate the emerging categories and themes, which were presented to them as 'concept maps with explanation' as a method of member-checking. Ten of the 12 member-checking visits were conducted face to face during the months of May and June 2010, while two were conducted by phone and email. The participants also communicated via phone and email to answer follow-up questions during the research process.
Data analysis
The coding was accomplished in three phases31: (i) organizational coding, in order to develop broad categories; (ii) axial coding (Fig1), using the in-vivo codes in order to develop a sense of concepts and beliefs from the participants as they developed from the emerging categories; and (iii) selective coding, which represented the concepts as derived from the axial coding and open coding, telling the story of connections between categories.
Organizational coding began with open coding, which consisted of line-by-line analysis of each transcript, with constant comparison to the research questions, the participants' observed actions, transcribed words, and literature.
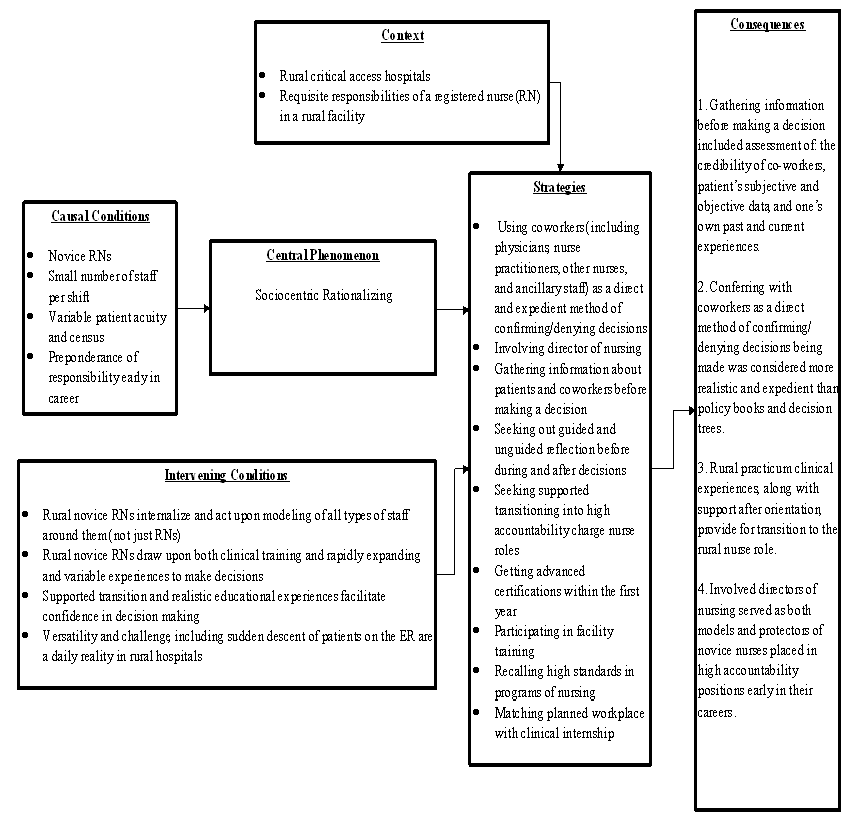
Figure 1: Axial Coding Paradigm. a conceptualization of the central phenomenon (sociocentric rationalizing) as it relates to clinical decision-making in the context of novice nurses in rural critical access hospitals35.
The analysis progressed to organization of the data into emerging categories, which were supported by the process of in-vivo coding. Memos were used throughout the transcripts, using sensitizing questions from the literature and the original research questions. Emerging categories were adjusted as new data was analyzed and as feedback were received during member-checking interviews.
Reformulating these categories, through axial coding, provided a means of inter-connecting the categories in phase 2 of analysis (Fig1). While phase 3 involved building a story that connected the categories through selective coding. Spending time immersed in the data concurrent to analysis contributed to understanding the meaning of the data within the context. This became crucial in making connections between the categories via the axial coding paradigm.
All interpretations in this study were based in a particular moment. That is, they were located in a particular context (the rural CAH) and situation and time (novice RNs with <2 years' experience post-orientation). Therefore, the research process was considered open to re-interpretation and negotiation through conversation. Member-checking was one means of ensuring the story truly belonged to these participants. Without the subjects' analysis of the process and product of the research, perceptions would have been largely subjective and of the researcher's making. Triangulation was employed to facilitate saturation of data and to search for both confirming and negating cases in this study. This included peer review by a trusted nurse colleague experienced in qualitative research, and a professor experienced in qualitative research. Further external checks were provided by rural nurses who were not involved in the study.
The reality for these novice rural nurses was that they were not able to remain on the periphery of decision-making for very long because once orientation was over, they often became the nurse in charge - or at the very least an equal in decision-making. Despite access to a number of resources at their disposal, including policy books, decision trees, standing orders, textbooks, and in some cases internet resources, the 12 novice nurses in this study indicated collaboration with co-workers was their most frequent strategy. The co-workers were not always present in the facility. Frequently, the participants called them on the phone for consult, and in some instances, called them to come in to work. These co-workers were not always other RNs. Participants cited consultation with LPNs, physicians, nurse practitioners, paramedics, nursing assistants, and technicians. Not only did the coworkers help the participants talk through situations and weigh options before making decisions, they were often a source of confirmation or re-direction when the new nurse had made a decision. Although there was, according to the participants, a wealth of social support from their co-workers and supervisors, there was not a formalized or consistent method for reflection on decision-making. Nor was there evidence of a conscientious application of EBP.
Sociocentric rationalizing
The central phenomenon, 'sociocentric rationalizing', was a core category labeled as such because it derived from and linked the categories developed during the open-coding process31. Sociocentric rationalizing (Fig1) refers to the sense of belonging and agency which impacted the decision-making in this small group of novice nurses in rural CAHs. It also illustrates the dominance of the social, rather than evidence based aspect of decision-making found in this study.
Discussion
Consequences with respect to the literature
The central phenomenon is illustrated, with selected excerpts from audiotaped interviews, as it relates to the consequences, which were outcomes of the strategies31 used by participants to manage the social phenomenon of decision-making (Fig1). Documentation of these consequences was supported by observations, analysis of interview transcripts, member-checking, and triangulation activities, including comparison to the literature.
Consequence one: gathering information before making a decision: Gathering information before making a decision included assessment of the credibility of co-workers, the patient's subjective and objective data, and the participant's experience. Knowing the patient in relation to expected patterns of presentation (eg a patient with chest pain, or chronic obstructive pulmonary disease) has been cited as a component of decision-making5,6,26,27. While experienced nurses demonstrate situation awareness by identifying the need to call for help in emergency situations by gathering information from touch, observation, listening, feeling or sensing and knowing26,27, arriving at a point of knowing is a turning point in the transition for the novice nurse10. Participants in this study recounted knowing what normal, versus abnormal, were in terms of vital signs' parameters and expected presentation of specific illnesses.
Meesha: With the elderly - maybe they weren't having trouble at the beginning of the shift, but half-way through they are and if I don't recognize that, then no one else will and they'll get worse. And then I think with the ER [emergency room], you are the first one in there and you get the background and sometimes they'll tell the nurse a little more.
Celeste: I brought this to another nurse: we had this COPD [chronic obstructive pulmonary disease] patient, she was there a while, and it got to the point where she didn't want her Bi-Pap anymore. So, we were trying to wean her off. She got to the point where she was very anxious, you know how COPD patients are.
Jewel: There are decisions I make that I don't consciously make. It's just something you get used to doing, like comfort measures, like hot packs or ice, and assessment of cognitive status. You make decisions about if they are okay or not, and whether to call the physician for something like O2 saturations and blood sugar.
Ally: Depending on what it is - if it's a medication question, I might just look it up. I probably ask people more than I should, but especially to reassure - especially if I think I know something but I don't for sure - I ask people a lot of questions.
These participants also gathered information about the credibility of those they turned to for advice (co-workers, physicians, directors of nurses). Some conceded that they had become selective about the person they sought advice from in a time of need.
Ally: I guess you just have to use your judgment. I guess too, it depends on who the nurse is. I know that isn't very nice.
Lailah: I had a patient one time--a transplant patient - on all the anti-rejection medications. When he came in, he was just shaky and had a cough and fever and wasn't feeling well and in the middle of the night he crashed. He got up to go to the bathroom and he was weak and dizzy. His BP was 70/40. I called the physician assistant and she said, 'Just watch him'. I called the physician assistant and she definitely didn't have the right answer. I probably should have called the doctor, but I didn't know if I should or not.
Eve: I don't know if you noticed, but [the experienced nurse] wanted the ER patient with a right sided weakness to have aspirin right away and I didn't give it. I guess I wanted the doctor to see her because I guess a bleed was in the back of my mind.
Consequence two: conferring with co-workers as a direct method of confirming/denying decisions: Co-workers are a 'more real' (Ally) source of information than policy books and decision trees. These results mirror those of a five-year longitudinal study of the post-entry competency of LPNs and RNs36 which revealed help-seeking from an experienced physician or nurse was typically a first action.
Jewel: If I am wondering about a hospital policy on something I will look in the policy book, but if it a patient situation, a patient concern, I'll go to the nurse I am working with.
The fact that most participants cited their nurse co-workers as a source of information was not surprising, but these novice nurses did not limit their source for cues to other nurses. Physicians, directors of nursing and unlicensed assistive personnel, including paramedics, certified nursing assistants (CNAs) and ancillary staff played a part as well.
Meesha: I look at the whole clinical picture, what the assessment findings are, what the labs are. There is not just one resource. I find myself looking at labs and then thinking, 'Do their lungs sound better today and how do their labs look?' I also think I have great resources in the staff I work with. We can always talk things out - even with the nursing assistants that have worked there 30 years.
Hannah: Linda is a great nurse. She's been here a long time. She'll come in and check out the patient, after I do and then together we decide if we should call the doctor.
While participants described careful consideration before calling the physician about patients, they also reported comfort with calling their physicians. Some commented that they knew this was not the case at larger facilities.
Isabel: I can call the doctor. In a rural community they're all really friendly and so I'm not really intimidated by them like you see some places. Of course they have their moments but everyone does.
Sarah: Everybody is willing to answer questions. They say there's no stupid question. I would argue there is, but they don't mind answering a question or showing you - even the providers - and the doctors, if you haven't done it, they understand that.
All the novice rural nurses gave examples of the help they sought from co-workers. The more costly and hazardous the possible mistakes, the heavier the reliance on observational learning from competent examples37. Asking others is an expectation when one is new, and especially when one is new in a healthcare setting; however, rural settings are uniquely tied to a sense of community38 in which practice is imbedded in belonging39.
Consequence three: rural practicum and support after orientation provide for transition: Participation in a rural nurse residency program has been attributed to increased retention of novice RNs1,4,40. While none of the study participants were in a formal residency, more than half had done a practicum in their senior semester or an internship prior to graduation at a rural hospital and reported they believed it to have been most helpful. Those who had chosen other areas for practicum expressed regret.
Isabel: I think a rural clinical would have been helpful. It's totally different than at a bigger hospital.
Sarah: Well, doing an internship in a rural hospital would help. I did mine in an ER, and I would say that, too, was very beneficial, because really, we are like a big ER. Anything can and does come in and you have to be organized. I learned about prioritizing.
Arial: A rural practicum would have been helpful. Like when I thought of working at a small hospital, I thought, 'Oh that's boring, there's nothing going on'. But on the other hand it's crazy. It's different than how I pictured working in a rural place.
The variable nature of patient acuity and census, along with the staffing ratios in rural health care, means that situations arise in which rural nurses must possess a high level of self-confidence and competence40. Even with a practicum or internship experience, participants identified the social support and thorough orientation as integral to their transition into higher level decision-making roles, such as charge nurse: 'I will not sign off to be charge until I feel ready - and that is okay here' (Hannah).
Grace: [Mary] is the main reason I'm still here. I tell her that. She just had a good attitude. She was welcoming. She helped me through orientation.
Jewel: If I need help, they don't have any problem helping me. And if they have something to show me, they do. If there is something they think would be interesting for me, they call me. I love that.
Meesha: Everyone is very willing to help out. I've never felt stupid if I had a question - if I was unsure of something that they wanted. If I said, 'Now why'd you do this?' they would help me learn.
Discussions with both directors of nursing and participants revealed the pitfalls to unsupported transition into higher accountability roles in rural hospitals where belonging has been described as central to the success of the individual nurse39.
Arial: When I started, I was told, 'Oh you'll have two months of orientation and this and that'. I didn't get all the orientation I was supposed to get and I just felt lost - just nervous all the time. I think if they didn't have the ER here, I'd be fine.
Some of the directors of nursing described methods to facilitate transition: availability of experienced staff on call; extra orientation to specialty areas (eg ER, intensive care, and labor and delivery); and advanced certification courses. The examples of supported decision-making given by these participants related to the 'social imbeddedness' of situated learning41,42. The necessity of appropriate support for transition to increased responsibility is well documented43-46. Without the collaboration of co-workers, and support of their directors of nursing, it was unlikely these novice nurses would continue to believe in their abilities, even if they had arrived to the workplace with a great deal of confidence.
Consequence four: involved directors of nursing served as both models and protectors: Involved directors of nursing served as both models and protectors of novices who were placed in high-accountability positions early in their career. The degree to which participants discussed interaction with their directors of nursing indicated the novices' comfort with asking for help from a nurse in a leadership position. The directors of nursing in these rural facilities were visible, according to participants, and this was verified by the researcher's observations. This is not necessarily the case in urban hospitals, where the director's function may be more supervisory than participative. With the exception of 'Arial', who was without a director of nursing for a period of time, participants described communications with their director regarding issues ranging from readiness to take on more responsibility to 'arrangement for debriefing of a critical event in the emergency room' (Celeste).
Sarah: We had a patient come in to the ER with a blood sugar of 1000. She wasn't responsive. The nurse I was working with was someone who thinks it is, sink or swim. So, she says, 'Well you're the charge nurse; you're supposed to know what to do, so do it.' At one point the doctor said he wanted some Kayexalate and I asked her where it was. She said, 'What?! You should know that by now.' I called [our director of nursing] and she came down right away. She helped me a lot.
Grace: The director of nursing wants to see me succeed. That is a good feeling. She's really helped me. She'll print things out and say, 'Here is a way to approach this'. If there is a decision to make, she'll let me make it and then we'll talk about it, or she'll say, 'This is how I would do this and next time this comes up, you can handle it'.
Meesha: A big part of my transition was my relationship with our director of nursing. She's really helped me develop my decision-making skills. She isn't afraid to say, 'You did this great, next time maybe we can try this or that.' I have a lot of trust in her. I'm never scared to call her in for help or questions.
Lailah: When the doctor came in the next morning, after I was gone, he wondered why he hadn't been called. I went in and visited with my director later, who basically told me, 'If you don't like the answer you get when you call, you can go above them. We have a policy written for that.' I think even her just telling me I did things well, even though I was scared to death, just verified in my mind that I can handle things.
Leadership is key to that process, because the most influential factor in whether workers feel valued and respected at work is their relationship with their supervisors47. One rural nursing director commented, after reviewing the axial coding paradigm with explanation from the researcher:
This only reinforces the fact that we need to be careful with our new nurses. This job is hard - it can be rewarding - but this confirms I need to remain alert to how orientation is going.
The central phenomenon was labeled 'sociocentric rationalization' upon consideration of the data, member-checking activities, and the literature. It was revealed that clinical knowledge in these rural settings was indeed socially embedded6 and that social context played a pivotal part in the transition of novice nurses to rural settings39,48. This research points to concerns, however, regarding how EBP does or does not play a central part in decision-making in rural CAHs. Specifically, reference to hospital policies, decision trees, literature, or even the phrase 'evidence based practice' was blatantly absent in the participants' discussions related to their clinical decision-making.
Efficacious decision-making relies heavily on what nurses know about a patient, the nurse's ability to engage a patient in discussion about his/her needs, and the nurse's ability to engage others6,26,42. For these participants, the ability to engage others was especially crucial and well demonstrated. They verbalized and demonstrated during observations the exchange of information between several health care disciplines, not just senior nurses with whom they worked. Although participants in this study demonstrated being at a point of knowing10 as they paid attention to cues gathered from the patient, such as vital signs, and cues from their own intuition (eg 'he didn't look right'), these nurses still recounted the necessity to engage others, including their directors of nursing. When they did so, there was not clear evidence that reflection on EBP was taking place; rather, the novice nurses verbalized relying on co-workers' opinions and judgments.
Naturalistic decision making focuses on the impact of context in decision-making. One of the main assertions of this theory is that decision-making is so contextual that 'rules of thumb' or decision trees cannot be easily applied to complex situations32. In addition, the more high stakes the decision (such as in emergencies), the less reliable cue recognition may be, because even experts tend to rely on others to make decisions in those situations26,32,37,41,42,49. In rural health care, where the patient census and patient acuity is highly variable, development of expertise in terms of recognizing familiar patterns and cues for similar patient situations may come at a different rate than in an urban center where a nurse works with a specific patient population. Therefore, recognizing the need to collaborate and engage others for the benefit of the patient was a necessity for these nurses.
While research using NDM models has largely focused on experts, it is important to understand the decision-making of the novice nurse - especially in a rural setting, where resources are different from the urban setting. Recent studies designed around the NDM model have shown knowledge management and shared decision-making to be particularly important factors for nurse decision making26,50.
The reality for these 12 nurses was one of general social support and mentoring in decision-making, without benefit of a formalized and consistent method to examine actions and outcomes in order to increase clinical knowledge and a capacity for clinical decision-making toward EBP. The results of this small qualitative study extend the findings of a larger national study36 in which peers, rather than EBP, was the first resource for decision-making.
Standard orientation and residency programs in rural areas have not begun to meet the needs of new graduates4,40. This study suggests a need to further investigate how the contextual factors (the social and emotional climate) of rural hospitals may be utilized in order to meet the needs of graduate nurses. While this small study indicated socialization was, by and large, positive and the novice nurses felt welcomed, it also revealed the participants to be somewhat afloat and very dependent on word of mouth rather than EBP in decision-making. ''One orientation plan fits all'' is no longer an appropriate response, particularly in rural settings40. Through support and mentoring, situational learning must be fostered, in order to 'cultivate the curious, creative, reflective minds of point-of-care nurses'51 as the novice nurse moves from legitimate peripheral participation in a junior partner role, to that of an experienced individual with increased responsibilities in the rural setting42.
References
1. Squires A. New graduate orientation in the rural community hospital. The Journal of Continuing Education in Nursing 2002; 33(5): 203-209.
2. National Rural Health Association. Recruitment and retention of a quality health workforce in rural areas. A series of policy papers on the rural health careers pipeline. Number 2: Nursing. Issue Paper. (Online) 2005. Available: http://www.ruralhealthweb.org/go/left/policy-and-advocacy/policy-documents-and-statements/official-policy-positions (Accessed 8 July 2010).
3. Nayda R, Cheri J. From enrolled nurse to registered nurse in the rural setting: the graduate nurse experience. Rural and Remote Health 8: 900. (Online) 2008. Available: www.rrh.org.au (Accessed 8 July 2010).
4. Molinari D, Monserud M, Hudzinski D. A new type of rural nurse residency. The Journal of Continuing Education in Nursing 2008; 39(1): 42-46.
5. Tanner CA. Thinking like a nurse: a research-based model of clinical judgment in nursing. Journal of Nursing Education 2006; 45: 204-211.
6. Benner P, Tanner C, Chelsa C. Expertise in nursing practice. Caring, clinical judgment, and ethics, 2nd edn. New York: Springer, 2009.
7. Duchscher J. Out in the real world: Newly graduated nurses in acute-care speak out. Journal of Nursing Administration 2001; 31(9): 426-439.
8. Duchscher J. Critical thinking: Perceptions of newly graduated female baccalaureate nurses. Journal of Nursing Education 2003; 42(1): 1-12.
9. Duchscher J. Transition shock: the initial stage of role adaptation for newly graduated Registered Nurses. (Online) 2008. Journal of Advanced Nursing, 1-11. doi: 10.1111/j.1365-2648.2008.04898.x Available: http://www.letthelearningbegin.com/documents/pdfs/shock.pdf (Accessed 8 July 2010).
10. Duchscher J. A process of becoming: the stages of new nursing graduate professional role transition. The Journal of Continuing Education in Nursing 2008; 39(10): 441-450.
11. Duchscher J, Myrick F. The prevailing winds of oppression: uUnderstanding the new graduate experience in acute care. Nursing Forum 2008; 43(4): 191-206.
12. Polit D, Beck C. Essentials of nursing research: methods, appraisal, and utilization, 6th edn. Philadelphia, PA: Lippincott Williams Wilkins, 2006.
13. Ritter B. Considering evidence-based practice. The Nurse Practitioner 2001; 26(5): 63-65.
14. Rycroft-Malone J, Seers K, Titchen A, Harvey G, Kitson A, McCormack B. What counts as evidenced-based practice? Journal of Advanced Nursing 2004; 47(1): 81-90.
15. Sackett D, Rosenberg W, Gray J, Haynes R, Richardson W. Evidenced?based medicine: what it is and what it isn't. Clinical Orthopaedics Related Research 2007; 455: 3-5.
16. Sigma Theta Tau International. Sigma Theta Tau position statement on evidence-based practice February 2007 summary. World Views on Evidenced-Based Practice 2008; 5(2): 57-59.
17. American Association of Colleges of Nursing (AACN). The essentials of baccalaureate education for professional practice. (Online) 2008. Available: http://www.aacn.nche.edu/Education/pdf/BaccEssentials08.pdf (Accessed 8 July 2010).
18. Anderson J, Wilson P. Clinical decision support systems in nursing. Synthesis of the science for evidenced-based practice. Computers, Informatics, Nursing 2008; 26(3): 151-158.
19. Choate K, Barbetti J, Currey J. Tracheostomy decannulation failure rate following critical illness: a prospective descriptive study. Australian Critical Care 2009; 22: 8-15.
20. Rashotte J, Carenvale F. Medical and nursing clinical decision making: a comparative epistemological analysis. Nursing Philosophy 2004; 5: 160-174.
21. Thompson C, Dowding D. Decision-making and judgement in nursing. Churchhill Livingstone, 2002.
22. Thompson C, Bucknall T, Estabrooks C, Hutchinson A, Fraser K, DeVos R et al. Nurses' critical event risk assessment: a judgment analysis. Journal of Clinical Nursing 2007; 18: 601-612.
23. Chin E, Sosa ME, O'Neill ES. The N-CODES project moves to user testing. Computers, Informatics, Nursing 2006; 24(4): 214-219.
24. Anderson J, Wilson P. Clinical decision support systems in nursing. Synthesis of the science for evidenced-based practice. Computers, Informatics, Nursing 2008; 26(3): 151-158.
25. O'Neill ES, Dluhy NM, Hansen A, Ryan JR. Coupling the N-Codes system with actual nurse decision-making. Computers, Informatics, Nursing 2006; 24(1): 28-34.
26. Cioffi J. A study of the use of past experiences in clinical decision-making in emergency situations. International Journal of Nursing Studies 2001; 38(5): 591-599.
27. Benner P, Tanner CA. Clinical judgment: how expert nurses use intuition. American Journal of Nursing 1987; 87: 23-43.
28. del Bueno D. A crisis in critical thinking. Nursing Education Perspectives 2005; 26(5): 278-282.
29. McCarthy M. Situated clinical reasoning: distinguishing acute confusion from dementia in hospitalized older adults. Research in Nursing and Health 2003; 26: 90-101.
30. Greipp ME. Greipps model of ethical decision making. Journal of Advanced Nursing 1992; 17(6): 734-737.
31. 32. Corbin J, Strauss A. Basics of qualitative research. Techniques and procedures for developing grounded theory, 3rd edn. Thousand Oaks, CA: Sage, 2008.
32. Zsambok CE, Klein G (Eds). Naturalistic decision making. (1997). New York: Routledge, 2009.
33. Oliver M. The cultural-ecological orientation of graduate nurses (novice) in medical-surgical nursing. International Journal of Nursing Practice 2007; 14: 342-346.
34. Offredy M, Kendall S, Goodman C. The use of cognitive continuum theory and patient scenarios to explore nurse prescribers' pharmacologic knowledge and decision-making. International Journal of Nursing Studies 2008; 45(6): 855-868.
35. Seright T. Clinical decision making of rural novice nurses. (Doctoral dissertation). University of North Dakota, Grand Forks, 2010.
36. National Council of State Boards of Nursing. Report of findings from the post-entry competence study. (Research brief, vol 38). Chicago: NCSB, 2009.
37. Bandura A. Social learning theory. Englewood Cliffs, NJ: Prentice Hall, 1977.
38. Bales R, Winters C, Lee H. Health needs and perceptions of rural persons. In: HJ Lee, CA Winters (Eds). Rural nursing: concepts, theory, and practice, 2nd ed. New York, NY: Springer, 2006; 53-65.
39. Sedgwick M, Yonge O. 'We're it', 'We're a team', 'We're family' means a sense of belonging. Rural and Remote Health 8: 1021. (Online) 2008. Available: www.rrh.org.au (Accessed 8 July 2011).
40. Keahey S. Against the odds. Orienting and retaining rural nurses. Journal for Nurses in Staff Development 2008; 24(2): E15-E20.
41. Lave J, Wenger E. Situated learning. Legitimate peripheral participation. New York: Cambridge University Press, 1991.
42. Gillespie M, Paterson B. Helping novice nurses make effective clinical decision: the Situated clinical decision-making framework. Nursing Education Perspectives 2009; 30(3): 164-170.
43. McKenna BG, Smith NA, Poole SJ, Coverdale JH. Horizontal violence: experiences of registered nurses in their first year of practice. Journal of Advanced Nursing 2003; 42(1): 90-96.
44. Schmalenberg C. Kramer M. Clinical units with the healthiest work environments. Critical Care Nurse 2008; 28(3): 65-77.
45. Simons S. Workplace bullying experienced by Massachusetts registered nurses and the relation of intention to leave the organization. Advanced Nursing Science 2008; 31(2): 48-59.
46. Schoessler M, Waldo M. First 18 months in practice: a developmental transition model for the newly graduated nurse. Journal for Nurses in Staff Development 2006; 22(2): 47-52.
47. McGilton K. Development and psychometric testing of the supportive supervisory scale. Journal of Nursing Scholarship 2010; 42(2): 223-332.
48. Sedwich MG, Rougeau J. Points of tension: A qualitative descriptive study of significant events that influence undergraduate nursing students' sense of belonging. Rural and Remote Health 10:1569. (Online) 2010. Available: www.rrh.org.au (Accessed 8 July 2011).
49. Benner P. From novice to expert: excellence and power in clinical nursing practice. Menlo Park, CA: Addison-Wesley, 1984.
50. Gazarian PK. Nurse decision-making and the prevention of adverse events. (Doctoral dissertation). University of Massachusetts Amherst, 2008.
51. Schultz A. The Clinical Scholar Program: creating a culture of excellence. Reflections on Nursing Leadership. (Online) 2008; 34(2). Available: http://www.reflectionsonnursingleadership.org/pages/home.aspx (Accessed 8 July 2011).
