Widely disparate cultures intersecting in the arena of the USA healthcare system provide opportunities for creative problem solving and personal growth. After completing a community needs assessment, such an opportunity was acted on by Saint Alphonsus Health Systems (SAHS) where a clinic was funded specifically to meet the complex perinatal and pediatric needs of refugees. Saint Alphonsus Health Systems comprises 4 rural hospitals, one urban medical center and several rural and urban health clinics located in the northwest region of the USA. A large 3 year grant from Trinity Health provided the funding for the initial development of a C.A.R.E. Clinic.
The C.A.R.E. (Culturally Appropriate Resources and Education) Clinic is a nurse-led clinical program that provides convenient, one-stop access to a seamless continuum of healthcare services and education provided in a group setting The clinic opened in 2009 at the Family Center located on the campus of Saint Alphonsus Regional Medical Center (SARMC) located in Boise, Idaho. The SARMC mission statement reflects its goal to provide compassionate care to vulnerable and underserved people. Boise is the largest urban city in the State of Idaho with a population of 620 000 living within a 45 min commute. The largely rural State of Idaho is ranked 14th of the 52 US states with an area of 214 044 km2 (82 643 miles2). Conversely, Idaho is ranked 39th for population, with 34% of Idaho's population living in rural areas1.
Opening the C.A.R.E. Clinic in a medium-sized urban setting provided the context to best establish new roles and good practices pertaining to refugee health care prior to rural expansion considerations. Refugees, who are some of the most disadvantaged and vulnerable healthcare consumers, are cared for in a culturally competent and culturally safe manner while receiving educational guidance to provide for their personal and their children's health and welfare as they transition into new lives in the USA. The success of the clinic is due, in part, to the implementation of a new role entitled C.A.R.E. Clinic Health Advisor. This new position was developed in conjunction with the organization and evolution of the C.A.R.E. Clinic. The purpose of this article is to describe and differentiate the roles of health advisor and certified medical interpreter (CMI). A study evaluating the lived experiences of the refugee women who are employed in these roles was conducted in the C.A.R.E. Clinic context and framed by the concept of cultural safety.
Background
A refugee is a person forced to flee his or her home due to a well-founded fear of being persecuted for reasons of race, religion, nationality, membership of a particular social group or political opinion, and who is unable or unwilling to return to his or her country of origin2. Boise, Idaho, is considered an open destination for refugees. That means refugees come to Boise if they have no known family in any other US city. Refugees from the Middle East, Far East, Asia, and many African countries have arrived in Boise over the past decade, bringing with them multiple languages and cultures.
Profound challenges are faced by refugees new to the USA. Some come from a refugee camp, having lived in the camp for more than 20 years. Some do not read or write in their own language and some do not understand the concept of numbers. Modern conveniences that appear simple to use, such as a can opener or frozen foods, are challenging for some refugees. However, some refugees are professionals who are familiar with Western culture. For most, however, navigating the US healthcare system can be frightening, based on prior experiences with the systems of their country of origin, in addition to propaganda regarding religion and politics in the USA3.
The challenges and barriers for refugees when navigating the US healthcare system may begin with transportation. With no assistance to learn the bus system or money for taxi services, clinic appointments have often been missed. Additionally, refugee patients often arrive in groups with all the arrivals expecting to be seen by a healthcare provider in a US system that is organized for individual appointments. Another barrier to refugee health care has been Medicaid application. Medicaid is a US government system of health insurance for those in need of financial assistance. Application for Medicaid insurance is often not initiated by a refugee or is initiated at more than one healthcare clinic, resulting in no payment for healthcare services rendered, or the patient being denied services due to lack of healthcare insurance. Contributing to this barrier is an application printed only in English. Assistance to complete the forms in a patient's preferred language may be unavailable. Reacting to missed appointments and no Medicaid insurance, the business sector of the US healthcare system has responded to these refugee challenges in ways that are monetarily beneficial to the institution and has refused care to many refugee patients. Even when care has been provided, a different provider is often seen at each visit and a CMI was not available, resulting in a refugee's personal medical history containing errors. As a result, refugees with non-emergent problems have frequented hospital emergency departments where they cannot be turned away.
Based on these needs observed by members of the SARMC healthcare team, focus groups were held with women from the refugee communities to identify and prioritize healthcare needs according to the refugee women's perceptions. Using input from these focus groups, the C.A.R.E. Clinic was organized and opened and the new role of health advisor was created to assist refugees in better coordinating and navigating the US healthcare system.
Conceptual framework
Ecological model
An ecological perspective (Fig1) was adapted from the National Cancer Institute's Theory at a glance: a guide for health promotion practice4. The double ecological model intersecting only at the community level provides structure in understanding the interaction of disparate cultures. In this instance, the disparate cultures are a refugee's culture and the culture of the healthcare team.
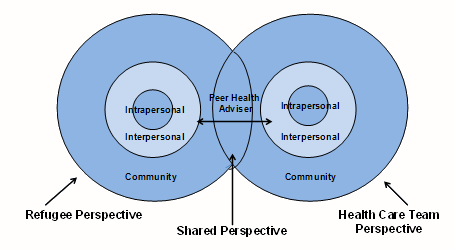
Figure 1: Conceptual framework: cultural safety in an ecological model (adapted from4).
A review of an ecological model shows three concentric circles. The Intrapersonal Level, or innermost circle, represents the individual characteristics that influence behaviors. For example, knowledge, attitudes, thoughts, beliefs and personality are individual traits. The Interpersonal Level represents processes and interactions with primary groups such as family, friends and peers. These interactions are a person's cultural and social support as well as his or her role definition. Finally, the Community Level represents institutional and community structures such as hospitals and refugee agencies. This level also encompasses the rules, regulations, policies, formal and informal structures that promote or inhibit behaviors that are recommended4.
It is at the level of community in the overlapping ecological model where a refugee's perspectives and the healthcare team's perspectives meet. A refugee patient brings to the meeting with a member of the healthcare team her lived experiences and knowledge of her culture. The member of the healthcare team brings his or her own cultural competence to the meeting. The health advisor is the rope that holds the model together because she brings knowledge of both the refugees' and health team members' cultures. The health advisor is able to move easily between both cultures because she brings knowledge of her lived experiences with her own people and knowledge of the healthcare structure where she is employed.
Cultural safety: The model of cultural safety is more than cultural competence4-7. Cultural competence is required in the US by The Joint Commission on Accreditation of Healthcare Organizations (JACHO)7 and supported by the American Association of Colleges of Nursing (AACN)8. Cultural competence, as described by Camphine-Bacote9, is a process for the delivery of health care that allows for growth, action and change. Cultural competence is composed of 'cultural awareness, cultural knowledge, cultural skill, cultural encounter and cultural desire' (p 1/1)9. This process-oriented model for practitioners implies that culture is dynamic and always changing among different and within same cultures9.
Cultural safety goes further than cultural competence by focusing on the power of healthcare systems and the healthcare professionals who work in the system. Cultural safety is predicated 'on understanding the power differences inherent in health service delivery and redressing these inequities through educational processes' (p 2)10. Cultural safety involves social change through partnership, participation and protection specific to vulnerable populations11. Cultural competence, however, does not address institutional power as a barrier for culturally diverse groups who access and navigate the healthcare system. Cultural competence does not raise the issue of reducing health inequalities for vulnerable populations12.
Two concepts specific to cultural safety that contribute understanding of the conceptual framework for this article are 'empowerment' and 'infrastructure'13. Empowerment, as conceptualized through the lens of cultural safety, levels the power differences in a provider-patient interaction. In an interaction between healthcare provider and refugee, there is a potential for acting on the inequality of power secondary to formal higher education and a vulnerable population without educational opportunities. Cultural safety implies that the refugee has a voice equal to that of the healthcare provider in how her health care is delivered. Indeed, cultural safety is defined by the recipient of care, not the provider of care, and involves participation, protection and partnership11,14. Infrastructure, as conceptualized by cultural safety, implies organization and structural facilities necessary to meet the cultural and healthcare needs of the refugee patient. Cultural safety claims that the people most able and equipped to provide such a culturally safe milieu are people from the same culture or community as the patient6. The role of health advisor contributes to a culturally safe infrastructure, thereby providing a physically, mentally, culturally and educationally safe context wherein refugees are empowered with voice, understanding and trust for the purpose of active engagement in their health care15.
Research design
A phenomenological interpretation within interpretivist thinking directed the methodology for studying the new role of health advisor. Phenomenological interpretivists seek to understand the complexity of lived experiences by collecting subjective data from which the researcher seeks to find meaning16.
Data collection
Qualitative data were collected to evaluate the lived experiences, efficiency and effectiveness of the role of health advisor. Data were collected from observations, focus groups, individual interviews with health advisors and members of the healthcare team. Quantitative data were collected from retrospective chart reviews for the purpose of validating patient healthcare outcomes. Data were collected from May 2009 to April 2011. A business model, a budget model and policies were also produced during this period. The business and budget models demonstrate clinic sustainability, with the largest expenditure being funding for health advisors and CMIs. Institutional review board approval was received from the medical center and the university.
Participants
During the first year of accepting patients into the C.A.R.E. Clinic, 14 C.A.R.E. Clinic Health Advisors were hired. Role descriptions of C.A.R.E. Clinic Health Advisor and CMI are provided (Fig2). During the following year of the clinic's operation, 5 health advisors moved out of the area or did not work due to personal issues. Four additional women were hired. As of 30 April 2011, the clinic had seen 227 (unduplicated) prenatal and pediatric refugee patients, each one receiving assistance from a health advisor who spoke the refugee's preferred spoken language and English. The C.A.R.E. Clinic schedules patient group appointments six times per month for prenatal care and four times per month for pediatric well-baby care. Languages spoken include Arabic, Burmese, Dari, Farsi, French, Karen, Kirundi, Lingala, Nepali, Pashtu, Russian, Somali, Swahili, and Uzbek. On average, 5 different non-English languages are spoken at each clinic.
One senior health advisor from the original group has taken on additional responsibilities including scheduling taxi transportation, education, and other office or community duties associated with the C.A.R.E. Clinic. She also received certification from The Cross Cultural Health Care Program (CCHCP)17 to train interested bilingual adults in the Boise area for competency to take the medical interpretation certification test.
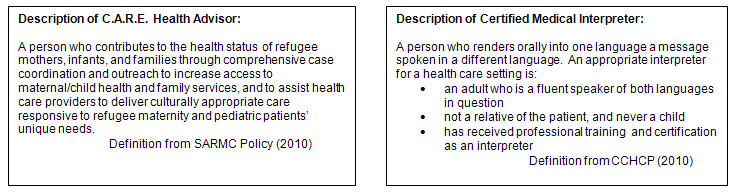
Figure 2: Comparative descriptions of C.A.R.E. Clinic Health Advisor and Certified Medical Interpreter17,18.
Clinic
Clinic structure: The idea and motivation for creation of the nurse-led C.A.R.E. Clinic came from three healthcare professionals: the nurse-director of the Family Center, a certified nurse midwife, and a Sister of the Holy Cross. Other members of the healthcare team currently associated with the C.A.R.E. Clinic include family practice physicians, certified nurse midwives, a pediatric nurse practitioner, registered nurses, a licensed case social worker, a dietician, medical assistants, and office staff.
Organization of the C.A.R.E. Clinic followed a classic logic model wherein the first year was for organization, equipment purchases or reallocations (eg weight scales, blood pressure monitors, exam table, lab supplies), curricular preparation for patient education, and personnel hiring including health advisors. At the start of second year, the clinic accepted its first patients. Adjustments and enhancements based on lived experiences contributed to continual improvement for patient care and cultural safety. During the third year of the clinic and the second year of accepting patients, the patient load continued to rapidly grow due mainly to the word-of-mouth from refugee patients. The state's refugee agencies also refer patients to the C.A.R.E. Clinic, but the growth occurs mostly from refugee referrals. The health advisor role also grew and evolved along with the growth of the C.A.R.E. Clinic. C.A.R.E. Clinic Health Advisors meet weekly for 2 hours with the C.A.R.E. Clinic director to discuss clinic issues and process. Meeting agendas may include discussions about role differentiation and rule compliance, development of additional responsibilities, or continuing education on new topics.
The C.A.R.E. Clinic is located in the Family Center, an out-patient building on the campus of the regional medical center. The clinic has easy access on the first floor. The mission for the Family Center is community service, including education and support for young families. Within the Family Center, the C.A.R.E. Clinic uses a large meeting room that is divided into two rooms with the largest portion used for group education. Chairs are assembled in a circle for the prenatal clinic, while clean sheets are spread on the floor for the pediatric clinics so that active babies have freedom to explore. Back rests are provided for mothers who sit on the floor with their babies. The other side of the partitioned room is for individual provider care for patients. A door-sized opening in the partitioned wall provides easy movement between the two sections of the clinic. Relaxing, soft music is played in the provider room to muffle provider-patient conversations, thereby respecting confidentiality. The music also enhances a milieu that supports refugee patients' feelings of comfort and safety. During the clinic hours, additional rooms are utilized in the Family Center, including a room for an incentive store and a kitchen for nutrition classes.
The clinic is decorated with art from refugees' native countries. A large map noting the native homes of all refugees hangs on a prominent wall. To assist the families, an incentive store is stocked with diapers, recycled and new children's clothing, baby necessities and personal hygiene necessities for mothers. Points for shopping in the incentive store are earned during clinic visits for such actions as appointment timeliness, good nutrition, and participation in healthcare services and education. Each clinic is scheduled for 2 hours. The average group size for each scheduled appointment is 10 patients.
Role descriptions
Discoveries and analyses of the health advisor role occurred simultaneously according to best qualitative research practices17. Analysis and discussion of those findings are presented in this section in three parts. The first part describes and differentiates the roles of the C.A.R.E. Clinic Health Advisor and CMI based on observations, hospital policies and federal mandates. The second part is an analysis of the lived experiences of the health advisor using data collected from focus groups, observations and individual interviews. The final part validates the effectiveness of the role of health advisor using quantitative data from retrospective reviews of patient chart.
Describing and differentiating roles: Discriminating between the different roles of health advisor and CMI was challenging for both the health advisor and the healthcare providers because most, but not all, of the health advisors are also CMIs. Both roles involve fluency in English and the patient's preferred spoken language. Confusion, therefore, was common until written descriptions were created. This section answers the question: What are the job descriptions for a CMI and a C.A.R.E. Clinic Health Advisor?
Certified Medical Interpreter: The need for a certified medical interpreter in the US is grounded in law. The legality of CMIs is in the 1964 Civil Rights Act which states that for any medical institution that accepts Medicaid, Medicare, federal grants or federal funding of any kind, the consequence of not using a 'certified' medical interpreter means the risk of losing all federal funds16. The regulations for CMI relate to language skills, ethics, cultural issues, and healthcare terminology. A CMI should provide only a literal translation of the communication between the patient and the provider. A CMI cannot ask a follow up question or explain cultural differences. These rules and regulations are much different from the job description of health advisor. Because many of the health advisors are also CMIs, there was often confusion for the health advisors as well as the healthcare team regarding the tasks and the law. Comparative descriptions of health advisor and CMI are provided (Fig2).
Peer health advisor: The paid position of health advisor is covered by a hospital contract that has been reviewed by the hospital's legal department. Competencies expected of a health advisor include those expected of all employees in the medical center: professionalism, knowledge of professional boundaries, cultural competence, patient safety and confidentiality as designated by the 1996 US Health Insurance and Portability and Accountability Act (HIPAA). Responsibilities specific to the health advisor job include the following:
- assist healthcare team members to build cultural knowledge and skills
- assist maternal and pediatric refugee patients with scheduling for provider appointments and educational classes
- support refugee patients in confronting barriers to healthcare access such as Medicaid insurance and transportation.
- advise refugee patients of Western medicine protocol, expectations and standard procedures
- build relationships with community partners to increase referrals for care and education of refugees
- support refugee patients to follow through on medical referrals for specialized care
- assist families of refugee patients to self-identify other health needs and resources
- support refugee families to find and transition into a medical home.
The health advisors are increasingly involved in preparing curriculum and teaching during the education section of the C.A.R.E. Clinic. Education topics presented at the 2 hour C.A.R.E. Clinics are to assist the refugee patients in skills needed in the USA, such as using transportation, home safety, and nutrition. Numerous refugee patients are amazed at iron-fortified dry cereal, white bread in a plastic bag, food in cans (and how to open them), dollars and cents, pounds versus kilograms. The refugee patients also learn about their pregnant bodies and healthy parenting.
Teaching in the C.A.R.E. Clinic is delivered with dialogue education as presented by Jane Vella19,20. Vella grounds her praxis in Paulo Friere's21 writings of problem based learning. Friere regarded the needs of the learner as the source of learning motivation. Based on writings from Friere, Vella stated that 'teaching with dialogue education involves listening to learners at every level, respecting them as decision makers of their own learning, and evoking their innate power' (p xix)20. Dialogue education contributes to empowering refugees, and empowerment is a component of cultural safety. One health advisor noted that 'unknown things are captured through stories'. It is the dialogue and the stories that capture and hold the learner's attention, thereby enhancing her knowledge; the learners are both the refugees and members of the healthcare team.
Finally, only women can apply for the position of health advisor for the prenatal and pediatric C.A.R.E. Clinic because refugee women in the C.A.R.E. Clinic have experienced trauma in their home countries and many come from patriarchal, gendered cultures. Therefore, the positions of health advisor and CMI must be culturally safe.
In conclusion, there are several languages and dialects spoken during every educational session. It is exciting to sit in a room and begin an educational dialogue with an anticipatory question stated in English and then hear a buzz around the room as many rare non-English languages are simultaneously spoken. Then the room quiets and a question or a response is stated in English so that a difficult concept can be explained, a question asked or a story shared. The role of health advisor contributes to a culturally safe healthcare infrastructure that empowers refugees.
Data analysis
To evaluate the lived experiences of the role of health advisor, focus groups were held with 7 health advisors who work for the C.A.R.E. Clinics. All of the health advisors in the focus group also work as CMIs. Consent forms were signed and the discussions were audio recorded. Questions for the focus group included the following:
- How would you describe your role as a C.A.R.E. Clinic Health Advisor?
- How would you describe your role as a certified medical interpreter?
- What are the strengths and weaknesses of each role?
- What would you change in each role?
The main themes emerging from the focus group included communication, navigating the system, and community. Together, the themes elicit the notion of trust and the valuing of self. Following is the individual analysis of each theme.
Communication
The importance of the health advisor role was recognized as important for cultural safety as evidenced by the following statement regarding a stronger refugee voice. It reflects understanding of the power differences between the culture of the refugee and the culture of the healthcare system.
C.A.R.E. Clinic Health Advisors help the healthcare workers understand different cultures and make the refugee's voice stronger.
The health advisors also expressed the burden and pride of their responsibility for their refugee communities. Being fluent in speaking English and a refugee's preferred spoken language provided community recognition for the health advisors as leaders for the women, as noted in the following quotation:
The people chosen to be health advisors were already playing the role within their communities before the role was created.
On the other hand, creating a job and giving it the title of health advisor sometimes created hardships for the health advisor. One health advisor stated that she often turns off her telephone when she is at home so that she can focus on her family without so many interruptions.
Finally, the caring and friendship extended to the refugees by the health advisors through communication is the basis for bridging the cultures and establishing trust in the healthcare system.
You work with the same person; you know their issues. People don't have to wonder where to go.
People call me asking what I think. They think that you can solve everything and it's hard for them to see if they are talking to you as a friend or a health advisor.
The biggest challenge for the health advisor is that the role is not given the same respect and power as that of CMI, as noted in the following health advisor quotations.
If you are not an interpreter, then you cannot go into the room with the doctor and patient and the doctor can't share information with you. Many times refugees don't understand what the doctor is saying and will say 'yes' to everything.
It's a different type of communication between the health advisor and certified medical interpreter. [As a CMI] You have to follow the guidelines for the role because you get too busy and worked up.
As interpreter, people ask what you think and you are unable to tell them.
Navigating the system
The following statement validates the importance of the health advisor role in communication and cultural understanding in navigating the healthcare system.
When you are only a health advisor you can't translate in the hospital, so there is a breakdown in communication because the healthcare worker can't tell and the patient is usually confused. You need a health advisor for all refugees because the case managers cannot do that job.
Many of the health advisors are refugees and have experienced traumatic events similar to those of the current patients. It is the health advisor who understands and encourages those questions that a patient may be embarrassed to ask. For some, that embarrassing question may be about transportation to and from the clinic. It is a problem frequently forgotten in our healthcare system, and it is the one of the first areas that a health advisor assists the refugee, as indicated in the following statement.
Now we can call for their transportation and remind them to make sure they come to their appointments.
Other observed barriers rooted in lack of experience and understanding in navigating the Western healthcare system included using the elevator to access specialty care on the second floor or fears that their blood was being drained when prenatal blood tests were drawn. The following statements reflect the importance of a health advisor in place of a case manager trained with a different skill set.
If you explain why different things are being done, then they [refugee patients] will be more likely to do them after they are taught in the clinic, making the teaching prevention useful.
Help healthcare workers to have a better understanding of the cultures that we work with.
We help [refugee patients] accept the new ideas of the US health system, like sharing ideas and being open and honest.
Community
The last theme from the focus group revolved around community. The health advisors spoke about passion for their communities. 'Community' for the refugees, however, takes on a larger scope than merely the place where they live. The environment of the C.A.R.E. Clinic creates a community of maternal and pediatric patients within the context of receiving health care and education. Pregnant women who initially would not make eye contact with anyone, within 2 weeks have been observed to be smiling and chatting with the other patients. Some of the following statements reflect pride the health advisors feel regarding their role in intervening and making suggestions that contribute to cultural safety for the refugee patients.
It's passion. You get paid more somewhere else with less work. But as a health advisor I have more voice. [With] information [and] knowledge, they [refugees] will do better. As a health advisor you can have a personal relationship, whereas an interpreter, you can't do that.
In the clinic, you get people from different communities together so they do not feel that they are the only ones with that problem.
Even if they don't have insurance, they can still attend the educational classes.
It is easier as a health advisor because we can have better connection with people. They have more trust because they feel it is somebody that is from their own community [rather] than just the healthcare provider.
I think we are a bridge between our community and the healthcare system.
Summary
The roles of CMI and health advisor each help increase the effectiveness of communication between the refugee and healthcare provider, but each role provides unique elements. The CMI role was viewed by most of the health advisors as a tool, often without human characteristics, as noted in the following quotation from a health advisor and CMI:
As an interpreter, I feel like I'm a machine. I do not see the value in myself. I don't have that self-satisfaction. But as a health advisor, I feel that value in myself. I can help people more. I don't feel like a machine.
The role of CMI does not allow for depth of understanding between the refugees and the healthcare provider because the interpreter cannot interpret culture, only words. Interpreters feel that this decreases the effectiveness of the communication, especially because the health advisor comes from the same refugee community as the patient and assists the refugees in overcoming barriers to successfully navigate the healthcare system. Their efforts also help establish a safe environment where a community of women is formed.
Retrospective chart reviews
Data from retrospective patient chart reviews that reflected on the success of the health advisor role included a drop in the 'no-show' rate, or missed clinic appointments, from 25% to 2.5%. The major reasons behind the high rate of missed appointments was the lack of transportation due to refugees not understanding the bus system, unable to afford a taxi and language barriers. The C.A.R.E. Clinic Health Advisors now remind the clients in their preferred spoken languages regarding appointment dates and times. Taxi services are arranged for each appointment but are only partially reimbursed by Medicaid, so refugee patients are encouraged towards independence in travel. With a decrease in language and transportation barriers, and as the no-show rates decreased, childhood immunizations are at 100% compliance through a baby's first year of life. The authors are confident that the role of C.A.R.E. Clinic Health Advisor has contributed to these outcomes.
Discussion and recommendations
The establishment of new roles as described in the C.A.R.E. Clinic is an important step in modeling a culturally safe method to meet the healthcare needs of the vulnerable, displaced refugee. Providing a sustainable healthcare clinic in a setting that provides opportunities for education and socialization in addition to health care is a model that assists patients and families to assimilate. It is also a model that recognizes the power of the patient to enhance her personal and her family's health.
The C.A.R.E. Clinic model and health advisor role are adaptable for other vulnerable populations such as migrant farmers, the socioeconomically disenfranchised, the elderly and other rural populations. This fits within the community mission for SARMC and the SAHS. A tool kit to assist in adapting this model is being developed.
This study has shown that the C.A.R.E. Clinic structure provides an increase in bi-directional cultural understanding, human caring, social justice and trust. For many who work in the clinic, these intangible elements have become their own rewards. The new role of health advisor as described through the framework of ecology and cultural safety has the potential to mitigate stress and enhance personal health by empowering the patient through voice, health care and education.
Acknowledgement
C.A.R.E. Clinic is a trademark of Saint Alphonsus Regional Medical Center in Boise, Idaho, USA, and may not be used without permission.
References
1. US Census Bureau. Idaho. Available: http://quickfacts.census.gov/qfd/states/16/1608830.html (Accessed 12 May 2011).
2. United Nations High Commission for Refugees. Convention and 1967 protocols relating to the status of refugees. Geneva: UNHCR, 1996.
3. Idaho Office for Refugees. Information and resources, 2011. Available: http://www.idahorefugees.org. (Accessed 12 May 2011).
4. National Cancer Institute. Theory at a glance: a guide for health promotion practice, 2nd edn. US National Institutes of Health no T052. (Online) 2005. Available: http://www.cancer.gov/cancertopics/cancerlibrary/theory.pdf (Accessed 7 December 2011).
5. Richardson S, Williams T, Finlay A, Farrell M. Senior nurses' perceptions of cultural safety in an acute clinical practice area. Nursing Praxis in New Zealand 2009; 25(3): 27-36.
6. Williams R. Cultural safety: what does it mean for our work practice? (Online) 1998. Available: http://www.ruralhealth.utas.edu.au (Accessed 6 October 2010).
7. Duke J, Connor M, McEldowney R. Becoming a culturally competent health practitioner in the delivery of culturally safe care: a process oriented approach. Journal of Cultural Diversity 2009; 16(2): 40-49.
8. Calvillo E, Clark L, Ballantyne JE, Pacquiano D, Purnell LD, Villarruel AM. Cultural competency in baccalaureate nursing education. Journal of Transcultural Nursing 2009; 20(2): 137-145.
9. Campinha-Bacote J. The process of cultural competence in the delivery of healthcare services. (Online) 2002. Available: http://www.transculturalcare.net/cultural_competence_model.htm (Accessed 8 September 2008).
10. Hart-Wasekeesikaw F. Cultural competence and cultural safety in First Nations, Inuit and Metis nursing education: an integrated review of the literature. Ottawa, ON: Aboriginal Nurses Association of Canada, 2009.
11. Ramsden I. Improving practice through research. Kai Tiaki, Nursing in New Zealand 2001; 7(1): 23-26.
12. Mortensen A. Cultural safety: does the theory work in practice for culturally and linguistically diverse groups? Nursing Praxis in New Zealand 2010; 26(3): 6-16.
13. Clear G. A re-examination of cultural safety: a national imperative. Nursing Praxis in New Zealand 2008; 24(2): 2-4.
14. Richardson S, Williams T. Why is cultural safety essential in health care? Medicine and Law 2007; 26(4): 699-707.
15. Street RL, Haidet P. How well do doctors know their patients? Factors affecting physician understanding of patients' health beliefs. Journal of General Internal Medicine 2010; 26(1): 21-27.
16. Schwandt TA. Constructivist, interpretivist approaches to human inquiry. In: NK Denzin, YS Lincoln (Eds). Handbook of qualitative research. Thousand Oaks, CA: Sage, 0000; 118-137.
17. Cross cultural health care program. Introduction to medical interpreting. Seattle, WA: CCHCP, 2010. Available: http://www.xculture.org (Accessed 11 February 2010).
18. Saint Alphonsus Regional Medical Center. Description of services for health care advisor. In: Contract Agreement for Health Advisor. Boise, ID: SARMC , 2010; 2/2.
19. Vella J. Learning to listen, learning to teach: the power of dialogue in educating adults (revised edn). Indianapolis, IN: Jossey-Bass, 2002.
20. Vella J. On teaching and learning: putting the principles and practices of dialogue education into action. San Francisco, CA: Jossey-Bass, 2008.
21. Friere P. Pedagogy of the oppressed. New York: Herder and Herder, 1972.


