Cardiovascular disease (including coronary heart disease, stroke, and heart failure) remains the leading cause of hospital admission and death in the USA, and elsewhere around the globe1. The risk factors for cardiovascular disease include hypertension and type 2 diabetes mellitus - conditions that commonly occur together2. And, while effective (and cost-effective) treatments exist for these risk factors, in the USA as many as 22% of people with hypertension and 30% of the people with diabetes may be unaware of their condition1.
Given this gap between current knowledge of cardiovascular risk factors and the ability to treat them on the one hand, and the actual level of diagnosis and treatment on the other, it is not surprising that improved cardiovascular risk screening is a central theme of many efforts to reduce the burden of this disease. The American Heart Association recommends that all asymptomatic adults receive a global cardiovascular risk screening (which includes the measurement of blood pressure [BP] and may also include the measurement of blood glucose) from their primary care provider3. Similarly, the US Preventive Services Task Force recommends BP screening by a primary care provider for all adults over 18 years of age4, and diabetes screening for adults with BP of greater than 135/805. These recommendations are supported by the US Department of Health and Human Services, which has made increasing the proportion of adults who have had their BP measured within the preceding 2 years and increasing the proportion of adults with diabetes whose condition has been diagnosed, two objectives of their 'Healthy People 2020' initiative6.
Rural areas continue to be plagued by shortages of primary care providers7 at a time when those living in non-metropolitan areas are more likely to suffer from diabetes, heart disease, and stroke (and to be uninsured) compared with urban dwellers8. This suggests that disease screening programs that do not make direct use of primary care physicians may be useful in rural areas. Thus, the US Department of Health and Human Services Healthy People 2020 objective of increasing the number of community-based organizations providing population-based primary prevention chronic disease prevention services6 may be of particular importance to those who live in rural areas.
Community-based organizations that wish to implement a cardiovascular disease risk factor screening program targeting rural populations need to make decisions about where and when to provide screening services to optimize the return on scarce resources. This article reports the experience of a BP and blood glucose screening program that screened more than 2450 Maine, USA residents at different types of community events in many different locations, including agricultural fairs, over a 4 year period. The results include a Geographic Information Systems (GIS) based analysis of: (i) the impact of rurality of residence on the risk factor prevalence of those screened; (ii) the impact of the type of community event and the rurality of the location of the event on the rurality of the residences of those screened; and (iii) the rurality distribution of those screened compared with that of the Maine population in general. These results allow conclusions to be drawn about the how decisions on screening locations affect the ability of the program to meet its goal of providing services to rural Maine residents. This may be of interest to others who are designing chronic disease screening programs to provide services to rural populations.
Research questions
In this correlational study, answers the following questions were sought:
- Are those screened more likely to live in rural areas compared with Maine residents in general?
- Among those screened, do rural residents have a different risk of hypertension or diabetes compared with non-rural Mainers?
- What characteristics of a community event predict that a screening conducted at that event will reach a high fraction of rural residents?
Setting and program
With an area of approximately 49890 km2 (31 000 miles2) and an approximate population of 1.3 million, including 546 000 who live in rural areas9, Maine is a place where access to primary medical care, including chronic disease screening, can be suboptimal10. Because it also has some urban areas (although they are small by national standards), Maine is also an interesting place to study the impact of chronic disease risk factor screening location on the rurality of residence of those screened.
The Maine Elks Association, a fraternal service organization11, and the Maine State Grange, a rural community service organization that focuses on agricultural issues12, have been working together under the leadership of a nurse practitioner since 2006 to run a mobile BP and blood glucose screening program in a specially equipped van. In this program, which has been described in detail elsewhere13, the van visits community and workplace events, including agricultural fairs, and administers voluntary screenings free of charge to anyone who desires to participate. During the summers of the period 2006-2009 the van visited many different types of events and screened all who wished to participate. However, its expressed purpose was to bring screening services to rural Maine residents.
Data collection
Van personnel determined BP with an automatic cuff (Welch Allyn, model CE0050-Ref#420; Skaneateles Falls, NY, USA) and blood glucose with a glucometer (Accu-Chek, 'compact' model; Roche Diagnostics; www.accu-chek.com). The values were supplied to the screenee on a card, and also recorded in a log, along with the screenee's name and town of residence, and the name of the event at which the screening took place. Later, this information was transferred to an electronic spread sheet for analysis. All screenees were advised to bring their cards to their next primary care health visit. Those with elevated values were told that their results were considered abnormal and advised to contact a primary care provider. They also received telephonic follow up at which they were reminded of their abnormal results and again advised to contact a primary care provider, although in some instances this follow up may not have occurred until the end of the summer 'fair season'.
Screenee names were removed from the project spread sheet to meet the requirements of the University of Southern Maine Institutional Review Board (which approved this protocol). Screenees who did not live in Maine were removed and fields were added for the town in which each screening took place, the hypertension status, and the diabetes status of each individual screened. Systolic BP of 140 mmHg or greater, or diastolic BP of 90 mmHg or greater was considered evidence of hypertension and systolic BP 120 to 139mm Hg or diastolic BP 80 to 89 mmHg was considered to be pre-hypertension in accordance with the Joint national committee (JNC) VII guidelines2. Blood glucose of 140-199 mg/dL was defined as pre-diabetes and a casual blood glucose of 200 mg/dL or higher was defined as evidence of diabetes, in keeping with current American Diabetes Association definitions14.
GIS construction
Map files of Maine's zip codes from the US Census Bureau15 and a table with the Rural Urban Commuting Area Codes (RUCA) of each zip code from the Rural Health Research Center16 were obtained. By joining these in a GIS environment (ArcGIS 9-ESRI; Redland, CA, USA), a map was created of Maine's zip codes with RUCA codes. This study chose RUCA codes over other systems for defining rurality because these codes allow analysis on a finer geographic scale (sub-county) and consider how the residents of an area live, in addition to more standard metrics of rurality such as population density and remoteness17. Also obtained were a map file of Maine's towns and a table with 2000 US Census data from the Maine Office of GIS18. Joining these produced a map of Maine's towns with population for each. The rurality map was joined to the towns map to assign a RUCA code to each town. This is reasonable in Maine because very few towns have more than one zip code. Finally, the project spreadsheet was imported into the GIS environment and executed joins based on town name to add a RUCA code field for the residence town of each screenee and the town location at which the screening took place. Also used was the GIS point-to-point distance function to compute the linear distance between the centroid of the town of residence and centroid of the town where the screening took place for each screenee. Then this table was exported for further analysis.
Data analysis
The RUCA codes consist of a 1-10 rating system of primary codes indicating increasing rurality with secondary codes that provide a more nuanced description of each location. The primary and secondary RUCA codes are organized into a 4 tier system that defines the following categories: urban core, sub-urban, large rural town, and small town/ isolated rural, as previously defined19. This system was adopted because it makes use of the secondary RUCA codes and produces a number of categories appropriate for this data set, and a rurality category was assigned to each screenee residence location and screening location. The resulting spreadsheet was input into an MS Access (2007) database.
The database was used to assemble the following:
- Distribution of screenees and the Maine population in general into rurality categories by residence. The distribution for screenees versus that for Maine residents was compared across residence rurality category by χ2 test.
- Lists of BP (systolic and diastolic) and blood glucose for each screenee residence location rurality category. These data were tested for normality and equal variances, and compared the mean BP and blood glucose values across screenee residence rurality category by ANOVA.
- Distribution of screenees into hypertension and diabetes categories for each screenee residence location rurality category. These distributions were compared across screenee residence rurality category by χ2 test.
- Numbers of screenings (categorized by the rurality of the screenees' residences) that took place at agricultural fairs (vs other types of events), and the numbers of screenings that occurred at events grouped by the rurality category of the event location. Using analysis by regression with categorical variables, it was determined if type of event or rurality of event location (independent variables) predicted the rurality of residence of the people screened at that event (dependent variable).
- Lists of distances screenees traveled from their town of residence to the screening location for each screenee residence location category. These data were tested for normality and equal variances, and the mean distances compared by Kruskal-Wallis test because the values were not normally distributed.
Statistical analysis was performed in SAS (www.sas.com) and Minitab (www.minitab.com). Significance was accepted at p<0.05.
Description of screenees and comparison to all Maine residents
Over the 4 year period of this study (2006-2009) 2451 Maine residents with residences in 254 different towns (Fig1) were screened by the van at 42 events located in 28 different towns (Fig2). The screenees' residence locations and the screening locations were distributed across areas that fall into different rurality categories (Fig3) with the largest number of screenees (42%) living in large rural towns (Table 1).
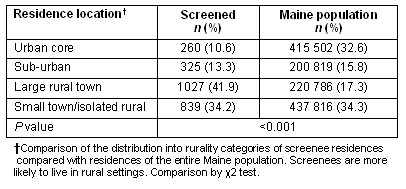
Of the Maine residents screened, 2420 were screened for hypertension and 2372 for diabetes. The distribution of residences for screenees was significantly more rural compared with that of Maine residents in general (p<0.001), and 76% of screenees lived in isolated rural areas/ small rural towns or large rural towns compared with 51% of Maine residents (Table 1).
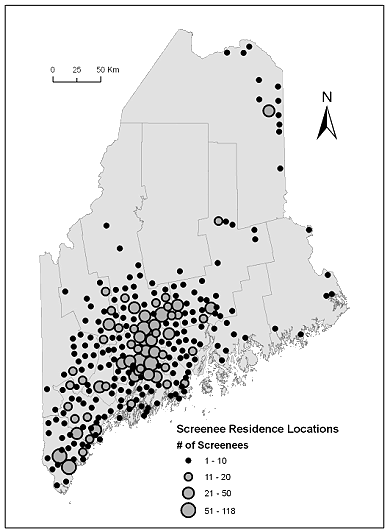
Figure 1: Map of the state of Maine with county lines shown for reference. Screenee residence locations (n=254 towns) are symbolized by the number of screenees living in each town.
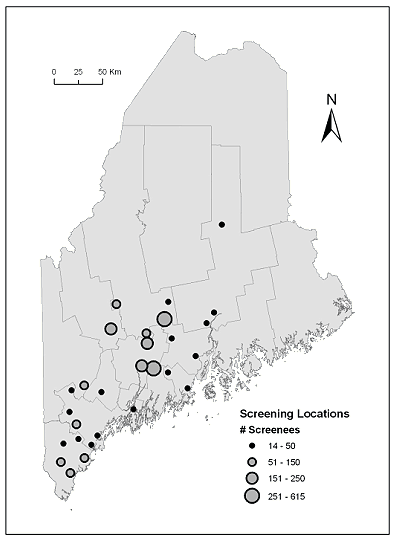
Figure 2: Map of the state of Maine with county lines shown for reference. Screening locations (n=28 towns) are symbolized by the number of screenings conducted at each location.
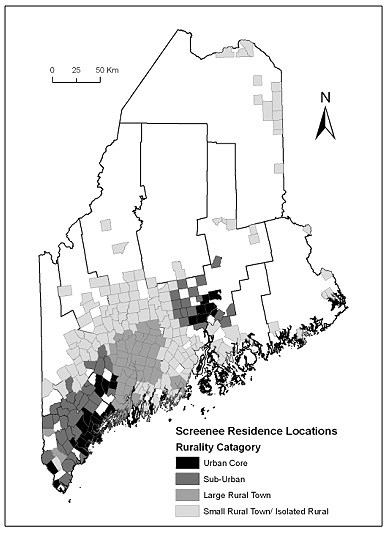
Figure 3: Map of the state of Maine with county lines shown for reference. Screenee residence locations with town lines (n=254 towns) are symbolized by the rurality category of each town.
Table 1: Comparison of screenees with Maine population by rurality of residence
Hypertension and diabetes among screenees
Mean systolic blood pressures differed significantly for screenees whose residences were in different rurality categories (p=0.001). Those living in large rural towns had, on average, systolic blood pressures that were 2.5 mmHg higher than those living in the suburbs and 4 mmHg higher than those living in urban areas (Table 2). However, neither screenees mean diastolic BP (Table 2) nor their blood glucose (Table 3) varied significantly by rurality of residence.
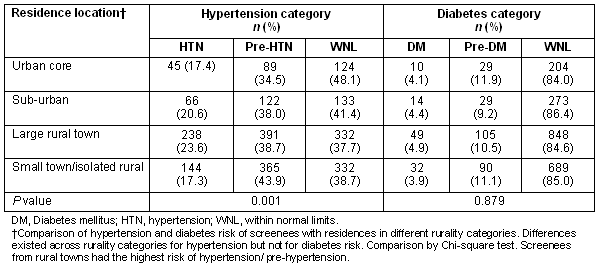
The distribution of screenees into hypertension categories varied significantly by rurality of residence (p=0.001) with 62% of large rural town residents and 61% of those living in small rural towns/ isolated rural areas either pre-hypertensive or hypertensive while 52% of screenees for urban areas had blood pressures fell into these abnormal categories (Table 4). The distribution of screenees into diabetes categories did not vary significantly by rurality of residence (Table 4). These results show that, among the screened population, those who live in large rural towns are at higher risk for hypertension than those from more urban areas.
Table 2: Blood pressure by rurality of screenee residence
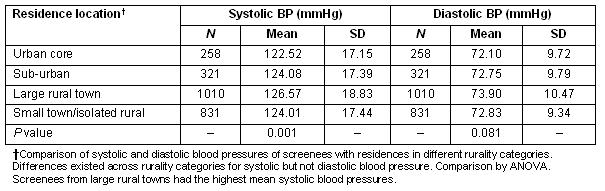
Table 3: Blood glucose by rurality of screenee residence
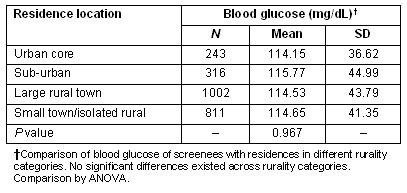
Table 4: Hypertension and diabetes by rurality of screenee residence
Predictors that a screening event will attract rural Mainers
In analysis by regression with categorical variables, the type of event at which the screening took place (agricultural fair vs other; p=0.003) and the rurality of the event location (p=0.001) both independently predicted the rurality of residence of those screened. Agricultural fairs and screenings located in rural areas preferentially attracted residence of rural areas. The fraction of rural-dwellers screened at agricultural fairs was nearly twice the fraction of urban/ suburban dwellers screened at these events and virtually all (>95%) of those living in rural areas were screened at rural locations (Table 5).
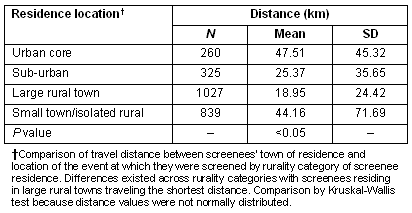
It was also found that the distance screenees traveled to the event at which they were screened varied by the rurality of residence of the screenees (p<0.05). Screenees from large rural towns traveled, on average, less than 20 km, while those from urban areas and those from small rural towns/ isolated rural areas traveled over twice this distance (Table 6). Both the locations of the screening events and the behavior of screenees could influence this result.
Table 5: Screening location by rurality of screenee residence
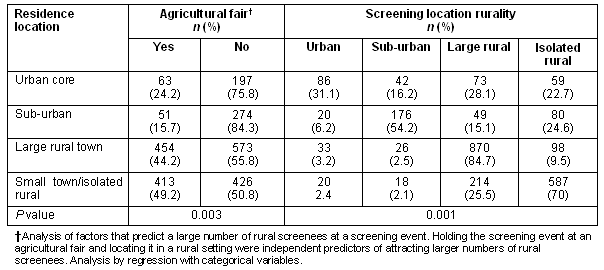
Table 6: Distance traveled to screening by rurality of screenee residence
Discussion
Targeting screening events to rural populations
Cardiovascular disease risk factor screening programs have been conducted in many different venues including fire stations20, pharmacies21, veterans administration hospitals22, community events23, workplaces24, and health fairs25. Some programs took advantage of several types of venues26. However, to the best of the authors' knowledge, this is the first report of cardiovascular risk factor screenings conducted at a wide range of events and, preferentially, at agricultural fairs. It was found that the screenees' residences were significantly more rural than the residences of Maine residents in general (Table 1). This suggests that the van program was indeed successful in its goal of bringing chronic disease screening to rural Mainers. It was also found that rural residents are more likely to be screened at events that are: (i) agricultural fairs; and (ii) located in rural areas (Table 5). This suggests that both the location and the type of event where a screening takes place can be used to target residents of rural areas.
In this study van screenings were preferentially conducted at agricultural fairs and in rural areas as a way of attracting rural Maine residents, and this was found to be effective. The idea of holding screenings in a setting where a target population congregates is similar to the approach of holding cardiovascular disease risk factor and diabetes screenings at churches to bring services to rural southern African Americans. This was found effective at identifying screenees with undiagnosed risk factors, although the educational aspect of the program did not produce significant increases in disease-specific knowledge27. A similar approach in a rural Georgia church demonstrated the feasibility of delivering a more in-depth (6 session) diabetes prevention program28. However, a rural North Carolina church-based program also identified the importance of ongoing support if a risk factor modification program is to have a lasting impact29.
The concept that the screening event should be held in a location that is similar to, and not too distant from, the area of residence of the target population has also proven effective before at reaching a population that is even more geographically isolated than rural Mainers. A cardiovascular disease risk factor screening program that brought services to the residents of an isolated island community off the coast of Maryland is an extreme example of this practice30. The lesson of these studies, and of the results reported here, is simple: to conduct a successful targeted cardiovascular disease risk factor screening program, go to the location of your target population - both geographically and culturally. Do not expect your target population to come to you.
Level of cardiovascular disease risk factors among rural populations
It is estimated that one-third of US adults have hypertension and one-tenth have diabetes1. Maine's cardiovascular disease death rate is 15% lower than the national average1; however, the prevalence of diabetes is known to be higher among rural than among urban dwellers31, and those who live in rural areas are considered to have high vulnerability to cardiovascular disease8. Rural residents commonly travel longer distances to obtain medical care than their urban counterparts32 and in Maine a longer travel distance to primary care is associated with a more advanced stage of colorectal cancer at diagnosis33. Thus, the goal of the program described here (to bring health screening to rural Mainers) is in general alignment with proposals that new approaches to cardiovascular disease risk factor management are needed for rural populations34.
Cardiovascular disease risk factor screening events report finding varying levels of risk factors. For instance, a workplace screening at a salami factory found that 25% of the workers screened had hypertension while a CDC-run community screening program found 75% of screenees either hypertensive or at risk for hypertension and 22% either diabetic or at risk for diabetes26, a pharmacy-based program found that 26% of those screened for blood glucose had elevated values, a Michigan community-based diabetes screening program found that 5% of screenees had elevated fasting blood glucose values35, and at a Nebraska screening program for poor women 6% had hyperglycemia and 10% had hypertension at their initial visit36.
In the results reported here, 20% of the screened population was hypertensive and an additional 40% was classified as having pre-hypertension; 4.4% had blood glucose levels consistent with diabetes while an additional 10.7% had values consistent with pre-diabetes (Table 4). Thus, the present findings are in general agreement with previous studies showing that community screening find a relatively high prevalence of risk factors. It was found that, in the population of people screened for this study, those who live in large rural towns are at higher risk for hypertension than those from more urban areas. This suggests that targeting a hypertension screening program to rural residents, as the van project does, is a reasonable approach for a community-based screening program.
Study limitations
This study has several limitations. First, because the van visited only events to which it was invited and screened only those who presented for screening, the populations of screenees are not random samples of the residents of the rurality categories in which they reside and screening sites were not randomly distributed around the state. For instance, the low levels of abnormal BP values among screenees who reside in urban areas may not reflect a lower level of this risk factor among Maine urban-dwellers in general. Rather, the long distance that urban-dwellers traveled to the events where they were screened (Table 6), suggests that these program participants almost certainly had access to a car, and this may indicate that urban screenees had a higher income than other urban-dwellers. Further, the lack of screening locations in northern Maine (Fig2) may have limited the access of residents from that area to screenings. However, some residents of northern Maine did attend screenings (Fig1) and the distribution of screenee residence locations (most in the southern half of the state with smaller numbers in 'Down East Maine' and along the northern cap of the state) approximate the population distribution of Maine resident in general. Most importantly, these results do show that the van program was successful in reaching a rural population with a high level of risk factors.
The results also do not include information about the total number of participants at the events where screenings were offered, so it is not possible to report acceptance rates. Nor do the results allow ruling out a small number of repeat participants over the 4 year period of the study.
Second, the van's protocol routinely took only one BP measurement (when multiple elevated readings are generally used to diagnose hypertension2), used a casual blood glucose value to suggest diabetes (when either a casual value plus symptoms or a fasting value is preferred14), did not collect additional demographic information (age, sex etc) or information on the screenees' knowledge of their health conditions, and involved only a single follow-up phone call. This screening protocol was designed to minimize the burden on screenees, and thus to increase participation. However, more detailed clinical data may have provided different results. Additional demographic information may have aided the interpretation of difference in risk factors by rurality of residence because the impact of age and socioeconomic status on cardiovascular disease risk is well documented37. Additional follow up might have allowed the study to ascertain the clinical impact of the screening program.
The results of a BP and blood glucose screening program conducted at community events including agricultural fairs and targeted at rural Mainers were reported. This program was successful at reaching rural Mainers, reaching them in larger percentages than they are found in the general Maine population. Screenings held at agricultural fairs and in rural locations were particularly successful at attracting rural screenees. Finally, rural screenees (in particular those who lived in large rural towns) were at significantly higher risk for hypertension compared with screenees from urban areas. These results suggest that it is possible to design a cardiovascular disease risk factor screening program to preferentially reach rural populations, and that these populations may be particularly likely to benefit from these screenings.
References
1. Lloyd-Jones D, Adams RJ, Brown TM, Carnethon M, Dai S, De Simone G et al, on behalf of the American Heart Association Statistics Committee and Stroke Statistics Subcommittee. Heart disease and stroke statistics - 2010 update: a report from the American Heart Association. Circulation 2010; 121: e46-e215.
2. National Heart Lung and Blood Institute. Seventh report of the Joint National Committee on prevention, detection, and treatment of high blood pressure. (Online) 2004. Available: http://www.nhlbi.nih.gov/guidelines/hypertension/jnc7full.pdf (Accessed 19 July 2011).
3. Greenland P, Alpert JS, Beller GA, Benjamin EJ, Budoff MJ, Fayad ZA et al. 2010 ACCF/AHA guideline for assessment of cardiovascular risk in asymptomatic adults: executive summary: a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines. Circulation 2010; 122: 2748-2764.
4. US Preventive Services Task Force. Screening for high blood pressure: US Preventive Services Task Force reaffirmation recommendation statement. Annals of Internal Medicine 2007; 147: 783-786.
5. US Preventive Services Task Force. Screening for type 2 diabetes mellitus in adults: US Preventive Services Task Force recommendation statement. Annals of Internal Medicine 2008; 148: 846-854.
6. The Healthy People Consortium. Healthy people 2020: The road ahead. (Online) 2011. Available: http://www.healthypeople.gov/hp2020/default.asp (Accessed 9 January 2011).
7. MacDowell M, Glaser M, Fitts M, Nielsen K, Hunsaker M. A national view of rural health workforce issues in the USA. Rural and Remote Health 10:1531. (Online) 2011. Available: http://www.rrh.org.au/journal/ (Accessed 9 January 2011).
8. Rural Healthy People 2010 Project. Final rural healthy people 2010 documents. (Online) 2011. Available: http://www.srph.tamhsc.edu/centers/rhp2010/ (Accessed 9 January 2011).
9. Rural Assistance Center. Maine. (Online) 2011. Available: http://www.raconline.org/states/maine.php (Accessed 9 January 2011).
10. Maine Center for Disease Control & Prevention. Office of rural health and primary care. (Online) 2011. Available: http://www.maine.gov/dhhs/boh/orhpc/ (Accessed 9 January 2011).
11. Maine Elks Association. Welcome to the Maine Elks Association Website. (Online) 2011. Available: http://www.maineelks.org/ (Accessed 9 January 2011).
12. Maine State Grange. Friends, family, community - growing together. (Online) 2011 Available: http://mainestategrange.org/ (Accessed 9 January 2011).
13. Hamel L, Harris DE. License to screen: a new mobile intervention program. The Nurse Practitioner 2009; 34(6): 42-47.
14. American Diabetes Association. Diagnosis and classification of diabetes mellitus. Diabetes Care 2007; 30: S42-S47.
15. US Census Bureau. Census Atlas of the United States. (Online) 2011. Available: http://www.census.gov/geo/www/maps/ (Accessed 9 January 2011).
16. WWAMI Rural Health Research Center. RUCA data. (Online) 2011. Available: http://depts.washington.edu/uwruca/ruca-download.php (Accessed 9 January 2011).
17. Vanderboom CP, Madigan EA. Federal definitions of rurality and the impact on nursing research. Research in Nursing & Health 2007; 30: 175-184.
18. Maine Office of GIS. GIS Data Catalog. (Online) 2010. Available: http://megis.maine.gov/ (Accessed 9 January 2011).
19. Washington State Department of Health. Guidelines for using rural-urban classification systems for public health assessment. (Online) 2011. Available: http://www.doh.wa.gov/data/guidelines/RuralUrban2.htm (Accessed 9 January 2011).
20. Campbell NRC, Jeffrey P, Kiss K, Jones C, Anton AR. Building capacity for awareness of risk factor identification in the community: the blood pressure assessment program of the Calgary Fire Department. Canadian Journal of Cardiology 2001; 17(2): 1275-1279.
21. Olenak JL, Calpin M. Establishing a cardiovascular health and wellness program in a community pharmacy: screening for metabolic syndrome. Journal of the American Pharmacists Association 2010; 50: 32-36.
22. Edelman D, Edwards LJ, Olsen MK, Dudley TK, Harris AC, Blakcwell DK et al. Screening for diabetes in an outpatient clinic population. Journal of General Internal Medicine 2002; 17: 23-28.
23. Patel JV, Gunarathne A, Lane D, Lim HS, Tracey I, Panja PC et al. Widening access to cardiovascular healthcare: community screening among ethnic minorities in inner-city Britain - the Healthy Hearts Project. BMC Health Services Research. (Online) 2007. Available: http://www.biomedcentral.com/1472-6963/7/192 (Accessed 9 January 2011).
24. Sonkodi B, Fodor JG, Abraham G, Legrady P, Ondrik Z, Lencse G et al. Hypertension screening in a salami factory: a worksite hypertension study. Journal of Human Hypertension 2004; 18: 567-569.
25. Aponte J, Nickitas DM. Community as client: reaching an underserved urban community and meeting unmet primary health care needs. Journal of Community Health Nursing 2007; 24(3): 177-190.
26. Patel K, Larson C, Hardgreaves M, Schlundt D, Wang H, Jones C et al. Community screening outcomes for diabetes, hypertension, and cholesterol: Nashville REACH 2010 project. Journal of Ambulatory Care Management 2010; 33(2): 155-162.
27. Frank D, Grubbs L. A faith-based screening/education program for diabetes, CVD, and stroke in rural African Americans. The ABNF Journal 2008; Summer: 96-101.
28. Davis-Smith M. Implementing a diabetes prevention program in a rural African-American church. Journal of the National Medical Association 2007; 99(4): 440-445.
29. Williamson W, Kautz DD. "Let's get moving: Let's get praising:" promoting health and hope in an African American church. The ABNF Journal 2009; Fall: 102-105.
30. Davidson MR. Establishing prevention, education and community awareness through a comprehensive diabetes, hypertension and hypercholesterolaemia screening programme: The Smith Island, Maryland, USA experience. International Journal of Nursing Practice 2004; 10: 242-246.
31. Mainous AG, King DE, Garr DR, Pearson WS. Race, rural residence, and control of diabetes and hypertension. Annals of Family Medicine 2004; 2: 563-568.
32. Chan L, Hart LG, Goodman DC. Geographic access to health care for rural Medicare beneficiaries. Journal of Rural Health 2006; 22(2): 140-146.
33. Parsons MA, Askland KD. Cancer of the colorectum in Maine, 1995-1998: determinants of stage at diagnosis in a rural state. Journal of Rural Health 2007; 23(1): 25-32.
34. Bale B. Optimizing hypertension management in underserved rural populations. Journal of the National Medical Association 2010; 102: 10-17.
35. Tabaei, BP, Burke R, Constance A, Hare J, May-Aldrich G, Parker S et al. Community-based screening for diabetes in Michigan. Diabetes Care 2003; 26: 668-670.
36. Feresu SA, Zhand W, Puumala SE, Ullrich F, Anderson JR. The frequency and distribution of cardiovascular disease risk factors among Nebraska women enrolled in the WISEWOMAN screening program. Journal of Women's Health 2008; 17(4): 607-617.
37. Banks J, Marmot M, Oldfiled Z, Smith JP. Disease and disadvantage in the United States and in England. JAMA 2006; 295: 2037-2045.
