Like other geographically large, developed countries, over the last 3 years the USA has grappled with significant challenges and reforms to the healthcare system in an attempt to improve national health outcomes while reducing costs and disparities1. Proposals in the Patient Protection and Affordable Care Act 2010 that are under consideration, or currently being implemented, include increasing health insurance coverage, promotion of innovations in healthcare delivery that support primary prevention, and reimbursement for patient-centered and personalized approaches to care. Although some policy analysts believe rural Americans will benefit from proposed changes in the Affordable Care Act2,3, the actual consequences of these reforms for rural individuals and families largely remain to be seen. In particular, reforms must actively address the considerable disparities in rates of chronic disease such as diabetes, obesity, hypertension, and coronary heart disease4,5, as well as receipt of preventive services like mammograms, Pap smears, and colorectal cancer screening5. Further, evidence suggests that rural areas will face increased difficulties in the coming years due to growing economic hardships and provider shortages6, and these must be considered when attempting new approaches to care.
Attending to the distinct nature of health and health-related issues in rural communities will be critical to implementing large-scale healthcare reform. Individuals and families residing in rural communities are unique in terms of their access to and utilization of heath care, especially when compared with their urban counterparts7,8.These differences can be broadly categorized into issues that are structural or cultural in their design or origin7, and may include factors that are perceived as strengths as well as barriers9. Structural issues include, but are not limited to: higher rates of healthcare underinsurance10,11 and uninsurance10,12, limited access to primary and specialty providers13, and time and transportation costs associated with traveling far distances for care14,15. Further, factors such as high unemployment rates, low community level education status, and an imbalance of young-to-old members can strain rural communities and lead to community level disenfranchisement8.These structural issues go hand in hand with poverty. Rural areas of the USA experience higher rates of poverty than urban areas (15.1% vs 12.9%)16. Further, persistent poverty, defined as a poverty rate of 20% or greater for at least four consecutive decades is primarily a rural phenomenon, and 88% of counties experiencing persistent poverty in the USA are rural17. Problems of healthcare access are exacerbated for rural families living at or near the poverty line due to the aforementioned structural barriers. In fact, structural barriers may be the primary explanation for the differences in the health status of low-income urban and rural residents8
Rural communities also have unique cultural issues that contribute to utilization of and access to health care7. As with any culturally distinct group, place of residence informs individual and community level perceptions, beliefs, and values regarding a range of issues, including health care18. For example, an ethic of self-reliance, which may have been cultivated due to distance from healthcare facilities or lack of access to healthcare providers, may contribute to rural individuals forgoing care or relying on self-care practices15. Rural residents also may rely on informal supports when coping with health-related challenges7,15 as the result of a strong sense of belonging or connection with others in their community, particularly during times of stress19. The cultural ethos of independence or self-reliance can be viewed as a strength, because it may prevent needless health-related expenses (eg going to a clinic for issues that do not warrant medical attention), and promote personal responsibility. However, independence and self-reliance may be problematic if they lead to later diagnosis of serious conditions, such as cancer or diabetes20.
While structural and cultural factors are key considerations for healthcare reform in rural areas, understanding the individual characteristics of rural individuals and families is a critical component of determining how rural residents manage their health21. That is, individual characteristics and behaviors, and how they are uniquely realized in contexts such as the rural community, must be considered when evaluating the potential efficacy and implementation of health reforms. For example, to derive benefit from health services, there are specific actions individuals must take to effectively manage their health and health care, such as seeking and accessing an appropriate provider when medically necessary22. So, while a primary component of the Affordable Care Act is to increase health insurance coverage, and research has shown that rural women who have health insurance are more likely to utilize health care23, simply having coverage does not ensure access. The intermediate step of seeking and accessing care is required. However, in a rural context, access may be tempered by structural, cultural, and/or individual factors than prevent health-promoting behaviors.
Although structural and cultural barriers in rural areas have been well documented in the USA and abroad (eg Canada and Australia), more limited research has been conducted on the individual factors influencing the management of health, especially from the voices of rural residents themselves. Thus, the goal of this study was to explore the experiences of low-income women's management of health conditions in rural communities. Specifically, mixed methods were used to explore the: (i) types and perceived severity of health conditions rural, low-income individuals report; (ii) perceived value and utilization of a usual source of care; and (iii) strategies these individuals employ to manage their health. The findings may be used to inform the design, implementation, and evaluation of healthcare reforms that attend to the unique challenges and strengths faced by rural Americans and their counterparts abroad.
Data were analyzed from a 16 state, US study of rural low-income women and their families, known as 'Rural Families Speak' (RFS). The RFS participants were recruited via fliers posted at places frequented by low-income residents such as Women, Infants and Children programs, food stamp and welfare offices, secondhand stores, public health clinics, and through referrals by county extension agents. The RFS enrolled 413 women in panel 1 and another 58 women in panel 2 between 2000 an 2001 who met the following inclusion criteria: 18 years and older; least one child under age 14 years living in the home; and household incomes of less than 250% of the federal poverty line (US$42,645 US for a family of four). The 250% threshold was established, because for participating states this was the highest state eligibility cut-off for access to Food Stamps and the Supplemental Nutrition Program for Women Infants and Children, which are federally funded programs that are managed at the state level. US Department of Agriculture Rural-Urban Continuum Codes (RUCC) were used to define 'rural'24, and participants lived in counties ranging from code 6 (urban population of 2500 to 19 999 adjacent to a metropolitan area) to 8 (completely rural or < 2500 urban population, adjacent to a metro area). The protocol was approved by the institutional review boards of all participating universities. Trained interviewers collected quantitative and qualitative data in semi-structured interviews in three waves annually between 2000 and 2003.
Chronic health conditions for participants and their partners (if applicable) were measured using the Adult Health Survey, which recorded self-reports (yes/no) for 15 health conditions, based on Sturm and Wells'25 study of morbidities associated with poverty, including: arthritis, asthma, back problems, bladder infections, cancer, chronic pain, diabetes, heart problems, hepatitis, high blood pressure, liver problems, migraines/headaches, permanent disability, reproductive problems, and seizure disorder. Pediatric chronic conditions were reported via the Child Health Survey, which was a maternal report (yes/no) of health conditions for each child, including: allergies, asthma, anemia, depression/anxiety, digestive problems, attention deficit/hyperactivity disorder, migraines/headaches, diabetes, cancer, and permanent disability.
Self-reported medication adherence for adults and children was measured by dichotomous variables (yes/no) assessing whether in the last year the participant delayed or did not fill medication prescribed by a healthcare provider, and whether in the last year the participant used medication differently from the way it was prescribed.
Having a usual source of care was assessed by asking the participant, 'Do you have a doctor or other healthcare professional that you usually see?' (yes/no). Each participant also responded to the same question for her partner ('Does your partner...') and for each child in her household ('Does your child...'). After each of these questions was asked, beliefs regarding the value of a usual source of care were assessed with the follow-up question, 'Do you think always seeing the same person influences your/ your partner's/ your child's health?' (yes/no) and then further explored with an open-ended response explaining her answer to the question.
Qualitative data included responses to open-ended questions about usual sources of care and health management practices. All qualitative data were digitally recorded and transcribed into rich-text documents. Participants either chose a pseudonym themselves, or had the study team provide one for them.
Data analysis
Mixed-methods were employed by triangulating the quantitative and qualitative data26. Year 3 data only were used from both panels (N=271) for this analysis, because there was a more extensive health survey in the RFS protocol. From the quantitative data SPSS v15.0 (www.spss.com) was used to generate frequencies of the number of chronic conditions reported by the participant for herself, her partner, and her children. Also tabulated were responses to questions on whether the participant reported having health insurance, identified a usual provider, believed her health interfered with activities of daily living (ADL), and adhered to prescription medications.
The qualitative data analysis generated a detailed description of how respondents managed health issues. Given the large sample size, a sub-sample was drawn for the qualitative analysis. To allow for the detection of thematic differences by insurance status, SPSS was used to randomly select 45 participants representing three health insurance statuses - privately insured, publicly insured, and uninsured - based on previous studies showing both insurance status and type of insurance affect healthcare utilization27,28. One interview transcript in the uninsured group did not follow the interview protocol, so this participant was excluded, leaving a qualitative sample size of 44 participants.
An integrative secondary thematic analysis of interviews was employed following procedures outlined by Burck29. To generate initial codes, the data were prepared by selecting 'fragments of text' (p249) from transcribed interviews about the central foci of this study, health conditions and their management. Three researchers reviewed the compiled data to organize the initial codes into themes, review the themes to ensure consistency with the initial coding, generate clear definitions of the themes by refining and naming them, and linking them to examples30. Strategies were followed recommended by Lincoln and Guba to bolster credibility, confirmability, transferability, and dependability of the findings31.
Quantitative
Demographics: The demographic data reported below represent the participants providing complete quantitative year 3 data (N=271). Appropriate analytic techniques (eg χ2 for categorical and t-tests for continuous variables) were applied to test for statistically significant differences between the participants included in the qualitative sub-sample (n=44) and the wave 3 participants not included in the qualitative sub-sample (n=227). Comparisons between these two groups are provided (Fig1) with statistically significant differences indicated where present. As a whole, the average age of participants at wave 3 was 31.9 years (SD=7.7). Almost two-thirds identified as non-Hispanic White (66%), followed by 20.8% Latina, 6.4% Black, and 5.6% other. The majority of participants was married (46.5%) or living with a partner (17.0%), while less than half were single (19.2%), divorced (11.1%) or separated (6.3%). A quarter of participants had less than high school education with 7.9% reporting an education level of 8th grade or less and 16.6% reporting some high school. Over a quarter had earned her high school diploma or General Education Development Test (GED; 28.7%). More than 4 out of 10 participants (43.0%) reported training beyond high school in the form of specialized technical, business, or vocational training (15.5%) or some college (27.5%). The remaining 3.8% were college graduates. On average, participants reported a household income at 136.2% of the federal poverty line (sd=93.04). Comparisons between the participants included in the qualitative sub-sample and those who were not yielded no statistically significant differences between the two groups on the above demographic characteristics.
As a whole, there was a 29.1% healthcare uninsurance rate among women in the sample. The qualitative sub-sample did not significantly differ from those not included in the sub-sample. Within the qualitative sub-sample, 31.8% were uninsured, 34.1% were privately insured, and 34.1% were publicly insured. Similarly, among those not included in the sub-sample, 28.5% were uninsured, 29.0% were privately insured, and 40.7% were publicly insured (Fig1f). Within the total sample, of those who were insured, 33.0% had private insurance, 64.2% had public insurance (eg Medicaid, state plan), and 2.8% had other insurance. Among partners, there was a 30.4% healthcare uninsurance rate, with 40.7% of partners of participants included in the qualitative sub-sample lacking insurance compared with 28.4% of other partners (Fig1g). These differences were not statistically significant. Of the insured partners, 68.2% had private insurance, 30.0% had public insurance, and 1.8%% had other insurance. Among children, the uninsurance rate was 11.6% with 68.6% of insured children on public insurance (Fig1h).

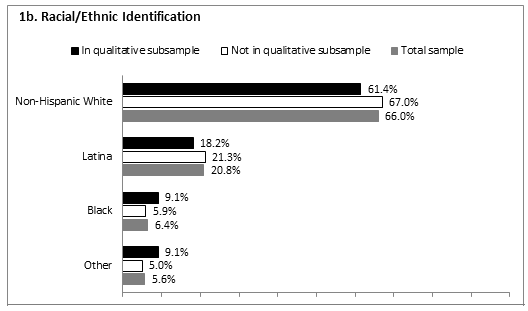
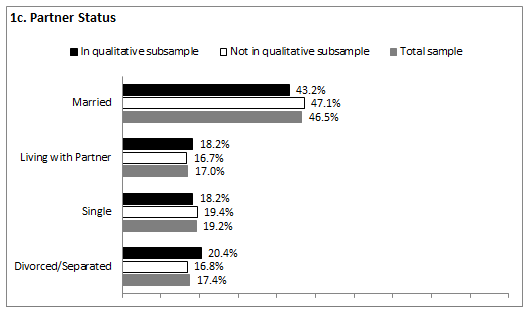
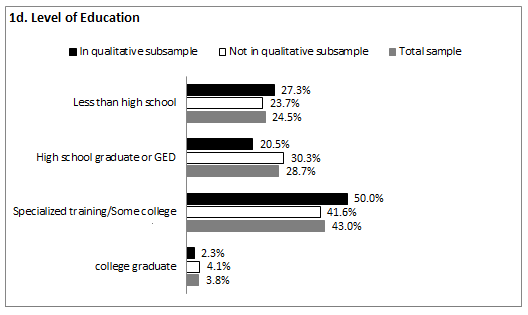
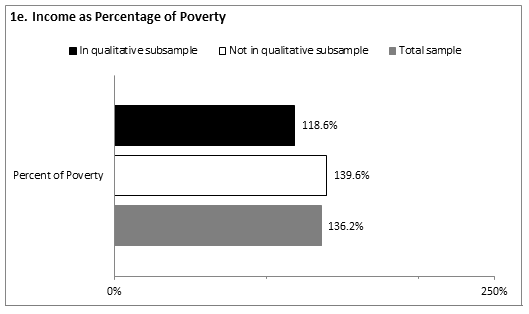
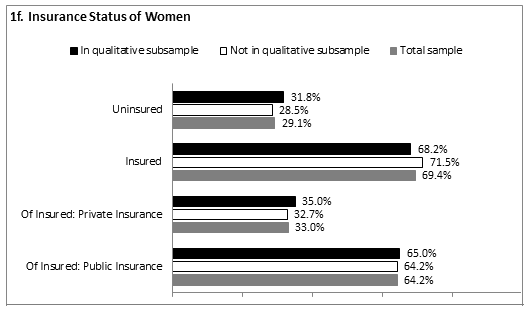
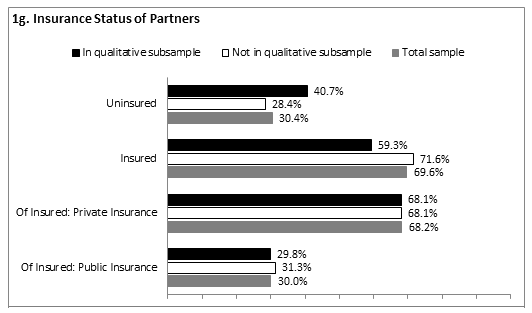
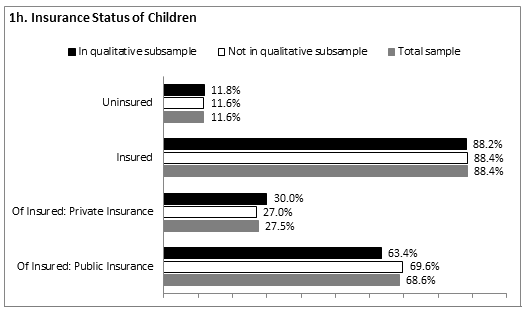 Figure 1: Demographic characteristics of sample (n=271). a: Mean age of women; b: Racial/ethnic identification; c: Partner status; d: Education level; e: Income as percentage of poverty; f: Insurance status of women; g: Insurance status of partners; h: Insurance status of children.
Figure 1: Demographic characteristics of sample (n=271). a: Mean age of women; b: Racial/ethnic identification; c: Partner status; d: Education level; e: Income as percentage of poverty; f: Insurance status of women; g: Insurance status of partners; h: Insurance status of children.
Medication adherence: The summary statistics on medication adherence for adults and children in the participant households are shown (Fig2). There were no statistically significant differences on any of these variables between the total sample and the qualitative sub-sample. Among all adults (women and partners) in the total sample, 30.4% reported delaying or not filling medications prescribed by a healthcare provider. The prevalence was 22.5% in the qualitative sub-sample. For all children in the total sample, 5.2% of parents reported delaying or not filling prescription medications; in the sub-sample the rate was 1.1%. Regarding use of medication differently than prescribed, 9.8% of the participants/partners in the total sample reported 'yes', and 13.5% of the qualitative sub-sample reported 'yes'. Compared with adults, the prevalence of using medication differently than prescribed was lower for children in both the total sample (4.3%) and qualitative sub-sample (7.0%).
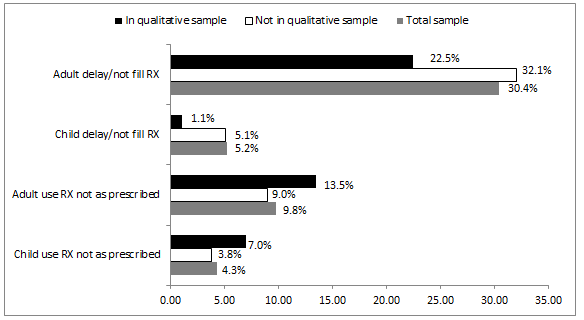 Figure 2: Medication adherence (n=271).
Figure 2: Medication adherence (n=271).
Health conditions: Summary statistics for health status among the participant families are presented (Fig3). The majority of participants (85.7%) reported having at least 1 chronic health condition (range 0-15); 43.8% reported managing 2-4 chronic conditions and 22.4% reported managing 5-15 chronic conditions. Interestingly, despite the high number of self-reported chronic health problems, 32.4% stated their health was 'very good' or 'excellent', and 46.9% stated their health was 'good', while 20.6% stated their health was 'fair' or 'poor'. The majority of participants (55.9%) did not perceive health to have improved over time with more than half rating their health as 'the same' (40.3%) or 'worse' (15.6%). Only 17.5% of participants reported their health was 'much better' than the previous year, while 26.6% of participants rated their health as 'somewhat better' than the year before. When asked to what extent their health has interfered with ADL, 53.3% reported 'not at all,' while 11.1% responded 'quite a bit' or 'extremely', and 35.6% reported 'slightly' or 'moderately'. The quantitative findings suggesting health did not improve over time are hypothesized to contribute to a lack of engagement in health management, a theme identified in the qualitative data.
Participants managed multiple health issues within their families. The majority of families (71.1%) had at least 2 family members with a chronic condition. Among partners, 41.9% had at least one chronic health condition (rage 0-8). Over half of the participants (56.6%) reported having at least one child with at least one chronic health condition (range 0-5). Of these, 35.3% reported having 2 children with a chronic health problem and 8.0% had 3 children with a chronic condition. The median number of chronic health conditions within a family was 4 (range 0-27). Examining the family as a unit, 42.1% reported 1-4 conditions, 31.4% reported 5-8 conditions, and 17.7% reported 9 or more conditions within the family.
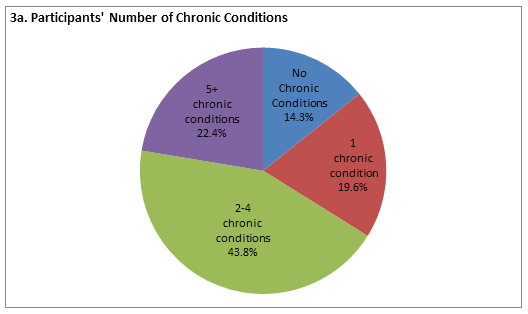
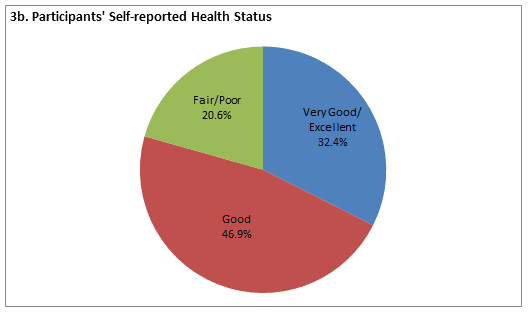
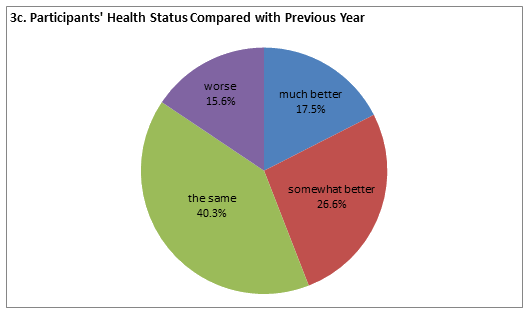
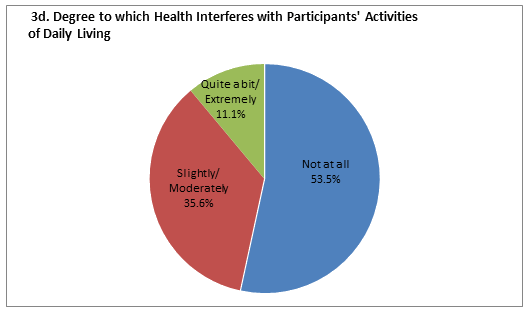
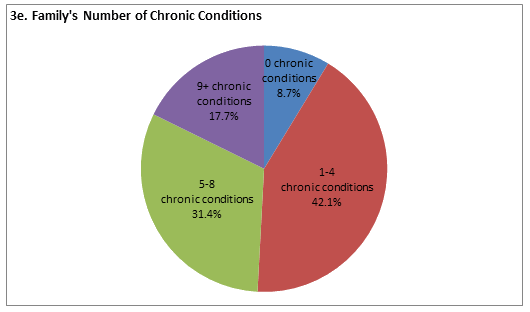 Figure 3: Health conditions in rural families (n=271). a: Participants' number of chronic conditions; b: Participants' self-reported health status; c: Participants' health status compared with previous year; d: Degree to which health interferes with participants' activities of daily living; e: Family's number of chronic conditions.
Figure 3: Health conditions in rural families (n=271). a: Participants' number of chronic conditions; b: Participants' self-reported health status; c: Participants' health status compared with previous year; d: Degree to which health interferes with participants' activities of daily living; e: Family's number of chronic conditions.
Usual source of care: Although having health insurance does not guarantee access to a usual source of care32, 79% of participants reported having a doctor or other healthcare professional that they usually see (Fig4). Similarly, 61.3% reported their partners had a usual provider, and 91.7% reported their children had a usual provider. Reports were not significantly different for the privately insured (89.8%) and the publicly insured (89.5%) groups; although this rate was significantly different between the uninsured (53.4%) and insured groups (?2=33.17, p=.000). Despite relatively high rates of having a usual provider, 28.8% of respondents reported going to the emergency department (ED) because the regular doctor was not available. Publicly insured respondents reported significantly greater ED use (30.1%) than either the privately insured (26.3%) or uninsured (25.0%) respondents. Barriers that participants confront in accessing their usual source of care, such as inflexible work schedules or delaying care to the point of needing emergency services, emerged in the qualitative data illustrating ways in which health management strategies are often ineffective.
Respondents also recognized the value of having a usual source of care with 78.4% of participants reporting that seeing a regular doctor influences their own health; 81.8% reporting it influenced their partner's health; and 80.2% reporting it influenced their children's health.
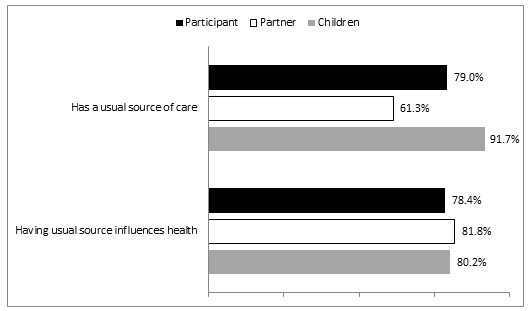 Figure 4: Usual source of care (N = 271).
Figure 4: Usual source of care (N = 271).
Qualitative
Usual source of care: Qualitative responses underscored the quantitative findings regarding having a usual source of care. Respondents identified benefits of having a consistent relationship with a healthcare provider who knows the past medical history. Erin of Ohio noted:
Well, it's, it's [sic] best to go to the doctor you already know because they know you, they know your history, you know, and then he could help you better. So it does benefit you.
Nanette of New York noted that having the same doctor improved the quality of care:
Interviewer (I): Does always seeing the same doctor influence your health?
Respondent (R): Yes, I'm guaranteed that, the fact that she knows my family and our needs other than seeing a stranger that wouldn't know that, 'Oh, you know, something doesn't look right'. You know? With her knowing us and knowing all three of the children and my husband, she can pretty much basically tell when there's something wrong.
Uninsured participants, although less likely to have a usual source of care, also noted the benefits, as in this example from Marilynn from Oregon:
I: Do you have a doctor or other healthcare professional that you usually see?
R: Yeah, the [name] Health Department.
I: So do you usually see the same person there?
R: Oh yea. Yes. Yeah definitely.
I: And do you think that always seeing the same person influences your health?
R: In a good way, yeah. Definitely.
I: And because?
R: Because they, you're not going from one person to the next, them not knowing what's common for you basically.
Mothers also indicated that the healthcare professional they usually see also sees their children. Nan from Maryland shared, 'And my doctor sees my children. Dr [name] is their - my children's doctor too'. In response to whether she thought it helps to always see the same doctor, Nan added, 'Yeah. It makes me more comfortable. And plus the doctor knows what I'm talking about, or they can see improvement'. Similarly, Jane from Massachusetts shared, 'Yes, it's comforting because she knows the history'. Gwenyth from Minnesota concured with, 'I think it helps because your prior medical situation'.
Management of health: Personal and family health was difficult for these women to manage within the context of their limited resources. Analysis of the qualitative data revealed two main themes regarding how health conditions were managed: (i) women were not engaged in managing their overall health; and (ii) ineffective utilization of healthcare services.
Not engaged in health management Many respondents did not report active engagement in their health. This lack of engagement must be understood within the context of their limited resources. The following excerpt from the interview with Ginny of Indiana demonstrates the lack of perceiving health as a basic necessity or resource to be managed:
I: To what extent do you think your income is enough for you to live on? Would you say it's not at all adequate? It can meet necessities only? You can afford some of the things you want, but not everything? You can afford about everything. Or you can afford about everything and still save money?
R: Three.
I: OK. And um when you think about the things you can afford, um those things [that are] necessities, what do you think of?
R: Keeping everybody fed.
I: OK.
R: Keeping our car going. Um.
I: OK. You mentioned also the phone as being a necessity. Anything else?
R: We like our cable.
I: OK. [pause] Alright.
R: We like our cable. I don't know if it's a necessity, but that's what we want.
At a later point, the interviewer inquired about changes in health. Ginny indicated that none of her previous health issues had been resolved and no new health issues have emerged:
I: At the previous interview, you mentioned that you had been dealing with depression/anxiety and that you were smoking. How has your health been since the last interview?
R: The same.
I: OK. Have there been any changes in your health?
R: No.
I: OK. Have you developed any new medical conditions?
R: No.
I: Since the last interview, have you had any injuries, surgeries or serious illnesses?
R: No.
I: Um. Since the last interview, have any of your health problems been resolved?
R: No.
I: OK. So you are still dealing with both. You are still smoking and you still have depression/anxiety?
R: Yes.
Shortly after addressing changes in health status, the interviewer inquired about barriers to accessing healthcare services:
I: OK. Has there ever been a time when you needed to see a doctor or go to the hospital but did not go?
R: Yes.
I: OK. And can you tell me a little about this?
R: Well, just when you get a really bad cold or bronchitis, um and that happens about every winter, and just feel like you need to go get something, and you just can't go and I could really, really need to get an annual exam, but.
I: OK.
R: Haven't done that.
I: And do you not do it because of the money issue?
R: Yeah. I should be able to get that squared around after we get the bills caught up.
I: OK.
R: I am going to make sure I have enough to go somewhere and get my annual exam. I haven't had one for three years.
Ginny reported that no new health issues had emerged for her, but she also shared that she has not had a women's health examination in the past 3 years (which would be prior to any data collection for this study). At the point of the interview when directly asked about needs to see a healthcare professional, she recognized this as a need. However, at the point of the interview quantitatively asking if her family's income is enough to live on, she passed over the first 2 response categories (1=it is not at all adequate; 2=it can meet necessities only) and selected the third (you can afford some of the things you want but not everything). This example suggests that Ginny did not consider the cost of managing her health as one of her necessities, despite the fact that later in the interview she acknowledged that she had not had an annual examination 'because of the money issue' and stated 'I should be able to get that squared around after we get the bills caught up'.
Lack of engagement was also exemplified in terms of the inability or proactive decision not to see a doctor to improve health status, the latter of which may exemplify the culture of self-reliance7,20 . Deborah of New Hampshire, after reporting that she struggled with chronic pain, depression, anxiety, migraines, vision problems, a learning disability, and permanent physical disability had the following exchange with the interviewer:
I: Now, have there been any changes in your health that are better or worse or any new conditions that you might have developed?
R: Nothing new.
I: Oh, that's good.
R: I think that's enough.
I: Since our last interview, have any of your health problems been resolved?
R: No.
I: You just know what they are now?
R: Yeah, well, I've always known what they were. You know, you don't need a doctor anymore unless you need medicine.
A similar exchange occurred with Lenore of Indiana:
I: Um. At the previous interviews you mentioned you had been dealing with a couple of different health issues. The notes from the past interview said that you had been dealing with depression/anxiety, frequent colds/flu/sinus, um eye or vision issues, joint problems, skin problems, alcohol/tobacco use, anemia, migraine headaches and arthritis. How has your health been since the last interview?
R: It hasn't changed much.
The interviewer followed up:
I: OK. Alright. Have you developed any new medical conditions?
R: No. Thank goodness.
I: OK. Since the last interview, have you had any injuries, surgeries, or serious illnesses?
R: No.
I: Since the last interview, have any of your health problems been resolved?
R: I wish.
I: OK. So no?
R: No.
Moments later, the interviewer inquired about healthcare provider visits:
I: About how many times have you been to see a doctor or other healthcare provider since the last interview?
R: Never.
Further, when asked if there had ever been a time when Lenore needed to see a doctor or go to the hospital but did not go, she replied, 'No'. Thus, despite reporting numerous health problems, she did not indicate need for health services.
Inability or unwillingness to improve health status was further exemplified by Louanne from Indiana who reported her current health as 'somewhat worse' than a year ago and indicated that her physical health had caused her to accomplish less than she would like:
R: My big health issue is that I am too fat. I am just too fat. And so it's miserable. So I just sit all the time.
I: OK.
R: And don't do anything.
However, despite Louanne's recognition that her physical health presented barriers in her daily life, and weight loss is a behavior over which she has some control, at a later point in the interview, she indicated that she did not expect her health to get better or worse. Conversely, Nan of Maryland expressed expectation that her health issue may never resolve:
I: What would make life better for your family, and why?
R: If I could get my back straightened out.
I: Get your back straightened out... And was your doctor very hopeful about that happening, does he think if you keep on having these treatments that'll happen, or-
R: No, basically I have to live with this.
I: Oh.
R: And then if they do surgery, Once they do do it, I have so many ruptured discs, that it's going to be like domino effect, and once they do it, and put a rod in, then it's going to be going down, then it's just going to keep on going. I'll be in and out of surgery all the time.
In each of the above examples, participants reported their conditions as static with no hope of resolution despite the fact that some of the reported conditions may be addressed with proper medical care and/or personal health behaviors, such as improved nutrition and exercise, further supporting the lack of engagement in health management.
Ineffective utilization of health care This theme describes the challenges confronted by women in the present study that contributed to ineffective utilization of health care for a variety of reasons. Despite reporting a usual source of care, Rebecca of Ohio described competing demands of work and seeing her physician:
Um, yeah. If I have a doctor's appointment, or- they don't like me to take off because they're short-handed. And they're so cheap they won't hire very many other people, so everybody's gotta cover it, so, it's- it's tough.
Similarly, Joanne of Maryland described how the distance to her pediatrician's office prompted her to make use of the ED instead:
R: We've taken the kids to the emergency room too...
I: And when the children went, is it because...
R : Just the doctor wasn't in and [name of location of pediatrician's office] was too far away. We didn't have the van, and we took, it was too far away to take the kids to see some half-time-want-to-be-doctor. So we take them to the emergency room. They didn't like it, but they have doctors. I don't want to hear it. Something's wrong with one of my kids, I want to know.
Nan of Maryland, who had a chronic back problem, reported using emergency services reactively rather than proactively managing her condition:
Well there was a couple of times when I had to go to the emergency room, but that was, I think it was last year before - when - I - my back was just out of sorts, and everything, and I couldn't get a hold of a doctor.
The following interchange with Nan exemplifies the barriers she confronted in following the advice of her healthcare providers:
R: I lost disability. And my medical. I've lost my medical [insurance]...
I: And you don't yet understand why. And you're fighting that, but you're going to figure that out.
R: Well, one doctor says I can go to work, but I can't sit long, I can't stand long, no bending, not dealing with the public, and to take breaks as often as I can, and there's like sixty thousand jobs out there nationwide. Where is there one in [this] county that I can do this? And yet, I've got two doctors statin' that I'm disabled, that I'm seein', but because of one doctor that I haven't seen in a while that was givin' me the back injections, my- I got a, um- I got a- I'm late on his payment bills, and he said that I'm able to work, so I think that's why.
I: Is he going to be the one you're going to see shortly?
R: No, I see the Family Clinic [in university town in neighboring state], and they can't write a report because they do Social Security re-evaluations.
I: So you need another opinion.
R: Basically, yeah.
When asked if she had thought about applying for Medicaid, Tailyn of Nebraska replied:
R: I, I did, but, I know the lady down there real well, and she said that all the cut's that were going on that she doubted, very much, that I'd get it.
I: Oh.
R: There was a young pregnant woman that were [sic] turned away, so....
At a later point in the interview she was asked if she was able to get medical care when needed:
R: Uh, that's on hold.
I: So, you haven't been going to the doctor lately?
R: No.
I: What about medicines, when you need medicines?
R: I have medicine, I need medicine, but I can't afford them.
I: So, you're just...
R: Doing without.
Despite the fact that Tailyn might have been eligible for Medicaid, she opted to not apply and simply go without.
Some women reported not going to the doctor/healthcare provider at all. Rather, they relied on family planning or other non-general medical clinics for their care. This exchange with Lenore of Indiana is illustrative of that situation:
I: How about to get to medical appointments?
R: Mmmmm. I don't go to the doctor.
I: OK. If you were to go to, um, any kind of healthcare provider if you don't have a specific doctor? Hospital? Anything?
R: Um. The hospital... I can get there within 20 minutes.
I: OK.
R: Normally I just go to Planned Parenthood.
These examples suggest that factors both within and outside of participants' control contributed to ineffective utilization of healthcare services.
Discussion
The rural low-income women in this study provide important insights to consider as reforms to the healthcare system in the USA and other geographically large, developed countries (eg Australia, Canada) are designed and implemented. The majority of participants reported having a usual provider and expressed great comfort in this. Participants appreciated receiving care from someone who knew their own and their family members' medical history. Previous studies have found that a consistent relationship between patient and provider is associated with a broad range of positive health related outcomes33. However, almost one-third of participants reported using the ED because their regular doctor was unavailable. This is consistent with other research that has shown rural individuals often identify a usual source of care, but have more difficulty reaching providers after hours34. The higher ED use among publicly insured respondents compared with privately insured respondents is consistent with research in non-rural samples35. Additionally, while Planned Parenthood as a usual source of care is a viable option for reproductive health needs, they do not provide whole-health services, such as immunizations or general wellness care.
Policy reforms that simultaneously recognize and value the need for a usual source of care and the challenges of providing such care in rural settings should be promoted. Initiatives such as the Patient-Centered Medical Home (PCMH) and Accountable Care Organizations (ACOs) are designed to improve the quality of service delivery while reducing costs. Health services researchers have suggested a number of ways to creatively establish PCMHs and ACOs in rural areas36-39 in the light of structural challenges, and specifically limited providers39. In the USA, much of the care in rural areas is provided by federally qualified community health centers, and the Affordable Care Act dedicates $11 billion in new funding over 5 years to expand their reach40. Strategies that will assist these centers in becoming National Committee for Quality Assurance-certified PCMHs will help to promote patient-centered and continuous care in rural areas. To achieve this, Nutting et al propose expanding the concept of the medical home to what they refer to as a 'healthcare neighborhood', which coordinates care across a broad network of hospitals, primary and special providers, nursing homes, and social service agencies (p440)38. They cite the importance of thinking broadly about the 'neighborhood boundaries', which may extend into urban areas through telemedicine or 'e-health'. Thinking broadly will help to address a critical issue in implementing reforms, namely, the shortages of primary and mid-level healthcare providers.
Similarly, implementing ACOs will require expanding what might be considered obvious or expected organizational entities. To be successful in rural areas, flexible models and payment structures that can be adapted to fit local communities and market conditions are critical. In fact, an analysis of health care in rural Vermont suggested that ACOs were possible in rural areas, but would require a consolidated performance pool that involved multiple payors and/or expanding the ACO to include multiple hospitals in order to achieve statistically meaningful measures of performance37. The Vermont evaluation also suggested that potential ACOs would depend more heavily on state and national infrastructure due to greater complication concerning governance issues when multiple insurers or hospital entities were included. Shortell et al suggested developing 'virtual ACOs' by following the example of Community Care of North Carolina36, which formed a 'virtual' physician organization comprised of several small, independent physician practices. The necessary leadership to provide infrastructure and resources, implement electronic medical records, and share information could be managed by a consortium of individual physicians in rural areas, a local medical foundation, a state Medicaid agency, or a similar organization. Further, Shortell et al argued that ACOs actually may help to address the issue of physician shortage by permitting primary providers to more efficiently care for greater numbers of patients through team-based practice while simultaneously increasing payment incentives. Combining this approach with a flexible package of retention measures (eg professional development, childcare, housing accommodations), as in Australian pilots, may further increase retention1).
In both PCMHs and ACOs, health information technology (IT) is going to be critical and will require systems that can support 'virtual and asynchronous communication' (p442)38. In fact, Shields et al noted that performance improvement for rural providers requires the ability to integrate small practices and use web-based communication to promote partnership41. However, a specific challenge to implementing health IT in rural communities is the gaps in broadband coverage. Beacon communities are attempting to overcome these challenges and still use health IT and telemedicine effectively41. For example, in rural Minnesota, telemedicine technologies will be implemented in schools and public health centers to facilitate treatment planning and care management between primary providers and school nurses for asthma. By relying on centers with IT available, they hope to overcome some of the access barriers. However, more work will need to be done to increase health IT capabilities to effectively coordinate care across time and providers, but this is not simply a rural phenomenon for it is true throughout the USA42.
Beyond the structural and cultural barriers to health care inherent in rural communities that may be attended to through the PCMH and/or ACO, the present findings demonstrate that low-income rural women and their families confront specific, interrelated challenges affecting their health management. These challenges can be described using a model proposed by Anderson and Newman21 that categorizes individual determinants of healthcare utilization into three categories: (i) predisposition to seek help; (ii) ability to access services; and (iii) illness level. First, these families are managing multiple healthcare needs with limited resources. As has been noted in other studies, low-income families make choices between basic necessities43, and research shows that families make 'tradeoffs' when it comes to managing health care44. Some mothers in the present study reported forgoing their own care in order to provide needed care to their children. Reports of primary medication non-adherence underscore this, as they were higher among adults than they were for children. The rate of delaying or not filling a prescription medication was also higher in this study than it was in another study of rural individuals, which reported a 21.6% rate45. This may reflect the fact that the present study focused on families with dependent children, whereas the comparator study was of individuals, only some of whom had dependent children.
Interestingly, several mothers did not identify healthcare needs, such as seeing a physician or medication, as basic necessities like food, shelter, and clothing, despite reporting health conditions that interfere with daily life and doing without such health care. Second, physicians and other healthcare providers were perceived as useful only for meeting prescription medication needs. They were not seen as partners in these participants' health or as a source of knowledge about how to achieve good health. Third, these patients had very low levels of engagement in their health and health care. They were often passive in managing their health, chalking up their good health to luck or good fortune as opposed to active efforts to achieve and maintain good health. This is consistent with the literature on fatalism, or a global outlook that health is destined to be a certain way and cannot be altered through changes in health behaviors46. However, this fatalism may serve as adaptive coping in the context of limited resources rather than a true belief that they are unable to take actions that can influence their health46. The lack of engagement also may reflect low health literacy, which has been documented in rural areas47, and this is consistent with the demographics of the sample, where more than one-half of participants had a high school education or less. Finally, little attention was given to planning for future health. Many women reported reacting to disease exacerbations and events as opposed to actively managing chronic conditions to prevent exacerbations and further progression.
Given the health challenges presented by the present study participants and the tradeoffs often made to address them, another strategy that could be utilized to improve rural health is personalized health planning (PHP)48. Personalized health planning is a strategic approach to care that engages patients with their providers to develop an individualized wellness and therapeutic plan. There are three main goals: (i) health risk assessment (HRA); prediction, and monitoring; (ii) patient participation and activation; and (iii) prevention or minimization of disease. Personalized health planning provides a mechanism for patients and providers to develop a collaborative relationship and work together to create and enact an individualized wellness and therapeutic plan. Through the planning process, patients are educated about their existing health conditions, as well as about their risks for future disease and how to mitigate them. In a rural low-income population in particular, additional time can be spent talking to the patient about what might get in the way of successfully enacting the plan, from challenges within the family unit to structural challenges in the community to financial challenges, and how to address these barriers. In other words, the planning process may increase patients' understanding of the tradeoffs involved in managing the healthcare needs of their families (eg should they decide to forgo medication for the mother so that a child can have medication). This also may improve medication adherence, given studies that have shown a positive patient-provider relationship is associated with better adherence49. Personalized health planning also can enhance a patient's understanding of health as a resource that can be managed, as opposed to something over which they do not have much control. The PHP also may help to frame health needs as a basic necessity in cases of chronic illness. Given the culture of self-reliance in rural areas15,50, PHP fits well by generating a process over which the patient has significant control and allows for providers to be seen as more than medication dispensers. Additionally, PHP provides a family context for health behavior change, so that all family members may benefit from positive behaviors like better nutrition or increased exercise.
Personalized health planning, combined with PCMHs and ACOs specifically adapted to rural settings, has the potential to benefit rural families who struggle to juggle resources, live with chronic conditions, and access knowledge about their specific health issues. In fact, Nutting et al noted that the 'patient-centered part of the medical home depends on having activated, engaged patients' (p439)38. The PHP provides a platform for patient engagement by promoting patient-provider interaction and developing plan that can be shared across multiple entities, thereby promoting coordinated care, a necessary component of PCMHs and ACOs. Finally, the PHP has the added benefit of providing an architecture through which national data can be captured in a uniform fashion and analyzed globally for patient population features, expenditures, and health outcomes51, a necessary component of comprehensive monitoring and evaluation of healthcare reforms1.
For PCMHs, ACOs, and PHPs to be implemented effectively, addressing the shortages of qualified health professionals in rural areas is necessary52. Evidence suggests there are clear, effective ways to increase both the supply of primary providers and the availability of services, including recruiting students to healthcare fields who are more likely to serve in rural areas and offering financial and lifestyle incentives for providers53. Bailey noted the Accountable Care Act addresses many of these issues, but these provisions have been an 'unsung' component of the law54. Following are just some of the programs and strategies in the law designed to provide greater and/or new funding to increase the rural primary care and allied health workforce: (i) authorization for increased and new funding for medical schools to recruit students most likely to practice in rural areas, new primary care residency programs with priority for those affiliated with Area Health Education Centers (AHECs), graduate medical education in rural, federally qualified health clinics and community-based settings in underserved areas, state and local training of mid-career and allied health professionals, and general, pediatric, and public health dentistry programs with a record of training students for rural populations; (ii) healthcare workforce loan programs for pediatric, medical, surgical, behavioral health, and public health specialists in underserved areas; (iii) funding for nurse-managed health clinics in underserved areas; and (iv) continuing and expanding AHECs. Furthermore, the law provides payment provisions to address reimbursement inequality, which may increase financial viability of existing practices, as well as incentivize providers to establish practices in rural areas54. For example, the law provides for a 10% incentive payment under Medicare for providers practicing in health professional shortage areas. There is a bonus payment for Medicare services provided by general surgeons and home health providers in rural areas. Adjustments were made to the Geographic Practice Cost Indices of Medicare to reduce payment disparities. Medicare also will begin paying for one annual personalized health planning visit in 2012. Despite the various provisions, it is unclear whether they are sufficient to solve these key structural issues and/or how changes at one level (eg reimbursement structure, provider training, community health centers) will influence (positively or negatively) changes at another53. As the Accountable Care Act is rolled out, it will be critical to monitor implementation of these strategies to assess intended and unintended consequences and determine whether there is both sufficient and effective rural healthcare delivery.
Limitations
This study has several limitations. First, although the qualitative data provide much needed depth of understanding, the small sample size limits generalizability. Second, these data are self-reported and include discussion of sensitive health information. Thus, there may be bias in reporting. Third, comparison urban, suburban, or middle/high income groups are not available to definitively say these are exclusively rural phenomena. However, this does not discount the importance of these findings for rural women and their families, and the need for reforms to address these phenomena in rural areas and beyond as appropriate. Fourth, there is no information from local services providers. These voices may have added important information about health decision-making that is not provided in the current study. Finally, the data are 8 years old. However, a recent publication showed that the overall state of health care for rural Americans has not improved within the last decade6 and, consequently, the experiences represented by these women in 2002-2003 are likely to hold true today.
The findings suggest that rural low-income women and their families may benefit from healthcare reforms designed to personalize care and promote self-reliance, which attend to rural cultural values. However, if careful consideration is not paid to the unique challenges of implementing these mandates in a rural setting, these benefits will not be realized. Approaches such as PCMHs, ACOs, and PHPs must be carefully designed to consider the existing healthcare challenges currently facing rural America: recruitment and retention of providers, low engagement in health, and, perhaps most importantly, cultural barriers that may prevent rural Americans from 'buying in' to a new model of care. By cons, idering the ways in which rural individuals approach their health and make decisions about healthcare utilization, strategies for implementing healthcare reform can be developed that attend to the unique needs of rural America, improve individual health status, and reduce health disparities.
References
1. Wakerman J, Humphreys JS. Sustainable primary healthcare services in rural and remote areas: Innovation and evidence. Australian Journal of Rural Health 2011; 19(3): 118-124.
2. Bailey J. Why healthcare reform can't wait: The benefits of health reform for rural America. Lyons, NE: Center for Rural Affairs, 2010.
3. Murray LR. Health reform to have significant benefits for rural Ameri, cans. The Nation's Health 2011; 41(4): 3.
4. Jones CA, Parker TS, Ahearn M, Mishra AK, Variyan JN. Health status and healthcare access of farm and rural populations. Washington, DC: US Department of Agriculture: Economic Research Service, 2009.
5. Bennett KJ, Olatosi B, Probst JC. Health disparities: A rural-urban chartbook. Columbia, SC: University of South Carolina: South Carolina Rural Health Research Center, 2009.
6. Seshamani M, Van Nostrand J, Ken, nedy J, Co, , chran C. Hard times in the heartland: Healthcare in rural america. Washington, DC: US Department of Health and Human Services; 2009.
7. Nelson WA. The challenges of rural healthcare. In: CM Klugman, PM Dalinis (Eds). Ethical Issues in Rural Healthcare. Baltimore, MD: Johns Hopkins University Press, 2008; 34-59.
8. Monnat SM, Beeler Pickett C. Rur, al/urban differences in self-rated health: Examining the roles of county size and metropolitan adjacency. Health & Place 2011; 17(1): 311-319.
9. Bourke L, Humphreys JS, Wakerman J, Taylor J. From 'problem?describing' to 'problem?solving': Challenging the 'deficit'view of remote and rural health. Australian Journal of Rural Health 2010; 18(5): 205-209.
10. Ziller EC, Coburn AF, Anderson NJ, Loux SL. Uninsured rural families. Journal of Rur, al Health 2008; 24(1): 1-11.
11. Ziller EC, Coburn AF, Yousefian AE. Out-o, f-pocket health spending and the rural underinsured. Health Affairs 2006; 25(6): 1688.
12. Lenardson JD, Ziller EC, Coburn AF, Anderson AJ. Profile of rural health insurance coverage: A chartbook. Portland, ME: University of Southern Maine: Maine Rural Health Research Center, 2009.
13. Merwin E, Snyder A, Katz E. Differential access to quality rural healthcare: Professional and policy challenges. Family and Community Health 2006; 29(3): 186.
14. South Carolina Rural Health Research Center. Mode of travel and actual distance traveled for medical or dental care by rural and urban residents. Columbia, SC: University of South Carolina: South Carolina Rural Health Research Center; 2006.
15. Morgan K, Hart AM. Families in rural settings: Values regarding acute respiratory infections. Families, Systems & Health 2009; 27(1): 85-97.
16. Denavas-Walt C, Proctor BD, Smith JC. U.S. census bureau current population report: Income, poverty, and health insurance coverage in the United States: 2009. Washington, DC: U.S. Government Printing Office, 2010.
17. Economic Research Service. Rural income, poverty, and welfare: Poverty geography. Washington, DC: United States Department of Agriculture, 2010.
18. Beard JR, Tomaska N, Earnest A, Summerhayes R, Morgan G. Influence of socioeconomic and cultural factors on rural health. Australian Journal of Rural Health 2009; 17(1): 10-15.
19. Harvey DJ. Understanding australian rural women's ways of achieving health and wellbeing-a metasynthesis of the literature. Rural and Remote Health 7: 823. (Online) 2007. Available: www.rrh.org.au (Accessed 14 February 2012).
20. Hall S, Holman CDAJ, Threlfall T, Sheiner H, Phillips M, Katriss P et al. Lung cancer: An exploration of patient and general practitioner perspectives on the realities of care in rural western Australia. Australian Journal of Rural Health 2008; 16(6): 355-362.
21. Andersen R, Newman JF. Societal and individual determinants of medical care utilization in the United States. Milbank Quarterly 2005; 83(4): 1-26.
22. Gruman J, Rovner MH, French ME, Jeffress D, Sofaer S, Shaller D et al. From patient education to patient engagement: Implications for the field of patient education. Patient Education and Counseling 2010; 78(3): 350-356.
23. Simmons LA, Anderson EA, Braun B. Health needs and healthcare utilization among rural, low-income women. Women and Health 2008; 47(4): 53-69.
24. Office of Management and Budget. Measuring rurality: Rural-urban continuum codes. Washington, DC: US Department of Agriculture: Economic Research Service; 2003.
25. Sturm R, Wells KB. Does obesity contribute as much to morbidity as poverty or smoking? Public Health 2001; 115(3): 229-235.
26. Creswell JW, Fetters MD, Ivankova NV. Designing a mixed methods study in primary care. Annals of Family Medicine 2004; 2(1): 7-12.
27. Long SK, Coughlin T, King J. How well does Medicaid work in improving access to care? Health Services Research 2005; 40(1): 39-58.
28. DeVoe JE, Tillotson CJ, Wallace LS. Usual source of care as a health insurance substitute for US adults with diabetes? Diabetes Care 2009; 32(6): 983-989.
29. Burck C. Comparing qualitative research methodologies for systemic research: The use of grounded theory, discourse analysis and narrative analysis. Journal of Family Therapy 2005; 27(3): 237-262.
30. Braun V, Clarke V. Using thematic analysis in psychology. Qualitative Research in Psychology 2006; 3(2): 77-101.
31. Lincoln YS, Guba EG. Paradigmatic controversies, contradictions and emerging confluences. In: NK Denzin, YS Lincoln (Eds). Handbook of qualitative research. Thousand Oaks, CA: Sage, 2000; 163-188.
32. DeVoe JE, Fryer GE, Phillips R, Green L. Receipt of preventive care among adults: Insurance status and usual source of care. American Journal of Public Health 2003; 93(5): 786-791.
33. Rosenthal TC. The medical home: Growing evidence to support a new approach to primary care. Journal of the American Board of Family Medicine 2008; 21(5): 427-440.
34. Maine Rural Health Research Center. Rural-urban differences in healthcare access vary across measures. Portland, ME: University of Main Muskie School of Public Service; 2009.
35. Peppe EM, Mays JW, Chang HC, Becker E, DiJulio B. Characteristics of frequent emergency department users. Washington, DC: Kaiser Family Foundation, 2007.
36. Shortell SM, Casalino LP, Fisher ES. How the center for Medicare and Medicaid innovation should test accountable care organizations. Health Affairs 2010; 29(7): 1293-1298.
37. Hester J, Lewis J, McKethan A, Fund C. The Vermont accountable care organization pilot: A community health system to control total medical costs and improve population health. New York, NY: Commonwealth Fund, 2010.
38. Nutting PA, Crabtree BF, Miller WL, Stange KC, Stewart E, Jaén C. Transforming physician practices to patient-centered medical homes: Lessons from the national demonstration project. Health Affairs 2011; 30(3): 439-445.
39. Hancock C, Steinbach A, Nesbitt TS, Adler SR, Auerswald CL. Why doctors choose small towns: A developmental model of rural physician recruitment and retention. Social Science & Medicine 2009; 69(9): 1368-1376.
40. Arora S, Kalishman S, Dion D, Som D, Thornton K, Bankhurst A, et al. Partnering urban academic medical centers and rural primary care clinicians to provide complex chronic disease care. Health Affairs 2011; 30(6): 1176-1184.
41. Shields MC, Patel PH, Manning M, Sacks L. A model for integrating independent physicians into accountable care organizations. Health Affairs 2011; 30(1): 161-172.
42. Blumenthal D. Stimulating the adoption of health information technology. New England Journal of Medicine 2009; 360(15): 1477-1479.
43. Kushel MB, Gupta R, Gee L, Haas JS. Housing instability and food insecurity as barriers to healthcare among Low?Income americans. Journal of General Internal Medicine. 2006; 21(1): 71-77.
44. Regan S, Wong S. Patient perspectives on primary healthcare in rural communities: Effects of geography on access, continuity and efficiency. Rural and Remote Health 9: 1142. (Online) 2009. Available: www.rrh.org.au (Accessed 14 February 2012).
45. Wroth TH, Pathman DE. Primary medication adherence in a rural population: The role of the patient-physician relationship and satisfaction with care. Journal of the American Board of Family Medicine 2006; 19(5): 478-486.
46. Powe BD, Finnie R. Cancer fatalism: The state of the science. Cancer Nursing 2003; 26(6): 454.
47. Paasche?Orlow MK, Parker RM, Gazmararian JA, Nielsen?Bohlman LT, Rudd RR. The prevalence of limited health literacy. Journal of General Internal Medicine 2005; 20(2): 175-184.
48. Williams RS, Willard HF, Snyderman R. Personalized health planning. Science 2003; 300(5619): 549.
49. DiMatteo MR. Variations in patients' adherence to medical recommendations: A quantitative review of 50 years of research. Medical Care 2004; 42(3): 200-209.
50. Murimi MW, Harpel T. Practicing preventive health: The underlying culture among Low?Income rural populations. Journal of Rural Health 2010; 26(3): 273-282.
51. Dinan MA, Simmons LA, Snyderman R. Personalized health planning and the patient protection and affordable care act: An opportunity for academic medicine to lead healthcare reform. Academic Medicine 2010; 85(11): 1665-1668.
52. Florell ML. Rural healthcare workforce: Opportunities to improve care delivery. Lyons, NE: Center for Rural Affairs; August 2009. Available: http://files.cfra.org/pdf/HealthCare_Workforce.pdf
53. McEllistrem-Evenson A. Informing rural primary care workforce policy: What does the evidence tell us? A review of rural health research center literature, 2000-2010. (Online) 2010. Available: http://www.ruralhealthresearch.org/pdf/primary_care_lit_review.pdf (Accessed 14 February 2012).
54. Bailey JM. Healthcare reform, what's in it? Rural communities and rural medical care. Lyons, NE: Center for Rural Affairs, 2010. Available: http://files.cfra.org/pdf/Rural-Communities-and-Medical-Care-brief.pdf

