Rural chronic disease management is a public health concern in Australia, with higher rates of chronic disease reported in non-urban areas1. Rural populations tend to be older, are more likely to be exposed to health risk factors and experience greater socioeconomic disadvantage2-4; these factors also impact on access to health services1,5.
Primary care services (formal care provided at point of entry into the health system) play a vital role in chronic disease care. While GPs deliver the bulk of primary care in Australia6, this is not always the case in rural settings, where access may be limited7,8. Instead, rural primary care is often delivered by nursing and allied health professionals, including through community health centres (CHCs); it is supplemented by pharmacists providing health information and advice7 as well as hospitals9,10, particularly among patients who do not have a regular provider11. More recently, the primary care role of complementary and alternative medical (CAM) providers has been highlighted12-14. Wardle et al14 found that CAM use was higher in non-urban localities due to social and cultural factors, including a preference for holistic care.
Despite national initiatives aimed at improving GP care in rural areas15, research suggests that the primary care needs of rural people with conditions including type 2 diabetes mellitus (T2DM) and cardiovascular disease (CVD) remain unmet4,16,17. This article describes primary care utilisation by people with T2DM and CVD, and explores the role of CAM in this. Based on previous research1, it was anticipated that while GPs would be the most commonly used providers of chronic disease primary care regardless of location, people residing in rural and remote communities would report higher use of non-medical professionals for primary care.
Study design and sample
The data reported here were collected as part of a multidisciplinary study exploring care-seeking, CAM, and self-management among people with T2DM and/or CVD (www.camelot.monash.edu). Ethics approval was obtained from the Monash University Human Research Ethics committee.
Between April and July 2010, a 71 item questionnaire consisting of five sections ('Getting information and use of health services'; 'Use of complementary and alternative medicine'; 'Health insurance'; 'Your health, lifestyle and preferences'; and 'About you') was distributed to 12 162 potential participants, with a web-link made available to an online survey version. Ten thousand hard copy questionnaires were sent to a random selection of National Diabetes Services Scheme (NDSS) registrants residing in Victoria, Australia; 672 were sent to Victorian Heart Support Australia (HSA) members. An additional 1490 hard-copy questionnaires were distributed via consumer and community-based organisations. Online responses were received from 376 participants, including 290 valid responses.
Questionnaires commenced with a consent statement; informed consent was assumed when participants returned their questionnaires. Respondents were aged 18 years or older, able to understand written English, and had been diagnosed with T2DM and/or CVD. While 3385 surveys were returned, 2915 valid survey responses (response rate = 23.97%) form the basis of this analyses. One participant was excluded due to not providing a postal code.
Geographical classification
Using residential postal codes, geographic location was determined on the basis of the Australian Standard Geographical Classification (ASGC)18, which categorises localities into five classes of remoteness (Major city, Inner regional, Outer regional, Remote, Very remote; also Migratory) based on the Accessibility/Remoteness Index of Australia (ARIA18). Each class summarises locality size as well as accessibility to health services.
The ASGC class was determined using the online Queensland Health Workforce postcode search tool19. This yielded four ASGC classes, with the exception of 'Very remote'; this reflects the population distribution of the state Victoria, where even the most remote communities are within several hours drive of secondary health services and very few communities are classified 'Remote'. The dataset contained two respondents living in 'remote' regions.
Analyses
Data were initially subject to appropriate exploratory analyses to test assumptions of normality, before χ2 contingency table analyses were conducted using PASW Statistics 18.0 (SPSS; Chicago, IL, USA).
Demographic characteristics of respondents
Almost two-thirds of the sample (n=1741, 59.2%) resided in major cities (n=956, 32.6% inner regional; n=215, 7.4% outer regional; n=2, 0.1% remote). Demographic characteristics are shown by geographic location (Table 1). Due to small participant numbers in this group, the two remote respondents were re-classified as 'Outer regional' for the purposes of analysis.
Table 1: Demographic characteristics of survey respondents (N=2914)
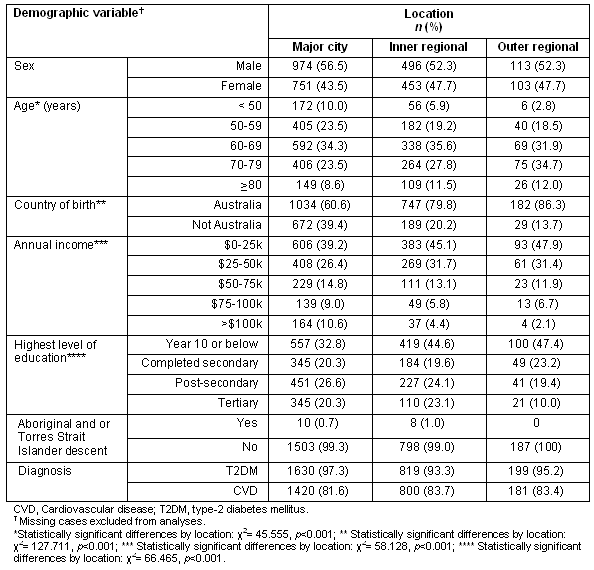
The majority of respondents were male, which reflected the composition of registrants from the NDSS. Respondents in regional areas (Inner or Outer regional) were significantly older than those living in major cities; similarly, a higher proportion reported having been born in Australia. Annual household income varied with rurality: more Outer regional respondents (47.9%) reported the lowest income bracket ($0-25,000) than Inner regional (45.1%) or Major city respondents (39.2%; χ2=58.128, p<0.001). Similarly, education levels varied by area of residence: 47.4% of outer regional respondents had not completed secondary school, compared with 44.6% inner regional and 32.6% major city respondents (χ2=66.465, p<0.001).
Health service utilisation
Outer regional respondents reported the highest attendance at allied health practitioners, district or practice nurses, and CHCs (Table 2). While respondents reported low rates of consultation with diabetes-specific nursing professionals, those in the two regional groups reported slightly higher rates than those from Major cities. This may relate to two factors. First, CHCs are present in non-urban areas where there may be no other health services; they are staffed by, or have regular visits from, nursing and allied health professionals20. Second, they typically charge fees which reflect the socio-economic status of the population served and thus are affordable. In addition, the complex nature of nursing care in rural settings21 may mean that nursing professionals fulfil multiple roles, including providing diabetes-specific care.
Use of hospital services increased with decreasing rurality. This may reflect the location of particular facilities and providers in larger regional or metropolitan centres. Similarly, the majority (n=410) of people who consulted CAM providers were located in Major cities, with only 33 residing in an Outer regional area.
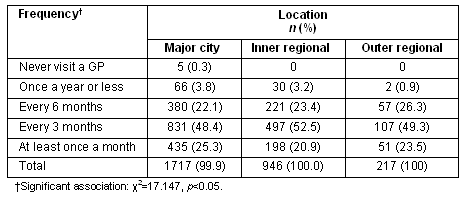
While use of GP clinics varied only subtly in relation to respondents' locality, the data indicated that increasing rurality was associated with less frequent use of these services (Table 3; χ2=17.147, p<0.05). Health service provision and issues of accessibility appeared to play an important role in shaping which providers respondents attended and, at least for GPs, their frequency of attendance.
Table 2: Reported use of primary care services in the past 12 months by location1,15,20
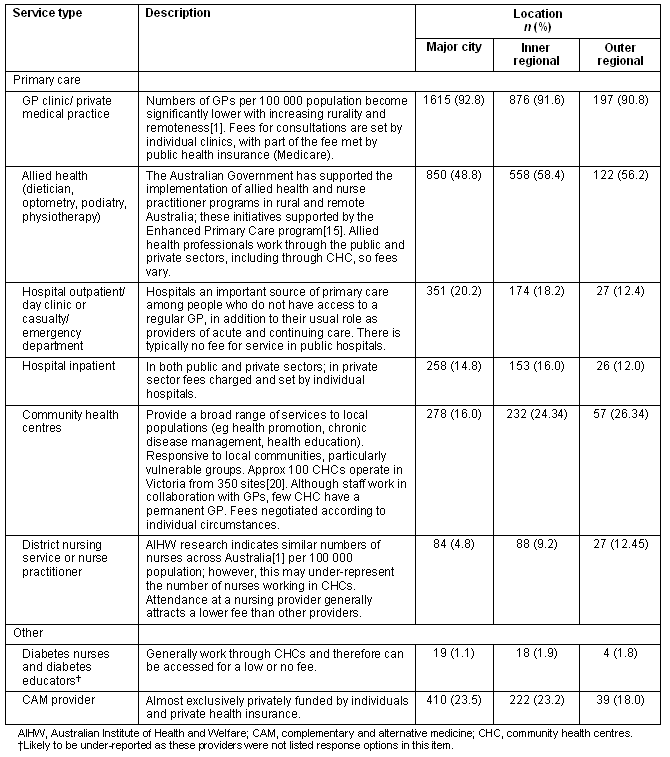
Table 3: Frequency of GP use by patients in metropolitan and rural areas
Discussion
General practitioners were the most common providers of chronic disease primary care, with over 90% of respondents in each group reporting they had visited a GP at least once in the past 12 months. Like other research22,23, the present results found that Major city respondents consulted with their GPs significantly more often than those in regional areas. Therefore, it was unsurprising that people in Inner and Outer regional areas reported relatively higher rates of attendance at nursing and allied health professionals. This may also reflect the distribution of services such as CHCs across the state.
The data indicated that almost one-quarter (23%) of the total sample with T2DM or CVD had consulted CAM providers in the preceding 12 months. Rates varied subtly by location, with a greater proportion of people in Major cities and Inner regional areas reporting their use compared with people in Outer regional areas. This suggests that geographical location may limit access to particular services.
These results provide insight into the rural people's patterns of primary care service usage when managing T2DM and/or CVD. Faced with GP shortages and limited accessibility, rural people living with these chronic conditions may instead use other primary care services. Of course, the models of care available in any community play an important role in usage, but it was not possible to determine from the data whether regional respondents consulted nursing and allied health professionals as a matter of choice or because access to GP care was limited. The five dimensions of access described by Penchansky and Thomas24, which elucidate social, economic, geographic and structural factors affecting use of health services, may be important here.
Future research is required to understand whether the trends identified extend to more remote parts of Australia. The research was limited by the absence of data regarding the frequency of patient visits to nurses, allied health professionals and hospitals. The low response rate suggests that the findings reported here may be characteristic only of particular sub-groups and thus may not be generalizable to all Victorians with T2DM or CVD.
Issues related to access to care may importantly influence the engagement of primary care services by people with T2DM and CVD in terms of both services consulted and frequency of consultation. These findings suggest the importance of the availability or non-GP primary care services in non-urban areas and have important implications for the provision of collaborative chronic disease management in Australia.
Acknowledgements
This article reported one aspect of a larger research project (the CAMELOT Study) supported by a project grant from the National Health and Medical Research Council (grant number: 491171). The authors gratefully acknowledge the contribution of the CAMELOT research team in the design and implementation of the broader project: Brian Oldenburg, Vivian Lin, Maximilian de Courten and Bruce Hollingsworth. The authors also extend their gratitude to the collaborating organisations: Diabetes Australia, Diabetes Australia - Victoria, the National Diabetes Services Scheme, and Heart Support Australia for their assistance in recruiting respondents.
References
1. Australian Institute of Health and Welfare. Cardiovascular medicines and primary health care: a regional analysis. Cardiovascular disease series 32, cat no 48. Canberra, ACT: AIHW, 2010.
2. Larson A. Rural health's demographic destiny. Rural and Remote Health 6: 551. (Online) 2006. Available: www.rrh.org.au (Accessed 16 February 2011).
3. Byles J, Powers J, Chojenta C, Warner-Smith P. Older women in Australia: ageing in urban, rural and remote environments. Australasian Journal on Ageing 2006; 25(3): 151-157.
4. Wan Q, Harris MF, Powell-Davies G, Jayasinghe UW, Flack J, Georgiou A et al. Cardiovascular risk levels in general practice patients with type 2 diabetes in rural and urban areas. Australian Journal of Rural Health 2007; 15(5): 327-333.
5. Dixon J, Welch N. Researching the rural-metropolitan health differential using the 'social determinants of health'. Australian Journal of Rural Health 2000; 8(5): 254-260.
6. Healy J. Australia. In: A Dixon, E Mossialos (Eds). Health care systems in eight countries: trends and challenges. London: London School of Economics and Political Science, 2002; 3-16.
7. Rogers A, Hassell K, Noyce P, Harris J. Advice-giving in community pharmacy: variations between pharmacies in different locations. Health and Place 1998; 4(4): 365-373.
8. Warren N. Markers of Midlife: interrogating health, illness and ageing in rural Australia. Koln: Lambert Academic, 2009.
9. Laurence CO, Beilby MJ, Campbell S, Campbell J, Ponte L, Woodward G. Process for improving the integration of care across the primary and acute care settings in South Australia: asthma as a case study. Australian Journal of Rural Health 2004; 12(6): 264-268.
10. Zeitz K, Malone G, Arbon P, Fleming J. Australian issues with the provision of after-hours primary medical services in rural communities. Australian Journal of Rural Health 2006; 14(3): 99-104.
11. Starfield B, Shi L, Macinko J. Contribution of primary care to health systems and health. Milbank Quarterly 2005; 83(3): 457-502.
12. Powell-Davies G, Fry D. General practice in the health system. In: Department of Health and Ageing. General Practice in Australia: 2004. Canberra:, ACT Australian Government, 2005; 420-465.
13. Rygh EM, Hjortdahl P. Continuous and integrated health care services in rural areas: a literature study. Rural and Remote Health 7: 766. (Online) 2007. Available: www.rrh.org.au (Accessed 4 March 2011).
14. Wardle JL, Adams J, Lui CW. A qualitative study of naturopathy in rural practice: a focus upon naturopaths' experiences and perceptions of rural patients and demand for their services. BMC Health Services Research 2010; 10: 185. Available: http://www.biomedcentral.com/1472-6963/10/185 (Accessed 27 October 2011).
15. Department of Health and Ageing. Enhanced Primary Care program. Canberra, ACT: Commonwealth of Australia. Available: http://www.health.gov.au/epc (Accessed 26 August 2011).
16. Clark RA, Eckert KA, Stewart S, Phillips SM, Yallop JJ, Tonkin AM et al. Rural and urban differentials in primary care management of chronic heart failure: new data from the CASE study. Medical Journal of Australia 2007; 186(9): 441-445.
17. Clark RA, Driscoll A. Access and quality of heart failure management programs in Australia. Australian Critical Care 2009; 22(3): 111-116.
18. Australian Institute of Health and Welfare. Rural, regional and remote health: a guide to remoteness classifications. Cat no PHE 53. Canberra, ACT: AIHW, 2004.
19. Health Workforce Queensland. RRMA/ASGC-RA Town/Postcode Search. (Online) 2010. Available: http://www.healthworkforce.com.au/main_rrma.asp?NodeID=27679 (Accessed 15 March 2011).
20. Better Health Channel. Community Health Centres: fact sheet. Melbourne, VIC: Victorian Government Department of Health. Available: www.betterhealth.vic.gov.au (Accessed 26 August 2011).
21. Scharff JE. The distinctive nature and scope of rural nursing practice: philosophical bases. In: HJ Lee, CA Winters (Eds). Rural nursing: concepts, theory, and practice. Amsterdam: Springer, 2006.
22. Britt H, Miller GC, Valenti L. 'It's different in the bush': a comparison of general practice activity in metropolitan and rural areas of Australia 1998-2000: BEACH Study. Cat no GEP 6. Canberra, ACT: University of Sydney and the Australian Institute of Health and Welfare, 2001.
23. Beilby JJ, Furler J. General practitioner services in Australia. In: Department of Health and Ageing. General Practice in Australia: 2004. Canberra, ACT: Australian Government, 2005; 128-213.
24. Penchansky R, Thomas JW. The concept of access: definition and relationship to consumer satisfaction. Medical Care 1981; 19(2): 127-140.




