Federally Qualified Health Centers (FQHC) are community based organizations whose purpose is to provide affordable, comprehensive healthcare services to underserved populations. The FQHCs provide primary and preventive care, dental care and mental health/substance abuse services to underinsured and uninsured populations. Federally Qualified Health Centers must demonstrate service to Medically Underserved Areas (MUA), areas designated by the Human Resources and Services Administration (HRSA) as having too few primary care providers, high infant mortality, high poverty and/or high elderly population, or Health Professional Shortage Areas, designated by HRSA as having shortages of primary medical care, dental or mental health providers1. Federally Qualified Health Centers receive funds from the Bureau of Primary Care to underwrite the indigent care provided to qualified patients, receive cost-based reimbursement from Medicare and Medicaid and offer a sliding fee for eligible 'self-pay' patients. Governance of an FQHC is provided by a volunteer, consumer board in which at least 51% of members are required to be users of the health center.
Portions of Montgomery County, Virginia were designated as a MUA in 2008, with a recent a poverty rate of 24.7% in 20122,3. Montgomery county is located in the southern sub region of the Appalachian Highlands4 and the population is predominantly White (89%) with approximately 10% of the population aged 65 years or older. As documented in previously published studies, rural Appalachian residents suffer from disproportionately high incidences of cancer, obesity, diabetes and cardiovascular diseases5-8. Higher rates of mortality parallel the geographical patterns of cardiovascular disease and obesity9. Social, cultural and economic causes have been previously described as potential contributors to poor health Appalachian residents. Understanding the cultural values and beliefs that may affect healthcare utilization is paramount to developing a successful medical home.
In September 2008, the authors were awarded a planning grant to assess healthcare needs for underserved residents in Montgomery County and to develop a strategic plan to best meet these needs. A steering committee composed of community members and local organizational partners was created to lead a study of healthcare needs of the residents of Montgomery County and to develop a strategic plan to meet the needs of the underserved. The steering committee included faculty from local universities and an osteopathic medical school, local physicians and dentists, county public school officers, local social service leaders, a pastor from the interfaith council, representatives from the Virginia House of Delegates, and representatives from local hospitals, the area free clinic and the Board of Supervisors.
The community assessment and steering committee was lead by faculty at the Virginia College of Osteopathic Medicine. Steering committee meetings were held on a monthly basis from November of 2008 to June of 2009 and task force committees were developed to conduct a comprehensive community needs assessment. The steering committee recognized the need for a community health assessment that incorporated both health indicators and a social, behavioral and environmental assessment.
The purpose of this study was to examine the social and cultural beliefs that may impact illness and healthcare utilization among underserved populations in Montgomery County. A qualitative needs assessment which utilized focus group discussions was conducted with underserved populations. Focus groups can be particularly helpful in gathering information to determine the perceptions of participants about services and opportunities10. The results from this study were used in the strategic planning process to design an appropriate service delivery model that is compliant with FQHC requirements.
The objective of this study was to investigate and describe the perceptions, beliefs and practices that impact healthcare utilization among underserved populations in Montgomery County, Virginia. A task force committee composed of members of the initial steering committee identified two broad categories of perceived need: (i) lack of access to care for underserved populations; and (ii) barriers to care of underserved populations. Additional subcategories were then identified under each category. The demographics of the focus group participants were representative of underserved populations in the community. Based on the initial review by the task force committee of health statistics from the Virginia Department of Health and anecdotal provider information, six distinct populations were targeted for the focus group sessions which were representative of underserved populations within the county: low-income children and families, low-income elderly recipients, low-income residents living in substandard housing, graduate and medical students and their families, and low-income pregnant women. One focus group for each population was conducted. A description of each focus group's composition and location is provided (Table 1).
Each focus group was composed of six to 15 participants, with a median of nine participants. Ethnicity of the focus group participants included Caucasian, African American, Hispanic and internationals from South Africa, the Netherlands, China, Taiwan, Korea and France. Focus groups included low-income parents of children aged 3-5 years, elderly and/or disabled residents of a Housing and Urban Development (HUD) subsidized retirement community, residents of a trailer park community, spouses of international students living in the community, medical students with children and pregnant women receiving prenatal care or case management services at the Health Department. Staff at the local Head Start program, Health Department, YMCA and retirement community assisted with recruitment of participants. In addition, participants were recruited through direct referrals and invitations from community providers and project team members and through direct advertising to the targeted populations.
Table 1: Focus group sites and participants

Community focus group discussions were conducted in locations familiar to participant populations. A discussion model which outlined the participants' utilization of services based on their perception of need and access and barriers to healthcare services was used to design the focus group discussions. Along with discussion prompts to further explore the participants' perceptions and experiences, three broad focus group disscusion questions were asked:
- What do you, or people you know, do when you need primary care services?
- What do you, or people you know, do when you need dental services?
- What do you, or people you know, do when you need mental health services?
The study was reviewed and granted 'exempt status' by the Institutional Review Board at the Virginia College of Osteopathic Medicine and all researchers were required to complete the National Institutes of Health (NIH) Office of Extramural Research course 'Protecting Human Research Participants'11. All participants were at least 18 years of age, were informed of the purpose of the focus group and completed a written informed consent prior to participating.
An experienced facilitator conducted the focus group sessions. A participatory style of focus groups was utilized using a semi-structured discussion guide with open-ended questions based upon the three broad questions listed above. Each focus group session was audiotape recorded and one or two team members recorded transcripts and observation notes throughout the session. No personal identifiers were associated with participant responses. The focus group sessions lasted approximately one to one-and-a-half hours.
Verbatim transcripts from the audiotapes, observation notes and demographic data were used for the data analysis. Data analysis was conducted using the Analysis Software for Word-Based Records v6.4 (AnSWR; Centers for Disease Control; Atlanta, GA, USA) developed for use in qualitative research. The analysis was conducted in a systematic manner utilizing specific coding procedures designed to build theory, facilitate the analysis raw data and to identify the conceptual building blocks of the theory12-15.
The interview questions served as a framework for organizing the data. Prior to the initial coding, three members of the project team reviewed the data and determined preliminary codes. A line-by-line analysis of the transcribed focus group interviews was then conducted and themes were identified. Themes were identified when several people within a focus group or from different focus groups repeated the statements or ideas, agreed either verbally or non-verbally or made similar statements. Following the initial coding, three members of the project team collectively reviewed a portion of the data to validate the accuracy and meanings of the codes. Additional codes were added as necessary. Concepts and their properties were identified and the structural relationships between subcategories defined. Diagrams and memos were then designed in order to visualize the interpretation, give direction for further data collection and identify relationships between categories. Finally, integration of major categories and the development of larger interpretation and theory was completed.
Three main themes emerged which impacted the healthcare utilization among underserved populations in Montgomery County, Virginia: (i) cultural perceptions of health care; (ii) perceieved barriers; and (iii) coping strategies. As is shown (Fig1), the data analysis revealed a relationship between cultural perceptions of health care, perceieved barriers and coping strategies. Participant perceptions of health care were often in conflict with their perceived barriers. This caused participants to develop specific coping strategies in order to achieve or maintain their desired health status. For example, most participants believed in their right to access quality healthcare services. However, due to financial constraints, few participants utilized routine preventive care and most reported recurrent use of emergency services. The end result of which was typically poor healthcare utilization leading to poor health status among the participants.
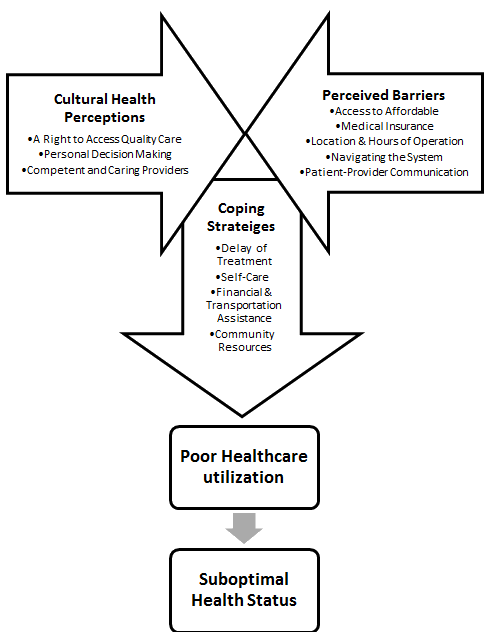
Figure 1: Experiences in healthcare utilization in Montgomery County, VA.
Cultural perceptions of health care
Three expectations emerged regarding healthcare services: (i) a right to access quality care; (ii) a conviction that personal healthcare decision making depended upon the individual's priorities; and (iii) a desire for competent and caring healthcare providers.
Most participants identified a right to access quality care. This was exemplified either by a sense of entitlement in which participants did not pay for services, or a sense of responsibility in which participants sacrificed to pay for services. For example, most participants viewed the Emergency Department (ED) as a 'free service' and as one single mother noted:
If you don't pay the ED hospital bills, they still can't refuse you when you go back.
In contrast, another participant stated:
I do without food or whatever else in order to pay the doctor's bill.
A generational gap also existed as participants discussed their right to access quality of care: elderly participants reported a sense of responsibility and would forgo other necessities in order to pay for healthcare services, while younger participants reported a sense of entitlement and often utilized healthcare services with no intent to pay for services.
Healthcare priorities varied among participants; however, the ability to make personal healthcare decisions for themselves and family members was important to most participants. Some participants identified a preference for basic necessities over healthcare and, as one noted:
When you have to pay your bills every month, health care is something you have to put off and put off.
Others valued preventative care, but noted a significant lack of access to preventative services such as annual exams, mammograms, eye exams or dental care and reported often suffering in chronic pain. Care for children remained a priority as most participants with children reported routine use of healthcare and case management services for their children and had a willingness to pay for these services out of pocket.
Finally, participants expressed a desire to receive health care from competent and caring providers. As one participant stated:
I want someone to understand what I need done and how soon it needs to be done... I need someone to sit down in a chair and look at me and listen to me.
Perrceived barriers
Participants identified barriers to nearly all healthcare services including primary care services, dental services, mental health services, medications, prenatal services, vision services, specialty care and diagnostic services. The perceived barriers to healthcare services reported by participants included: (i) limited availability of affordable care; (ii) lack of medical insurance; (iii) inconvenient locations and hours of operation for facilities; (iv) complicated medical care systems; and (v) poor patient-provider communication.
The financial and logistical complexities of utilizing the various types of health insurance options created a significant burden for participants. Regardless of payer status, medical insurance posed a significant barrier, often limiting their use of healthcare services. As one participant noted:
Insurance is what causes the problems. Here if you do not have access to insurance you do not have health care.
Many participants reported limited services due to their insurance status. As one noted:
I had to have 7 teeth taken out at once, Medicaid paid for it. All they would pay for is to knock me out and take the teeth out. Now I can't get them replaced. The doctor called it a demolition.
Other participants reported having 'disaster insurance', as one participant explained:
I have insurance, I'm lucky. But, I can't afford the deductible, so we only use it if we have to.
Limited hours of operation with extended wait times for appointments, limited service hours and requirements for advance scheduling were perceived by the participants as barriers to obtaining healthcare services. As one noted:
It takes a week to get an appointment if you're sick. It is faster if you go to the ED.
Limited public transportation, the lack of personal transportation, and the need to travel outside of the Montgomery County for care limited healthcare services for many participants. Several participants reported using an ambulance for transportation for medical services. As one noted:
We are transported to the ED by an ambulance; however, we do not have transportation home.
Poor patient provider communication and the complexity of navigating the healthcare system were also limiting factors in accessing healthcare services. Poor communication due to low levels of health literacy among participants, a perceived lack of cultural understanding among providers and a lack of interpretation services limited access to healthcare services. As one noted:
If they were already seeing a general doctor he would refer them to a heart doctor. It's complicated. It's much too complicated.
Coping strategies
Most participants developed coping strategies in order to overcome the perceived barriers to accessing healthcare services. These strategies included delaying treatment and self-care, seeking financial and transportation assistance and seeking assistance through community resources.
Participants shared a desire to be healthy. However, the majority of participants did not seek preventative care and as a result often lived in chronic pain or disability due to a delay in or lack of treatment. One participant when describing the consequences of her inability to access vision care stated, 'I just go blind, like I am'. Participants also utilized self-care strategies when delaying treatment such as purchasing over-the-counter medication and non-prescription reading glasses, and herbal remedies.
In order to pay for needed services, participants reported seeking financial assistance through charity care services and using discounted services or sliding fee scales. In order to access healthcare services when transportation became problematic, participants reported utilizing medical ride services, pharmacy delivery services, Medicaid and free clinic financial assistance and emergency ambulance services for non-emergent conditions. Participants were creative in seeking health services and used a variety of community resources including crisis pregnancy centers for pregnancy testing, the Lions Club for free eye-glasses, graduate student health centers for mental health and primary care services, free clinics for primary care services, the Health Department for prenatal services, the Department of Social Services for case management services, nurse triage phone services for care and treatment recommendations and family or friends for recommendations on care and treatment.
Discussion
Current data in the USA reflect increasing health disparities among underserved populations resulting in an increased necessity to improve access to healthcare services, provide culturally competent care and remove barriers to healthcare utilization16. Researchers often rely on epidemiologic and quantitative data to assess healthcare utilization. However, qualitative research which is designed to reveal a target population's behaviors and perceptions can provide further insight into community priorities for effective community health planning and improvement.
The inclusion of qualitative data collection and analysis within a greater community needs assessment provides an opportunity to focus on individuals and their relationship to the community, evaluate complex behavior and motivations and engage the community in the research process. Qualitative data can add value to quantitative measurements by providing a more detailed description of the community member's experience and can add vitality to program reports. Qualitative data can provide background information for strategic planning or can be used as part of an on-going surveillance program. Inclusion of qualitative data such as focus groups can provide insight into individual and community perceptions, beliefs, motivations and patterns of behavior. Healthcare delivery systems that address the perceived barriers to care can more effectively improve access to care. When used in the strategic planning process for the development of a FQHC, qualitative data can provide insight into patterns of healthcare utilization, identify individual differences within the community.
Appalachian communities in Virginia shoulder the burden of significantly higher rates of poverty and lower educational levels contributing to decreased access to preventive and medical care17,18. A 2006 Virginia Department of Health report recognized that the southwest region of Virginia is the most medically underserved region in the state19. Previous studies have shown that patients in Appalachia are less likely to obtain regular preventive screenings and are more likely to present with more advanced disease20,21. Our study revealed multiple perceived barriers that may contribute to those disturbing statistics. Participants reported having difficulty navigating a complex medical system without adequate insurance coverage for primary and preventive care. In addition, providers were perceived as not understanding their clients' needs and clinics were not open at times convenient for patients. These findings are consistent with previous studies which have reported a perception of a lack of available providers and clinics, particularly those who are American born and who are willing to stay in a community for a prolonged time22. Based on our results, culturally appropriate educational programs, extended hours and case management directed towards helping individuals navigate the healthcare system may encourage utilization of preventive services. The perceived barriers reported in this study must be addressed to ensure that the health center develops a successful medical model to care for the underserved in Montgomery County.
Limitations
This study is not without limitations. The focus groups discussions were designed to be influenced by group dynamics and facilitation and it is possible that quieter participants may have been inhibited by the more vocal participants and did not share their thoughts or opinions. Focus group discussions also rely on participant ability to accurately report their experiences and may be subject to human error or perspective. Because qualitative data collection can be subjective, they may be subject to human error and perspective.
Despite these possible limitations, the findings are a sample of the healthcare experiences in Montgomery County and provide a voice to underserved and indigent populations within the county. While it is not possible to use these results to characterize other areas of the Appalachian Highlands, the regional sample allows us to examine potential cultural barriers that could impede the effectiveness of a proposed FQHC.
This study was completed as part of the Bureau of Primary Care High Poverty Initiative Planning Grant and was funded by the Federal Bureau of Primary Care. The findings from this qualitative study assisted in addressing specific gaps in health care, identifying community strengths and understanding the challenges and complex needs of the community. As a result, the Virginia College of Osteopathic Medicine in collaboration with the Southwest Virginia Community Health Systems has submitted a grant application to the HRSA to open a FQHC in Montgomery County and are currently waiting on their review and feedback. If funding is successful, the health center will serve as a medical home to the many who currently lack access to care in the area.
Acknowledgements
The authors acknowledge the members of the steering committee, the director of Membership Services for Virginia Community Healthcare Association; the National Association of Community Health Centers; the CEO for Southwest Virginia Community Health Systems and other FQHC staff throughout VA who provided technical assistance and support during the project period. Funding for this project was provided by the Federal Bureau of Primary Care.
References
1. US Department of Health and Human Services, Health Resources and Services Administration, Bureau of Primary Health Care. Health Centers: America's Primary Care Safety Net, Reflections on Success, 2002-2007. Rockville, MD: Department of Health and Human Services, 2008.
2. Appalachian Regional Commission. The Appalachian Region. (Online) 2012. Available: http://www.arc.gov/reports/socio_report.asp (Accessed 10 April 2012).
3. National Center for Health Workforce Analysis. MUA/P Designations in Virginia. Rockville, MD: Shortage Designation Branch, HRSA Bureau of Health Professions, 2009.
4. USGS. Geological Provinces of the United States: Appalachian Highlands Province. (Online) 2012. Available: http://geomaps.wr.usgs.gov/parks/province/appalach.html (Accessed 10 April 2012).
5. Blackley D, Behringer B, Zheng S. Cancer Mortality Rates in Appalachia: Descriptive Epidemiology and an Approach to Explaining Differences in Outcomes. Journal of Community Health. (Online) 2011. Available: http://www.ncbi.nlm.nih.gov/pubmed/22101638 (Accessed 10 April 2012).
6. Barker L, Crespo R, Gerzoff RB, Denham S, Shrewsberry M, Cornelius-Averhart D. Residence in a distressed county in Appalachia as a risk factor for diabetes, Behavioral Risk Factor Surveillance System, 2006-2007. Prevention of Chronic Disease 2010; 7(5): A104. Available: http://www.cdc.gov/pcd/issues/2010/sep/09_0203.htm
7. Appalachian Regional Commission. 2004. Cancer Mortality in Appalachia. An Analysis of Disparities in Health Status and Access to Health Care in the Appalachian Region: An ARC Report. (Online) 2004. Available: http://www.arc.gov/assets/research_reports/AnalysisofHealthDisparitiesIntroductionExecutiveSummary.pdf (Accessed 10 April 2012).
8. Appalachian Regional Commission. Heart Disease Mortality in Appalachia. An Analysis of Disparities in Health Status and Access to Health Care in the Appalachian Region: An ARC Report. (Online) 2004. Available: http://www.arc.gov/assets/research_reports/Mortality_HEARTDISEASE.pdf (Accessed 10 April 2012).
9. Ezzati M, Friedman AB, Kulkarni SC, Murray CJL The reversal of fortunes: Trends in county mortality and cross-county mortality disparities in the United States. PLoS Medicine 2008; 5(4): e66.
10. Krueger R, Casey MA. Overview of Focus Groups. In: Focus Groups: A Practical Guide for Applied Research. Thousand Oaks, CA: Sage, 2009.
11. National Institutes of Health Office of Extramural Research. Protecting Human Research Participants. Bethesda, MD: National Institutes of Health, 2008.
12. Strauss J, Corbin A. Basics of Qualitative Research: Techniques and Procedures for Developing Grounded Theory. Thousand Oaks, CA: Sage, 1998
13. Hancock B. Trent Focus for Research and Development in Primary Health Care: An Introduction to Qualitative Research. London: Trent Focus Group, 2002.
14. Lacey D, Luff A. Trent Focus for Research and Development in Primary Health Care: Qualitative Data Analysis. London: Trent Focus Group, 2001.
15. Dudley T, Phillips N. Seven Steps to Analyzing Focus Group Data. Dallas, TX: UT Southwestern Medical, 2006.
16. Mead H, Cartwright-Smith L, Jones K, Ramos C, Woods K, Siegel B et al. Racial and Ethnic Disparities in US Healthcare: A Chartbook. Washington DC: The Commonwealth Fund, 2008.
17. Appalachian Regional Commission. The Appalachian Region. (Online) 2012. Available: http://www.arc.gov/reports/socio_report.asp (Accessed 10 April 2012).
18. McGarvey E, Leon-Verdin M, Killos L, Guterbock T, Cohn W. Health Disparities Between Appalachian and Non-Appalachian Counties in Virginia USA. Journal of Community Health 2011; 36(3): 348-356.
19. Virginia Department of Health. Chronic Disease in Virginia: A Comprehensive Data Report, Division of Chronic Disease Prevention and Control. (Online) 2006. Available:http://www.vahealth.org/cdpc/documents/2007/2006%20Chronic%20Disease%20Data%20Report_040607.pdf (Accessed 11 April 2012).
20. Hall I. Uhler R, Coughlin S, Miller D. Breast and Cervical Cancer Screening among Appalachian Women. Cancer Epidemiological Biomarkers 2002; 11(1): 137-142.
21. Fleming S, Love M, Bennett K. Diabetes and Cancer Screening Rates among Appalachian and Non-Appalachian Residents of Kentucky. Journal of the American Board of Family Medicine 2011; 24: 682-692.
22. Coyne CA, Demian-Popescu C, Friend D. Social and cultural factors influencing health in southern West Virginia: a qualitative study. Prevention of Chronic Disease. (Online) 2012. Available: http://www.cdc.gov/pcd/issues/2006/oct/06_0030.htm (Accessed 11 April 2012).
