Humans who have close contact with livestock, wild or feral animals can risk acquiring zoonotic infections such as brucellosis, Q fever, and leptospirosis. Brucellosis is a zoonotic infection caused by small, Gram-negative aerobic coccobacilli from the Brucella genus1. Four Brucella species are associated with moderate to significant human pathogenicity, specifically Brucella melitensis which is found primarily in goats, Brucella suis in pigs, Brucella abortus in cattle and Brucella canis in dogs. Humans have also very infrequently been infected with Brucella species from marine mammals2. Globally B. melitensis more frequently affects humans than the other species and is the most virulent, pathogenic and invasive species, followed by B. suis, B. abortus and B. canis1. B. abortus has been eradicated from Australia and B. melitensis and B. canis are not found in Australia3.
Brucellosis symptoms in humans are non-specific, including undulating fever, sweats, malaise, anorexia, headache and back pain. The onset can be insidious or acute, generally beginning 2-4 weeks after exposure, but can occur up to 6 months later4. Depression and chronic infection can occur5 with delays in diagnosis increasing the risk of complications6.
Human infection with B. suis (swine brucellosis) follows occupational or recreational exposure to infected animals, inhalation of infectious aerosols, laboratory exposure, or consumption of inadequately cooked contaminated meat5. Worldwide many cases of human infection follow contact with infected feral pigs or 'wild boars'7.
Approximately 20-30% of feral pigs are Brucella-positive by serology in Italy, the USA and Croatia7. B. suis infection in feral pigs is characterised by infertility and abortion in sows, deaths of piglets and orchitis in boars. Genital secretions are the most important source of infection. Infected feral pigs rarely show macroscopic post-mortem lesions and thus may be overlooked during evisceration and meat inspection8.
Brucellosis in Australia is mainly an occupational disease of farm workers, veterinarians, hunters and abattoir workers with exposure to infected animals or their tissues3. The national incidence is 0.2/ 100 000 population with 80% of cases occurring in the state of Queensland. The majority of cases are male and aged between 15 and 49 years3.
In recent years there has been a growing Australian market for exporting 'wild boar' meat to Europe. Accredited hunters kill feral pigs with a rifle or knife, gut and eviscerate them and then transport the fresh carcasses to 'chillers'. Pig dogs play an integral role in feral pig hunting in Australia. Dogs have been reported to be infected with B. suis internationally9, but their contribution to B. suis transmission in feral pigs and humans in Australia is currently unknown.
A recent retrospective review conducted in Queensland, Australia of 32 patients with swine brucellosis contracted between 1996 and 2009 found that feral pig hunting explained 30 of the cases (94%), none of whom used protective equipment during hunting6.
Between December 2006 and December 2009, five men from New South Wales (NSW), Australia, were diagnosed with brucellosis following regular recreational or occupational feral pig hunting in north-west NSW near the border with Queensland10,11. All cases had butchered feral pig carcasses without using personal protective equipment. None reported any other risk factors for contraction of brucellosis10. Blood samples from 200 trapped feral pigs in the region where the human cases occurred were negative for Brucella serology, but 20 were positive for Leptospira spp10.
It is reported that the most important means of preventing disease in humans is to take precautions when coming into contact with animals (Fig1)12,13.

Figure 1: Summary of the recommended precautions to prevent swine
brucellosis in humans when coming into contact with animals12,13.
There has not been an evaluation of the acceptability of the recommended risk reduction strategies in the settings where feral pig hunting and evisceration occurs. Feral pig hunters are likely to be hard to reach with health promotion strategies.
The NSW Food Regulatory Authority provides detailed information about the techniques to be used to harvest 'wild boar' meat to make it safe for human consumption14.
Aims
This study aimed to:
- explore the appropriateness of current swine brucellosis risk reduction strategies for feral pig hunters
- identify strategies that are acceptable and appropriate for feral pig hunters
- investigate the most appropriate methods of disseminating health-related information to reach professional and recreational feral pig hunters.
This work was conducted applying a grounded theory approach, developing an explanatory theory of basic social processes within the environments in which they occur15. Grounded theory can give voice to those who are otherwise rarely heard, such as the participants in this research16. Theoretical sampling was used for recruiting participants so that different experiences and dimensions were explored. Sampling started with health service and community contacts then, using a snowballing method17, each participant was asked to recommend the study to people they knew who hunted feral pigs.
Semi-structured interviews and small focus groups were conducted with participants to explore their experiences with hunting and their views on the brucellosis prevention strategies. Interview questions asked about their most recent feral pig hunting activity. The participants were specifically asked how the recommended risk reduction strategies could have been applied during that most recent hunt. Respondents were also asked about appropriate dissemination methods for health messages to feral pig hunters. Each in depth interview and focus group was conducted by two researchers (PM, BP). Extensive interview notes taken by both researchers were then combined into a single collated data set.
Interview and focus group notes were thematically analysed. Emerging themes from the early interviews were explored in subsequent interviews15. Researchers (PM, BP) separately coded the data. An open coding system was used, where codes were noted freely across all notes. The coding system was refined iteratively as the notes were re-analysed. Coding was then compared between researchers, deconstructed and reconstructed. Once the coding system was finalised, all notes were re-coded. Relationships between codes/categories were then assessed across the notes. This was done by selecting codes or topics that were emerging as significant for the research and looking for coded text that could explain or contribute to the phenomenon18. Illustrative quotes were then drawn from the notes. Recruitment and interviews continued until data saturation occurred.
Study rigour was guaranteed by having two researchers independently conduct the data analysis and then discuss emergent themes with the remaining authors, enhancing the ''reflexivity'' of the analysis and confirming the coding scheme. All research activities were thoroughly documented to permit a critical appraisal of methods. The role of prior assumptions and experience was acknowledged and, when possible, eliminated19,20.
Ethical approval to conduct this research was provided by the Hunter New England Human Research Ethics Committee (10/11/17/5.02).
During the study period, December 2010-March 2011, five feral pig hunters participated in semi-structured interviews. Additionally, two focus groups of two and three hunters were conducted. Participants were all males from north-west NSW aged between 22 and 41 years. Four were from large towns and with no known social links. The remaining participants were from farming areas and a small village. The two focus groups consisted of people who hunted together. Most participants had occupations other than hunting, such as farm work, driving, service industry or public service.
There was a range of hunting experiences from a very professional hunting approach to a purely recreational approach that included some poaching (which in this context involves hunting while trespassing on private property). Most participants hunted pigs for sport and recreation. Five of the participants described that in addition to the enjoyment provided, selling carcasses provided enough income to cover their alcohol purchases.
The main domains that emerged from participants' experiences during their most recent feral pig hunting activity, and reflecting on current swine brucellosis risk reduction strategies, were (Table 1):
- You've gotta be tough to be a feral pig hunter.
- Most of the suggested strategies won't work.
- Reducing risk in the scrub.
- How to let pig hunters know.
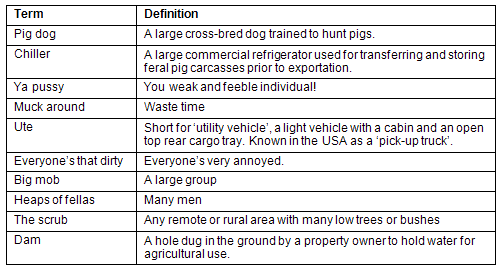
Table 1: Definitions of Australian colloquial terms in the qualitative material
You've gotta be tough to be a feral pig hunter
Participants spoke about feral pig hunting as a 'tough' activity but also as good fun. 'I go with a group of mates, we are more about the fun and sport', was a common sentiment among participants.
Participants explained that most hunting involves chasing pigs through the scrub with dogs and knives. The dogs catch and hold the pig until the hunter slaughters the pig with a knife thrust to the heart or lungs. The pig is then dragged back to the truck where it is lifted up onto a hook and eviscerated. Being a tough person who can drag and lift pig carcasses, and is willing to get injured and covered in blood during the chase and the gutting, emerged as expected hunter traits.
You get covered in blood, particularly if you go through the shoulder, blood bubbles and sprays out of the lungs and you get sprayed up the arms, even on the lips and face.
You get covered in it...and ya stink.
You always get cuts. Barbwire or sticks, I've had a few nicks from the knife.
This toughness is also expressed through the actions taken following an injury. Four of the participants spoke about ignoring injuries while continuing their hunting activity.
I've got a little scar on my finger from a pig's tusk, it just turned and split me a bit - not much of a drama. At the time we were 25 km from town at 2.30 in the morning. I just checked it, it wasn't too deep and rinsed it off and kept going.
Get plenty of nicks. Give it a wipe or do some swearing. If it's bad, you give it a wash. Most people just keep going which probably doesn't help.
Participants also spoke about the peer-pressure to exhibit toughness. One participant spoke about the perceived reaction of his mates to him wearing gloves and said, 'I think a lot of people don't wear gloves, they think "Ah ya pussy".'
Most of the suggested strategies won't work
Participants reported that covering cuts does not work because the dressings do not adhere in the wet and rough conditions. Wearing gloves was not a common practice among the participants. Reasons for not wearing gloves included peer pressure and 'you can feel a lot better without them'.
Washing hands was acceptable but the focus was getting rid of the smell of the pigs, rather than the perceived health and safety benefits. As one participant said, 'If you are in the scrub and just killed a pig you do it as soon as you can, if there's a dam about you rinse off'. Some hunters wash their hands frequently but still struggle to wash as often as advised by the food regulatory authority. Others commented that if one was busy, cleanliness may be neglected, 'you might get 20 [pigs] in a mob. Sometimes you'll go a few hours without washing your hands!' Using a disinfectant was uncommon.
One of the Queensland Health and World Health Organization brucellosis prevention strategies is avoiding exposure to blood. Implementing this strategy was considered impossible by participants. Participants said 'Definitely hard!' and 'You can't, they're not going to lift themselves' referring to the direct handling of carcasses required.
Washing down work areas was considered by many respondents to be 'a good idea but not something the boys would do'.
Burning or burying remains was not considered practicable. As one participant said, 'Can't see guys doing this, you should see some of the ground I hunt in, it'd take an hour to dig a hole'. The remains are left on the ground: as another participant said, 'Nah, never do it. The crows and foxes would starve!'.
Reducing risk in the scrub
Participants were aware that there was a risk of infection from diseased animals but thought this could be judged by the animal's condition. 'Unless they're fat and healthy, don't take 'em'. Personal risk assessment appeared related to knowledge of a hunter with infection, 'Until it [an illness] happens to them or someone they know, they just turn a blind eye to it'.
Strategies to reduce risk in the scrub emerged from the interviews. Taking more time and watching hands when making cuts was the clearest theme that emerged from the interviews, 'Just a matter of slowing down and taking care'; 'Can't rush in and go slit, slit, slit'; and 'I've seen heaps of fellas get cut 'cause they're in too much of a hurry'. Particularly, hunters need to 'always look for your f***** hands, you don't wanna [want to] cut them'.
Ensuring good lighting into the carcass, such as headlamps or adjustable extension arms for the spotlights on the back of the truck were recommended. A participant explained, 'A few wear headlamps, a few are old fashioned and still muck around with torches'.
Taking care in the vicinity of a sow's uterus when gutting a pig was also considered a worthwhile strategy for reducing risk. One participant described how he is 'careful to keep the womb intact and take it 10 metres away from the ute. I don't give it to the dogs'. Another said, 'If you're not careful you can split it [the uterus]'.
Using surgical type gloves to cover cuts was suggested by some participants because they considered these gloves more effective than the recommended dressings. One man said, 'If I get a bad cut, I glove it with a latex glove and tape it and then just try not to use that hand'.
How to let pig hunters know
Several different methods of information delivery were suggested by respondents. Trade magazines, websites and information at the chiller were methods recommended by all participants for communicating with hunters. In relation to pig hunting magazines, one participant said, 'Nearly all of the boys I know read that stuff. If not buying it you'd at least flick through it at the newsagent'. Websites and hunting blog sites were also popular. As one person said, 'I know heaps of people who read that [website]'.
Regarding messaging at the chiller, the advice was to have 'just a short message, you don't want a lot of text'. In addition, it was advised not to lecture hunters: 'A lot of these pig hunters, they're pretty non-helpful blokes; if you try to tell them something they won't listen, but if you make it like you're providing information they will'.
Many participants described animosity towards the food regulatory authority. As one participant said, 'Everyone's that dirty with Safe Foods [NSW Food Authority] we'd take one look [at safety info] and throw it over the shoulder. People are over 'em.'.
Limitations
This study was conducted in the north-west area of the Australian state of NSW and with a relatively small number of participants. Data saturation occurred during the interview process, the issues identified by the semi-structured interview were also found in the focus groups, and the participants were from three different locations. However, this study may not be representative of Australian feral pig hunters.
Discussion
The infectious disease and injury risk of feral pig hunting in Australia and internationally are well established. Swine brucellosis in humans in the USA is predominantly associated with exposure to infected feral pigs4. Two cases were reported in 2004, in hunting partners from a hunt club who had killed and dressed feral pigs in South Carolina21. Also three cases of swine brucellosis were detected in feral pig hunters after hunting and butchering pigs in Florida. No personal protective equipment was worn during these procedures, and no other risk factors for brucellosis were identified4. Also in Florida between 1963 and 1975, eight hunters contracted swine brucellosis attributed to contacts with feral pigs22.
The environment and nature of feral pig hunting: rough terrain, frequently nocturnal, weapon use, close proximity to wild animals and butchering process, challenge traditional risk reduction strategies. The recreational nature and prevailing 'macho' nature of participants demand a pragmatic approach to risk reduction if it is going to prove acceptable to feral pig hunters. The 'you've gotta be tough to be a feral pig hunter' context of the activity and the reality that many feral pig hunters participate with little preparation and a 'just keep going' approach, may counteract currently recommended risk reduction strategies. These findings reflect those of previous research into the culture of farm safety in Australia23.
The alternate strategies that emerged from the interviews need to be tested in the real world, especially evisceration in the scrub. But the following ideas were grounded in the participants' experiences:
- take more time and watch your hands when making cuts
- have good lighting
- take care when cutting near a sow's uterus
- use latex gloves to cover cuts on hands.
Taking more care during butchering may well be challenging. Not only is there self-driven need for speed when faced with a 'big mob' of pigs, but current food authority regulations place time constraints on the gutting and delivery to the 'chiller' to ensure that pig meat remains fresh. These regulations may be inadvertently increasing hunters' health risks. Achieving a better balance needs to be considered by both the authorities and hunters.
Feral pig hunters appear to weigh up their risk of illness depending on whether they 'know someone' with the illness. The use of authorised stories of people who have had brucellosis in pig hunting magazines and websites may be a useful method for increasing awareness and the reality of brucellosis for hunters.
Swine brucellosis is a zoonosis of concern for feral pig hunters in many parts of Australia, including north-west NSW. Many of the current strategies to reduce the risk of brucellosis did not appear appropriate or acceptable to the feral pig hunters interviewed. More acceptable strategies when eviscerating - such as taking more time, watching hands, ensuring good lighting, being careful in the vicinity of the uterus and using a latex glove to cover cuts on hands - need to be tested in the field. Further development of the food safety regulations is required to also support zoonosis risk-reduction strategies.
Acknowledgements
The authors acknowledge, for assistance with the project design and development, Belinda Walker, Technical Specialist, Animal Biosecurity, NSW Department of Trade and Investment, Regional Infrastructure and Services Animal Health; and Shaun Slattery, Senior District Veterinarian, North West Livestock Pest and Health Authority.
References
1. Bossi P, Tegnell A, Baka A, Van Loock F, Hendriks J, Werner A et al. Bichat guidelines for the clinical management of brucellosis and bioterrorism-related brucellosis. Euro Surveillance 2004; 9(12): E15-E16.
2. Van Bressem MF, Raga JA, Di Guardo G, Jepson PD, Duignan PJ, Siebert U et al. Emerging infectious diseases in cetaceans worldwide and the possible role of environmental stressors. Diseases of Aquatic Organisms 2009; 86(2): 143-157.
3. Newman L, Stirzaker S, Knuckey D, Robinson K, Hood J, Knope K et al. Australia's notifiable disease status, 2008: Annual Report of the National Notifiable Diseases Surveillance System. Communicable Diseases Intelligence 2010; 34(3): 157-224.
4. Brucella suis infection associated with feral swine hunting - three states, 2007-2008. Morbidity & Mortality Weekly Report 2009; 58(22): 618-621.
5. Young E. Brucella species. In: G Mandell, J Bennett, R Dolin (Eds). Mandell, Douglas, and Bennett's principles and practice of infectious diseases, 7th edn. Philadelphia, PA: Churchill Livingstone Elsevier, 2009; 2623-2642.
6. Eales K, Norton R, Ketheesan N. Brucellosis in northern Australia. American Journal of Tropical Medicine and Hygiene 2010; 83(4): 876-878.
7. Meng X, Lindsay D, Sriranganathan N. Wild boars as sources for infectious diseases in livestock and humans. Philosophical Transactions of the Royal Society of London B: Biological Sciences 2009; 364(1530): 2697-2707.
8. Al Dahouk S, Nöckler K, Tomaso H, Splettstoesser W, Jungersen G, Riber U et al. Seroprevalence of brucellosis, tularemia, and yersiniosis in wild boars (Sus scrofa) from north-eastern Germany. Journal of Veterinary Medicine Series B-Infectious Diseases and Veterinary Public Health 2005; 52(10): 444-455.
9. Lucero NE, Ayala SM, Escobar GI, Jacob, NR. Brucella isolated in humans and animals in Latin America from 1968 to 2006. Epidemiology and Infection 2008; 136(4): 496-503.
10. Irwin M, Massey P, Walker B, Durrheim D. Feral pig hunting: a risk factor for human brucellosis in north-west NSW? New South Wales Public Health Bulletin 2009; 20(11-12): 192-194.
11. New South Wales Department of Health, Communicable Diseases Branch. Communicable Diseases Report, NSW, November and December 2009. New South Wales Public Health Bulletin 2010; 21(1-2): 43-47.
12. Queensland Government. Brucellosis. Queensland Health Fact Sheet. (Online) 2010. Available: http://access.health.qld.gov.au/hid/InfectionsandParasites/BacterialInfections/brucellosis_fs.asp (Accessed 29 April 2011).
13. World Health Organization. Brucellosis in humans and animals. (Online) 2006. Available: http://www.who.int/csr/resources/publications/Brucellosis.pdf (Accessed 29 April 2011).
14. New South Wales Food Authority. Wild Game Meat Field Harvester Food Safety Program. (Online) 2010. Available: http://www.foodauthority.nsw.gov.au/_Documents/industry_pdf/Wild_Game_Meat_Field_Harvester_FSP.pdf (Accessed 29 April 2011).
15. Glaser B, Strauss A. The discovery of grounded theory: strategies for qualitative research. New York: Adline de Gruyter, 1967.
16. Sofaer S. Qualitative methods: what are they and why use them? Health Services Research 1999; 34(5): 1101-1118.
17. Chaim N. Sampling knowledge: the hermeneutics of snowball sampling in qualitative research. International Journal of Social Research Methodology 2008; 11(4): 327-344.
18. Coffey A, Atkinson P. Making sense of qualitative data. Thousand Oaks, CA: Sage, 1996.
19. Strauss A, Corbin J. Basics of qualitative research: Grounded theory procedures and technique. Newbury Park, CA: Sage, 1998.
20. Lee T. Using qualitative methods in organizational research. Thousand Oaks, CA: Sage, 1999.
21. Starnes C, Talwani R, Horvath J, Duffus W, Bryan C. Brucellosis in two hunt club members in South Carolina. Journal of the South Carolina Medical Association 2004; 100(4):113-115.
22. Bigler W, Hoff G, Hemmert W, Tomas J, Janowski H. Trends of brucellosis in Florida. An epidemiologic review. American Journal of Epidemiology 1977; 105(3): 245-251.
23. Durey A, Lower T. The culture of safety on Australian farms. Rural Society 2004; 14(1): 57-69.




